Abstract
Research suggests that mental health symptoms and disorders are historically underdiagnosed and undertreated, in part due to the siloed nature of medicine. Yet, approximately 50 million American adults experience a mental health disorder. As the field of lifestyle medicine continues to emerge and grow, there is an important opportunity to address mental health from a lifestyle medicine perspective, as well as to ensure that lifestyle medicine can be utilized for all patients, including those with mental health conditions. To effectively address mental health, the field of lifestyle medicine would benefit from understanding and leveraging the decades of science and practice from the fields of psychiatry and psychology, as well as the expertise of psychiatrists and psychologists who are familiar with the science and trained in lifestyle medicine. Incorporating empirical literature from other areas, utilizing well-established conceptual frameworks, and addressing the overlap between lifestyle medicine and mental health early in, and throughout, training and education, are important steps to move toward addressing mental and behavioral health with a lifestyle medicine approach.
‘In the United States, almost 20% of the many years of life lost due to disability are attributable to mental illness.’
Mental health symptoms and disorders are globally pervasive and greatly affect productivity and quality of life for many. Mental health refers to a cognitive state characterized by psychological and emotional well-being, ability to cope and adjust to stressors, capacity to engage in healthy relationships, and minimal influence of disabling psychological symptoms 1 (Table 1). In the United States, approximately 50 million, or 1 in 5, adults experience a mental disorder. 2 Among young adults, aged 18 to 25 years, rates of mental illness are as high as 30%; and as of 2018, suicide was the tenth leading cause of death among American adults.2,3 Furthermore, mental illness is profoundly costly. The global cost of mental illness, accounting for medical expenses, lost productivity, and so on was 2.5 trillion dollars in 2010, with mental illness accounting for more than 30% of disability.4,5 In the United States, almost 20% of the many years of life lost due to disability are attributable to mental illness. 5
Key Definitions.
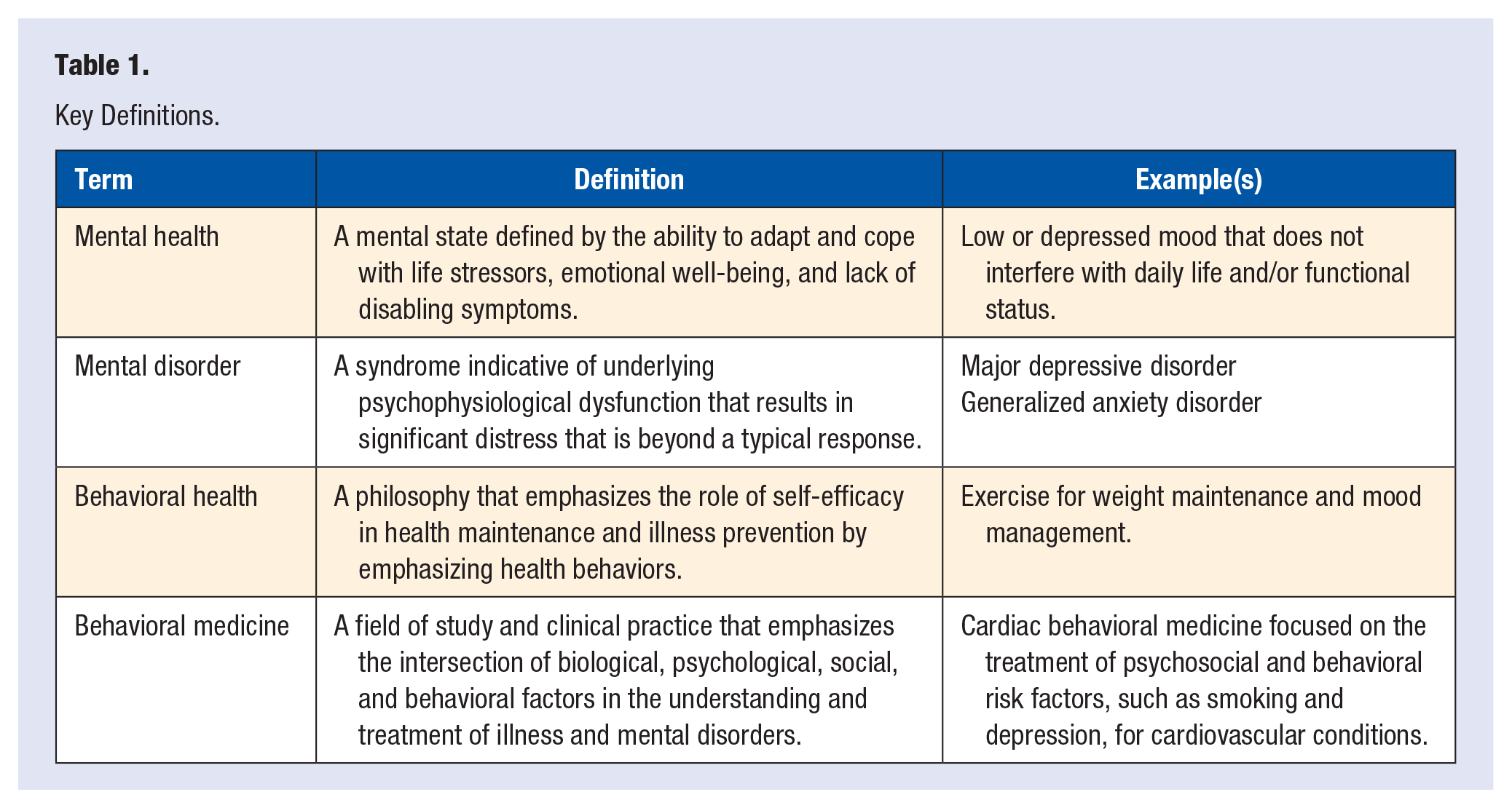
In response to these needs, most individuals with a mental health disorder will first seek mental and behavioral health care from their primary care physicians (PCP). 6 Behavioral health is an area of specialty practice that attends to mental health while also emphasizing engagement in the prevention, treatment, and maintenance of health and medical conditions through health behaviors such as diet and exercise. 7 Astoundingly, approximately half of psychotropic medications are prescribed by PCPs, and yet up to two-thirds of PCPs struggle to find and understand where to refer their patients for mental health treatment.6,8 Of the few patients who are referred to speciality psychiatric care, up to half of them never follow up due to pervasive stigma around mental health diagnoses and treatment.9,10 Practices in recent decades have sought to reduce such gaps in care through the creation of evidence-based models that better integrate of mental and behavioral health in both primary care and specialty medicine settings (eg, the Primary Care Behavioral Health collaborative care model).6,11 Thus, the integrative nature of lifestyle medicine could well extend such efforts to integrate care and reduce the burden of mental health.
Meeting the Goals of Lifestyle Medicine
The burgeoning field of lifestyle medicine uniquely attends to the role of lifestyle in disease prevention, treatment, and disease reversal. Lifestyle medicine clinicians utilize evidence-based approaches to leverage lifestyle changes for the prevention and treatment of chronic health conditions. One strength of lifestyle medicine isits interdisciplinary nature. Lifestyle medicine professional organizations draw on a range of clinicians, researchers, and other practitionerswho contribute a rich depth of knowledge and expertise to the growing field. For example, lifestyle medicine builds on disease prevention research by Dean Ornish, MD, as well as nutrition and obesity work by David Katz, MD.
Lifestyle Medicine and conventional allopathic medicine have much in common. Lifestyle medicine accepts the same pathophysiology of the etiology of disease and is consistent with conventional medicine’s emphasis and utilization of evidence-based principles. Lifestyle medicine differs in focus in clinical practice from conventional medicine. The most common areas of emphasis within lifestyle medicine include (plant-predominant) nutrition, sleep, physical activity, tobacco cessation, risk reduction of substance use, and social connectedness. These pillars are consistent with the foundational literature on health behaviors and lifestyle for optimal health and quality of life.12-14 Specifically, lifestyle medicine has been shown to prevent and reverse disease by encouraging an active role by both the provider and the patient in treatment while conventional medicine focuses on acute symptoms and employs a less active approach.12-14 Preventative Medicine is similar to Lifestyle Medicine in its focus on prevention. The major difference is that preventative medicine addresses health promotion of communities and individuals often from a public policy lens. Lifestyle medicine is distinct from other areas of medicine, including, integrative, functional, and complementary and alternative medicine (CAM)12-17 (Table 2).
Unique and Overlapping Areas of Specialty Medicine.
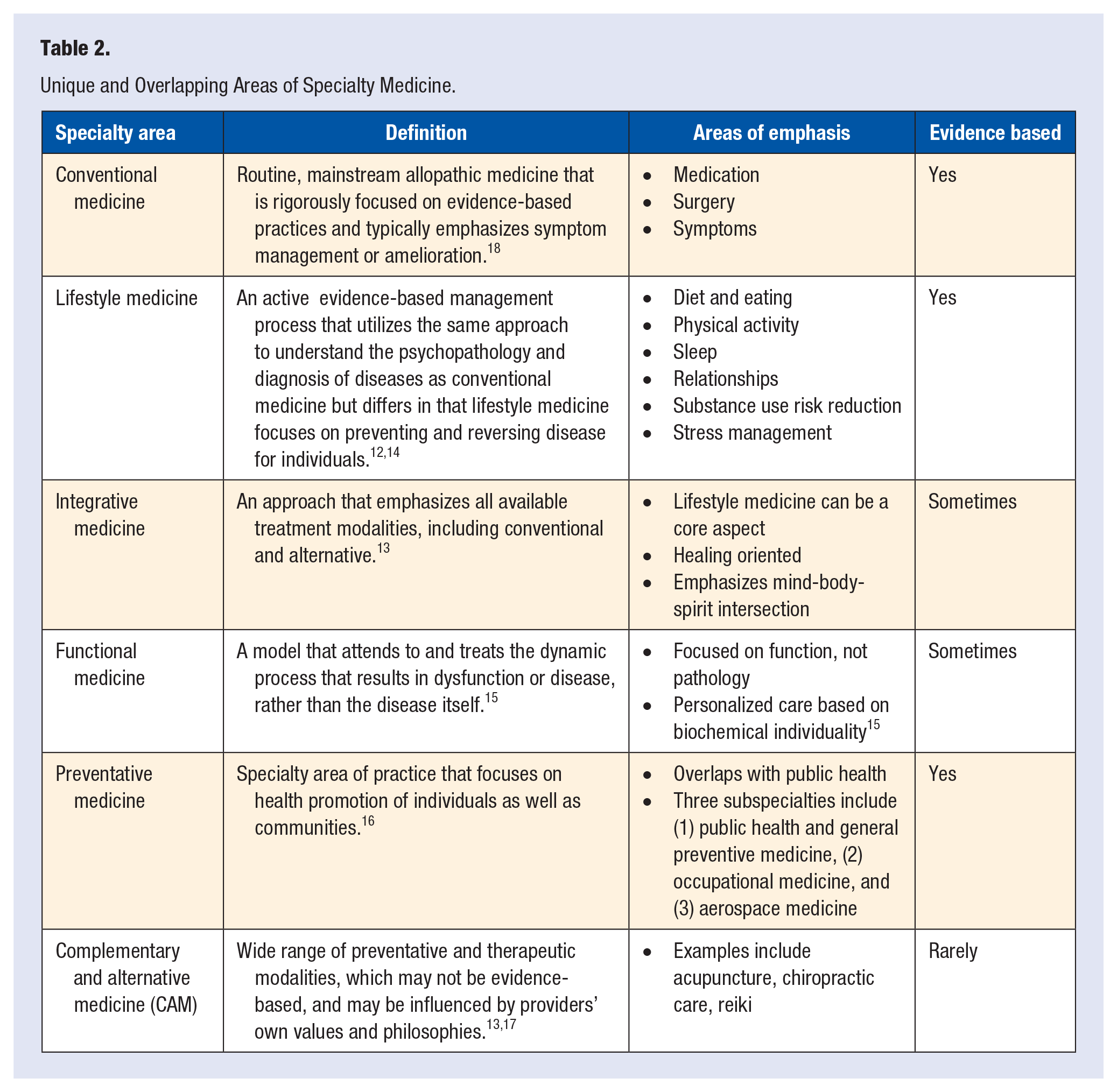
Because lifestyle medicine is nascent, there exists significant opportunity to leverage the expertise of diverse contributors to the field and to further develop research and clinical practice that serves all patients well. Specifically, addressing mental and behavioral health from a lifestyle medicine perspective is needed to best serve individuals with a range of mental health symptoms and conditions. In doing so, it is important to acknowledge the core theoretical frameworks employed by psychiatry and psychology, which have informed hundreds of years of clinical practice. This will ensure an evidence-based approach to mental health from a lifestyle medicine perspective. Analogous to PCPs learning and understanding foundational lifestyle medicine knowledge and interventions, the same rigor is necessary in approaching lifestyle interventions for mental and behavioral health.
What is known as the streetlight effect (ie, lamppost bias) in scientific research, or the bias of attending to only the information that is “under the light,” is also relevant to the growth of emerging areas of medicine.19,20 Lifestyle medicine is not immune to the regularly occurring streetlight effect that is pervasive in research and medicine, and thus, must make specific and targeted effort to look beyond the light and incorporate other areas of practice, diverse types of providers, and care for diverse patient populations, into the field.
The Need for Mental and Behavioral Health Within Lifestyle Medicine
Lifestyle plays an important role in the manifestations of mental health symptoms, treatment outcomes, and a person’s quality of life. The development of mental health symptoms and disorders is influenced by a multitude of intersecting factors, including biological predisposition (ie, genetics), psychological influences (ie, stress, coping skills), social factors (ie, health relationships), and environmental factors (ie, clean water, access to green space). Furthermore, mental disorders are well understood to be chronic in nature, and many traditional treatments have been associated with less than optimal success and treatment outcomes. 21 Thus, it is important to attend to behavioral mediation that affects mental disorders and mental health outcomes.
Risk factors do not directly correspond to outcomes, but rather, they are influenced by an individual’s health behaviors that occur in the context of their greater sociocultural environment and one’s access to resources. Fortunately, lifestyle factors can be leveraged to both to prevent symptoms of mental illness for “mentally well” individuals and to address and treat symptoms concurrently with traditional mediums (ie, medications, psychotherapy). Given the pervasive global impact of mental health and the traditional medical model of treating symptoms only after they become problematic, lifestyle medicine’s approach has much to lend to improving mental and behavioral health. Specifically, lifestyle medicine needs to incorporate mental and behavioral health research and practice, just as the fields of mental and behavioral health need to better study and incorporate lifestyle medicine.
Robust literature exists within the fields of psychiatry and psychology (including behavioral medicine 22 ) that address a range of concepts, practices, and interventions that overlap between mental health and lifestyle medicine. Reviewing current scholarship from psychiatry and psychology with the same rigor we use to assess other areas of medicine, such as primary care and cardiology, can strengthen the development of scientific literatureand lifestyle medicine practice to address and support mental and behavioral health. While there are many bodies of literature, it is well established that fields, and even specialty areas within fields, such as medicine, tend to be siloed, with little attention to the areas in which research and practice overlaps.23,24 This has been especially true with regard to chronic health conditions, such as diabetes, and chronic mental health conditions, such as depression. Given the multifaceted and interdisciplinary approach of lifestyle medicine, the integration of work in both physical and mental health is both relevant and necessary. The expertise of lifestyle medicine clinicians and researchers, whose foundational expertise is in mental and behavioral health, can thus be leveraged to adapt and expand the already existing work and develop a body of knowledge and practice that is lifestyle medicine driven.
Leveraging Expertise in Mental and Behavioral Health
Psychiatrists and psychologists can bring a unique perspective to lifestyle medicine because they are well trained in assessing and treating mental health symptoms and disorders with evidence-based practices, as well as interpreting, and even conducting important research in these areas. Many clinicians are already addressing aspects of lifestyle, given the emerging science in areas such as the role of nutrition on mental health.25,26 The comprehensive inclusion of mental and behavioral health within lifestyle medicine also has an important opportunity to continue to shift medicine, and areas of specialty practice such as psychiatry, toward a more comprehensive, whole-person approach to treatment.
Psychiatry and Psychology: Education, Training, and Expertise
To understand and outline the opportunity to leverage the expertise of those with specialty training in mental and behavioral health, this section will first outline the training of psychiatrists and psychologists. In our previous work, Mental Health in Lifestyle Medicine: A Call to Action, we began the discussion by describing the disciplines in some detail. 27 While this article will focus on psychiatrists and doctoral-level clinical and counseling psychologists, the authors acknowledge there are several other areas of specialty that are relevant to clinical practice within mental and behavioral health, including clinical social workers, counselors, master’s level psychologists, marriage and family therapists, and advanced practice providers (ie, psychiatric nurse practitioners, physician assistants).
Psychiatry Education and Training
Psychiatry is an area of medicine that attends to prevention, diagnosis, and treatment of mental and behavioral disorders. Psychiatrists are first and foremost medical doctors, who have typically earned a medical degree (MD or DO) before pursuing advanced training in psychiatry. Psychiatry residencies are 4 years in duration and include training in a variety of modalities and settings (ie, inpatient, outpatient, therapy, etc). Following residency, psychiatrists often pursue board certification with the American Board of Psychiatry and Neurology (ABPN), which requires recertification every 10 years. 28 Additionally, some psychiatrists pursue training in subspecialty areas after their 4 years of residency. The ABPN offers certification in 15 subspecialties, each of which have unique training and experiential requirements.29-31 Such breadth of subspecialties speaks to the range of clinical and research expertise within this area of medicine (Figure 1).
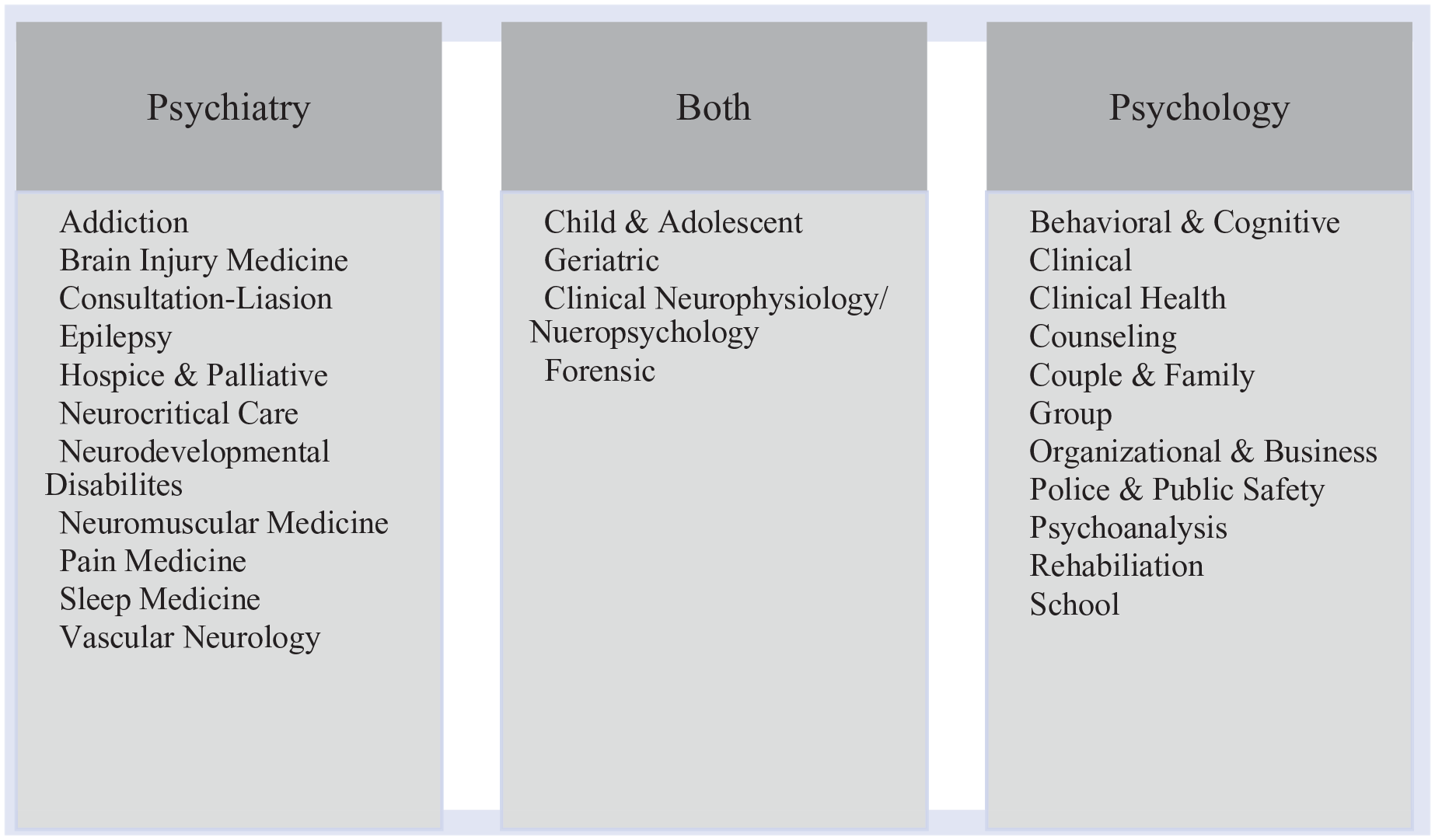
Areas of specialization and board certification in psychiatry and psychology.
Psychology Education and Training
The field of psychology is broad, with many subspecialties of research and practice. The current article will focus only on doctoral-level psychology training that prepares trainees for clinical practice in the United States. Practicing psychologists typically fall within 1 of 3 domains; clinical psychologists who earn a doctorate of philosophy (PhD) in (clinical) psychology or doctorate of psychology (PsyD), and counseling psychologists who earn a doctorate of philosophy (PhD) in counseling psychology. PhD programs typically take 5 to 7 years to complete, while PsyD programs tend to take 4 to 5 years to complete. 32 Each of these degrees provide the necessary training for students to pursue a full-time clinical residency (internship) and eventually licensure as a clinical psychologist.32,33 Many clinical and counseling psychologists will also complete at least 1 year of postdoctoral training in fellowship programs that emphasize clinical work, research, and/or teaching (ie, medical education)32,33 (Table 3).
Doctoral-Level Training in Psychology.

Psychology Subspecialties
Within clinical and counseling psychology, there are subspecialties with diverse areas of clinical practice and research. The American Board of Professional Psychology (ABPP) is the governing body that oversees the examination and certification of professional psychologists who engage in specialty clinical practice. Similar to the specialty practice in psychiatry, each specialty board has unique requirements to earn board certification and ABPP designation. 35 ABPP aligns well with medicine’s board certification model and provides psychologists a public recognition of competence in a specialty area of practice (Figure 1). Understanding the areas of expertise reflected by board certification is key to appreciating the overlap among the growing number of diverse health professionals who have also earned board certification in lifestyle medicine from the American Board of Lifestyle Medicine and the American College of Lifestyle Medicine.
Mental Health Conceptual Frameworks for Integration
The conceptual frameworks that serve as a foundation to training and education in mental health diagnosis and treatment for psychiatrists and psychologists are also relevant to the conceptualization of mental health from a lifestyle medicine approach. In the following section, we will discuss these frameworks in the order they were introduced in the literature. These include: the psychodynamic, biological/physiological, cognitive, cognitive behavioral, and humanistic frameworks, and their relevance to lifestyle medicine. These aspects can be used to conceptualize mental health within lifestyle medicine, as well as address mental health symptoms and conditions from a lifestyle medicine perspective.
Psychodynamic Framework
The psychodynamic framework laid important foundations for modern mental disorder conceptual frameworks. Psychodynamic theory emphasizes individual development, the role of early life experiences in one's view and interactions with the world, the key role of interpersonal interactions in shaping development, and the role of the therapeutic relationship in treatment with attention to transference and countertransference. 36 Furthermore, the psychodynamic approach focuses on communication, with attention to the reciprocal nature of both communication and relationships.36,37 The core concepts of causality, mutual influence, and feedback remain important to more modern mental health conceptual frameworks and play important roles in both mental health research and interventions. Unlike some of the newer conceptual frameworks, which have been transplanted into manualized treatments, for example, cognitive behavioral therapy (CBT), treatment that uses a psychodynamic framework is not manualized, but rather focuses on the previously noted areas of emphasis. Both the attention to early childhood experiences and to relationship communication are highly relevant to lifestyle medicine practice. Adverse childhood events (ACEs) are strong predictors of adult health and health behaviors and must be considered in context when prescribing individually specific and culturally sensitive lifestyle interventions. 38 Furthermore, patient-provider relationship is a predictor of treatment engagement and adherence to lifestyle interventions, such as plant-based dietary recommendations. 39
Biological/Physiological Framework
Early research on the brain, nervous system, and neural activity served as a foundation to the biological/physiological mental health framework. As early as the mid-1800s, research on physiological sensitivity threshold led to foundational appreciation of the connection between mind and body. Evolving science on the brain and consciousness eventually resulted in a more modern understanding of the role of neurotransmitters in mental illness. 40 The biological framework has been especially applied to our understanding of depression, with which major depressive disorder is believed to occur as a result of neurotransmitter and/or metabolic dysfunction. More recent biological hypotheses have emphasized the role of the stress-activated hypothalamus-pituitary-adrenal (HPA)-axis and inflammation.41,42 The impact of physiological processes, such as stress and inflammation, are also relevant to lifestyle medicine. For example, some dietary interventions have been associated with a reduction in systemic inflammation, and thus many support mental health functioning, including mood symptoms.43,44
Behavioral Framework
Behavioral conceptualizations of mental health symptoms and conditions stem from foundational understandings of operant and respondent styles of learning. Behavioral therapy has thus embraced learning theory, while also incorporating a focus on in-depth analysis of behavior (ie, behavioral analysis). 45 With this conceptualization, treatment is focused on identifying functional issues, such as poor stimulus control, and treatment is focused on a specific intervention to address and change said behavior. Behavioral treatment may include community contingency management (ie, token economy) or individual contingency management (ie, self-control procedures), exposure interventions (ie, systematic desensitization), and social skill development. 45 Behavioral interventions can also serve as an important foundation to lifestyle changes, which emphasize the change and maintenance of key health behaviors. For example, key behavioral interventions, such as reward systems and positive reinforcement, have been demonstrated to reduce some of the barriers to lifestyle change for individuals with severe mental illness, including lack of motivation due to mental health symptoms and medication side effects. 46
Cognitive Framework
The cognitive framework emerged from an understanding that a behavioral stimulus-response approach could not account for the important role of cognition. Cognitive theory instead focuses on processes of knowing and understanding, thus emphasizing the mental processes that occur in response to events rather than the stimulus-response characteristic of behaviorism. 40 Cognitive theory goes beyond understanding cognitions themselves to describe how they are organized and the human ability to actively participate in the acquisition of information. For instance, choosing to focus on and remember some information more than others. 40 The cognitive theory is especially relevant in the conceptualization of the important, and often underlying, cognitive processes that influence an individual’s ability to engage in, and maintain, lifestyle changes. Arguably most important among these processes are motivation and self-efficacy, as health behavior change theory clearly outlines that high levels of motivation and self-efficacy are necessary for effective change. 47
Cognitive Behavioral Framework
While both cognitive and behavioral theories can be utilized to distinctly make sense of human behavior and mental health, the cognitive behavioral framework is a clinical approach that ties together both of these theories. In CBT, the cognitive processes that impact how one feels and behaves and an individual’s behavioral engagement with the environment are considered in combination. 48 The cognitive behavioral framework is fairly broad, though typically employed through 1 of 3 approaches: coping skills, problem solving, and/or cognitive restructuring (the examination and change of dysfunctional thoughts). 49 Clinicians have applied the cognitive behavioral framework to numerous mental health symptoms and diagnoses, from depression to eating disorders, and CBT is the current gold-standard treatment for many mental health conditions, in part because it is the most well researched psychological intervention.50,51 The combined attention to both behaviors and cognitions is highly relevant to lifestyle medicine. CBT has been effectively employed in broad-ranging populations, such as type 2 diabetes mellitus, and resulted in both positive physiological and psychological outcomes. 52
Humanistic Framework
The humanistic framework was created as a direct response to psychoanalytic and behavioral conceptualizations of mental health conditions and treatment. Humanistic framework sought to move away from understanding people in the ways we understand machines and animals; thus, humanism centers on the belief in the wholeness of human nature by emphasizing free will, human strength, conscious experience, and positive aspirations. 40 Humanistic theory typically focuses more on positive attributes that contribute to psychologically healthy individuals, rather than focusing solely on negative attributes or deficits. 40 Some argue that positive psychology, developed by psychologist Martin Seligman, stems from the humanistic framework. 53 Psychological well-being, satisfaction with life, and social connectedness are all concepts that stem from humanistic theory, and influence overall health and well-being.40,53 Emphasizing the positive and helping patients live their best lives in alignment with their unique values can serve as an important foundation to effective lifestyle medicine practice. Understanding these foundational conceptual frameworks for mental and behavioral health can thus allow for thoughtful selection and utilization of the well-established scientific literature in psychiatry, psychology, and related areas. This thoughtful, interdisciplinary selection has the potential to break down silos and better incorporate mental and behavioral health within lifestyle medicine approaches.
Breaking Down the Health Care Silos
It is common practice in both medicine and psychology to stick to one’s area of specialty and/or practice. It is just as common for specialties to publish on the same topicwith little reach or research across the aisle. With the ever-emerging literature, it is difficult for providers to keep up with the science even in a very focused area or journal. Thus, it is unusual for clinical providers to spend time reading or gaining exposure to other areas of science. For example, burnout has been an important mental health topic in recent years, even more so in the context of the COVID-19 pandemic. The Journal of Healthcare Leadership, Psychiatry Research, Frontiers in Psychology, and the International Journal of Mental Health Nursing have published important work on burnout.54-57 Yet we know that many providers are not reading and learning from a wide range of areas. Because lifestyle medicine is early in growth and development, there is an opportunity to integrate the already existing and well-established work of other fields and to further the reach of the field.
One of the strengths of the lifestyle medicine approach, and the field of lifestyle medicine at large, is its interdisciplinary nature. Interdisciplinary team-based care has been associated with many positive outcomes, including patient safety, patient satisfaction, reduction in length of hospital stays, and overall improvement of quality outcomes. Team-based care has been associated with such outcomes in a variety of outpatient and inpatient settings, including emergency rooms, intensive care units, and operating rooms. 58 When optimized, interdisciplinary teams can draw on collective intelligence in science and practice, better quality of shared information, and leverage team member expertise to allow for fewer errors and better patient care. 59 Lifestyle medicine could similarly draw from the expertise of psychiatrists, psychologists, and other professionals to integrate mental and behavioral health science and practice, allowing lifestyle medicine to most effectively support patients.
The siloed nature of American medicine is well established, and its structure does not lend itself to optimal physical or mental health outcomes, as evidenced the prevalence of medical errors and poor outcomes, as well as high rates of heart disease, obesity, and depression, among other conditions.60,61 The relevance of lifestyle medicine to all areas of general and specialty practice makes it uniquely suited to support both patients and providers and to create necessary systemic changes. Thus, the field of lifestyle medicine has much to gain from incorporating the science of mental and behavioral health, and the broad fields of psychiatry and psychology also have much to gain from lifestyle medicine. For example, within psychology specialists in health psychology (often interchanged with behavioral medicine) who have typically undergone specialty training and clinical practice and may work in primary care or specialty medicine (eg, cardiology) settings. However, as of 2015, only 7% of psychologists indicated that health psychology was their primary specialty, which may limit patient access to experts in evidence-based health behavior change, as well as mental health. 62 Providing exposure to, and education in, lifestyle medicine early on in training programs will be critical to creating future generations of providers who are grounded in lifestyle medicine principles and approaches.
Leveraging (Early) Education
Education across the training trajectory and through postgraduate continuing education would benefit from great attention to lifestyle medicine, and the field has a unique opportunity to bring together both pre- and postgraduate education. Drawing from the expertise of diverse lifestyle medicine professionals could further support such efforts to address education as early as possible in the training trajectories of not only psychiatrists and psychologists, but medical students and other health professional trainees, from nursing students to physical therapy students. Interestingly, early interprofessional education, which includes students from two or more professions learning together, has been associated with positive attitudes toward members of other professions and greater skills for collaboration as compared to traditional learning.63,64 One review found this to be true among trainees from diverse fields (eg, nursing, social work), who received clinical training in mental health. 64 This could serve as an important model for the attention and integration of lifestyle medicine into early education and training which could lay a foundation for lifestyle medicine approaches throughout providers’ careers. Interprofessional education may also encourage professional advocacy for interdisciplinary care, which for mental health has been shown to be more effective than co-located care or referral to an outside provider. In fact, data has indicated that most people with mental health symptoms seek care from their primary care providers first and that mental health is addressed at greater rates in primary care settings than in specialty mental health settings.65,66
Research suggests that attention to prevention, lifestyle, and the role of health behaviors is lacking in medical education. For example, a 2019 review found that nutrition education during medical school remains insufficient on an international scale, and that medical students do not graduate with sufficient preparation to address nutrition with patients. 67 Lifestyle medicine could lead the effort to expand early medical education by specifically addressing the role of mental and behavioral health in lifestyle change and maintenance, as well as addressing the importance of lifestyle medicine approaches in various specialty areas of medicine and other areas of clinical practice (eg, nutrition, nursing). 68 While many schools and preprofessional training programs have student interest groups, there are opportunities to change the curriculum to better incorporate lifestyle medicine principles. 69
With the changing landscape of health care and quality-based care initiatives, learners are eager to learn diverse approaches to treatment, and interdisciplinary care. 69 To date, there have been some excellent examples of lifestyle medicine education, with unique approaches based on level of education and training. 70 In fact, lifestyle medicine experts have argued that introduction to lifestyle principles and practices may be beneficial as early as middle school.70-72 Such education can also be utilized to help students appreciate the role of mental and behavioral health in lifestyle medicine approaches and general health. Appreciating the foundational role of lifestyle medicine as both primary treatment, and adjunct to traditional treatment, particularly in the case of mental health, is incredibly important for future generations of providers. Furthermore, key conceptual mental health frameworks can serve as a foundation to move forward with the integration of mental and behavioral health into lifestyle medicine, the inclusion of expertise from psychiatry and psychology science and practice, and early approaches to medical education.
Conclusions
As the field of lifestyle medicine continues to grow and solidify its reach and influence on medicine, there is a critical need to consider and include mental and behavioral health. Doing so will not only serve to make lifestyle medicine research and practice more robust, but also will offer opportunities for lifestyle medicine approaches to be applied and tailored for individuals with mental health symptoms and disorders who may otherwise be excluded from lifestyle medicine approaches. Given the well-established scientific and clinical fields of psychiatry and psychology, as well as the range of subspecialty expertise within both disciplines, it makes sense to leverage the preexisting bodies of literature to further lifestyle medicine theory and approach.
Furthermore, lifestyle medicine would benefit from the expertise of psychiatrists and psychologists, as well as other types of mental and behavioral health professionals. Similar to the expertise demonstrated by board certification in lifestyle medicine, the professional psychiatry and psychology boards each offer board certification in these areas, as well as subspecialties such as addiction psychiatry and clinical health psychology. Emphasizing the diverse and multidisciplinary nature of lifestyle medicine can empower the field and associated professional organizations to be leaders in crossing the aisle and breaking down the silos that are pervasive in medicine. Given that up to 70 percent of mental health is assessed and treated by primary care physicians, specific attention should be paid to increasing attention to the intersection of lifestyle medicine and mental health. 73 Additionally, such work should begin by engaging students and trainees in lifestyle medicine education as early as possible.
In sum, to well address mental and behavioral health, the field of lifestyle medicine needs to rigorously evaluate the literature and leverage the quality science that already exists. While a strength of lifestyle medicine is approaching health and health care through a unique lens, there are gems within the abundant mental and behavioral health literature that can strengthen attention to mental health from a lifestyle medicine perspective. Leveraging the depth and breadth of knowledge of expert psychiatrists and psychologists can help navigate and support the thoughtful selection of the empirical literature and interventions to support mental and behavioral health with a lifestyle medicine approach, for example to meet the mental health demand within primary care. Employment of critical analysis and reasoning can evaluate the already well-studied mental and behavioral health interventions for inclusion in the armamentarium of lifestyle medicine for mental and behavioral health. Moving forward, lifestyle medicine providers, researchers, and students, as well as the field at large, have an important and unique opportunity to address the mental illness pandemic in a way that could benefit both patients and lifestyle medicine providers, and meet the overarching goals and values of lifestyle medicine.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
