Abstract
To advance the integration of lifestyle medicine into clinical settings, continuing medical education (CME) for practicing clinicians must be designed using evidence-based educational frameworks that align with adult learning principles. This article reviews foundational curriculum development models in medical education, defines instructional approaches, and highlights their core features. Successful implementation of lifestyle medicine interventions into routine clinical practice requires a strategic approach towards CME efforts.
Keywords
“Adult learning theory suggests that adults bring rich life experiences, established knowledge frameworks, and specific motivations to learning situations.”
Background
Lifestyle medicine (LM) addresses the root cause of many chronic diseases and shows promise in reversing America’s worsening non-communicable disease epidemic. As a newly boarded specialty, LM shifts away from traditional allopathic reductionist approaches to patient-centered evidence-based holistic care. The program and evidence are so strong that many health care providers seeking LM certification implement lifestyle changes in their own lives. To successfully apply LM in clinical practice, a health care provider must study and acquire new knowledge and competencies related to the LM specialty. 1 Additionally, they must also implement a new set of validated tools for lifestyle assessments, 2 support patients seeking resources, know how to work together with a health care team, and finally, learn new rules around reimbursement through proper coding and billing. To be effective, LM approaches should be culturally sensitive, focus on social determinates of health (SDOH), and accommodate the influx of digital health in everyday care—all of which add to the complexity of providing LM in the clinical setting.
The American College of Lifestyle Medicine, as well as other organizations, offer live and online continuing medical education (CME) and continuing education (CE)-accredited events to enhance practicing clinician skills in LM. However, a challenge for the CME/CE courses is to meaningfully include LM curricular elements, while ensuring that the educational utility of the course can support clinicians to transfer their knowledge into clinical practice. For those clinicians who want to incorporate LM into their practices, we ask “is there one instructional approach that best facilitates practicing clinicians applying new evidence-based knowledge into everyday clinical practice?”
Medical Education Curriculum Development
The education and training of physicians and clinicians have changed dramatically over the past century with medical education emerging as a complex, transformative process. In the 1970s, Malcolm Knowles amplified education focused on adult learners. 3 Adult learning theory suggests that adults bring rich life experiences, established knowledge frameworks, and specific motivations to learning situations. Thus, clinical education should be geared toward immediate relevance and practical value, with programs explaining why the new material is important and how it connects to adult learners’ existing knowledge and goals.
There are different leading educational frameworks to help ensure adult learning theories are being applied to new curricular programs and support systematic curriculum development and implementation of new material. In medical education, several widely used curriculum design frameworks include Kern’s six-step approach, Four-Dimensional Curriculum Framework (4DF), Understanding by Design (UbD), and the 3P-6C (personal, program, practice) toolkit.4-7 Each of these educational frameworks provide structure, consistency, and adaptability to meet the changing needs of health care providers and are a critical component of CME course design.
Effective Medical Education Instructional Approaches
Instructional approaches are included within each educational framework. They describe the way new material is taught to learners. Historically, medical education instructional approaches consisted of apprenticeships until about 1910, when universities became the home of many medical schools and the famous Flexner report emphasized standardized curricula. 8 Throughout the early 20th century, as courses grew more numerous and specialized, their content became narrower and instructional approaches more didactic. As a consequence, medical education instruction has been primarily lecture-based learning (LBL). 8 LBL approaches can be problematic for learners to process complex material such as LM.
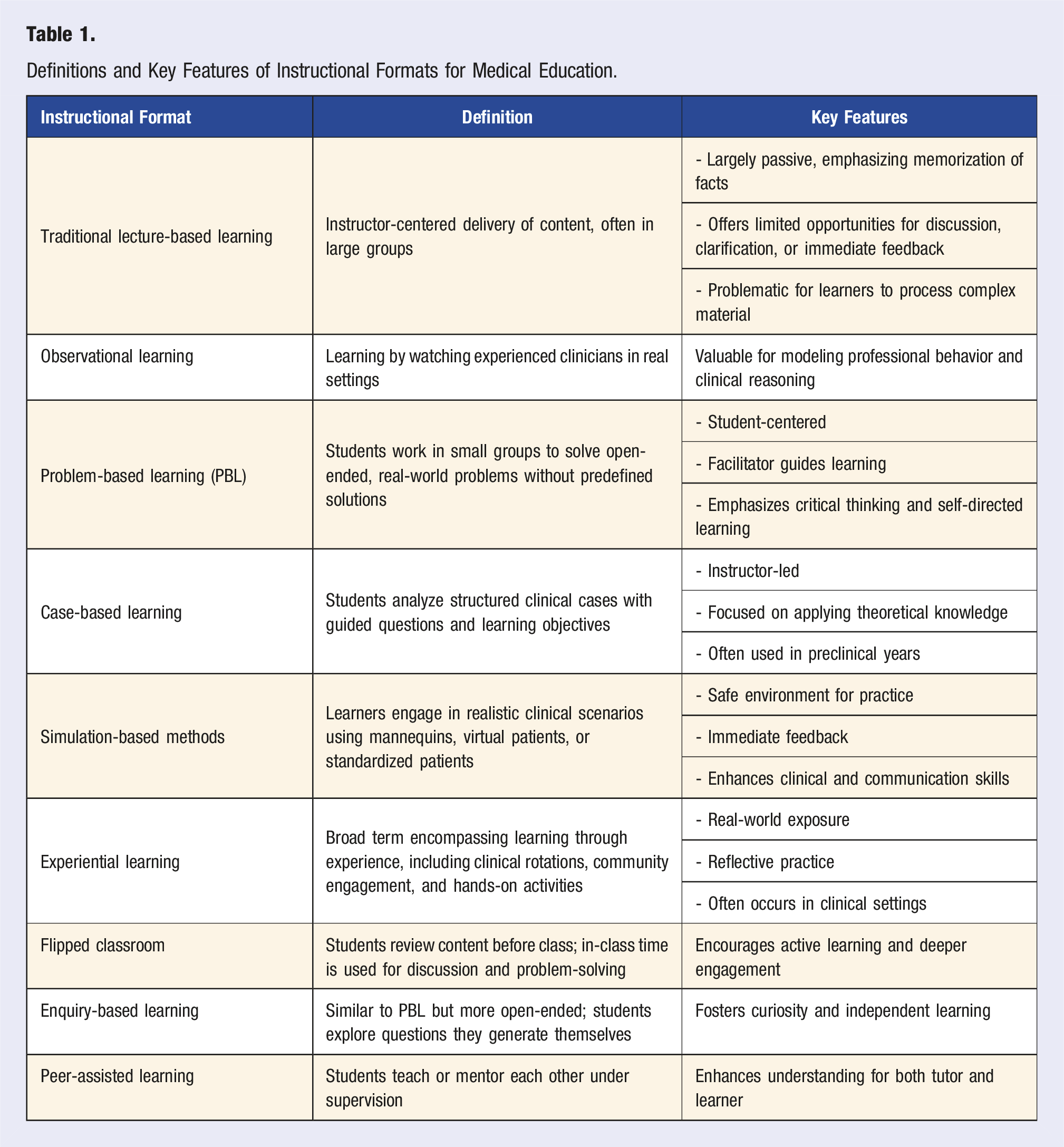
Definitions and Key Features of Instructional Formats for Medical Education.
CME-Accredited Lifestyle Medicine Courses for Practicing Physicians
Several CME/CE curricula exist for physicians and clinicians to gain LM knowledge and skills. These programs vary in their teaching approaches, from online modules to in-person workshops and blended learning formats. Nonetheless, we found that these courses did not appear to have guiding frameworks, lacked reasons for their chosen instructional methods, and have not yet evaluated their impact on actual clinical practice.
We completed a systematic internet search for LM CME courses available in the United States and found a total of 15 accredited courses that build and assess skills in each of the 6 pillars of LM for novice learners who are already out in clinical practice. For the purposes of this article, we highlight courses that are geared toward practicing physicians that currently offer CME credit. We excluded 12 courses either because (1) didactics in all 6 LM pillars were not covered, (2) the course was designed for allied health professionals, (3) the course offered a certificate of completion rather than CME credit, or (4) the course was no longer publicly available or CME credit expired. The courses we include after meeting our inclusion criteria are listed below: (1) “Foundations of Lifestyle Medicine Board Review” is a self-paced, online course offered by the American College of Lifestyle Medicine (ACLM). This course covers foundational knowledge and addresses core competencies in LM. This course was designed by physicians and field experts as a study tool for clinicians preparing to take the American Board of Lifestyle Medicine (ABLM) certification exam. The course features an interactive eBook manual and 10 hours of online review lectures. Participants take 10 quizzes and 10 survey evaluations which correspond with manual sections and lectures to test content comprehension. The Foundation of Lifestyle Medicine Board Review course uses primarily LBL methods. Once certified in LM, maintenance of certification (MOC) requires reviewing 3 pre-selected journal articles by ABLM/ACLM each year and 30 hours of LM-related CME every 5 years. (2) The ACLM Annual CME Conference is an alternative option for novices to be introduced to a variety of topics within LM or for more experienced practitioners to hone or update their knowledge and skills in areas of LM that need strengthening. This 5-day conference allows participants to attend either in-person or online, and all participants can access the conference recordings for a full year. Participants attending in-person workshops can hear about the latest research in LM, work through case studies, and leave with tools that can be applied in real-world settings. Presentations are primarily meant to inform and inspire, while research abstracts provide insights into the latest research supporting LM practice. The CME obtained through the annual meeting counts as the “20-hour event CME prerequisite needed for lifestyle medicine certification.” Additionally, ACLM members can obtain CME/CE credits through ACLM’s online course catalogue and by reading and answering quiz questions about CME-approved articles in the American Journal of Lifestyle Medicine. These options for CME to strengthen one’s knowledge base in LM are important to remain current in the field. (3) “Lifestyle Medicine: Tools for Promoting Healthy Change” is an immersive 2-day course created by Harvard Medical School and the Institute of Lifestyle Medicine (ILM) at Spaulding Rehabilitation Hospital. This course offers over 20 hours of live-streamed presentations on LM topics ranging from weight loss to effective interventions for sleep problems. The program is geared toward new learners to LM. The program includes interactive remote education, features live Q&A sessions with presenters, audience polling, and session recordings which are available to participants after course completion. The course uses evidence-based strategies, tools, and techniques, but it is unclear whether the course uses LBL or CBL instructional formats. Additionally, it is not explicitly stated what framework was used to design the program. (4) “Lifestyle Medicine in Practice” is an online course developed by the American Academy of Family Physicians (AAFP). Participants are given access to pre-recorded sessions with faculty and can study at their own pace and complete “Translation to Practice” exercises following course completion for additional credit. “Translation to Practice” exercises are designed to help learners apply concepts from the course to their clinical practice, enhancing the patient care they provide. Despite having this application component, the AAFP course is taught using primarily LBL methods with few interactive components.
Conclusion
LM is a new specialty with core competencies that promise to have a large impact on the health of many patients in the United States. However, due to the complexity of its holistic approach to patient care, inclusion in one’s personal life, and the coordination with other members on the care team, LM CME/CE educational efforts need to be grounded in proven educational frameworks and apply instructional approaches that meet adult learning needs. Greater efforts are needed to ensure that current LM CME courses consistently incorporate proven educational frameworks and instructional methods that support adult learning. A strategic educational approach—one that integrates knowledge acquisition, experiential learning, and system-level support—is essential for the successful implementation of lifestyle medicine in clinical practice.
Footnotes
Author Contributions
EMG developed the concept, drafted the manuscript, and led the review and editing process as the primary author. EK conducted a systematic search of publicly available CME-accredited lifestyle medicine courses available in the United States and contributed to drafting the manuscript. BF conducted manuscript review and editing and provided overall guidance.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
