Abstract
The Complete Health Improvement Program (CHIP) is an intensive therapeutic lifestyle modification program (ITLMP) with well-documented success in decreasing risk factors for cardiovascular disease (CVD). Plant-based diets and physical activity are components of the program that contribute to these improvements. Yet, there are few studies on how ITLMPs affect risk factors specifically for the geriatric population. The goal of this study was to examine results of CHIP participants with a focus on the older (greater than 65 years) population in Athens, Ohio. Retrospective data from 2011 to 2017 were analyzed for 26 CHIP classes. Recorded variables included body mass index (BMI), blood pressure (BP), total cholesterol (TC), triglycerides, low-density lipoprotein cholesterol (LDL), high-density lipoprotein cholesterol (HDL), blood glucose (BG), and exercise level. Among geriatric participants, significant changes were found in BMI, BP, TC, LDL, HDL, BG, and exercise level (P < .001). As compared to the younger population, changes in variables were equivalent in the geriatric population in all variables (P > .05). These improvements in CVD risk factors among the elderly support the hypothesis that CHIP should be considered for CVD prevention and treatment in the geriatric population.
Introduction
Cardiovascular disease (CVD) remains the leading cause of death in the United States and is expected to escalate in upcoming years. 1 Older populations are at increased risk of developing clinical CVD due to age-related declining cardiovascular function.2,3 Physical activity and healthy lifestyle practices have shown to not only decrease and prevent disease in the elderly but also lower premature mortality.3,4 Lifestyle modification programs, focusing on consuming plant-based, whole foods, have been successful in reducing modifiable risk factors for CVD, including elevated body mass index (BMI), elevated blood pressure (BP), and abnormal lipid levels.5-8
The Complete Health Improvement Program (CHIP) is an intensive, therapeutic lifestyle modification program (ITLMP) that promotes a plant-based whole food diet, physical activity, and stress management in a variety of settings including clinics, workplaces, communities, and online programs. 9 The goal of CHIP is to encourage positive lifestyle habits mainly through diet and exercise, leading to improvements in chronic medical conditions, such as diabetes, hypertension, and dyslipidemia.9,10 Although there is an increase in elderly patients in the United States, the geriatric population remains understudied, lifestyle modification studies being mainly focused on younger populations.9,11,12 This current study evaluated the effectiveness of CHIP to reduce CVD risk factors specifically in the geriatric population, as compared to the younger population.
Methods
Retrospective data were evaluated from consenting CHIP participants in 26 CHIP classes, delivered in 16–18 sessions over 2–4 months, in Athens, Ohio, from 2011 to 2017. The format of CHIP changed from 16 to 18 sessions during the time period studied. Timing of delivery of content was flexible; sessions were being delivered in a time span of up to 16 weeks (1–3 sessions per week). Comparison groups were formed based on age: those under 65 years and those 65 and older.
Complete Health Improvement Program classes were provided by Live Healthy Appalachia, a local nonprofit organization in Athens, Ohio, that promotes healthy eating and active lifestyles in the region. Complete Health Improvement Program participants were asked to sign a consent permitting use of their data to be de-identified and aggregated for analytical purposes. Nonconsenting individuals for this data collection were still eligible to participate in CHIP classes but were excluded from this study. Approval was obtained from the Ohio University Institutional Review Board (16-X-44) and registered with ClinicalTrials.gov (NCT03025451).
CHIP Intervention
Complete Health Improvement Program has been utilized in clinics and communities for over 25 years to empower participants to choose healthy lifestyle habits to prevent, arrest, and reverse chronic lifestyle-related disease, and has gone through many modifications. 9 In this study, participants took part in 16–18 sessions over 2–4 months. Prerecorded videos and group activities were used for instruction. Group activities consisted of discussions, physical exercise, and cooking demonstrations.9,10 Participants were instructed to follow a minimally processed, predominantly plant-based, whole foods diet, focused on vegetables, fruits, cooked whole grains, legumes, and limited nuts and seeds. Daily dietary objectives of CHIP were fat less than 20% of calories, less than 10 teaspoons of added sugar, less than 2000 mg of added salt, cholesterol less than 50 mg, and 35–40 g of fiber. 10 Complete Health Improvement Program also promoted at least 30 minutes of moderate physical activity or 10 000 steps daily. Strength training exercises with a duration of 20–30 minutes, 2–3 days a week, were also advised. 10
Data Collection
At the beginning of the course, and
Data Analysis
Descriptive statistics were performed to describe and summarize the data. The corresponding frequency, percent distribution, mean, and standard deviation (SD) were reported. Bivariate analysis was performed using the paired sample t-test to compare pre- and post-measures to determine effectiveness of the intervention in each age group, and percent changes between groups; P value < .05 was considered significant. All analyses were performed using SAS 9.4
Results
Age and Gender of Complete Health Improvement Program Participants.
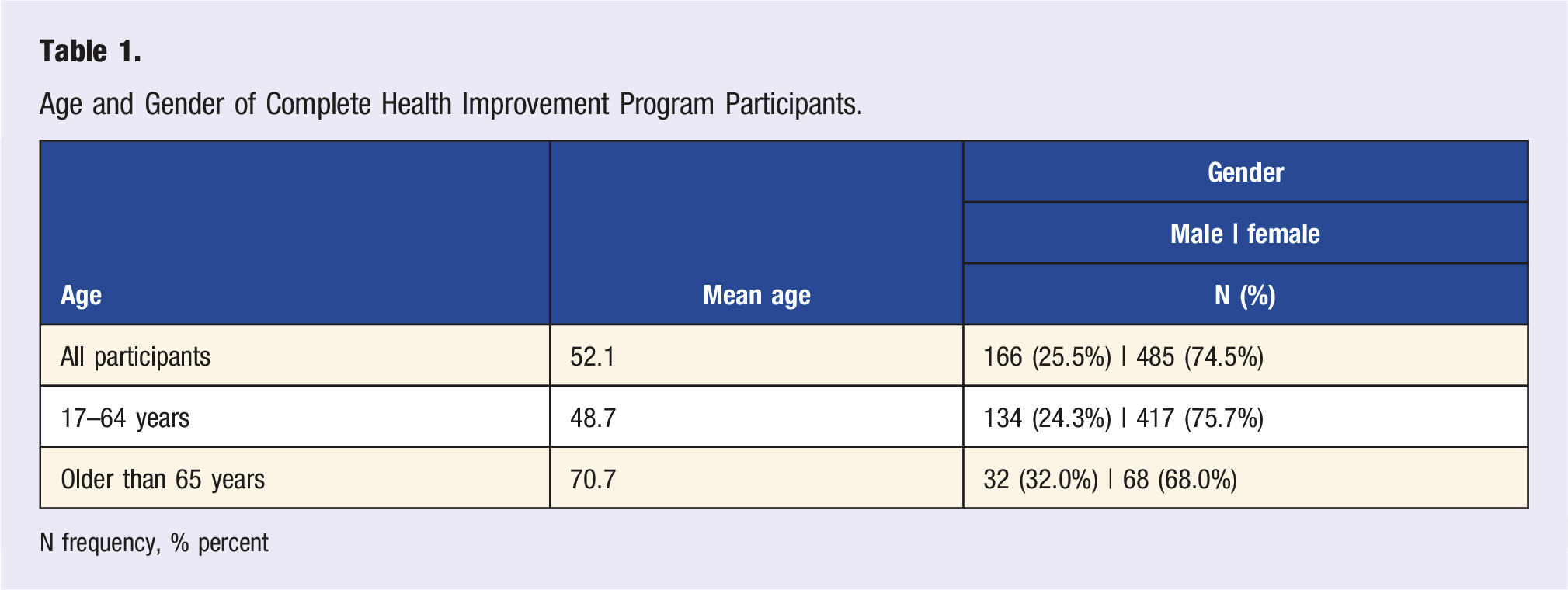
N frequency, % percent
Results of CHIP Participants Separated by Age; 17–65 Years and 65 Years and Older Reported with Standard Deviation in Parentheses.
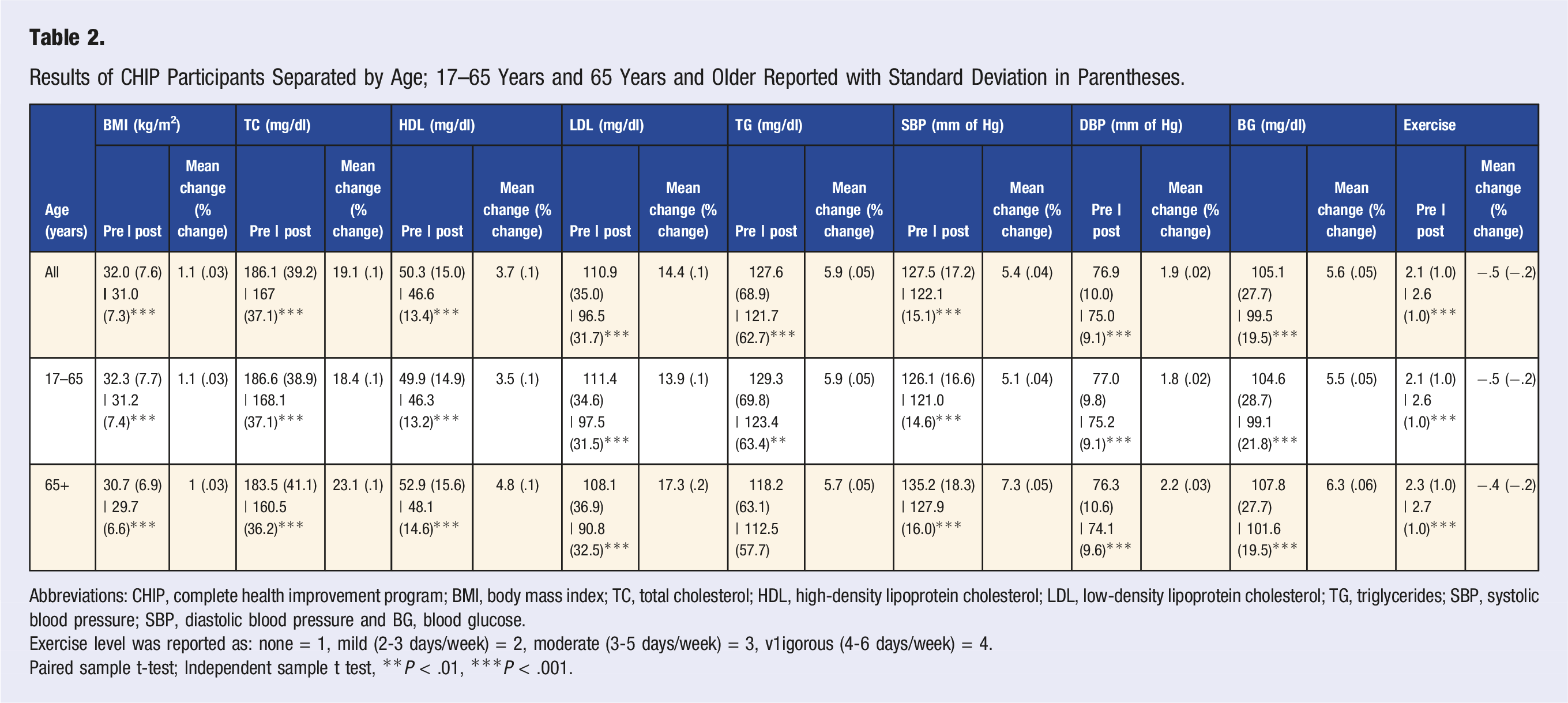
Abbreviations: CHIP, complete health improvement program; BMI, body mass index; TC, total cholesterol; HDL, high-density lipoprotein cholesterol; LDL, low-density lipoprotein cholesterol; TG, triglycerides; SBP, systolic blood pressure; SBP, diastolic blood pressure and BG, blood glucose.
Exercise level was reported as: none = 1, mild (2-3 days/week) = 2, moderate (3-5 days/week) = 3, v1igorous (4-6 days/week) = 4.
Paired sample t-test; Independent sample t test, **P < .01, ***P < .001.
Discussion
The primary aim of this study was to compare outcomes of geriatric CHIP participants compared to younger participants. Complete Health Improvement Program, generally, across populations, and specifically, in Athens, Ohio, showed improvements in CVD risk factors including improvements in BP, TG, LDL, and BG.9,10,12 This study focused on those older than 65 years, demonstrating that CHIP is effective in reducing CVD risk factors for the elderly. Though research incorporating lifestyle modifications in the geriatric population is limited, these findings align with previous studies.
The effectiveness of CHIP in reducing risk factors for CVD is well established.9,12 Plant-based diets have been shown to improve rates of atherosclerosis,13,14 glycemic control,15,16 and lower BP.17,18 Individuals adhering to vegetarian diets typically have lower BMI, and lower incidences of heart disease, type II diabetes, and hypertension.19-23 One reason for these findings could be plant-based products are rich in polyphenols, antioxidants, and fiber that decrease inflammation and promote insulin sensitivity.14,24-26
Elderly populations benefit from daily physical activity. A minimum of 30 minutes of physical activity 5 times a week lessens or prevents age-related morbidities and mortality related to CVD among the elderly.27-28 Positive outcomes for mental health such as less feelings of depression and loneliness, as well as improvements in perceived support, were seen among elderly individuals that engaged in regular physical activity. 29
Aging has been associated with increased atherosclerosis and inflammation, which leads to higher risks of myocardial infarction or ischemic stroke.30-32 Mediterranean diets consisting mainly of vegetables, fruits, and legumes, with limited red meat and dairy consumption, showed lower risks of mortality and decreased inflammation in elderly populations. 33 Diets focused on plant-based whole foods not only decrease plaque formation but also obesity, cardiovascular morbidity, hypertension, CVD, and stroke, as well as mortality in the elderly.5,14,21,34 These benefits are likely from protective nutrients such as antioxidants and anti-inflammatory compounds in plant-based foods35,36 that work through multiple mechanisms, such as folate which helps lower plasma homocysteine. 37
Improvements in cognition were discovered among elderly patients that follow Mediterranean diets, which may be the result of lowering inflammation, which otherwise can cause cerebral damage over time and lead to cognitive decline. 38 Adherence to plant-based foods also showed improvements in systemic inflammation and insulin sensitivity, in an elderly population with chronic kidney disease. 39
Consistent with other studies on plant-based diets, HDL levels decreased in the short term. This has been discussed elsewhere and is thought to be a rapid compensatory response to the dramatic decrease in LDL. 10 In unpublished 6-month follow-up data on CHIP participants, the principal investigator of this study (DD) found that HDL increases over time, even when LDL stays low, possibly more slowly responding to the increased exercise of CHIP participants.
The current study’s findings support the benefits of CHIP in promoting positive health outcomes not just for the general population, but the elderly as well. Therefore, lifestyle modification programs, such as CHIP, should be considered as an intervention to improve overall health and well-being for this age group.
Limitations
Participants self-selected to enroll in CHIP, and in this study. No control group was utilized. Medication usage and changes in medications during the program were not considered in the analysis for either group, which could have impacted the results. The second data collection occurred after the 11th session, which, depending on the particular class, may have been after as little as 3 weeks of onset of intervention, or as long as 12 weeks. This variability was equal for both age groups. It is unclear how quickly the intervention reaches its maximum impact; the data possibly underrepresenting the full benefit of the program. Factors such as race, socioeconomic status, individual behaviors, and environment were also not accounted for. There was a female predominance in the population, which has been the case in all CHIP studies. Exercise data on the CHIP survey may have been interpreted differently by different participants since each value could be interpreted as number of days per week of exercise, or by intensity of exercise. However, if the participant was consistent in interpreting the question for both data points, a change in number would likely indicate a change in level of physical activity.
Conclusion
This study demonstrates the effectiveness of CHIP in the geriatric population in reducing CVD risk factors in the short term, focusing on a plant-based whole foods diet, physical activity, and stress management. Aging is a prominent risk factor for CVD. The geriatric population will continue to increase in the coming years, leading to higher social health burdens from CVD and other lifestyle-related diseases. Programs like CHIP may be a cost-effective tool to be considered in treatment plans for the elderly.
Footnotes
Author’s Note
Future studies focused on the geriatric population and lifestyle modification should consider the effect on medication use, comorbidities, and outcome measures, emphasizing an impact on health expenditures.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
