Abstract
Over 2 decades ago, the United States National Academy of Sciences described injuries as “the most under-recognized major public health problem facing the nation.” Our progress since then has been limited. Injuries still account for nearly 1 out of every 10 deaths in the world, and the global burden of injury is projected to increase over the next decade, predominately in low- and middle-income countries. Despite this, injury prevention receives scant attention from legislators, the education system, and, most strikingly, the health care system. The lifestyle medicine community, however, is beginning to focus on injury prevention and will play an increasing role in helping control the burden of injury. Lifestyle medicine practitioners are in a tremendous position to promote injury prevention. Physical activity and positive lifestyle changes can be accompanied with an increased focus on preventing injury. Lifestyle medicine can prevent injuries by supporting legislation, advancing medical advocacy, providing community education, and linking clinical care with injury prevention.
‘In the United States, the burden of injury disproportionately affects the young and is the number one cause of death among children and adults under the age of 45 years.’
Injury: A Leading Killer
Injury is defined as physical damage to an individual caused by the transfer of energy and can be from either unintentional or intentional causes.1,2,3 Unintentional injuries typically include motor vehicle collisions, falls, burns, drowning, and poisonings. Intentional injuries are purposeful, either through self-harm (suicide) or inflicted injury (homicide, assault, sexual violence, child abuse, elder abuse). Injuries are a leading cause of death worldwide. 1 In the United States, the burden of injury disproportionately affects the young and is the number one cause of death among children and adults under the age of 45 years. 4
Even so, these numbers are still minor in comparison to the tens of millions of annual emergency department visits and hospital admissions from nonfatal trauma, in the United States alone. 5 Trauma is the leading cause of potential years of life lost, and the economic burden is in the hundreds of billions of dollars. 6 This still fails to capture the extent to which injuries affect the well-being of the individual, their families, the community, and society.
Current medical practice can attempt to treat the severely injured patient, but the majority of trauma-related deaths occur at the scene of the injury.7,8,9 Most estimates are that over half of severely injured patients die at the scene or shortly after presenting to the emergency department.7,8,9 Those patients that do present to the hospital with severe injuries have a very grim prognosis. Neurological damage in particular is largely irreversible. The only cure for these injuries is prevention.
The Ripple Effect of Traumatic Injury
It is difficult to comprehend or measure the impact of injury on individuals and their families. For example, an individual who is involved in a motor vehicle collision and sustains a traumatic brain injury accrues the cost of acute hospital care, plus months if not years of rehabilitation. This patient may require care for the remainder of his or her life. This represents an enormous productivity loss. For families that care for injured loved ones, the psychological effects can be equally devastating. Yet injuries are preventable. So why has more not been done to prevent a leading cause of death and disability?
Obstacles to Injury Prevention
Injuries and the need for injury prevention has been recognized for decades, but not until the 1985 Institute of Medicine report was there a recognition that public health and medicine should take on this challenge. 10 Yet progress has been slow. Despite the high burden from injury, legislative responses have been guarded. Similarly, support for injury prevention research is disproportionately low compared with heart disease or cancer.11,12
Injury prevention is a multistep process that requires participation from all levels of government, law enforcement, justice, education, and health. Injuries are inherently complex, requiring a systematic approach to understand their etiology. 13 Health care professionals are essential in framing the problem, but need the expertise of epidemiologists, engineers, economists, and legislators. Interdisciplinary teams certainly add complexity to the problem of injury prevention, but information technology is beginning to make advanced collaborations possible. 14
How to Prevent Injuries
Approaches to injury prevention can be either passive or active. Passive strategies are those that operate automatically—they are installed or implemented in such a way that they do not require repeated action by the user or individual at potential risk. Common passive injury prevention measures are automatic sprinklers in a home to put out a fire, child resistant safety caps on medications to prevent childhood poisoning, 4-sided pool fences to prevent drowning, and automatic vehicle airbags. Active strategies, on the other hand, require repeated user participation, such as fastening seat belts or wearing lifejackets. Both strategies can be highly effective in injury prevention. Passive strategies inherently have greater potential for large population benefits if they are designed properly, work effectively, and are not disengaged by human actions.15,16
Examples of Recent Success
There has been recent success in preventing injury, best exemplified by the safety advances with the motor vehicle. Motor vehicle–related deaths have been declining for decades, as numerous safety measures have been implemented in vehicles. 17 This begins with understanding the problem of motor vehicle–related injuries, how they occur, and how they can be prevented. To do this, a national regulating body provides timely feedback as to how injuries and fatalities are occurring, and makes injury prevention recommendations (eg, recommendations on seat belts or specific product recalls). Vehicles are subject to these rigorous safety standards that constantly evolve and injury rates are monitored over time. 18
Driver behavior has also changed as a result of improvements in policy, education, training, and efforts to reduce impaired driving.19,20 Few areas of injury prevention have been as systematic and rigorous as the efforts to reduce drinking and driving. 21 One approach that may advance motor vehicle safety may be the autonomous (driverless) vehicle. 22 Vehicles that are designed to reduce human error have the capacity to further reduce motor vehicle collisions. The safe testing and production of these vehicles holds potential to reduce injury, but still requires development.
Australia has made great progress in the domain of injury prevention.23,24,25 Legislative interventions have included strict limits on blood alcohol level (0.05%) and random breath testing. Speed limits have been reduced in many urban areas and are enforced, although convincingly, the territory with the most liberal speed laws has the highest number of fatalities. 26 Australia was also the first country to make seat belt use compulsory, and helmet use by motorcyclists in Australia approaches 100% compliance.26,27 While more work is needed, Australia has made tremendous progress in a short period of time and stands as a model for advancing injury prevention using a comprehensive approach of legislation, education, advocacy, and political will.
Injury Prevention: Can We Legislate Safety?
There are convincing data that safety legislation can have a profound impact on reducing injuries and death. This includes seat belts and child restraints, airbags, helmets for motorbikes and bicycles, installing smoke alarms, and 4-sided fencing for pools and open water.28,29 Different localities have had various degrees of success in passing safety legislation. Public pushback largely limits what legislation can be passed. But with appropriate consultation, the public largely does support injury prevention legislation. 30 Cellphone-free driving is a good example whereby the public may benefit, yet there is not a widespread adoption of such legislation. 30
Legislators in North America have had success in passing laws that restrict driving under the influence of alcohol. 20 Despite this, driving under the influence of alcohol remains a major cause of motor vehicle collisions. 31 Media campaigns and law enforcement is needed to ensure compliance with drinking and driving legislation. Sobriety checkpoints, license revocation, age 21 drinking laws, and other system-based interventions have been shown to be effective. 32 Legislators, politicians, and law enforcement cannot do this without advocacy from the medical community. The lifestyle medicine community specifically can support legislators and policy that eliminates driving under the influence.
Education: Teaching Injury Prevention
The education system has an important role in protecting children and youth from injury. Lifestyle medicine practitioners should work with the education system to develop and foster early interest in sport and healthy activities. Early education programs that focus on injury prevention can help sustain lifelong habits. Youth need to know that injury is real and preventable, especially those that take part in high-risk activities (impact sports like football or hockey, or adventure sports like skiing or mountain biking). Practitioners that work with active youth should be knowledgeable about the appropriate safety equipment particular to their respective sports and activities. Formal sport and activity programs should encourage injury prevention activities such as pre-activity warm-up and flexibility exercises, and the mandatory use of appropriate safety equipment.
Lifestyle medicine can help sport and activity organizations, educators, and coaches advocate for injury prevention. Organizations that promote sport and activity are often the first to realize the types of injuries that occur in their sport. Governing organizations can take an active role in promoting safe lifestyle change in these and other sports. For example, requiring a helmet for hockey or cycling sets a good example to those that follow the sport, particularly children. Closer to sport, coaches and mentors are in a great position to positively influence youth’s perception of injury and promote sport-specific injury prevention behaviors.
Media: If It Bleeds It Leads
Media has capitalized on the public interest in violence. Violent incidents capture headlines, in particular car crashes and the use of firearms. The media often portrays these as terrible accidents that can happen to anyone. 33 However, these are not random accidents but rather predictable events that occur when injury prevention measures fail. This discussion can be improved and terminology is important. Lifestyle medicine professionals must speak of injury rather than accidents, since an accident denotes a chance event, whereas an injury refers to the damage inflicted. For example, language that attributes a traumatic event to just a fall, or a car accident, is unhelpful and does not focus on the predictable nature of injury, nor address that injuries are preventable.
Health care professionals should emphasize that injuries can be prevented and work with the media to portray this message. Headlines that capture the preventable nature of injuries can encourage communities to expect change. Lifestyle medicine practitioners have authority to help shape this debate.34,35 Lifestyle medicine experts can address the fact that positive lifestyle change and activity is a good thing and can be done safely. Scare tactics about the dangers of sport and leisure is unhelpful. Rather, a frank discussion about injuries and prevention can help patients achieve healthy, safe lifestyles.
Health Care: A Renewed Focus on Preventive Medicine
The management of injuries is complex, interweaving prehospital care, transport, and hospital-based care. The care of these patients comes at incredible cost to the individual and to the system. Injuries are an end result, and little focus is paid to the core problem: the predictable circumstances that lead to injuries. The lifestyle medicine practitioner has an opportunity in the patient relationship to prevent injury. Many lifestyle interventions involve increasing activity, which has its own potential for injury. This represents an opportunity for lifestyle medicine to promote positive lifestyle change while preventing injuries, at the patient encounter and with medical advocacy.
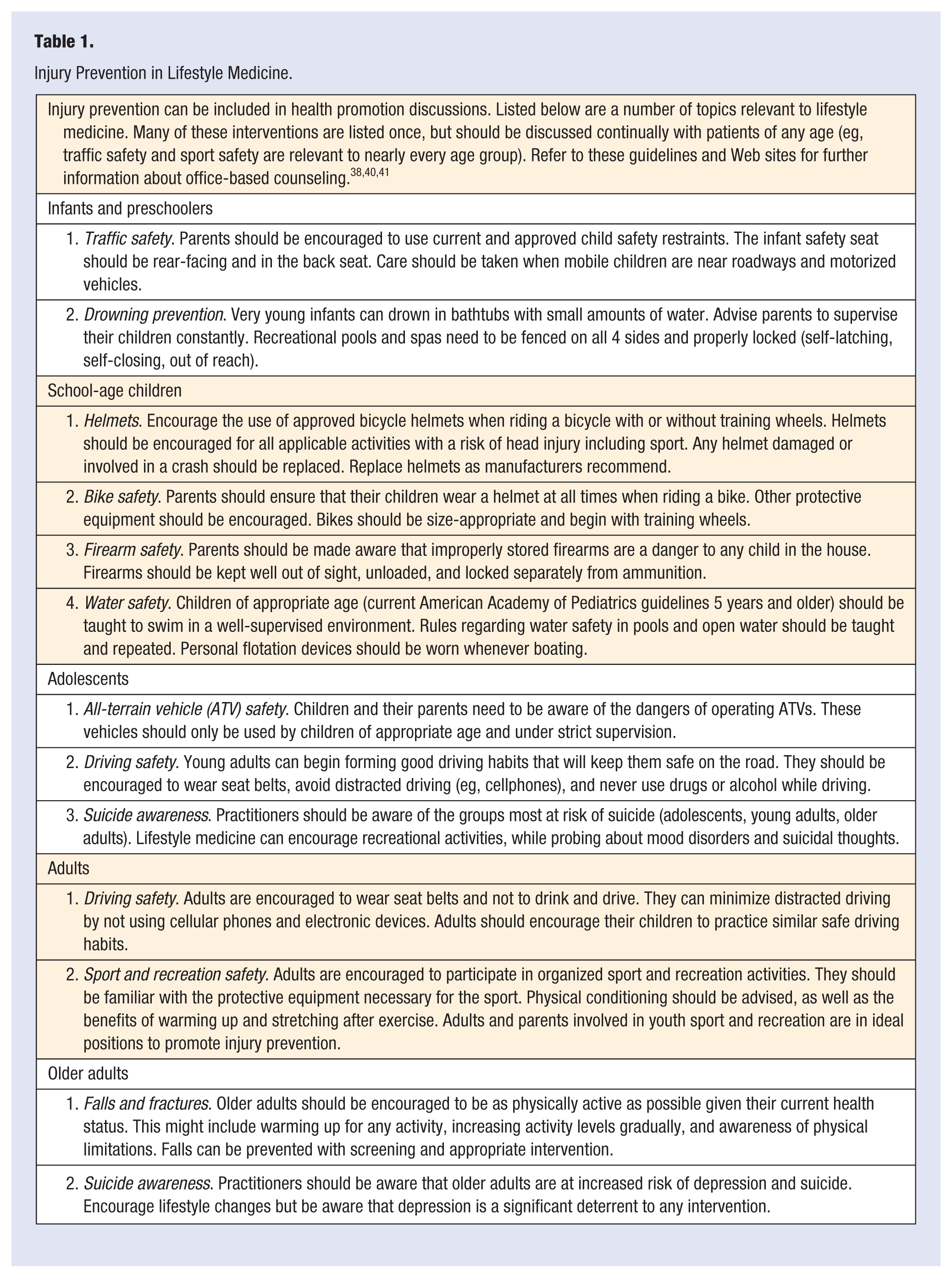
Lifestyle medicine interventions for injury prevention have been shown to lower the risk of injury, and should be included in health promotion activities. 36 We encourage lifestyle medicine practitioners to inquire about high-risk lifestyles, document risk factors, and intervene where appropriate. Listed in Table 1 are a number of injury prevention topics relevant to lifestyle medicine. The discussion about preventing injury needs to be tailored to the age of the patient or patient’s children, their recreational interests, and their activity level. This should be an open dialogue that encourages activity, identifies the potential risks for injuries involved, and promotes specific injury prevention behaviors. This includes the value of risk recognition, proper training and certification, the use of personal protective equipment, and adherence to safety rules and regulations.
Injury Prevention in Lifestyle Medicine.
Health care providers can advocate for their patients by promoting public safety legislation and policy. This begins with defining the injury and outlining preventative strategies to relevant stakeholders (Figure 1). Health care professionals can also advocate by supporting organizations that promote injury prevention.37,38 Community-based organizations, volunteer groups, nongovernmental organizations, and sports organizations are often invaluable in delivering the message of injury prevention to the public. Finally, lifestyle medicine practitioners can also advocate for better preventive medicine from their health care institutions, which should have an organized and evidence-based approach to injury prevention. 39 Trauma teams are often inundated with the task of caring for the injured patient, and little time or education is devoted to injury prevention. 39 Health care advocates can encourage trauma centers to implement and measure their preventive medicine efforts.
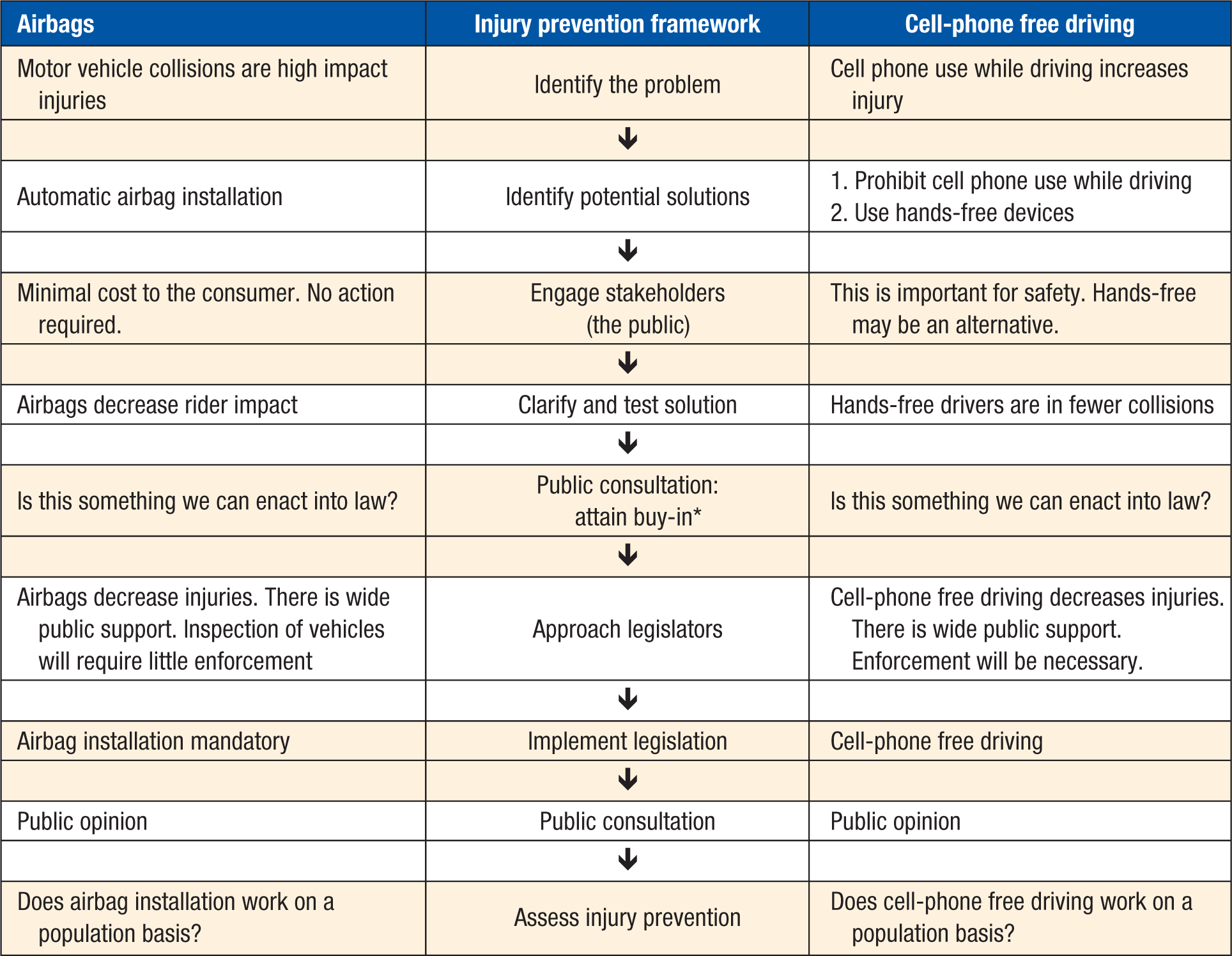
A Framework for Injury Prevention Advocacy.
Moving Forward With Injury Prevention
Injury is a critical public health problem that has an immeasurable social cost. Individuals, families, communities, and societies are all affected by injury. The health system should view injury as a preventable disease, as it does for infections or chronic diseases, such as heart disease. Practitioners that encourage activity and healthy lifestyles can also encourage injury prevention. This is a multidisciplinary, team effort that involves the education system, media, and lifestyle medicine. The education system can emphasize that injuries are preventable, and the media can assist with supportive messaging. The public needs to see injury not as random accidents but as foreseeable and preventable events. Lifestyle medicine practitioners are in a position to shape the discussion on injury prevention, improving the health and well-being of their patients and the communities in which they practice.
