Abstract
Intense lung inflammation characterizes respiratory failure associated with Pneumocystis pneumonia. Our laboratory has previously demonstrated that alveolar epithelial cells (AECs) elaborate inflammatory cytokines and chemokines in response to the Pneumocystis carinii cell wall constituent β-(1→3)-glucan (PCBG), and that these responses require lactosylceramide, a prominent glycosphingolipid constituent of certain cell membrane microdomains. The relevance of membrane microdomains, also termed plasma membrane lipid rafts, in cell signaling and macromolecule handling has been increasingly recognized in many biologic systems, but their role in P. carinii-induced inflammation is unknown. To investigate the mechanisms of microdomain-dependent P. carinii-induced inflammation, we challenged primary rat AECs with PCBG with or without pre-incubation with inhibitors of microdomain function. Glycosphingolipid and cholesterol rich microdomain inhibition resulted in significant attenuation of P. carinii-induced expression of TNF-α and the rodent C-X-C chemokine MIP-2, as well as their known inflammatory secondary signaling pathways. We have previously shown that protein kinase C (PKC) is activated by PCBG challenge and herein show that PKC localizes to AEC microdomains. We also demonstrate by conventional microscopy, fluorescence microscopy, confocal microscopy and spectrophotofluorimetry that AECs internalize fluorescently-labeled PCBG by microdomain-mediated mechanisms, and that anti-microdomain pretreatments prevent internalization. Taken together, these data suggest an important role for AEC microdomain function in PCBG-induced inflammatory responses. This offers a potential novel target for therapeutics for a condition that continues to exert unacceptable morbidity and mortality among immunocompromised populations.
Introduction
Pneumocystis pneumonia remains an important problem in the management of immunocompromised patients.1–3 Despite medical advances, the case mortality for Pneumocystis pneumonia ranges between 15% and 40%, with significantly worse outcomes among non-AIDS immunocompromised persons.1–3 An intense lung inflammation characterized by excess neutrophils and CD8+ lymphocytes is characteristic of severe Pneumocystis pneumonia and results in diffuse alveolar damage, gas exchange impairment and respiratory failure.1,4,5 Notably, the degree of lung inflammation has been shown to be a stronger predictor of respiratory failure and death rather than the fungal organism burden.2–4,6–9 The mechanism by which Pneumocystis organisms induce lung inflammation remains incompletely elucidated, but recent studies implicate the Pneumocystis cell wall constituent β-(1→3)-
Alveolar epithelial cells (AECs) appear to play an important role in Pneumocystis pneumonia. Ultrastructural studies identify Pneumocystis organisms closely associated with the alveolar epithelium of infected human and animal lungs, supporting the hypothesis that the binding of Pneumocystis to AECs is an integral part of the establishment of infection. 12 Evidence also strongly supports that AECs, once considered simply passive gas exchange barriers, actively participate in host defenses against this organism. Our laboratory has demonstrated that rat AECs produce macrophage inflammatory protein-2 (MIP-2) in response to P. carinii β-glucan challenge.13,14 MIP-2, the rodent ortholog of the human C-X-C chemokine IL-8, is a potent neutrophil chemoattractant. We have also shown that AECs produce TNF-α following PCBG challenge, a cytokine known to have numerous pro-inflammatory effects.13–15 We have further demonstrated that, on a cell-by-cell basis, AECs produce more of these inflammation mediators than do identically challenged alveolar macrophages. 14 Thus, we have postulated that MIP-2 and TNF-α produced by AECs contribute to the lung inflammation observed during severe Pneumocystis pneumonia. 11
The mechanisms by which Pneumocystis β-glucans stimulate inflammatory cytokine and chemokine production remain incompletely elucidated. 16 Previous investigations from our laboratory indicate that lactosylceramide, a prominent cell membrane glycosphingolipid, functions as a major β-glucan receptor on AECs, facilitating the subsequent inflammatory responses. 17 Microdomains (lipid rafts) are known to facilitate cellular internalization and transcytosis of a variety of macromolecules by AECs.18,19 Further, microdomain function is required for the establishment and propagation of several known infectious processes among both respiratory and non-respiratory epithelia.19–23 The current investigations explore the relevance of functional AEC membrane lipid microdomains in Pneumocystis β-glucan-induced inflammatory cytokine expression and AEC handling of PCBG.
Materials and methods
Reagents and organisms
Unless otherwise noted, all general reagents were from Sigma Chemical Co. (St Louis, MO, USA). All animal experiments were reviewed and approved by the Mayo Institutional Animal Care and Usage Committee prior to initiation of these studies. Pneumocystis carinii was originally obtained through the American Type Culture Collection (ATCC, Bethesda, MD, USA) and maintained in our colony of dexamethasone-treated immunosuppressed Long Evans rats (HSD, Inc., Indianapolis, IN, USA), as previously reported. 24
A PCBG isolate was prepared, as previously described. 10 Briefly, P. carinii organisms were isolated from lungs of heavily infected rats, autoclaved and disrupted by ultrasonication. Glucan was isolated by NaOH digestion and lipid extraction, washed first with 0.1% SDS, and then vigorously washed with distilled physiologic saline to remove the detergent. This isolate was confirmed to contain a predominantly glucose-rich complex carbohydrate complex, which was largely degraded by β-(1→3)-glucanases. Only those β-glucan preparations that consistently displayed <0.125 units of endotoxin by the limulus amebocyte lysate method were utilized in these studies.
Alveolar epithelial cell isolation
In our hands, primary alveolar epithelial cells provide the most robust chemokine responses to P. carinii β-glucans, and provide the advantage of studying rat host-specific epithelial cells challenged with rat-derived PCBG. Accordingly, rat AECs were isolated as described by Dobbs and colleagues. 25 In short, pentobarbital-anesthetized rats (∼250 g) were sacrificed by transection of the inferior vena cava. The pulmonary vasculature was perfused with saline. The trachea was isolated and the lungs depleted of alveolar macrophages by multiple lavages. AECs were separated from the basement membrane by incubation with porcine elastase and the lungs were minced, filtered and centrifuged. Recovered cells were suspended in serum-free DMEM and incubated for 1 h in Petri dishes coated with rat IgG to remove residual macrophages. The supernatants ware collected and centrifuged prior to suspension of the epithelial cells in DMEM containing 10% bovine calf serum, penicillin (50,000 units/l) and streptomycin (50 mg/l). AECs were counted using a standard hemocytometer. The AECs were incubated (37°C, 5% CO2) and allowed to adhere to culture plates for at least 48 h. The medium was changed after the initial 24 h. After 48 h, the cells had largely lost lamellar inclusion bodies, and were flattened and well spread, as well as firmly attached—displaying morphology more reminiscent of Type I cells than the Type II cells. Prior studies have demonstrated that Pneumocystis interacts predominantly with Type I cells, but also interacts with Type II cells to a lesser extent. 11
PCBG challenge of AECs and MIP-2 responses
As we previously reported, primary AECs were maintained in monolayer culture for approximately 48 h prior to challenge with PCBG (100 µg/ml, ∼5 × 106 particles/ml) for 6 h. Culture media was then collected and submitted to MIP-2 sandwich ELISA (Biosource, Camarillo, CA, USA) to characterize the inflammatory response. To define the effects of inhibitors of internalization on eventual PCBG-induced MIP-2 expression, we challenged AECs with or without various pretreatments. Endocytotic function was nonspecifically impaired by maintaining the cell culture at 4°C for 30 min prior to challenge and throughout the challenge. Microdomain formation and function was disrupted by 30 min pretreatment with concentrations of agents known to inhibit plasma membrane lipid microdomains, including: genistein 5 µM; methyl-β-cyclodextrin 5 mM; or nystatin 25 µg/ml (Sigma Nystatin N1638) prior to challenge of the AECs with PCBG.26,27 In contrast, clathrin-mediated internalization was impaired by 30 min pretreatment with chlorpromazine 8 µg/ml. 26,27
Microdomain-localized protein kinase C activation
We have previously demonstrated that PCBG challenge induces MIP-2 production by NF-κB and protein kinase C (PKC)-dependent mechanisms. 13 As PKC has been reported to be associated with certain membrane microdomains, we isolated microdomains from both PCBG challenged and PCBG naïve AECs by Triton X-100 fractionation. 28 After homogenization of the samples, the microdomains were separated by SDS-PAGE and then submitted to immunoblotting using a rabbit monoclonal phospho-PKC (pan) Ab (Antibody 9371, Cell Signaling, Danvers, MA, USA). The samples were next exposed to HRP-conjugated anti-rabbit secondary Ab and enhanced chemiluminescent detection (ECL) (Amersham, Piscataway, NJ, USA).
Conventional, fluorescence and confocal microscopy detection of PCBG internalization
Dichlorotriazinylaminofluorescein (DTAF, 10 mg in 0.1 M Borax solution) was incubated overnight with 30 mg PCBG then repeatedly centrifuged and rinsed with sterile 0.9% normal saline until all unbound DTAF was removed. AECs grown in monolayers on LabTek II slides were exposed to DTAF-labeled PCBG for 1 h, with or without pretreatment to impede internalization. Cultures were maintained at 4°C for 30 min prior to challenge and throughout the subsequent challenge to nonspecifically impair internalization. Glycosphingolipid-cholesterol rich microdomain internalization was impaired using nystatin (25 µg/ml) applied 30 min prior to challenge. 29 In addition, we also pretreated the cells with anti-lactosylceramide Ab (anti-CDw17, 200 µg/ml) or anti-lactosylceramide Ab in the presence of added exogenous lactosylceramide (1 mg/ml). 13
Samples were then challenged for 2 h with DTAF-labeled PCBG. The media were removed and the cells submitted to two rapid washes with PBS before repeated acid stripping with DMEM at pH 2.2 to remove all non-internalized PCBG. Next, the cells were aggressively washed with cold PBS, fixed with 4% paraformaldehyde and quenched with glycine. The media chambers were removed from the slides and coverslips applied with Slow Fade (Molecular Probes, Carlsbad, CA, USA). The cells were examined by fluorescence (excitation 490 nm, emission 520 nm) and phase contrast microscopy using an Olympus IX70 microscope (Melville, NY, USA).
To confirm the internalization of the DTAF-labeled PCBG, AECs were grown and challenged as described above (no pretreatments were performed). The cells were acid-stripped and fixed as described above. To define the plasma membrane borders, the challenged cells were incubated with Vybrant DiI cell labeling solution (Molecular Probes, Eugene, OR, USA; 1:200 dilution; absorption 549 nm, emission 565 nm) for approximately 8 min. The fixed, labeled cells were then submitted to confocal microscopy using a Zeiss model 510 microscope equipped with a 100 × (1.4 numerical aperture) objective. Sequential laser acquisition was performed for the two dyes and all images were examined in multiple z-planes to confirm cellular location of the DTAF-labeled PCBG particles.
Spectophotofluorimetric assessment of PCBG internalization
To quantify the effects on AEC internalization of PCBG, we pretreated cells with several different inhibitors of internalization for 30 min prior to challenge. We utilized pretreatment with anti-CDw17 and nystatin to inhibit lactosylceramide rich microdomains. We also pretreated with Abs against an arbitrary membrane glycosphingolipid, anti-GM1 (200 µg/ml), as well as cytochalasin D (5 µg/ml) to generally inhibit phagocytic function. Four hours after PCBG challenge, the cells were acid-stripped, then lysed with 2 N NaOH. The lysates were submitted to conventional spectrophotofluorimetry using an Aminco SLM 8000C spectrophotofluorimeter (SLM Instruments, Inc., Urbana, IL, USA), optimized for DTAF as noted above. Samples were maximally shielded from light prior to analysis and agitated to ensure even distribution of particles immediately before analysis. At least three trials for each condition and at least four aliquots from each sample were analyzed.
Data analysis
All data analysis was preformed using JMP 5 software (SAS Institute, Cary, NC, USA). The data are expressed as mean ± standard error of the mean. Differences between groups were defined using a two-tailed Student's t-test, with P <0.05 being considered a significant difference.
Results
MIP-2 production following PBCG challenge is inhibited by low temperature and by inhibitors of plasma membrane microdomains
We have previously demonstrated that challenge AEC with PCBG induced robust chemokine production.
13
Consistent with our previous reports, by 6 h after PCBG challenge, the AECs had generated significant concentrations of MIP-2 in the culture media (Figure 1). Furthermore, production of MIP-2 was significantly inhibited by culturing the cells at 4°C or by treating the cells with all three tested inhibitors of membrane microdomain function: genistein, methyl-β-cyclodextrin or nystatin.
30
In contrast, treatment of AECs with chlorpromazine at concentrations known to inhibit clathrin-coated pit-mediated internalization had no effect on MIP-2 production. These results suggest that AEC stimulation to release chemokines following PCBG stimulation required intact cell membrane microdomain function, but not clathrin mediated function.
Disruption of microdomain function impairs P. carinii β-glucan-induced inflammatory cytokine expression. In order to determine the effect of various internalization mechanisms, primary AECs were challenged with PCBG with or without inhibitory pretreatment. To impair general internalization, cells were maintained at 4°C for 30 min prior to challenge. Microdomain function was disrupted by several mechanisms, including 30 min pretreatment with genistein, methyl-β-cyclodextran or nystatin. In contrast, internalization via clathrin-mediated mechanisms was inhibited by 30 min pretreatment with chlorpromazine. ELISA detection of MIP-2 was performed on the supernatant after 4 h of challenge. These experiments showed significant suppression of PCBG-induced MIP-2 expression following both cold and anti-microdomain pretreatments, while anti-clathrin pretreatment had little effect. (*P <0.05).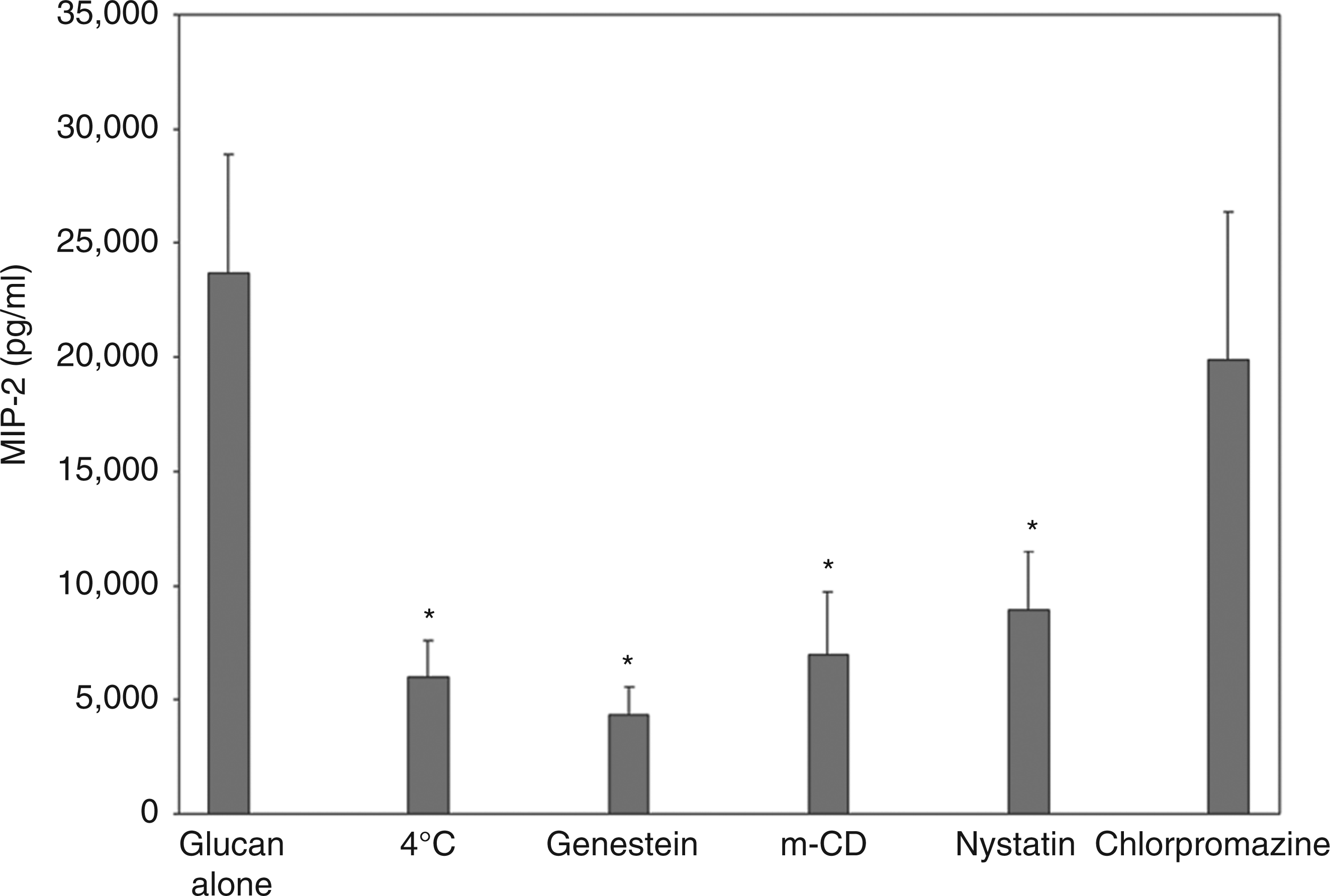
PKC activation by PCBG is localized to membrane microdomains
We have also previously demonstrated that PCBG-induced cytokine and chemokine production by AECs is PKC-dependent.
13
We next sought to determine whether active phospho-PKC was localized to the microdomains of AECs following PCBG stimulation (Figure 2). Indeed, PKC was found to localize to isolated microdomains as early as 15 min following PCBG stimulation. By 30 min the PKC signal was decreased. Our studies further revealed that this PKC effect was best appreciated when using Abs against pan-phospho-PKC (shown), suggesting that non-α/non-β PKC isoforms may play a prominent role in this function.
P. carinii β-glucan induces microdomain-localized protein kinase C activation. Primary AECs were harvested from a monolayer with or without PCBG challenge. Lipid microdomains (rafts) were then isolated from the samples by Triton X-100 fractionation.
28
Following homogenization, the samples were separated by SDS-PAGE then submitted to Western blotting using a pan-phospho-PKC Ab. Samples were exposed to HPR-conjugated secondary Ab and ECL chemiluminescent detection system prior to autoradiography. While the unchallenged cell samples showed little activated (phosporylated) PKC, the PCBG-challenged cells demonstrated a significant increase in the autoradiographic signal. Double bands are noted caused by multiple PKC isoforms. This effect appeared maximal at 15 min and began to decline at around 30 min.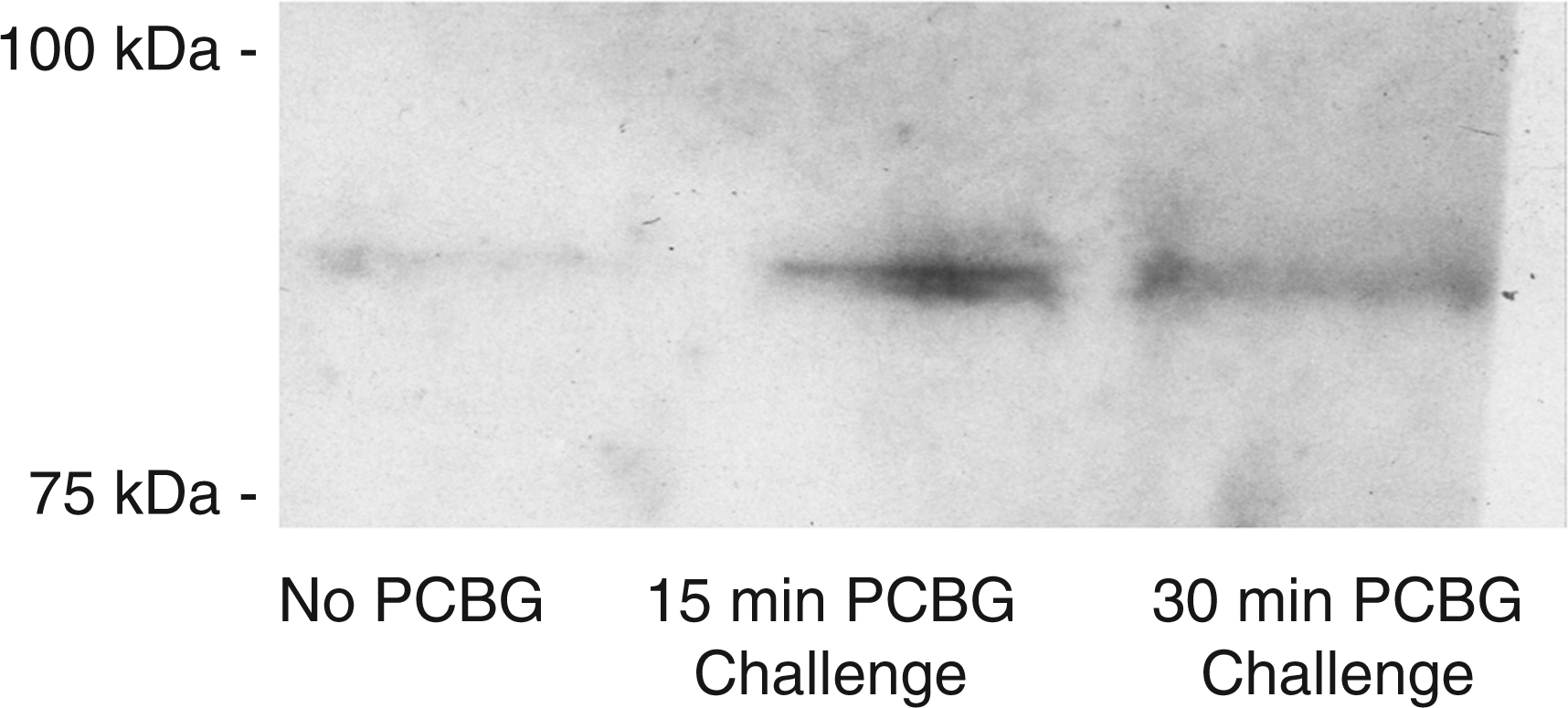
PCBG is internalized by AECs, which can be suppressed by inhibitors of membrane microdomain function
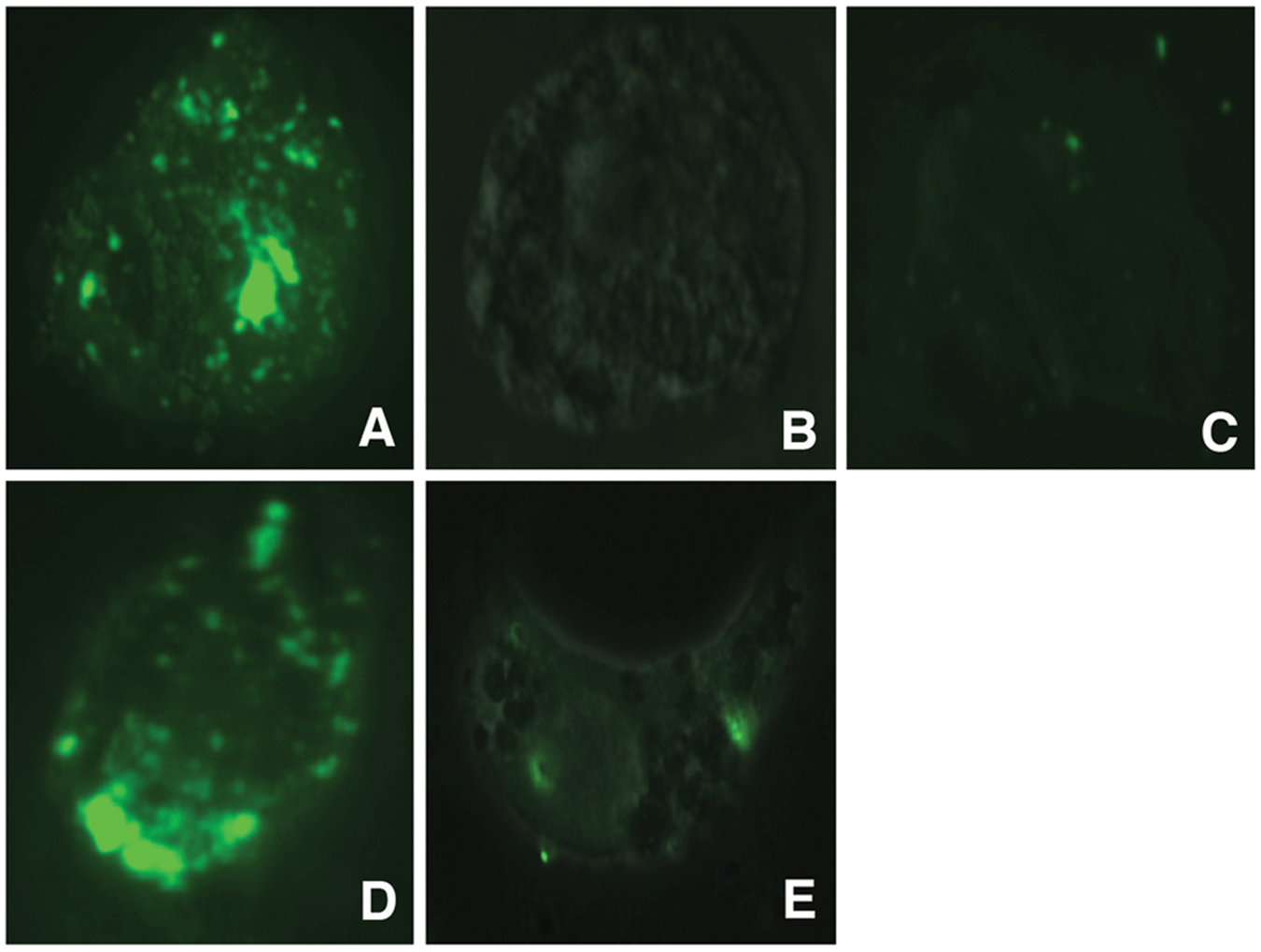
Confocal microscopy was further utilized to determine whether PCBG is internalized by AECs (Figure 3). Fluorescent DTAF-labeled PCBG was fully internalized by AECs within 1 h of challenge. The internalized location was confirmed by analysis in multiple z-planes, using lipophilic labeling to delineate the cell extent. We then demonstrated that PCBG internalization was interrupted by disrupting microdomain function, either by directing Abs against lactosylceramide, culturing the cells at 4°C at the time of challenge or pretreatment with nystatin—an agent that inhibits glycosphingolipid-cholesterol rich microdomains, including caveoli (Figure 4).
Alveolar epithelial cells internalize fluorescently labeled P. carinii β-glucan. After approximately 48 h culture, primary AECs were exposed to DTAF-labeled PCBG for 1 h. The samples were then acid-stripped, formalin-fixed and treated with a lipophilic counterstain prior to being submitted to confocal fluorescent microscopy. Multiple images in the z-plane were obtained to confirm complete internalization of PCBG particle. This photomicrograph demonstrates DTAF-labeled PCBG (green) in various stages of internalization. The internalized PCBG displayed yellow coloration when imaged in this manner. Microdomain disruption impairs internalization of DTAF-labeled P. carinii β-glucan by AECs. Primary AECs were challenged with DTAF-labeled PCBG with or without pretreatment, and then submitted to conventional fluorescence microscopy. (A) DTAF-labeled PCBG was internalized by alveolar epithelial cells 2 h after challenge at 37°C. (B) In contrast, culture of the AECs at 4°C prevented PCBG uptake. (C) Monoclonal Abs targeting the microdomain glycosphingolipid constituent lactosylceramide also prevented PCBG uptake. (D) However, pre-incubation of the anti-lactosylceramide Ab with free lactosylceramide abrogated this effect. (E) Finally, disruption of lipid microdomains with nystatin also inhibited PCBG uptake.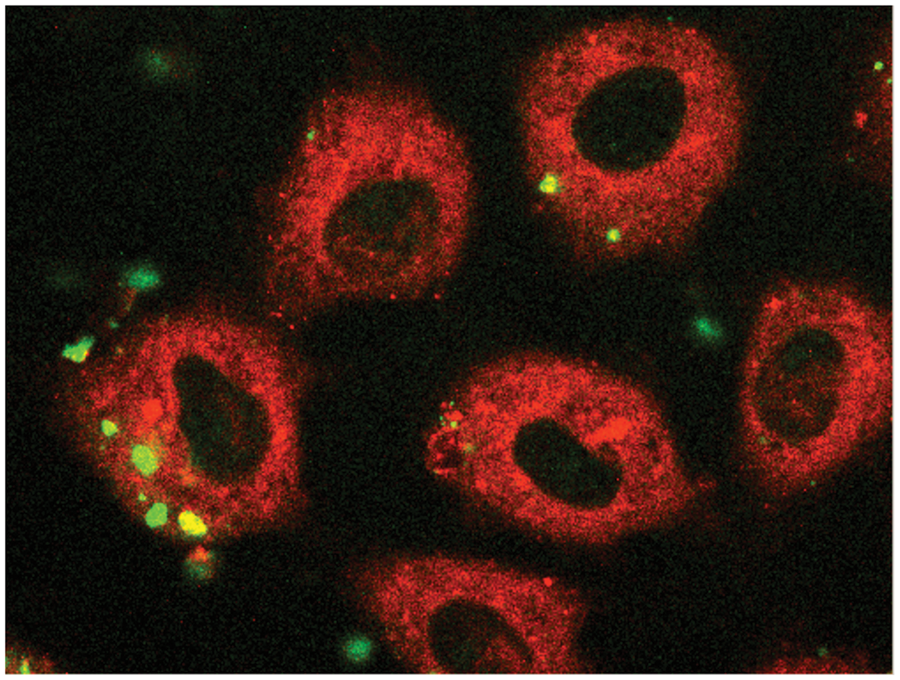
To further quantify the amount of labeled PCBG internalized under various conditions, spectophotofluorimetry of the cultured AEC lysates was performed following various AEC membrane treatments and PCBG challenge (Figure 5). Once again, treatment with either nystatin or anti-lactosylceramide Abs that impaired microdomain function each significantly suppressed PCBG internalization. In contrast, Abs against an arbitrary glycosphingolipid (GM1) had no such effect. As anticipated, generalized impairment of actin function with cytochalasin D impaired internalization approximately as much as anti-lactosylceramide antibody pretreatment, but less than nystatin inhibition of caveolae. Overall, these data support that membrane microdomains rich in glycosphingolipids and cholesterol, particularly lactosylceramide, participate in epithelial cell activation to release cytokines in response to the pro-inflammatory Pneumocystis β-glucan cell wall components.
Impaired microdomain function decreases internalized DTAF-labeled P. carinii β-glucan signal. Primary rat AECs were challenged with DTAF-labeled PCBG with or without pretreatment by a variety of inhibitors of internalization. After 4 h of challenge, the samples were acid-stripped, then lysed with sodium hydroxide. Homogenized equal volumes from each sample were then assayed by conventional photospectrofluorimetry. Anti-lactosylceramide Abs and nystatin both significantly impaired the internalization of DTAF-labeled PCBG, as measured by this method. Cytochalasin D had a lesser, but still significant, effect. Abs against an arbitrary glycosphingolipid (GM-1) had no effect on PCBG uptake (*P <0.01).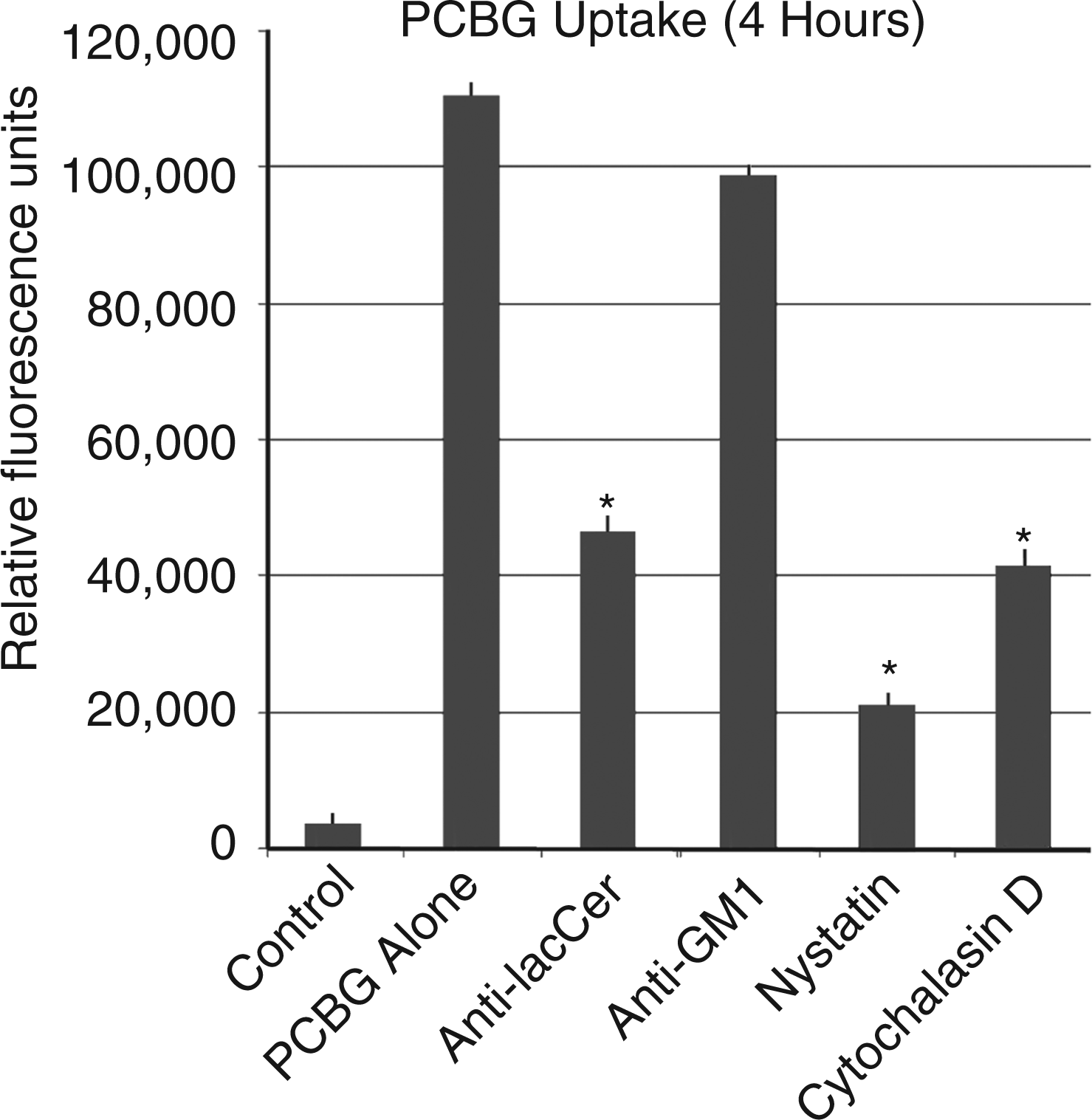
Discussion
Our prior investigations have convincingly demonstrated that PCBG induces inflammatory responses from AECs.13,14 Further, we have shown that these responses are dependent upon PCBG interaction with lactosylceramide at the cell surface and that secondary signaling by NF-κB and PKC occur following challenge.13,14 The current investigations further emphasize the importance of plasma membrane microdomain function in PCBG-induced inflammation.
Handling of macromolecules in the airspaces is highly dependent upon the AECs and alveolar macrophages that internalize the particles that deposit peripherally. AECs are essential for the recycling of surfactant proteins and are adept at bidirectional transcytosis of proteins and carbohydrates.18,31 –36 Given the mass of particles inhaled as humans ventilate around 10 l ambient air per min, this macromolecule processing function of epithelial cells is critical as it would overwhelm the capacity of professional phagocytes, such as the infrequently encountered alveolar macrophage. AECs are also known to internalize cellular elements and toxins from respiratory pathogens, 23 as well as whole organisms, including Aspergillus fumigatus, 21 Streptococcus pneumoniae, 22 and Pseudomonas aeruginosa. 20 Membrane microdomains appear necessary for internalization of several pathogens, including atypical caveolar endocytosis of SV-40 virus and FimH-associated endocytosis of Escherichia coli. 19 Pathogen internalization functions of microdomains have been demonstrated in several organs and cell types, but we are unaware of any data regarding microdomain-mediated internalization of Pneumocystis or any of its components.
Microdomains are localized regions of the plasma membrane enriched in glycosphingolipids and cholesterol measuring 10–200 nm in size.19,31,37 Microdomains have been implicated in cell signaling and uptake of particulate material. 29 Thus, it is intriguing that 1–2 µm PCBG particles require microdomain function for internalization. This may be possibly explained by the notion that internalization is initiated by microdomain-localized cell signaling events (perhaps PKC activation), while the process of mechanical internalization occurs by otherwise microdomain-independent phagocytosis. This would be consistent with our observation that both microdomain disruption and cytochalasin D pretreatment inhibit internalization. It is also notable that Pneumocystis interaction with AECs during lung infection induces plasmalemmal activation, resulting in dramatic alterations of the surface membrane structure of the type 1 and type 2 pneumocytes observed by electron microscopy. 38 It has been speculated that this allows the pathogen to more efficiently extract nutrients from the host.
The relevance of the current observation lies primarily in the potential therapeutic implications. Pneumocystis pneumonia continues to exert an unacceptably high case-mortality rate among immunocompromised patients, particularly those who are immunosuppressed for reasons other than HIV disease.1–3 The improved mortality observed following the introduction of systemic corticosteroids to the typical antimicrobial regimens for P. carinii pneumonia in the 1980s first indicated the importance of host inflammation in the morbidity associated with the disease. 39 Additional studies revealed that, in fact, markers of exaggerated host inflammation were stronger predictors of mortality than were pathogen factors, such as organism burden.6–8
Previous data from our laboratory have suggested that inhibition of NF-κB signaling can reduce the AEC-generated PCBG-induced inflammatory response.13,14 In addition, inflammatory mediator release is also significantly reduced with PKC inhibition. Both of these interventions provide potential therapeutic targets to improve human outcomes. The observation that membrane disruption with nystatin inhibits both internalization of PCBG and dramatically attenuates PCBG-induced chemokine production may offer an additional appealing target to modulate Pneumocystis-induced inflammation. Nystatin is a polyene antibiotic with fungistatic and fungicidal properties. The in vitro antifungal activity probably arises because of sterol binding resulting in excessive cell membrane permeability. 40 Binding to mammalian cholesterol appears to also underlie its anti-microdomain effects, as well.
It is further important to note that we observed nystatin to inhibit internalization, cell signaling and mediator release in response to PCBG. In addition, as Pneumocystis organisms appear to establish infections at the level of type 1 pneumocytes and that such associations may alter activation of microdomains in AECs, we further speculate that treatment with nystatin (or a similar agent) may also impede the establishment or propagation of infection with this pathogen, though that hypothesis remains to be tested. The therapeutic potential for reducing Pneumocystis-induced inflammation by nystatin is particularly attractive. At the present time, clinical data does not exist to support its use and the current study was not designed to address the anti-Pneumocystis activity of any of the inhibitors in the overall progression of infection and lung injury. Nonetheless, these investigations do suggest novel therapeutic targets that may eventually benefit patients facing this severe infection.
Footnotes
Acknowledgements
These studies are dedicated to the memory of our departed collaborator, Richard E. Pagano, PhD, who provided key insights and assistance during our studies of the roles of glycosphingolipids in initiating inflammation. We also thank Zvezdana Vuk-Pavlovic and David Marks for many helpful discussions during these studies.
Funding
These investigations were funded by the Mayo Foundation and NIH grant R01-HL62150 to AHL.
