Abstract
Health status during the reproductive years influences fecundity, fertility, and the future health of males and their offspring. There remains a dearth of literature examining men’s preconception health, especially among high-risk populations, such as those with disabilities. The objective of this study was to examine indicators of preconception health, including chronic medical conditions, lifestyle behaviors, and health care utilization, among males of reproductive age with and without disabilities in the United States. Data were from 3,702 males of reproductive age (18–44 years) who participated in the National Health and Nutrition Examination Surveys, 2013–2018. Approximately 14% of males reported having at least one disability related to vision, hearing, cognition, mobility, self-care, or independent living. Among all men, suboptimal preconception health indicators were prevalent including poor or fair self-rated health; low education and household income status; lack of health insurance and no recent utilization of health care and dental care; cigarette smoking; frequent alcohol consumption and binge drinking; marijuana and illegal drug use; obesity; low fruit and vegetable intake and no multi-vitamin use; low physical activity; short sleep durations; depressive symptoms; and hypertension and asthma. Compared to males with no disabilities, males with any disabilities were more likely to have suboptimal preconception health indicators. Strategies to promote and improve sexual health, preconception care, and family planning services among all men are needed. For males with disabilities, specifically, further investigation of their specific health needs related to sex, reproduction, family planning, and fatherhood, as well as interactions with health care providers, is required.
Introduction
There is increasing knowledge that a man’s health during his reproductive years influences fecundity and pregnancy outcomes, his personal long-term health and chronic disease risk, as well as the health and development of his offspring (Frey, 2010; Kotelchuck & Lu, 2017). Efforts to improve men’s preconception health and health care lag substantially in comparison to similar efforts for women. Less than 10% of men report that their primary-care physician discussed preconception health with them (Frey et al., 2012). In 2005, the U.S. Centers for Disease Control (CDC) organized the National Summit on Preconception Care and the Select Panel on Preconception Care with the goal of creating recommendations for both preconception health and care (Johnson et al., 2006). Although men were included in the first recommendation, which addressed individual responsibility across the lifespan and the development of a reproductive life plan, the remainder of these recommendations focused on women’s preconception and prenatal health (Johnson et al., 2006). In 2013, the federal multi-agency conference on Paternal Involvement in Pregnancy Outcomes expanded the conceptualized timeframe of fatherhood to include preconception health, highlighting a research agenda necessary for advancing practice and policy (Kotelchuck & Lu, 2017). There remains a dearth of literature examining men’s preconception health, especially among populations that may be at higher risk for suboptimal health, such as those with disabilities.
In the United States, approximately 15% of men of reproductive age (18–44 years) report at least one disability related to hearing, vision, cognition, mobility, self-care, or independent living (Okoro et al., 2018). Adolescent and adult males with disabilities are sexually active at similar, if not potentially higher, rates as their counterparts without disabilities (Everett Jones & Lollar, 2008; Horner-Johnson, Senders, et al., 2021; Shandra et al., 2016). Adolescents with disabilities may be more likely to engage in risky sexual behaviors, including not using condoms, having multiple partners, and using alcohol or drugs at the time of intercourse (Horner-Johnson, Senders, et al., 2021). In an analysis of data from the U.S. National Survey of Family Growth (2011–2017), fathers with disabilities were nearly twice as likely to report their last birth as unwanted compared to fathers without disabilities (Namkung & Mitra, 2021). There remains little investigation of the preconception health and health-related factors of males of reproductive age, particularly by disability status. The U.S. National Health and Nutrition Examination Survey (NHANES) is a nationally representative program of studies that collects sociodemographic, health, disability, and clinical data from individuals of all ages (National Center for Health Statistics [NCHS], Centers for Disease Control and Prevention, 2021]. In this study, we use these data to examine indicators of preconception health, including chronic medical conditions, lifestyle behaviors, and health care utilization, among males of reproductive age with and without disabilities.
Methods
Data were from individuals aged 18 to 44 years who identified their gender as male and participated in NHANES cycles 2013–2018. NHANES is conducted annually by the NCHS to assess the health and nutrition status of the U.S. population; interview, physical examination, and laboratory data are collected from a nationally representative sample of approximately 5,000 individuals (NCHS, Centers for Disease Control and Prevention, 2021). A disability questionnaire was added to NHANES beginning in 2013. Descriptions of NHANES and all procedures are extensively detailed online (https://www.cdc.gov/nchs/nhanes/index.htm). There were 3,754 participants who met inclusion criteria, 52 were excluded from the analytic sample due to missing disability status (n = 1) or missing covariate data (n = 51). All participants provided informed consent, and approval was obtained from the NCHS Research Ethics Review Board. This study was exempt from human subjects review by the University Institutional Review Board.
Self-Reported Disability Status
The disability questionnaire consisted of six questions regarding whether or not the individual had physical, mental, or emotional conditions that caused serious difficulty with hearing (including deafness); seeing (including blindness); concentrating, remembering, or making decisions; walking or climbing stairs; dressing or bathing; or doing errands alone, such as visiting a doctor’s office or shopping. Disability status was dichotomized as none or any disabilities (an affirmative response to at least one of the six questions).
Preconception Health Indicators
Previously, the 2007 Core State Preconception Health Indicators Working Group’s list of women’s preconception health indicators was adapted based on data available in NHANES (Broussard et al., 2011; Deierlein et al., 2022). For the current analyses, we examined similar preconception health indicators among males (there are no specific indicators developed for males), omitting indicators specific to females (e.g., having a regular period, seeing a physician because they were unable to become pregnant), within the following eight preconception health domains:
General health status—self-rated general health status was categorized as excellent/very good, good, fair, or poor.
Social determinants of health—educational level (less than high school, high school graduate, college graduate or higher) and ratio of family income to poverty guidelines ≤2.00 (yes or no, calculated by dividing the family or individual income by the poverty guidelines specific to the survey year).
Health care utilization—current health insurance type (private, public, none or other); had a health care visit within the previous year (yes or no); and had a dental visit within 1 year, 1–3 years, or >3 years.
Tobacco, alcohol, and substance use—cigarette smoking (current, former, and never); secondhand smoke exposure (current smoker, nonsmoker with exposure, nonsmoker with no exposure); alcohol consumption during the past year (less than once per week, 1–2 times per week, 3 or more times per week); binge drinking during the previous month (defined as the number of days with consumption of five or more alcoholic drinks in one sitting; none or 1 or more days); ever use of marijuana (yes or no); ever use of illegal drugs (i.e., cocaine, heroin, methamphetamines, and injected drugs; yes or no); and ever attend a drug treatment or drug rehabilitation program (yes or no).
Mental health—depressive symptoms during the previous 2 weeks were assessed using the Patient Health Questionnaire-9 (PHQ-9, total points = 27) and categorized as none/minimal symptoms (0–4 points), mild symptoms (5–9 points), and moderate/severe symptoms (≥10 points) (Kroenke et al., 2001). Participants also responded whether they saw a mental health professional within the previous year (yes or no).
Nutrition and physical activity—meeting recommendations of five or more daily servings of fruits and vegetables, excluding white potatoes, (yes or no) were determined from one 24-hour dietary recall administered during the in-person interview. Multivitamin use during the previous month was defined as defined as taking a least one supplement containing two or more vitamins (yes or no). Body mass index (BMI, kg/m2) was calculated using weight and height, which were measured by trained health technicians using standardized procedures during the in-person medical exam; participants wore an examination gown and no shoes (NCHS, Centers for Disease Control and Prevention, 2021). BMI was categorized as underweight (<18.5 kg/m2), healthy (<25 kg/m2), overweight (25–<30 kg/m2), and obese (≥30 kg/m2). Meeting recommended levels of recreational physical activity (yes or no, defined as ≥150 minutes of moderate and/or vigorous recreational physical activities per week) was based on questions regarding the amount of time and frequency spent doing moderate and vigorous recreational activities during the previous week (Broussard et al., 2011). Self-reported number of hours of weeknight sleep was categorized as short, <7 hours; ideal, 7–9 hours; and long, >9 hours (Grandner et al., 2013).
Chronic conditions—self-reported diabetes (yes/borderline or no), hypertension (yes or no), and asthma (yes or no).
Infections—ever tested for human immunodeficiency virus (HIV, yes or no) and ever told by a doctor that they had sexually transmitted infections of chlamydia, gonorrhea, genital warts, or genital herpes (yes or no, only queried in NHANES 2013–2014 and 2015–2016).
Other Sociodemographic Characteristics
Males self-reported their age (years), race and ethnicity (designated in NHANES as non-Hispanic white, non-Hispanic black, Mexican American, Other Hispanic, and Other Race including multi-racial), and marital status (single or married/living with partner).
Statistical Analyses
Analyses were conducted using Stata version 15.1 (College Station, TX, USA) and weighted as required for the complex survey design of NHANES. Unweighted counts, survey-weighted counts, survey-weighted means with standard errors (SE, continuous variables), and survey-weighted proportions (categorical variables) were calculated for the total population and stratified by disability status (no disabilities and any disabilities). Bivariate associations of disability status and preconception health indicators were tested with t-tests for continuous variables and chi-square tests for categorical variables. Poisson regression models estimated associations (prevalence ratios [PRs] and 95% confidence intervals [CI]) of disability status with each preconception health indicator. Multivariable models included age, race and ethnicity, and marital status, as well as education level and health insurance status (when applicable). Approximately 11% (n = 395) of males were missing information on ratio of family income to poverty guidelines. Models were constructed with and without adjustment for this variable and no appreciable differences in the magnitude or precision of effect estimates were observed; therefore, it was not included in final regression models.
Results
There were 3,702 males who met inclusion criteria; 14% (weighted %, n = 514) reported having a disability (hearing or seeing, 3%, n = 112; concentrating, 4%, n = 168; walking, 0.7%, n = 29; dressing/bathing or running errands, 0.6%, n = 17; two or more types of disabilities, 5%, n = 188). On average, males were 30.7 years old (standard error, SE, 0.16). Approximately half of males identified as non-Hispanic White (57%, n = 1,235) and were married or living with a partner (54%, n = 1,892) (Table 1). Suboptimal preconception health indicators were common, with 20% to 95% of males reporting a ratio of family income to poverty ≤2.00; no health insurance; no recent health care or dental visit; weekly alcohol consumption; using marijuana or illegal drugs; consuming <5 daily servings of fruits and vegetables; not taking a multivitamin during the previous month; obesity; not meeting physical activity recommendations; short sleep duration; depressive symptoms; and never having an HIV test (Table 1).
Distributions of Sociodemographic Characteristics and Preconceptional Health Indicators of Men of Reproductive Age (18–44 Years) by Self-Reported Disability Status (Categorized as None and Any Disabilities) National Health and Nutrition Examination Surveys (NHANES) 2013–2018 (Unweighted n = 3,702).

Note. BMI = body mass index; HIV = human immunodeficiency virus; STI = sexually transmitted infection.
All percentages are weighted for NHANES survey design. bp value comparing to men with no self-reported disabilities. cDefined as ≥150 minutes of moderate and/vigorous physical activity per week. dOnly included in NHANES surveys 2013–2016.
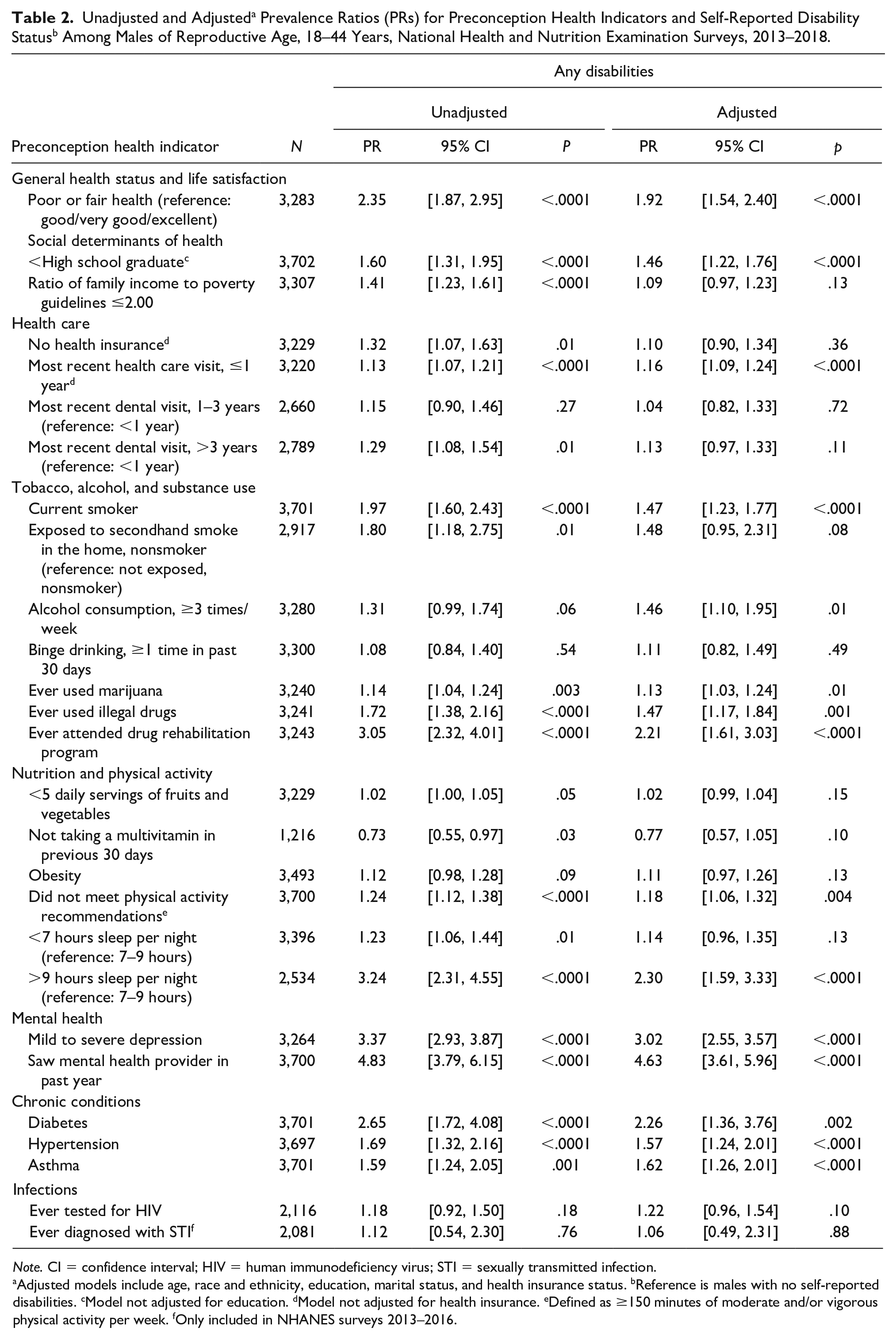
For the majority of preconception health indicators, distributions varied by disability status (Table 1). Greater proportions of males with disabilities reported suboptimal indicators of poor or fair health; low education and household income status; no recent dental visit; current smoking, frequent alcohol consumption, marijuana and drug use; inadequate physical activity; issues with mental health; and chronic health conditions (Table 1). In multivariable Poisson regression models (Table 2), many of the associations observed in bivariate analyses remained. Compared to males without disabilities, those with disabilities were 1.1 to 1.9 times more likely to report poor or fair health, less than a high school education, a recent health care visit, being a current smoker, frequent alcohol consumption, binge drinking, marijuana use, illegal drug use, not meeting physical activity recommendations, hypertension, and asthma. Males with disabilities were approximately two to four times as likely to have ever attended a drug rehabilitation program (aPR, 2.21; 95% CI, 1.61–3.03), long sleep durations (aPR, 2.30; 95% CI, 1.59–3.33), mild to severe depressive symptoms (aPR, 3.02; 95% CI, 2.55–3.57), saw a mental health provider in the past year (aPR, 4.63; 95% CI, 3.61–5.96), or have diabetes (aPR, 2.21; 95% CI, 1.61–3.03) than males without disabilities (Table 2).
Note. CI = confidence interval; HIV = human immunodeficiency virus; STI = sexually transmitted infection.
Adjusted models include age, race and ethnicity, education, marital status, and health insurance status. bReference is males with no self-reported disabilities. cModel not adjusted for education. dModel not adjusted for health insurance. eDefined as ≥150 minutes of moderate and/or vigorous physical activity per week. fOnly included in NHANES surveys 2013–2016.
Discussion
In this analysis of a large, nationally representative sample of U.S. males aged 18 to 44 years, suboptimal preconception health indicators were prevalent. These indicators included poor or fair self-rated health; low education and household income status; lack of health insurance and no recent utilization of health care and dental care; cigarette smoking; frequent alcohol consumption and binge drinking; marijuana and illegal drug use; obesity; low fruit and vegetable intake and no multi-vitamin use; low physical activity; short sleep durations; depressive symptoms; and hypertension and asthma. Approximately 14% of men reported having at least one disability related to vision, hearing, cognition, mobility, self-care, or independent living. Compared to males with no disabilities, males with any disabilities were more likely to report poor or fair health, low education, current smoking, frequent alcohol consumption, drug use and rehabilitation, physical inactivity, long sleep durations, depression, and chronic medical conditions.
Even with an acknowledged need for reproductive health, preconception care, and family planning services for males of reproductive age (Gavin et al., 2014), few previous studies have examined indicators of preconception health in this population. In an analysis of the U.S. National Survey of Family Growth, 2006–2010, 60% of males (aged 15–44 years) were deemed to be in need of preconception or family planning care, especially those who were in the younger age group (15–29 years) (Choiriyyah et al., 2015; Marcell et al., 2016). Need for care was based on various factors including sociodemographic characteristics, birth intentions, fecundity, sexual behaviors, health behaviors (e.g., obesity, alcohol, drug use), and receipt of health services (Choiriyyah et al., 2015; Marcell et al., 2016). Similarly, among males, aged 35 to 39 years, participating in the National Survey of Adolescent Males (2008–2010), 33% were in need of preconception care, 40% were in need of family planning, and 12% were in need of both (Casey et al., 2016). In studies of males who were trying to conceive or had partners with current or recent pregnancies, alcohol consumption, smoking, poor sleep hygiene, use of prescription medication or marijuana, and low levels of screening for sexually transmitted infections were commonly reported despite some positive behavior changes in response to pregnancy, such as improved nutrition or physical activity, elevated BMI (>25 kg/m2) (Bodin et al., 2017; Dennis et al., 2022; Shawe et al., 2019). Collectively, these findings are consistent with those from this study; in addition, we found that significant proportions of males reported drug use, depressive symptoms, and chronic medical conditions. Although lack of health insurance or health care utilization may partially account for these health disparities, more than 70% of males reported having access to these resources. This suggests that despite many males having recent health care visits, they may not be receiving necessary health counseling and services (e.g., screening and testing for sexually transmitted infections) during these visits (Choiriyyah et al., 2015).
Importantly, similar to our previous results among females with disabilities (Deierlein et al., 2022), we found that males with disabilities were more likely to have suboptimal preconception health indicators compared to their counterparts without disabilities. Much of the current, though still limited, literature focuses on the preconception and prenatal health of disabled women, revealing differences in health and lifestyle behaviors, health care services, subfertility, sexually transmitted infections, unintended pregnancies, and sexual violence (Deierlein et al., 2022; Holdsworth et al., 2018; Horner-Johnson et al., 2019, 2020; Horner-Johnson, Akobirshoev, et al., 2021; Mitra et al., 2012). Less information is available for males of reproductive age with disabilities. Greater likelihood of sexual dissatisfaction, sexual anxiety, sexual dysfunction, and sexually transmitted infections have been reported among males with disabilities compared to those without disabilities (Bollier et al., 2019; McCabe & Taleporos, 2003). Among fathers participating in the 2016 Behavioral Risk Factor Surveillance System, those with disabilities were approximately 1.5 to 5.5 times more likely than their nondisabled counterparts to report insufficient sleep, current smoking, poor or fair health, frequent physical distress, or frequent mental distress (Namkung et al., 2019). Fathers with disabilities, particularly those who were married, were also more likely to report unintended births (Namkung & Mitra, 2021). Much more research is necessary to understand issues related to sexual health, intimate relationships, preconception health, family planning, and fatherhood among adolescent and adult males with disabilities.
In an essay by Kotelchuck and Lu, they review the influence of men’s preconception health and health care on pregnancy and offspring outcomes, as well as on men’s overall health throughout the life course (Kotelchuck & Lu, 2017). Cultural views on men’s roles as partners and fathers have evolved over the past several decades, and there is a growing body of literature from public health (e.g., life course epidemiology, maternal and child health, and environmental health) and child development fields supporting paternal contributions to reproductive, women’s, and children’s health (Kotelchuck & Lu, 2017). The “well-man visit” is one strategy to ensure delivery of preconception health and family planning care among males of reproductive age (Frey et al., 2008; Warner & Frey, 2013). A comprehensive framework for health care providers has been developed, which includes content related to family and social history; health behaviors; nutrition; mental health; physical health and laboratory medicine; health promotion; and clinical and psychosocial intervention (Frey et al., 2008; Warner & Frey, 2013). Development of personal reproductive life plans during these visits may also help to increase awareness of reproductive health and pregnancy intentions (Frey, 2010; Warner & Frey, 2013). Both receiving preconception health information from a health care provider and self-seeking health information have been associated with improving knowledge and health and lifestyle behaviors (Barker et al., 2007; Bersamin et al., 2017; Hemsing et al., 2017). Self-care interventions that engage men to participate in activities related to their own health (e.g., use of telemedicine and digital platforms for reproductive health) are also positively associated with men’s health-seeking behaviors, which could improve both immediate and long-term health outcomes (Narasimhan et al., 2021).
In this study, males with disabilities were more likely to report having a health care visit within the previous year compared to those without disabilities. Males with disabilities often interact with multidisciplinary health care teams, including primary-care providers, neurologists, and physical medicine and rehabilitation specialists. These interactions may offer greater opportunities for health care providers to incorporate discussions regarding sexual activity, reproductive health, and family planning while addressing other health concerns with their patients. Sexual and reproductive health needs among persons with disabilities have traditionally been disregarded by society, and the health care field, with assumptions that these individuals are asexual, unable to reproduce, and incapable of romantic relationships and parenthood (Addlakha et al., 2017; Esmail et al., 2010; Neufeld et al., 2002). Medical school curricula often do not include formal training in caring for persons with disabilities (Rotoli et al., 2020; Sapp et al., 2021) or sexual health care (outside of gynecology and urology) (Beebe et al., 2021). Increasing awareness through formal and informal educational experiences may help to greatly reduce barriers to care in this population. Clinical practice guidelines on sexual health, which emphasize integration of sexual health training within health care teams, are available for spinal cord injury and could be adapted for other disabilities (“Sexuality and Reproductive Health in Adults With Spinal Cord Injury: A Clinical Practice Guideline for Health-Care Professionals,” 2010). Training programs within the rehabilitation medicine setting have been successful at improving providers’ knowledge and ability to recognize sexual health issues, as well as their comfort level and conversational skills with discussing patients’ sexual health (Pieters et al., 2018). Further implementation and evaluation of programs are necessary to encourage proactive discussions, information sharing, and provision of screenings/treatments related to sexual and reproductive health between providers and their patients with disabilities.
This study has several strengths. Data were from a nationally representative sample of U.S. males of reproductive age that included the collection of numerous sociodemographic-, health-, and lifestyle-related factors. We examined preconception health indicators for the entire sample, as well as stratified by disability status. The quality of the data was limited, however, by self-report (all indicators except BMI) and the cross-sectional study design. The disability questionnaire only asked participants about having serious difficulty with functional domains (yes or no), which differs from the Washington Group questions that assess level of difficulty: no difficulty, some difficulty, a lot of difficulty, cannot do at all (Madans et al., 2011). Owing to limited sample size, we were unable to examine associations stratified by type of disability (e.g., vision, hearing, and physical) or other sociodemographic factors. Finally, as highlighted by Kotelchuck and Lu, men’s preconception health often encompasses more factors than those related to sperm health, such as their maturity, financial stability, and psychological readiness to enter fatherhood (Kotelchuck & Lu, 2017). Studies are needed to better understand how these factors may differentially affect males with disabilities.
Conclusions
The overall health and well-being of the male partner greatly contributes to pregnancy outcomes, as well as the health and well-being of the female partner and their offspring. Irrespective of family planning intentions, men’s health during the reproductive years is critical for preventing chronic disease development later in life. Our findings highlight the prevalence of suboptimal preconception health indicators among U.S. men ages 18 to 44 years including low education, household income, and health care utilization; cigarette, alcohol, and drug use; inadequate physical activity, sleep, and fruit and vegetable intakes; and chronic medical conditions. When stratified by disability status, males with disabilities were more likely to have suboptimal indicators compared to those without disabilities. Strategies are necessary to promote and improve sexual health, preconception care, and family planning services among all males of reproductive age. For males with disabilities, specifically, further investigation of their specific health needs related to sex, reproduction, family planning, and fatherhood, as well as interactions with health care providers, is required.
Footnotes
Acknowledgements
None.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by a grant from the New York University Research Challenge Fund Program.