Abstract
Background: The objective of this study was to assess the efficacy of an Exercise is Medicine on Campus® program on university student biometrics and muscular endurance. It was hypothesized that participants in the 12-week program would experience significant improvements in body mass index, blood pressure, body fat percentage, waist circumference, and muscular endurance. Methods: To be eligible for the program, participants must have met two of the three criteria: (1) blood pressure over 140 and/or 90 (3 consecutive measurements over 2 weeks), (2) BMI over 30, and/or (3) diagnosed chronic condition or currently taking medication for chronic condition. Participants engaged in six bi-weekly exercise instructional meetings that lasted approximately 30 minutes in length. Participants completed measures of resting heart rate, waist-to-hip ratio, body composition percentage via bioelectrical impedance, and muscular endurance before and after the program. Results: Although not statistically significant, there was a decrease in BMI, blood pressure, body fat percentage, and waist circumference from pre- to post-program. Two-tailed t-tests revealed significant improvements in squats (P = .04), pushups (P = .05), and curl-ups (P = .03) from pre- to post-program. Conclusion: The results are discussed in terms of current research and future university campus application.
“This twelve-week implementation of the EIM-OC program resulted in significant improvements in muscular endurance via push-ups, squats, and curl-ups.”
Exercise is Medicine on Campus® (EIM-OC) is being promoted for world-wide campus implementation because many college students do not engage in regular PA or the recommended 150 minutes of moderate-to-vigorous PA.1,2 This is important because regular PA can help reduce mental and emotional illness (i.e., stress, anxiety, depression) along with chronic diseases (i.e., hypertension, diabetes, coronary heart disease, cancers). 3 It is necessary to continually assess the use of prescribed exercise as medicine to ensure continuous and long-term benefits of such practice.4,5 While there have been a few publications indicating the efficacy of EIM-OC on physical activity and other health metrics,6,7 most studies have examined participation, reach, and barriers to implementation.8-11
There are currently 156 universities that have earned the Exercise is Medicine on Campus (EIM-OC) designation for promoting a culture of wellness on campus. 12 The main EIM-OC criteria include (1) making movement part of daily campus culture, (2) assessing student physical activity (PA) at health visits, (3) providing resources and tools for students to strengthen PA habits, and (4) connect health care providers and fitness specialists on campus for exercise prescription. 13 Some of the biggest barriers to EIM-OC implementation include instituting the referral system for the campus-wide program, assessing the impact of exercise on PA and other variables, lack of student and campus involvement, and lack of campus awareness. 11 The EIM-OC program for this study has been implemented at gold standard for the past seven years. 12 Although campus standardization has been successful, the program needs to be continually evaluated for all aspects of programming, including needs assessments, process evaluations, and outcome impact. The primary objective of this study was to assess participant pre-program data and compare it to post-program data to provide recommendations for EIM-OC programming.
Materials and Methods
Participants
Participants included students who expressed interest in the Exercise is Medicine® (EIM) on Campus and met the inclusion criteria. To be eligible for the program, participants must have met two of the three criteria: (1) blood pressure over 140 and/or 90 (3 consecutive measurements over 2 weeks taken by Wolf Wellness Lab personnel or physician), (2) BMI over 30, and/or (3) diagnosed chronic condition or currently taking medication for chronic condition (documentation required). A chronic condition may include but was not limited to pre-diabetes, diabetes, high blood pressure, anxiety, depression, arthritis, osteoporosis, asthma. The in-depth criteria and details of the EIM-OC program can be found in another publication. 6
Measures
Each of the assessments and questionnaires were conducted via paper-and-pencil format.
Medical history profile
This questionnaire included self-reported height, weight, age, gender, BMI, and an exercise pre-participation health screening.
Biometric screening
The baseline and follow-up assessments included valid and reliable measures of body mass index, body composition via biometrical impedance analysis, 14 and muscular endurance (i.e., pushups, squats, and curl-ups in 60 seconds).15-18
Adverse events and participant satisfaction
This questionnaire was implemented to elicit feedback from participants on EIM-OC satisfaction and adverse events (e.g., Did they enjoy the EIM program? Did it encourage them to be more active than usual? Did they experience an event that negatively impacted participation? If so, provide details.).
Procedure
Following IRB approval, students meeting the inclusion criteria were referred from Counseling and Health Services, University Health Services, or by self-referral to the EIM-OC program. Other methods of registration included communication from Campus Recreation or campus-wide fliers. Interested students attended a 30-minute initial consultation in which they were assessed for necessary inclusion criteria, completed informed consent, all questionnaires, and biometrics. Participants were then screened for eligibility and safe participation in prescribed exercise by an ACE Personal Trainer, EIM certified faculty, and ACE Personal Trainer-certified students. Participants then engaged in six bi-weekly exercise plan and instruction meetings that lasted approximately 30 minutes in length. The recommended exercise plan was created, reviewed, and provided to participants by research staff that are certified ACE Personal Trainers. Before and after the program, participants completed measures of resting heart rate, waist-to-hip ratio, body composition percentage via bioelectrical impedance, and muscular endurance. Details of the prescribed training sessions and more in-depth procedures can be found in a previous publication. 6
Data Analysis
Descriptive statistics examined means, standard deviation, and ranges for demographic variables and biometric outcome variables. Paired sample t-tests were used to examine group differences in pre- and post-program variables (i.e., BMI, BP, body fat %, biometric screening results).
Results
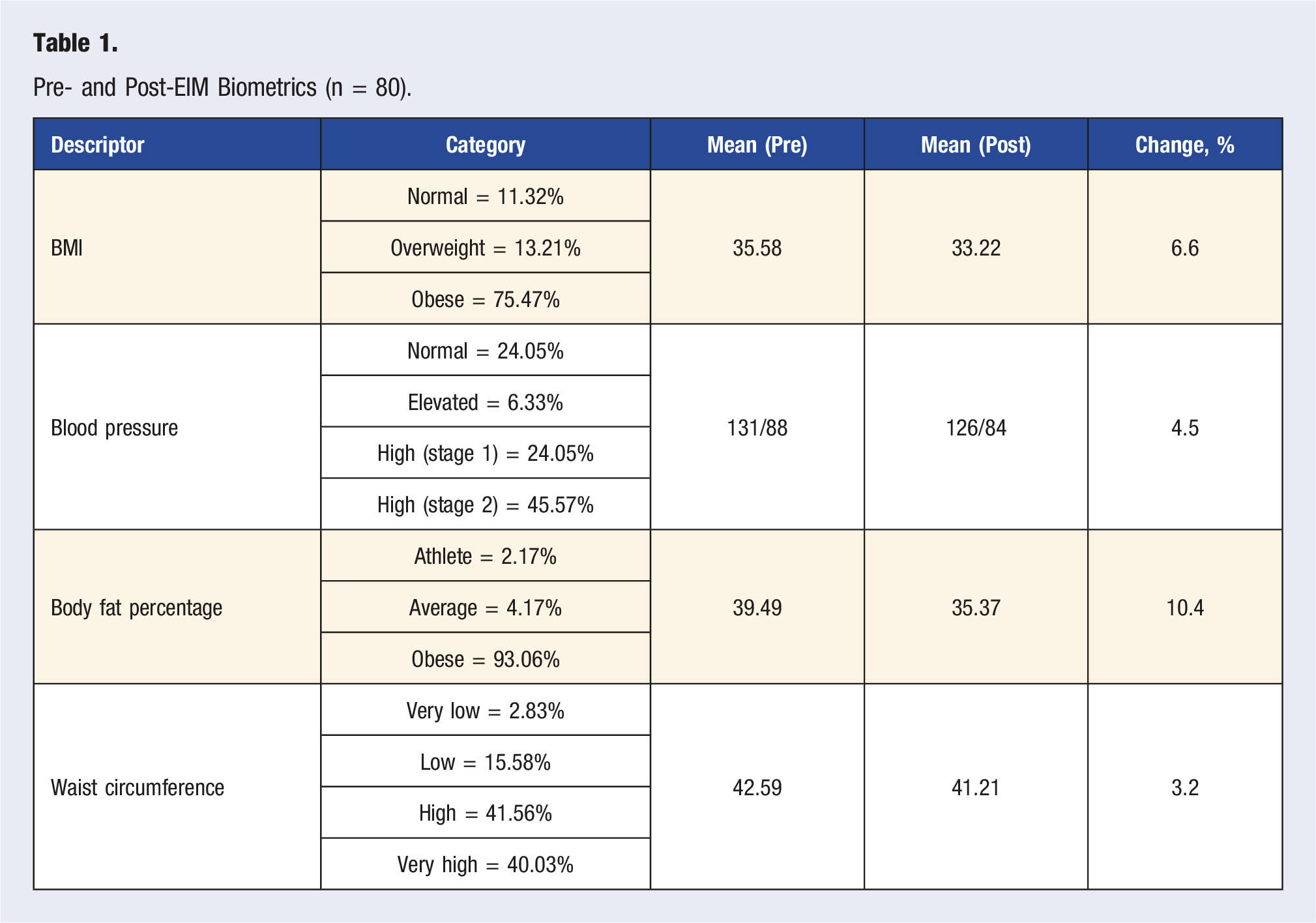
Pre- and Post-EIM Biometrics (n = 80).
Pre- and Post-Program Physical Fitness Testing.
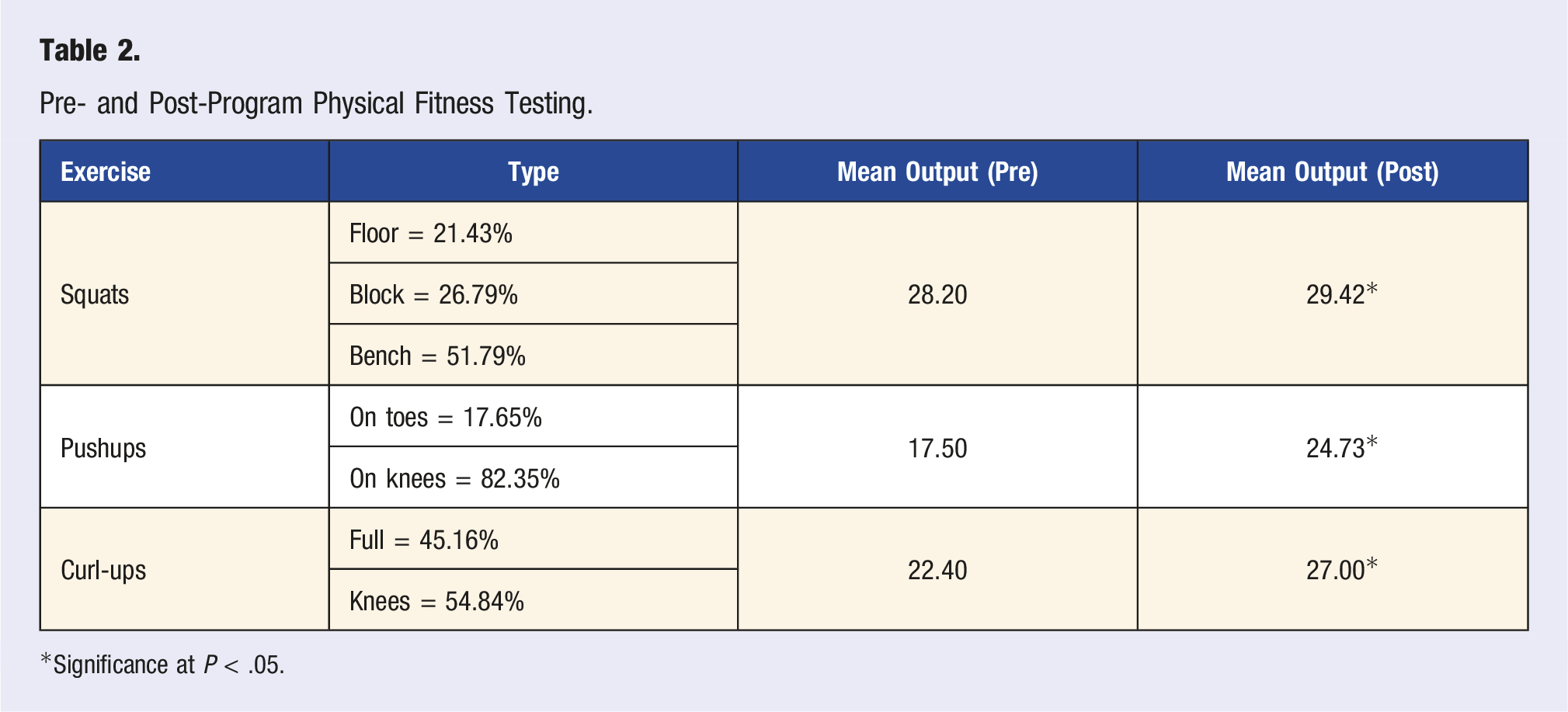
*Significance at P < .05.
Separate two-tailed t-tests revealed significant improvements in squats (P = .04), pushups (P = .05), and curl-ups (P = .03) from pre- (M = 22.40) to post-program (M = 27.00).
Discussion
The purpose of this study was to assess participant pre-program data and compare it to post-program data following participation in the Exercise is Medicine® on Campus (EIM-OC) program. The implementation of this EIM-OC program follows the best practices as outlined in the American College of Sports Medicine. 19 However, this is one of the first studies to evaluate the effectiveness of EIM-OC on college participant biometrics and fitness. This twelve-week implementation of the EIM-OC program resulted in significant improvements in muscular endurance via push-ups, squats, and curl-ups. Improvements in muscular strength and endurance in obese populations protects against cardiometabolic risk and is associated with reduced risk for cardiovascular disease risk factors, type 2 diabetes, obesity, and all-cause mortality, regardless of BMI, lean mass, cardiorespiratory fitness, or physical activity levels.22,23 While there are not many studies implementing and evaluating EIM-OC, a previous implementation of this protocol reported similar improvements in muscular endurance. 6 Furthermore, a previous study revealed the effectiveness of a 14-week strength training program on muscular endurance in college students. 20 Another study with Malaysian university students improved muscular endurance through a 4-week training program. 21 For future EIM-OC implementation, it is important to consider shorter program duration with more frequent exercise sessions to enhance effectiveness.
The EIM-OC program participant reduced blood pressure (BP), body composition (BC), resting heart rate (RHR), and waist circumference following from bi-weekly informational and training sessions, as well as self-directed exercise. Although the results were not statistically significant, the pre- to post-program results had a downward trend, which is consistent with previous research. 6 Even though there was not significance, and as previously mentioned, improvements in muscular fitness can have long-term health benefits, regardless of body composition. It is important to replicate this study to understand the independent effects of independent variables on outcome health measures. A previous EIM-OC study was descriptive, indicating improvements in self-report bouts of PA and enhanced EIM-OC awareness. 8 A different EIM-OC evaluation was implemented with the same 12-week duration and, although there was no evaluation of biometrics or fitness levels, indicated improvements in student PA levels, self-efficacy, and intention to continue engaging in PA. 24
Participants in this EIM-OC program expressed their top reasons for participation, including losing weight (80%), reducing health risk (73.33%), and increasing strength (56.67%). A 1-week EIM-OC evaluation also found that students engaged in the program due to perceived health improvements, weight control, and stress relief. 7 They also reported factors that would contribute to successful program adherence, including accountability, exercise program planning, and instruction on proper technique/form. An evaluation of EIM-OC found that lack of willpower, fear of injury, lack of skill, and insufficient resources were some of the most cited barriers to EIM-OC PA participation. 25 Given the design and effectiveness of the implementation of the current EIM-OC program, there is potential for the combination of informational, instructional, and supervised training sessions to help university students overcome such barriers.
Limitations
Although this study was effective in terms of improving muscular endurance and participant biometrics, there are various limitations. First, participants engaged in either traditional or modified push-ups, squats, and curl-ups based on functional mobility levels. This study did not evaluate PA levels throughout the program. It would be beneficial to assess PA levels using accelerometry during the supervised training sessions, during self-directed training, and following completion of the program. Another limitation was that most participants in this study were female. This is consistent with a review of physical activity interventions and could be due to the fact that women are more likely to engage in PA for weight loss and toning reasons when compared to men.26,27 Based on previous research, future implementation could improve male participant recruitment by determining exercises or sports they enjoy as that is one of the strongest motivators for male participation. 27 Lastly, participants were not stratified based on BMI, body fat percentage, race, or gender. It would be interesting to assess the impact of the EIM-OC program on various body classifications, risk levels, and across both gender and race.
Conclusion
The purpose of this study was to assess the impact of EIM-OC program on muscular endurance, BMI, BP, and body fat percentage. The EIM-OC program resulted in significant improvements in muscular endurance, and insignificant decreases in BMI, blood pressure, body fat percentage, and waist circumference from pre- to post-program. Future implementation and evaluation of EIM-OC could consider shorter program duration with more frequent bouts of exercise. A deeper understanding of participant knowledge about PA could also be assessed pre- and post-program implementation through qualitative analysis. Given COVID-19 restrictions, a synchronous, online implementation of EIM-OC could assess the efficacy of virtual programming on college student PA knowledge, biometrics, and fitness levels. With more substantial resources and staffing, an evaluation of campus-wide EIM-OC with students with varying mental and physical health statuses could take place.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
