Abstract
There is a lack of standardized measurement tools globally to assess knowledge, attitudes, and perceptions of expecting women toward prenatal screening. The purpose of this systematic review was to identify reasons women pursue or decline prenatal screening and compare the strengths and limitations of available measurement tools used to assess pregnant women’s perceptions, knowledge, and attitudes toward prenatal screening. This review followed the five-step York methodology by Arksey and O’Malley and incorporated recommendations from the Preferred Reporting Items for Systematic Reviews and Meta-Analysis checklist for the extraction, analysis, and presentation of results. The five steps consisted of: (1) identification of the research questions; (2) searching for relevant studies; (3) selection of studies relevant to the research questions; (4) data charting; and (5) collation, summarization, and reporting of results. Four online databases (PubMed, Embase, Web of Science, and Cochrane Library) were selected after the librarian’s development of a detailed search strategy. The Rayyan platform was used between June 2023 and August 2023 to epitomize the articles produced from our search. A total of 68 eligible studies were included in the analysis. The top five major reasons for declining prenatal screening uptake included (1) being unsure of the risk of prenatal screening and harm to the baby or miscarriage (n = 15), (2) not considering action such as termination of pregnancy for prenatal screening to be considered as necessary (n = 14), (3) high cost (n = 12), (4) lack of knowledge about testing procedures and being anxious about the test (n = 10), and (5) being worried about probability of false negative or false positive results (n = 6). Only 32 studies utilized scientifically validated instruments. Difficulties in capturing representative, adequately sized samples inclusive of diverse ethnicities and demographics were pervasive. Findings highlight the need for rigorous validation of research measurement methodologies to ensure the accuracy and applicability of resulting data regarding the assessment of prenatal screening perceptions, knowledge, and attitudes across diverse female populations.
Plain Language Summary
The following systematic review provides a comprehensive summary and quality evaluation of measurement tools used globally to assess the role of knowledge, attitudes, and perceptions of pregnant women in seeking prenatal tests.
Introduction
Since the early 2000s, the improvements in maternal and child health indicators have been attributed to better diet and advances in medical care, including the implementation of prenatal tests in pregnant women. 1 The two main types of prenatal testing are screening tests and diagnostic tests. 2 Prenatal screening tests encompass a variety of tests that are used to identify women with increased chances of having children with chromosomal abnormalities or birth defects.3,4 These tests are non-invasive procedures and include fetal nuchal translucency ultrasound, maternal serum blood tests, cell free fetal DNA, and the “quadruple marker” screen. 3 Although prenatal screening tests can identify whether the baby is at-risk of having certain birth defects, they cannot be used for making a definitive diagnosis. 2 In this case, prenatal diagnostic tests are recommended to confirm the diagnosis. 2 These tests include procedures such as amniocentesis and chorionic villus sampling (CVS) and are more invasive as compared to screening tests. 3
Prenatal screening is an essential aspect of maternal healthcare, providing early insights into potential fetal abnormalities and facilitating informed decision-making for expectant mothers. 5 Nevertheless, several barriers persist that limit pregnant women’s ability to benefit from these essential services. 6 Accessibility remains a major obstacle for many women attempting to undergo these tests for a variety of reasons, 7 including geographic, financial, and socioeconomic factors. 8 Women in rural or remote regions often struggle to access medical facilities offering screening, facing higher risks of inadequate prenatal care.6 –8 The limited availability of screening services frequently forces women to travel long distances, incurring logistical and financial burdens.8,9 Patients living in urban areas can also experience challenges obtaining timely appointments at local clinics, particularly in disadvantaged neighborhoods.10,11 Additionally, the lack of culturally appropriate care and language services further impedes women, especially from marginalized communities in accessing and understanding screening options.11 –13
Financial barriers can also impede access to prenatal screening. Out-of-pocket costs for tests, transportation, and lost wages from appointments can be prohibitive.14 –16 In many areas, paying for screening is expensive, especially if insurance coverage is limited.14 –16 Additional expenses like travel, taking time off work, and childcare exacerbate the economic strain.17,18 Fragmented insurance may not cover all needed prenatal tests, heightening challenges in regions with limited coverage and restricting access.19 –21 This may result in disparities and adverse health outcomes.19 –21 Multiple studies reveal financial obstacles disproportionately affecting marginalized groups, amplifying existing healthcare inequities.10,15,19,20 Ultimately, these accessibility barriers contribute to disparities in prenatal care, with potentially severe implications for maternal and fetal health.8,9,11 –13
Despite readily available, high quality information, misconceptions still deter many pregnant people from seeking out prenatal screening. Beyond the misinformation available, seemingly at every turn, studies reveal concerns about risks of procedures, misunderstandings regarding test accuracy, and cultural/religious beliefs that associate tests with bad omens among pregnant women.22 –27 Fears about invasiveness or potential harm also contribute to hesitation.28 –30 Additionally, anxiety about discovering anomalies, coupled with uncertainty around available options after diagnosis lead some to avoid screening.23 –26,28,31 Addressing these misconceptions and concerns is crucial for ensuring equitable access to prenatal tests, which are vital for early detection and effective management of potential maternal and fetal health issues.28 –30
Although prenatal screening is critically important during pregnancy, there is a global scarcity of standardized tools to evaluate women’s knowledge, attitudes, and perceptions of such tests.32 –35 The purpose of this systematic review was to identify reasons women pursue or decline prenatal screening and compare the strengths and limitations of available measurement tools used to assess these reasons. This analysis also highlighted the theoretical underpinnings used to validate these tools to inform their broader usage across different countries. Ultimately, findings from this review may facilitate the development of standardized global assessment tools focused on women’s knowledge, attitudes, and perceptions of prenatal screening.
Methods
The study sections 1–5 were organized using the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guideline as a checklist reference. 36 This review followed the York methodology by Arksey and O’Malley (2005) 37 for the extraction, analysis, and presentation of results in systematic reviews.
Step 1. The guiding research questions
The four guiding research questions for this systematic review were: (1) Which measurement tools have been used globally to assess attitudes, knowledge, and perceptions of pregnant women toward prenatal screening? (2) What are the major reasons for uptake or decline of prenatal screening tests among pregnant women? (3) What are the limitations of these tools, and to what extent have these tools been validated? (4) Which theoretical constructs have been used in the development of these tools and were significantly associated with the uptake or decline of prenatal screening?
Step 2. Search for relevant studies
Keywords were developed in collaboration with a research librarian (MK) experienced in systematic review protocols. The search terms focused on: measurement tools, surveys, questionnaires, theoretical frameworks, pregnancy, perceptions, prenatal screening, prenatal diagnosis, attitudes, and knowledge. Four online databases (PubMed, Embase, Web of Science, and Cochrane Library) were selected after the librarian’s development of a detailed search strategy (Supplemental File 2). The Rayyan platform was used between June 2023 and August 2023 to epitomize the articles produced from our search, performed by the senior author (LS) and co-authors (SB, YZ, GO, AL, SA, MG, ST, SK).
Inclusion criteria
Included peer-reviewed articles were published between 2013 and 2023 that (1) focused on pregnant women, (2) included measurement tools assessing perceptions toward invasive (amniocentesis, CVS) and non-invasive (magnetic resonance imaging, ultrasound) prenatal screening, (3) were qualitative, observational, and experimental studies, and (4) included pregnant women who completed or did not complete prenatal screening.
Exclusion criteria
Excluded were articles that focused on genetic counselling rather than prenatal screening and genetic testing, non-pregnant women, women undergoing termination of pregnancy or any type of prenatal preparation or decision aid not involving screening, articles that did not include measurement tools for assessment of knowledge, attitudes or perceptions toward prenatal screening, and scoping, systematic, and narrative reviews or experimental studies.
Step 3. Selection of studies relevant to the research questions
All co-authors (SB, YZ, GO, SA, MG, AL, ST, SK) extracted and summarized data. Senior author (LS) reviewed all tabulated data to resolve any discrepancies. Summary tables included one evidence table describing study characteristics such as country, study design, study population, age range, study purpose, constructs of interest measured, other constructs, social determinants of health (SDOH), status of prenatal screening uptake at the start of the study, association between constructs of interest and outcome, major reasons for prenatal screening uptake, and major reasons for declining prenatal screening uptake (Supplemental File 1). Table 1 includes the type of analysis used in measuring associations between pregnant women’s knowledge and attitudes toward prenatal screening and test uptake, whether the tool used was validated or not, mode of tool administration, and when relevant, theoretical framework used and specific constructs measured. Table 2 is a lessons learned table. Basic qualitative content analysis was used to identify similar themes in future directions across studies. Table 3 consists of the application of the Critical Appraisal Skills Programme (CASP) Checklist to assess study rigor and quality.
Methodological applications and type of analysis in prenatal screening assessment tools.
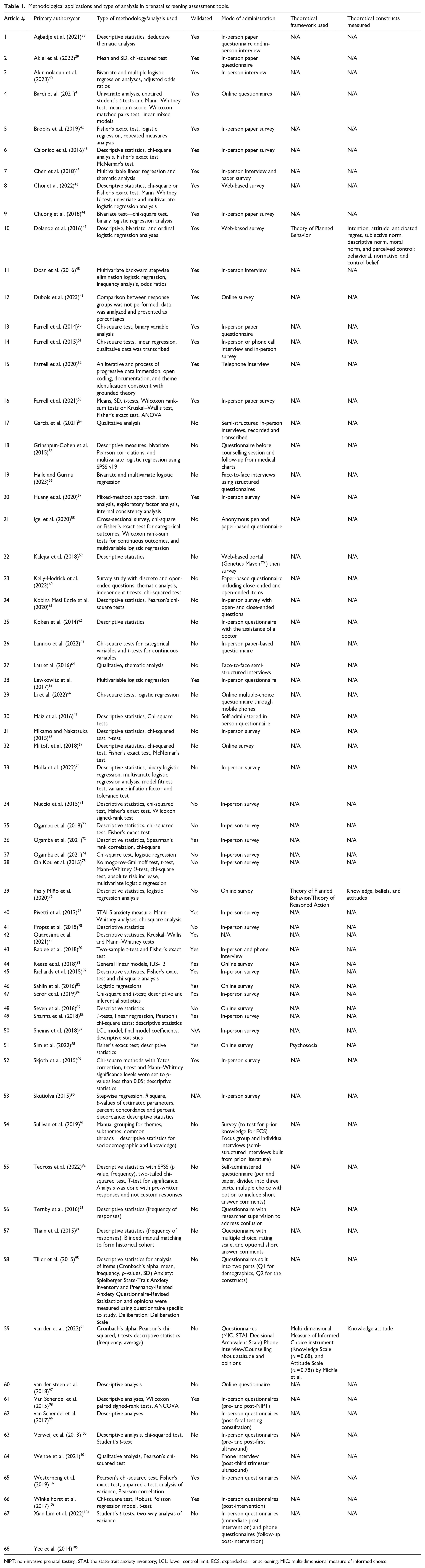
NIPT: non-invasive prenatal testing; STAI: the state-trait anxiety inventory; LCL: lower control limit; ECS: expanded carrier screening; MIC: multi-dimensional measure of informed choice.
Qualitative findings of major reported tool limitations across studies.

NIPT: non-invasive prenatal testing.
Critical appraisal skills programme checklist for assessing study rigor and quality.

Quality score = total number of indicators reported by each study, which is marked as yes.
Indicators that scored in a reversed manner.
Steps 4 and 5. Data charting and collation, summarization, and reporting of results
Study characteristics were tabulated for primary author and year of study, location of each study, study design, sample size, study population, age range, study purpose, constructs of interest, types of SDOH, completion status of prenatal screening at the start of the study, association between constructs of interest and outcome, and reasons for prenatal screening completion/declining of test uptake (Supplemental File 1). Types of analysis used were tabulated for each study alongside the status of validation for each survey and its mode of administration, theoretical framework used, and theoretical constructs of interest measured which included perceptions, attitudes, and knowledge (Table 1). Limitations of the measurement tools used in each study were listed for each author and publication (Table 2). The three phases of qualitative content analysis for the results of primary qualitative research described by Elo and Kyngas (2008) were applied to summarize and highlight major reported limitations across included studies: (1) preparation, (2) organizing, and (3) reporting.
One of the co-authors, SK, evaluated the validity and quality of the study using the CASP checklist. 106 The CASP checklist determines the risk of bias and examine methodological quality and has been used in previous systematic reviews.107,108 Within this systematic review, the CASP checklist provided insight into the following criteria: (1) clarity of stated study aims and objectives, (2) appropriateness of study methods, (3) adequate description of the methodology, (4) bias in sample selection, (5) representativeness of the sample for generalizability of the study results, (6) utilization of a statistical power analysis for sample size calculation, (7) response rate, (8) utilization of reliable and valid measures, (9) examination for statistical significance, and (10) inclusion of confidence intervals (CI) in study findings.107,108 The response to each criterion is classified as either “yes,” “no,” or “unsure,” and a quality score was calculated by summing the number of “yes” responses for each criterion, with the response of item 4. A score of >4 indicates high quality, a score of 3–4 shows moderate quality, and a score of <3 represents low quality. 109 For the quality score, the score of “no” for item 4 was summed, as this indicated study rigor, which was positively reflected in the quality score. 109 The CASP checklist findings are shown in Table 3.
Results
The initial study extraction resulted in 3150 studies from PubMed (n = 1630), Embase (n = 1102), and Web of Science (n = 418). Studies were excluded if they focused on populations other than the one defined in this study (pregnant women) (n = 905), directed at partners or health professionals (n = 753), were not qualitative, observational or experimental studies (n = 381), were not related to the assessment of attitudes and knowledge but more of informed choice (n = 65), addressed subjects undergoing termination of pregnancy (n = 64), and were published in a foreign language (n = 10). Duplicate studies were deleted (n = 894) (Figure 1).

PRISMA flow chart for study selection process.
Seventy-eight studies met inclusion criteria from PubMed (n = 51), EMBASE (n = 22), and Web of Science (n = 5). An additional 10 studies were excluded following a full study review due to being published abstracts rather than full peer-reviewed articles (n = 6), missing measurement tools for assessment of knowledge and attitudes toward prenatal screening (n = 3) and focusing on cervical cancer screening rather than prenatal screening (n = 1). A total of 68 eligible studies were retained for analysis38 –105 (Figure 1).
The 68 retained studies were published between 2013 and 2023. Most studies (41/68, 68%) were published in 2018 or later (n = 41). Study designs included qualitative studies (n = 5), cohort studies (n = 10), randomized controlled trials (n = 4), mixed methods studies (n = 3); and cross-sectional studies (n = 46). The sample size ranged from n = 15 to n = 2430 participants. Retained studies were conducted in the following countries: Canada (n = 4), China (n = 3), Czech Republic (n = 1), Denmark (n = 2), Ethiopia (n = 3), Finland (n = 1), France (n = 1), Ghana (n = 1), India (n = 1), Iran (n = 1), Italy (n = 2), Japan (n = 1), Korea (n = 1), Netherlands (n = 10), Nigeria (n = 4), Saudi Arabia (n = 1), Singapore (n = 3), Spain (n = 2), Sweden (n = 2), Taiwan (n = 1), Turkey (n = 2), USA (n = 19); and Vietnam (n = 2).
Major constructs and SDOH explored
The major SDOH explored included age (n = 56), education (n = 56), religion (n = 30), socioeconomic status (n = 27), employment (n = 20), ethnicity (n = 18), marital status (n = 18), race (n = 15), health literacy (n = 11), number of children (n = 8), language (n = 6), residence (n = 5), nationality (n = 3), birthplace (n = 3), access to healthcare (n = 3), transportation (n = 1), and insurance (n = 1). The frequency of constructs of interest measured across the studies were as follows: attitudes (n = 53), knowledge (n = 43), preferences (n = 13), perceived risk (n = 12), awareness (n = 6), psychological outcomes (n = 3), barriers (n = 3), perceived usefulness (n = 1), and acceptability (n = 1). Other constructs measured consisted of obstetric history (n = 35), demographics (n = 22), personal values (n = 18), anxiety (n = 10), health literacy (n = 8), medical history (n = 5), deliberation (n = 4), satisfaction (n = 4), stigma (n = 4), external influence (n = 3), expectations (n = 3), informed choice (n = 3), intention (n = 2), individual autonomy (n = 2), sadness (n = 1), anger (n = 1), doubt (n = 1), confidence (n = 1), reassurance (n = 1), convenience (n = 1), efficiency (n = 1), and psychiatric history (n = 1). The total number of significant associations between constructs of interest (n = 97) and prenatal screening uptake or decline was greater than reported nonsignificant associations (n = 11).
Reasons for accepting or declining prenatal screening uptake
The top five major reasons for accepting prenatal screening uptake included the need to (1) have time to plan and adapt for possible medical conditions (n = 16), (2) have as much information as possible regarding the health of the fetus (n = 15), (3) have reassurance about the health of the fetus (n = 14), (4) have the ability to make decisions regarding possible early termination of pregnancy (n = 14), and (5) having high perceived maternal risk status (age, consanguineous relationship) as well as low perception of accuracy about screening measures and low risk of the procedures (n = 8). The top five major reasons for declining prenatal screening uptake included (1) being unsure of the risk of prenatal screening and harm to the baby or miscarriage (n = 15), (2) not considering action such as termination of pregnancy for prenatal screening to be considered as necessary (n = 14), (3) high cost (n = 12), (4) lack of knowledge about testing procedures and being anxious about the test (n = 10), and (5) being worried about probability of false-negative or false-positive results (n = 6).
Methodological applications and type of analysis in prenatal screening assessment tools
A variety of methods were used to analyze the data across the 67 studies. Descriptive statistics (n = 41) was by far the most common methodology used, followed by chi-squared tests (n = 31), t-tests (n = 16), various logistic regression models (n = 16), and Fisher’s exact tests (n = 12). Other methods included qualitative analysis (n = 6), Mann–Whitney U tests (n = 6), thematic analysis (n = 5), Wilcoxon tests (n = 5), various linear regression models (n = 4), and ANOVA (n = 4), among others. Of the included studies, 32 used validated tools to gather data. Methods of administration included in-person paper surveys (n = 45), online surveys (n = 13), in-person interviews (n = 9), and telephone interviews (n = 5). One of the studies included did not specify how they collected their data. Three of the studies used at least one theoretical framework when conducting their analyses, including the theory of planned behavior (n = 2), the theory of reasoned action (n = 1), and the psychosocial theory (n = 1).
Limitations of measurement tools
A qualitative analysis across multiple relevant studies revealed several common limitations in existing questionnaires and measurement tools used to assess pregnant women’s knowledge, attitudes, and perceptions regarding prenatal screening (Table 2). Thematic analysis indicated issues such as potential biases stemming from social expectations or influences from healthcare personnel and medical settings. Studies noted how instructions and surveys may lack comprehension for those with varied literacy levels, languages, or cultural backgrounds. Researchers encountered difficulties obtaining sufficiently large and representative samples across diverse ethnicities and demographics. Many highlighted the need for improved stratification when segmenting participant samples (Table 2). Additionally, several studies raised reasonable doubts regarding the reliability and validity of current assessment tools in capturing high-quality, generalizable data. Data collection methods and the integrity of data itself were also identified as lacking in numerous cases. Together, these interrelated themes coalesce around gaps in accuracy, inclusiveness, and depth of understanding. By addressing such limitations in research design and methodology, future efforts may enhance representation and comprehensiveness when evaluating this vital domain of prenatal care. Standardization of knowledge assessments and attitude surveys stands to benefit providers and families alike.
CASP checklist
Overall, all included studies reported their study aim and study design (Table 3). Sixty-seven of the 68 included studies reported how their subjects were selected. Although most, n = 44 (65%) studies did not mention selection bias as a limitation, less than half, n = 31 (46%) of the studies reported sample generalizability. In addition, n = 26 (38%) studies reported a statistical power estimate of the sample, with n = 29 (43%) reporting their survey response rates. Of all included studies, n = 32 (47%) utilized valid measures. Most of the included studies, n = 59 (87%), reported statistical significance; however, only n = 20 (29%) reported CI. The quality score of the included studies ranged from three (n = 2, 3%) to ten (n = 2, 3%) out of ten. Most, n = 22 (32%) studies had a score of six, with n = 1 (1%) study with a score of four, n = 11 (16%) studies with a score of five, n = 16 (24%) studies with a score of seven, n = 11 (16%) studies with a score of eight, and n = 3 (4%) studies with a score of nine. Studies with a quality score of six or seven indicate a high-quality score with moderate rigor; n = 38 (56%) studies fit this classification (Table 3).
Discussion
The purpose of this systematic review was to comprehensively explore the quality of measurement tools used to assess pregnant women’s knowledge, attitudes, and perceptions regarding both invasive and non-invasive prenatal screening procedures. Key influences emerged from the analysis regarding factors driving pregnant women’s decisions to accept or decline prenatal screening tests. These included knowledge, attitudes/perspectives, and risk perception related to screening procedures. A 2022 study by van der Meij et al. 110 assessing women’s views on non-invasive prenatal testing (NIPT) found higher rates of informed choice among test acceptors (76.8%) versus decliners (59.6%). Additionally, most women reporting uninformed decisions stated they had insufficient knowledge or had not adequately deliberated their choice, indicating knowledge gaps. 110 Several studies also demonstrated that attitudes significantly impacted the intent to pursue screening.111 –113 Pop-Tudose et al. (2018) found nearly 75% alignment between women’s attitudes about testing and their decision to undergo available screening. A study by Seror et al. 84 on attitudes toward invasive and non-invasive procedures for high-risk pregnancies had comparable findings, with choices reflecting patient attitudes.
Perceived risk also influenced choice, with Kowalcek 111 showing anxiety around both the invasive methods as well as the resulting information. However, despite identifying those impactful factors, only three studies embedded relevant frameworks such as the theory of planned behavior that evidence recommends including in measurement tools.113 –116 The importance of theoretical frameworks in establishing evidence-based measurement tools tailored to populations of interest is highlighted throughout several previously published studies. For example, a study by Dusin et al. 113 found that frameworks that do not integrate patient values have a reduced chance of success. Hence, future studies should integrate relevant theoretical frameworks to provide guidance on how to address pregnant women’s attitudes toward and risk perceptions and knowledge of prenatal screening acting as barriers hindering test completion.
Our analysis shows that SDOH such as encompassing financial stability, education, healthcare access, neighborhood and environment, and social contexts should be considered when evaluating prenatal screening behaviors. This is in line with prior research, which demonstrates that SDOH provide critical insights into disparities observed across groups in pursuing screening.114,116 For example, a 2022 study by Priti et al. examining patient portal engagement for prenatal care found variation across risk levels and race/ethnicity. Prior evidence links portal use to better medication adherence, disease awareness, self-management, and care quality. 115 However, Singh et al. found that non-Hispanic Black women had the lowest portal utilization rates regardless of SDOH elements and risk status, reflecting systemic disadvantages. 116 Gadson et al. applied the three-delays model capturing the SDOH influence on prenatal care access across populations. 114 This framework identifies delays in (1) seeking care, (2) reaching care and (3) receiving adequate care as driving maternal health outcomes. Evidence shows lower, slower access for minority women, including timely affordable care. 117 National statistics indicate higher inadequate care rates among Black versus White/Hispanic mothers. 118 SDOH-related barriers also reduce adequate utilization among younger, less educated Black women and those facing unstable circumstances like unplanned pregnancies or uninsured status.119,120 Thus, SDOH require research consideration as major, measurable contributors to prenatal screening inequities.
Our systematic analysis of measurement tools assessing knowledge, attitudes, and perceptions of prenatal screening revealed a significant limitation—only 32 of the 68 studies utilized scientifically validated instruments. This gap is highly concerning given the array of challenges identified across study tools. Several core themes emerged highlighting critical areas needing improvement. These included risks of bias, especially from societal expectations or influences from healthcare staff administering surveys. Comprehension issues were also noted for those with varied literacy, languages or cultural perspectives. Difficulties in capturing representative, adequately sized samples inclusive of diverse ethnicities and demographics were pervasive. Better stratification during sampling was highlighted for enhancement. Additionally, reasonable doubts exist regarding reliability and validity across numerous current tools to robustly measure complex perceptions. Finally, flaws in data collection approaches and the integrity of the resulting data itself were uncovered. Addressing these measurement limitations is imperative for accurate, generative assessment of knowledge and attitudes within this vital domain of prenatal care. Employing scientifically validated instruments, free from pervasive biases, comprehension gaps, sampling errors, validity questions or data quality issues is essential to produce actionable insights that enhance understanding and better support families.
Implications for practice
Considering the diverse backgrounds of pregnant women globally, especially those in underserved communities or ethnic/minority groups, employing culturally tailored tools is vital. Instruments incorporating varied literacy levels, languages, and cultural perspectives are essential for equitable access and understanding regarding prenatal screening. This contributes to improved health outcomes across women with diverse backgrounds.45,47,114 Our findings highlight the need for rigorous selection and validation of research measurement methodologies to ensure the accuracy and applicability of resulting data across diverse female populations. Effectively addressing barriers hindering screening test uptake requires appropriate assessment tools, particularly those addressing knowledge, attitudes, and risk perceptions, which were highlighted as significant influential factors in the prenatal screening decision-making process. The formal assessment of existing prenatal screening surveys conducted in this study offers guidance for developing standardized approaches physicians could adopt to decrease misconceptions, enhance positive attitudes, and communicate potential risks in pregnant patients. Tailoring comprehension of prenatal screening to patients’ needs and circumstances may expand access to specialized care and associated health benefits. Additionally, the identified limitations of current measurement tools spotlight opportunities to advance methodologies by addressing pervasive risks of bias, sampling errors, validity doubts, and data integrity issues. Employing scientifically sound instruments strengthened against such weaknesses is imperative for generating actionable insights to guide families and providers. Ensuring pregnant women globally are equipped with substantive understanding of screening options holds significance for enabling informed decisions and enhancing maternal–fetal health through early detection and management.
Limitations
This systematic review aimed to explore reasons women pursue prenatal screening, and evaluate measurement tools used globally to assess knowledge, attitudes, and perceptions of prenatal screening among pregnant women. However, some limitations should be acknowledged.
First, gray literature and reference list tracing were not included, possibly omitting relevant unpublished studies. Second, only English language publications were encompassed, excluding potentially pertinent non-English research despite the review’s international scope. Third, some relevant search terms around screening barriers, attitudes, or knowledge may have been unintentionally discarded given the emergence of new terminology in a rapidly evolving field. However, the detailed mesh terms, PRISMA guidelines and protocol support likely minimized such risks. Fourth, the 2013–2023 timeframe may have excluded informative historical measurement approaches.
Additionally, further validation is needed for existing measurement tools, as our formal quality assessment using the CASP checklist indicated. Future research studies could inform standardization around adequately and comprehensively assessing patient and social factors influencing prenatal screening uptake. Exploring theoretical constructs beyond knowledge, attitudes, and perceptions that predict screening behaviors could also be illuminating.
Overall, this review provides timely and robust initial insights into the current limitations of prenatal screening measurement tools and reasons women pursue or decline prenatal screening. Ongoing advances in methodology are needed toward inclusive, equitable, and clinically actionable assessments that elevate understanding to support patients and families.
Conclusion
Our systematic review sought to examine the advantages and drawbacks of measurement tools utilized to gauge the attitudes, knowledge, and risk perceptions of pregnant women regarding prenatal screening on a global scale. The findings offer insights that could enhance the development of a standardized measurement tool in clinical settings, aiming to boost overall prenatal screening rates and alleviate knowledge, negative attitude, and misconception barriers impeding the adoption of prenatal tests. The findings of this study suggest that effective strategies for disseminating and promoting information on prenatal screening successfully should consider SDOH, attitudes, knowledge, and risk perceptions of pregnant women as they can influence the decision-making process of prenatal test uptake.
Supplemental Material
sj-docx-1-whe-10.1177_17455057241273557 – Supplemental material for Exploring measurement tools used to assess knowledge, attitudes, and perceptions of pregnant women toward prenatal screening: A systematic review
Supplemental material, sj-docx-1-whe-10.1177_17455057241273557 for Exploring measurement tools used to assess knowledge, attitudes, and perceptions of pregnant women toward prenatal screening: A systematic review by Lea Sacca, Yasmine Zerrouki, Sara Burgoa, Goodness Okwaraji, Ashlee Li, Shaima Arshad, Maria Gerges, Stacey Tevelev, Sophie Kelly, Michelle Knecht, Panagiota Kitsantas, Robert Hunter, Laurie Scott, Alexis Piccoli Reynolds, Gabriela Colon and Michele Retrouvey in Women’s Health
Supplemental Material
sj-docx-2-whe-10.1177_17455057241273557 – Supplemental material for Exploring measurement tools used to assess knowledge, attitudes, and perceptions of pregnant women toward prenatal screening: A systematic review
Supplemental material, sj-docx-2-whe-10.1177_17455057241273557 for Exploring measurement tools used to assess knowledge, attitudes, and perceptions of pregnant women toward prenatal screening: A systematic review by Lea Sacca, Yasmine Zerrouki, Sara Burgoa, Goodness Okwaraji, Ashlee Li, Shaima Arshad, Maria Gerges, Stacey Tevelev, Sophie Kelly, Michelle Knecht, Panagiota Kitsantas, Robert Hunter, Laurie Scott, Alexis Piccoli Reynolds, Gabriela Colon and Michele Retrouvey in Women’s Health
Supplemental Material
sj-docx-3-whe-10.1177_17455057241273557 – Supplemental material for Exploring measurement tools used to assess knowledge, attitudes, and perceptions of pregnant women toward prenatal screening: A systematic review
Supplemental material, sj-docx-3-whe-10.1177_17455057241273557 for Exploring measurement tools used to assess knowledge, attitudes, and perceptions of pregnant women toward prenatal screening: A systematic review by Lea Sacca, Yasmine Zerrouki, Sara Burgoa, Goodness Okwaraji, Ashlee Li, Shaima Arshad, Maria Gerges, Stacey Tevelev, Sophie Kelly, Michelle Knecht, Panagiota Kitsantas, Robert Hunter, Laurie Scott, Alexis Piccoli Reynolds, Gabriela Colon and Michele Retrouvey in Women’s Health
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
