Abstract
The purpose of this article is to discuss the important role for physicians in advocating for the prevention of road traffic and firearm injuries. Physicians have shown to be effective advocates for a variety of injuries, and this needs to continue and be enhanced for these injury categories. Road traffic and firearm injuries are among the leading causes of death across the lifespan. The influence and credibility of physicians enhance the messages they provide in advocacy efforts. It is important that physicians educate and counsel patients in a variety of healthcare settings along with joining advocacy efforts of professional associations. Recommendations are provided for advocacy components related to these injuries. Also, it is very important that physicians receive training in medical school and/or residency about injuries and how to successfully advocate for evidence-based injury prevention strategies.
The voices of physicians could make a measurable difference in the number of injuries and deaths
There is a critical role for physicians and public health professionals to play in public health advocacy and building advocacy skills. 1 Because many of our greatest health achievements include clean water, passage of laws limiting toxic substances, laws removing lead from products, and use of seatbelts and more, 2 learning and using public health advocacy skills is considered a good investment. 3 The role of the physician as an advocate has been supported by several national and international physician organizations, including the Accreditation Council of Graduate Medical Education in the United States as advocacy has been added to the core competencies. 4 Also, the role of physician responsibility in relation to influences on health has been shown to lie in domains of professional obligation, including individual patient care and addressing socioeconomic influences and access to care. 5 Also more professional aspirations (beyond obligations) may include physicians, along with citizens, having a role in addressing broader health determinants and global health influences. 5 The important take-home message here is the need for physicians to be advocates not only for individual patients but when at all possible for the broader healthcare system.
Physicians have a unique opportunity to be advocates due to the credibility and power of the profession to promote policies and legislation regarding several areas of injury, including road traffic injuries and firearm safety. 6 This perspective will focus on these 2 major types of injury as they are among the leading causes of injury morbidity and mortality across the lifespan in the United States. In addition, a focus will be on the ways physicians can contribute to injury prevention and control as well as dealing with the assumption that advocacy is not a physician’s job.
Firearms: In 2019, there were nearly 40 000 deaths in the United States due to firearms—most of these being suicide.
7
It has recently been reported that firearm deaths cost over 280 billion dollars per year.
8
In 2019, 44 major medical and injury prevention organizations joined the American Bar Association to address firearm injury as a true threat to public health at the Medical Summit on Firearm Injury Prevention. Special policy recommendations include the following:
9
Comprehensive criminal background checks for all firearm purchases, including sales by gun dealers, sales at gun shows, private sales, and transfers with limited exceptions. Research to help better understand the causes and consequences of firearm-related injury and death and to identify, test, and implement strategies to reduce these events. Offenders who have been adjudicated guilty of a crime of violence against a family member or intimate partner, including dating partners, cohabitants, stalkers, and those who victimize a family member other than a partner or child should be reported to the National Instant Criminal Background Check System and be prohibited from purchasing or possessing firearms. Safe storage of firearms particularly in homes with children, adolescents, people with dementia, people with substance abuse disorders, and the small subset of peoples with serious mental illnesses that are associated with greater risk of harming themselves and/or others. Improved access to mental health care and caution against broadly including all individuals with a mental health or substance use disorder in a category of individuals prohibited from purchasing firearms. Extreme risk protection order (ERPO) laws where families and law enforcement can petition a judge to temporarily remove firearms from individuals at imminent risk for using them to harm themselves or others should be enacted in a manner consistent with due process. Physicians can and must be able to advise patients on issues that affect their health, including counseling at-risk patients about mitigating the risks associated with firearms in the home and firearm safety. This can occur confidentially during examinations. A common-sense approach to reducing casualties in mass shooting situations must address high-capacity magazines and firearms with features designed to increase their rapid and extended killing capacity.
Advocating for these changes and promotion of related legislation and policies could make a real difference in morbidity and mortality related to firearm violence. Physicians have already shown to be important advocates in many areas of injury prevention including wearing bicycle helmets, promotion of four-sided pool fencing and drowning prevention, use of seatbelts, and more.
Being advocates and working with the injury prevention community are common and ethical roles for the medical profession. 6 In addition to patient visits to physicians, there are good opportunities to intervene with education and counseling when treating injured firearm and other injury victims at trauma centers and other locations. 10 Trauma centers are excellent venues for injury prevention education as this is a requirement for verification by the American College of Surgeons. Success has been shown with these educational endeavors. In addition, advocacy related to firearm safety needs to be part of curricula for medical students and residents. For example, researchers recently found that very few medical school curricula include gun violence, which is the leading method for suicide, yet there are ample ways to do this within existing curricular components. 11 A few examples of curricular areas where gun violence could be incorporated include pathology, trauma care, identifying risk factors and prevention screening questions, adverse childhood events, the biopsychosocial model, psychiatry, exam/interview skills, surgery, mass casualty management, spinal cord injuries, rehabilitation, medical ethics, and more. 11 In addition, interdisciplinary coursework/modules/programs focused on advocacy skills, building and working with coalitions, policy and legislative processes, and communication skills could help medical students and residents learn those skills that will prepare them to reach patients and families with evidence-based firearm injury prevention strategies. 12 Such curricula are available for use. 12
Road Traffic Injuries: Around 1.36 million people die in road traffic crashes (RTCs) every year and more than 50 million suffer from nonfatal injuries worldwide. 13 Road traffic crashes and injuries are increasingly becoming a public health issue all over the world.
Evidence of the societal impact of road traffic injuries (RTIs) are grave; for instance, US medically consulted motor-vehicle injuries costs totaled 4.5 million in 2019, and total motor-vehicle injury costs were estimated at $463 billion that included medical expenses, wage and productivity losses, administrative expenses, motor-vehicle property damage, and employer costs. 13 Despite the COVID pandemic, the National Highway Traffic Safety Administration reported that an estimated 28 190 people in the United States died in motor vehicle traffic crashes in the first 9 months of 2020, which is higher than in the same period in 2019. 14
The safe systems approach to road safety was developed in Sweden—where it is locally known as “Vision Zero”—to curb the road crash–related mortality and morbidity. This approach recognizes that humans are imperfect and thus encourages a shared responsibility between road users, vehicles, and infrastructure to ensure an elevated level of safety. 15 The safe system approach builds on the unique strength of each sector—governmental agencies, private organizations, and non-governmental organizations (NGOs)—to integrate road safety into different policies systematically, both vertically within each sector and horizontally across sectors.
In this complex situation, the health sector is well-positioned to play a leading role in developing and integrating road safety into its mainstream agenda. Reducing the incidence of road traffic injuries not only improves population health but also likely has far-reaching health benefits by addressing the key risk factors for road safety. 16
It is important to recognize that the health sector bears a large part of the socioeconomic burden of road injury. Physicians and their patients would benefit from better road injury prevention through fewer hospital admissions, reduced severity of injuries, and rehabilitation of the survivors. There are several ways where physicians could play a key role in highlighting the need for concerted efforts for road safety as described below: (1). Promoting safe road practices is key. Behavioral factors including driving under the influence, speeding, distracted driving, under-utilization of seatbelts and child restraints, driver fatigue, lack of knowledge about road safety procedures, and dangerous pedestrian behaviors are some of the leading causes of road crashes across the world. Physicians treating road injury victims could become powerful advocates for helmet use, car restraints, increased visibility of vulnerable road users, respect for pedestrians and bicyclists, and avoidance of alcohol and recreational drugs while on roads or anticipating road travel while working with patients at the bedside and through follow-up visits. (2). Forming intersectoral partnerships, telling stories of survivors, and highlighting long- and short-term impacts of road injuries would be an effective way to engage with people to promote understanding of their own risks. (3). Working to join and form strong health coalitions to improve post-crash outcomes, from appropriate and life-saving measures at the scene of the crash through rehabilitation services. (4). Promoting multidisciplinary research to study the effectiveness of road safety measures, policy interventions, and improvement of post-crash care services. (5). Our knowledge about the longer-term physical, psychological, and economic impacts is still scant, as is our knowledge about the impact of RTIs on healthcare systems. Consequently, developing a research agenda to access this information might provide a useful stimulus to mobilize resources and action. (6). Providing technical guidance to aid in evidence-based policy changes, whenever possible.
While medical education prepares physicians to provide the best care available, better approaches are needed to take a closer look at the behavioral, social, and economic risk factors exposing individuals and society to the broader impacts of firearm and road traffic injuries. This should begin with including offerings focused on the socio-economic determinants of health, injuries and advocacy into undergraduate and medical school and residency curricula. Earnest and colleagues defined physician advocacy as “action by a physician to promote those social, economic, educational, and political changes that ameliorate the suffering and threats to human health and well-being that he or she identifies through his or her professional work and expertise.” 17 Formal basic training in advocacy needs to be interwoven into educational curricula so that physicians are better prepared and feel confident for actual advocacy implementation. For example, the Advocacy Mentoring Initiative (AMI) uses a successful cascading mentoring model to guide hands-on advocacy training for undergraduate medical students where undergraduates serve as peer mentors to at-risk youth, while being mentored by physician residents themselves. 4
Using evidence to inform policy and advocating for equitable resources for vulnerable populations, increasing health coverage, and improving outcomes have long been well-established strategies used by clinical researchers. 18 Physician efforts through medical society affiliation and state healthcare reform, coalition and board leadership, being an advisor to school boards, being healthcare advisors for policy makers, being a health liaison to media, and being an advocate for change in one’s own settings are examples of mechanisms for change. 17 The voices of physicians could make a measurable difference in the number of injuries and deaths.
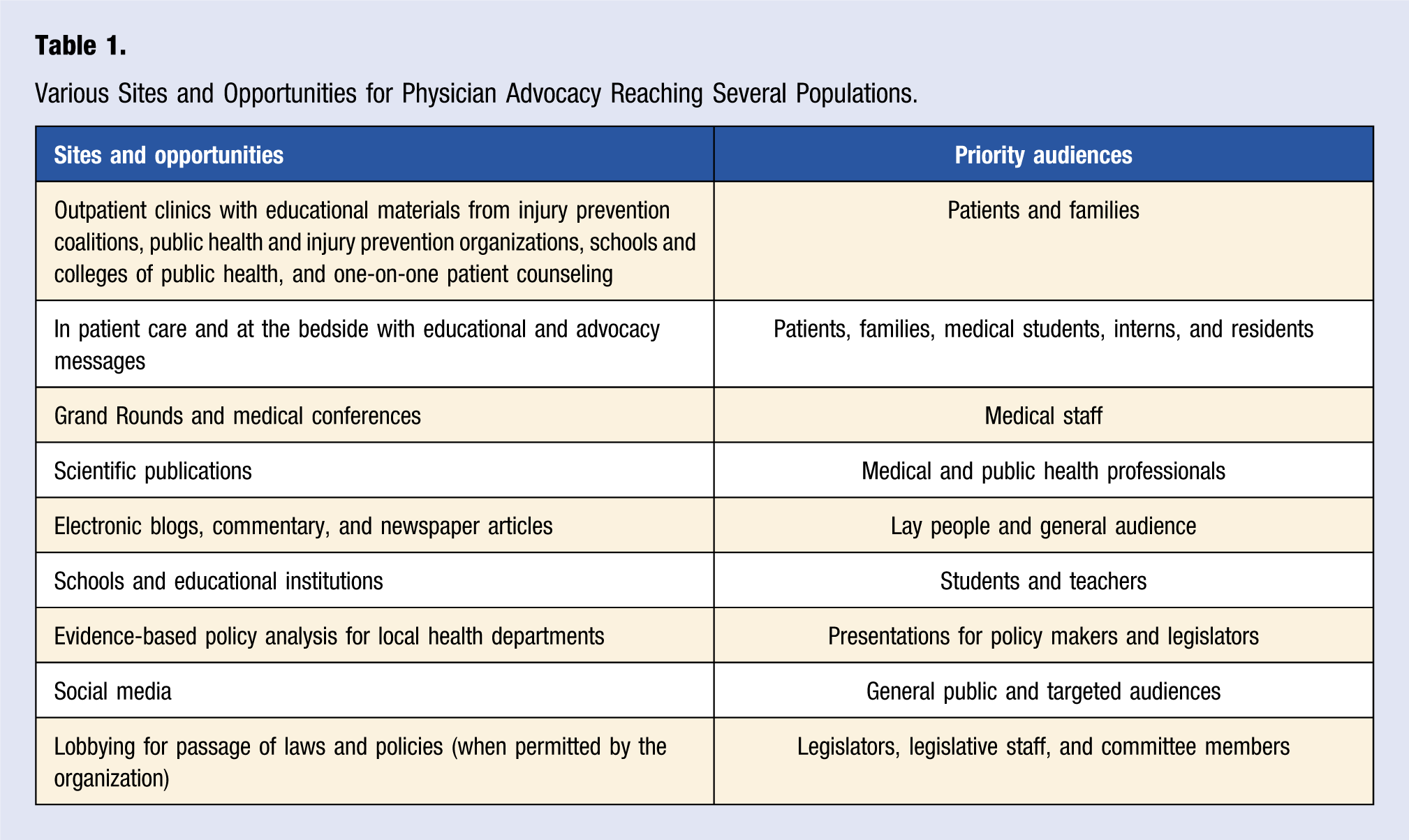
Various Sites and Opportunities for Physician Advocacy Reaching Several Populations.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
