Abstract
Background:
Helicobacter pylori (H. pylori) is a group 1 carcinogen and the etiological agent of gastric diseases such as gastritis, ulcers, and gastric cancer. It infects approximately half of the world’s population. Risk factors associated with H. pylori infection include socioeconomic status, lifestyle, and diet.
Objectives:
This study aimed to evaluate the association between eating habits and H. pylori infection in patients from a reference hospital in Central Brazil.
Design:
This cross-sectional study included 156 patients from 2019 to 2022.
Methods:
Data were collected using a structured questionnaire on sociodemographic and lifestyle characteristics and a validated food frequency questionnaire. The H. pylori infection status (positive versus negative) was determined using the histopathological method. After grams/day, foods were stratified into tertiles of consumption (low, medium, and high). Simple and multiple binary logistic regression models were used in the analysis of odds ratios (ORs) and their respective 95% confidence intervals (CIs), with a 5% significance level.
Results:
The prevalence of H. pylori infection was 44.2% (69/156 patients). Infected individuals had a mean age of 49.6 ± 14.6 years; 40.6% were men, 34.8% were aged 60 years or older, 42.0% were unmarried, 7.2% had higher education, 72.5% were non-white, and 30.4% were obese. In the H. pylori-positive group, 55.1% were alcohol drinkers and 42.0% were smokers. The results of multiple analyses showed that the chance of H. pylori infection was higher among male participants (OR = 2.25; CI = 1.09–4.68) and individuals with obesity (OR = 2.68; CI = 1.10–6.51). Participants with moderate consumption of refined grains (bread, cookies, cakes, breakfast cereal) (OR = 2.41; CI = 1.04–5.62) and fruits (OR = 2.53; CI = 1.08–5.94) were more likely to be infected.
Conclusion:
In this study, male sex, obesity, and the consumption of refined grains and fruits were positively associated with H. pylori infection. Further research is needed to investigate this association and elucidate the underlying mechanisms.
Background
Helicobacter pylori (H. pylori) is one of the most prevalent human pathogens, affecting half of the world’s population. Prevalence can vary significantly by geographic region and is the highest in developing countries. 1 The prevalence of H. pylori infection in Latin America and the Caribbean is estimated to be 69.26% in adults. 2 Brazil is the largest country in Latin America and has regional differences in the quality of life and health. This reflects a great variation in the prevalence of H. pylori infection, which is higher in the north than in the south of the country.3,4 In the Midwest region, a prevalence of 69.2% and 61.1% has been reported.5,6
Chronic infection caused by H. pylori can lead to gastrointestinal diseases such as gastritis, peptic ulcer, mucosa-associated lymphoid tissue lymphoma, and gastric adenocarcinoma (GAd). 7 Since 1994, H. pylori has been recognized as a group 1 carcinogen by the International Agency for Research on Cancer. 8 In addition, H. pylori-related extragastric manifestations have been reported in the scientific literature. Although for several of these supposed associations, the potential pathogenic mechanism remains obscure, the eradication of H. pylori is already a well-established therapeutic alternative for iron deficiency anemia, primary immune thrombocytopenia, and vitamin B12 deficiency.9–11
The main known risk factors for H. pylori infection include conditions related to low socioeconomic status such as poor sanitation, inadequate hygiene practices, overcrowding, and intrafamily grouping. In addition, diet is an important risk factor for infection. 12
Frequent consumption of fresh fruits and vegetables has been associated with protection against H. pylori infection. 13 In addition, a diet consisting of a high intake of whole grains, roots and tubers, vegetables, mushrooms, various beans, vegetable oils, nuts, and seeds is associated with a decreased risk of infection. 14 These associations may be attributed to the properties of some compounds present in these foods such as vitamin C, polyphenols, and flavonoids. These compounds may protect the gastric mucosa and inhibit the colonization of bacteria. 15
In contrast, a diet high in carbohydrates, sweets, sausages, hamburgers, mayonnaise, and soft drinks was positively associated with H. pylori infection.16,17 Furthermore, a dietary pattern characterized by a high consumption of refined grains, pickled vegetables, bacon, salted fish, salted pickled eggs, processed and cooked meat, wine, and tea is associated with an increased risk of the infection. 14
Brazil, especially in the Midwest region, has a high prevalence of H. pylori infection. Since the presence of this infection can be influenced by diet, it is important to know the foods that act as protective factors as well as those that may favor infection. However, data on the association between dietary habits and H. pylori infection in this region are limited. Therefore, this study aimed to evaluate the association between eating habits and H. pylori infection in patients admitted to a reference hospital in the Brazilian Midwest.
Methods
Study design and participants
This was a cross-sectional study conducted from March 2019 to February 2022 at a referral hospital located in Central Brazil. Participants were recruited from the Department of Digestive Tracts.
Dyspeptic patients of both sexes aged between 18 and 75 years who underwent upper digestive endoscopy were included. Individuals who did not have an available histopathology report, those with cancer, or those without physical and/or psychological conditions to participate in the study were excluded.
Ethical aspects
The reporting of this study conforms to the STROBE statement. 18
Data collection and evaluation
Data were collected using structured questionnaires completed during an interview and transferred online to the Research Electronic Data Capture (REDCap™) EPGC version 7.4.4.
A food frequency questionnaire (FFQ), validated in Brazilian populations with patients treated for colorectal cancer and patients from a case–control study of GAd, was administered during the interview.19,20 The FFQ contained more than 120 food items, and each question was divided into three categories: (1) consumption frequency ranging from 1 to 10; (2) the unit of consumption (daily, weekly, monthly, or yearly); and (3) the size of the portion eaten (small, medium, or large) which were represented in grams or milliliters and their equivalents in home measures, for example teacups, cups, tablespoons, slices, among others. The responses were converted to food intake (grams per day or milliliters per day if applicable). The foods were selected and categorized according to Table 1, based on similar characteristics and nutritional content.
Food groups analyzed between 2019 and 2022 in Goiania, Goiás, Brazil.

During the interviews, a questionnaire regarding sociodemographic data and lifestyle habits was administered. In this study, data were collected regarding body mass index (BMI), age, marital status, ethnicity, level of education, and alcohol and tobacco consumption.
BMI was categorized according to the World Health Organization guidelines, which is calculated by dividing the weight (kg) by the square of the height (m). The adult population was categorized into underweight (>18.5 kg/m2), normal weight (18.5–24.9 kg/m2), overweight (25.0–29.9 kg/m2), and obese (⩾30.0 kg/m2); and the elderly population (60 years and older) into underweight (<23 kg/m2), normal weight (23–27.9 kg/m2), overweight (28–29.9 kg/m2), and obese (⩾30 kg/m2).21,22
Marital status was categorized into married and unmarried (single, widowed, divorced/separated). 23 For ethnicity, two categories were created: white and non-white (black, brown). 24 Educational attainment was categorized into <12 years (illiterate, less than 5 years, 6–8 years, and 9–11 years), 12 years (high school), and ⩾13 years (undergraduate and graduate). 23
Diagnosis of H. pylori infection
H. pylori status (positive versus negative) was determined by histopathological examination, which is considered the gold standard, with a sensitivity and specificity of approximately 94%. 25 Reports of the histopathological examinations performed at the Department of Digestive Tract were accessed. The examinations were carried out using biopsies of the gastric body and antrum stained with hematoxylin–eosin and Giemsa staining methods.
Statistical analyses
The variables are described using absolute and relative frequencies, and measures of central tendency and dispersion. After classification in grams per day, foods were stratified into tertiles of consumption (low, medium, and high). The chi-square test or Fisher’s exact test was used for association analysis of categorical variables when appropriate and Student’s t-test for continuous variables.
Simple and multiple binary logistic regression models were used to analyze odds ratios (ORs) and their respective 95% confidence intervals (CI). In the construction of the multiple model, simple regression analysis were conducted employing a p value of ⩽0.20 as an entry criterion in the modelling process. A stepwise forward methodology was used to select the most appropriate model. The Hosmer–Lemeshow test was used to verify the adequacy of the model.
The significance level adopted was 5%. All statistical analysis were performed using IBM Statistical Package for the Social Science (IBM SPSS) version 25.0.
Results
A total of 218 individuals were recruited; however, 62 individuals were excluded because they did not meet the eligibility criteria. After exclusion, 156 participants were eligible (Figure 1).

Flowchart of participant eligibility for the study conducted during the period 2019–2022, in Goiania, Goiás, Brazil.
In this study, the prevalence of H. pylori infection was 44.2% (69/156). Infected individuals had a mean age of 49.6 ± 14.6 years; 40.6% were men, 34.8% were 60 years or older, 42.0% were unmarried, 7.2% had higher education, 72.5% were non-white, and 30.4% were obese (Table 2).
Sociodemographic characteristics and lifestyle habits of the study participants from 2019 to 2022 in Goiania, Goiás, Brazil.

Pearson’s chi-square test.
BMI, body mass index.
Non-infected individuals had a mean age of 48.2 ± 15.7 years; 27.6% were men, 28.7% were 60 years or older, 40.2% were unmarried, 8.0% had higher education, 75.9% were non-white, and 17.2% were obese. There was no significant difference between the positive and negative groups for bacterial infection regarding the sociodemographic variables evaluated (Table 2).
In the H. pylori-positive group, 55.1% were alcohol drinkers and 42.0% were smokers. In the negative group, the frequencies of individuals who consumed alcohol and tobacco were 44.8% and 37.9%, respectively. There was no difference in lifestyle habits between the groups (Table 2).
Regarding food consumption, there was no difference between infected and non-infected individuals for the intake of the food groups refined grains, milk and dairy products, fruits, cereals and legumes, vegetables, sweets, salted and processed meats, red meats and offal, white meats, sugar-sweetened beverages, hot beverages, and alcoholic beverages (Table 3).
Dietary habits of the study participants from 2019 to 2022 in Goiania, Goiás, Brazil.

Pearson’s chi-square test.
Fisher’s exact test.
In the univariate analysis, sociodemographic and lifestyle variables were not associated with the presence of H. pylori infection (Table 4).
Univariate logistic regression analysis of H. pylori infection, sociodemographic characteristics, and lifestyle habits from 2019 to 2022 in Goiania, Goiás, Brazil.

BMI, body mass index; CI, confidence interval; OR, odds ratio.
Regarding eating habits, in the univariate analysis, individuals with a moderate consumption of refined grains had a higher chance of being infected with H. pylori (OR = 2.40; 95% CI = 1.08–5.32). Patients with moderate fruit consumption also had a higher chance of being infected with H. pylori (OR = 2.36; 95% CI = 1.07–5.20). The consumption of milk and dairy products, cereals and legumes, vegetables and legumes, sweets, salted and processed meats, red meats and offal, white meats, sugar-sweetened beverages, hot beverages, and alcoholic beverages was not associated with H. pylori infection (Table 5).
Univariate logistic regression analysis of H. pylori infection and eating habits from 2019 to 2022 in Goiania, Goiás, Brazil.
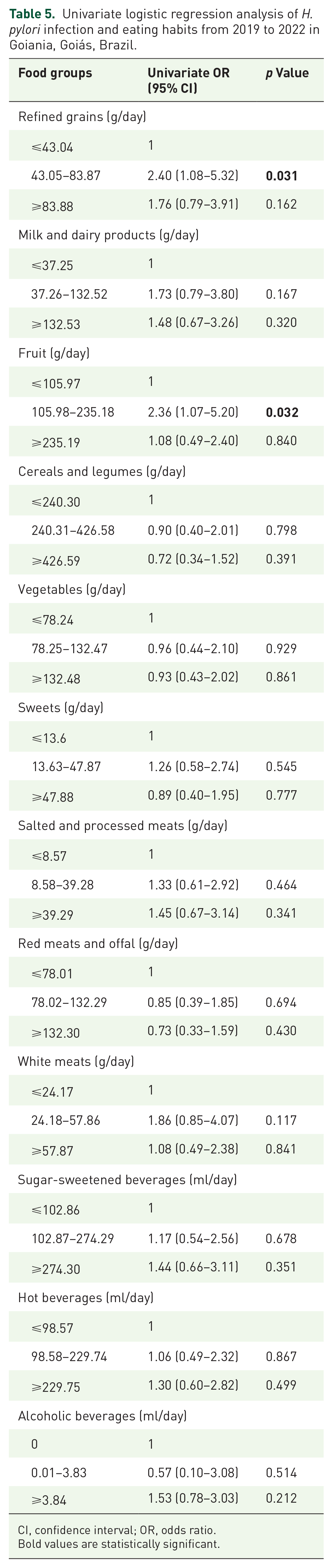
CI, confidence interval; OR, odds ratio.
Bold values are statistically significant.
In the multiple logistic regression analysis, male individuals had a higher chance of being infected with H. pylori (OR = 2.25; 95% CI = 1.08–4.67). Participants with obesity also had a higher chance of being infected (OR = 2.67; 95% CI = 1.10–6.51), compared to underweight and eutrophic individuals. Regarding dietary habits, participants with moderate consumption of refined grains had a higher chance of being infected with H. pylori (OR = 2.41; 95% CI = 1.03–5.617). Individuals with moderate fruit consumption also had a higher chance of being infected with H. pylori (OR = 2.53; 95% CI = 1.08–5.93) (Table 6).
Multiple logistic regression analysis of H. pylori infection, sociodemographic characteristics and eating habits from 2019 to 2022 in Goiania, Goiás, Brazil.

BMI, body mass index; CI, confidence interval; OR, odds ratio.
Bold values are statistically significant.
Discussion
In this study, the prevalence of H. pylori infection was 44.2%. This value is considered high when compared with data from developed countries such as Switzerland and Australia, which have prevalence rates of 18.9% and 24.6%, respectively. 26 A recent meta-analysis reported a prevalence of 69.26% in adults in Latin America and the Caribbean. 2 In Brazil, the prevalence is heterogeneous in different regions, with proportions of 31.7%, 61.1%, and 91% in the Southeast, Midwest, and North regions, respectively.3,4,6 The prevalence of infection depends on different factors, and it is necessary to consider that these values may have been influenced by the living conditions of the population, different diagnostic methods, genetic characteristics of patients and bacteria, and lifestyle habits, among others.
Male individuals were more likely to be infected with H. pylori. Some studies have found no relationship between sex and infection.1,2 However, the results of this study corroborate a robust meta-analysis that showed a male predominance in the prevalence of H. pylori in adult populations from all continents. 27 Differences in sex in the prevalence of H. pylori infection among adults may be explained by distinct exposure to environmental factors such as smoking, which has been associated in the literature with an increased risk of H. pylori infection. 28 It has also been hypothesized that physiological differences, especially sex hormones, may affect immunity and inflammatory responses to H. pylori differently in males and females. These hormones may interfere directly or indirectly with cell receptors, thereby altering the immune response. 29
In this study, obesity was found to increase the risk of H. pylori infection. However, data on the association between this infection and obesity are conflicting. Some studies have suggested an inverse association between H. pylori prevalence and obesity. 30 Consistent with the findings of the present study, meta-analyses have indicated a positive correlation between the risk of H. pylori infection and prevalence of obesity.31,32 Furthermore, a cohort study demonstrated that H. pylori infection was positively associated with increased BMI regardless of socioeconomic status and other confounding factors. 33
The mechanisms involved in the relationship between H. pylori infection and obesity are not well established. However, it has been suggested that regulation of the gastrointestinal hormones ghrelin and leptin may be involved. Individuals positive for H. pylori have lower plasma leptin levels. The reduction in this hormone delays the feeling of satiety, favoring obesity. 34 Low ghrelin levels have also been identified in H. pylori-infected obese patients. The reduced production of this hormone may be the result of atrophic gastritis. 35 Another mechanism that may contribute to the development of obesity in H. pylori-infected individuals is increased insulin resistance identified in these patients. 36 In addition, impaired immune function of the gastrointestinal tract in the obese population may favor H. pylori survival. 37 Few studies have investigated the frequency of H. pylori virulence factors in the obese patients. A recent observational study revealed a high prevalence of vacA and cagE followed by cagA, dupA, iceA1, oipA, and babA2 genotypes in H. pylori strains isolated from obese patients diagnosed with gastric ulcer, duodenal ulcer, and gastric cancer. 38
Moderate consumption of the ‘refined grains’ food group, characterized by breads, cakes, cookies, and breakfast cereal, was positively associated with H. pylori infection. These foods are rich in carbohydrates with a high glycemic index and are present in the diet of Brazilians. 39 Different studies have also shown a positive relationship between the intake of breads, refined grain products, and carbohydrates in the diet and the risk of H. pylori infection.16,17,40 In addition, Sohouli et al. showed that a high glycemic load and a high glycemic index in the diet significantly increased the risk of H. pylori infection. 40
The intake of carbohydrates and acquisition of H. pylori infection may be related to the effect of these compounds on blood glucose levels. High blood glucose levels can lead to the development of enteric neuropathy, increasing the production of pro-inflammatory cytokines, and eventually causing neurodegeneration. Consequently, delayed gastric emptying, decreased acid secretion, and increased bacterial colonization favor H. pylori infection. 41 In addition, several recent studies have shown an association between H. pylori infection and metabolic syndrome. 36 Other studies have reported a higher prevalence of this infection in individuals with diabetes. 42 Considering that carbohydrate intake is associated with metabolic syndrome and diabetes, these findings reinforce a possible link between carbohydrates and H. pylori infection. 43
Moderate fruit consumption was positively associated with H. pylori infection. This result contrasts with studies demonstrating that fruit consumption has a protective effect against this bacterium. 13 However, it is worth considering that the consumption of raw fruits and vegetables, often irrigated by water contaminated by feces, has been associated with H. pylori transmission.44,45 Bacteria can form a biofilm, which favors the persistence of microorganisms in the environment for long periods. Moreover, the cells in biofilms are highly resistant to elimination by sanitizing agents. Thus, raw vegetables can potentially serve as vehicles for the transmission of this pathogen. 46
Food can also be contaminated with H. pylori owing to poor hygiene practices during processing. Food handling can contribute to contamination via hands, nails, and oral and nasal secretions. Previous studies have shown that some types of raw ready-to-eat foods, such as fruit salad, can be sources of resistant and virulent H. pylori strains. 47
Some limitations of this study should be considered when interpreting these results. The sample comprised individuals who sought health care; these patients are probably more likely to have been diagnosed with H. pylori and thus changed their eating habits. Owing to the nature of the self-reported questionnaire, there is information and memory bias, and the amount of food intake may not be accurate. Another limiting factor was the lack of information regarding the previous treatment of the infection. Finally, the cross-sectional design precludes inference of causality. However, this study has several strengths. This is the first study to examine the association between H. pylori infection and dietary habits in this region. A previously validated FFQ (food frequency questionnaire) was used to assess dietary intake.19,20 In addition, the method used to assess the presence of infection is considered the gold standard. 25
Conclusion
The prevalence of H. pylori infections was 44.2%. Males and obese individuals are more likely to be infected with H. pylori. The findings of this study indicated that dietary habits influence the presence of H. pylori infection. Consumption of refined grains increases the chance of infection, which may reinforce the role of H. pylori in metabolic diseases. Interestingly, fruit consumption also had a positive association with the presence of bacteria, probably because of its role as a vehicle for transmission of this pathogen. Further research is required to elucidate the mechanisms underlying the associations identified in this study.
