Abstract
In this perspective we describe our experience in developing a novel approach to delivering nutrition education through the hospital patient menu to a broad audience. Using an evolving, themed ‘weekly specials’ patient menu, unique nutrition education materials were developed across a range of topics, aligned with menu themes to be delivered to patients, staff and the broader community. The current strategy has successfully been implemented over a 3 year period. It has been driven by a series of patient menus showcasing nutritious, varied and sustainable nutrients and ingredients accompanied by a diverse range of education mediums including in-service education sessions for staff, printed nutrition education materials for patients and social-media messaging for the broader community. We are unaware of any other hospital (or institution) that consistently draws on their core patient menu to inspire and educate staff and the broader community. Opportunities for application in other institutions such as schools and worksites are evident.
‘The nutrition intervention activities were developed based on Experiential Learning Theory and Ecological Systems Theory’.
Background
The hospital menu is the core communication tool between foodservices and the hospital community. At minimum, the menu creates opportunities for patients to select healthy meals for consumption while in hospital. The menu can also act as a resource to educate patients about how food be used to manage their health condition, such as with chronic diseases. When patients are assigned a therapeutic diet that tailors their ordering to their condition, they can learn about appropriate food choices and try new foods that are suitable for their condition.
While appropriate food provision in hospital supports patients to eat well during their stay, ongoing support is needed to assist patients to eat well after discharge. Traditionally, this nutrition education has been delivered by the hospital dietetic team through bedside counselling or printed resources at discharge, though this may not be the only or most effective mode of delivery for patients.
In general, hospital foodservices have not yet realized their full potential to use the menu to influence food choices and provide nutrition education to improve nutrition choices for healthcare staff and the community more broadly. It is well recognized that the foods and beverages available in healthcare settings for staff and visitors are not congruent with health eating practices. These unhealthy food environments likely contribute to the poor eating and health indicators of healthcare staff. 1 A growing body of research suggests that, in general, healthcare workers eat too few fruits and vegetables, too many discretionary foods, and have high rates of overweight/ obesity.1-4 This is important as good nutrition is critical for preventing chronic diseases and supporting emotional wellbeing.5,6
In recent years, a range of interventions and policies and guidelines 7 have been implemented to make healthy food choices in healthcare settings the norm. These policies and guidelines can be difficult to implement, audit and sustain, particularly in settings where the commercial foodservice arms of the hospital are contracted to external providers. 8 Moreover, the focus of these initiatives is on improving the nutritional quality of the foods and drinks provided, with less emphasis on nutrition education. As such, opportunities for nutrition education for staff are warranted.
The current perspective describes a novel approach to deliver nutrition education to healthcare staff and the broader hospital community by leveraging the patient menu. We will discuss our unique approach to nutrition education, give detailed examples of nutrition messages and methods of delivery, and consider opportunities for extension both within our healthcare setting and more broadly.
Approach and Setting
Mater Health South Brisbane is a large (approximately 800 beds), urban, tertiary healthcare campus employing approximately 6000 staff. Mater Dietetics and Foodservices prides itself in implementing innovative and effective foodservice models to support the nutritional needs of patients. Mater South Brisbane was the first healthcare provider in Australia to implement a cook on demand, room service model. Similar to a hotel, patients can order meals or snacks, suited to their individual dietary requirements between 6
At Mater, patient meal ordering options include both digital (through a bedside tablet) or personal (by phoning the call centre) options. The patient menu provides some nutrition education tools such as symbols noting options that may be suitable for patient conditions (e.g. heart healthy) or noting the servings of carbohydrates and glycaemic index ratings (for patients with diabetes). The call centre staff can play an additional role in limited nutrition education for patients who choose to call them.
In Australia, healthcare services are funded publicly by Medicare (Australia’s public healthcare system) or privately (by health insurance). At Mater all patients have access to the cook-fresh, room service foodservice model. Patients who are privately-funded have additional options for their meal choice; these are offered to create a differentiator and to meet patient expectations of paying privately for an enhanced experience. Mater South Brisbane has partnered with an Australian celebrity chef to offer seasonal chef’s special menus offering restaurant quality meals. The chef’s special menu rotates on a 4-week cycle around a specific theme and the themes change approximately 3-4 times a year.
For staff and visitors, the Mater South Brisbane campus offers 5 cafes and approximately 40 vending machines. These outlets are contracted to an external provider. In 2019, the Queensland state government passed a directive to ensure that healthy foods and beverages are sold, provided, promoted and advertised at healthcare facilities. The directive sets clear targets for proportion of foods and beverages that should be healthy and limits the number of unhealthy foods and beverages. Though some early achievements were made in compliance with the directive, the most recent audit of the cafes onsite at Mater were not compliant. This is despite research demonstrating that healthcare workers at Mater have poor eating behaviours in general and want healthier food and beverage options onsite. 9
Given this, the Mater Dietetics and Foodservices team saw an opportunity to leverage the rotating chef’s special menu to launch a range of general nutrition education strategies for patients, staff and the broader community. As the chef’s special menu changes three-four times a year, the key nutritional messages and modes of delivery could change to align to the specific theme of the menu. Educational messaging focused largely on specific nutritional aspects of foods/ meals, promoting dietary variety, and/ or highlighting environmentally friendly features of the menu.
Development and Implementation of the Nutrition Education
The nutrition intervention activities were developed based on Experiential Learning Theory and Ecological Systems Theory. Experiential Learning is the process of ‘learning through reflection on doing’, as opposed to learning that is rote, didactic or passive. Ecological Systems Theory contextualizes human development (and behaviour) as the product the interactions between a person and their environment. Ecological Systems Theory acknowledges that there are multiple layers of a person’s environment that each have their own cultures, rules and expectations that influence how a person develops or behaves.
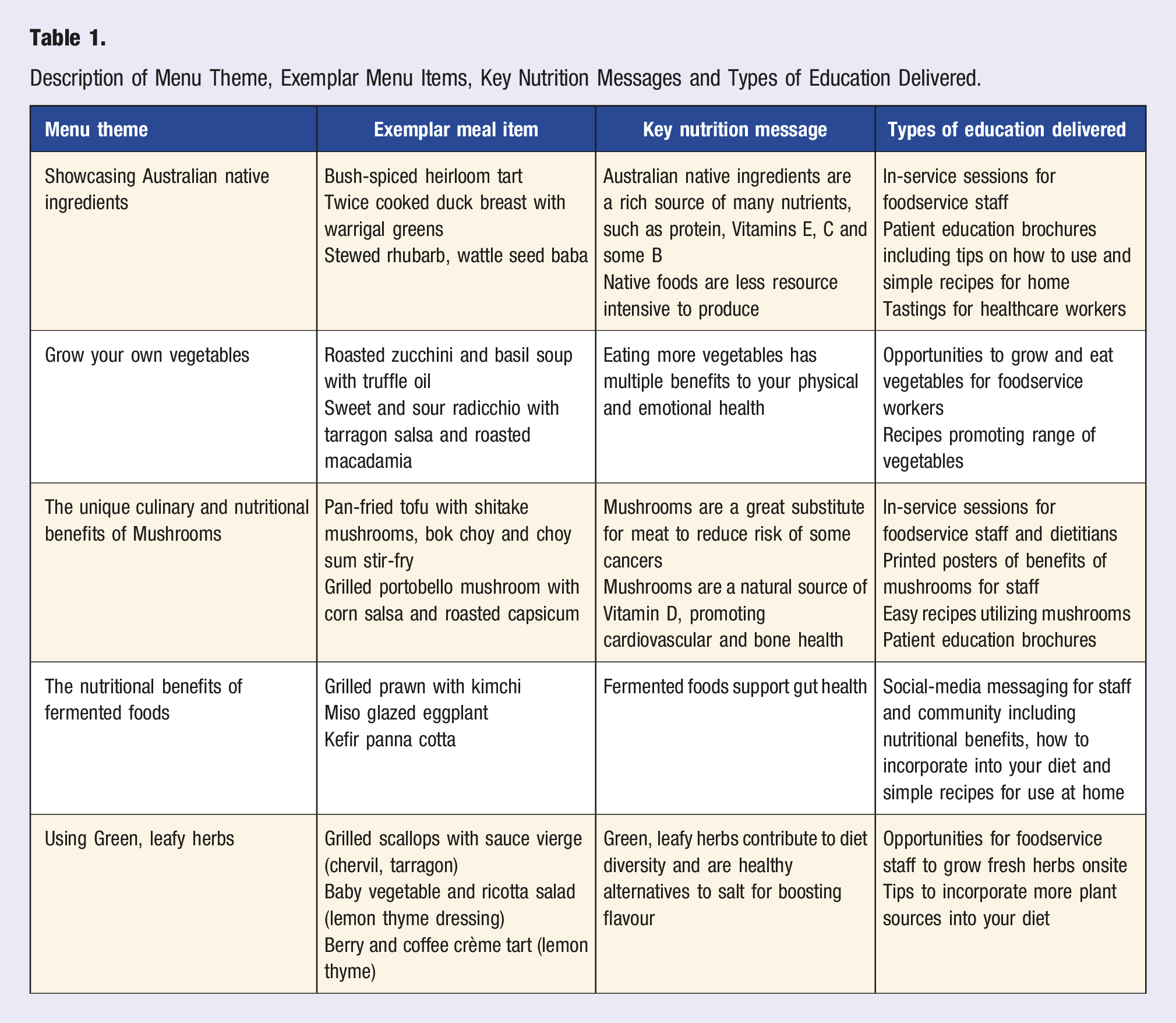
The Table 1 includes a summary of the implemented nutrition education messages, activities and alignment to menu themes. Nutrition education activities were multi-modal, in attempt to integrate multiple concepts of the theories. Evaluation activities for each menu were varied, largely focussing on reach, engagement and staff experience.
As an example, the grow your own vegetables themed menu aimed to communicate to staff and patients that diets rich in vegetables have multiple benefits to your physical and emotional health, such as reduced risk of heart disease, diabetes, some cancers and emotional distress.5,6 In preparation for the menu launch, the dietetics and foodservices teams partnered with a local company that manufactured raised garden beds who donated the supplies necessary to establish vegetable and herb gardens onsite for staff. The partnering company also offered a discount for staff wanting to purchase their own raised beds for their home. The establishment of the staff vegetable garden created an opportunity for staff to actively experiment with vegetable production (Experiential Learning) and share their experiences with colleagues (relationships in Ecological Systems Theory). An evaluation of the staff garden found that nearly 40% of staff had taken something home from the garden and that staff reported their experiences with the garden favourably. 10
The menu showcasing Australian native ingredients was identified to align to the organization’s development of a Reconciliation Action Plan, a framework that actively contributes to reconciliation between Aboriginal and Torres Strait Islander people and non-indigenous Australians and to coincide with numerous holidays of related cultural significance. The key nutritional messages highlighted that Australian native foods are a rich source of many nutrients. Compared to Western counterparts, Australian native fruits have more protein, Vitamin E, Vitamin C, and some B vitamins. 11 Patient education materials and staff in-service sessions were delivered to build basic knowledge of native foods and their nutritional qualities (an individual factor of Ecological Systems Theory). Over the intervention period, more than 8000 patient education brochures were delivered and nearly 50 foodservices staff attended an in-service session about the unique aspects of the menu. 12 There were additional tasting opportunities for staff that provided a concrete experience of tasting a new food and reflecting on their perceptions (Experiential Learning). Approximately 1500 cold-pressed juices (made onsite and featured a native ingredient) were distributed to staff throughout the hospital to taste and to acknowledge their service.
Implications for Practice
Description of Menu Theme, Exemplar Menu Items, Key Nutrition Messages and Types of Education Delivered.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
