Abstract
Objective:
The clinical implications of B7H1 and B7H4 in pancreatic cancer have been described however, the prognostic significance of these genes in pancreatic cancer patients remains inconclusive. The aim of the present study was to evaluate the prognostic role of B7H1 and B7H4 in pancreatic cancer patients.
Methods:
Electronic databases (PubMed, EMBASE, and the Cochrane Library) were searched for relevant articles published before May 2019. Meta-analyses were performed by pooling the hazard ratios (HRs) between overall survival or cancer-specific survival and high or low expression of B7H1/B7H4 in pancreatic cancer patients. Subgroup and sensitivity analyses were performed, and sources of variabilities were explored by performing meta-regression.
Results:
Sixteen studies (1434 patients’ data) were included. Compared with low expression, high expression of B7H1 was associated with significantly poor overall survival (HR 1.92 (95% confidence interval (CI) 1.35, 2.74); P<0.001) and cancer-specific survival (HR 2.46 (95% CI 1.55, 3.90); P<0.001). High expression of B7H4 also predicted poor overall survival (HR 2.38 (95% CI 1.89, 3.00); P<0.001). In subgroup analyses, a significant association between B7H1 and overall survival was observed for trials conducted in China (HR 2.08 (95% CI 1.29, 3.34)) but not in Japan (HR 1.98 (95% CI 1.33, 2.96)); or in studies with <50% patients having high expression (HR 2.02 (95% CI 1.40, 2.91)) but not in studies with >50% patients with high expression (HR 1.40 (95% CI 0.87, 2.26)).
Conclusion:
The current study suggests that high B7H1 and B7H4 expression is associated with a poor prognosis in pancreatic cancer patients.
Introduction
Pancreatic cancer (PC) is among the most lethal malignant tumors, which ranks as the fourth leading cause of cancer-related mortality. 1 Because symptoms remain unspecific during early phases, PC is usually diagnosed at an advanced stage, which makes prognosis poor with median overall survival (OS) of <1 year and 5-year OS of approximately 5%. 2 Even for patients with operable PC, the 5-year survival rate is not good (18%–24%). 3 The scenario thus necessitates identification of new biomarkers to predict the prognosis of PC patients and to individualize treatment.
Tumor cells are capable of creating a microenvironment by altering their immunogenic properties, especially the co-stimulatory molecules, such as the B7 family, which are not usually produced by the normal cells.4,5 Over the past decade, many research groups have emphasized the importance of B7 family molecules in cancer surveillance; currently, several clinical trials are targeting these pathways.6,7
B7H1 is a member of B7 family of immunoglobulin (Ig) superfamily. Like other B7 family molecules, the extracellular domain of B7H1 has an IgV, and an IgC, with a transmembrane domain and an intracellular domain. Although the messenger RNA of B7H1 has been found to be widely distributed in almost every tissue, cell surface B7H1 only exists in Kupffer cells of the liver, and macrophage-derived cells, such as pneumocyte, which can be detected by immunohistochemistry using the human B7-H1-specific monoclonal antibody (mAb). By contrast, B7H1 is abundant on the surface of many human cancers, and its expression is easily induced by interferon (IFN)-gamma. 8
B7H4 also belongs to the B7 ligand family. Many members of this family are involved in the immune processes and carcinogenesis. Overexpression of B7H4 leads to epithelial transformation and anoikis prevention. 9 Previous studies have shown that B7H4 may be a useful biomarker for cancer diagnosis and prognosis.10,11 The expression of B7H4 in pancreatic cancer has been reported12,13 and it has been found that the expression level of B7H4 is related to the adverse pathological characteristics of pancreatic cancer. 14
Several studies have reported the association between B7H1 and/or B7H4 and the prognosis of pancreatic cancer, but the outcomes vary across these studies. The aim of this meta-analysis was to evaluate the association between B7H1 or B7H4 expression and survival outcomes in pancreatic cancer patients.
Methods
The present study was carried out by following the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines. 15 All analyses were based on data obtained from previously published studies; thus, no ethical approval and patient consent were required.
Literature search strategy
Databases (PubMed, EMBASE, and the Cochrane Library) were systematically searched to identify articles evaluating the prognostic value of B7H1 and/or B7H4 expression in pancreatic cancer published before May 2019. Articles were identified with search terms including “B7H1” OR “B7H4” OR “CD274” AND “pancreatic cancer” AND “prognosis” OR “prognostic”. A secondary search included the scrolling of reference lists of relevant research and review articles.
Study selection
Inclusion criteria were: Study (a) recruited patients with pathologically proven stage I–IV pancreatic cancer; (b) investigated the relationship between the expression level of B7H1 and/or B7H4 and the prognosis of PC patients; and (c) reported the hazard ratios (HR) of B7H1 and/or B7H4 for OS or cancer-specific survival (CSS), or reported data that could be used to calculate HRs. Exclusions included abstracts and unpublished studies, or multiple research articles of same study.
Data extraction
Demographic, clinical, and pathological characteristics of the patients, study design features, study conduct, methodology and analysis details, outcome measures and outcomes were extracted from research articles of the respective studies.
Statistical method
Meta-analyses were performed by pooling the individual study data to achieve overall HR and its 95% confidence intervals (CI). Subgroup analyses were performed with regard to country of study conduct, sample size, percentage of patients with high B7H1 expression, or method used to determine B7H1.
Statistical heterogeneity (between-studies inconsistency in outcomes) was estimated by using the I2 index. Meta-regression analyses were performed to identify the source/s of variability. Sensitivity analyses were performed to test the effect of the exclusion of each study (one at a time) on the outcomes. The publication bias assessment was performed with the visual inspection of funnel plots and by performing Begg’s and Egger’s tests. All statistical analyses were performed with Stata software (version 12; Stata Corporation, TX, USA).
Results
Characteristics of the studies
Figure 1 shows a flowchart of study identification and selection procedure. In a literature search, 251 articles were identified. Manual review of the reference lists of retrieved manuscripts concerning B7H1 or B7H4 expression in pancreatic cancer yielded four additional studies that met the inclusion criteria for this meta-analysis. However, 16 studies16-31 were finally selected for meta-analysis after the removal of duplicates and the application of eligibility criteria.
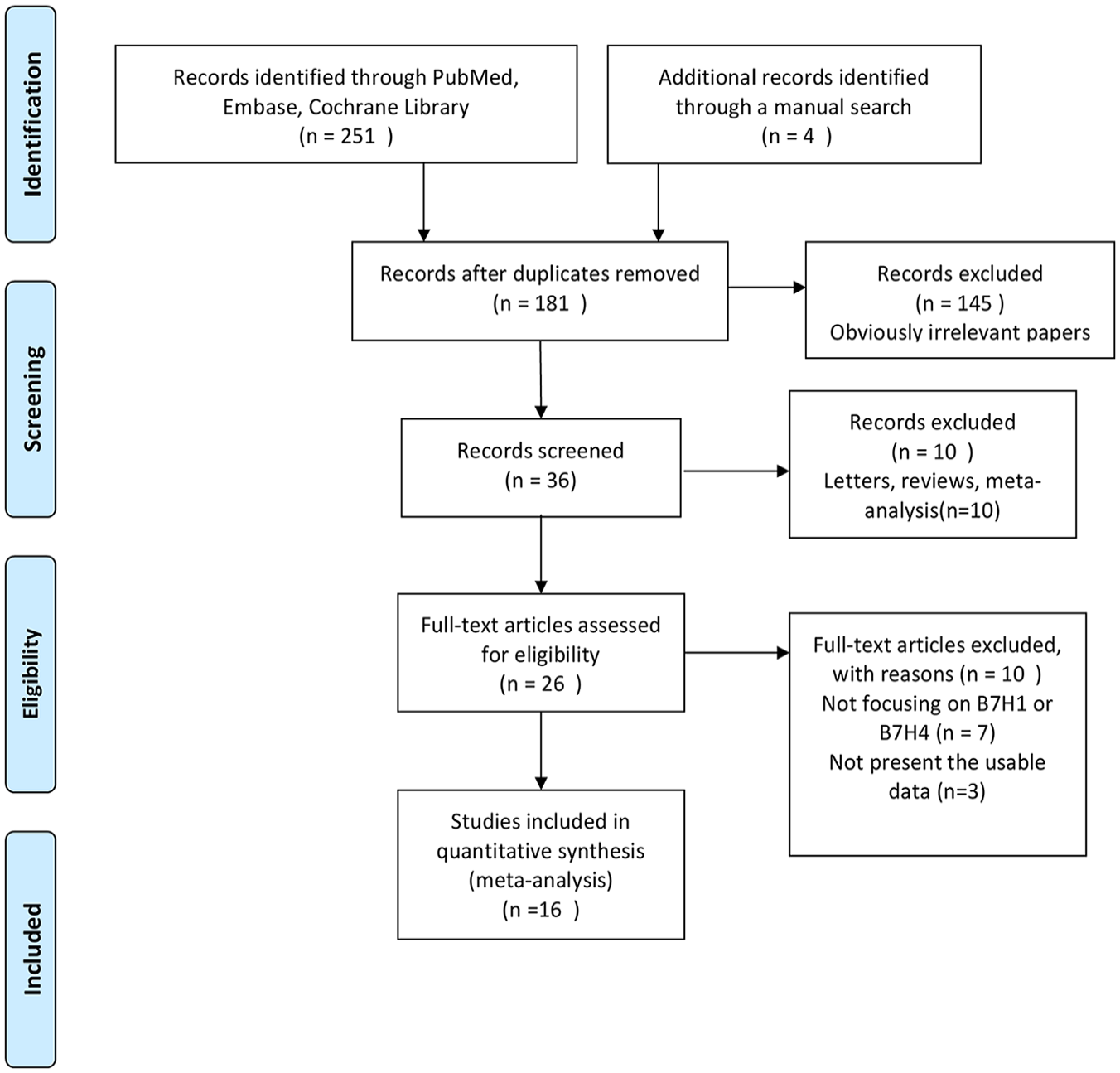
Flow diagram of study identification and selection.
Among these studies, 11 trials investigated B7H1, and 4 studies investigated B7H4, whereas 1 study investigated both B7H1 and B7H4. The overall population of this meta-analysis consisted of 1434 (range, 32 to 373) PC patients. The average age of these patients was 63.6 years (range, 18 to 89 years). These trials were conducted in six countries (China, France, Germany, Greece, Japan, USA) and these studies were published from 2007 to 2019. Table 1 presents the characteristics of the included studies.
Characteristics of randomized controlled trials included in this meta-analysis.
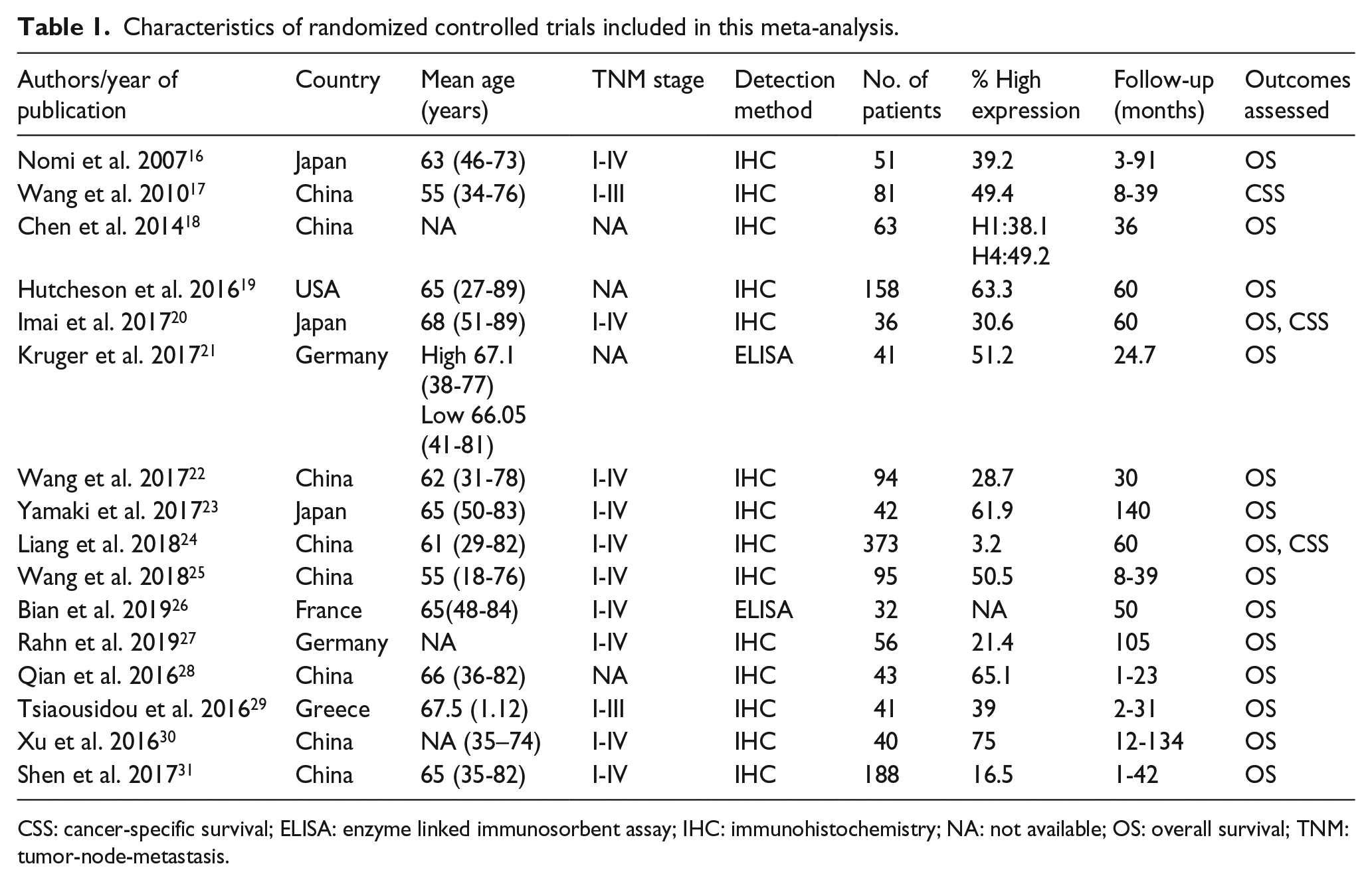
CSS: cancer-specific survival; ELISA: enzyme linked immunosorbent assay; IHC: immunohistochemistry; NA: not available; OS: overall survival; TNM: tumor-node-metastasis.
Quantitative synthesis
A random-effects meta-analysis of 11 studies (1122 patients) showed that, compared with low expression, high expression of B7H1 was associated with significantly poor OS (HR 1.92 (95% CI 1.35, 2.74); P<0.001; Figure 2(a). Between-studies statistical heterogeneity was significant (I2=79.8%; P<0.0001) in this meta-analysis.
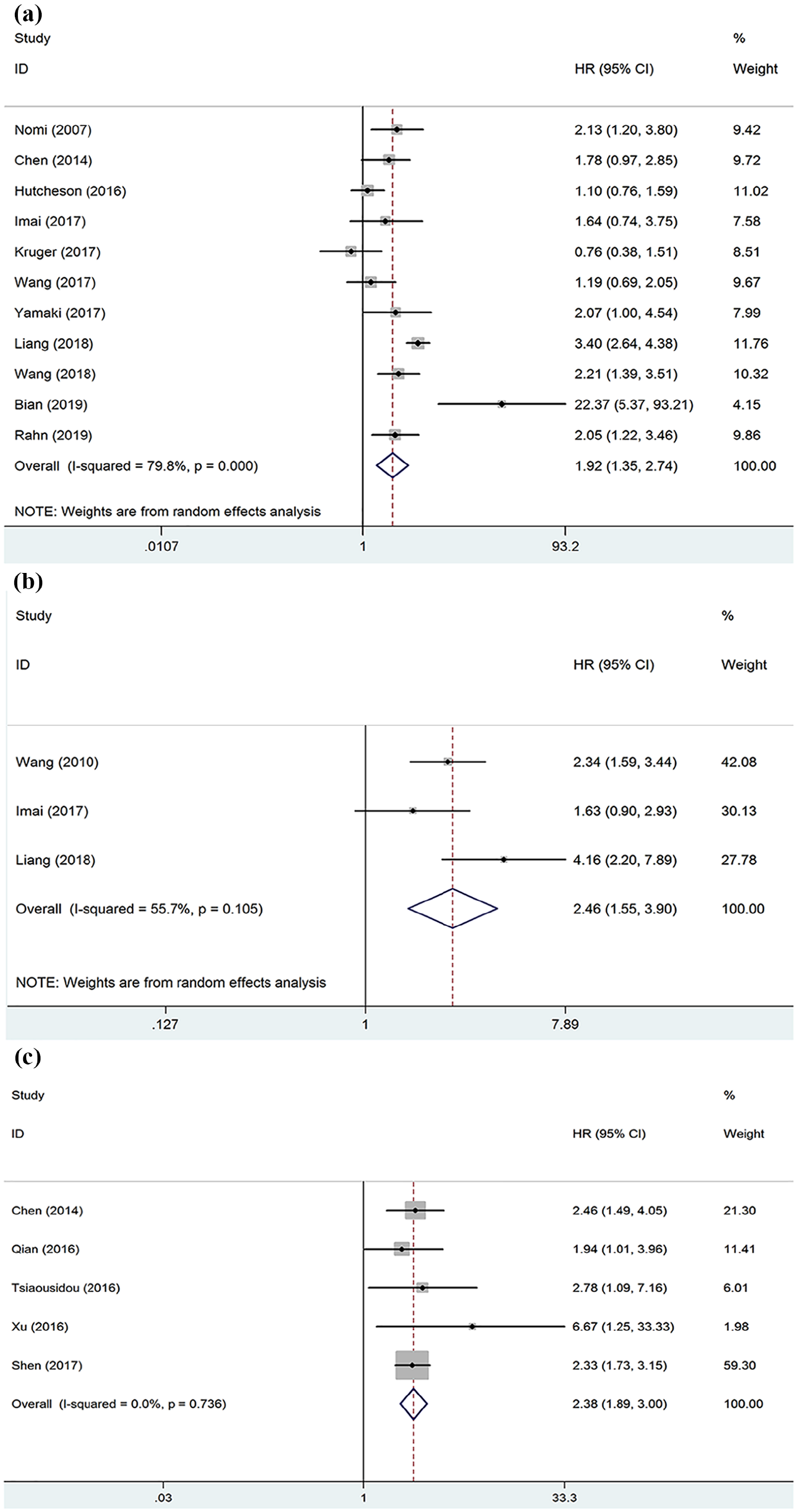
Forest plots showing the hazard ratios of high B7H1 expression in pancreatic cancer for (a) overall survival; (b) cancer-specific survival; (c) overall survival.
A random-effects meta-analysis of three studies (490 patients), which reported the CSS outcomes, showed that the high expression of B7H1 was associated with significantly poor CSS compared to low expression (HR 2.46 (95% CI 1.55, 3.90); P<0.001; Figure 2(b)). Statistical heterogeneity was just over moderate levels (I2=55.7%; P=0.105) in this meta-analysis.
For the evaluation of the relationship between OS and B7H4, we had five studies (375 patients’ data). A meta-analysis of these studies showed that high B7H4 expression was associated with significantly poor OS compared to low expression (HR 2.38 (95% CI 1.89, 3.00); P<0.001; Figure 2(c)). There was no between-studies statistical heterogeneity (P=0.736, I2=0%).
Subgroup and meta-regression analyses
In subgroup analyses, a significant association between B7H1 and OS was observed for trials conducted in China (HR 2.08 (95% CI 1.29, 3.34)), but not in Japan (HR 1.98 (95% CI 1.33, 2.96); Table 2).
Subgroup analysis of B7H1 in overall survival.
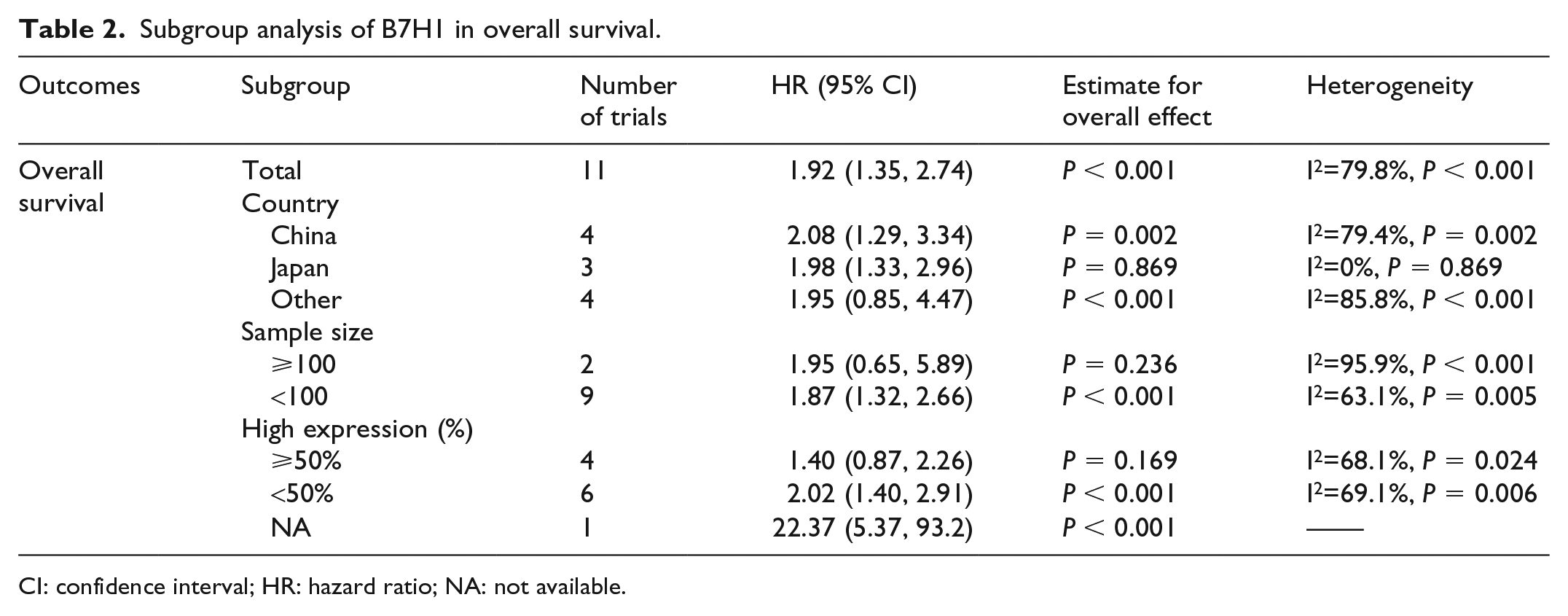
CI: confidence interval; HR: hazard ratio; NA: not available.
The HR of the association between B7H1 and OS in studies with fewer than 100 subjects was 1.87 (95% CI 1.32, 2.66); in studies with more than 100 subjects, the HR was 1.95 (95% CI 0.65, 5.89) (Table 2).
The percentage of patients with high expression B7H1 was significantly associated with OS in studies with <50% patients having high expression (HR: 2.02 (95% CI: 1.40, 2.91)) but not in studies with >50% patients with high expression (HR 1.40, 95% CI 0.87, 2.26) (Table 2).
However, in meta-regression analyses, we found that none of the examined factors, including country (P=0.739), detection method (P=0.723), sample size (P=0.960), and the percentage of patients with high expression (P=0.454), were responsible for heterogeneity across studies.
Sensitivity analysis
Sensitivity analyses were performed by sequentially excluding each of the eligible studies from the analysis. When a study was excluded, the overall statistical significance for the OS–B7H1 relationship (Figure 3(a)) and the OS–B7H4 relationship (Figure 3(b)) did not change, which indicated the reliability of the results.
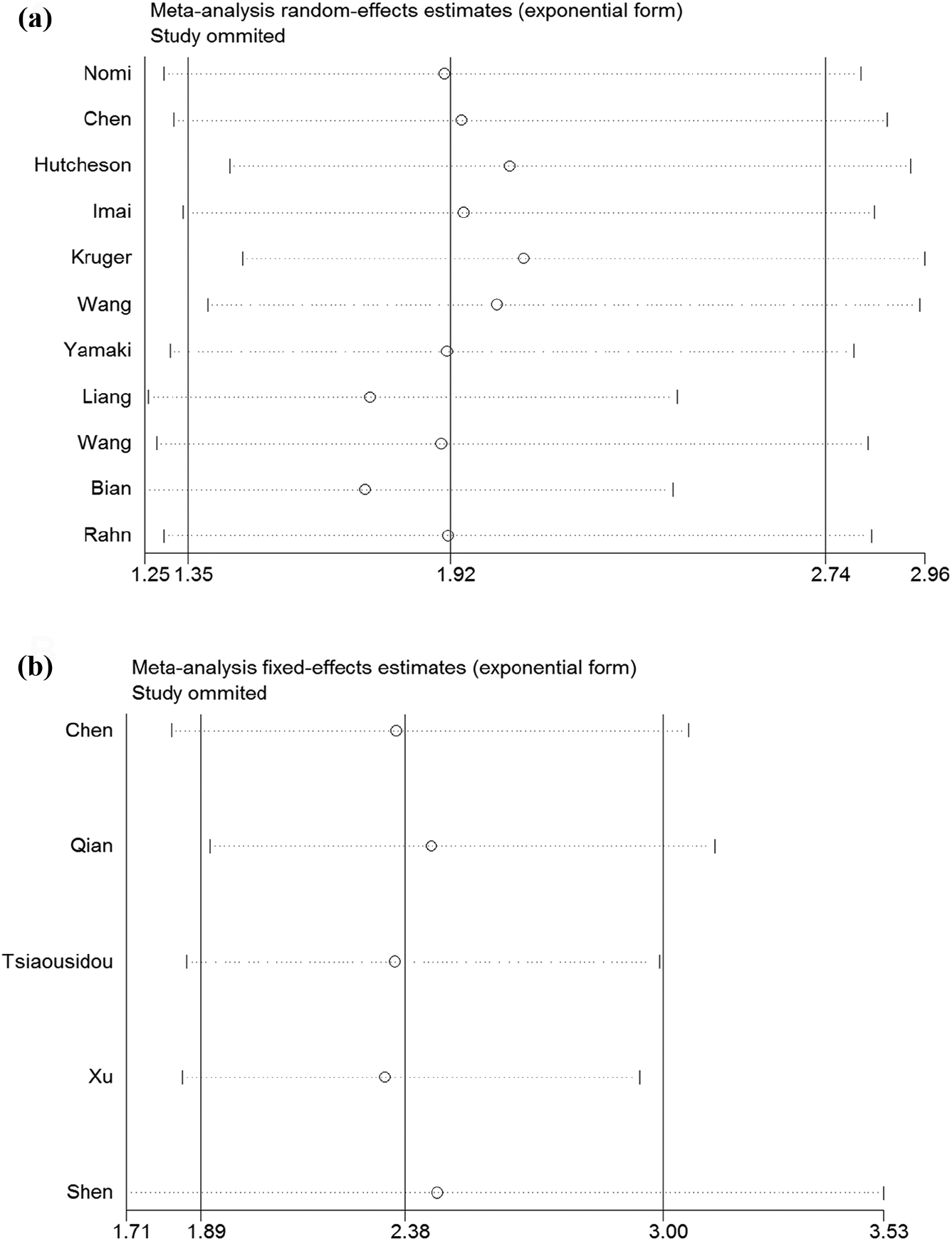
Sensitivity analysis for the meta-analyses. (a) Association of B7H1 with overall survival corresponding to Figure 2(a); and (b) association of B7H4 expression with overall survival corresponding to Figure 2(c).
Publication bias
Visual inspection of the funnel plot was insufficient to decide about the presence of the publication bias. Thus, we performed Begg’s funnel plot and Egger’s test. There was no evidence of the presence of publication bias for either the OS–B7H1 relationship (Begg’s test P=0.876; Egger’s test P=0.596) or the OS–B7H4 relationship (Begg’s test P=0.221; Egger’s test P=0.269) (Supplementary Figure 1(a) and (b)).
Discussion
The clinical manifestations of B7H1 and/or B7H4 expression in PCs is described by several authors, but to date the prognostic association between B7H1 or B7H4 expression with PC is not reviewed and therefore remains inconclusive. We could identify a total of 16 papers comprising 1434 patients for our meta-analysis that have shown that the expression of B7H1 or B7H4 leaves a poor prognosis in PC patients.
B7H1 is an inhibitory checkpoint molecule belonging to the B7 family, which has become a novel target for cancer immunotherapy. 32 B7H1 binds to programmed death protein-1 (PD-1) to produce an inhibitory signal for the cytotoxicity of CD8+ tumor-infiltrating lymphocytes (TILs). 32 The expression pattern of B7H1 is very different from that of B7H4. B7H1 is expressed by some normal cells but B7H4 is rarely expressed by healthy tissues. 33
B7H4 is highly expressed by the majority of human cancers. 34 It has been shown that in PC patients, the expression of B7H1 has an association with tumor size, whereas the expression of B7H4 has associations with tumor size, lymph node metastasis, and depth of invasion. 18 In this meta-analysis, we found that the higher expression of B7H1 or B7H4 was significantly associated with lesser OS. Thus, B7H1 and B7H4 may serve as novel prognostic markers as well as targets for therapeutic intervention for PC.
Heterogeneity is an important factor in interpreting the outcomes of a meta-analysis. 35 In this meta-analysis, both overall and subgroup analyses were statistically heterogeneous, which necessitated the use of a random-effects model. However, meta-regression and subgroup analyses indicated that none of the examined factors—including country, detection method, sample size, and percentage of patients with high expression—were responsible for heterogeneity across studies. Therefore, it is likely that differences in patient characteristics and methodological issues could have played a role in statistical heterogeneity observed herein.
We acknowledge that although we tried to perform a comprehensive analysis, our meta-analysis still has some limitations. First, the number of included studies for some groups was less in subgroup analysis. Second, in study articles where HRs were not reported, we extracted data from the survival curves to calculate HRs, and there can be minor quantitative discrepancies in numerical values to affect the accuracy of the results. Third, the detection of B7H1 and B7H4 expression levels by immunohistochemistry may have interfered with the reliability of overall outcomes.
To our knowledge, this is the first meta-analysis to seek relationships between two important inhibitory checkpoint molecules belonging to the B7-family (B7H1/B7H4) and the prognosis of PC to indicate an association between the expression levels of B7H1 or B7H4 and the survival of PC patients. These findings suggest that B7H4 may be a new target for future tumor immunotherapy.
In a subgroup analysis, we found that the association between B7H1 and OS was statistically significant when the detection method was immunohistochemistry (IHC) for tumoral B7H1 (HR 1.88 (95% CI 1.37, 2.58)) but not when enzyme-linked immunosorbent assay (ELISA) was used for soluble B7H1 (HR 3.88 (95% CI 0.14, 106.59)). Therefore, future studies should have a comparative account of IHC- versus ELISA-measured expressions of B7H1 to seek its association with survival in PC patients.
Supplemental Material
Supplementary_Figure_1 – Supplemental material for The prognostic value of B7H1 and B7H4 expression in pancreatic cancer: A meta-analysis
Supplemental material, Supplementary_Figure_1 for The prognostic value of B7H1 and B7H4 expression in pancreatic cancer: A meta-analysis by Zi-juan Qi, Dan Yu, Chun-hong Chen, Hong Jiang, Ran Li and Yong-ming Kang in The International Journal of Biological Markers
Footnotes
Author contributions
QZJ interpreted the data and wrote the manuscript. YD and CCH analyzed the data; JH and LR collected the data; KYM approved the manuscript. All authors read and agreed the final manuscript. Zi-juan Qi and Dan Yu contributed equally to this study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Research Project of Health Commission of Heilongjinag Province (2014-159).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
