Abstract
The Physical Activity Guidelines for Americans (Guidelines) advises older adults to be as active as possible. Yet, despite the many benefits of physical activity, less than 15% of people ages 65 years and older meet the Guidelines. To address this, the U.S. Department of Health and Human Services developed a Midcourse Report focused on the strategies and settings that can help increase physical activity levels among older adults. Internists are well positioned to encourage older adults to be more physically active. Health care providers can leverage this position to talk about the importance of regular physical activity; assess physical activity levels; share information and resources about how to safely get started; and provide counseling, guidance, and/or referrals to additional providers or programs for further support. This article provides an overview of the recently released Physical Activity Guidelines for Americans Midcourse Report: Implementation Strategies for Older Adult and highlights the role of internists and other health care providers to encourage and support their patients to be more physically active.
“SMART goals help patients turn a general goal of increasing physical activity into a tangible action.”
Introduction
Physical inactivity is among the strongest predictors of physical disability in older people. 1 Even small amounts of moderate-intensity aerobic activity provide some health benefits. 1 Unfortunately, most older adults are not getting the physical activity they need to get and stay healthy. Internists are well positioned to encourage older adults to be more physically active. People ages 65 and older need 150 minutes or more of moderate-intensity aerobic activity each week and 2 days of muscle-strengthening physical activity for substantial health benefits. 1 Additionally, as part of their weekly physical activity, older adults should do multicomponent physical activity that includes balance training as well as aerobic and muscle-strengthening activities. 1 Less than 15% of older adults do enough physical activity, 2 and over 37% do no leisure-time physical activity. 3 For older adults in particular, many benefits accrue at levels below those recommended in the Physical Activity Guidelines for Americans (Guidelines). Benefits include better sleep, lowered blood pressure, reduced risk of development of chronic diseases, slowed progression of chronic conditions, and improved functional ability. 1
Health care providers are trusted sources of health information and information about physical activity. 4 Older adults are a population that has more frequent visits with a health care provider compared to other age groups. 5 Each encounter is an opportunity for health care providers of all levels, from intake staff, nurses, internists, and specialists to talk to their patients (and any family members or caregivers accompanying them on the visit) about the importance of regular physical activity; assess physical activity levels; share information and resources about how to safely get started; and provide counseling, guidance, and/or referrals to additional providers or programs for further support.
The Physical Activity Guidelines for Americans 1 provides recommendations on the amounts and types of physical activity that are needed for individuals to get and stay healthy. They are released every 10 years by the U.S. Department of Health and Human Services and are based on the current scientific evidence on physical activity and health outcomes. The Move Your Way® campaign was developed to communicate the Guidelines to a variety of audiences, including health care providers and the general public, 6 similar to how MyPlate helps consumers make healthy eating choices based on the Dietary Guidelines for Americans. 7 In between full editions of the Guidelines, a midcourse report is released. The most recent midcourse report, released in 2023, extends the work of the Guidelines by focusing on the strategies and settings that can help increase physical activity levels among older adults. 8 Health care providers are identified in the Midcourse Report for their important role in encouraging older adults to be more physically active.
This article provides an overview of the recently released Physical Activity Guidelines for Americans Midcourse Report: Implementation Strategies for Older Adults 8 and describes the role of internists and other health care providers to encourage and support their patients to be more physically active. The article also provides tools and resources to help motivate behavior change and tips on how to start the conversation.
Key Guidelines for Older Adults
Older adults should follow the key guidelines for adults, and there are additional guidelines specific to older adults (defined as ages 65 and older). Older adults should include aerobic, muscle-strengthening, and multicomponent physical activities in their weekly routine (Figure 1). Older adult physical activity guidelines dosage recommendations.
Key Guidelines for Adults
• Adults should move more and sit less throughout the day. Some physical activity is better than none. Adults who sit less and do any amount of moderate-to-vigorous physical activity gain some health benefits. • For substantial health benefits, adults should do at least 150 minutes (2 hours and 30 minutes) to 300 minutes (5 hours) a week of moderate-intensity aerobic activity or 75 minutes (1 hour and 15 minutes) to 150 minutes (2 hours and 30 minutes) a week of vigorous-intensity aerobic physical activity, or an equivalent combination of moderate- and vigorous-intensity aerobic activity. Preferably, aerobic activity should be spread throughout the week. • Additional health benefits are gained by engaging in physical activity beyond the equivalent of 300 minutes (5 hours) of moderate-intensity physical activity a week. • Adults should also do muscle-strengthening activities of moderate or greater intensity that involve all major muscle groups on 2 or more days a week, as these activities provide additional health benefits.
The key guidelines for adults also apply to older adults. In addition, the following key guidelines are just for older adults: • As part of their weekly physical activity, older adults should do multicomponent physical activity that includes balance training as well as aerobic and muscle-strengthening activities. • Older adults should determine their level of effort for physical activity relative to their level of fitness. • Older adults with chronic conditions should understand whether and how their conditions affect their ability to do regular physical activity safely. • When older adults cannot do 150 minutes of moderate-intensity aerobic activity a week because of chronic conditions, they should be as physically active as their abilities and conditions allow.
It All Adds Up
Examples of Physical Activities for Older Adults.
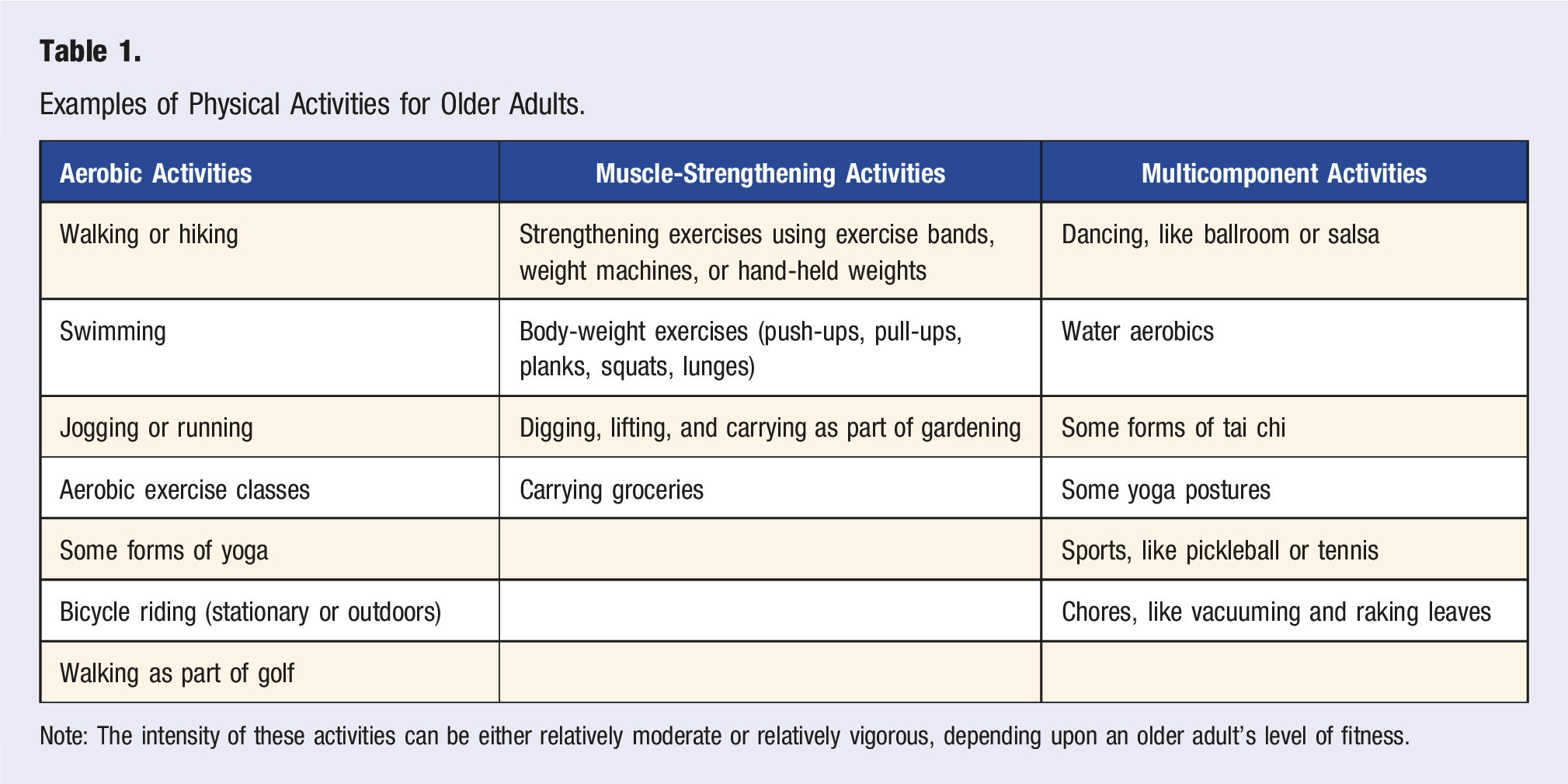
Note: The intensity of these activities can be either relatively moderate or relatively vigorous, depending upon an older adult’s level of fitness.
Defining Terms
Intensity
Intensity refers to how much work someone is doing, or the magnitude of the effort required to perform an activity or exercise. Intensity can be expressed in absolute or relative terms.
Absolute intensity is the amount of energy expended during the activity but does not take a person’s cardiorespiratory fitness into account. Examples of absolute moderate-intensity activities include brisk walking, recreational swimming, doubles tennis or pickleball, general yardwork and home repair work, ballroom or line dancing, and exercise classes such as water aerobics.
Relative intensity uses a person’s level of cardiorespiratory fitness to assess level of effort. Certain activities that are considered light-intensity—such as some types of yoga or tai chi—may be perceived as moderate- or vigorous-intensity for some older adults.
Either absolute or relative intensity can be used to monitor progress toward meeting the key guidelines. Because older adults expend more energy than younger adults for the same task, and because aerobic capacity declines with age, older adults should use relative intensity to guide their level of effort rather than absolute intensity. 1 People can easily gauge relative intensity by using the talk test.
The Talk Test
The Talk Test is a simple way to measure relative intensity. When using relative intensity, people pay attention to how physical activity affects their heart rate and breathing. As a rule of thumb, a person doing moderate-intensity aerobic activity can talk, but not sing, during the activity. A person doing vigorous-intensity activity cannot say more than a few words without pausing for a breath.
Multicomponent Physical Activity
Multicomponent physical activity incorporates aerobic, muscle-strengthening, and balance components. For older adults, multicomponent physical activity is especially important because it can improve physical function and decrease the risk of falls or fall-related injury. 1 People can do multicomponent physical activity at home or in a structured group setting. Many studied interventions combine all types of exercise (aerobic, muscle-strengthening, and balance) into 1 session, and this has been proven effective. A multicomponent physical activity program could include walking a dog (aerobic), doing bicep curls (muscle-strengthening), and standing on 1 foot (balance). Recreational activities such as dancing, yoga, tai chi, gardening, or sports can also be considered multicomponent because they often incorporate multiple types of physical activity.
Benefits of Physical Activity for Older Adults
Health Benefits Associated With Physical Activity for Older Adults.

Source: U.S. Department of Health and Human Services. Physical Activity Guidelines for Americans, 2nd edition. Washington, DC: U.S. Department of Health and Human Services; 2018.
Being Active with a Chronic Health Conditions or Disability
Health Benefits Associated With Regular Physical Activity for People With Chronic Health Conditions and Disabilities.
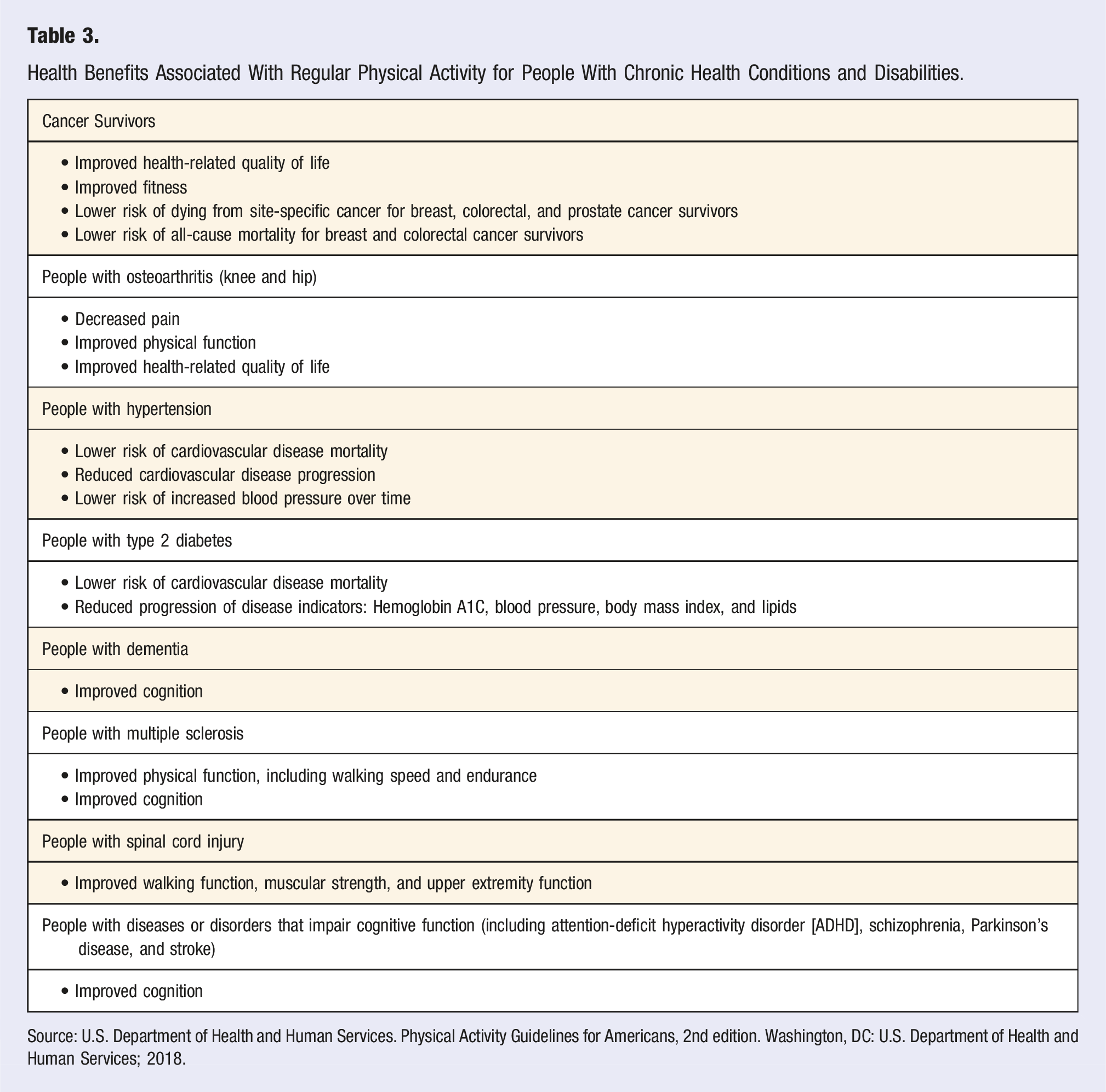
Source: U.S. Department of Health and Human Services. Physical Activity Guidelines for Americans, 2nd edition. Washington, DC: U.S. Department of Health and Human Services; 2018.
Regular physical activity provides important health benefits for people with physical disabilities. The benefits include improved cardiovascular and muscle fitness, improved brain health, and better ability to do activities of daily living. 1 Though much remains to be learned about the benefits of activity for specific types of disabilities, adults with disabilities should do regular physical activity and have the same key guidelines as individuals without disabilities. 1
The Physical Activity Guidelines Midcourse Report
An important message to reinforce to older adults is that it is never too late to start or restart being active. Benefits can occur with a single bout of activity and there are many ways older adults can add physical activity into their lives. Helping older adults determine how to incorporate physical activity into their routines can help them build confidence, stay motivated, and reap the benefits of an active lifestyle.
The Midcourse Report highlights strategies that professionals and others working with older adults can employ to increase physical activity among older adults in key settings and reinforces the amount and types of physical activity needed for health benefits. These strategies can be implemented wherever older adults spend their time and include policy, systems, and environmental approaches; behavior change; and physical activity programs.
Key Settings
While people can be physically active in many locations, the Midcourse Report identifies 3 key settings for successful physical activity interventions: • Health care locations—like doctors’ offices, rehabilitation/physical therapy centers, or nursing homes • Community locations—like schools, gyms, senior centers, or outdoor parks or trails • At home—where older adults spend much of their time and may be most comfortable
Many older adults have regular interactions with the health care system. Familiarity with a patient’s disease status, risk factors, symptoms, mobility, and socioeconomic status enables providers to give tailored guidance and physical activity recommendations. Providers also play an important role in connecting patients to community-based programs and helping patients transition from structured, supervised programs to continuing physical activity safely at home.
Effective Strategies
Population-level strategies involve policy, systems, and environmental approaches, like those related to transportation and neighborhood environments. These strategies aim to create safe, easy access to physical activity opportunities. For example, improving walkability of neighborhoods through community design can make it safer and easier for older adults to walk, bike, or wheelchair roll for recreation, fitness, or transportation.
Individual-level strategies involve behavior change strategies and physical activity programs. Behavior change approaches, like cognitive behavioral strategies and physical activity counseling, are often part of physical activity programs and interventions, and can help increase self-efficacy and encourage people to get active. Cognitive behavioral strategies include approaches such as increasing physical activity knowledge or awareness, goal setting, self-monitoring, and barrier identification and problem-solving. There are many different types of physical activity programs that can help older adults become more active. Structured exercise programs guide people through specific exercises, while lifestyle-based physical activity programs encourage people to become more active throughout the day—either through structured exercise or daily activities, like chores or walking to the store.
The Role of Internists to Encourage and Promote Physical Activity
Providers can employ these individual-level strategies with their patients to assess activity levels, counsel patients on how to increase their activity, and connect them to programs to help them meet their goals. While this section is framed around the role for internists, any member of the health care team can be involved in implementing these strategies and coordination from across the health care team can help further support patients’ physical activity. 12
Assess
Older adults are a varied group with a wide range of functional capabilities and health conditions. They are also at different life stages, with some still actively working and others retired and potentially living a very sedentary lifestyle. All adults experience a loss of physical function with age—but some more than others. This diversity means that some older adults can run several miles, while others struggle to walk to the mailbox or the bathroom. Once you have an idea of their current activity level, you can suggest small changes to help them get more active.
Some health care systems, such as Kaiser Permanente,
13
assess patients’ physical activity levels at each provider visit with an exercise vital sign included in the electronic health record. If your health system does not gather this information within the health record, you can obtain this information by asking a few questions: 1. On average, how many days per week do you engage in moderate-to-vigorous physical activity (like a brisk walk)? 2. On average, how many minutes do you engage in physical activity at this level? 3. On average, how many days per week do you engage in physical activities designed to strengthen your muscles such as lifting weights or doing body-weight exercises?
For the first 2 questions, multiply the number of days per week by the number of minutes to get the total minutes per week of physical activity. These data can be incorporated into the electronic health record and patient intake forms.
In addition to asking questions to assess their physical activity levels, you can ask questions to better understand their physical activity motivations. Does your patient want to complete everyday tasks more easily? Play with their grandkids without pain? Maintain their independence as they age? Knowing their motivations and what is standing in the way can help you work together to set achievable goals.
Counsel
Educate
You can help your patients understand the health benefits of physical activity, how much and what types of physical activity they need, and the role of physical activity in healthy aging. The Move Your Way Fact Sheet for Health Care Providers Caring for Older Adults (see supplemental materials) provides conversation starters, information on the dosage recommendations, and messages about specific benefits of physical activity that resonate with older adults. 14 As a provider, you can further tailor your conversation based on the medical information and health history of your patient.
Address Safety Concerns
Older adults with chronic conditions may have questions about whether their conditions or medications limit, in any way, their ability to do regular physical activity. Some patients may also worry about falling or getting hurt during physical activity.
You can provide advice on appropriate types of activities and ways to progress at a safe and steady pace. Encourage them to start with activities they are confident they can do. To reduce the risk of injuries and other adverse events, older adults can choose types of physical activity that are appropriate for their current fitness level and health goals. Such a conversation can help people learn about the types and amounts of physical activity that are appropriate for their abilities and chronic conditions.
Recommendations for safe physical activity also include using appropriate gear and sports equipment, where applicable; choosing safe environments for activity; following rules and policies of facilities or locations for physical activity; and making sensible choices about when, where, and how to be active.
Find Solutions to Barriers
Examples of Barriers and Potential Solutions for Older Adults.
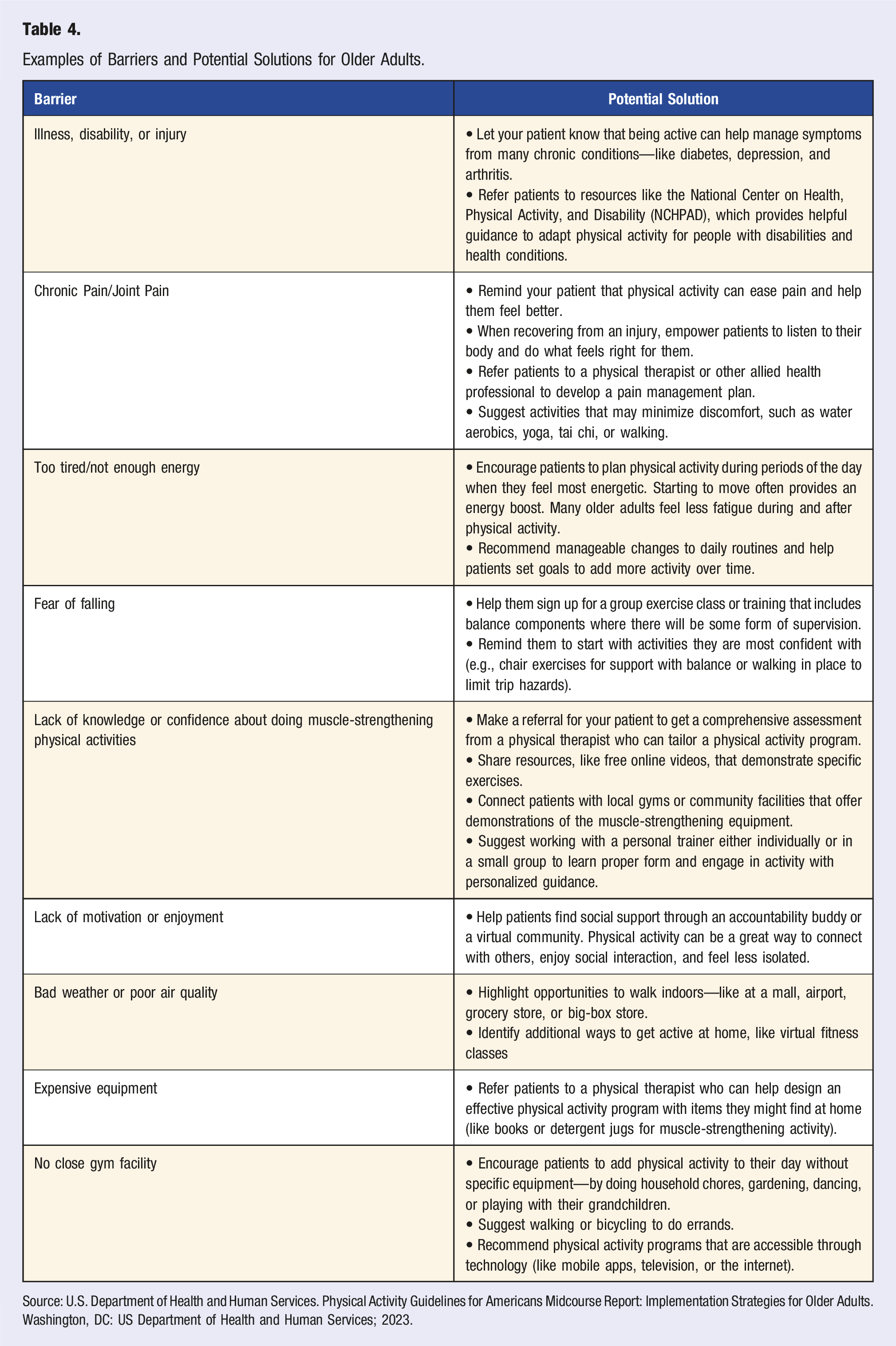
Source: U.S. Department of Health and Human Services. Physical Activity Guidelines for Americans Midcourse Report: Implementation Strategies for Older Adults. Washington, DC: US Department of Health and Human Services; 2023.
Set Goals
As a provider, you can help your patients set SMART goals (specific, measurable, achievable/attainable, realistic/relevant, and time-bound) to gradually increase physical activity levels. If the patient is regularly seen in your office, you can use that timing to align goals to upcoming visits. This also allows for a patient to gradually increase the amount or intensity of physical activity over time which can reduce their risk for injury.
SMART goals help patients turn a general goal of increasing physical activity into a tangible action. Inactive people should “start low and go slow” by starting with lower intensity activities and gradually increasing how often and how long activities are done. For example, if your patient is not currently active, you may start by prescribing a 5-10-minute light-intensity walk 3 times per week.
At their next visit, check in on their progress. You may be able to recommend setting new goals, or you may need to adjust the intensity, frequency, duration, and/or type of activity with your patient to empower them for success before their next visit. Activity should be progressed when the level of difficulty decreases and/or the behavior becomes consistent.
Example progressions include: • Increasing the duration of the walk in 5- or 10-minute intervals, • Increasing the frequency of the walk from 3 to 4 times per week, or • Increasing the intensity of the walk from light (casual) to moderate (brisk)
Monitor Progress
Tracking and recording physical activity in written or digital form can be a strategy to prompt and encourage increased physical activity. You could ask your patients to share their physical activity tracking at the next visit, providing you with an additional opportunity to give further feedback and encouragement to follow through. The Move Your Way Activity Planner is an interactive tool where patients can create a personalized weekly physical activity plan and tracker to monitor their progress. 15
Prescribe Physical Activity
Understanding your patients’ physical activity levels, motivations, challenges, and goals, will help you make well informed referrals and prescriptions. For many, prescribing physical activity just as you would prescribe a medication can help convey to your patient the importance of physical activity. This could be something as simple as incorporating 10 minutes of movement into the day through a walk, active transportation, or encouraging the use of the stairs. Exercise is Medicine Health Care Providers’ Action Guide 16 is a step-by-step implementation framework to help providers assess patients’ current physical activity levels, integrate physical activity into treatment plans, and refer patients to evidence-based exercise programs and qualified exercise professionals. An exercise prescription form is included in the guide, along with a series of patient handouts and other resources, such as exercise prescriptions for specific medical conditions (e.g., hypertension, chronic obstructive pulmonary disorder), to further support providers in integrating physical activity into practice.
Refer to Programs and Professionals
Through referrals or recommendations, you can share information about physical activity programs, especially those tailored to older adults or specific demographic populations, and can help older adults identify relevant physical activity opportunities. You can link patients to people or information for additional guidance based on their unique needs.
For example, if your patient has never done muscle-strengthening physical activity, telling them to join a gym may leave them overwhelmed. Instead, you could direct them to a specific program (close to their home) tailored to older adults that provides 1:1 or group guidance on how to properly do muscle-strengthening physical activity. A patient that has graduated from a program within the health care system, such as a cardiac rehabilitation program, may need continued guidance and support through a community program to continue physical activity.
There are many national programs with local chapters or groups, such as the National Diabetes Prevention Program, Gerofit, and Walk With Ease, and there are also likely several local programs that are unique to your community. Exercise is Medicine created a community resources handout template 17 with ideas on places to walk, bike, or roll; community fitness clubs and medical fitness facilities; national programs with local chapters; and websites to find a personal trainer. Handouts like these can be customized by an office manager to include an updated list of in-network referrals for specialty care as well as information on physical activity programs in the local area. Additionally, a list of federally supported physical activity initiatives and resources for older adults are included in the Appendix of the Midcourse Report (see supplemental materials). 18
Additionally, many patients, particularly if they are managing chronic disease or have had a recent injury, would benefit from a referral to an additional provider or exercise professional, such as a personal trainer, physical therapist, or occupational therapist. These additional providers can assess older adults’ mobility and help them create an individualized activity plan.
Occupational therapists—clinicians who help people across the lifespan do the things they want and need to do through the therapeutic use of daily activities (occupations). Occupational therapists help people promote health and prevent—or live better with—injury, illness, or disability.
Physical therapists—clinicians who have specialized training in human movement. Physical therapists provide hands-on care, patient education, and prescribed movement to help people manage pain and chronic conditions, improve physical function and fitness, and improve quality of life.
Exercise professionals—individuals who facilitate and lead physical activity programs in community-based settings such as health and fitness facilities, recreation centers, and senior centers (e.g., exercise physiologists, personal trainers, fitness and yoga instructors, certified exercise professionals, trained recreation leaders, program managers).
Conclusion
Increasing physical activity may allow older adults to live independently longer, be healthier, have better quality of life, and need less medical care, thus benefiting older adults themselves, and the population overall. Internists, as trusted members of a health care team, can help their patients gain confidence, stay motivated, and create a sustainable and enjoyable physical activity routine. Health care professionals, organizations, policymakers, and community members can coordinate across sectors to create opportunities and environments that help promote access to physical activity among older adults. It is never too late to start being active and getting the benefits of an active lifestyle.
Supplemental Material
Supplemental Material - Physical Activity in Older Adults: What Every Internist Needs to Know
Supplemental Material for Physical Activity in Older Adults: What Every Internist Needs to Know by Katrina L. Piercy, Malorie Polster, Bianca Macias, and Alison Vaux-Bjerke in American Journal of Lifestyle Medicine
Supplemental Material
Supplemental Material - Physical Activity in Older Adults: What Every Internist Needs to Know
Supplemental Material for Physical Activity in Older Adults: What Every Internist Needs to Know by Katrina L. Piercy, Malorie Polster, Bianca Macias, and Alison Vaux-Bjerke in American Journal of Lifestyle Medicine
Footnotes
Acknowledgments
The author would like to acknowledge the additional members of the Physical Activity Guidelines for Americans Midcourse Report: Implementation Strategies for Older Adults federal writing team for their contributions to the report including: Ken Rose, MPA, David R. Brown, PhD, FACSM, Geoffrey P. Whitfield, PhD, MEd, Christina Dahlstrom, MPH, and Graycie Soto, MPH, from the Centers for Disease Control and Prevention; Dana L. Wolff-Hughes, PhD, Richard P. Troiano, PhD, Lyndon Joseph, PhD, Stephanie M. George, PhD, MPH, MA, and Adrienne Jackson, PT, PhD, MPA, from the National Institutes of Health; and Noelle Harada, MPH from the Office of the Assistant Secretary for Health.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The development of the Physical Activity Guidelines for Americans Midcourse Report: Implementation Strategies for Older Adults was funded by the U.S. Department of Health and Human Services.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
