Abstract
Background:
Postpartum depression is a significant public health challenge. Understanding the predictors of postpartum depression can inform targeted interventions and support systems for new mothers.
Objectives:
To identify and quantify sociodemographic and obstetric predictors of postpartum depression among mothers in Kumasi, Ghana.
Design:
A cross-sectional multicenter prospective study.
Methods:
A total of 502 postpartum mothers from five hospitals were included. Bayesian logistic regression analysis was used to assess model uncertainty and complex interactions between sociodemographic, economic, and obstetric factors on postpartum depression.
Results:
The pooled prevalence of postpartum depression was 25% (range 13% to 31%). Education attainment [coefficient = −0.43, 95% credible interval: −0.57 to −0.29, (adjusted odds ratio (aOR) = 0.65] and economic support from multiple earning members (coefficient = −0.28, 95% credible interval: −0.33 to −0.22, aOR = 0.75) substantially reduced the likelihood of postpartum depression. Being a single mother (coefficient = 0.34, 95% credible interval: 0.24 to 0.44, aOR = 1.40) increased the risk of postpartum depression. Planned pregnancies (coefficient = −0.25, 95% credible interval: −0.28 to −0.21, aOR = 0.78), doing physical exercise (coefficient = −0.26, 95% credible interval: −0.30 to −0.23, aOR = 0.77), and exclusive breastfeeding (coefficient = −0.23, 95% credible interval: −0.28 to −0.19, aOR = 0.79) were protective factors for postpartum depression. On the other hand, cesarean sections (coefficient = 0.34, 95% credible interval: 0.24 to 0.43, aOR = 1.40) and spontaneous vaginal deliveries (coefficient = 0.56, 95% credible interval: 0.47 to 0.65, aOR = 1.75) increased the risk of postpartum depression.
Conclusion:
Our findings emphasize the importance of identifying modifiable predictors of postpartum depression, including sociodemographic, economic, and obstetrical factors, in Kumasi, Ghana. Interventions addressing these factors, such as financial support programs, maternal education, and physician training, may significantly reduce the regional burden. Policies tailored to low-resource contexts and exhibiting local cultural sensitivity are needed for enhancing maternal–child health outcomes in Ghana and comparable regions.
Introduction
Maternal health – defined as the physical, mental, and social well-being of women during the period of pregnancy and the postpartum period – represents a fundamental aspect of public health and has been identified as a priority by the World Health Organization.1,2 It is a critical factor in determining favorable outcomes not only for the mothers themselves but also for their offspring, thereby influencing the health of future generations. Postpartum depression (PPD) is a prevalent form of depression that can have a detrimental impact on maternal health. The symptoms associated with PPD include, but are not limited to, severe mood swings, intense irritability, feelings of hopelessness, and difficulty bonding with the infant.3,4
These symptoms may appear within the first few weeks postpartum and, if left untreated, may persist for several months or longer,5,6 severely affecting a mother’s ability to care for herself and her child. The consequences of PPD extend beyond the affected mothers, impacting the cognitive and emotional development of their children and the overall family dynamics. 7 It has been demonstrated that children of mothers with untreated PPD are more likely to experience developmental delays, behavioral problems, and mental health issues later in life.7 –9 These adverse consequences can exert a deleterious effect on familial relationships, resulting in long-term social and economic ramifications.
Globally, the prevalence of PPD exhibits significant variability; however, it is particularly pronounced in low- and middle-income countries, including those in Africa, where prevalence rates range from 17% to 22%.10 –12 The reported high rate of PPD can be attributed to several factors, including limited healthcare resources, socioeconomic challenges, and cultural attitudes toward mental health. These factors often result in insufficient support and delayed diagnosis and treatment for affected mothers. In Ghana, PPD represents a substantial public health issue, yet the existing body of research is constrained by limitations such as small sample sizes and regional biases. A recent systematic review by Keku et al. 13 highlighted that most studies were conducted in urban areas like Greater Accra, potentially overlooking the unique challenges faced by mothers in other regions of the country.
Furthermore, studies to date have focused narrowly on certain predictors, often neglecting the broader spectrum of socioeconomic, medical, and cultural factors that could influence the onset and severity of PPD. This is further compounded by the research landscape in Greater Kumasi region, which remains sparse with only a few studies conducted to date.14,15 This lack of comprehensive data emphasizes the need for broader large-scale studies that consider diverse predictors including sociodemographic characteristics, obstetric history, economic conditions, and social support systems. Addressing PPD in these regions is crucial for enhancing maternal and child health outcomes, along with fostering sustainable community development.
Hence, we conducted a multicenter cross-sectional study in Kumasi to identify and understand the various interactions between sociodemographic and obstetric predictors of PPD. Given the complexity and uncertainty inherent in real-world data, we relied on the Bayesian logistic regression framework for this study. This approach is superior to the frequentist approach as it facilitates the updating of beliefs regarding the validity of obstetric and socioeconomic predictors from prior research based on the data we collected. The Bayesian framework offers a coherent and interpretable framework for quantifying uncertainty, which is crucial for informing both policy and clinical practice. The posterior distributions for these predictors enable direct probability statements concerning the likelihood of PPD, thereby supporting more informed decision-making.
Our approach is particularly well-suited for modeling complex interactions and hierarchical structures, which are often observed in multifactorial conditions like PPD. We believe our findings within Ghana, and specifically in Kumasi, will inform healthcare providers, the Ghana Health Service, and policymakers, enabling the development of effective mental health services and support systems tailored to the needs of new mothers in this region. Furthermore, our findings promise to inform the development of more effective, culturally sensitive policies and interventions suited to the unique challenges faced by African mothers in other regions with similar socioeconomic, cultural, and societal landscape.
Methods
The present cross-sectional, multicenter study was conducted at five public hospitals in the city of Kumasi, Ghana. The study was approved by the Committee on Human Research, Publications, and Ethics (CHRPE) of the School of Medical Sciences at Kwame Nkrumah University of Science and Technology, Ghana (approval no. CHRPE/AP/148/23 dated February 27, 2023). The study protocol was supported by individual approvals from the five hospitals. The Helsinki Declaration, 2013 guidelines were followed, and the participants were asked to provide signed informed consent before enrolment in the study.
Study setting
We collected data from the maternal units of five public hospitals in Kumasi, Ghana – Suntreso Government Hospital, Tafo Government Hospital, Manhyia District Hospital, Ashanti Regional Hospital, and the Maternal and Child Hospital. The five public hospitals selected represented a mix of secondary and tertiary healthcare facilities. All facilities provide comprehensive services, including obstetrics and gynecology, apart from the Maternal and Child Hospital, which specializes in maternal and child health services only. Together, these hospitals serve the region’s diverse population and treat thousands of patients annually.
Study design
Given the chronic and persistent nature of PPD, a cross-sectional study design was chosen for its ability to measure point prevalence rather than incidence rates. The collection of data at a single point in time enabled the assessment of relationships between PPD and demographic, obstetric, and socioeconomic factors. We anticipate that the adopted methodological approach will facilitate the formulation of hypotheses for subsequent research in our region. Moreover, it offers a cost-effective and efficient overview of the current state of PPD and its associated factors, which is crucial for effective public health planning.
Estimated sample size
The theoretical minimum sample size required was calculated using the Cochran formula 16 :
where, n represents the estimated total sample size required for the study, Z is the Z-score corresponding to a 95% confidence level (1.96), p is the estimated prevalence of PPD in the local population (31.39% or 0.3139), 14 and d is the level of precision or margin of error acceptable in our results (5% or 0.05). Based on this calculation, the minimum sample size required for the study was determined to be 331. However, during patient screening, according to the study design, it was planned a-priori to exceed this minimum. This was done to buffer for anticipated attrition and ensure sufficient power even if some data were excluded during quality checks (such as incomplete answers or withdrawal of consent). Given the diversity of the study population, a larger sample also ensured adequate representation across various societal strata, reducing the risk of skewed estimates and improving generalizability for the entire study area.
Inclusion and exclusion criteria
The inclusion criteria for the study were as follows: (i) all mothers who were within 6 weeks postpartum at the time of enrolment; (ii) who had been registered at any of the five study facilities for the administration of mandatory immunizations for their infants; and (iii) those who provided consent to participate in the study. Exclusion criteria included mothers beyond the 6-week postpartum period, those experiencing severe health complications, those with underlying chronic conditions, and those who refused consent. These criteria were adopted to ensure the homogeneity of the study population.
Data collection
We collected demographic characteristics, obstetric factors, and socioeconomic status using structured questionnaires and review of patient medical records. Face-to-face interviews were conducted to address any missing data. The likelihood of PPD was assessed using the Edinburgh Postnatal Depression Scale (EPDS)17,18 a widely validated 10-item self-reporting scale with a 1-week recall period. To assess the social support needs of postpartum women, we employed a modified version of the ENRICHD Social Support Inventory (ESSI). 19 The ESSI was adapted to include six items rated on a Likert scale ranging from 1 (never) to 5 (all the time), addressing both practical and emotional aspects of social support. Previous studies have demonstrated the effectiveness of both EPDS and ESSI in screening for PPD and assessing social support, respectively.19 –22 Both scales are presented in Supplementary File 1 for reference.
The administration of the questionnaires, scales, and interviews was conducted by a team of eight master’s students who were employed as teaching assistants at the university. The consulting physicians, nurses, and other hospital staff were not involved in data collection. To mitigate social desirability bias, interviews were conducted privately in a comfortable environment by trained teaching assistants who emphasized confidentiality and used culturally adapted and acceptable decent phrasing. Participants were assured that their responses would not affect their medical care and were anonymized prior to analysis.
Patients were randomly assigned to a team member who was responsible for collecting the data. The team spent 2 weeks at each facility, after which they moved on to the next facility. The administration of the questionnaires and scales was conducted in Twi, the predominant local language in the region. The questionnaire, initially developed in English, was verbally translated into Twi by the teaching assistants, who are proficient in both languages. Given the potential for variations in individual comprehension and the informal nature of spoken language, the teaching assistants were trained to deliver consistent and accurate translations. This verbal approach enabled on-the-spot clarifications and ensured that participants comprehended each question.
Pilot and instrument validation
A preliminary trial of the study, simulating the real data collection phase, was conceptualized and implemented in early March 2023 at Suntreso Government Hospital, one of the five designated study centers. The objective was to assess the feasibility, consistency, applicability, and effectiveness of the questionnaire, measurements, interview, and recruitment process. The pilot phase was conducted with 20 patients, ensuring that each research assistant interviewed at least two participants independently. The feedback gathered from these participants was used to make refinements to the questionnaires, with the objective of enhancing their clarity and relevance within the context of the local societal and cultural norms. The adapted ESSI demonstrated strong internal consistency (Cronbach’s α = 0.84) indicating good reliability measuring the same construct of social support within the local context. The EPDS, on the other hand, has previously been used by other studies in Ghana validating its application in the local context.23 –25 We also undertook expert reviews to ensure accuracy in the instrument construct. Noticeably, the data collected from the pilot phase was not included in the final analysis to mitigate the potential for any undue biases.
Patient recruitment
A total of 502 postpartum mothers attending immunization appointments between mid-March 2023 and June 2023 were recruited using convenience sampling. This nonprobability sampling method was selected due to its practicality and efficiency in settings with limited access to a representative sample. None of the participating mothers were awarded any financial or material provisions in exchange for their consent to participate in the study. No amendments were made to the routine obstetric and gynecological checkups, the infant’s immunization schedules, or their medication protocols. At the end of the interview, participants reporting high EPDS scores were provided voluntary referral to appropriate psychological services. The referrals were provided by the medical physician in our study team.
Inter-assessor reliability
To ensure the consistency of data collection by different members of the team, inter-assessor reliability checks were performed. Two members independently and blindly collected data from the same participants’ medical records, and their results were compared to assess reliability. Coherency in extracted data was observed in 95% of the records, resulting in a kappa statistic of 0.9, indicating strong agreement. Further crosschecks and referencing with the consulting physician were undertaken to ensure accuracy. Corrections and updates were made as necessary.
Operational definitions
The likelihood of a participant experiencing PPD was determined using the EPDS which ranges from 0 to 30 points, with higher scores indicating a heightened likelihood of PPD. A cut-off value of 11 points was employed, with participants who scored 11 points or higher being categorized as likely to be experiencing PPD. Conversely, participants who scored below 11 points were categorized as likely to be experiencing normal postpartum, indicative of the potential absence of depressive symptomatology. This cutoff was selected based on the principle of maximizing sensitivity (81%) and specificity (88%) in the classification of PPD. 26 Of note, in the present article we used “likely depressed” and “not likely depressed” as EPDS is a screening tool and cannot replace a clinical evaluation and diagnosis by a psychiatrist.27,28 Since our study did not include psychiatric evaluations, we describe our results as “likely.”
Social support was assessed using the ESSI. To categorize the levels of social support in our study, we employed an equal interval method. This approach involved dividing the social support scale, which ranges from 6 to 30 points, into three equal intervals. Scores from 6 to 13 points were categorized as low social support, scores from 14 to 21 points as medium social support, and scores from 22 to 30 points as high social support. The equal interval method was chosen for its simplicity and clarity, providing a clear and intuitive framework. By ensuring that the data is evenly distributed across the low, medium, and high categories, this method facilitates meaningful comparisons between groups and minimizes the risk of skewed data.
Statistical analysis
Data normality were assessed using quantile–quantile (Q–Q) plots. Descriptive statistics were used to summarize the data, and comparisons of numerical and categorical variables were conducted using t-tests and χ² tests, respectively. A Bayesian model was developed using the <rstanarm> package in R, with 10,000 posterior sampling iterations to ensure model convergence and reliability. The model incorporated a prior distribution of ∼N (−0.641 to 0.072), informed by the meta-analyzed prevalence of PPD in sub-Saharan Africa. 10
To evaluate the Bayesian model, the probability of direction (PD) and region of practical equivalence (ROPE) were calculated. The PD quantifies the likelihood that a parameter’s effect is positive or negative (e.g. a PD of 95% indicates a 95% probability that the effect is in a specific direction). The ROPE defines a range of values around a null effect that is considered practically equivalent to no effect. A 95% credible interval (95% CrI) falling entirely outside the ROPE suggests a meaningful effect, while an interval entirely within the ROPE suggests no practical effect. When the 95% CrI partially overlaps the ROPE, the result is considered inconclusive, indicating uncertainty about the practical significance of the effect.
Additionally, Bayesian equivalence testing was performed to complement the ROPE using a combination of the highest density interval (HDI) and ROPE decision rule.29,30 This test evaluates whether a parameter’s effect is significant in the sense of being important enough to be practically relevant. The test checks the percentage of the HDI of the posterior distribution that lies within the ROPE. If this percentage is sufficiently low, the null hypothesis is rejected, indicating that the effect is meaningful. If the percentage is sufficiently high, the null hypothesis is accepted, indicating that the effect is practically equivalent to the null. Intermediate percentages suggest uncertainty about the practical significance of the effect. These metrics were computed and visualized using the <easystats> package. All analyses were performed using R version 4.4.2 (R Foundation for Statistical Computing). The Strengthening the Reporting of Observational Studies in Epidemiology Statement guidelines were used for reporting in our present study (Supplementary File 2). 31
Results
We recruited 502 participants from five regional hospitals – Suntreso Government Hospital (105 participants), Tafo Government Hospital (99 participants), Manhyia District Hospital (106 participants), Ashanti Regional Hospital (92 participants), and the Maternal and Child Hospital (99 participants). Hospital-stratified data is presented in Supplementary File 3.
Sociodemographic and economic characteristics
Among the 502 study participants, significant sociodemographic predictors of PPD included the level of education (p < 0.001) and the number of family contributors to household income (p = 0.007). Higher educational attainment was associated with a lower prevalence of PPD, with the lowest prevalence observed among women with university education (9%) and the highest among those with no formal education (38%). Households with fewer family contributors to income exhibited higher rates of PPD (Table 1). Social support was significantly associated with depression status (p < 0.001). Participants with low social support had the highest percentage of depression (57%), followed by those with medium support (36%) and high support (14%).
Sociodemographic and economic characteristics of study participants (n = 502).

EPDS: Edinburgh Postnatal Depression Scale; ESSI: ENRICHD Social Support Inventory.
Data for continuous variables is presented as mean (standard deviation), rounded off to the nearest tens. p value derived from t-test.
The Bayesian logistic regression analysis hinted at several significant socioeconomic predictors for PPD. Apart from the age, weight, marital status of the mother, working status of partner, and number of people in the household, all socioeconomic predictors had a negative direction of effect, that is, reduced the likelihood of PPD (Figure 1). The marital status of the mother emerged as a significant factor with being single (coefficient = 0.34, 95% CrI: 0.24–0.44, aOR = 1.40) markedly increasing the likelihood of PPD compared to being married. Similarly, a working partner (coefficient = 1.20, 95% CrI: 0.96–1.44, aOR = 3.32) significantly increased the odds of PPD, compared to partners who were not working.

PD and the ROPE for various socioeconomic characteristics. The light blue region indicates the ROPE range within which the effect size is considered practically equivalent to zero, meaning it has no meaningful impact. Proportions of samples inside the ROPE (−0.18 to 0.18).
Nonetheless, the age of the mother (coefficient = 0.03, 95% CrI: 0.02–0.04, aOR = 1.03), the weight of the mother (coefficient = 0.01, 95% CrI: 9.59e−03 to 0.01, aOR = 1.01), and the number of people in the household (coefficient = 0.14, 95% CrI: 0.12–0.16, aOR = 1.15) were deemed practically insignificant, with 100% of their values residing within the ROPE. Conversely, among the factors with a negative direction of effect, cohabitation with a partner (coefficient = −0.42, 95% CrI: −0.52 to −0.31, aOR = 0.66) compared to living alone, and different levels of education – middle school (coefficient = −0.70, 95% CrI: −0.82 to −0.58, aOR = 0.50), secondary education (coefficient = −0.59, 95% CrI: −0.71 to −0.47, aOR = 0.55), and university education (coefficient = −0.43, 95% CrI: −0.57 to −0.29, aOR = 0.65) in comparison to no formal education, were associated with a reduced likelihood of PPD.
Similarly, a higher number of income contributors within a household (coefficient = −0.28, 95% CrI: −0.33 to −0.22, aOR = 0.75) compared to fewer contributors, and medium-level social support (coefficient = −0.65, 95% CrI: −0.79 to −0.52, aOR = 0.52) compared to low-level social support, were both linked to a decreased likelihood of PPD. Indeterminate factors included the employment status of the mother (coefficient = −0.27, 95% CrI: −0.37 to −0.16, aOR = 0.76) and high-level social support (coefficient = −0.21, 95% CrI: −0.35 to −0.08, aOR = 0.81), with 3.57% and 29.87% of their values inside the ROPE, respectively (Figure 2). These percentages suggest that most values were outside the ROPE and their potential effects on PPD warrant further investigation.
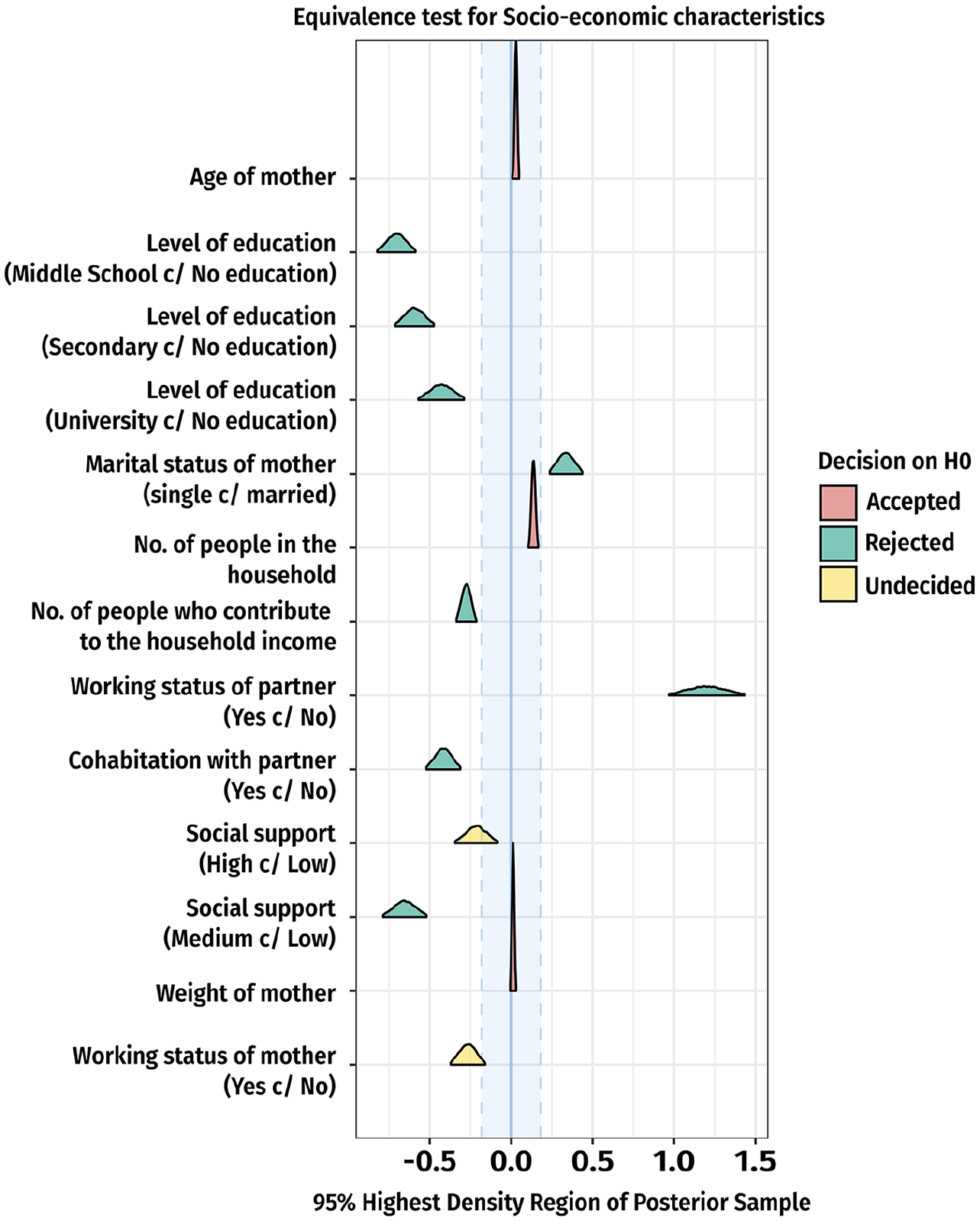
Equivalence test for socioeconomic characteristics with 95% HDR of the posterior sample.
Obstetric characteristics
Among the obstetric characteristics, planned pregnancy (p = 0.011), desired pregnancy (p = 0.006), and exercise during pregnancy (p = 0.040) were significant predictors of PPD. Mothers with planned and desired pregnancies and those who exercised during pregnancy had lower rates of PPD (Table 2). No significant differences were found in relation to gestational age, birth weight, hospitalization during pregnancy, mode of delivery, expected sex of baby, blood transfusion during delivery, exclusive breastfeeding, presence of other biological children, and outcome of pregnancy.
Obstetric characteristics of study participants (n = 502).

EPDS: Edinburgh Postnatal Depression Scale.
Data for continuous variables is presented as mean (standard deviation), rounded off to the nearest tens. p value derived from t-test.
The Bayesian logistic regression analysis revealed that the gestational age, birthweight, desired pregnancy, and mode of delivery were associated with positive direction of effect, that is, increased the likelihood of PPD (Figure 3). Nonetheless, both gestation age (coefficient = 0.02, 95% CrI: 0.01–0.03, aOR = 1.02) and birthweight (coefficient = 0.16, 95% CrI: 0.11–0.20, aOR = 1.17) were either accepted as practically insignificant or undecided, with 100% and 91% of their values inside the ROPE, respectively. A desire to have a pregnancy (coefficient = 0.53, 95% CrI: 0.43–0.64, aOR = 1.70) significantly increased the odds compared to an unwanted pregnancy. Similarly, the mode of delivery by C-section (coefficient = 0.34, 95% CrI: 0.22–0.45, aOR = 1.40), and spontaneous vaginal delivery (coefficient = 0.56, 95% CrI: 0.45–0.67, aOR = 1.75) were associated with a higher likelihood of PPD compared to assisted vaginal delivery.

PD and the ROPE for various obstetric characteristics. The light blue region indicates the ROPE range within which the effect size is considered practically equivalent to zero, meaning it has no meaningful impact. Proportions of samples inside the ROPE (−0.18 to 0.18).
Among the factors with a negative effect of direction, the presence of planned pregnancy (coefficient = −0.25, 95% CrI: −0.29 to −0.20, aOR = 0.78) and doing physical exercise (coefficient = −0.26, 95% CrI: −0.31 to −0.22, aOR = 0.77) were associated with a lower likelihood of PPD. Similarly, when the sex of the baby met the expected sex of the mother (coefficient = −0.28, 95% CrI: −0.34 to −0.22, aOR = 0.75), we observed a decrease in odds for PPD. Mothers who received blood transfusion during delivery (coefficient = −0.26, 95% CrI: −0.32 to −0.20, aOR = 0.77) and mothers who exclusively breastfed (coefficient = −0.23, 95% CrI: −0.28 to −0.18, aOR = 0.79) also demonstrated lower odds for PPD. We also observed that pregnancy involving twins or more children (coefficient = −0.63, 95% CrI: −0.77 to −0.49, aOR = 0.53) had a maternally protective effect compared to pregnancy involving a single child.
Finally, the factors that were undecided in our model included hospitalization during pregnancy (coefficient = −0.23, 95% CrI: −0.29 to −0.18, aOR = 0.79; Figure 4); and having other biological children (coefficient = −0.21, 95% CrI: −0.26 to −0.16, aOR = 0.81). These factors had 1.04% and 9.25% of their values inside the ROPE, respectively. These percentages suggest that most values were outside the ROPE and their potential effects on PPD warrant further investigation.

Equivalence test for obstetric characteristics with 95% HDR of the posterior sample.
Discussion
The present study provides crucial insights into the significance of various sociodemographic and obstetric factors as predictors of PPD among mothers in the Kumasi region of Ghana. A global meta-analytic study estimated the prevalence of PPD to be 17.2% (95% confidence interval: 16.0–18.5), with African-specific data estimating PPD rates to range between 7% and 47%.32,33 The pooled prevalence of PPD (likely diagnosis) in our study was observed to be 25%, though hospital-level prevalence varied between 13% (Ashanti Regional Hospital) and 31% (Tafo Government Hospital). This discrepancy between the various study sites is likely due to the differences in patient volume, timing of sampling, and the diversity in the demographics of the serviced population between the hospitals.
Sociodemographic and economic characteristics
The socioeconomic factors influencing the likelihood of PPD identified in our study offer valuable insights into the complex interplay between various cultural and societal aspects in Ghana. For instance, while studies have demonstrated an association between educational attainment and a reduced likelihood of experiencing PPD in developed economies such as Japan34,35 and Greece, 36 these observations have not been universally validated in Africa. Contradictory evidence has been presented from African countries, with studies from Sudan 37 and Somalia 38 failing to observe any association, while studies from Ethiopia, 39 Kenya 40 and Malawi 41 supporting our observations. Education provides women with a range of skills and resources that can help them cope more effectively with the challenges of pregnancy and motherhood. This notion is supported by studies from Ethiopia and the Democratic Republic of Congo, where the authors found that educated mothers were more likely to engage in health-seeking behaviors and had better access to information about childcare and available support services.42 –44 In addition, education often correlates with higher socioeconomic status, which may alleviate some of the financial and social stressors that may contribute to PPD.
Consistent with previous studies from regional countries, single mothers were found to be more likely to develop PPD than married mothers.45,46 This may be due to the lack of emotional and practical support that typically accompanies parenthood. Single mothers may face increased financial pressures, social isolation, and the absence of a partner to share parenting responsibilities. Similarly, mothers who did not live in the same household as their partner were more likely to experience PPD, underscoring the importance of a supportive co-parenting environment. The presence of a partner can provide emotional support, practical help, and shared responsibilities that can ease the stress and demands of early motherhood.47,48
The employment status of both the mother and her partner played an important role in predicting PPD. Our analysis showed that maternal employment status, yes compared to no, had an indeterminate effect on the odds of PPD. The coefficient of −0.27 suggests a potentially beneficial effect, but with 3.57% of its values within the ROPE, the results are inconclusive. Such inconclusiveness has been observed in the literature, with reports supporting both protective 49 and detrimental effects. 50 Noticeably, a study found significant differences in the likelihood of developing PPD according to workload (part-time, full-time) and job type (professional, office, other) among Japanese mothers. 51 At the same time, the employment status of the partner had an opposite effect; partners who worked increased the likelihood of the mother developing PPD. This may be due to the reduced availability of the partner to provide support at home, leaving the mother to shoulder more of the childcare and household responsibilities alone. The absence of a partner for significant periods of the day can lead to loneliness and feeling overwhelmed, all of which may contribute to the onset of PPD.
Economic stability, which in our study was additionally assessed by the number of people contributing to the household income, was associated with a significantly lower likelihood of PPD. Having multiple contributors to the household income may alleviate financial pressures, ensure better access to essential resources, and reduce the economic burden on the mother. Next, the impact of social support on PPD is a crucial aspect highlighted by this study, in line with reports from other countries.52 –54 Social support can come in various forms, including emotional, informational, and functional assistance, 55 all of which may contribute to a mother’s ability to cope with postpartum challenges. While moderate-level social support demonstrated a significant protective effect against PPD, the equivocal effect of high-level social support suggests a complex relationship that warrants further investigation in the local context.
In our study, maternal age appears to have a minimal effect on the likelihood of developing PPD. The modest increase in the OR and ROPE indicates a negligible effect, underscoring the complex interplay of sociodemographic and obstetric factors. Our findings are consistent with studies that have failed to identify a strong or consistent relationship between maternal age and PPD. For instance, a cross-sectional study conducted in Brazil involving 811 mothers found that while maternal age was associated with a slight reduction in PPD risk (OR = 0.96, p = 0.019), this effect was not modified by the number of children at home, suggesting that age alone may not be a robust predictor of PPD. 56 Similarly, a longitudinal study of 4866 mothers in the Upstate KIDS cohort identified four trajectories of postpartum depressive symptoms but found that maternal age was not a significant predictor of persistent or severe depressive symptoms. 57
Maternal weight also showed no significant association with PPD. The OR for weight indicated a minor effect, reinforcing that maternal weight does not significantly contribute to the likelihood of experiencing PPD. While maintaining a healthy weight is crucial for overall maternal and infant health, our finding suggests that maternal age and weight may not be critical factors when considering the risk of PPD and could be offset by other more critical sociodemographic and obstetric factors.
Obstetric characteristics
Among the obstetric factors, gestational age, and birthweight, while crucial for neonatal health, were found to be practically nonsignificant predictors. This suggests that their influence on maternal mental health is minimal, underscoring the need to focus on more impactful predictors when addressing PPD. On the other hand, the protective nature of planned pregnancies was more evident as women who planned their pregnancies were significantly less likely to develop PPD. Planned pregnancy, in local context, refers to pregnancies that occur when a woman has actively decided to become pregnant and has taken steps to prepare for it. This emphasizes the emotional preparedness and stability that planned pregnancies confer, facilitating better psychological readiness for motherhood, and thereby reducing the risk of depressive symptoms. Meta-analyses of unplanned pregnancies and PPD corroborate our findings, affirming that unplanned pregnancies are associated with higher risks of depression during and after pregnancy.58 –60
Conversely, the increased likelihood of PPD among women with desired pregnancies compared to those with unwanted pregnancies warrants further investigation. This glaring paradox could stem from the psychological and social pressures associated with desired pregnancies. Desiring a pregnancy simply indicates a wish to have a baby but does not necessarily imply that the woman has taken any specific actions to prepare and plan for conception and pregnancy. In many African societies, there is considerable pressure to give birth soon after marriage, which can add to the stress and expectations placed on women.61,62 Such pressures to conform to idealized standards of motherhood, compounded by societal and familial expectations, can exacerbate feelings of inadequacy and depression.
Physical exercise emerged as a significant protective factor against PPD. Regular physical activity is well-documented for its benefits in alleviating symptoms of depression and anxiety, promoting physical health and enhancing mood through endorphin release.63,64 This suggests that integrating physical activity into antenatal and postnatal care programs could be a valuable strategy for supporting maternal mental health. Encouraging postpartum women to engage in suitable physical activities tailored to their abilities and preferences may serve as an effective preventive measure against PPD.
Mode of delivery also played a critical role in influencing the likelihood of PPD. Cesarean sections and spontaneous vaginal deliveries were associated with higher odds of PPD compared to assisted vaginal deliveries. The physical and emotional stresses associated with Cesarean Sections, including prolonged recovery times and potential complications, may heighten susceptibility to PPD.65 –67 Similarly, spontaneous vaginal deliveries, though typically less invasive, can still pose significant physical and emotional challenges. Exclusive breastfeeding emerged as a strong protective factor against PPD. This aligns with previous studies highlighting the psychological benefits of breastfeeding, such as enhanced maternal–infant bonding and favorable hormonal changes.68,69 The act of breastfeeding stimulates the release of oxytocin, which promotes bonding and reduces stress and anxiety.70,71 Additionally, breastfeeding triggers the release of endorphins. 72 The reduced physiological stress response and better sleep patterns associated with breastfeeding may further contribute to lowering the likelihood of PPD.73,74
The study also found that meeting the expected sex of the baby significantly reduced the likelihood of PPD. This is in tandem with the findings of studies conducted in Ethiopia and Basra.75,76 This highlights the impact of cultural and personal expectations regarding the baby’s gender on maternal mental health. Societal and familial pressures about the baby’s gender can lead to significant emotional outcomes postpartum. Counterintuitively, requiring blood transfusion during delivery and being hospitalized during pregnancy emerged as protective factors, reducing the odds of PPD. These findings may suggest that mothers who receive appropriate care and support during pregnancy and delivery may feel more supported and less vulnerable to PPD. In fact, comparable observations have been described in a randomized controlled trial from Slovenia that found no differences in risk of PPD among mothers who were treated for postpartum anemia with different intravenous ferrous preparations compared to the general population. 77
Multiparity, as discussed before, was found to be associated with a reduced likelihood of PPD. The presence of other children might imply that the mother has prior experience with childbirth and child-rearing,78,79 which can enhance her confidence and competence in managing the demands of a new baby. Experienced mothers may have established coping strategies and a better understanding of the postpartum period, reducing the likelihood of being overwhelmed by the challenges of new motherhood. Furthermore, older children can sometimes offer practical assistance and emotional support, contributing to a more supportive home environment.
Limitations
This study has several limitations that warrant consideration. The sample was restricted to five hospitals in Kumasi, Ghana, which might not represent the broader national population. This geographical limitation could impact the generalizability of our findings to other regions. Additionally, the data on PPD and social support were collected using self-reported measures, specifically the EPDS and the ESSI scale. The reliance on self-reported data introduces the potential for recall bias or social desirability bias, especially in a cultural context where mental health issues may carry stigma. Moreover, the cross-sectional design of our study precludes the establishment of causal relationships between the predictors and PPD. Another significant limitation is the omission of potential unmeasured confounders, such as genetic predispositions or detailed mental health histories, which could have influenced our results. Future research should employ longitudinal designs to elucidate the temporal relationships among these variables and address potential confounders comprehensively.
Conclusions
Our study identifies socioeconomic instability (single motherhood, limited education), unplanned pregnancy, and delivery-related stressors as key modifiable predictors of PPD in Ghana. Protective factors, including multi-earner household support, physical exercise, and exclusive breastfeeding, highlight actionable avenues for policy intervention. Our model highlighted the disproportionate psychological risks associated with delivery modes, challenging assumptions about spontaneous vaginal delivery as inherently low risk. These findings emphasize the need for culturally tailored strategies, such as integrating mental health screening into prenatal care, expanding financial safety nets for single mothers, and training physicians to address delivery-related psychological trauma.
Supplemental Material
sj-docx-1-whe-10.1177_17455057251343953 – Supplemental material for Predictors of postpartum depression among new mothers in Kumasi, Ghana: A multicenter study using Bayesian analysis
Supplemental material, sj-docx-1-whe-10.1177_17455057251343953 for Predictors of postpartum depression among new mothers in Kumasi, Ghana: A multicenter study using Bayesian analysis by Joyce Emakayor Bening, Felix Darko, Richard Anterkyi, Vera Korkor Narh, Nana Yaa Agyeman Prempeh, Nityanand Jain, Albert Lawrence Kwansa, Ernest Kissi Kontor and Michael Ntim in Women’s Health
Supplemental Material
sj-docx-2-whe-10.1177_17455057251343953 – Supplemental material for Predictors of postpartum depression among new mothers in Kumasi, Ghana: A multicenter study using Bayesian analysis
Supplemental material, sj-docx-2-whe-10.1177_17455057251343953 for Predictors of postpartum depression among new mothers in Kumasi, Ghana: A multicenter study using Bayesian analysis by Joyce Emakayor Bening, Felix Darko, Richard Anterkyi, Vera Korkor Narh, Nana Yaa Agyeman Prempeh, Nityanand Jain, Albert Lawrence Kwansa, Ernest Kissi Kontor and Michael Ntim in Women’s Health
Supplemental Material
sj-docx-3-whe-10.1177_17455057251343953 – Supplemental material for Predictors of postpartum depression among new mothers in Kumasi, Ghana: A multicenter study using Bayesian analysis
Supplemental material, sj-docx-3-whe-10.1177_17455057251343953 for Predictors of postpartum depression among new mothers in Kumasi, Ghana: A multicenter study using Bayesian analysis by Joyce Emakayor Bening, Felix Darko, Richard Anterkyi, Vera Korkor Narh, Nana Yaa Agyeman Prempeh, Nityanand Jain, Albert Lawrence Kwansa, Ernest Kissi Kontor and Michael Ntim in Women’s Health
Footnotes
ORCID iDs
Ethical considerations
The study was approved by the Committee on Human Research, Publications, and Ethics (CHRPE) of the School of Medical Sciences (SMS) at Kwame Nkrumah University of Science and Technology, Ghana (approval no. CHRPE/AP/148/23 dated February 27, 2023). The study protocol was also supported by individual approvals from the five study centers.
Consent to participate
All participants provided signed written informed consent before enrollment in the study. For participants facing literacy barriers, the consent process was conducted verbally in their native language by a trained female teaching assistant. The study’s purpose, procedures, risks, benefits, and withdrawal rights were explained in a private setting to ensure understanding and minimize potential discomfort. Given the sensitivity of the topic and confidentiality concerns, the requirement for a third-party witness was waived in accordance with the study protocol. To confirm comprehension, participants were asked open-ended questions requiring them to restate key elements of the study in their own words. Consent to participate was documented by a thumbprint on the consent form, which was countersigned by the researcher.
Consent for publication
All participants provided informed consent for publication of data.
Author contributions
Joyce Emakayor Bening: conceptualization; project administration; funding acquisition. Felix Darko: methodology; data curation; investigation. Richard Anterkyi: methodology; investigation; data curation. Vera Korkor Narh: methodology; investigation. Nana Yaa Agyeman Prempeh: project administration. Nityanand Jain: software; writing – review and editing; formal analysis; visualization. Albert Lawrence Kwansa: software; formal analysis; writing – review and editing. Ernest Kissi Kontor: writing – original draft; writing – review and editing; software; formal analysis; methodology. Michael Ntim: conceptualization; project administration; supervision; writing – original draft; writing – review and editing; validation; resources; methodology.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
An anonymized version of the data may be obtained from the corresponding authors on a reasonable request for non-commercial purposes only.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

