Abstract
Lumbar spinal stenosis (LSS) is an increasingly prevalent condition that has major health and economic implications. While there are many options for the treatment of LSS, exercise is widely considered a first-line intervention as it is associated with reduced complications and cost as compared to more invasive options. Currently, it is not clear if exercise is an effective approach to managing pain and perceived disability in patients with symptomatic LSS. Therefore, the purpose of this systematic review is to evaluate the published literature that has investigated exercise as a primary intervention for LSS. A search was conducted in electronic databases including PubMed, PEDro, SPORTDiscus, CINAHL, and AMED using the key words lumbar spinal stenosis, exercise, physical therapy, rehabilitation, and conservative treatment. Inclusion criteria consisted of published randomized controlled trials written in English that included exercise as the primary treatment in at least one of the groups, and had reported measures of pain and disability clearly stated. The search identified 310 studies of which 5 met all the inclusion parameters. Exercise appears to be an efficacious intervention for pain, disability, analgesic intake, depression, anger, and mood disturbance among patients with LSS. Further research is needed to determine which type of exercise is the most effective in managing symptoms associated with lumbar spinal stenosis.
‘The most common symptoms of LSS are low back pain, neurogenic claudication, and radiculopathy. Causes of LSS can be congenital or acquired, with the latter being more common.’
Lumbar spinal stenosis (LSS) is characterized by narrowing of spaces in the spinal canal or lateral foramina 1 as well as reduced blood flow around the spinal nerve roots. 2 Narrowing of these regions, depending on the degree, may cause pressure on the thecal sac and nerves resulting in pain and an associated decline in function. Due to the sensitivity of the spinal nerves, LSS can lead to neurological deficits and functional disabilities. 3 The most common symptoms of LSS are low back pain, neurogenic claudication, and radiculopathy. Causes of LSS can be congenital or acquired, with the latter being more common. 1
The incidence of LSS increases with age and this condition is becoming more prevalent with the reported increase in life expectancy. 4 Patients with LSS increased (94 000 to 102 000) from 2004 to 2009 according to an analysis of national data in the United States by Bae et al. 5 A study by Kalichman et al 6 found a 3-fold increase in the prevalence of low back pain (LBP) due to LSS. This LBP results in a decrease of the quality of life for those with LSS. 4 Unfortunately, LSS is not only common but very expensive. Overall, costs for low back pain have been estimated between $50 and $100 billion per year. 7 Although the contribution of LSS to this number is not specifically defined, the combined expenses from pharmaceutics, outpatient procedures, and inpatient procedures for the treatment of LSS are likely to be substantial.
There are many medical treatments available for LSS, ranging from conservative to invasive. Surgery is a common treatment and includes decompressive procedures performed with or without spinal fusion. Epidural steroid injections (ESIs) are also a medical intervention that patients with LSS can receive. This type of medical intervention is a less costly option at the early stages of LSS; however, injections are often repeated in order to maintain reduced pain levels over time. 8 With the average time frame of pain relief being only 3 weeks, 9 this can lead to a multitude of injections and many repeated hospital visits. Park et al 10 reported that ESIs were effective for short-term relief only. Another study by Radcliff et al 11 showed an increase in dural tear rates for patients with injections, which would cause potential increased length of stay and cost. The literature reports mixed results on the effectiveness of injections for patients with LSS, which combined with adverse effects such as dural puncture, increased blood glucose, and the need for many to discontinue routine anticoagulant, use make it a less than desirable option.
Many different kinds of pharmacological therapies and alternative substances have been studied to determine their effect on LSS. In a single-blind study performed by Sahin et al, 12 calcitonin in combination with physical therapy treatment (including an exercise program) demonstrated no significant differences when compared to physical therapy treatment and exercise alone. Gabapentin, on the other hand, was found to decrease pain and increase daily functioning in 78 patients described as having intense pain due to LSS. 13 Gabapentin was given orally for 3 months to the experimental group, and when assessed, walking distance increased while pain decreased in these patients. Prostaglandin E1 derivatives, another substance tested for effectiveness in controlling pain associated with LSS, such as limoprost, are seen to increase physical functioning as well as decreasing pain and increase overall satisfaction.2,14 Limoprost, along with other prostaglandin E1 derivatives, increase blood flow to the area of pain, which ultimately leads to temporary pain relief.
While these pharmacological treatments may be effective in managing LSS, other conservative treatments may benefit patients as well. One type of conservative treatment is therapeutic exercise, which includes aerobic activity, flexibility and mobility training, muscle strengthening, and a combination of these 3 categories. Some examples of aerobic exercise are low-intensity cycling 15 and treadmill exercise with body weight support. An exercise program involving a treadmill with body weight support has been shown to decrease pain and increase functioning in patients with LSS. 16 The movement orientation of exercise can also have an effect on LSS treatment. For example, a study by Weiner et al 17 reported that treatment that included flexion biased movements was shown to increase walking time and distance before symptom onset in those with LSS. This apparatus is meant to allow the researcher or therapist to position the patient in the most comfortable position while walking on the treadmill. With flexion and mobility training, a decrease in pressure due to tight muscles and an increase in the strength of these muscles are seen, resulting in a decrease in pain in the area of focus.
Therapeutic exercise may address strength or flexibility deficits targeting the lower extremities, abdominal and back musculature, which can lead to increased mobility and decreased pressure on the structures associated with LSS.15,18 A balance of select strengthening and flexibility may facilitate an optimal approach for rehabilitation. For example, flexibility training of select muscle groups such as the hip flexors and strengthening of the abdominal musculature may lead to better position of the lumbopelvic complex and decreased pressure on the posterior element of the spine. 19
Combinations of interventions are often used simultaneously. For example, exercise treatments are prescribed with a combination of medications, corticosteroid injections, and even electrotherapy. 20 In a randomized control study done by Goren et al, 15 a combination of stretching and strengthening exercises for lumbar, abdominal, and leg muscles showed a decrease in pain and disability as reported using the Oswestry Disability Index (ODI). Also, exercises combined with physical modalities such as ultrasound were considered to be effective in decreasing pain and analgesic use. 15 Another randomized control study by Whitman et al 21 showed the group treated with a combination of physical therapy treatment, flexion exercises, and walking on a treadmill recovered faster than the group that included a flexion exercise, body weight–supported treadmill walking, and ultrasound. Both the body weight–supported treadmill and the basic treadmill were flat. The study included 58 patients over a 6-week period after which the patients were rated on criteria including perceived recovery, pain, and other health care resources. These patients were followed-up after 1 year, and 62% recovered in the physical training, exercise, and walking group compared to only 41% of the flexion exercise, treadmill walking, and ultrasound group. These outcomes were based on questionnaires with an end result of a numerical global rating of change scale. This illustrated that individuals can benefit from physical therapy treatment in reduction of low back pain. Individual, one-on-one therapy that includes a combination of spine mobilization and stabilization exercises is another exercise combination seen to be effective in a study done by Lewis et al. 22
Nonoperative treatment involving exercise is favorable as the patient is not exposed to a hospital, has no recovery time, complications, or blood loss. 23 It is also less costly as surgery expenses have been shown to vary between $23 000 and $27 000 for LSS. 23 The possibility of reoperation may also result in higher costs for patients. Of particular concern is that certain surgical techniques for LSS have been shown to have reoperation rates of up to 23%. 24 Atlas et al 25 found that surgical pain relief decreases over time while nonsurgical treatment improvement stays constant in patients with LSS. While this is an interesting finding, it certainly does not represent the status of those individuals with severe neurological signs.
Currently, it is not clear if exercise can be considered a viable treatment for LSS. In patients with LSS, most cases are long-lasting, not life-threatening, and the majority do not have symptoms that worsen over time due to compensatory postural changes. 18 Because there are few trials that examine the effectiveness of exercise, there is little agreement on the effects of exercise in those with LSS. While surgery does improve LSS symptoms, patients with more mild symptoms may benefit from conservative care. Therefore, a systematic review of the literature is necessary to determine if exercise is indeed efficacious for the treatment of LSS.
Methods
Data Sources and Searches
A computerized database search was performed on PubMed (181 studies), PEDro (18 studies), SPORTDiscus (24 studies), CINAHL (70 studies), and AMED (17 studies) up to March 27, 2014. Key words used in the search included exercise, lumbar spinal stenosis, physical therapy, rehabilitation, and conservative treatment.
Study Selection Criteria
To be included in the analysis, a study must have met the following criteria: a randomized controlled trial, peer reviewed, in the English language, used exercise as the primary treatment in one of the experimental groups, and included outcome measures for pain and disability. The search used electronic databases and resulted in 310 studies for potential inclusion. Of these studies, 15 were considered possible candidates for this review based on superficial information such as the title and abstract. After careful reading of each full-text study, 10 were excluded because treatment was not specifically for improvement of symptoms associated with LSS or exercise was not the experimental variables.
Quality Assessment
The quality of the selected studies was assessed using the PEDro Scale, which is regarded as one of the most widely used assessment tools in physical therapy–related research. In a study done by Maher et al, 26 Kappa (κ) values for individuals using the PEDro scale varied between 0.36 and 0.80 while κ values for a consensus varied between 0.5 and 0.79. Maher et al 26 then concluded that the conclusion of item reliability ratings were “fair” to “substantial” while the total reliability ratings were “substantial” to “good.”
Results
Included Studies
After all studies were vetted and deemed to meet the inclusion criteria, 5 studies were selected for this systematic review (Figure 1).
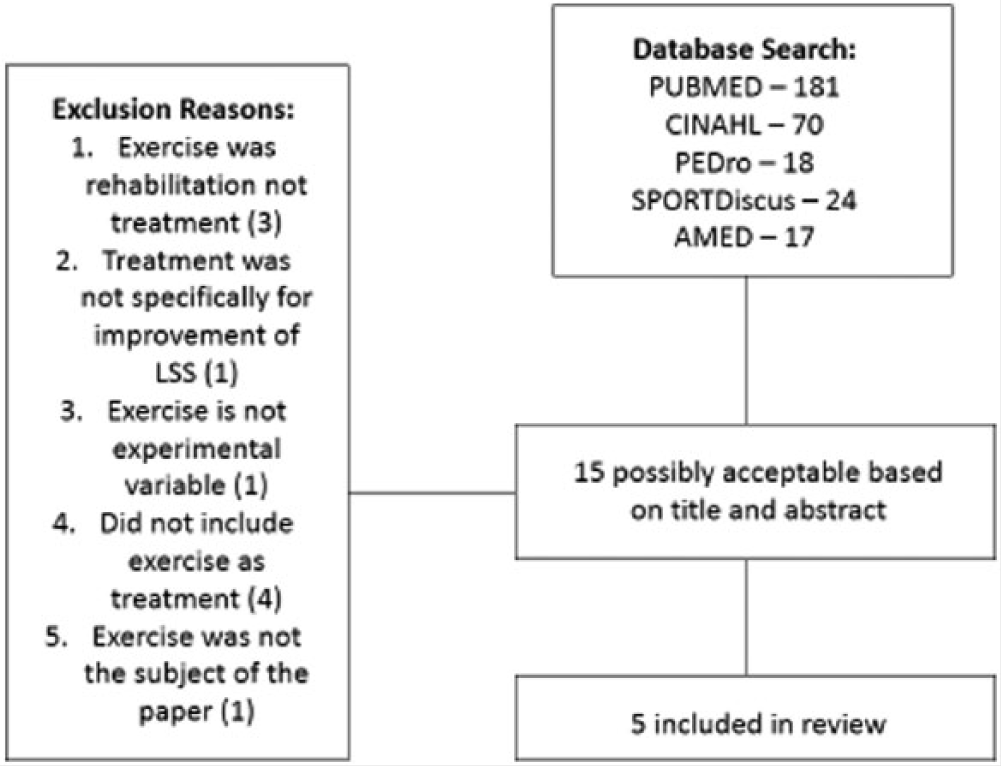
Search Strategy for Selected Studies.
Methodological Quality
The mean PEDro score of the 5 studies selected was 6.2 (out of 10) with a range between 2 and 8 (Table 1). All the studies included blind subjects except the study done by Sculco et al. 27 Also, all studies used random assignment with the study done by Sculco et al 27 using a matched stratified design to accomplish this.
Studies Involving Exercise Treatment for Lumbar Spinal Stenosis.
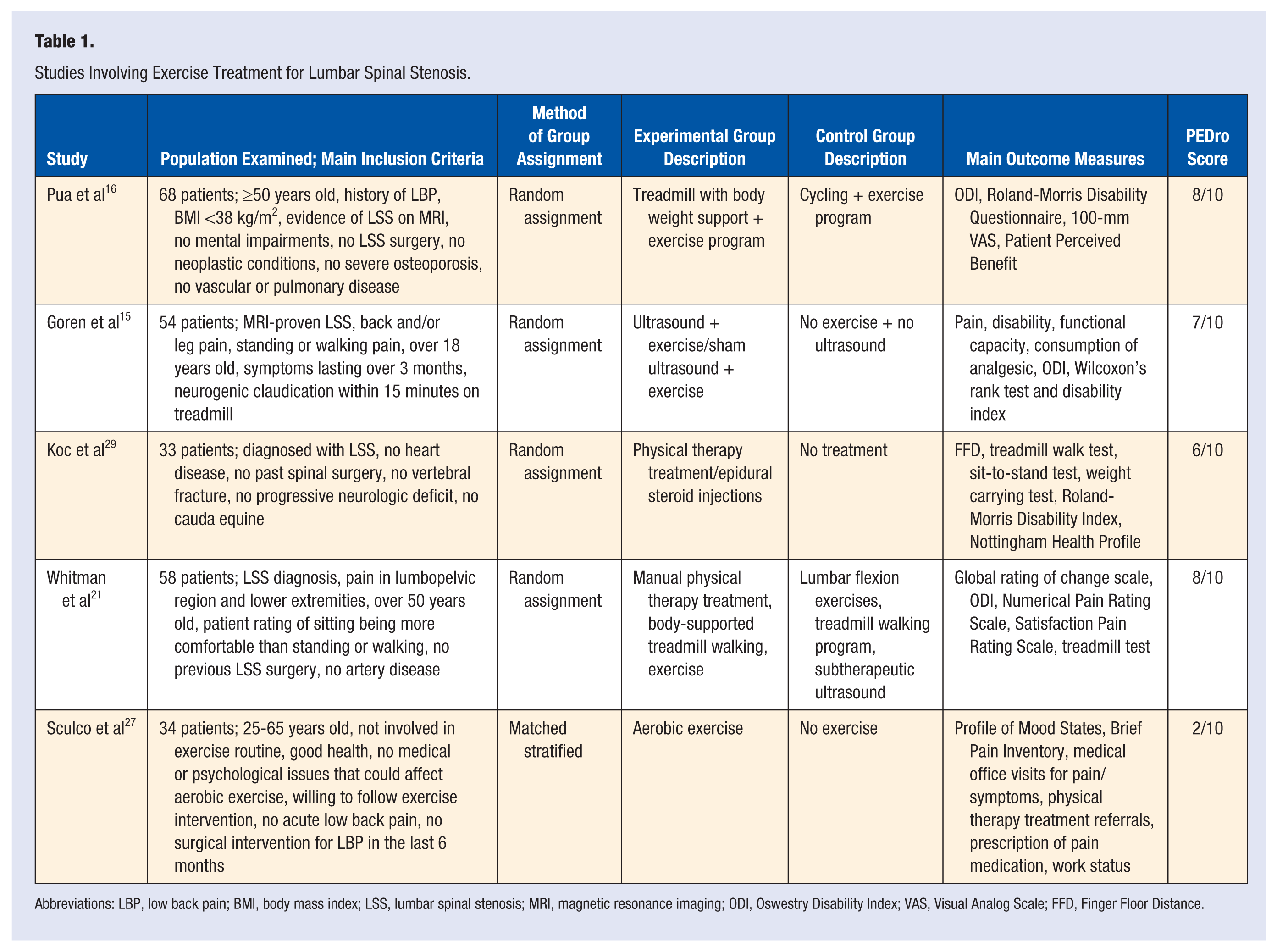
Abbreviations: LBP, low back pain; BMI, body mass index; LSS, lumbar spinal stenosis; MRI, magnetic resonance imaging; ODI, Oswestry Disability Index; VAS, Visual Analog Scale; FFD, Finger Floor Distance.
Study Characteristics
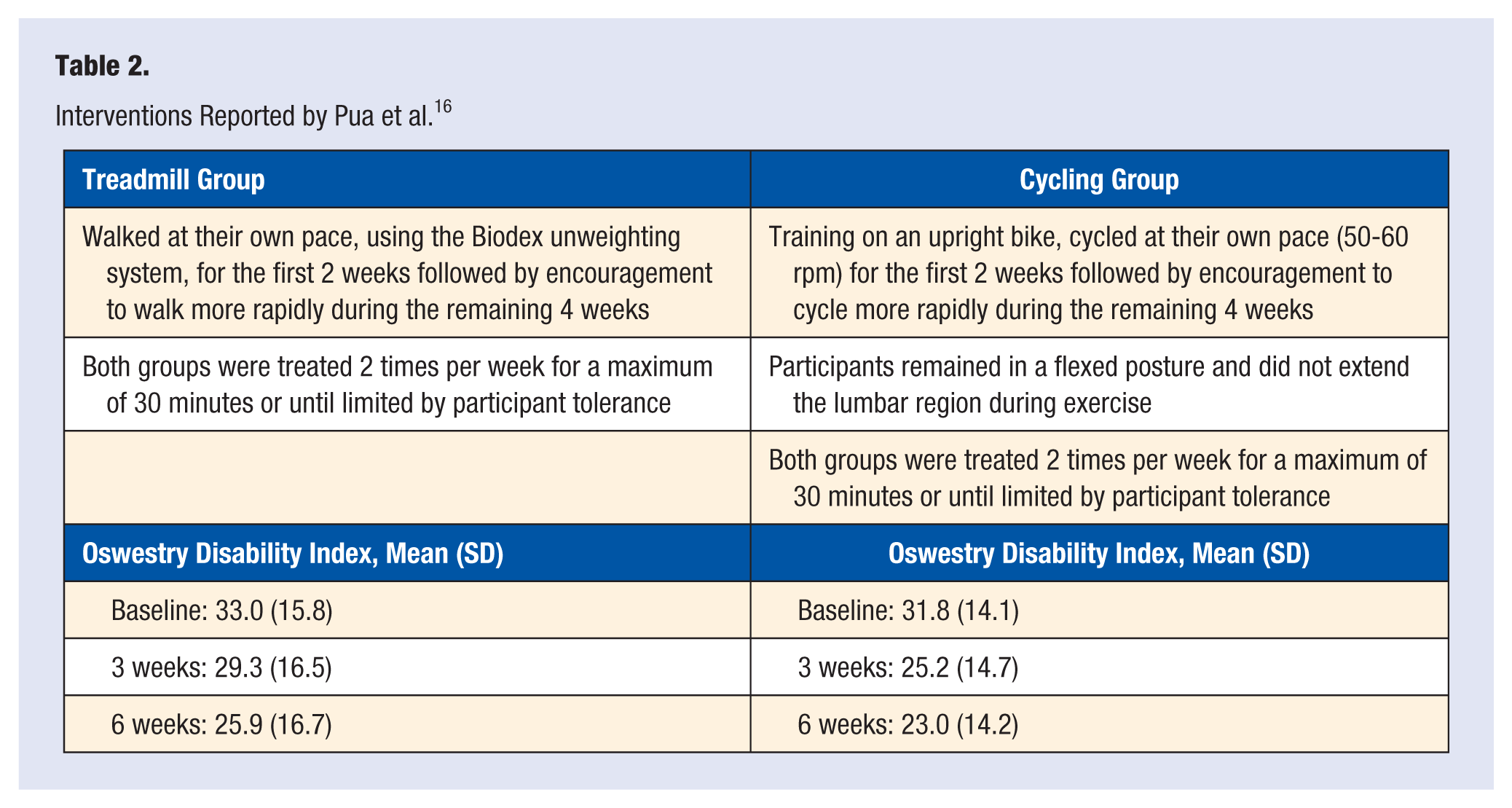
In the study done by Pua et al, 16 68 patients were split between 2 types of exercise groups. The first group jogged on a treadmill using body weight support as a means of decreasing axial load and the second group cycled. Both groups participated in a flexion exercise program that consisted of 3 flexion exercises that aimed to improve circulation in the spinal region and to help with range of motion of the spine. Pain and disability outcomes, based on the ODI and the Roland-Morris Disability Questionnaire, improved in both groups and overall outcomes were similar, suggesting the flexion exercises and any type of non-extension-based aerobic activity is efficacious (see Table 2).
Interventions Reported by Pua et al. 16
In a study by Goren et al, 15 54 patients were randomized into an ultrasound plus exercise group, a sham ultrasound plus exercise group, and a control group that neither received ultrasound nor participated in exercise. The 2 exercise groups participated in the same exercise program, which included flexibility exercises (stretching hamstrings, quadriceps, and lumbar paraspinal muscles), strengthening exercises (abdominals), and concluded with low-intensity cycling. While there was no statistical difference between the 2 exercise groups, there were significant differences between the exercise groups and the control group. According to a study by Kim et al, 28 flexion exercises are shown to increase the central canal space that results in increased spinal mobility and increased abdominal strength. The significant differences were evidenced by lower scores on the ODI and lower reported pain in the leg(s). The result of this study suggest that exercise may be effective in decreasing disability and pain in LSS patients and the effect of therapeutic ultrasound is questionable (see Table 3).
Interventions Reported by Goren et al. 15
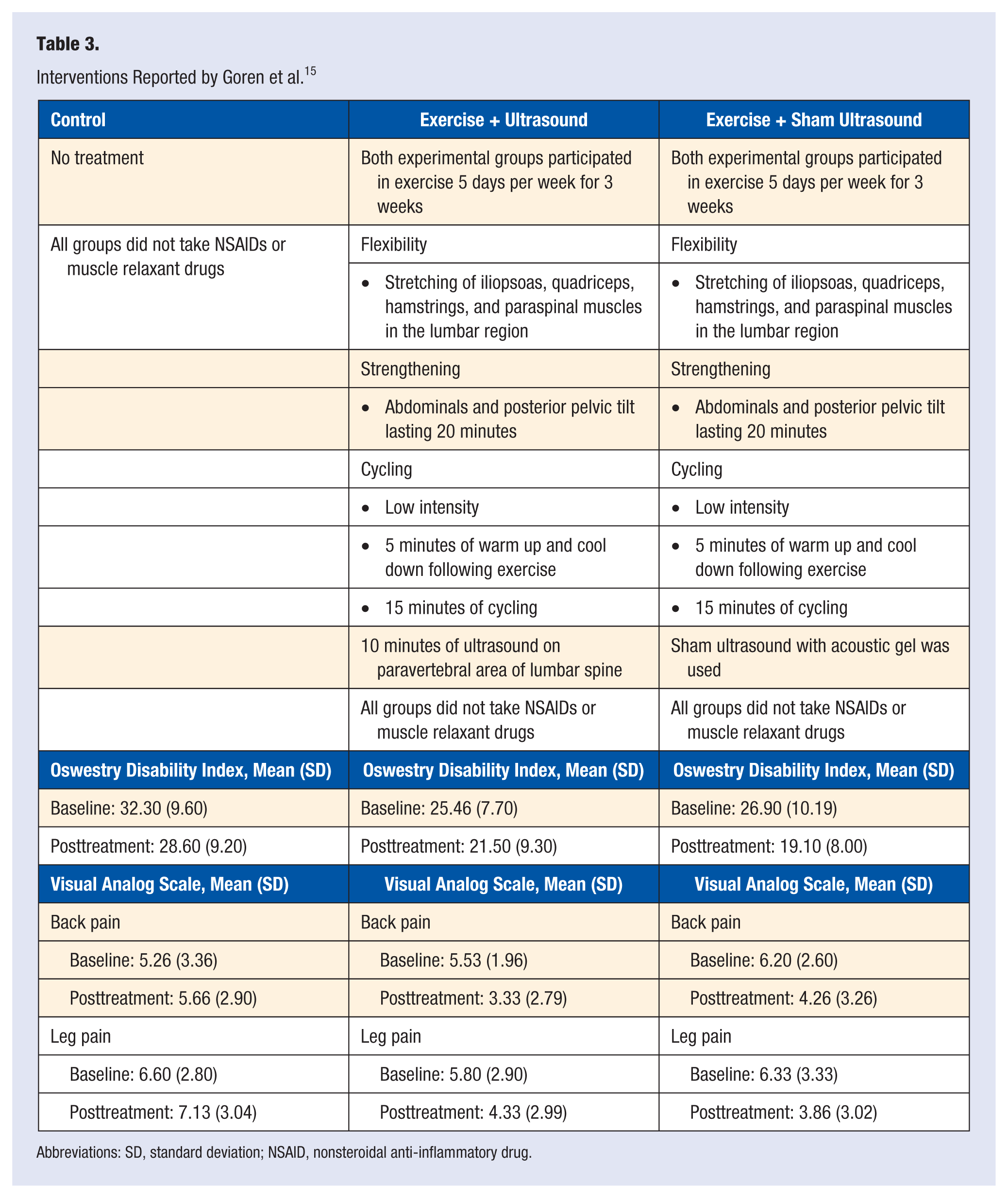
Abbreviations: SD, standard deviation; NSAID, nonsteroidal anti-inflammatory drug.
Koc et al 29 randomly allocated 33 patients into 3 groups (physical therapy treatment only, epidural steroid injection only, and no treatment/control) to investigate the effectiveness of physical therapy treatment and corticosteroid injections on pain and disability in people with LSS. Evaluations were performed after 2 weeks, 1 month, 3 months, and 6 months for multiple parameters including VAS (visual analog scale), FFD (finger floor distance), a treadmill walk test, a sit-to-stand test, and a weight-carrying test. After analyzing the results, no significant difference was found between the physical therapy treatment only group and the ESI only group. As stated by Genevay et al, 30 both the treatment groups had decreased pain and improved function measures; however, the only significant difference found was within the ESI group at the 2-week measurement. In this measurement, there was a significant improvement in the VAS score (pain intensity) of the group receiving corticosteroid injections only compared to the control group (see Table 4).
Interventions Reported by Koc et al. 29
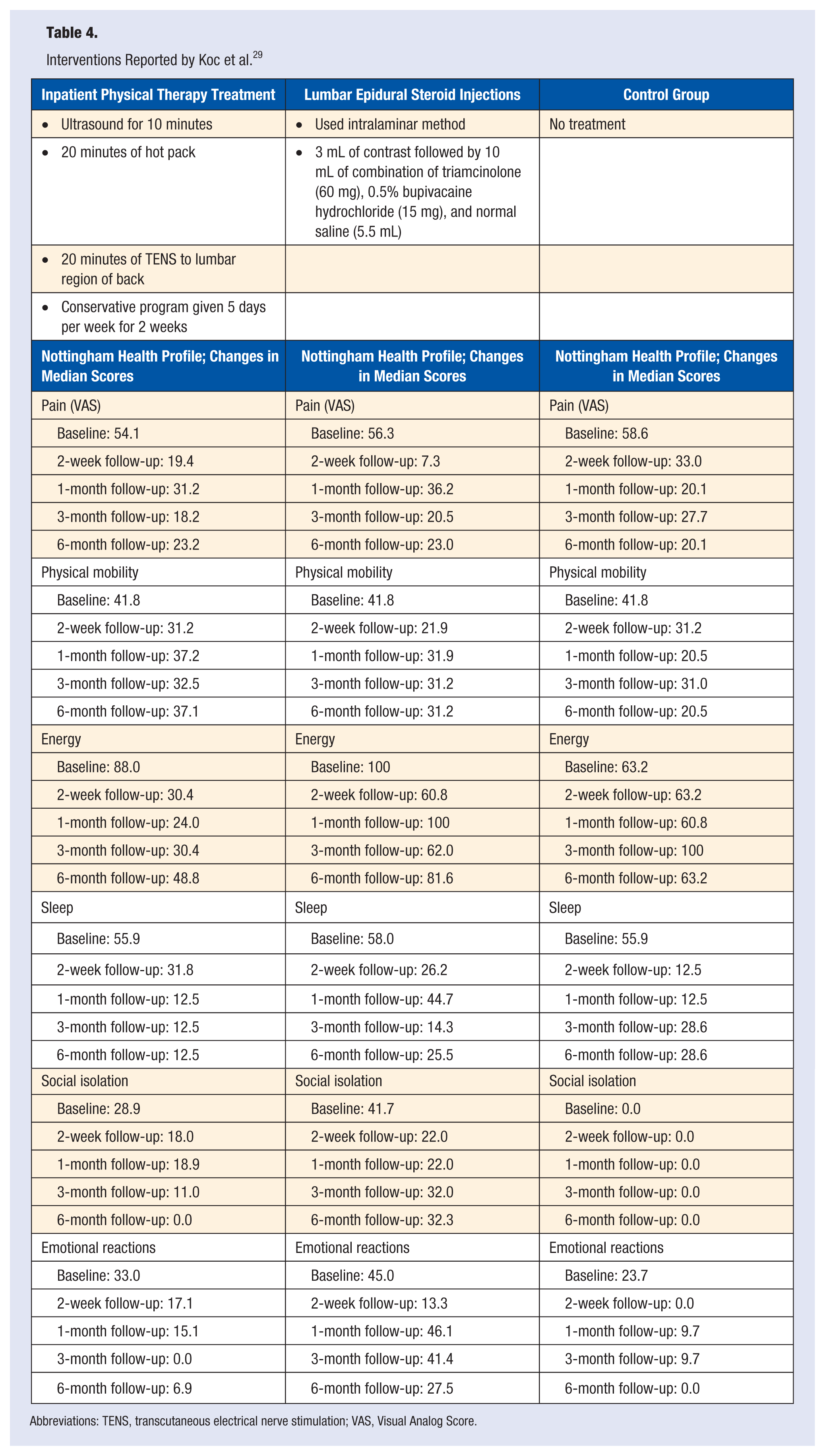
Abbreviations: TENS, transcutaneous electrical nerve stimulation; VAS, Visual Analog Score.
In a 6-week experiment done by Whitman et al, 21 58 patients were randomly assigned to either an exercise and walking combination group or an exercise, walking, and manual physical therapy treatment combination group. Exercises were focused on flexion of the spine. A body weight–supported treadmill was used for the walking program. Body-supported treadmill exercise has been shown by Joffe et al 31 to be more effective than unaided treadmill exercise because the unloading of the spine results in less pain and discomfort. Participants walked for a maximum of 45 minutes depending on their pain tolerance. The manual physical therapy intervention focused on techniques for the lumbar spine, hips, and legs. After 1 year, the exercise, walking, and manual physical therapy treatment combination group improved greater (62% vs 41%) than the exercise and walking combination group based on perceived recovery (see Table 5).
Interventions Reported by Whitman et al. 21
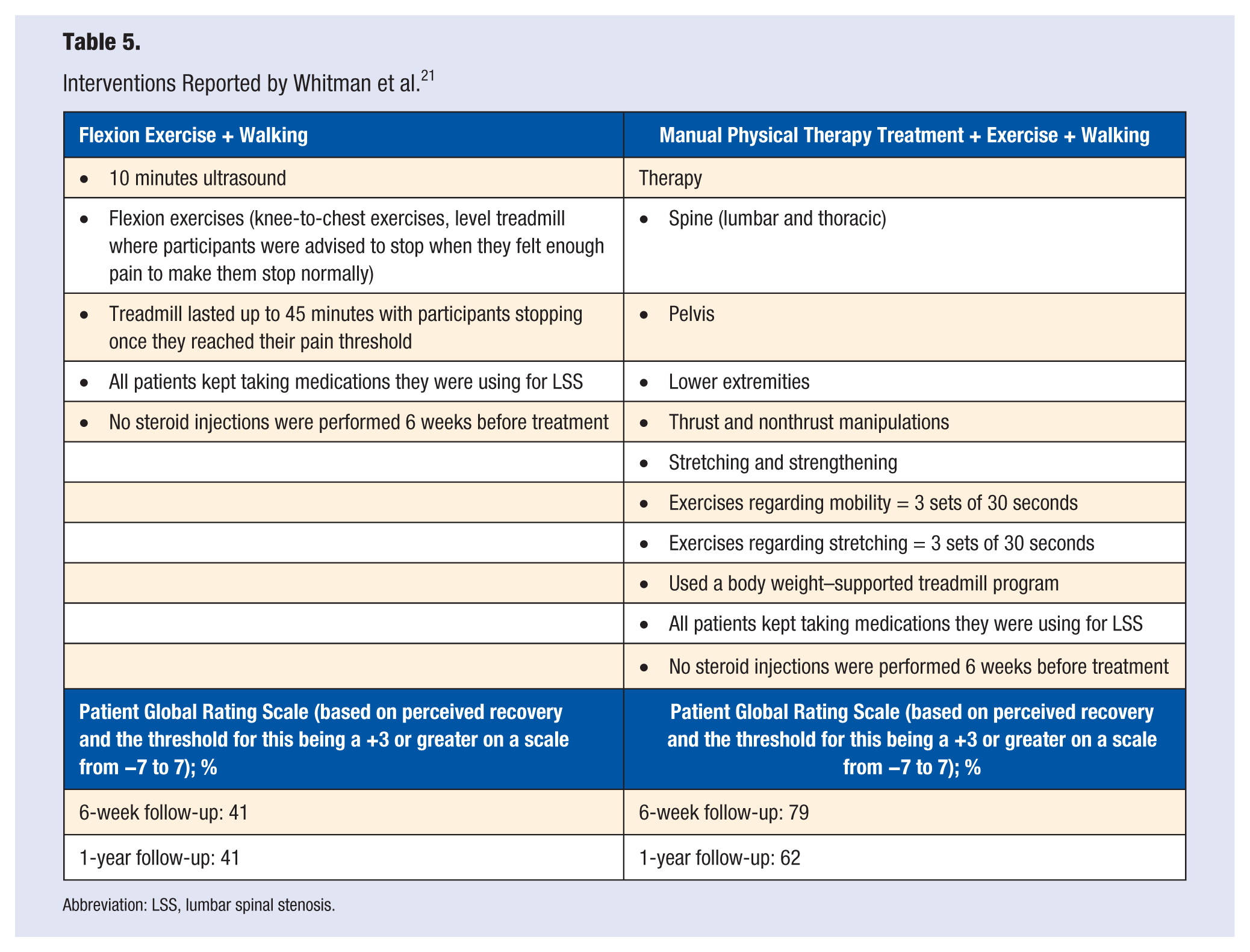
Abbreviation: LSS, lumbar spinal stenosis.
In a study done by Sculco et al, 27 34 patients were randomly assigned to either an aerobic exercise group or a control group that performed no exercise. Participants in the aerobic exercise group were given a 2.5-month home exercise program that consisted of cycling or walking for 4 days per week. After 10 weeks, the aerobic exercise group reported a decrease in depression, anger, and mood disturbance. Bjornsdottir et al 32 demonstrated that mental health issues such as depression increase in patients with chronic pain because of the loss of everyday function and discomfort associated with the condition. Participants completed follow-up measures after 2.5 years, and the aerobic exercise group had fewer analgesic prescriptions, fewer referrals to physical therapy treatment, and an increased work status compared to the no exercise control group (see Table 6).
Interventions Reported by Sculco et al. 27
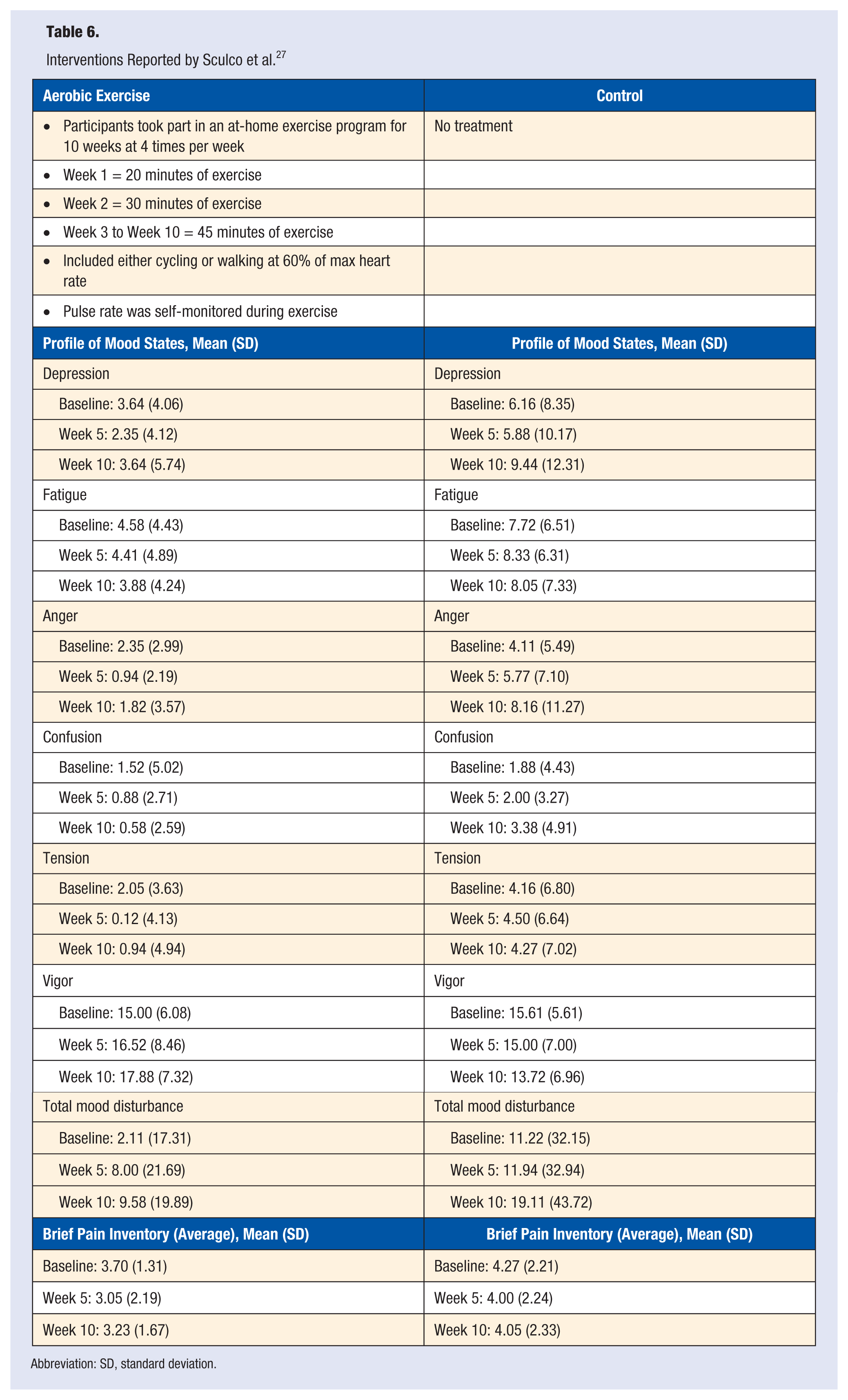
Abbreviation: SD, standard deviation.
Discussion
While these studies showed that exercise is an effective treatment for LSS, study design limitations were noted. First, the participants included in the studies were disproportionately female. The Koc et al 29 and Goren et al 15 studies included 56 females out of a total of 88 (63.6%) participants. This underrepresentation of males could have had an effect on the external validity of the study. According to an article published by the Centers for Disease Control and Prevention, more men than women met the set guidelines for muscle strengthening and aerobic exercise (23.4% vs 17.9%). 33 In a retrospective analysis of 160 LSS patients, Kim et al 34 aimed to analyze the difference in sensitivity to pain between males and females. The patients received a pain sensitivity questionnaire on their first visit to a clinic and were asked to rank their pain based on perception. This study found that, in relation to the severity of the injury, females had a significantly higher pain sensitivity than males and that this resulted in a lower quality of life. 34 This study clearly illustrates that the differences in pain sensitivity found between the genders is an important consideration for studies of exercise efficacy given that gender, pain, and exercise tolerance are associated.
In the previously discussed study by Koc et al, 29 the physical therapy treatment intervention was prescribed as a home program. In comparison, however, a systematic review done by Fokkenrood et al 35 evaluated the effect of supervised physical therapy treatment compared to nonsupervised physical therapy treatment to determine if one was more effective. 35 After reviewing 14 studies regarding supervised and nonsupervised physical therapy treatment, patients receiving supervised physical therapy treatment demonstrated significantly greater walking distance improvements compared to nonsupervised physical therapy treatment patients using a treadmill walking test. 35 While nonsupervised physical therapy treatment was effective, supervision was found to be ideal in regard to a physical therapy treatment regimen with respect to walking distance. Prescribing a home physical therapy treatment program could result in many additional limitations including poor patient compliance and inaccurate documentation of the procedures.
Every study included in this systematic review had a limited sample size.15,16,21,27,29 While small sample sizes are a common and an understandable by-product of clinical patient-based research, the small sample sizes could have had an effect on the outcomes based on an inability to detect small differences. Freiman et al 36 conducted a review of 71 randomized controlled trials and found that 67 could have missed a 25% increase in improvement and 50 could have missed a 50% increase due to therapy. Thus, stating that there was no difference between groups or compared to a control could have been as a result of sample size leading the study to be underpowered. This limitation should be considered in future studies so that the results are able to detect a small effect size due to similarities between interventions.
The duration of the exercises was also noted as a limitation of the studies included in this review.15,29 Koc et al 29 assigned a physical therapy treatment program for 2 weeks while Goren et al 15 assigned a 3-week program. In a study with 116 subjects in a rehabilitation program, Kirk-Sanchez et al 37 demonstrated the effect that duration of exercise has on the level of patient mobility. Those researchers found that the duration of physical therapy treatment was positively correlated with their score on the FIM (Functional Independence Measure), which includes information on mobility throughout the process. 37 Kirk-Sanchez et al 37 concluded that patients who were involved in a physical therapy program longer had improved mobility when compared to those who have been treated with less time based on the FIM. This illustrates the limitation created by the use of short-term exercise programs in the experimental design of studies like this; potential positive outcomes from the exercise/physical therapy treatment group may not be detected.
Studies performed by Whitman et al, 21 Goren et al, 15 and Sculco et al 27 showed a possible response or nonresponse bias because the follow-up questionnaires about symptoms and pain severity were mailed to participants. Response bias could skew the results toward a positive outcome because patients feel pressure to meet the goals of the study. Also, nonresponse bias could affect the results of the study by underrepresenting a certain group of patients. In a study performed by Sheikh and Mattingly, 38 significant differences in rehabilitation outcomes were found between the 84% of participants who responded and the 16% that did not respond to the mailed questionnaire. The researchers concluded that nonresponse rates can create bias that could negatively impact the results of a study.
A high level of participant attrition in some of the studies may have also compromised the study interpretation. It is fairly common to have participants who decide not to complete or participate in every part of the study. An example is seen in the study by Whitman et al, 21 in which a patient chose to not perform the treadmill test due to possible hypertension.15,16,21,27,29 In the same study, 2 patients failed to complete treadmill tests: one because of allergy symptoms and the other because of a grand mal seizure that was unrelated to the study. 21 However, an intention-to-treat principle was used, which may have influenced the outcome. Raboud et al 39 aimed to evaluate the effect of attrition by observing 245 patients in which only 52% completed the study. The attrition contributed to an underestimation of the treatment effect because those who did not finish the study could have showed a significant improvement compared to those who did.
Finally, the ODI differences were often not large enough to be of clinical importance. The ODI has been shown to be an effective outcome measure in the treatment of spinal issues by Fairbank and Pynsent. 40 The difference between posttreatment and pretreatment for Group 1 and 2 and the control group in the study done by Goren et al 15 was −3.94 ± 7.20, −7.80 ± 10.26, and −3.60 ± 11.66, respectively. However, according to a review of data done by Copay et al, 41 the minimum clinically importance difference (MCID) for the ODI is 12.8 among patients receiving surgeries for back pain. According to Goren et al, 15 this lack of an MCID could be due to the low number of physical therapy treatment sessions and short duration of the physical therapy treatment program in the study.
Conclusion
LSS is an increasingly prevalent condition and surgical intervention is costly. Exercise is a low-cost, noninvasive, and convenient treatment option that should be considered before surgery for patients with milder symptoms. Research has shown that exercise is effective to decrease pain level, disability, and pain medication intake as well as increase psychological stability by decreasing anger, depression, and mood disturbance. 15 However, further research is needed to determine which type of exercise is the most efficacious and if exercise is superior to other treatments available for LSS.
