Abstract
“Factors such as poor sleep quality, lack of exercise, and the psychological stress associated with fear of relapse can weaken the body and overall well-being.”
Objective
Breast cancer is the most diagnosed cancer in women worldwide.1,2 As mortality rates decrease, the number of breast cancer survivors (BCS) is steadily rising. However, many survivors experience long-term effects from the disease or its treatment, including low estrogen levels, an increased risk of cardiovascular disease, impaired cognitive function, reduced bone density, chronic pain, and lymphedema. These factors can significantly reduce their quality of life. 3 Importantly, some of these effects, such as lymphedema, may be mitigated through lifestyle modifications, including a balanced diet. Given this, there is a growing international interest in lifestyle interventions to support BCS.
Lifestyle medicine offers a promising non-pharmacological approach to improving the quality of life in BCS. It encompasses several key areas, such as physical activity, nutrition, stress management, sleep hygiene, smoking cessation, alcohol reduction, social support, and restorative sleep. 4 Research shows that one year after treatment, BCS often report significantly lower scores in emotional well-being, social functioning, fatigue, insomnia, and body image. Therefore, considering the long-term effects of breast cancer and its treatments, lifestyle medicine can be an effective intervention for enhancing survivors’ quality of life.3,5 Quantitative studies have shown that moderate physical exercise can reduce the risk of breast cancer recurrence by up to 40%. 6 A meta-analysis using a random-effects model found that a higher-quality diet was associated with a 23% reduction in all-cause mortality among BCS. 7 Additionally, cognitive-behavioral therapy has been shown to help BCS manage chronic insomnia. 8 However, alcohol intake remains a significant risk factor, with an analysis of four cohort studies showing a 28% increase in the risk of late recurrence (>5 years after diagnosis) among BCS who consumed alcohol. 9
This systematic review aims to evaluate the health behavior outcomes of lifestyle medicine interventions in breast cancer survivors.
Methods
Search Strategy
We conducted a comprehensive search across five online databases: PubMed, Embase, BMC, Sage Journals, Korea Science and Google Scholar. Our goal was to identify scientific studies examining the impact of lifestyle medicine on breast cancer survivors. Additionally, we retrieved one relevant study from secondary resources. 10
Search Terms and Number of Results Retrieved.
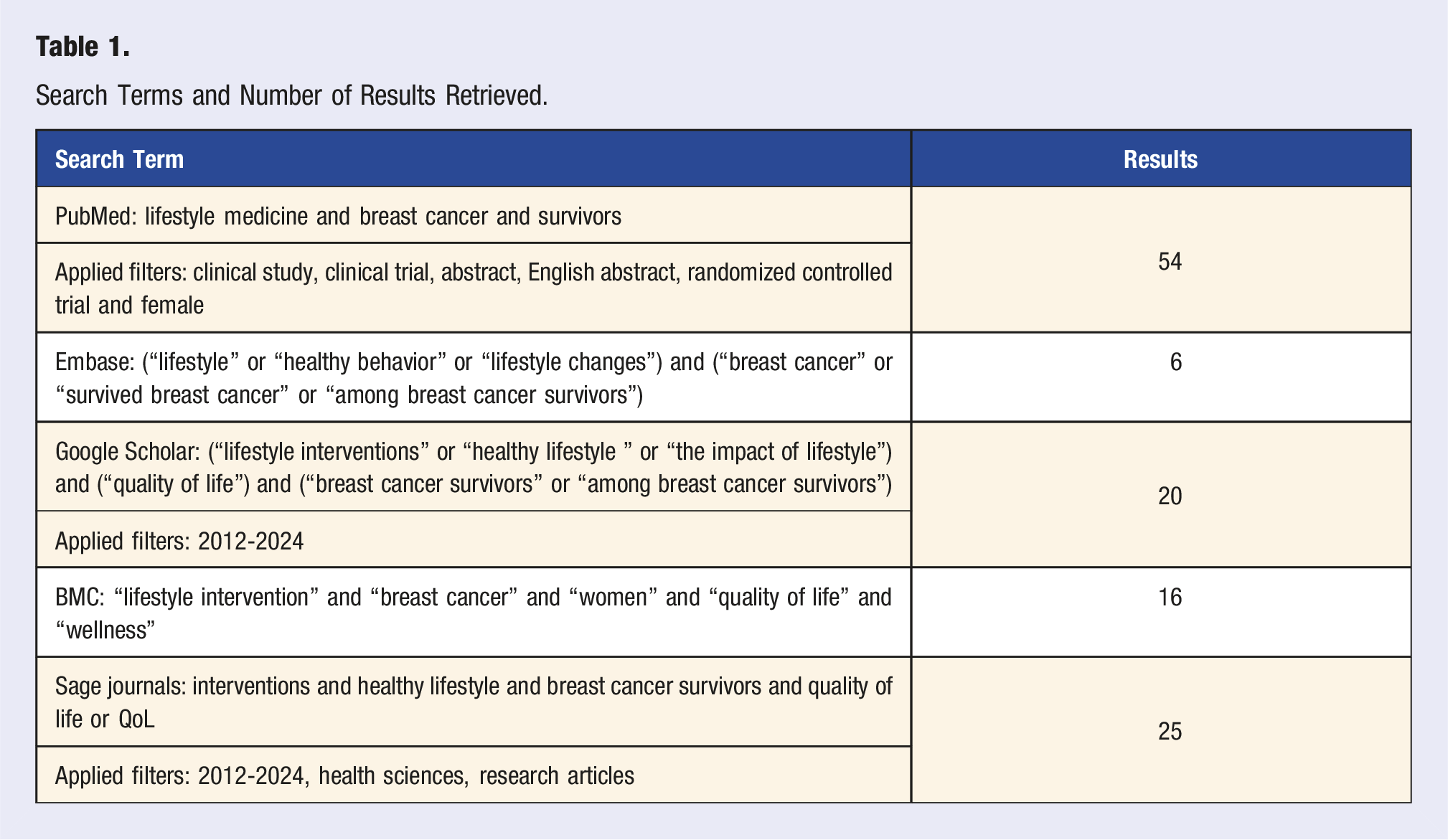
All searches were conducted between March 2024 and July 4, 2024. The search across the aforementioned databases yielded 60 articles from formal literature and 62 from gray literature, covering publications dated between September 30, 2012, and July 4, 2024.
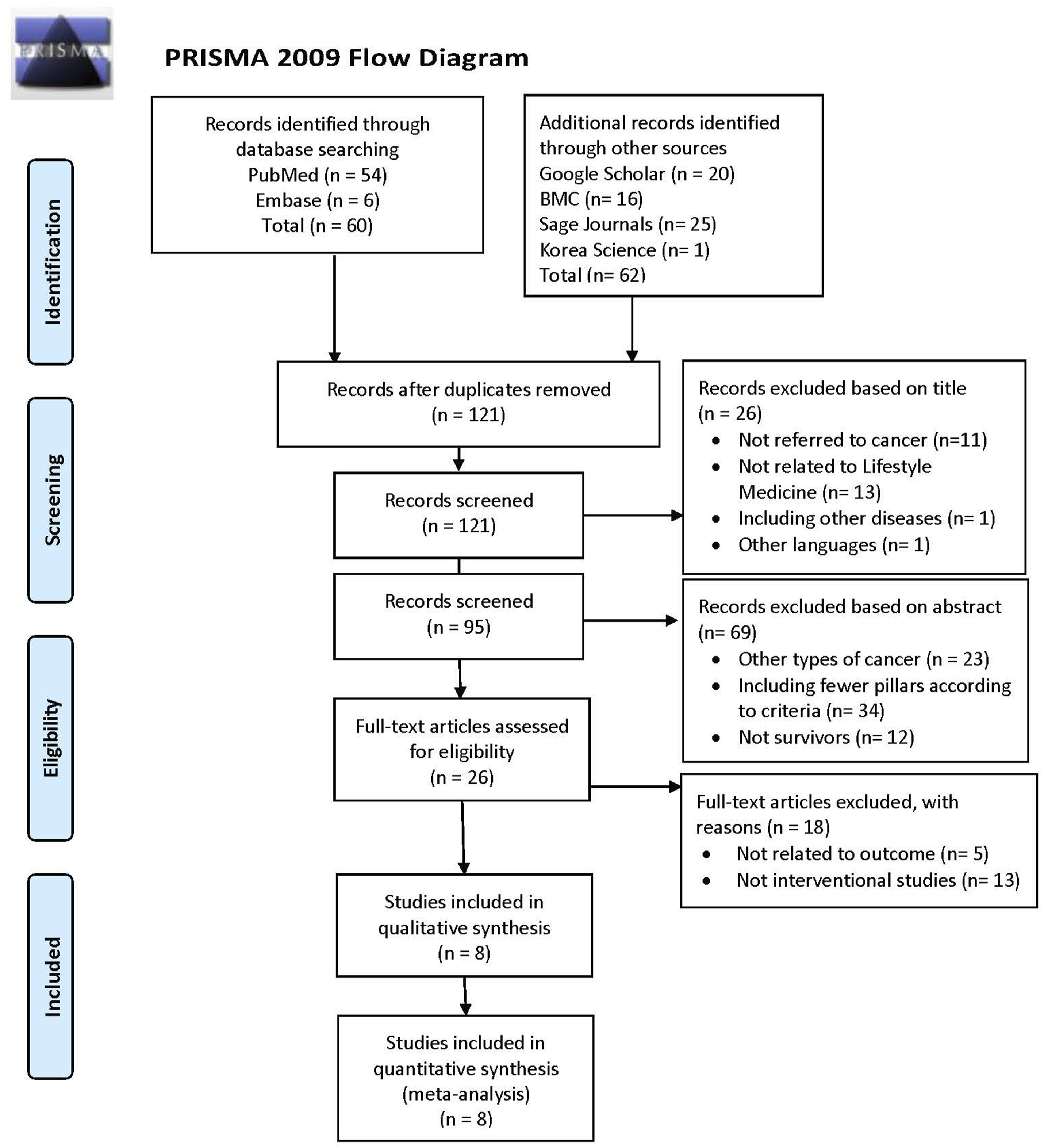
The following procedure was used to evaluate the articles: 1. Duplication Check: After removing duplicates, 121 unique articles remained. 2. Title and Abstract Screening: The titles and abstracts of the 121 articles were reviewed, leading to the exclusion of 95 articles that did not meet the inclusion criteria (as outlined in Figure 1). 3. Full-Text Screening: The remaining 26 articles underwent thorough screening to confirm their eligibility. Following this detailed review, 8 articles were retained for the systematic review, based on the criteria presented in the flow chart. PRISMA-2009-flow-diagram.
Inclusion Criteria
The following inclusion criteria were applied during the first and second screenings of the articles: 1. Language: Articles published in English. 2. Study Population: Women who have survived breast cancer, not women currently undergoing treatment for breast cancer. 3. Chemotherapy Status: Participants must have completed chemotherapy, whether immediately prior to the intervention or at any point months or years before. 4. Intervention Type: Studies focused specifically on lifestyle interventions, excluding other forms of intervention. 5. Outcome Measures: Studies reporting both qualitative and quantitative outcomes.
The following exclusion criteria were applied during the first and second screenings of the articles: 1. Document Types: Conference papers, narrative reviews, textbook chapters, and editorials. 2. Scope of Lifestyle Medicine: Studies addressing only 1 or 2 pillars of lifestyle medicine; the inclusion requirement was interventions involving at least 3 pillars. 3. Study Population: Women currently undergoing chemotherapy. 4. Cancer Types: Studies focused on cancers other than breast cancer, or those that did not specifically mention breast cancer survivors (BCS). 5. Comorbidities: Studies including other diseases or comorbidities unrelated to breast cancer.
For the third screening, the following inclusion criteria were applied:
Data Synthesis
Given the heterogeneity of the included studies in terms of intervention type, outcome measures, and study design, we employed a narrative synthesis approach following the guidelines of Popay et al. 32 This approach allows for a structured textual summary of findings when a meta-analysis is not feasible due to variations in methodology.
Studies were grouped based on the number of lifestyle medicine pillars they addressed (3-6 pillars), and findings were synthesized within these categories to ensure coherence in interpretation. Additionally, we considered the methodological quality of each study in our synthesis, giving greater weight to high-quality randomized controlled trials (RCTs) while acknowledging the contributions of medium- and low-quality studies.
To enhance transparency, we have reported key themes, patterns, and differences across studies, while also discussing the potential impact of study heterogeneity on our conclusions.
Study Design
Randomized controlled trials (RCTs) or quasi-experimental designs, with or without a control group.
Focus
Studies related to health outcomes or improvements in quality of life.
Results
Included Studies
The results of the review process are illustrated in Figure 1. The searches conducted in PubMed and Embase returned a total of 4 articles. An additional 4 articles were identified through secondary resources, resulting in a total of 8 articles assessed in this review.
Study Characteristics
Characteristics of Included Studies on Lifestyle Medicine Interventions in Breast Cancer Survivors.
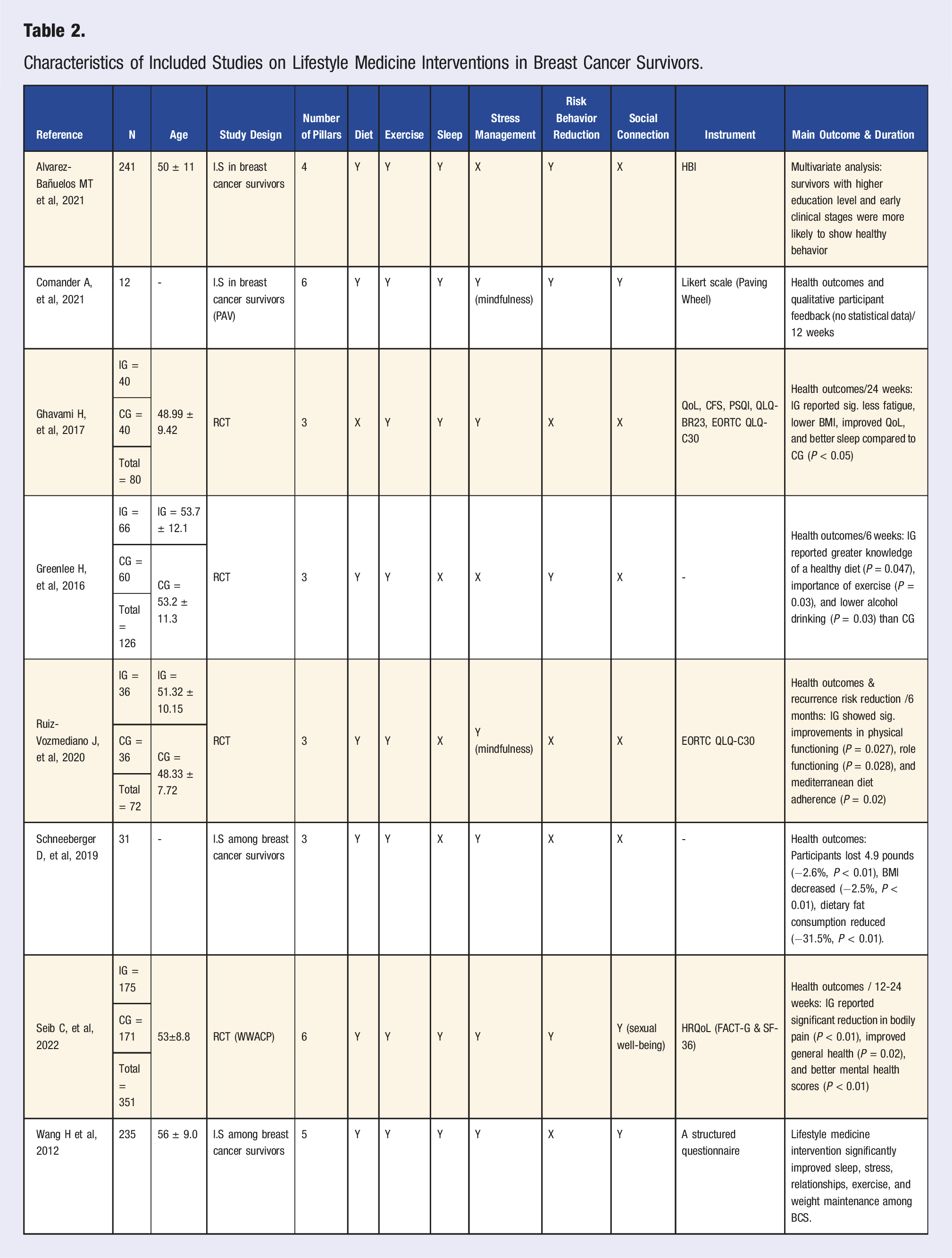
All studies included in this review focused on the effects of lifestyle medicine on female breast cancer survivors (BCS). It is important to clarify that our original hypothesis aimed primarily at assessing the efficacy of all six pillars of lifestyle medicine in this population. However, due to the limited number of articles (only 2) that specifically examined all six pillars, we decided to stratify our analysis to include studies focusing on the impact of 3 to 6 pillars. This decision was made because other systematic reviews have already addressed the effectiveness of interventions involving 2 pillars.
Among the 8 studies, 4 were randomized controlled trials (RCTs),11-14 while the remaining 4 were intervention studies without a control group.10,15-17 Notably, 2 studies14,16 included women with breast cancer who were not survivors, as well as participants with other types of cancer. We removed any passages from these studies that did not address our primary research question, retaining only the relevant sections focused on breast cancer survivors.
Sample sizes and compositions varied across the studies. The total sample sizes ranged from 12 to 351 participants, encompassing both intervention and control groups. The research populations differed in their demographic characteristics.
The personal characteristics of participants showed some consistency. All participants were women, aligning with the focus of our research question. The average age of participants was over 48.9 years, with the oldest participant being 56 years. However, it should be noted that two studies did not report the mean age of their participants.16,17
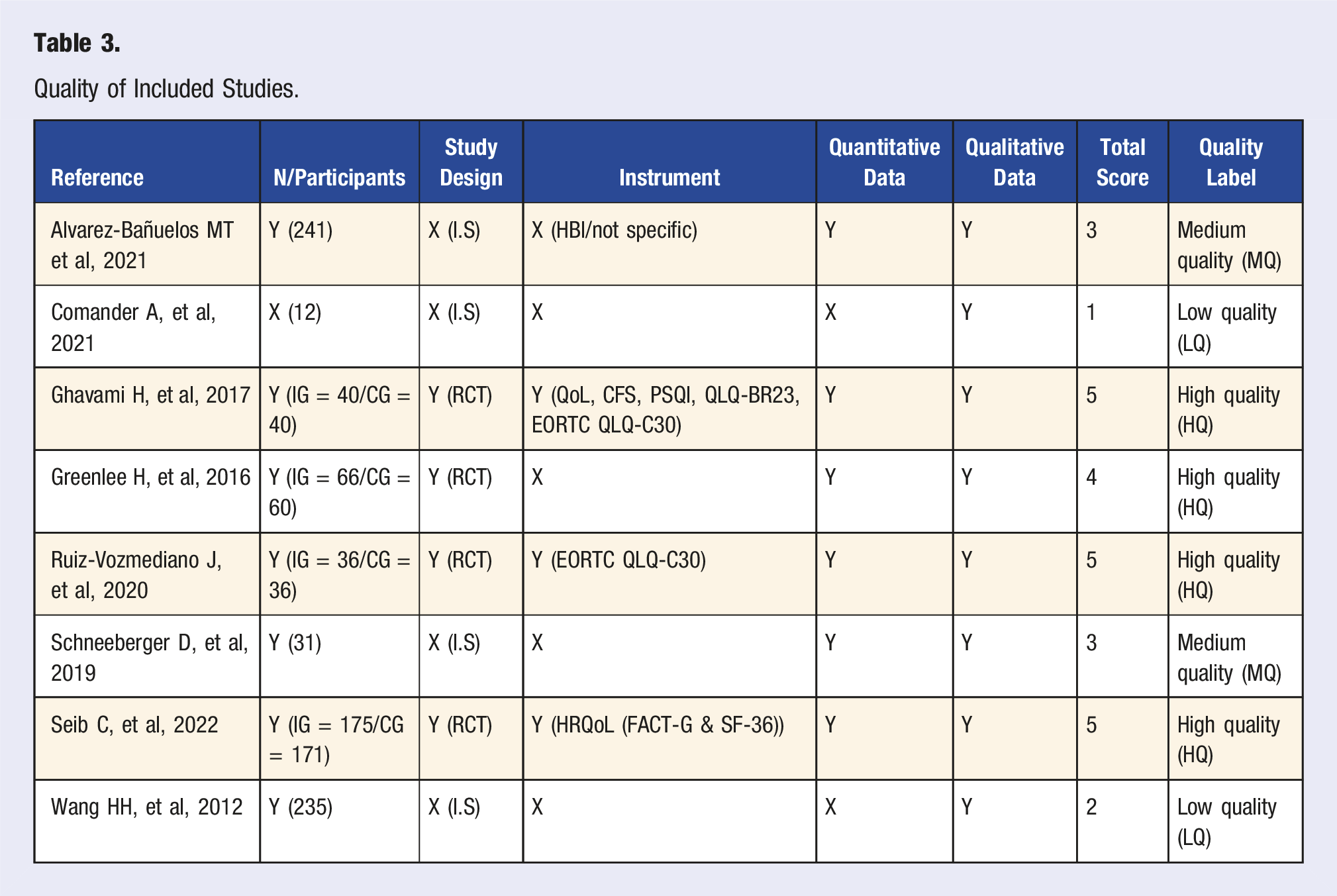
Quality of Included Studies.
The Effects of Lifestyle Medicine on Female Breast Cancer Survivors
This section presents the effects of lifestyle medicine on female breast cancer survivors. Most studies employed questionnaires to measure outcomes; however, 3 studies did not utilize any questionnaires.12,16,17 Additionally, two studies10,15 lacked a specific questionnaire. Only one common questionnaire was shared between two studies,11,13 while the remaining studies utilized different measurement tools. Nevertheless, the primary focus across all questionnaires was the assessment of quality of life.
All results are presented in Table 2.
Diet
Seven of the 8 studies reviewed assessed the effects of diet on female breast cancer survivors.10,12-17 These studies demonstrated that participants made dietary changes, including a substantial adoption of healthy eating choices, which significantly contributed to improvements in their quality of life. For example, in study, 13 there was a significant reduction in body mass index (BMI) (P = 0.04) and weight (P = 0.05).
Exercise
It is noteworthy that the only pillar included in all 8 studies was physical exercise, highlighting its beneficial role in managing stress. Most participants learned to prioritize exercise through the interventions, whether it involved walking or participating in a group program. For instance, study 13 demonstrated significant improvements in physical functioning in the intervention group (IG) compared to the control group (CG) (P = 0.027).
Sleep
Sleep was incorporated as an intervention element in 5 studies.10,11,14-16 Notably, in the study conducted by Ghavami et al (2017), 11 the intervention group exhibited better sleep quality compared to the control group over a 24-week period (P < 0.05).
Avoiding Harmful Behaviors and Addictions
The pillar related to avoiding tobacco and alcohol use was addressed in 4 articles.12,14-16 Specifically, in article, 12 participants in the intervention group reported a lower frequency of alcohol consumption compared to the control group (P = 0.03).
Stress Management
Stress management was incorporated as a method in 6 studies.10,11,13,14,16,17 However, not all studies utilized the same approach, as there are numerous reliable and effective methods available. For instance, the studiesof Ruiz-Vozmediano et al. 13 and Alvarez-Bañuelos et al. 16 implemented mindfulness-based stress reduction techniques. Additionally, the study of Schneeberger et al. 17 reported changes in psychosocial variables, including perceived stress and depression, although these changes were not statistically significant.
Relationships
The parameter of social interactions was addressed in 3 studies.10,14,16 Notably, in the “PAVING the Path to Wellness” program 16 for breast cancer survivors, significant emphasis was placed on fostering high-quality connections with family, friends, and the broader community throughout the intervention. The ultimate goal was to facilitate meaningful relationships among participants.
Quality of Life Outcomes
Improvement in quality of life was a common outcome across all studies. Notably, regardless of whether the intervention involved 3 pillars or 6, all approaches significantly impacted the overall quality of life for women who survived this challenging disease. Factors such as poor sleep quality, lack of exercise, and the psychological stress associated with fear of relapse can weaken the body and overall well-being. The reported outcomes included increased physical and mental well-being, reduced physical pain, and a decrease in the burden of symptoms among women who had previously undergone treatment.
Reducing the Risk of Relapse Outcome
A reduction in the risk of recurrence was reported in two studies.13,16 The first study, conducted in 2019, utilized the 6 pillars of lifestyle medicine and demonstrated a reduction in the risk of breast cancer recurrence. In 2023, a subsequent study 18 evaluated the short-term effects of the “PAVING the Path to Wellness” program on behavioral and psychological outcomes, further confirming that it reduced the risk of breast cancer recurrence. The second study highlighted the roles of a healthy diet, exercise, and mindfulness in potentially lowering the risk of recurrence among breast cancer survivors.
Discussion
To the best of our knowledge, this is the first systematic review assessing the effectiveness of lifestyle medicine interventions in female breast cancer survivors (BCS). This review aims to fill the gap in the existing literature by identifying 8 articles representing 8 studies on the effects of lifestyle pillars, categorized into 4 high-quality, 2 medium-quality, and 2 low-quality studies, published between 2012 and 2024.
The ultimate goal is to de-escalate treatments that may negatively impact the quality of life for breast cancer survivors. 19 Generally, breast cancer survivors report increased challenges related to cognition, sexual function, fatigue, and anxiety. Therefore, they should be closely monitored and offered interventions when possible, with the aim of adopting healthy behaviors. 20
There is a significant need for practical and effective interventions for breast cancer survivors that can help alleviate residual effects from chemotherapy and the stress experienced during their illness. 21 Ernst Wynder first coined the term “Lifestyle Medicine” in 1988, and in 1999, James Rippe published the first text titled Lifestyle Medicine in the USA. As of January 1, 2018, there were 239 references to the term identifiable in PubMed. 22
General Findings
Lifestyle Medicine Intervention
Of the 8 studies reviewed, 611-14,16,17 reported results related to the improvement of healthy behaviors. Notably, the study by Wang et al. 10 highlighted that the lifestyle medicine intervention was significant for breast cancer survivors (BCS), as participants reported challenges with sleep quality, stress, relationships, exercise, and weight maintenance.
This finding is particularly impressive because research demonstrating the importance of improving quality of life for individuals recovering from breast cancer predates the formal establishment of the term “lifestyle medicine.” Additionally, the study by Alvarez-Bañuelos et al. 15 revealed through multivariate analysis that survivors with a higher level of education were significantly more likely to engage in healthy behaviors (OR: 0.3, 95% CI 0.12 - 0.8), as were those diagnosed at earlier clinical stages (OR: 0.4, 95% CI 0.2-0.9).
Other Results
There was considerable diversity in the tools used to measure quality of life, with each scale assessing different parameters. The scales present in all studies included the Health Behaviors Inventory (HBI) scale,15,23 the Cancer Fatigue Scale (CFS), 24 and the Pittsburgh Sleep Quality Index (PSQI). 25 Additionally, the EORTC QLQ-BR23 26 is a breast cancer-specific questionnaire comprising 23 items that address the effects of treatment, outlook for the future, body image, and sexuality. Other scales used included the EORTC QLQ-C30, 27 the Health-Related Quality of Life (HRQoL) measures such as the Functional Assessment of Cancer Therapy-General (FACT-G), 28 and the Short Form Health Survey (SF-36). 29
Most variables were assessed using symptom-focused negative outcome measures (e.g., cancer-related fatigue, treatment effects on self-image), while some employed positive symptom-focused measures (e.g., sleep quality, subjective well-being). Few variables were evaluated using process-focused measures, leading to mostly general conclusions. This may be due to the relatively new status of Lifestyle Medicine within the medical community, which is still being tested in practical applications.
We believe it would have been beneficial to focus more on patients’ anxiety about relapse and the potential of lifestyle interventions to reduce this risk. Specifically, only two studies13,16 mentioned qualitatively that lifestyle interventions could reduce the risk of relapse. It is important to note that self-report measures are inherently biased; participants who invest considerable time and energy in a treatment program, such as lifestyle medicine, may be less likely to provide negative feedback. Therefore, obtaining behavioral reports from relevant others could serve as a valuable addition to the data.
Future research on lifestyle interventions for breast cancer survivors should consider evaluating a range of outcomes, including pre- and post-intervention biological measures (e.g., cortisol reduction) and telomere length, which may demonstrate improved cellular aging among participants, as highlighted in the study by Brown et al. 30 Moreover, future research could benefit from differentiating the components of lifestyle medicine interventions that utilize all six pillars in comparison to those employing three or four pillars.
Our search method, which included holistic programs of lifestyle medicine, revealed only two relevant studies,14,16 both of which had low quality and small sample sizes and were not randomized controlled trials (RCTs). Lifestyle practices are often employed in clinical settings to prevent various diseases and may also help mitigate the onset of breast cancer. 4 However, these practices could be particularly beneficial for breast cancer survivors, as the stigma of anxiety, weakness, and side effects resulting from hormone therapy require significant attention. There is a pressing need for future research to assess the impact of lifestyle medicine on breast cancer survivors and to evaluate the quality of the outcomes.
Contraindications
Currently, the literature indicates that there are no contraindications for the practice of Lifestyle Medicine among breast cancer survivors, suggesting a fertile ground for its implementation. However, the effectiveness and long-term outcomes of these interventions remain open questions. Future randomized clinical trials are needed to investigate whether Lifestyle Medicine truly delivers effective results over time. It is also important to note that none of the studies reviewed provided specific allusions to the duration of the observed outcomes.
Limitations
While this systematic review provides valuable insights into the impact of lifestyle medicine on the quality of life of breast cancer survivors, several limitations must be acknowledged.
Study Design Variability and Risk of Bias
The included studies exhibited substantial variation in research design, ranging from randomized controlled trials (RCTs) to quasi-experimental and observational studies. While RCTs provide a higher level of evidence, the inclusion of non-randomized studies introduces potential biases, particularly in participant selection and outcome assessment. Additionally, the absence of blinding procedures in several studies may have influenced self-reported results, leading to response bias.
Heterogeneity in Interventions and Measured Outcomes
One of the most significant challenges in this review was the high variability in interventions and outcome measures. Studies implemented different combinations of lifestyle medicine pillars, with variations in duration, intensity, and adherence tracking. This lack of standardization makes it difficult to compare results across studies and limits the ability to draw generalized conclusions.
Furthermore, the tools used to assess quality of life and health outcomes were inconsistent across studies. Some employed well-validated instruments (e.g., EORTC QLQ-C30, FACT-G, SF-36), while others relied on non-standardized or self-reported data, which may not fully capture the impact of lifestyle interventions.
Given this variability, our findings should be interpreted with caution, and future studies should aim to establish standardized protocols for intervention implementation and outcome measurement.
Potential Publication Bias
Publication bias remains a concern in lifestyle intervention research. Studies reporting positive outcomes may be more likely to be published than those reporting neutral or negative effects. 31 This bias could lead to an overestimation of the effectiveness of lifestyle medicine in breast cancer survivors. To address this issue, future research should incorporate pre-registered protocols and systematically report both positive and negative findings.
Limited Sample Sizes and Generalizability
Many of the included studies had small sample sizes, which may impact the statistical power and reliability of their findings. Additionally, demographic details such as age distribution, socioeconomic status, and ethnicity were not consistently reported, limiting the generalizability of the results. Future studies should aim for larger, more diverse participant groups to ensure broader applicability of findings across different populations of breast cancer survivors.
Short-Term Follow-Ups and Lack of Longitudinal Data
Most studies assessed outcomes immediately following intervention completion, with few providing long-term follow-up data. As a result, it remains unclear whether the observed benefits are sustained over time. Future research should incorporate longitudinal designs with extended follow-up periods to determine whether lifestyle modifications lead to lasting improvements in quality of life and recurrence risk reduction.
Conclusion
This systematic review provides compelling evidence that lifestyle medicine interventions can significantly enhance the quality of life for breast cancer survivors. The findings emphasize that comprehensive approaches integrating multiple lifestyle pillars—such as physical activity, nutrition, stress management, and social support—yield notable benefits in physical and psychological well-being. Improvements in fatigue reduction, sleep quality, mental resilience, and overall health were evident across the studies, reinforcing the potential of lifestyle medicine as an essential component of survivorship care.
Despite the heterogeneity of interventions and study designs, the collective evidence supports the positive impact of holistic lifestyle modifications on survivors’ well-being. While limitations such as variability in study methodologies and short-term follow-ups exist, this review underscores the necessity of incorporating lifestyle interventions into clinical practice to provide non-pharmacological, patient-centered strategies for enhancing long-term health outcomes.
To further strengthen the field, future research should focus on standardized intervention protocols, larger sample sizes, and longer follow-up periods. By addressing these gaps, the role of lifestyle medicine in breast cancer survivorship can be further clarified, ultimately empowering survivors to take an active role in their recovery and long-term well-being.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
