Abstract
“Patient activation toward health is associated with a strong physician–patient relationship, specifically through high-quality, positive communication.”
Introduction
Lifestyle medicine aims to address chronic disease through evidence-based lifestyle changes, including a whole-food, plant-based eating pattern, adequate physical activity, healthy sleep, stress reduction, positive social connection, and avoidance of substance use 1 —recommendations corroborated by major medical societies. For example, the American Heart Association recommends a healthy eating pattern emphasizing vegetables, fruits, whole grains, legumes, nuts, and fish, with limited red and processed meats, refined carbohydrates, and sweetened beverages; 150 min of moderate physical activity per week; 7-9 h of sleep per night; and avoidance of tobacco. 2 The American Cancer Society has published similar guidelines on nutrition and physical activity. 3
Though medical education typically offers minimal training in lifestyle medicine, it remains imperative that medical professionals, particularly those practicing preventive medicine, communicate the benefits of healthful lifestyle behaviors, including a whole-food, plant-based eating pattern, in order to address rising rates of cardiometabolic and chronic diseases.1,4 In this study, we explore patient experiences with provider support, or lack thereof, when seeking to engage in a healthy lifestyle as a primary method for managing chronic conditions.
Materials and Methods
The IRB at the New York University (NYU) Grossman School of Medicine as well as the Office of Research and Administration for Implementation at NYC Health + Hospitals/Bellevue approved all procedures for this study (i18-01319). All participants provided informed consent.
Study Design and Sample
As part of a larger implementation evaluation, we conducted 2 focus groups with program participants (n = 17) from a novel plant-based lifestyle medicine (PBLM) program implemented in a safety-net healthcare system. 5 Adults with type 2 diabetes, prediabetes, heart disease, high blood pressure, high cholesterol, and/or excess weight (BMI ≥25) were eligible to participate. The goals of the program were to reduce cardiometabolic risk through adoption of 6 pillars of healthy lifestyle behaviors: a whole-food, plant-based eating pattern, improved sleep, increased physical activity, stress management, positive social connections, and avoidance of substance use. Participants learned of the program through earned media (e.g., TV news, newspapers), social media, announcements from the office of the Brooklyn Borough President, and limited health care provider referrals from within Bellevue. Thus, most patients self-selected into the program and joined by adding their name to a waitlist. Enrollment in the program was on a first-come, first-serve basis. Through the program, participants received support from trained clinicians on the 6 pillars. Individuals were eligible to participate in the focus groups if they made an initial appointment in the program, consented to participate in the evaluation, and agreed to be contacted about participating in focus groups. To maximize diversity of focus group participants in age, gender, time in the program, and success in the program, the evaluation team worked with two of the program providers (registered dietitian and health coach) to create a list of prioritized eligible individuals. A member of the evaluation team contacted the prioritized eligible individuals to invite them to participate in a focus group and obtain verbal consent.
Focus Group Procedures
The focus groups were conducted in-person by a trained moderator using a semi-structured guide. Two evaluation team members were present to observe nonverbal cues, take notes, and ask clarifying questions. The focus group discussions covered a range of topics related to the participants’ interest in joining the program, experiences with the program, as well as their experiences with the healthcare system and lifestyle medicine outside of the program. Relevant to this study, they were asked, “Why did you decide to participate in the PBLM program?” and were probed on what goals they had in mind when signing up for the program, why they felt it was the right program for them, what made them ready to commit to participating in the program, and who encouraged them to enroll in the program. In an effort to explore the role of the PBLM program in their overall healthcare participants were asked, “How does the PBLM program fit into your regular health care?” and were asked follow-up questions on where they go for routine preventive care and whether/why they are seeing other providers. Finally, we explored barriers to participation asking, “What has the biggest challenge you have experienced in trying to follow the recommendations made by the PBLM program?” The focus groups were conducted at New York University Grossman School of Medicine offices in October and November of 2019 and lasted approximately 90 min each. Participants received a $25 gift card incentive for their time and effort. The focus groups were audio-recorded and professionally transcribed.
Analyses
Focus group data were analyzed using a hybrid deductive-inductive thematic analysis approach. 6 For the current study, we thematically analyzed all references in the focus group transcripts of participant interactions with healthcare providers outside of (not affiliated with) the lifestyle medicine program. To do this, we employed a rapid coding process 7 in which the research team independently reviewed transcripts, met to discuss themes, and jointly created a summary template to systematically extract main point and illustrative quotes for each theme. The summary template was protocol driven with codes for the primary research questions (deductive) and additional codes for the themes that were identified through review and discussion (inductive). Three researchers (RO, RM, SA) coded the transcripts independently. At the conclusion of coding, researchers met to compare coding side-by-side to assess the amount of data extracted and attribution to specific domains, resolve discrepancies through discussion, and synthesize the data across the summaries.
Results
Characteristics of Focus Group Participants (n = 17).
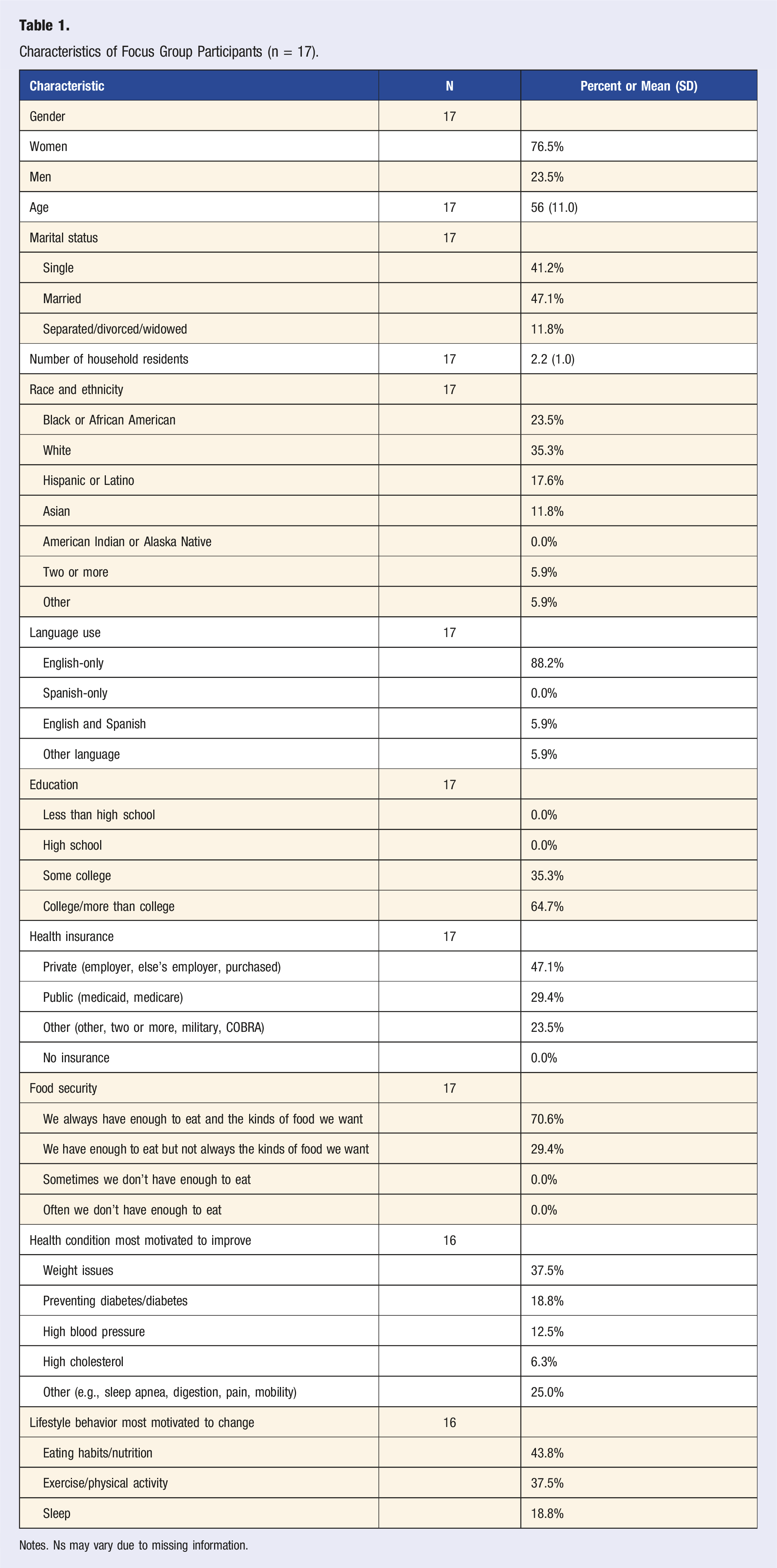
Notes. Ns may vary due to missing information.
We organized the results around 2 themes related to participant experiences with the healthcare environment: (1) discordant perspectives between patients and outside providers (providers not affiliated with the lifestyle medicine program) regarding the benefits of lifestyle medicine in treating lifestyle-related chronic illness, and (2) provider support in the context of exposure to lifestyle medicine. Across the 2 focus groups, these themes were organically discussed by 6 of the 17 participants without querying in equal measure (i.e., 3 shared comments related to theme 1 and 3 respondents shared comments related to theme 2).
Discordant perspectives between patients and non-lifestyle medicine program affiliated providers regarding the benefits of lifestyle medicine in treating lifestyle-related chronic illness. Focus group participants shared their experiences communicating with providers about lifestyle medicine as treatment for chronic conditions. For some, there was a sense that providers were not open to listening to their treatment preferences, favoring instead medications as first-line therapy. Below, 2 respondents describe repeated disunity between themselves and their provider. “My primary care doctor was always at odds with me. He’s the classic pill pusher. So, all he wanted to do was have me take blood pressure medication and cholesterol medication and so on. In spite of my attempts to give him background as to the lifestyle that I wanted to pursue—I gave him books and things like that—he still created a lot of tension. Every time I went there, it was a struggle.” (Male, Age 64, White, hypertension, hyperlipidemia; Lifestyle most motivated to change: “Eating habits/nutrition”) “I was not getting the support from doctors who just wanted to give me medicines.” (Man, Age 63, White, hypertension; Lifestyle most motivated to change: “Exercise/ physical activity”) In some cases, focus group participants disclosed their providers lacked fundamental knowledge about the benefits of following a plant-based eating pattern. One respondent recommended that providers receive enhanced or ongoing training on plant-based nutrition. “My endocrinologist told me that she didn’t want me to do vegan, because that would cause me to eat too much carbs, and then my blood sugar would go up. There should be also a component for doctors. To educate, some kind of training. Not mandatory. Maybe they have to do it voluntarily, but I think doctors need to—because now, there’s so much research now that a lot of stuff they’re telling people are not factual anymore…Yeah, outdated. And a lot of these doctors, I don’t know what doctors do. I’m a paralegal. But they seem to be out of sync. One time, I said to my doctor, I’ve seen research—and she looked at me like I just said I’m growing a second head. And I’m saying, I thought this was something that they hear about or know about, but apparently not.” (Woman, Age 65, Black, diabetes, hypertension, psoriasis; Lifestyle most motivated to change: “Exercise/ physical activity”) This respondent went on to share that the lack of support for lifestyle medicine encountered in the healthcare setting resulted in looking for alternative providers who explicitly support a whole-food, plant-based lifestyle. “I’ve been searching for a whole food plant-based doctor ever since I started the program, because my primary [care] doctors are just starting to annoy me. They’re starting to annoy me because now that I have this information [about lifestyle medicine], I’m like ‘why aren’t you following me?’ And you’re telling me all this stuff, and I’m hearing it, and I’m witnessing that it is not the case.” (Woman, Age 65, Black, diabetes, hypertension, psoriasis; Lifestyle most motivated to change: “Exercise/physical activity”)
Provider support in the context of exposure to lifestyle medicine. Importantly, participants shared examples of providers supporting healthy lifestyle modification after exposure to the concept of lifestyle medicine as a primary treatment for chronic disease. Below, 2 participants cited instances where providers became familiar with the lifestyle medicine program, either through communicating with a program provider or through exposure at their workplace, and were supportive of participation. “I switched to a [primary care] doctor out where I live in Long Island. He’s very supportive. In fact, he was so impressed by [one of the lifestyle medicine doctors]. He called my primary care and he had conversations and my primary care said, ‘That’s an amazing program’.” (Man, Age 64, White, hypertension, hyperlipidemia; Lifestyle most motivated to change: “Eating habits/nutrition”) “My [partner] works at [hospital name], and he had a cardiac, he had to have two stents put in in September, and in the recovery room, the doctor was talking about this program, and I had high blood pressure … so I called [to make us appointments].” (Woman, Age 49, Asian, hypertension; Lifestyle most motivated to change: “Exercise/physical activity”)
Discussion
When patients’ enthusiasm to make healthy lifestyle changes is unmet by their providers, there is a missed opportunity to practice evidence-based guidelines, and a risk of harm for patients with multi-morbidities. The lifestyle medicine program in which participants in the current study were enrolled has shown improvements in clinical markers of cardiometabolic risk (e.g., hemoglobin A1c, weight), lifestyle behaviors (e.g., diet quality, physical activity), and nutrition knowledge.8,9 The opportunity to incur these benefits may have been lost for these patients had they not pursued this program and the adoption of pillars of lifestyle medicine despite the perception of their physicians’ opposition.
Patient activation toward health is associated with a strong physician–patient relationship, specifically through high-quality, positive communication. 10 As described by a Scientific Statement from the American Heart Association, the reluctance to actively encourage patient participation in lifestyle medicine may stem from medical education prioritizing pharmacological intervention over lifestyle behavior change interventions. 4 Given that nearly 80% of deaths from cardiovascular disease, the leading cause of death in the United States, may be preventable through lifestyle modifications, 11 lifestyle medicine training should be emphasized. In-depth, skill-building curricula require significant time and resources. However, our findings suggest that as a starting point, simply enhancing exposure to and awareness of lifestyle medicine may reduce barriers to patient engagement in healthful lifestyle interventions, and potentially improve clinical outcomes.
Given that lifestyle medicine is a first-line, evidence-based recommendation in the practice of preventive medicine, and that increasing frequency of its practice reduced clinician burnout, 12 identification of provider-level barriers to its use is critical. Clinician training and education may be particularly crucial to supporting patients through the implementation of lifestyle medicine in practice. Further, such education should be multi-disciplinary given it has been demonstrated that the challenges of integrating lifestyle medicine into every day clinical practice are eased by and benefit from a multi-disciplinary team approach. 13 For each provider on the multi-disciplinary team it is suggested that the transfer of knowledge is the main pathway to the adoption of new medical practices. 14 Applying the adopter model of new behaviors, providers may align with different steps along the spectrum, from full adoption to rejection. 15 For lifestyle medicine, this may generally follow 3 groups: (1) those who fully embrace lifestyle medicine, (2) those who embrace its importance but are less familiar with how to practice it or where to refer for evidence-based programming, and/or may require additional training, and (3) those who embrace rejection, resistance or significant barriers to its adoption in practice.
Prior findings from the PBLM program demonstrate its efficacy,8,9 and so for those in the first adopter group, convincing of this efficacy is not a barrier, yet external barriers may need to be addressed such as dissemination of lifestyle medicine practices in public hospital systems5,16 and increased capacity for lifestyle medicine providers to practice.17,18 One qualitative study of primary care providers elucidated what aligns with the potential second group. The study assessed perspectives on barriers to the use of lifestyle behavior change in practice found that even though providers in this study were familiar with the recommended guidelines of leading medical organizations, including the American Heart Association, to use lifestyle behavior change as first line in preventive medicine practice, providers remained unsure where to refer patients for lifestyle medicine and felt there was no overtly stated or specified supports from the healthcare systems in which they practiced. 19 For adopters in the second group, barriers to lifestyle medicine practice may need to be addressed with a slightly more individualized approach such as with increased professional training and adaption to time limitations during clinical encounters, 17 and challenges balancing other demands in workload. 15 Finally, for those who perceive greater barriers to lifestyle medicine adoption (e.g., the third group of proposed adopters), personal practice beliefs may need to be empathically addressed. That is, some providers may feel the clinical benefit of lifestyle medicine practices may be limited, presuming that lifestyle change would not help to improve patients’ medical condition(s) and instead prioritize medication over behavior change, even with the latter as an adjunct. 19 Therefore, the literature taken together with our study suggests that exposure to lifestyle medicine resources, as well as personal practice and beliefs, may influence the prioritization and use of lifestyle behavior change in patient care, which is especially relevant to the practice of preventive medicine. Importantly, given that personal perceptions of health influence the approach to lifestyle behavior change practice with patients, 20 it is crucial to acknowledge that such beliefs are vulnerable to historical and social contexts, and potential biases, further perpetuating disparities. 21 This may especially occur in populations seen in safety-net clinics and hospitals such as the one that served as the source of the current study. Health equity, therefore, must be considered in the approach providers take in their exposure to, and acceptance and use of, lifestyle medicine. 22
Importantly, a systematic review of numerous studies about patient–physician communication related to behavior change found the approach to this topic most often investigated is how providers perceive and initiate behavior change intervention for patients. 23 Our study findings suggest that more research is needed to explore how provider communication, beliefs and support are impacted by patient initiation of behavior change approaches or treatments. Research is particularly needed around the contribution of both the patient and provider for patient populations that are not already self-motivated to engage in lifestyle behavior change as those in our study. For example, investigators have suggested that factors like understanding of options, emotional state, and their relationship with their provider influence patients’ preference and readiness for participation in shared decision making. 24 The current study population reflects patients who were self-motivated and who had already made the decision to engage in a lifestyle medicine program with readiness for behavior change despite their providers’ perspectives. Therefore, in the current population, sentiments of a lack of support from providers may be less related to challenges in shared decision making and more reflective of a perceived lack of an openness of those providers to all approaches to care, including favoring the scope of practice from lifestyle change to pharmaceutical intervention. However, the general population who may have less prior knowledge of and/or less self-motivation for the option of lifestyle medicine may rely much more significantly on a providers’ ability to be both open to a full scope of practice and able to practice shared decision making communication. Our hypothesis-generating study therefore demonstrates the importance of provider perspectives on lifestyle medicine as foundational to bidirectional communication and shared decision making around the use of lifestyle medicine for treatment of non-communicable diseases. Taken together, our work in the context of the literature supports the need to engage providers in education about lifestyle medicine as a field, but also in addressing their own beliefs about its practice.
There are a few important limitations to note related to this study. First, this was part of a larger evaluation assessing the demand and feasibility of implementing a lifestyle medicine program in a safety-net setting. Thus, it was not an a priori research question to assess patients’ experiences with providers outside of the program. Further research is needed to understand the range of experiences patients have with providers using lifestyle-based care as the first-line therapy in the prevention and management of chronic illness. Second, the current findings may underestimate potential barriers faced by patients from their providers, given that individuals not captured in our study population ultimately may not have pursued this or other lifestyle interventions. Lastly, our findings may be sensitive to the participants in the focus groups. That is, the majority of participants were individuals from a higher socioeconomic status as evidenced by their educational attainment and food security. This lack of diversity is likely due to the first-come, first-serve enrollment procedures implemented by the program. However, we believe it is unlikely that a more diverse sample would have had different experiences with providers external to the program.
Conclusions
While the current study has limitations, including that the focus group data for this study were not collected with an a priori research question of assessing patient experiences with provider perspectives of lifestyle medicine, our hypothesis-generating findings suggest the need for future studies to explore how patients’ health is impacted by their providers’ perspectives of lifestyle medicine.
While preliminary, our findings suggest that patient engagement in, and chronic disease benefit from, evidence-based lifestyle behavior change programs may be best supported by general provider awareness of and exposure to lifestyle medicine.
Footnotes
Acknowledgments
We thank Barbara Tagliaferro for her help facilitating focus groups, the focus group participants for their time and candor, and the PBLM Program staff for their help with recruitment.
Author Contributions
All authors conceptualized the paper. MM designed the PBLM Program. RO, RM, and SLA analyzed the qualitative data and wrote the manuscript. All authors reviewed and edited the manuscript.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr Robin Ortiz reports receiving personal fees for consulting with the ACEs (Adverse Childhood Experiences) Aware Initiative, outside of and unrelated to, the current work. Dr Ortiz is board certified in lifestyle medicine. The authors have no additional conflicts to report.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by NYC Health + Hospitals. Dr. Robin Ortiz is supported by a Harold Amos Faculty Development Award through the American Heart Association and the Robert Wood Johnson Foundation as an AHA AMFDP scholar (Award number 23AMFDP1161309).
Ethical Statement
Data Availability Statement
The data that has been used is confidential.
