Abstract
Background: Whole-food, plant-based (WFPB) dietary patterns can be used as a lifestyle modification to lower blood pressure and lose weight. This study aimed to observe the effects of WFPB dietary patterns and improve nutrition education in medical school. Methods: Forty-six medical students participated in the four-week Plant Plunge challenge, which consisted of a pre- and post-challenge health screening, weekly nutrition seminars, and the personal challenge to eat more WFPB. Afterward, an anonymous survey was sent to participants to analyze nutrition education quality in medical school. Results: The Wilcoxon Signed Rank test indicated statistically significant improvement in weight and blood pressure (BP) (N = 33). The median (interquartile range) difference in weight from pre- to post- was −.9 (−2.2, .0, P < .0461) pounds, whereas the differences in systolic and diastolic BP were −5.0 (−9.0, −.5, P < .049) and −7.0 (−11.0, −2.0, P < .0037) mmHg, respectively. Participants were significantly more likely to advocate for the integration of nutrition information into the medical school curriculum (P = .0162). Conclusions: Short-term lifestyle modifications with WFPB dietary patterns help reduce weight and BP. Incorporating nutrition seminars in medical education may improve long-term patient outcomes.
“Participants who adhered to the program, as self-reported, demonstrated statistically significant improvements in weight and blood pressure.”
Introduction
Dietary modifications serve as a strong lifestyle modification for the foundation of preventive medicine.1–3 The Standard American Diet (SAD), which is high in fats, refined carbohydrates, sugar, sodium, and calories, has long been implicated in the development of obesity and chronic diseases such as cardiovascular disease, diabetes, high cholesterol, high blood pressure, and even cancer.1,2 Recent evidence from a systematic review and meta-analysis highlights the profoundly negative impact the pathophysiology behind obesity has on health. The likelihood of experiencing multiple chronic health conditions increases by 26% in individuals who are overweight and doubles in individuals with obesity. Since 1975, the global obesity rate has tripled, with 39% of adults globally considered to have obesity, and expected to continue to rise. 4 Not surprisingly, the chronic diseases associated with obesity continue to rank as the leading chronic diseases in the United States, and their rates are expected to rise concurrently with the projected rise in obesity rates. These conditions can be prevented with modifiable lifestyle factors, such as dietary patterns and physical activity.1–3
Whole-food, plant-based (WFPB) dietary patterns can be omnivorous but the foundation is composed of foods that are derived from plants, which includes fruits, vegetables, legumes, whole grains, nuts, and seeds. 2 Unlike other dietary patterns, such as vegetarianism or veganism, WFPB diets do not limit individuals from consuming animal products. Rather, they encourage individuals to increase the proportion of foods from plant sources and to limit processed foods.2,3 Current literature suggests that incorporating healthy dietary patterns rather than single food groups or nutrients is more beneficial to prevent cardiovascular disease, aligning with the philosophy of WFPB diets.5,6 Previous studies have demonstrated that WFPB dietary patterns can lead to weight loss and improved weight status, with an emphasis on the necessity for more diverse population studies.7,8 Further research has indicated that adherence to WFPB dietary patterns is associated with a lower risk of all-cause mortality and coronary heart disease mortality. 9 WFPB dietary patterns have also been shown to lower the risk of developing type 2 diabetes, effectively contributing to weight management.10,11 Collectively, these findings underscore the potential of WFPB dietary patterns in improving health outcomes and emphasize the need for continued research in this area.
Numerous reputable organizations, including the American Society for Clinical Nutrition and the American Medical Student Association, emphasize the essential nature of nutrition training in medical education. 12 However, studies have shown that there is still a need for improvement in nutrition education within medical schools, with a call for institutional commitment to make nutrition education compulsory, establishment of nutrition competencies, and funding for innovative curriculum initiatives. 13 Despite the demand from medical students to receive nutrition education, the status of nutrition education in the medical curriculum remains largely neglected. 14 Although the National Academy of Sciences recommends medical students receive at least 25 hours of nutrition education, many institutions fall short of this recommendation, limiting primary prevention education for student doctors. 15 “In the USA, the time devoted to nutrition during medical school is limited, with an average of 19 hours divided over 4 years.”14,16 One review discussed the distribution of 30 nutrition education learning experiences offered in various medical schools, revealing integrated lectures made up 33%, sessions made up 57%, and electives made up 10%, which although provided diversity of learning experiences across many institutions, still lacked consistent nutrition objectives across institutions. 17 The Nutrition Education in Medical Schools project found knowledge gaps between medical school curricula in nutrition education and pushed for a multidisciplinary approach to teach basic, applied, and clinical nutrition. 18 Furthermore, the lack of robust nutrition education in medical undergraduate programs is seen as a barrier to improvements in nutritional care within medical practice. 19 It is evident that nutrition education should be an essential component of medical education and medical practice, as it can positively impact patient outcomes.20,21 However, the current status of nutrition education is perceived as insufficiently incorporated into medical education, regardless of country or year of medical education. 12 Ultimately, there are proposed recommendations to the Liaison Committee on Medical Education and Association of American Medical Colleges, 22 which will hopefully lead to standardized nutrition objectives in medical school in the United States.
Dietary patterns in medical students have been explored, where one study found that only 20% of first and third year medical students ate 40 grams of fruits and vegetables every day, which is the recommendation by the World Health Organization, and medical students had dietary patterns high in animal fats and salt, which are known contributors to chronic diseases. 23 During the COVID-19 pandemic, one study reported statistically significant increases in fast food consumption, energy drink consumption, and decreased physical activity. 24 To help address these recent lifestyle changes, nutrition and lifestyle interventions may be helpful to promote wellness in these areas. One experimental study reported statistically significant improvements in nutrition care knowledge, self-efficacy in nutrition care, increased consumption of fruits and vegetables, and dietary diversity after attending a 4-week nutrition education intervention. 25 Our study hopes to integrate this information to not only improve health outcomes with incorporating more WFPB dietary patterns, but also hope to provide data to improve the diversity of experiential nutrition education in medical school.
Chickpea and Bean is a non-profit organization based in Detroit whose mission is to educate people about the power and benefits of a WFPB lifestyle through in-person nutrition seminars via the Plant Plunge. The Plant Plunge is an initiative that Chickpea and Bean pioneered as a way to actively engage individuals in incorporating a plant-based lifestyle. It is a four-week, self-paced program with 3 objectives: (1) a personal challenge to incorporate more WFPB dietary patterns during the duration of the Plant Plunge, (2) attend one-hour, weekly nutrition seminars that educates participants about important nutrition information (including how to read and understand food labels, identifying nutrient-dense foods, incorporating healthy substitutes, and showcasing health narratives of participants who successfully reversed chronic diseases by living a WFPB lifestyle), and (3) directly measure the short-term benefits of a WFPB lifestyle by offering health screenings, which include blood pressure, weight, serum glucose, and lipid panel, to participants before and after taking part in the Plant Plunge.
In this single institution observational study at Oakland University William Beaumont School of Medicine (OUWB SOM), we observed the short-term health effects of incorporating WFPB lifestyles and weekly nutrition seminars as part of the Plant Plunge, hosted by Chickpea and Bean. We also wanted to address medical students’ perceptions of the quality and quantity of nutrition education in medical school, in order to promote stronger primary prevention in the education of student doctors. Despite the vital role nutrition plays in maintaining health, medical students do not receive the level of education needed to adequately counsel patients on this topic in their future careers. 11
Aim 1: Determine the clinical biomarker changes in participants who incorporated more plant-based meals in their diets for 4 weeks, including blood pressure, weight, lipids, and blood glucose.
Aim 2: Determine the quality of nutrition education presented during the Plant Plunge and assess the need for more supplemental nutrition education in the medical school curriculum.
We hypothesized that a majority of the Plant Plunge participants would see a decrease in at least one of the following categories over the course of the four-week program: blood pressure, weight, blood glucose, total cholesterol, high-density lipoproteins (HDL), triglycerides, low-density lipoproteins (LDL), or non-HDL cholesterol. We also hypothesized that medical students would be exposed to new nutrition information, thereby promoting preventive health care.
Materials and Methods
Plant Plunge
This was a single institution observational study on the effects of WFPB dietary patterns on clinical biomarkers and the efficacy of supplemental nutritional seminars in medical school provided by Chickpea and Bean via the Plant Plunge challenge. The purpose of the Plant Plunge was to encourage and empower individuals to incorporate more WFPB meals into their diets over a 4-week period and assess the potential benefits of WFPB dietary patterns on their health. The Plant Plunge consisted of a pre- and post-challenge health screening; 4, weekly, 1-hour nutrition seminars that included a plant-based lunch; and a self-paced challenge component that highly encouraged participants to adhere to WFPB dietary patterns for 4 weeks. The nutrition seminars took place in person at OUWB SOM in a lecture-style presentation, with Chickpea and Bean leading the seminars through a PowerPoint. Week 1 of the Plant Plunge nutrition seminars topics included: personal health narratives of individuals who reversed chronic diseases such as Type II Diabetes Mellitus, hypertension, and obesity with switching to a WFPB lifestyle and research studies that support the implementation of a WFPB lifestyle. Week 2 of the Plant Plunge nutrition seminar topics included how to read nutrition labels, how to shop for plant-based substitutes, and how to read ingredient labels to ensure participants purchase nutrient-dense foods. Week 3 of the Plant Plunge nutrition seminar topics included WFPB recipe examples and the cost of WFPB diets compared to the cost of groceries for an average Standard American Diet. Week 4 of the Plant Plunge nutrition seminar topics included a guest speaker from an Integrative Medicine-certified Internal Medicine physician on how they practice lifestyle medicine with their patients. Participants were encouraged to ask questions throughout the presentations and at the end of the nutrition seminars to ensure full understanding and participation.
The health screenings collected participants’ weight, blood pressure, blood glucose, and fasting lipid panel (total cholesterol, high-density lipoproteins (HDL), triglycerides, low-density lipoproteins (LDL), and non-HDL cholesterol). After completion of the 4-week Plant Plunge program, an anonymous survey was sent out to all forty-six participants to assess the effectiveness of the 4 weekly nutritional seminars presented by Chickpea and Bean.
Participants
The Lifestyle Medicine Interest Group at OUWB SOM marketed the Plant Plunge for medical students to attend and participate in the challenge via posting flyers, emailing members on the email listserv for the Lifestyle Medicine Interest Group, and posted advertisements in GroupMe and Facebook pages for all medical students at OUWB SOM. All medical students were encouraged to participate and attend as many nutrition seminars as possible, even if they could not attend all 4 in-person nutrition seminars. There was no cost to participate in the Plant Plunge. Forty-six students at OUWB SOM voluntarily signed up to participate in the nutrition seminars and attended all 4 in-person nutrition seminars and self-paced WFPB challenge, and thirty-three of those students opted to participate in both the pre-Plant Plunge and post-Plant Plunge health screening. At each nutrition seminar, there were over 50 participants who attended, which indicated that medical students encouraged other peers to attend, even if they did not formally sign up to attend initially. A placebo group was not included in this study, as this program and study was intended to be a preliminary study to gather as many medical students to participate in the Plant Plunge and eat as many WFPB meals as possible this year, and we did not want to exclude any participation in order to implement a placebo group.
Health Screening Data Analysis
Participants who signed up to attend the Plant Plunge seminars were offered the opportunity to obtain a pre- and post-health screening. Executive board members of the Lifestyle Medicine Interest Group were trained on how to collect health screening data by Chickpea and Bean on January 30, 2023. The same executive board members were stationed at the same health screening station at the Pre- and Post-Health Screening to ensure consistency in data collection. Weight was collected using an electric scale, blood pressure was obtained using manual blood pressure cuffs, and blood serum labs were collected using 10989 Cassette Test Lipid Profile Cholestech LDX (BX 10). Pre-Plant Plunge health screening took place on February 3, 2023 at OUWB SOM and the Post-Plant Plunge health screening took place on March 3, 2023. Participants were given their Pre-Plant Plunge and Post-Plant Plunge health screening information and were educated on what abnormal values may indicate.
Survey Data Analysis
Forty-six participants signed up to participate in the Plant Plunge prior to the Pre-Health Screening, where their email addresses were collected. An anonymous survey was sent to these forty-six participants at the conclusion of the Plant Plunge to obtain opinions regarding their perspectives on implementing more nutrition seminars in medical school, the quality of the information presented at the Plant Plunge nutrition seminars, and participants’ experience eating more WFPB during the duration of the Plant Plunge challenge. For each survey question, a Likert scale ranging from 1 to 5 (1 - strongly disagree, 5 - strongly agree) was assigned to statements in the anonymous survey regarding the information presented at the Plant Plunge and statements about implementing more nutrition seminars in the medical school curriculum. The Likert scale responses were then broken down into 2 groups: (1) Agree group (includes responses of agree and strongly agree) and (2) Disagree group (includes responses of neutral, disagree, and strongly disagree). An equal variance two-sample t test was then used to compare these 2 groups, with a Fisher exact P-value calculated for statistical significance.
Statistical Analysis
The Wilcoxon Signed Rank test was used to analyze the mean health screening data. In this study, participants self-reported adherence to WFPB diets, allowing for the Wilcoxon Signed Rank Test to more accurately compare the mean Pre- and Post-health screening data. Likert scale survey responses were assigned numerical values (1 - strongly disagree to 5 - strongly agree) and the mean and standard deviation were calculated based on a normal distribution.
Institutional Review Board
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Institutional Review Board of Oakland University (IRB#: IRB-FY2023-222 on March 22, 2023). Informed consent was obtained from all subjects in this study.
Results
Health Screening Data Indicated Improved Blood Pressure and Weight Loss from Adhering to WFPBD During the Plant Plunge
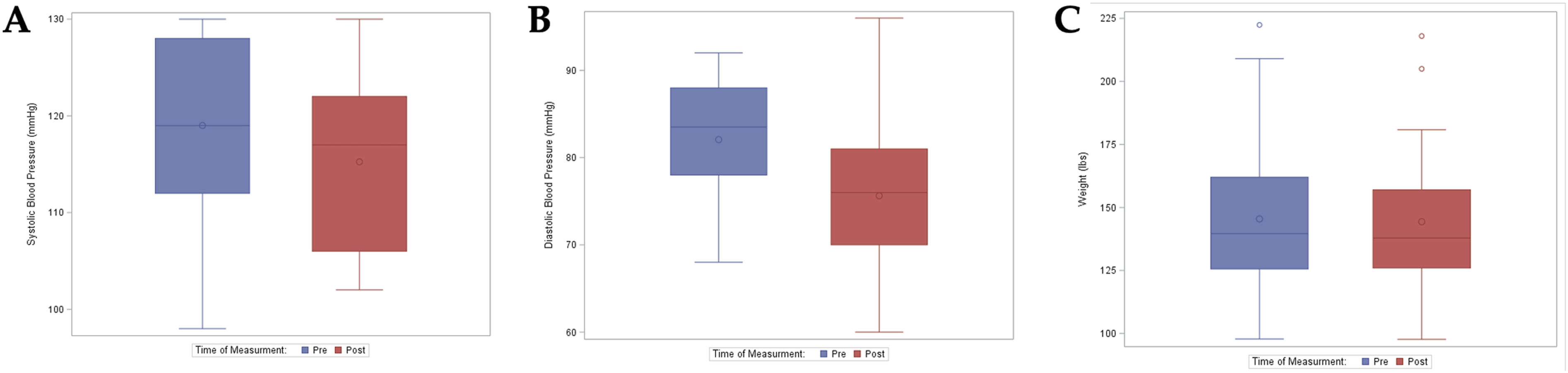
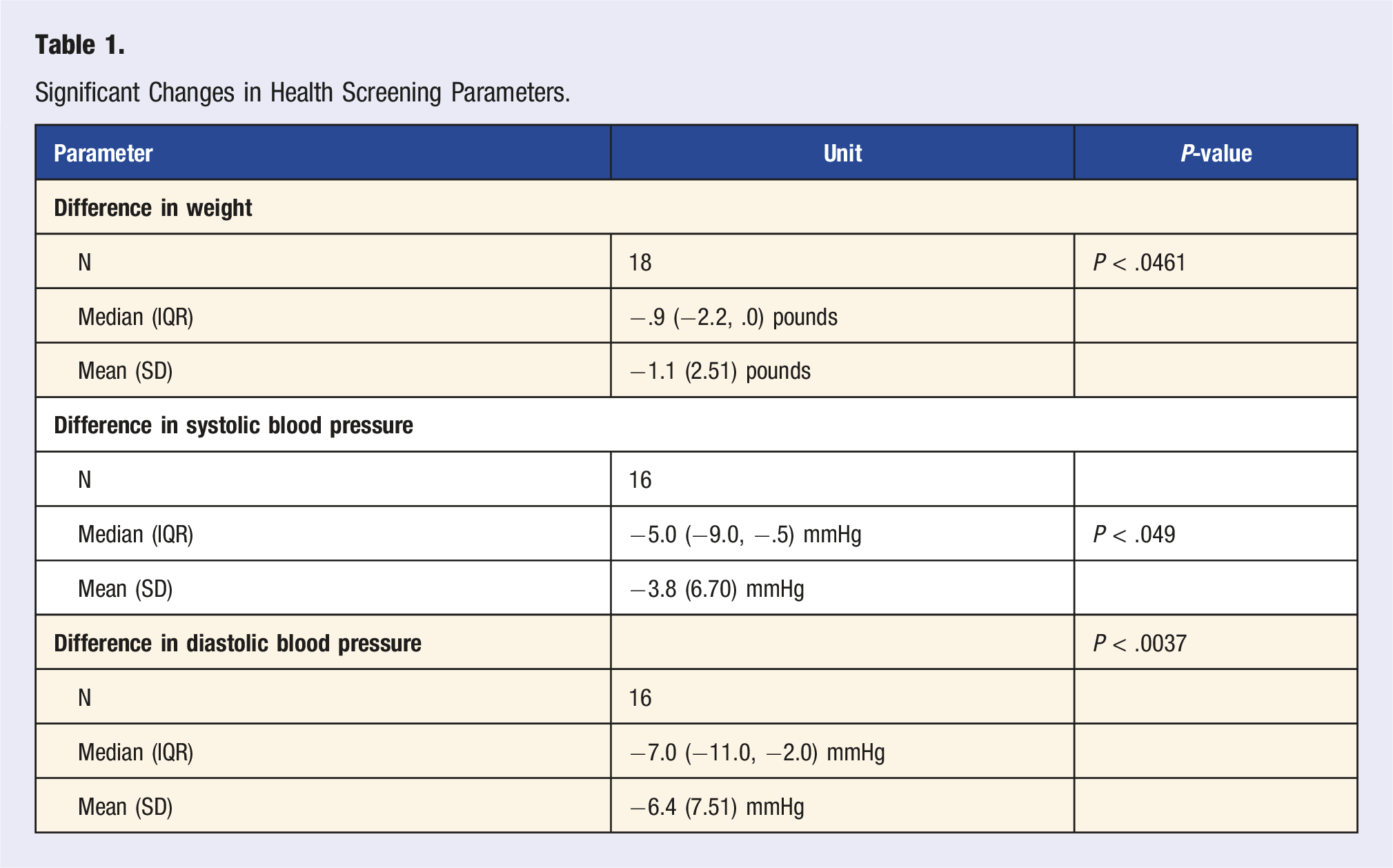
Thirty-three individuals participated in both the Pre- and Post-Health Screening. The Wilcoxon Signed Rank test was used to compare the paired pre- and post-Plant Plunge health screening data. The results indicated that participants had marginally statistically significant improvement on the following clinical biomarkers: weight, systolic blood pressure and diastolic blood pressure (Figure 1, Figure 2). The median (interquartile range) difference in weight from pre to post was −.9 (−2.2, .0, P < .0461) pounds, whereas the differences in systolic blood pressure and diastolic blood pressure from pre to post was −5.0 (−9.0,-.5,P < .049) and −7.0 (−11.0, −2.0, P < .0037) mmHg, respectively (Figure 2, Table 1). Our data demonstrate that achieving short-term goals, such as reducing cholesterol levels, blood pressure, or weight in just 4 weeks, can be accomplished by transitioning to a WFPB lifestyle. While we did not observe statistically significant changes in some of the other health statistics, such as HDL and LDL cholesterol levels, we did notice an overall trend towards improvement in these categories (Figure 1). It is important to note that participation in the Pre- and Post-health screening was heavily encouraged, but voluntary, and not all participants were able to attend both data collection points, resulting in a lower-than-expected sample size for each variable. It is also important to note that participants were asked to fast prior to both data collection times, but not all participants were able to fully adhere to this recommendation, as we were limited to scheduling these health screening times around the medical school lecture schedule. Participants’ overall change in health screening parameters from pre- and post-health screening data. Pre-health screening and post-health screening data of (a). systolic blood pressure, (b). diastolic blood pressure, and (c). weight. Significant Changes in Health Screening Parameters.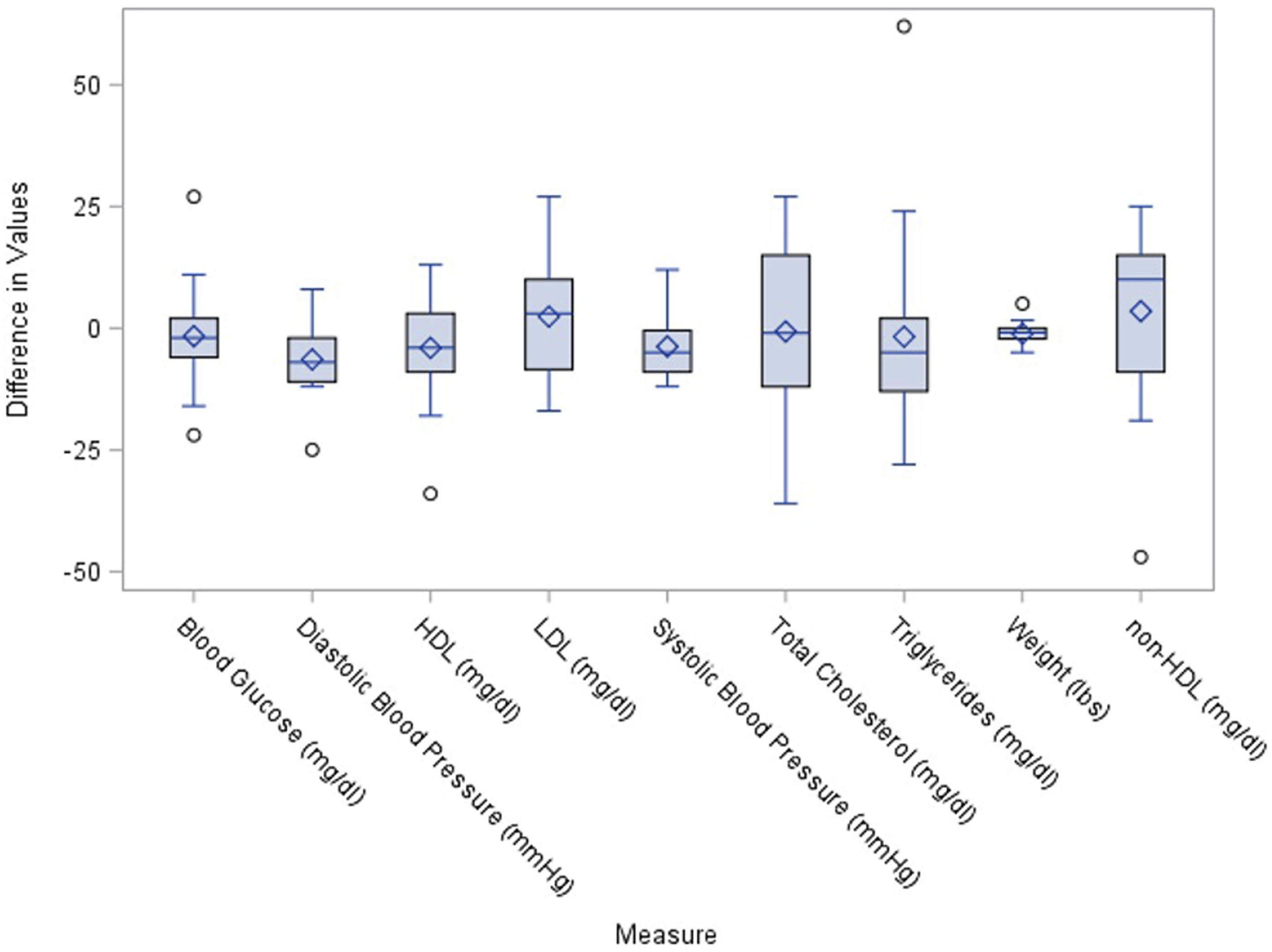
Survey Results Suggest Nutrition Seminars are Beneficial for Medical Education Curriculum
Participants’ Anonymous Survey Responses.
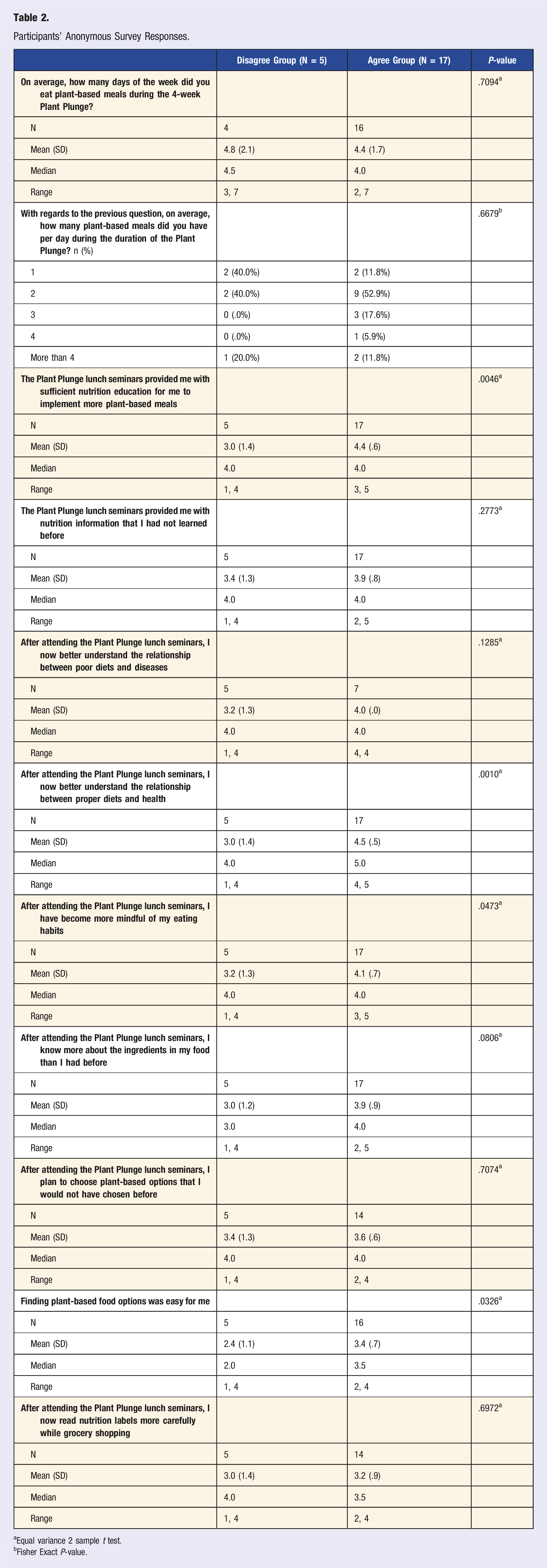
aEqual variance 2 sample t test.
bFisher Exact P-value.
In addition to the previously mentioned findings, it is worth noting that students who expressed an improved understanding of the relationship between proper dietary patterns and health after attending the Plant Plunge lunch seminars were significantly more likely to advocate for the integration of plant-based diet information into the medical school curriculum (P = .0162) (Table 2). This connection underscores the potential impact of nutrition education on students’ perspectives regarding the importance of incorporating such knowledge into their medical education. It further emphasizes the potential value of including plant-based dietary pattern education within the medical school curriculum to better prepare future health care professionals to address the crucial role of diet in overall health and well-being.
Discussion
Our study offers preliminary evidence supporting the positive impacts of a short-term WFPB dietary pattern intervention and concurrent nutrition education for medical students. Participants who adhered to the program, as self-reported, demonstrated statistically significant improvements in weight and blood pressure. These findings align with existing research indicating that low-fat, plant-based dietary changes alone, without additional lifestyle interventions, effectively reduce cardiovascular risk factors and contribute to weight management.26,27 Notably, a study by Brown et al. revealed a significant average weight loss of 4.4 kg in individuals adopting plant-based diets compared to controls. 28 While changes in other health parameters, such as cholesterol levels, did not reach statistical significance in our study, the observed trends towards improvement further align with clinical studies that demonstrated prolonged-release of nicotinic acid, a component of WFPB dietary patterns, leads to marked, long-term increases in HDL-cholesterol, with additional beneficial effects on triglycerides and LDL-cholesterol.29,30
A key strength of this study is its focus on a real-world setting with busy medical students, demonstrating the feasibility of incorporating WFPB dietary patterns even within time-constrained schedules. This aligns with research highlighting the practicality and effectiveness of plant-based dietary interventions in diverse populations, including those with limited time or resources. 31 Our findings are also consistent with another intervention study that indicated positive dietary changes in medical students after a 4-week nutrition education intervention, 25 supporting the implementation of supplemental nutrition seminars in medical school as a means for both education and lifestyle behavior changes. If these changes can be applied to other, more diverse populations, the differences that are seen can possibly be even more dramatic. However, limitations include the self-reported nature of dietary adherence, which introduces potential bias, and the small sample size, limiting generalizability. Additionally, the change in weight represents the average overall change, as the data was collected anonymously and not linked, which may obscure significant changes for individual participants. Future research employing objective measures of WFPB dietary pattern adherence and involving larger, diverse populations is warranted to confirm our findings and elucidate the long-term health impacts of this dietary approach. While our study observed improvements in weight and blood pressure, more research could delve deeper into the physiological mechanisms by which WFPB dietary patterns potentially improve specific chronic disease markers. This could involve analyzing changes in inflammatory markers, insulin sensitivity, and gut microbiome composition in participants adhering to a WFPB dietary pattern intervention. This study was intended to be a preliminary study to examine medical student lifestyle changes to adhere to WFPB dietary patterns in hopes to improve health parameters and to examine the efficacy of supplemental nutrition seminars in medical school. Our findings are limited since the number of participants was recruited on a volunteer basis with a busy medical student schedule and this was the first year that the Plant Plunge was formally reviewed for a research study. However, the Lifestyle Medicine Interest Group at OUWB SOM intends to continue this program annually and gather more participant data from this programming.
Our data also demonstrates the positive impact of incorporating nutrition seminars into medical education. A significant majority of participants found these seminars valuable in providing nutrition education, directly correlating with their belief in their ability to educate and empower future patients regarding healthier dietary patterns. Moreover, our findings support calls for integrating comprehensive nutrition education into medical school curricula, as outlined by the American Society for Clinical Nutrition and the American Society for Parenteral and Enteral Nutrition.32,33 This could include mandatory coursework, interactive workshops, and peer-led learning opportunities focused on WFPB dietary patterns and other evidence-based dietary approaches to preventive health. Moreover, our study’s peer-driven approach to data collection demonstrates the potential for peer learning and the positive influence that medical students can have on each other when it comes to promoting healthier dietary patterns and nutrition education within the medical community. This aligns with research highlighting the effectiveness of peer-led interventions in promoting behavior change and healthy lifestyle patterns among medical students.34,35 Another approach to promoting peer-led learning is implementing lifestyle and nutrition electives during didactic and clerkship years in medical school to integrate lifestyle changes with preventive health practices. This collaborative effort not only benefits participants but also has broader implications for future health care practices and patient outcomes.
Conclusions
Incorporating more WFPB dietary patterns show promise in lowering systolic and diastolic blood pressures and losing weight in 4 weeks. The Plant Plunge seminars positively influenced medical students’ understanding of diet-health relationships. Following the seminars, 91.6% of students acknowledged a better grasp of this link. This high agreement highlights the effectiveness of the seminars. Those with an enhanced understanding were more supportive of integrating plant-based dietary pattern information into medical school curricula (P = .0162), suggesting the potential of nutrition education in empowering future health care professionals. The data supports WFPB dietary patterns for healthier lifestyles, demonstrating success even among time-constrained individuals like medical students. This implies broader public feasibility. Integrating nutrition seminars into medical education could offer more benefits for enhanced nutrition understanding for future physicians.
Footnotes
Acknowledgments
We would like to sincerely thank Chickpea and Bean for hosting the Plant Plunge at Oakland University William Beaumont School of Medicine. We would also like to thank the Physicians Committee for Responsible Medicine and VegMichigan for providing the materials required for the pre- and post-program health screenings and plant-based lunches at the weekly nutrition seminars for all participants.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Institutional Review Board of Oakland University (IRB#: IRB-FY2023-222 on March 22, 2023). Informed consent was obtained from all subjects in this study.
Informed Consent
Informed consent was obtained from all subjects involved in the study.
Disclaimer
The statements, opinions, and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of the editor(s). The editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions, or products referred to in the content.
Data Availability Statement
Data supporting reported results, including links to publicly archived datasets analyzed or generated can be found at MDPI.
