Abstract
Keywords
“In the present survey, the majority of respondents felt that fast-food restaurants should not be part of the hospital environment.”
Introduction
In 2017, the American Medical Association passed a resolution calling on health care facilities to improve the health of patients, staff, and visitors by: (a) providing a variety of healthy food, including plant-based meals, and meals that are low in saturated and trans fat, sodium, and added sugars; (b) eliminating processed meats from menus; and (c) providing and promoting healthy beverages. 1 Despite this policy, a large number of hospitals in the United States maintain contracts with fast-food outlets whose offerings are at odds with these nutritional principles.
Many foods served at fast-food restaurants are high in sodium, saturated fat, cholesterol, and added sugar and low in fiber. According to data collected from three U.S. national fast-food chains, common foods such as cheese and French fries are major contributors of sodium, while burgers and fried chicken are high in saturated fats. 2
Individuals who frequent fast-food restaurants are at increased risk of developing type 2 diabetes and coronary heart disease. 3 Eating a single weekly fast-food meal has been shown to be associated with a 20% increased risk of dying from heart disease, compared with avoiding such exposures. 4 Consuming four or more fast-food meals per week was associated with a nearly 80% increased risk.
The hospital food environment plays an important role for patients’ health outcomes and in modeling future dietary behavior 5 and is similarly important for the health of hospital staff and visitors. Hospitals also serve as educational setting for medical trainees. The extent to which healthful foods are or are not on offer in hospitals sends a message to medical students and others who are learning about health, nutrition, and medicine.
In a 2006 survey, 6 63% of medical schools maintained at least one fast-food outlet at one of their affiliated hospitals. In a 2011 survey of more than 100 hospitals, some hosted as many as five different fast-food outlets. 7
Objective
The purpose of this study was to determine the current prevalence and type of fast-food outlets at medical-school-affiliated hospitals and compare them to previous findings in order to assess progress in improving the hospital food environment.
Methods
Invitations to participate in Sogolytics surveys were distributed to medical students at medical and osteopathic schools, the American Medical Student Association, the Physicians Committee student database, and student interest groups. To complete the survey the student had to be a current student at a medical or osteopathic school and had to have studied at the school for at least a year in order to be familiar with the surrounding areas. The student members of the research team contacted any acquaintances who were currently medical students at other schools and who met the guidelines to complete the survey. For the remaining medical schools for which neither student team member had known acquaintances, the team members contacted leaders in each medical school’s student government and asked them to complete the survey if they fulfilled the aforementioned guidelines or to distribute the survey to a student who satisfied the guidelines. The contact information for the students in student government were obtained from email addresses posted on school websites or by calling and speaking to staff regarding email addresses for student government members.
The survey asked medical students to list up to six of their main teaching hospitals or medical centers through which they rotated and to identify fast-food restaurants in each hospital. For the purpose of this survey, a fast-food restaurant was defined by the researchers, based on a previous definition, as a restaurant that fulfills two or more of the following criteria: expedited waiting times, minimal to no wait staff, expected payment before receiving food, and the option of takeout. 8 Those who reported there were no fast-food restaurants located in the hospitals affiliated with their schools were not required to name these hospitals. The survey provided a list of popular fast-food chains to select and instructed users to fill in additional brand-name fast-food restaurants not listed. Data were collected from March through July 2022. Participants were also asked if they agreed or disagreed with the statement, “It is acceptable for fast-food restaurants to be in hospitals.”
The study protocol and survey were submitted and granted exemption from International Review Board oversight.
Results
Of 192 medical and osteopathic schools, 255 individual completed surveys were received from 146 schools.
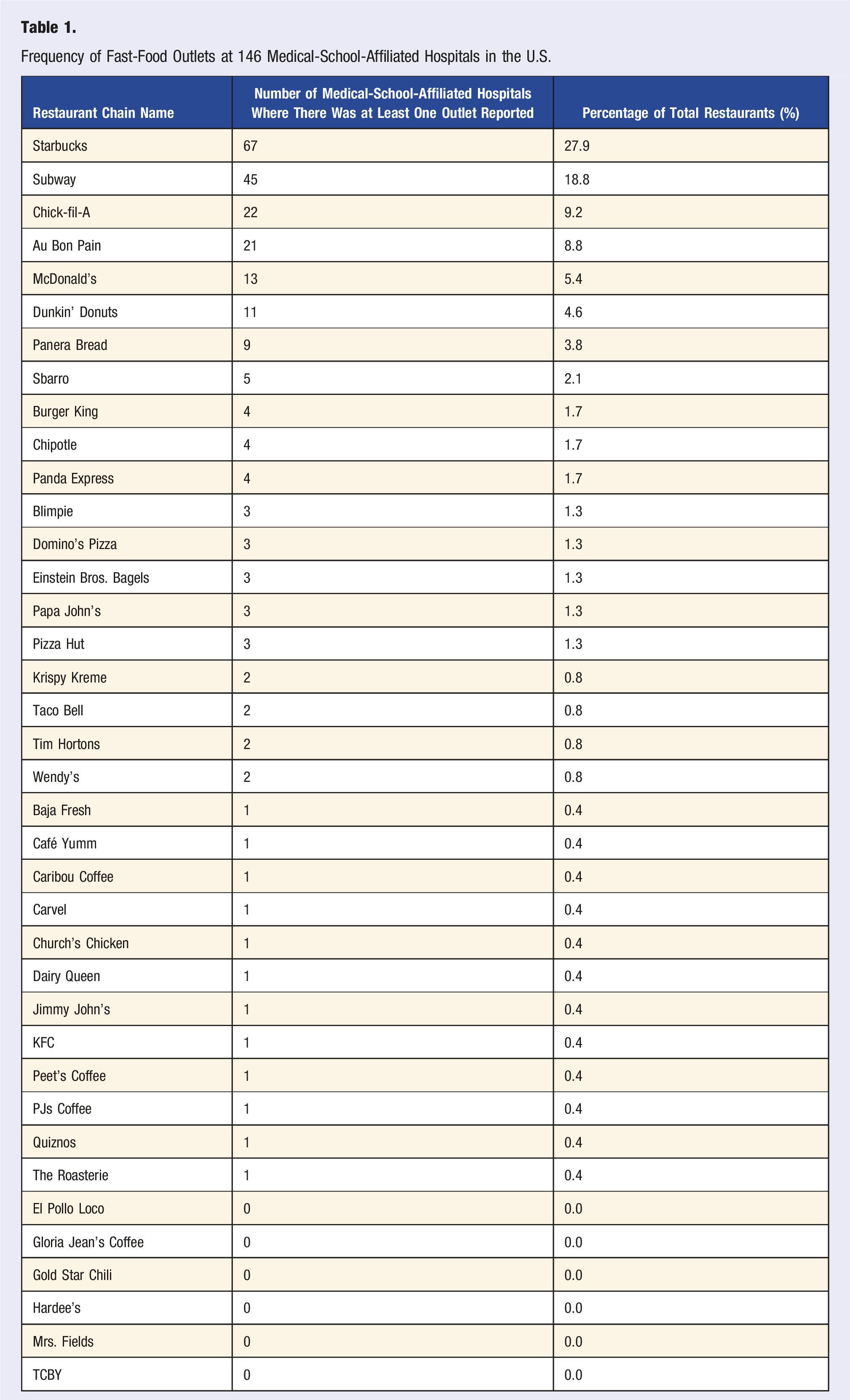
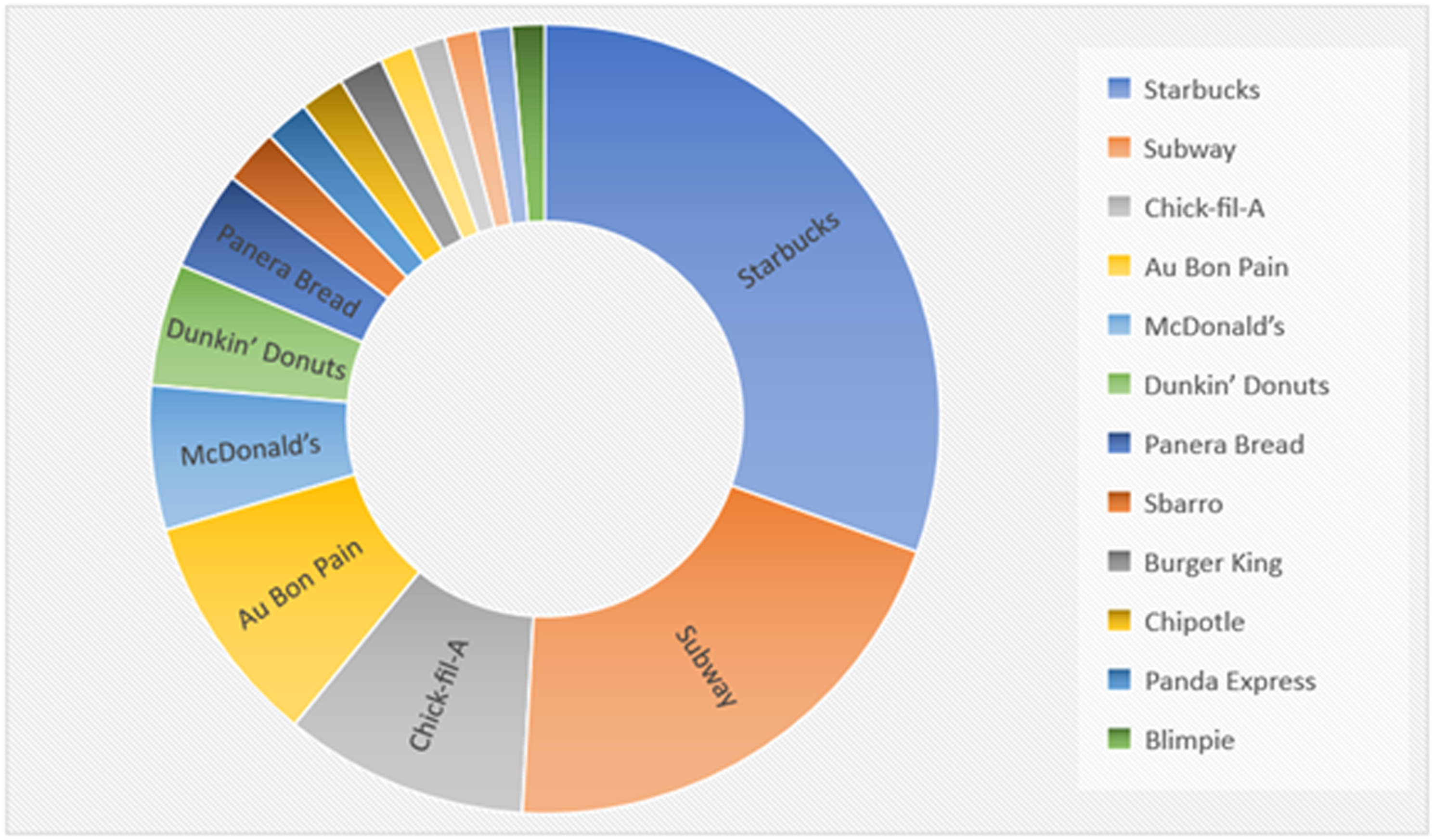
Of the 146 medical schools, 101 schools (69.2%) reportedly hosted at least one fast-food restaurant associated with the hospitals at which students rotate, these include 15.1% schools that gave a mixed response to the question if fast-food restaurants are present in any affiliated hospitals. 45 schools (30.8%) reported no fast-food restaurants in any affiliated hospitals, which is similar to previous research findings (Figure 1). Table 1 shows the prevalence of fast-food restaurants reported in at least one medical or osteopathic school-affiliated hospital. The five most common fast-food restaurants reported were Starbucks (27.9%), Subway (18.8%), Chick-fil-A (9.2%), Au Bon Pain (8.8%), and McDonald’s (5.4%) (Figure 2). Prevalence of fast-food restaurants in medical-school-affiliated hospitals. Frequency of Fast-Food Outlets at 146 Medical-School-Affiliated Hospitals in the U.S. Distribution of fast-food outlets reported in at least one medical-school-affiliated hospital.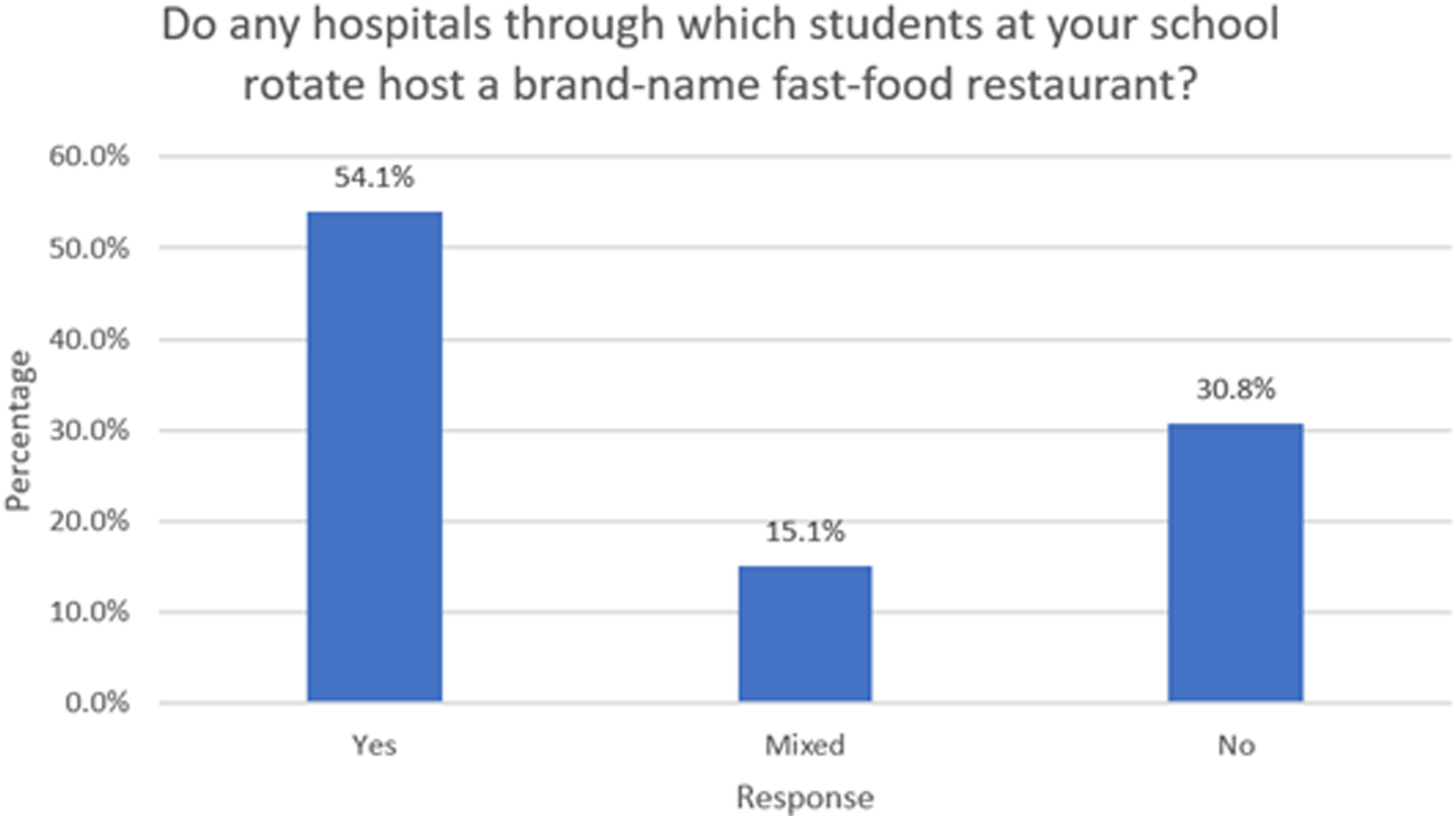
Regarding the statement, “It is acceptable for fast-food restaurants to be in hospitals,” 27.8% of students strongly disagreed, 29.0% somewhat disagreed, 16.9% neither agreed nor disagreed, 21.2% somewhat agreed, and only 5.1% strongly agreed (Figure 3). Acceptability of fast-food restaurants in hospital.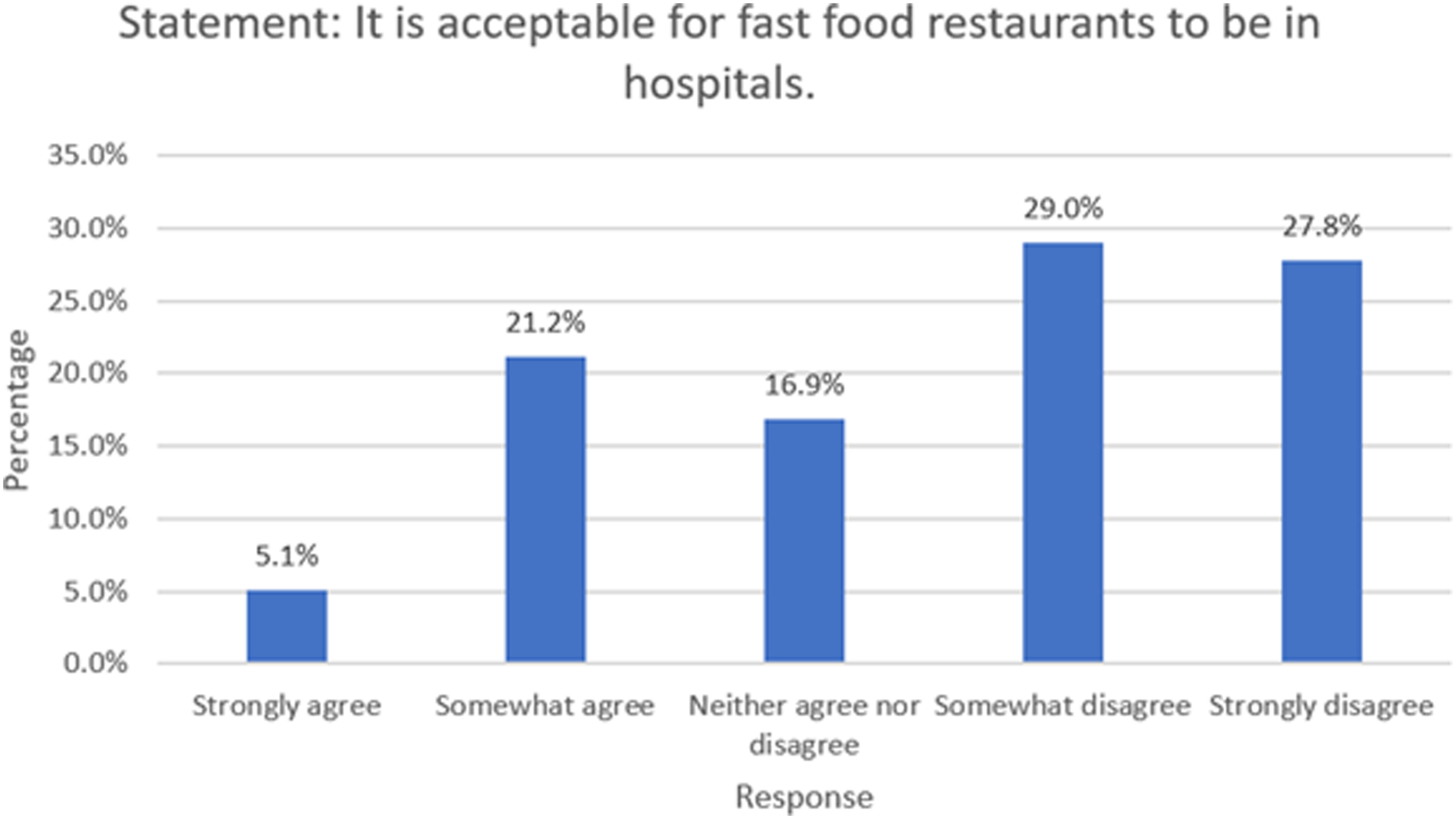
Discussion
Fast-food outlets are common at hospitals affiliated with U.S. medical schools. Despite increasing evidence of associations between fast-food consumption and medical conditions, the current finding that 69.2% of medical and osteopathic schools host at least one brand-name fast-food restaurant at their hospitals is similar to findings in 2006, 6 when 63% of medical schools had affiliated fast-food outlets. Many U.S. hospitals host more than one fast-food outlet.
The Impact of Fast-Food Consumption on the U.S. Population and Public Health
Fast-food consumption and out-of-home eating behavior is linked to higher energy and fat intake and lower intake of certain micronutrients, particularly vitamin C, calcium, and iron. 9 The majority of Americans do not consume sufficient amounts of fruit and vegetables 10 and the availability of unhealthful food and drinks negatively influences food choices, potentially crowding out more healthful choices. 11
Frequent consumption of fast-food is linked to obesity, dyslipidemia, diabetes, and heart disease, the latter two of which are among the top 10 causes of death in the U.S., according to the Centers for Disease Control and Prevention. 12
A report published in The Lancet Public Health in 2020 found that 27% of health care spending was attributable to modifiable risk factors relating to diet and lifestyle. 13 Of this, $238.5 billion was attributable to a high body mass index and $171.9 billion to a high fasting plasma glucose.
The consumption of fast-food is therefore not only an individual health issue, but also a public health and economic issue.
Colorectal cancer is a leading cause of cancer death among young Americans, aged 20-39 years. 14 Processed and red meat, commonly served at fast-food restaurants, contribute to this problem and are classified as Group 1 and 2A carcinogens, respectively, according to the World Health Organization and the International Agency for Research on Cancer.
The Impact of Fast-Food Restaurants in Hospitals on Consumer Perception
Having a fast-food restaurant on-site in hospitals affects people’s frequency of consumption and perception of the healthfulness of the foods served. A study published in Pediatrics found that when there was a McDonald’s operating inside a hospital, parents and their children who were attending the hospital as outpatients were more likely to purchase McDonald’s, and four times more likely to consume fast-food the day of their appointment compared with those attending a hospital that did not have McDonald’s onsite. 15 Visitors to a hospital that had a McDonald’s onsite were also more likely to rate McDonald’s food healthier. Hospitals that have fast-food restaurants onsite are inadvertently encouraging unhealthy eating behaviors.
In 2021, the World Health Organization urged governments to ensure healthy food access and to limit the sale of fast-foods in public facilities (e.g., hospitals). 16 Similarly, the American Medical Association has called for healthful food in health care facilities for the benefit of patients, staff, and visitors. Despite these policies and abundant evidence of deleterious effects of unhealthful foods, such products are offered widely in health care settings.
A survey of junior doctors at Oxford University Hospitals found that 97% agreed that hospitals should set an example of a healthy living and act as a positive role model. 17 Similarly, in the present survey the majority of respondents felt that fast-food restaurants should not be part of the hospital environment.
The Impact of Fast-Food Access on Health Care Professionals
The effects of unhealthful food in hospitals extend to health care professionals. A survey of registered nurses in North Carolina found that the abundance of unhealthful options and fast-food restaurants in a hospital posed a significant barrier to healthy eating, particularly since unhealthful options were often particularly affordable. 18 Another survey of 234 health care professionals found there was a 58% increase in fast-food consumption during the COVID-19 pandemic. 19 Easy accessibility to fast-food outlets at work has been associated with greater odds of being obese. 20
The Impact of Health Care Professionals’ Habits on Patient Outcomes
Health care workers’ habits may not only affect their personal health but also their patients’ health. Approximately one third of health care providers struggle to provide counseling to their patients for conditions they themselves struggle with, such as obesity and weight loss. 21 Physicians with overweight and obesity also report a lower perceived self-efficacy and confidence in providing lifestyle change counseling. 22 Patients have been found to have a mistrust of doctors who are overweight, to be less inclined to follow their advice, and to be more likely to change health care providers, according to the results of a 2013 survey. 23
Looking Forward
Given the prevalence of fast-food restaurants in U.S. hospitals, the apparent solutions include (1) encouraging fast-food chains to provide healthful menu options or (2) replacing such restaurants with others providing healthful choices. Indeed, some fast-food chains have made progress, incorporating various cholesterol-free products.24-26 Food manufacturers have developed a variety of plant-based burgers and similar products and have funded studies suggesting potential nutritional advantages, such as reduced body weight and low-density lipoprotein cholesterol, 27 and improved gut health.28,29 Whole grains and legumes are readily incorporated in restaurant offerings and are associated with improved health outcomes when compared with animal products.30,31
Limitations
This study has its limitations. Given that those who reported no fast-food restaurants in their medical-school-affiliated hospitals were not required to name these hospitals, we could not confirm whether there were discrepancies between hospitals where fast-food restaurants were and were not reported. The responses recorded were all self-reported by medical students and not validated through calling or visiting the hospitals, therefore the accuracy of each response could not be authenticated. The survey links were shared through connections to the Physicians Committee and the researchers, which may have led to a selection bias, and thus the results may not be a complete representation of all osteopathic and medical-school-affiliated hospitals. Further research is required to confirm these findings.
Conclusion
Despite wide recognition of their potential adverse influences on health, fast-food outlets remain prevalent in hospitals affiliated with U.S. medical schools. Hospitals should take steps to improve or eliminate these facilities.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Neal Barnard is the founder and president of the Physicians Committee for Responsible Medicine, which is a non-profit organization that promotes plant-based nutrition, however, he does not receive compensation for this role. He writes books and articles and gives lectures related to nutrition and health and has received royalties and honoraria from these sources. Zeeshan Ali, Anna Herby, and Roxanne Becker are all full time employees with the Physicians Committee for Responsible Medicine and receive compensation for their work. Roxanne Becker is also the vice president of the South African Lifestyle Medicine Association which promotes plant-based nutrition in South Africa; however, she receives no compensation for this role.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
