Abstract
This study from a national sample of Gulf War Veterans (N = 1098) examined the association between physical activity level and (a) past-year suicidal ideation and (b) risk for suicidal behavior as defined by a score of
“Being physically active was associated with lower odds of reporting past-year suicidal ideation, as well as lower odds of being classified as high risk for suicidal behavior.”
Suicide rates continue to increase among United States military veterans. 1 The unadjusted suicide rate for veterans in 2001 was 23.3 per 100,000 people and rose to 33.9 per 100,000 in 2021. In comparison, among non-veterans, the suicide rate was 12.6 per 100,000 in 2001 and rose to 16.7 per 100,000 in 2021. 1 Veterans are at an elevated risk for suicidal behavior compared to the general population, in part because of higher rates of established risk factors,2-7 such as posttraumatic stress disorder (PTSD) and depression,8,9 substance use disorders,10,11 nonsuicidal self-injury12,13 and chronic pain 14 are also prevalent in veterans and are associated with elevated suicidal ideation.
Suicide prevention remains a top priority for Veterans Affairs (VA) and the Veterans Health Administration (VHA), which has expanded access to evidenced-based interventions for depression and suicidal ideation. 1 The VHA has developed a suicide prediction statistical model based on electronic health record data and has implemented a clinical program known as Recovery Engagement and Coordination for Health-Veterans Enhanced Treatment (REACH VET), which is designed to engage high-risk veterans in treatment. 15 Additionally, the VHA has increased access to several evidenced-based interventions for depression which have been shown to effectively decrease suicidal ideation. 16 These interventions are critically necessary and save lives, although they are limited by a sole focus on only those at highest risk for suicide. Nearly 40% of veterans who died by suicide in 2021 did not have a mental health or substance use disorder diagnosis. 1 A focus on broader health factors may improve intervention efforts. Therefore, identifying additional modifiable factors that could reduce suicidal ideation remains an important research priority. 17
Health behaviors, such as exercise, may be important for reducing suicidal ideation in veterans. 17 Exercise and physical activity have been associated with lower levels of depression in cross-sectional studies and experimental studies18,19 and there is preliminary evidence suggesting exercise may also reduce PTSD symptoms in veterans. 20 A recent systematic review and meta-analysis examining the relationship between physical activity and suicidal ideation found that people who are active (i.e., engaged in at least 150 minutes per week of moderate physical activity or at least 75 minutes per week of vigorous physical activity) had lower suicidal ideation in both adolescents and adults. 21 Research examining the association between physical activity in veterans, however, is limited and has produced mixed findings. In a study of veterans with PTSD (N = 346), performing exercise in the past month, operationalized as engaging in activity to “work up a sweat” at least once in the past month, was lower among those endorsing suicidal ideation than veterans without suicidal ideation. 18 In another broad sample of veterans seeking VHA care (N = 103), 22 there was no significant association between past week physical activity (i.e., metabolic equivalent of task (MET) minutes in the past week) and suicidal ideation. Hence, additional research is necessary to further clarify the relation between physical activity level (i.e., active versus less than active) and suicidal ideation among veterans.
The present study examined the cross-sectional association between physical activity level and suicidal ideation and risk for suicidal behavior in veterans who served during the first Gulf War. It was hypothesized that “active” activity level would be inversely related to suicidal ideation and suicide risk and would remain statistically significant, independent of established predictors of suicide including diagnoses of depression, PTSD, substance or alcohol use disorder, pain, and nonsuicidal self-injury.3,7,10,12,23,24
Method
Participants and Procedures
Data for this study came from a large national survey investigating the healthcare needs of Gulf War Era veterans (Gulf War Research and Individual Testimony: Grant I01HX001682). The survey was conducted January 2019 to August 2020 and was administered to a national cohort of deployed Gulf War and non-deployed Gulf War Era Veterans. Potential participants were first identified through a VA administrative database to include both users and non-users of VA healthcare. Potential responders were identified based on a history of military service during the Gulf War, regardless of whether they deployed, resulting in an initial cohort of 1,098,991 Gulf War Era veterans. Participants were then categorized into 8 geographic regions to provide nationwide representation. For a more detailed description of all study information and recruitment procedures see Blakey et al. (2021). 25 A total of 1153 veterans completed and returned the survey, resulting in a response rate of 42.33% (1153 out of 2724). Study procedures were approved by the Durham VA Medical Center Institutional Review Board and the Salt Lake city VA Medical Center Institutional Review board. The final sample used in the present analyses included 1098 veterans with non-missing data on physical activity and suicide items. The associations between suicidal ideation and PTSD, cannabis use, and pain have previously been described for this sample (Grove et al., 2023). 10
Measures
Sociodemographic information
Participants self-reported their age, biological sex (male = 0; female = 1), race (recoded to Black, White, or Other), income (dichotomized as household income of < $75,000 versus
Physical Activity
Eight items from the Rapid Assessment of Physical Activity (RAPA) 26 were used to assess physical activity levels (i.e., light, moderate, and vigorous). The RAPA is a well-validated self-report assessment of typical participation in light, moderate, and vigorous physical activities. 27 The RAPA has been previously used to assess physical activity in a large-scale cohort of Veterans. 28 The RAPA instrument defines each level of physical exercise in terms of physiological changes and example activities. “Light” activities are defined as activities where the heart beats slightly faster than normal, but you can still talk and sing and provides examples such as walking leisurely or stretching. “Moderate” activities are defined as activities where the heart beats faster than normal and you can talk and not sing with examples such as fast walking, aerobics class, and strength training. “Vigorous” activities are defined as activities where the heart rate increase a lot and large breaths are taken between talking with examples such as running, jogging, stair machine, and tennis. The RAPA asks respondents to answer items with “yes” or “no” responses based on “typical” level of activity rather than a set time frame (e.g., “I do moderate physical activities every week, but less than 30 minutes a day or 5 days a week”). Activity levels were dichotomized according to validated scoring as “active” (coded as 1) if a respondent engaged in 1) 30 minutes or more a day of moderate physical activities for 5 or more days a week, or 2) if they engaged in 20 minutes or more a day of vigorous physical activities for 3 or more days a week. 26 All other respondents were coded as 0 (less than active).
Suicide Risk
The Suicidal Behaviors Questionnaire-Revised (SBQ-R) 29 is a 4-item measure that assesses risk for suicide as a combination of past ideation and planning, prior suicide attempts, and likelihood of future attempts. Higher total score indicates greater overall risk of suicidal behavior. The recommended cutoff score indicating high-risk status is ≥7. 29 Individuals who met or exceeded this cutoff were coded as 1 (i.e., high risk), all others were coded as 0 (i.e., low risk). A single item from the SBQ-R was used to assess past-year suicidal ideation (i.e., “How often have you thought about killing yourself in the past year?”) using a Likert scale from 1 (never) to 5 (very often). Any past-year suicidal ideation was dichotomized as any (coded as 1) vs none (coded as 0).
NSSI
Past-year NSSI was assessed with the Screen for Nonsuicidal Self-Injury, 30 a brief 10-item screen designed to identify individuals currently engaging in NSSI. Participants were presented with a definition of NSSI before being asked to indicate whether they had engaged in 10 forms of NSSI (e.g., cutting, burning, scratching, self-mutilation) using a yes/no response format. Participants were coded as having past-year NSSI if they endorsed engaging in any of these behaviors in the past year.
Psychosocial Functioning
The Brief Inventory of Psychosocial Functioning (BIPF) 31 is a 7-item self-report measure of past-30-day psychosocial functioning. Items are scored on a scale of 0 (never) to 6 (always). A scoring algorithm excluding items marked as “not applicable” yields a total score ranging 0 to 100, with higher scores indicating poorer psychosocial functioning. 31
Combat Exposure
Combat exposure was assessed with Critical Warzone Experiences (CWE) questionnaire. 32 A score of greater than 0 was used to define lifetime exposure to any combat experiences.
Self-Rated Health and Weight
Self-rated health was assessed with a single item from the SF-36, 33 “In general, would you say your health is poor, fair, good, very good, or excellent?” Self-rated health was dichotomized as good/very good/excellent (coded as 0) vs fair/poor (coded as 1). Self-reported weight was assessed with a single item, “In thinking about your weight class, do you consider yourself to be: overweight, about the right weight, or underweight?” Weight was dichotomized as overweight (coded as 1) vs about the right weight/underweight
Pain
A 3-Item Scale Assessing Pain Intensity and Interference with Life (PEG) 34 was used to assess pain in the “past week.” Pain levels were dichotomized to indicate the presence of moderate or severe pain (coded as 1) vs mild or no pain (coded as 0).
Cannabis Use
A two-item measure was used to assess past year cannabis use, “in the past 12 months, have you used marijuana/cannabis as prescribed” and “in the past 12 months, have you used marijuana/cannabis recreationally” with responses of yes or no. A response of yes for either of the 2 items was coded as positive for past year cannabis use, if both responses were no then cannabis use was coded as negative.
Psychiatric Diagnoses
Veterans indicated whether they had ever been diagnosed with common medical and psychiatric diagnoses including Gulf War Illness, depression, PTSD, and alcohol or substance use disorder. These responses were dichotomized as either having a lifetime diagnosis of the specific condition (coded as 1) or no history of having been diagnosed with the specific condition (coded as 0).
Data Analysis Plan
Chi-square tests of independence were used to examine the bivariate associations between physical activity levels (i.e., “active” and “less than active”) and demographic and clinical variables. Logistic regression was used to examine the bivariate and adjusted associations between physical activity, other known clinical risk variables, demographics, and past-year suicidal ideation (Model 1) and between physical activity, covariates, and suicidal behavior risk status (i.e., high risk determined by the SBQ-R; (Model 2). Multiple imputation was used to impute any missing data on covariates. All analyses were conducted in SAS version 9.4 (SAS Institute, Inc, 2023).
Results
Demographic and Clinical Associations With Activity Level.
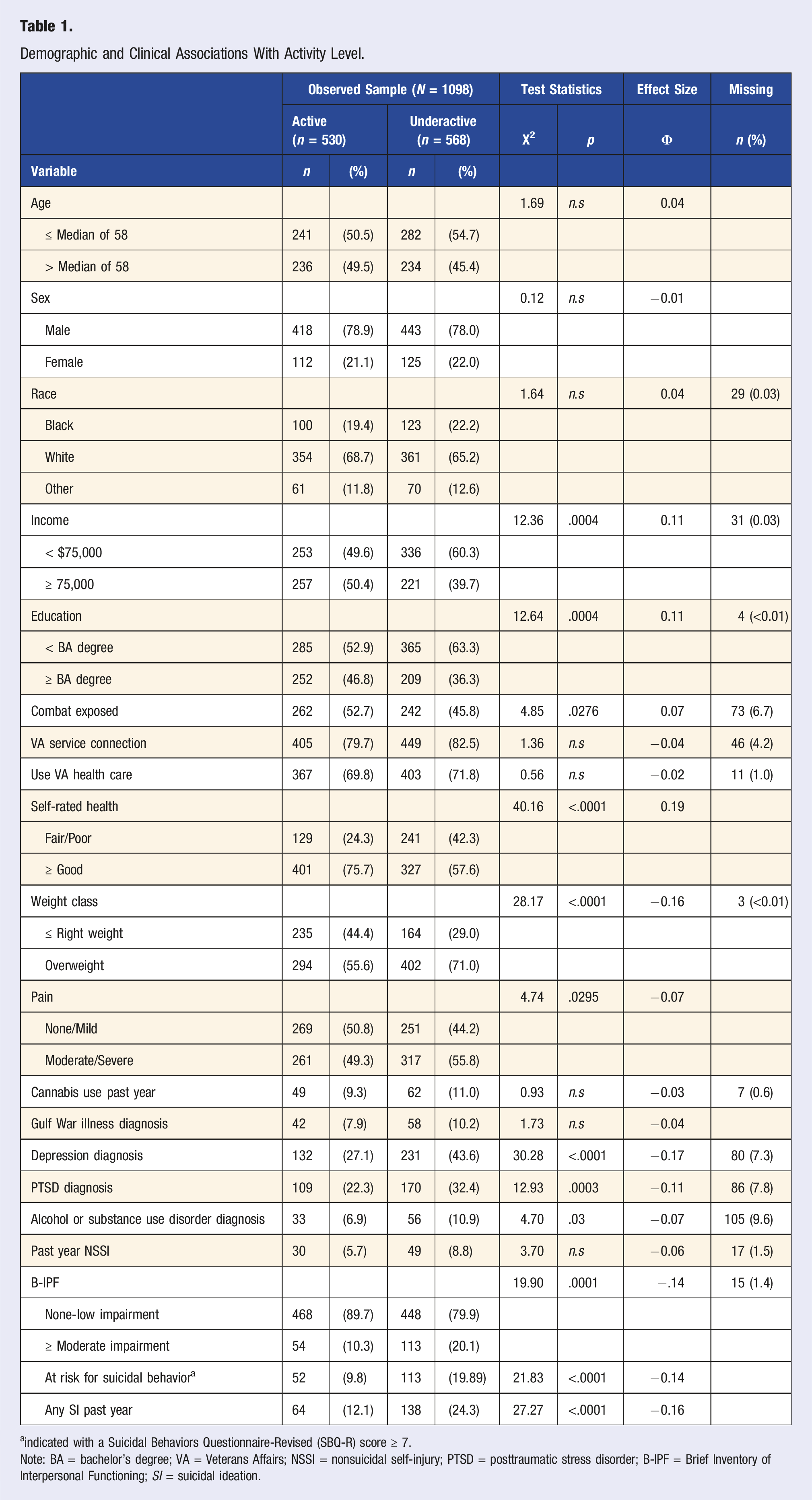
aindicated with a Suicidal Behaviors Questionnaire-Revised (SBQ-R) score ≥ 7.
Note: BA = bachelor’s degree; VA = Veterans Affairs; NSSI = nonsuicidal self-injury; PTSD = posttraumatic stress disorder; B-IPF = Brief Inventory of Interpersonal Functioning; SI = suicidal ideation.
Unadjusted and Adjusted Associations With Any Past-Year Suicidal Ideation.
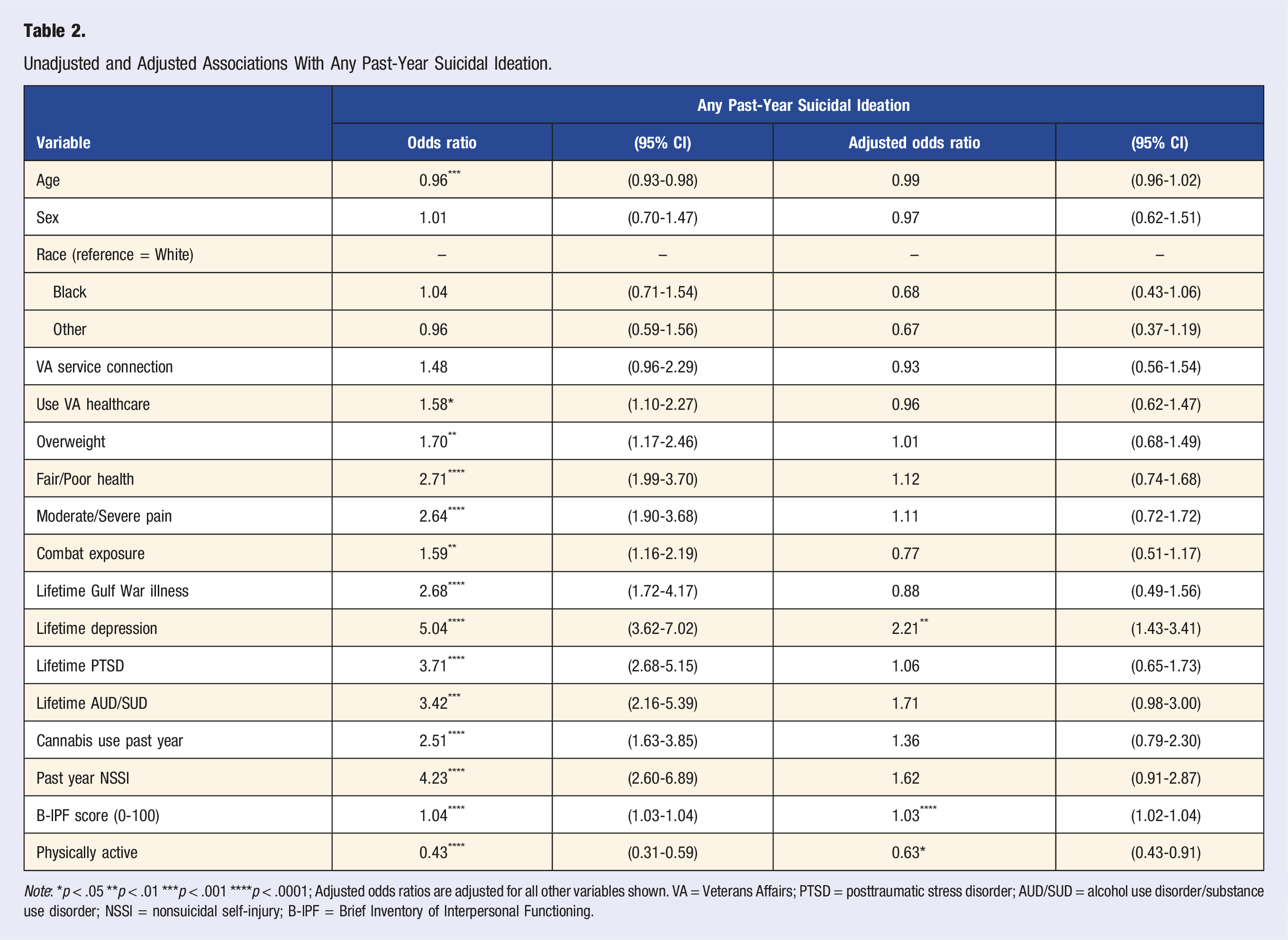
Note: *p < .05 **p < .01 ***p < .001 ****p < .0001; Adjusted odds ratios are adjusted for all other variables shown. VA = Veterans Affairs; PTSD = posttraumatic stress disorder; AUD/SUD = alcohol use disorder/substance use disorder; NSSI = nonsuicidal self-injury; B-IPF = Brief Inventory of Interpersonal Functioning.
Unadjusted and Adjusted Associations With High Risk for Suicidal Behavior.
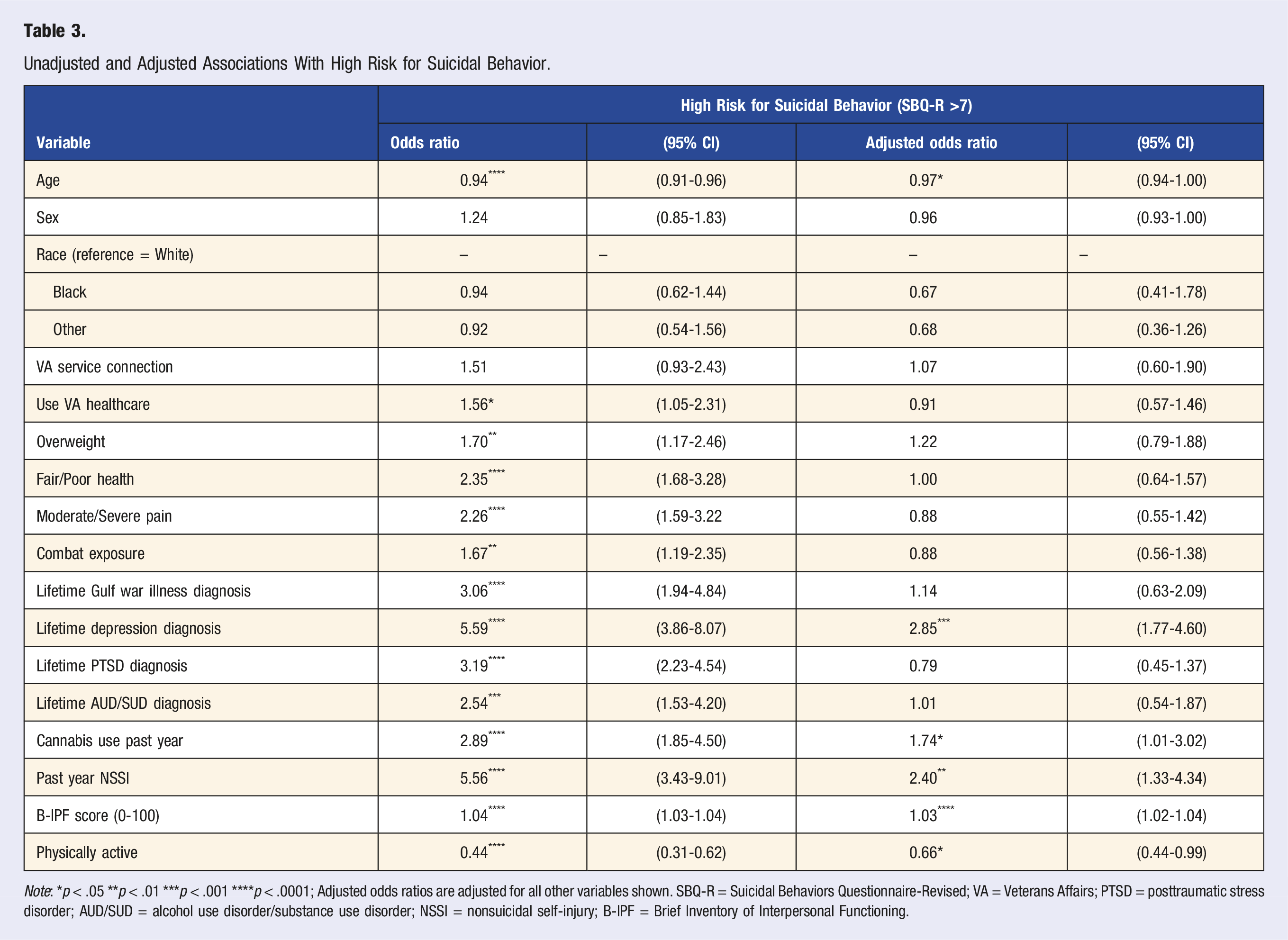
Note: *p < .05 **p < .01 ***p < .001 ****p < .0001; Adjusted odds ratios are adjusted for all other variables shown. SBQ-R = Suicidal Behaviors Questionnaire-Revised; VA = Veterans Affairs; PTSD = posttraumatic stress disorder; AUD/SUD = alcohol use disorder/substance use disorder; NSSI = nonsuicidal self-injury; B-IPF = Brief Inventory of Interpersonal Functioning.
Discussion
Physical activity is known to be related to suicidal ideation in non-veterans 21 but studies examining veterans have provided mixed results.18,22 Results of the current study indicate associations with physical activity and suicidal ideation and high risk for suicidal behavior in a large sample of veterans who served during the first Gulf War in 1990-1991. Even after adjusting for established risk factors for suicide including depression, PTSD, nonsuicidal self-injury, and current levels of psychosocial functioning, being physically active was associated with lower odds of reporting past-year suicidal ideation, as well as lower odds of being classified as high risk for suicidal behavior.
The difference between the present study’s findings and the mixed results from prior work on this topic may be explained by the timeframe for assessing these variables. The present study assessed “typical” levels of physical activity (i.e., “active” and “less than active”), and the presence of suicidal ideation was assessed over the past year. Suicide risk was based on a both lifetime and past year events. In contrast, Gutierrez and colleagues 22 assessed suicidal ideation in the past month and exercise habits in the past week and did not find evidence for a significant relationship. Davidson and colleagues 18 assessed present suicidal ideation and exercise habits over the past month and did find a significant inverse relationship between physical activity and suicidal ideation. Given that the proposed benefits of exercise on mental health are neurobiological (e.g., modulates levels of dopamine and serotonin, release of endocannabinoids), 35 it may be that exercise habits need to be sustained for a reasonable amount of time before conferring benefits on mental health.
Consistent with previous work, 18 physical activity was related to depression and PTSD where those who were physically active were less likely to report a diagnosis of depression or PTSD. The mechanisms between physical activity and psychiatric distress are not well understood. Proposed mechanisms include neuroendocrine and inflammatory responses to activity which may result in long-term adaptations including changes to neural architecture 36 as well as acute activation of the endocannabinoid system (e.g., “runner’s high”). 37 Proposed psychosocial mechanisms include more social interaction and social support and improved physical self-perceptions including higher self-esteem and self-efficacy. 36
Results also demonstrated associations between physical activity levels and social determinants of health. Veterans with higher household income and education were more likely to be sufficiently physically active, compared to those from lower income and educational backgrounds. Although there may be promise in implementing exercise interventions as a method to protect against both psychiatric distress and suicidal ideation, attention should be paid to factors associated with social determinants of health that may moderate response. For example, neighborhood deprivation might attenuate treatment effects. 38 A meta-analysis of interventions to increase health behaviors in persons from low-income populations found a small but statistically significant improvement in physical activity post-intervention, however, the effect was not evident at follow-up. 39 Future studies should consider the impact of social determinants of health on interventions to increase physical activity levels in veterans.
The cross-sectional design of the current study precludes any conclusions about causality. The majority of studies demonstrating the association between physical activity and suicidal ideation have been cross-sectional. There is a clear need for additional prospective studies to examine this association as well as interventional studies that examine the impact of increasing activity levels in veterans on distress and suicidal ideation risk. Because the survey included select items from the RAPA, we could only compare active individuals to those that were less than active. We are unable to evaluate the impact of other self-reported doses of activity. Self-reported physical activity rather than an objective measure also limits the study design. In a recent meta-analysis examining the association between physical activity and risk of depression, Pearce and colleagues 40 found that those who accumulated just half the recommended volume of physical activity had 18% lower risk of depression compared to those that reported no activity. Assessing the impact of dose of activity on suicidal ideation may be a promising area for future studies. Another limitation to consider is the reliance on self-report data and inability to assess response bias. It is possible that non-content responding, overreporting, and underreporting may influence the current findings. Additionally, participants were asked to self-report diagnoses and future work should seek to include confirmed diagnoses. Finally, 80% of participants in the present study were service-connected which may indicate that participants were, on average, experiencing poorer mental health and more impaired psychosocial functioning. 41
Despite these limitations, there are several noteworthy strengths of the current study. First, the sample was a large, national sample of Gulf War veterans that oversampled female veterans and represents the largest study to date that has examined the association between physical activity level and suicidal ideation in veterans. Notably, Gulf War Era veterans represent the largest cohort of US veterans and make up over one-quarter of veterans enrolled in VA healthcare, underscoring the generalizability of study findings.42,43 The analytic plan examined the unique association between physical activity and suicidal ideation and risk while adjusting for a host of other known risk factors including depression, PTSD, substance use disorders, nonsuicidal self-injury, and current psychosocial functioning. Results are consistent with findings in civilian populations, that indicate physical activity may be an important modifiable predictor of suicide risk. Findings will hopefully inform future studies examining the impact of physical activity on risk of suicide in veterans.
Footnotes
Author Contributions
E. McRae Calhoun (conceptualization, formal analysis, methodology, writing—original draft preparation); Jack D. Wiese (conceptualization, formal analysis, methodology, writing—original draft preparation); Samantha J. Meckes (writing—reviewing and editing); Jeremy L. Grove( writing—reviewing and editing), Kirsten Dillon (writing—reviewing and editing), Mary J. Pugh (funding acquisition, investigation, methodology, project administration, resources, writing—reviewing and editing); Nathan A. Kimbrel (funding acquisition, investigation, methodology, project administration, resources, writing—reviewing and editing); Tate Halverson (writing—original draft preparation, supervision).
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs or the United States government. The authors have no conflicts of interest to report.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by grant I01HX001682 from VA ORD HSR&D awarded to Drs. Kimbrel and Pugh. This work was supported by the Department of Veterans Affairs, Veterans Health Administration, Office of Academic Affiliations VA Quality Scholars Advanced Fellowship Program. Program Award Number 3Q042019C. Dr Halverson was supported by a Career Development Award from VA RR&D (IKRX004803). Dr Dillon was supported by a Career Development Award from VA RR&D (IKRX002965). Dr Grove was funded by NIH NIAAA Career Development Award (K23AA031035). Dr Pugh was supported by a Research Career Scientist Award from VA HSR&D (IK6HX003762). Dr Kimbrel was supported by a Research Career Scientist Award from VA BLR&D (IK6BX006523).
Ethical Statement
Data Availability Statement
The data that support the findings of this article are available upon reasonable request from the authors.
