Abstract
Background
This study aims to provide a general overview of cancer risk perceptions and reported sunburns to prevent sunburn and reduce the long-term risk of developing skin cancer.
Methods
Data were obtained from the 2022 Health Information National Trends Survey 6 and analysis was carried out with SPSS. Descriptive statistics were conducted to explore sociodemographic characteristics, cancer risk perceptions, and behaviors surrounding sunburns in our sample. Associations between number of sunburns and sociodemographic variables were reported using multinomial regression analysis.
Results
When asked how confident patients felt about their ability to take good care of their own health, most respondents felt either very confident (44.0%) or completely confident (27.3%). When asked how often they experienced a sunburn in the past 12 months, 2.1% reported experiencing more than 6 sunburns, 30.3% reported having between 1-5 sunburns, and 67.6% reported experiencing no sunburns. Using multinomial regression analysis, statistically significant associations were reported between number of sunburns and age, gender, occupation status, marital status, education, Hispanic origin, race, and income level.
Conclusion
The results of our study reinforce the need for public health interventions that effectively disseminate information on skin cancer risk across ethnic minority groups, especially in underserved communities within the U.S.
“Our findings solidify the correlation between risk of alcohol consumption and increased sunburn incidence.”
Introduction
Skin cancer, characterized by the uncontrolled growth of abnormal skin cells, is one of the most prevalent forms of cancer in the United States. 1 Skin cancer is primarily manifested by three major pathologies: basal cell carcinoma, squamous cell carcinoma, and melanoma. 1 Basal cell and squamous cell carcinomas, collectively known as non-melanoma skin cancers, are the most common and typically have lower rates of malignancy. Melanoma is less frequent but is significantly more dangerous due to its higher likelihood of spreading to other organs. 1 According to the American Cancer Society, millions of non-melanoma skin cancers and tens of thousands of melanoma cases are diagnosed annually in the U.S. 2 Individuals with fair skin, a history of sun exposure or tanning bed use, and a genetic predisposition are at a heightened risk for developing skin cancer. As such, there is a critical need for targeted prevention and education efforts in these populations. 3
Several barriers hinder the widespread adoption of preventive and protective behaviors against skin cancer among U.S. adults. 4 Significant obstacles are present in the lack of awareness and misunderstanding regarding the severity of skin cancer and the effectiveness of prevention measures, such as regular use of sunscreen, wearing protective clothing, and avoiding peak sun exposure times. 4 Additionally, cultural preferences for tanned skin and aesthetic norms can undermine public health messages advocating for sun protection. 5 Economic factors also play a role, as not all individuals have easy access to or can afford sun protection products. 6 Moreover, existing disparities in education and healthcare access disproportionately affect lower-income and minority communities, further complicating efforts to promote and implement routine skin cancer prevention practices across the entire population. 6
A systematic review found that the perceived severity of UV harm was generally low in children, young adults, and older adults, which coincides with the belief of a “healthy tan.” 7 Based on the Health Information National Trends Survey (HINTS) data, Black Americans have a lower perceived likelihood of developing skin cancer in the future in comparison to White Americans. 8 Black Americans also less often considered regular skin examinations important in increasing the chance of finding skin cancer early. 8 Similarly, older adults and those with lower education levels were more likely to perceive their risk of future skin cancer as low. 8 Perceived absolute risk, perceived comparative risk, and worry about skin cancer development have all been individually associated with sunscreen use when controlling for race, gender, and education. 9 A survey of indoor tanning users found that increased perceived susceptibility to cancer, along with both cancer fatalism and external risk attribution beliefs, was generally associated with higher indoor tanning use. 10 However, high-quality research on the effectiveness of sunscreen in preventing skin cancer has been limited and has largely focused on White populations.11,12
Between 1990 and 2019, the burden of skin cancer in the United States, as measured by disability-adjusted life years (DALY), decreased for melanoma and remained stable for squamous cell carcinoma and basal cell carcinoma. 1 However, the estimated annual costs of skin cancer treatment rose from $8 billion to $8.9 billion between the years of 2012-2018. 13 Skin cancer is more prevalent among those older than 64-years-old than those aged 18 to 64, which is concerning due to the growing elderly population in the U.S. 13 While Black Americans are less likely to develop skin cancer, they are more likely to be diagnosed at a later stage compared to White Americans, which could contribute to higher mortality rates from skin cancer.14,15 When looking at individual behavior, an analysis of the costs of indoor tanning in the U.S. found that restricting indoor tanning for those under 18-years-old would prevent an estimated 61,839 cases of melanoma and 6735 deaths from melanoma. 16 As such, low-risk perceptions of skin cancer combined with low skin protection behaviors contribute to the burden of skin cancer in the U.S. today.
The Health Information National Trends Survey (HINTS) is a population-based survey collecting nationally representative data about changing patterns, needs, and opportunities in the healthcare field within the U.S. and Puerto Rico. Recently, the 2022 HINTS survey included survey items to measure risk perceptions about being at-risk of cancer and skin protection behaviors. Our study aims to provide a general overview of cancer risk perceptions and the prevalence of skin-protective behaviors to prevent sunburn and reduce the long-term risk of developing skin cancer. The results of the study derived from the HINTS 6 2022 dataset will guide future researchers in understanding nationally representative estimates for skin cancer risk perception and adoption of relevant protective behaviors and the sociodemographic variables associated with increased prevalence of reported sunburns.
Methods
For the purpose of this study, the data were obtained from the 2022 Health Information National Trends Survey 6 (HINTS 6). HINTS has been administered routinely by the National Cancer Institute (NCI) since 2003. The aim of HINTS is to synthesize data regarding the population’s attitudes toward health-related information, including their health behaviors, opinions, and knowledge, and is nationally representative of the American public.17,18 The target population of this survey is adult civilians who live in the United States. The version of the HINTS survey used in this study is the most recent iteration (HINTS 6) and was administered from March 7 – November 8, 2022, with the goal of reaching 7000 completed questionnaires. This version was selected for our study because of the inclusion of questions regarding risk perceptions about developing cancer, skin cancer protective behaviors, and the sociodemographic variables of interest for this topic.
Survey Administration
Based on the success of the mixed-method sample collection for HINTS 5, Cycle 3, HINTS 6 was offered to participants either online or on paper. Participants were randomly assigned one of three groups: to be offered both modes together (concurrently), or to be offered one mode before the other (sequentially, two groups). There was an unexpectedly low response rate to the traditional HINTS mailings, so HINTS 6 included a fourth mailing to a subsample of non-respondents. These non-respondents were selected using a systematic sampling approach. This extra mailing was conducted between September 27 and November 8, 2022, and included an additional payment incentive for completion. Additionally, for HINTS 6, certain PO Box addresses were excluded from the potential samples to improve the rate of deliverable mail.
Sample Selection
The HINTS 6 survey employed a two-stage sampling strategy. In stage one, a stratified sample was selected from a collection of residential addresses. Then, one adult was selected from each residence. This methodology differs from previous HINTS samples as it expands from two strata (high-minority and low-minority) to four strata (by additionally breaking out into rural and urban geographic areas). This further stratification provided a means to increase the number of rural samples collected. Data collection for HINTS 6 ran from March 7 to November 8, 2022. The survey was administered both online and by paper and was offered in English and Spanish. All groups received a $2 prepaid monetary incentive to encourage participation. Bonus incentive was offered to respondents in the control group to complete the survey online.
The HINTS 6 overall weighted response rate was 28.1%, but this differed significantly by stratum. On average, the high-minority strata had lower response rates than the low-minority strata (21% and 31%, respectively). There was no significant difference in response rates between urban and rural strata. The high-minority urban stratum had a slightly higher percentage of undeliverable households compared to all others. The total sample size for HINTS 6 was 6252.
Definitions and Measures
Three items were selected from the HINTS survey related to the survey respondents’ perception of cancer risk as follows: (1) Overall, how confident are you about your ability to take good care of your health?; (2) Compared to other people your age, how likely do you think you are to get cancer in your lifetime?; and (3) How worried are you about getting cancer? The answers to all three items were 5-point Likert scales. For confidence in ability to care for one’s health, the scale ranged from “Completely Confident” to “Not Confident at All.” Regarding likelihood of cancer compared to one’s age cohort, the scale was from “Very Unlikely” to “Very Likely,” with a separate response category if the respondent has already had cancer. When asked about worry level about getting cancer, survey answers ranged from “Not at all” to “Extremely.”
Questions related to sunburns within the past year were also selected from the survey, specifically: (1) After several months of not being in the sun very much, if you went out in the sun for one hour without sunscreen, a hat or protective clothing, what describes what would happen to your skin? (2) On the most recent time you were sunburned, what were you doing? and (3) Were you drinking alcohol at any of the times when you were sunburned? These were all characterized against a question of how many times the survey respondent had a sunburn, even a small portion of skin turning red or hurting for 12 or more hours, in the past year from too much sun exposure. This was originally a continuous variable but was redefined into the categories of no sunburns, 1-5 sunburns, or >=6 sunburns in the past year. The justification for these categories is that experiencing 6 or more blistering sunburns between the ages of 15 and 20 years has been shown to increase one’s melanoma risk by 80% and non-melanoma skin cancer risk by 68%. 19
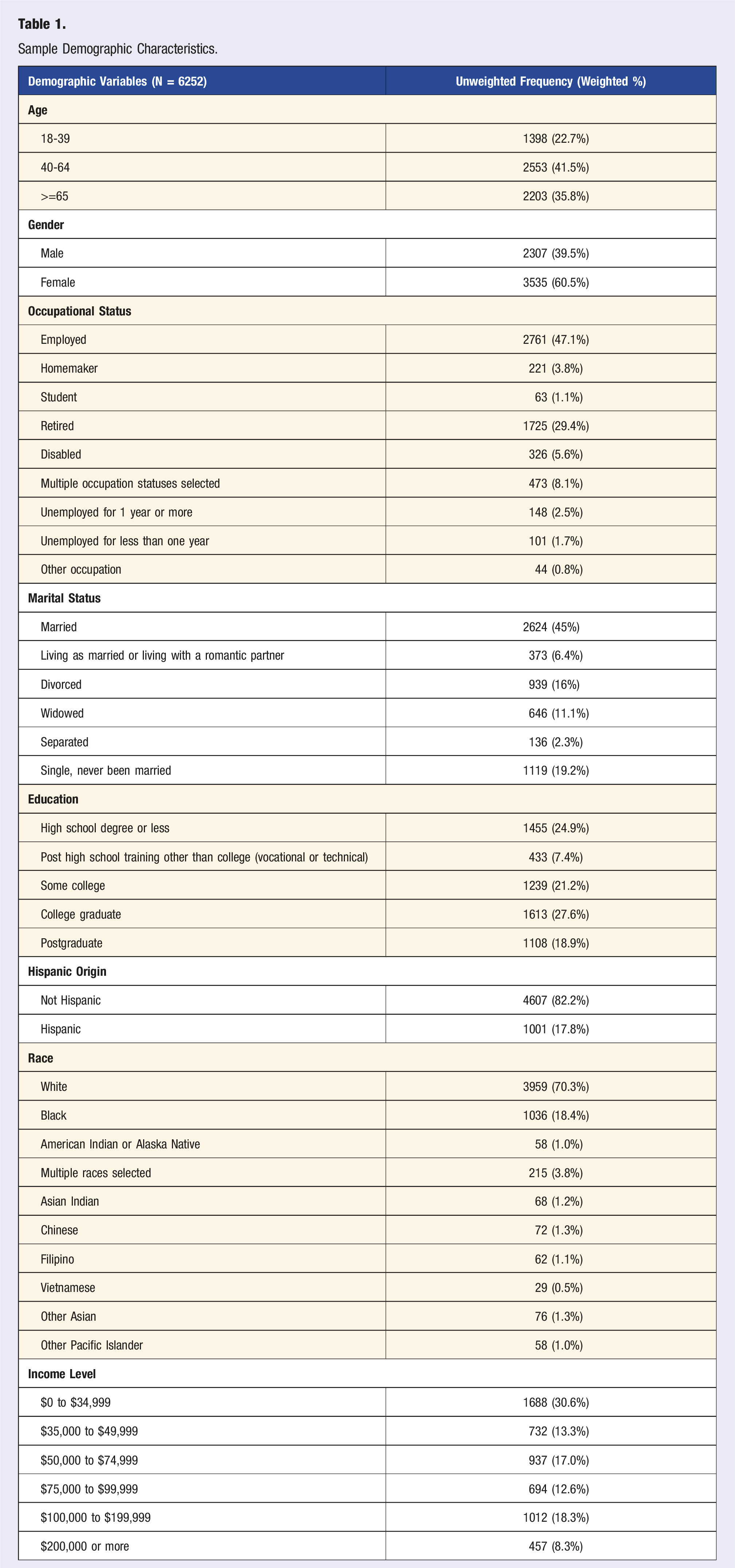
Sample Demographic Characteristics.
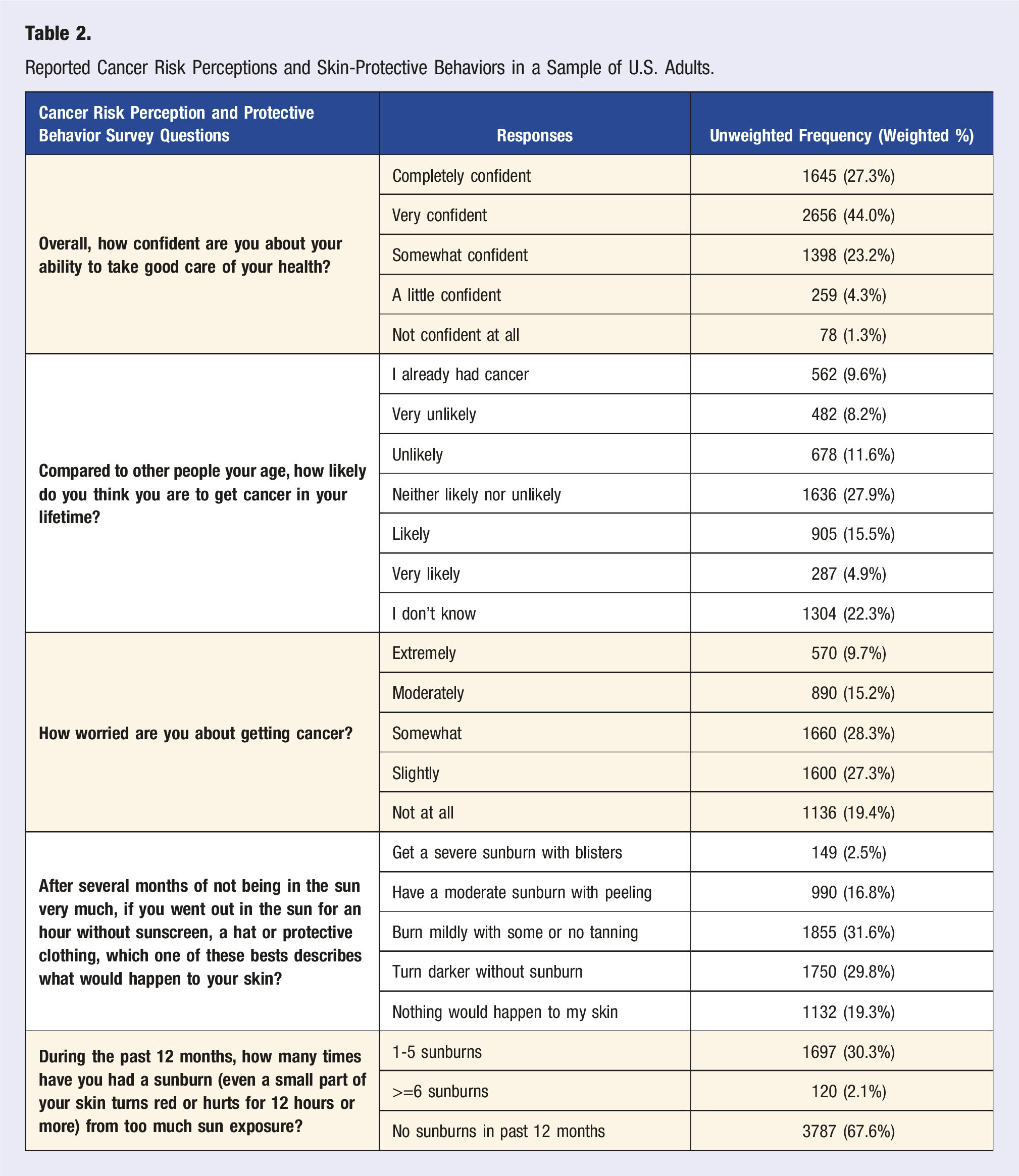
Reported Cancer Risk Perceptions and Skin-Protective Behaviors in a Sample of U.S. Adults.
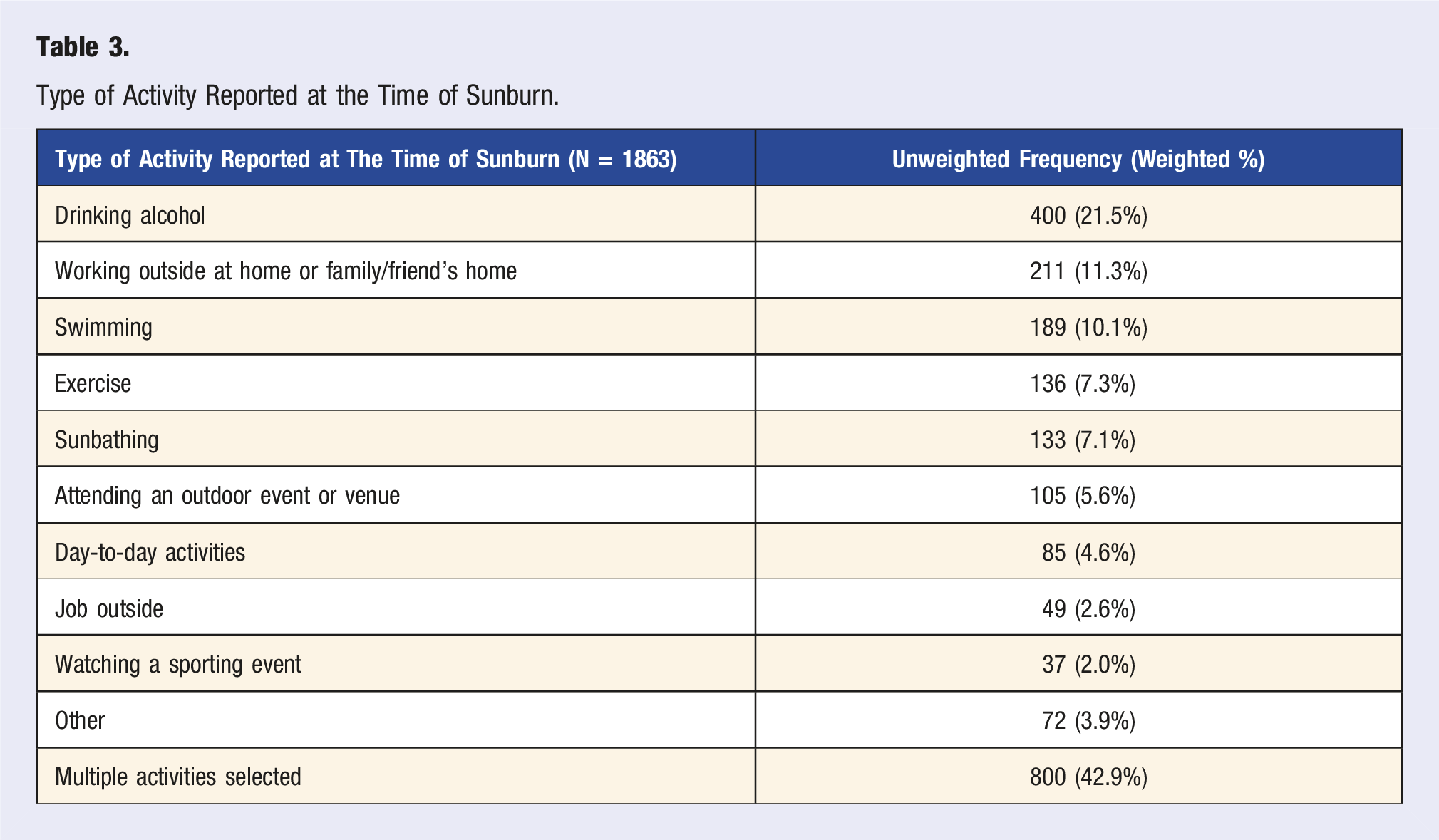
Type of Activity Reported at the Time of Sunburn.
Statistical Analyses
Data analysis was carried out with SPSS (version 29) using replicate weights. Descriptive statistics were first conducted to explore sociodemographic characteristics, cancer risk perceptions, and behaviors surrounding sunburns in our sample. Associations between number of sunburns (recoded into 0 sunburns, 1-5 sunburns, and >=6 sunburns) and sociodemographic variables were reported using chi-squared tests and multinomial regression analysis.
Results
Participant Characteristics
A total of 6252 participants participated in the survey. More than half of the respondents were female (60.5%), White (70.3%), and non-Hispanic (82.2%). The majority of respondents were 40 years old or older (77.3%), had more than a high school degree (75.1%), were married (45.0%), and were either employed (47.1%) or retired (29.4%). Over half of the respondents had a combined household income level above $50,000 (56.2%) with 17.0% reporting an income between $50,000 and $74,999, 12.6% between $75,000 and $99,999, 18.3% between $100,000 and $199,999, and 8.3% reporting $200,000 or more. Table 1 lists all sociodemographic characteristics for our study sample.
Cancer Risk Perceptions
When asked how confident patients felt about their ability to take good care of their own health, most respondents felt either very confident (44.0%) or completely confident (27.3%). Regarding how likely they felt they were to get cancer, most felt neither likely nor unlikely (27.9%) or were unsure (22.3%), and the majority were either somewhat (28.3%) or slightly (27.3%) worried about getting cancer. Only 9.7% (n = 570) reported being extremely worried about getting cancer (Table 2).
Sunburn and Skin Protection
More than half of the respondents felt that after not being in the sun very much and then spending an hour in the sun without any protection, they would either burn mildly with some or no tanning (31.6%), tan without burning (29.8%), or experience no change at all to their skin (19.3%) (Table 2). When asked how often they experienced a sunburn in the past 12 months, 2.1% reported experiencing more than 6 sunburns, 30.3% reported having between 1-5 sunburns, and 67.6% reported experiencing no sunburns (Table 2). Of the 33.80% (n = 1863) valid responses indicating they had experienced a sunburn, 21.5% (n = 400) reported drinking alcohol, 11.3% (n = 211) had been working outside, 10.1% (n = 189) were swimming, while 42.9% (n = 800) selected performing multiple activities during the most recent time they were sunburned (Table 3).
Multinomial Regression Analysis
Multinomial Regression of the Association Between Sociodemographic Characteristics and Number of Reported Sunburns.
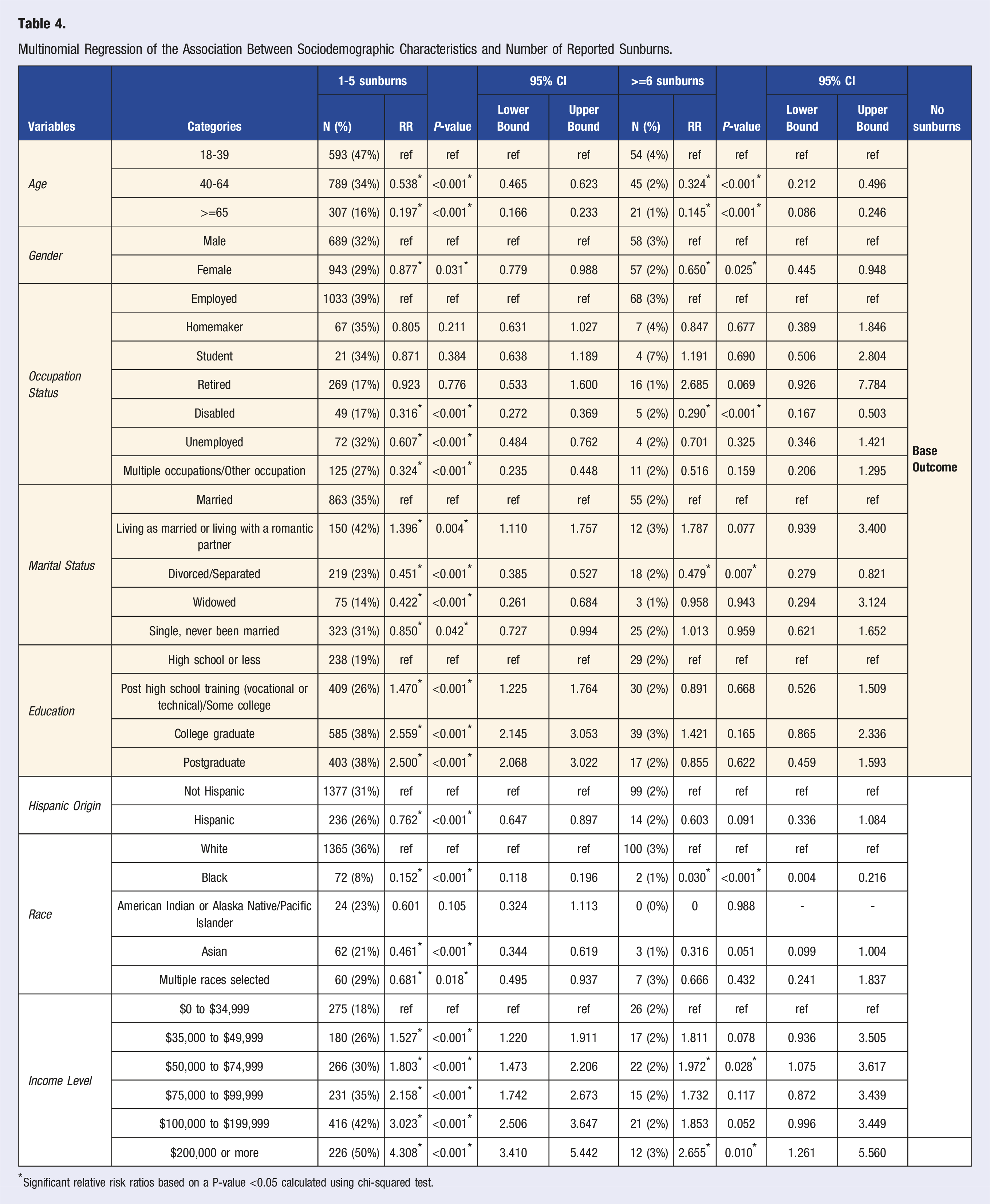
*Significant relative risk ratios based on a P-value <0.05 calculated using chi-squared test.
Discussion
The present research seeks to offer an understanding of the general perception of skin cancer risk alongside the prevalence of protective actions to prevent sunburns and reduce subsequent skin cancer risk in a national sample of U.S. adults. Using the HINTS 6 2022 dataset, our analyses provide nationally representative estimates that could help future researchers approximate skin cancer risk perception and the rate at which protective behaviors are used. Furthermore, our study identifies and reports the demographic factors associated with higher occurrence of sunburns and additionally examines the distribution of cancer risk perceptions alongside respondent characterizations of their sunburns and the environmental factors contributing to them.
Our results showed that perceptions are primarily intermediate when it comes to skin cancer risk perception, as only 9.1% (n = 570) reported being extremely worried about getting cancer, while the majority of respondents were either somewhat (26.6%) or slightly (25.6%) worried about getting cancer. It should be noted that most survey respondents were White (63.3%), and non-Hispanic (73.7%). These results highlight a need for public health programs or resources aimed toward cultivating additional awareness about skin cancer susceptibility and risk across all demographics. Several studies since 2010 have drawn attention to the low-risk perceptions held in ethnic minority groups within the U.S. despite their having a similar prevalence of skin cancer to other ethnic groups.8,20–22 One study performed in 2012 by Buster et al. determined that Black Americans and individuals without a college degree perceived themselves as having significantly lower risk of developing skin cancer. 8 This result is corroborated by a literature review performed in 2014 that found a significant trend across multiple studies, in that Black Americans and Hispanics had very low-risk perceptions when it came to the prospect of developing skin cancer. 21 The results of our study, in the context of similar research findings, further reinforce a long-standing need for public health interventions that effectively disseminate information on cancer susceptibility and risk across the spectrum of ethnic minority groups, especially in underserved communities within the U.S.
Our study also revealed that 27.1% of participants reported having experienced between 1-5 sunburns in the past 12 months. Previous studies have highlighted how sunburns are a major risk for developing melanoma and non-melanoma skin cancer. 23 It should be highlighted that there is a dose-response relationship between the number of sunburns and risk for developing skin cancer, notably melanoma. 23 Additionally, our study found that 6.4% (n = 400) of the participants reported consuming alcohol while being sunburned. Alcohol intake has been identified as a risk factor for sunburn in prior reports. 24 In a cross-sectional study, it was identified that heavier average alcohol use was positively associated with the number of sunburns an individual has experienced. 24 Our findings further solidify the correlation between risk of alcohol consumption and increased sunburn incidence.
Through a multinomial regression analysis, our study revealed statistically significant associations (P < 0.05) across all sociodemographic variables in relation to the reported number of sunburns over the past year. Social determinants of health, including race/ethnicity, sex, income, and employment status have been associated with risk for sunburn and skin cancer.8,25,26 While minority populations have a lower prevalence of sunburn, it has been identified that, through the acculturation process, Hispanics develop a higher perceived benefit of exposure to ultraviolet radiation, leading to an increased risk of sunburns. 8 While lower prevalence of sunscreen use has been identified among Black American and Hispanic individuals, factors such as sex, education, and income also affect one’s sunscreen practices. 8 Among Black Americans and Hispanics, female sex, education, income, and age were associated with increased sunscreen use. 8 Male sex and lower educational attainment has been previously associated with decreased odds of sun protective behaviors and increased risk for across the general population.25,26 In addition, income has also been associated with risk for sunburns, with higher income being associated with increased odds of frequent sunburn. 25 However, outdoor labor, which is perceived with lower socioeconomic status, is associated with increased sun exposure and increased risk for skin cancer. 27 In the United States, Hispanic individuals are overrepresented in the field of outdoor work and are therefore at even greater risk for UV exposure and increased skin cancer risk. 27
This study has several limitations related to its cross-sectional nature. The data was collected from the HINTS 6 survey, which was conducted with a nationally representative sample using a combination of structured interviews, either by phone or in person. Conducting the survey via random digit-dial telephone methods can result in low response rates and may reduce the validity of some baseline measurements. The sample predominantly consisted of White, non-Hispanic individuals, which may have influenced the findings related to risk perception and skin protection behaviors, along with the associations reported between sociodemographic variables and reported number of sunburns over the past year. Moreover, social desirability bias might have been introduced by having participants answer higher perceived risk of skin cancer and/or lower number of sunburns to align with the perceived correct societal responses. Furthermore, since HINTS is a cross-sectional study, causality cannot be established and the verisimilitude of the differences seen in the reported number of sunburns across social determinants of health (SDoH) variables requires additional study. Despite these limitations, this study is one of the few studies exploring associations between reported number of sunburns and sociodemographic characteristics, in addition to examining prevalence of protective skin behaviors adopted by the U.S. adult population in a nationally representative sample. Future research should attempt to further elicit the role of various SDoH in influencing skin protection behaviors, with the goal of developing interventions targeting specific groups identified as having higher risk of skin cancer, thus decreasing the socioeconomic burden of U.S. adult skin cancers.
Conclusion
Understanding perceptions of the risks of skin cancer and the prevalence of skin-protective behaviors is crucial in reducing the risk of developing skin cancer, especially among vulnerable groups. This study highlights the necessity of increasing awareness about skin cancer susceptibility and risk. All sociodemographic variables were significantly associated with the number of reported sunburns in the past year. Subsequent studies should build upon this foundation to explore how additional SDoH affect both the incidence of sunburns among ethnic minority and low-income groups and behaviors related to sunburn prevention. Understanding these factors is essential to any effort aimed at mitigating the various harms wrought by skin cancer among U.S. adults.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
