Abstract
The aim of the current study was to compare lower urinary tract symptoms (LUTS), erectile dysfunction (ED), and quality of life (QoL) in poststroke and healthy men. Thirty poststroke men with stroke-related LUTS, and as controls, 96 healthy men participated in this controlled, cross-sectional study. Participants filled in the Danish Prostate Symptom Score (DAN-PSS-1) Questionnaire, the International Index of Erectile Function (IIEF-5), the 36-Item Short Form (SF-36), the Nocturia Quality-of-Life (N-QoL) Questionnaire. In the age group ≤55 years, comparing poststroke men with healthy controls both with LUTS, the results indicated DAN-PSS-1, total score median 13 (4-17) versus 3 (2-6), p = .05; IIEF-5 25 (14-25) versus 24 (23-25), p = .06; SF-12, total score 499 (360-679) versus 695 (644-734), p = .02; and N-QoL 98 (70-100) versus 96 (90-100), p = .65. In the age group >55 years, comparing poststroke men with healthy controls both with LUTS, the results indicated DAN-PSS-1, total score 13 (8-24) versus 5 (2-7), p < .01; IIEF-5 13 (5-20) versus 25 (24-25), p < .01; SF-36, total score 585 (456-718) versus 742 (687-772), p < .01; and N-QoL, total score 81 (66-95) versus 98 (80-100), p < .01. The results demonstrated that in age group above, but not below 55 years, poststroke men with LUTS had significantly higher frequency of severe and bothersome LUTS and ED than the healthy controls with LUTS, while QoL and N-QoL were significantly lower in comparison. It is recommended to identify and assess older poststroke men for LUTS, ED, and QoL.
Introduction
Lower urinary tract symptoms (LUTS; Abrams et al., 2002) are highly prevalent in men. The rate increases with age (Andersson, Rashidkhani, Karlberg, Wolk, & Johansson, 2004; Coyne et al., 2009; Irwin, Milsom, Kopp, Abrams, & Cardozo, 2006) and for patients with prostate-related (Smith et al., 2014) and neurological diseases (McLean, 2004; Panicker, Fowler, & Kessler, 2015; Williams, Srikanth, Bird, & Thrift, 2012). In poststroke men, the prevalence of LUTS varies from 15% to 94% depending on the time since the previous stroke (Tibaek et al., 2008; Williams et al., 2012). These poststroke men with LUTS often have to cope with the problem and its significant transient or persistent negative impact on quality of life (QoL).
Erectile dysfunction (ED) is highly prevalent. In the sexually active men, its prevalence increase from 18% in men aged 30 to 39 years to 66% in those aged 70 years or older (Christensen et al., 2011). In poststroke men, the prevalence of ED has been reported to be up to 71% (Bener, Al-Hamaq, Kamran, & Al-Ansari, 2008; Carod, Egido, Gonzalez, & Varela De Seijas, 1999; Monga, Lawson, & Inglis, 1986).
ED is defined as the consistent or recurrent inability of a man to attain and/or maintain a penile erection sufficient for sexual performance (Lue, 2000). ED is complex in poststroke men due to its vascular etiology and the several comorbidities, including diabetes mellitus, coronary heart disease, and hypertension (Calabro, Gervasi, & Bramanti, 2011). For poststroke men, the blood pressure has to be kept low due to the risk for a further stroke. On the other hand, a certain blood pressure is necessary to maintain penile erection (Wespes & Schulman, 1990). For both poststroke and healthy men, penile erection in sexual activity is an integral part of QoL.
The impacts of LUTS and ED on QoL in poststroke men have often been overshadowed by other physical and cognitive poststroke deficits, although data indicated that, particularly, LUTS in stroke patients may impede full participation in rehabilitation (Eldar, Ring, Tshuwa, Dynia, & Ronen, 2001). Frequency of LUTS in men has been reported from large European (Corona et al., 2010) and worldwide population-based epidemiological studies (Coyne et al., 2009; Irwin et al., 2009). Likewise, data on LUTS and ED in men are available from Danish community-based population studies (Christensen et al., 2011; Kay, Stigsby, Brasso, Mortensen, & Munkgaard, 1999). However, in recent years, data are lacking on LUTS, ED, and QoL in poststroke men as well as data on LUTS, ED, and QoL in healthy men. The aim of the current study was to compare data for LUTS, ED, and QoL reported by groups of poststroke and healthy men.
Material and Method
Participants
Between February 1, 2010, and December 31, 2012, 31 poststroke men from the Departments of Neurology at Glostrup and Herlev Hospitals, University of Copenhagen, were included in a randomized, controlled trial where the overall aim was to evaluate the effect of pelvic floor muscle training (Tibaek et al., 2016; Tibaek, Gard, Dehlendorff, Iversen, Biering-Soerensen, et al., 2015; Tibaek, Gard, Dehlendorff, Iversen, Erdal, et al., 2015).
The inclusion criteria were (a) men aged 18 years or older, diagnosed with a stroke clinically defined by the World Health Organization (1989) and confirmed by CT or MRI scan; (b) at least 1 month since their last stroke; (c) normal cognitive function (minimal mental examination score >25); (d) LUTS, according to the International Continence Society definition (Abrams et al., 2002) with start or aggravation closely related to the stroke and measured by the Danish Prostate Symptoms Score (DAN-PSS-1) Questionnaire (Meyhoff et al., 1993); (e) ability to walk independently indoors for at least 100 m with or without walking aids; (f) ability to visit the toilet independently; and (g) outpatient.
Exclusion criteria were (a) prior history of LUTS surgery, pelvic surgery, or trauma; (b) more than two hospital-diagnosed strokes; (c) other severe neurological diseases, including dementia; (d) severe dysphasia; (e) severe psychiatric disease; (f) prostate cancer; and (g) not speaking Danish or English.
Demographic, neurological, urological, and physical baseline characteristics were obtained from the medical records and at the first study consultation. Detailed methodological descriptions have been published previously (Tibaek, Gard, Dehlendorff, Iversen, Biering-Soerensen, et al., 2015; Tibaek, Gard, Dehlendorff, Iversen, Erdal, et al., 2015). The participants received verbal and written information and signed an informed consent before entry into the study.
Healthy Controls
For comparison as controls, a sample of 120 healthy men was recruited by an invitation in the local newspapers of the capital region of Copenhagen and from a Danish Web page for trials (www. forsøgsperson.dk).
Inclusion criteria were the following: (a) men and (b) at least 18 years old. Exclusion criteria were the following: (a) history of LUTS surgery or treatment and (b) known neurological or psychiatric disease.
A cross-sectional study was conducted in which the controls were included. Information letter, anonymized questionnaires, and prepaid reply envelopes were posted to the participants at their address. Participants were asked to fill in four questionnaires and return them to the investigator.
For comparison analysis, the sample of eligible healthy controls was divided into two categories based on their LUTS status: healthy controls with LUTS and healthy controls without LUTS.
The study was approved by the Ethical Committee of the Copenhagen County (H-B-2009-069) and registered in the Danish Register for Data Protection and in the ClinicalTrials.gov Protocol Registration System (Clinical Trials NTC01042249).
Questionnaires
The Danish Prostate Symptom Score (DAN-PSS-1) Questionnaire
The DAN-PSS-1 Questionnaire (Meyhoff et al., 1993) consists of 12 questions related to LUTS in the 2 weeks prior to response. Each question has two parts, A and B.
In Part A, the participants are asked to state the frequency and severity of the symptoms (symptom score) and in Part B, the impact on their daily life of the symptoms if present (bother score). The respondents classify all answers in a four-ranked scale from 0 to 3, 0 being absence of symptoms or bother and 3 the maximum severity. The total DAN-PSS-1 index was calculated as symptom score × bother score.
The DAN-PSS-1 Questionnaire has been reported test–retest reliable and content and face valid in a sample of poststroke men and women (Tibaek & Dehlendorff, 2009; Tibaek, Jensen, Klarskov, Iversen, & Gard, 2006).
The International Index of Erectile Function (IIEF-5) Questionnaire
The IIEF-5 assess the prevalence and severity of ED, according to the classification system developed by Rosen, Cappelleri, Smith, Lipsky, and Pena (1999). It consists of five questions scored from 0 to 5 on each question. Question 1 addresses confidence in the erectile function, Questions 2 to 4, the actual erectile function capacity, and Question 5, intercourse satisfaction.
The IIEF-5 sum score is the sum of the ordinal responses to the five items. The severity levels are classified for the sum score 22 to 25 (inclusive) = no ED, for 17 to 21 = mild ED, for 12 to 16 = mild to moderate ED, for 8 to 11 = moderate ED, and for 1 to 7 = severe ED. The IIEF-5 is a patient-administrated questionnaire. In this study, the participants were asked to fill in the IIEF-5 based on the previous 1 month in contrast to 3 months in the original IIEF-5 version.
The 36-Item Short Form (SF-36) Health Survey Questionnaire
The SF-36 (Ware & Sherbourne, 1992) is a generic QoL Questionnaire which consists of 36 items grouped in eight health-related domains: physical functioning, role limitations due to physical problems, body pain, general health perceptions, vitality, social functioning, role limitation because of emotional problems, and general mental health and well-being. Each scale ranged from 0 (worst case) to 100 (best case).
The reliability and validity of SF-36 have been studied in several populations, including stroke patients (Anderson, Laubscher, & Burns, 1996; Garrat, Ruta, Abdalla, Buckingham, & Russel, 1993).
The Nocturia Quality-of-Life (N-QoL) Questionnaire
The impact of nocturia on QoL was measured by the N-QoL Questionnaire (Abraham et al., 2004). It consists of 13 items grouped in three domains: sleep/energy (the first 6 items), bother/concern (another 6 items), and a global QoL question. Each item was scaled on a Likert-type response scale from 0 (least impact) to 4 (most impact).
For statistical analysis, the scores of the first 12 items were summed and transformed into an N-QoL score from 0 to 100, with 100 indicating the best QoL. In addition, the scores from the sleep/energy and bother/concern domains were separately calculated (0-50 for each domain).
The questionnaire has been validated for men with nocturia (McKown et al., 2010). The original version was developed in English, but has been translated and culturally validated into numerous languages (including Danish) using the accepted Translation Methodology (McKown et al., 2010).
Statistics
Statistical analyses were carried out using IBM SPSS (Statistical Package of Social Science) version 20. and R, version 2.5.0 (R Development Core Team, 2006). Data are presented as numbers (n) and percentage (%) and continuous data as median and interquartile range. The null hypothesis between groups was tested by the Mann–Whitney U-test. Correlations were analyzed using Spearman’s correlation coefficient (ρ).
With 90% power (β = .9) and a significance level at p = .05. The calculation indicated that a total of 120 participants and 120 healthy controls were needed for the study. For all tests, the level for statistic significant was set to <.05. A correlation coefficient ρ > .70 was considered as to indicate a strong correlation.
Results
Participants
In total, 31 poststroke men and 100 healthy controls were included in this study. One poststroke man dropped out (unknown reason) and 4 healthy controls did not complete all questionnaires, leaving 30 (97%) poststroke men and 96 (96%) healthy controls for statistical analysis.
The demographic, neurological, urological, and physical baseline characteristics of the poststroke men indicated median age 68 (60-74) years, Mini-Mental State Examination score 29 (28-30), Barthel Index score 100 (100-100), time since last stroke 59 (50-86) days, sports activity per week 0 (0-2) hours, and Timed Up and Go score 22 (18-26). Further baseline characteristics has been published previously (Tibaek, Gard, Dehlendorff, Iversen, Biering-Soerensen, et al., 2015; Tibaek, Gard, Dehlendorff, Iversen, Erdal, et al., 2015). The median age for the healthy controls was 41 (24-59) years, which was statistically significantly lower compared with poststroke men (p < .01). The median age for the poststroke men >55 years was 76 years (67-79) and for the healthy men >55 years, 63 years (59-66) which was statistically significant different (p < .01). None of the poststroke men or the healthy controls had contacted medical health services for advice, diagnosis or treatment for their LUTS or ED.
LUTS
The median values for LUTS measured on the DAN-PSS-1 Questionnaire (symptoms, bother, and total scores) are presented in Table 1. The results of comparing poststroke men and the healthy controls with LUTS in the age group ≤55 years and the age group >55 years indicated higher frequency and bother of LUTS (p < .01).
Comparison of LUTS Measured on the DAN-PSS-1 Questionnaire and Erectile Dysfunction Measured on the IIEF-5 in Poststroke Men and Healthy Men.
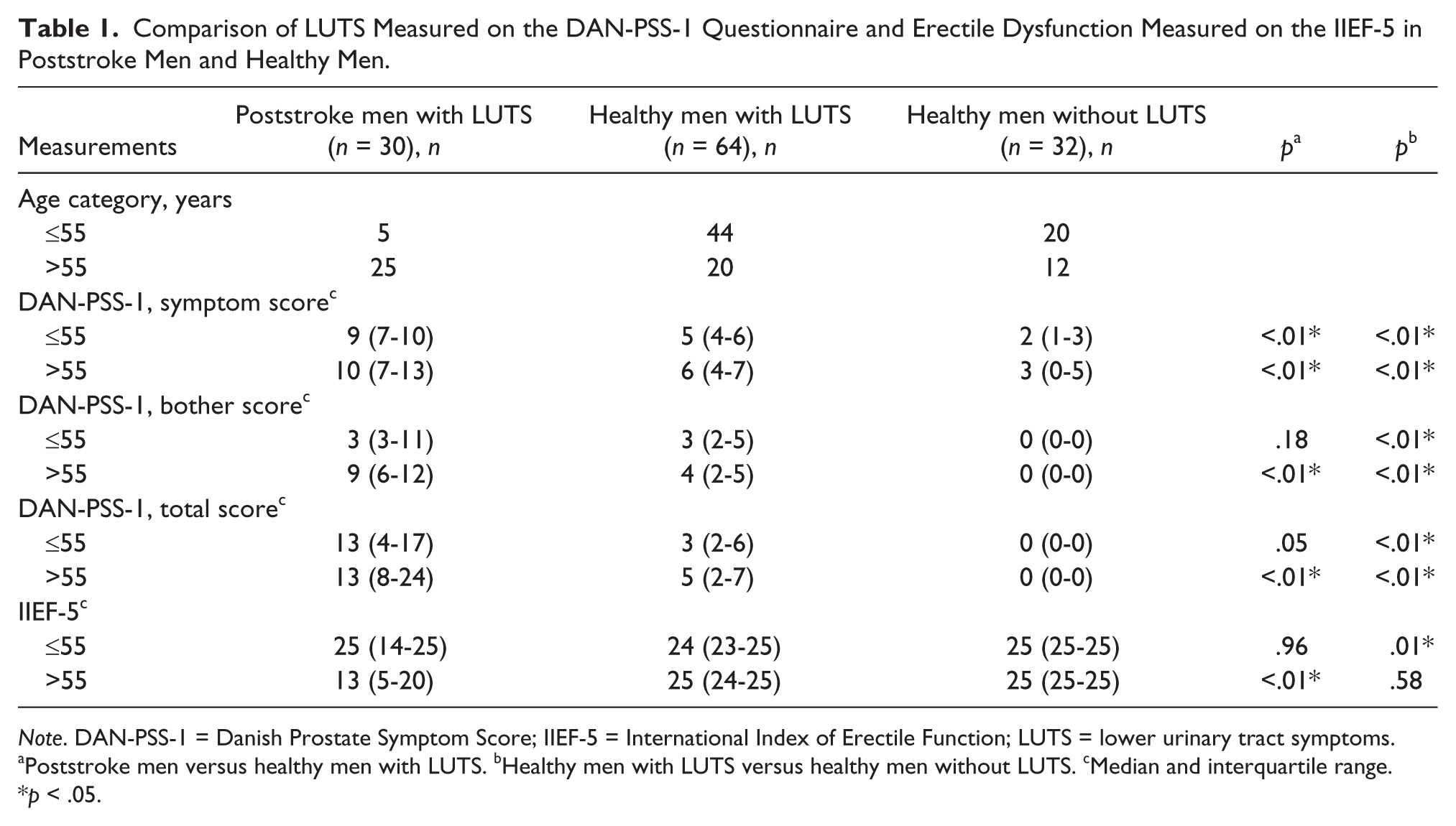
Note. DAN-PSS-1 = Danish Prostate Symptom Score; IIEF-5 = International Index of Erectile Function; LUTS = lower urinary tract symptoms.
Poststroke men versus healthy men with LUTS. bHealthy men with LUTS versus healthy men without LUTS. cMedian and interquartile range.
p < .05.
Comparing symptoms, bother, and total score measured on DAN-PSS-1 Questionnaire between the healthy controls with LUTS and the healthy controls without LUTS, the frequency of LUTS and severity of symptoms were higher (p < .01).
Symptoms
The most frequent symptom in poststroke men was urgency (n = 27, 90%), followed by nocturia (n = 26, 87%), incomplete emptying (n = 25, 84%), and daytime frequency (85%). In the healthy controls with LUTS, the most frequent symptom was urgency (85%), followed by terminal dribbling (75%), incomplete emptying (60%), and nocturia (58%). Data from the 12 symptoms in DAN-PSS-1 Questionnaire are presented in Figure 1.
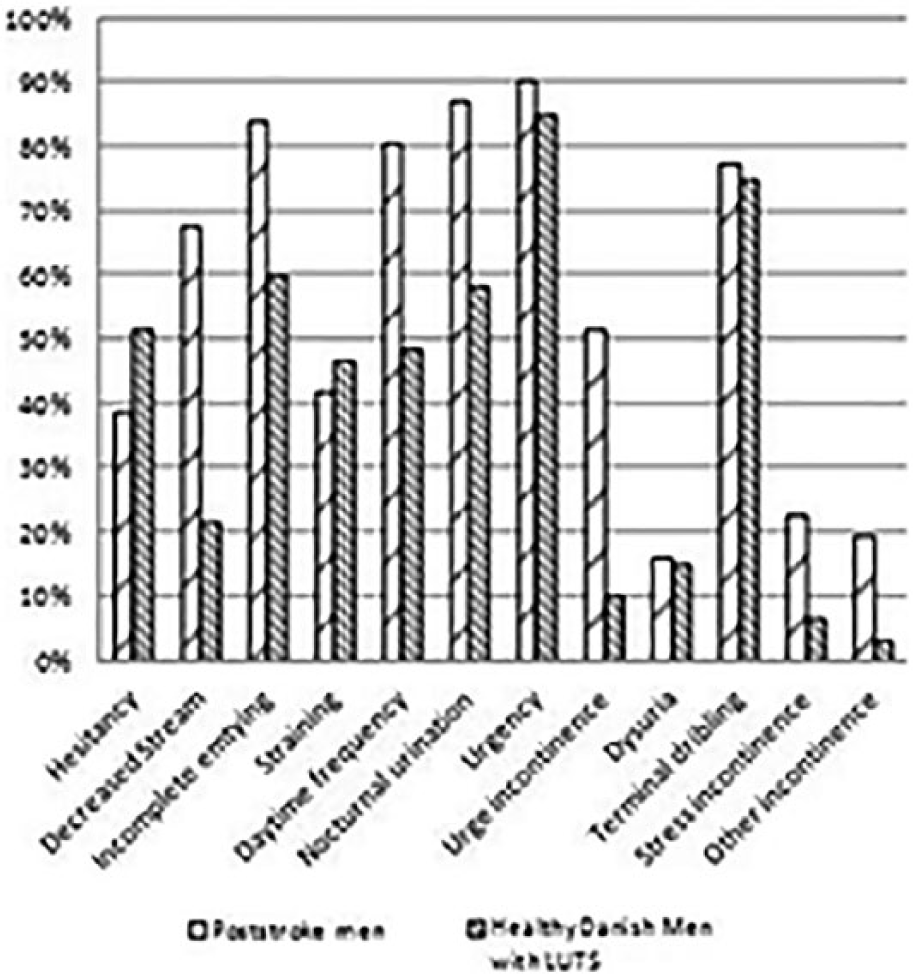
Prevalence of lower urinary tract symptoms (LUTS) in poststroke men compared with healthy men with LUTS.
Bother
The two most frequent symptoms bothering the poststroke men were urge incontinence (100%) and other incontinence (100%), followed by terminal dribbling (96%), urgency (93%), and incomplete emptying (81%). In the healthy controls with LUTS, the two most frequent symptoms which bothered were terminal dribbling (53%) and urgency (47%), followed by nocturia (42%) and incomplete emptying (35%; Figure 2).

Prevalence of bother of lower urinary tract symptoms (LUTS) in poststroke men compared with healthy men with LUTS.
Total Score
The distribution of total score in poststroke men compared with healthy controls with LUTS was as follows, respectively: total score 1 to 8: 37% versus 85%; total score >8: 63% versus 15%, and statistically significant different (p < .01).
ED
The median value for ED measured on IIEF-5 in the poststroke men compared with healthy controls with LUTS in the age group >55 years was higher (p < .01; Table 1). Moreover, the results in the healthy controls with LUTS compared with healthy controls without LUTS in the age group ≤55 years indicated a similar pattern (p < .01: Table 1).
Among the poststroke men, eight (27%) scored 1 to 7 points on IIEF-5, classified as severe ED, compared with one (1%) in the healthy controls with LUTS.
SF-36
The medium values for QoL measured on SF-36 in the poststroke men and the healthy controls are presented in Table 2. In the age group >55 years, there was a statistically significant difference between poststroke men and healthy controls with LUTS (p < .01) in the total score and in the five items, whereas for body pain, general health and mental health, the differences were insignificant (Table 2).
Comparison of Quality of Life Measured on SF-36 and N-QoL in Poststroke Men and Healthy Men.

Note. SF-36 = Short Form Health Survey; N-QoL = Nocturia Quality-of-Life; LUTS = lower urinary tract symptoms.
Poststroke men versus healthy men with LUTS. bHealthy men with LUTS versus healthy men without LUTS. cMedian and interquartile range.
p < .05.
The total score in the age group ≤55 years was also lower in poststroke men compared with the healthy controls with LUTS (p < .01).
To analyze if any correlation between the results of the DAN-PSS-1 and the SF-36 questionnaires, a correlation analysis was made. A Spearman’s correlation analysis between total score on DAN-PSS-1 and total score on SF-36 in poststroke men indicated ρ = .01 and p = .97. Likewise, a Spearman’s correlation analysis between total score on DAN-PSS-1 and total score on SF-36 in healthy controls with LUTS ≤55 years showed ρ = −.02 and p < .90. The analysis between total score on DAN-PSS-1 and total score on SF-36 in healthy controls >55 years showed ρ = −.56 and p = .04.
N-QoL
The median values of impact for nocturia on QoL measured on N-QoL in poststroke men and the healthy controls are presented in Table 2. Comparison between poststroke men and healthy controls with LUTS in the age group >55 years indicated statistically significant differences in items sleep/energy and in total score (p < .01; Table 2).
Comparing health controls with LUTS and health controls without LUTS in age group ≤55 years, the results were lower and statistically significant differences (p < .01) in items bother/concern and total score (Table 2).
A Spearman’s correlation analysis between total score on DAN-PSS-1 and total spore on N-Qol in poststroke men indicated ρ = .45 and p = .01. The Spearman’s correlation analysis between total score on DAN-PSS-1 and total score on N-QoL in healthy controls with LUTS ≤55 years indicated ρ = .12 and p < .49. The analysis between total score on DAN-PSS-1 and total score on N-QoL in healthy controls with LUTS >55 years indicated ρ = .55 and p = .05.
Discussion
The main results of the current study demonstrated that in age group >55 years poststroke men with stroke-related LUTS had significantly higher frequency of severe and bothersome LUTS and ED than the age matched healthy men with LUTS and significantly lower QoL and N-QoL. In the age group ≤55 years, poststroke men with LUTS had a tendency to higher frequency of severe LUTS and ED than the healthy controls with LUTS, and their QoL was significantly lower in comparison.
Previous Studies
As far as the authors are aware, no previous studies have compared LUTS, ED, QoL, and N-QoL in poststroke men with healthy controls.
LUTS
The authors hypothesized a difference in the frequency and bother of LUTS between the two groups, but as most of the strokes were of mild to moderate severity, twofold differences in frequency and bother of LUTS were unexpected.
Consistent with previous results, the current results indicated that the most frequent LUTS in poststroke men were urgency and nocturia (Tibaek et al., 2008). In addition, urge incontinence, the most bothersome symptom in poststroke men, was in line with the current results. Terminal dribbling was the most frequent LUTS, which bothered the healthy controls, which may be explained by substantial etiological differences.
ED
A twofold (median value) higher frequency of ED in poststroke men compared with the healthy Danish men with and without LUTS calls for a systematic screening for ED in practice, otherwise diagnosis and treatment will be overlooked as in this study, where 27% of the poststroke men scored between 1 and 7 on IIEF-5, classified as “severe ED.”
QoL
QoL (median values) in six domains and total score of SF-36 were 2% to 50% lower in poststroke men than in the healthy controls with LUTS and age >55 years. These findings are in line with previous studies in poststroke patients showing that overall QoL decreases after stroke, particularly in vitality, emotions, and mobility (Baumann, Le Bihan, Chau, & Chau, 2014).
Thus, the authors cannot state with certainty that LUTS and ED findings were the cause of lower QoL, rather were they associated with other poststroke deficits.
N-QoL
There was a statistically significant and positive correlation between total score on DAN-PSS-1 and total score on N-QoL in poststroke men. Likewise, a trend of statistically significant and positive correlation between total score on DAN-PSS-1 and total score on N-QoL in healthy controls with LUTS >55 years.
Methodological Considerations
First, the generalizability of these findings is limited because of its relatively small sample size of poststroke men consequent on the multiple inclusion and exclusion criteria (Taylor-Piliae, Boros, & Coull, 2014; Tibaek, Gard, Dehlendorff, Iversen, Biering-Soerensen, et al., 2015; Tibaek, Gard, Dehlendorff, Iversen, Erdal, et al., 2015). Moreover, the group of healthy controls may not be representative of Danish men in general. The response rate in the oldest healthy Danish men was rather low. Older men are usually more willing to participate in surveys, but using advertisements and particularly www.research.dk young people were targeted. The healthy controls were more representative of a group of younger men with better health than older men (>55 years) who are likely to have more frequent LUTS and ED. In this perspective, distributing in the two age groups may be relevant, although still a bias.
Second, the number of baseline characteristics of healthy controls was limited. In the current study, a large number of demographic, urological, and physical baseline characteristics in poststroke men (Tibaek, Gard, Dehlendorff, Iversen, Biering-Soerensen, et al., 2015) but only age in the healthy controls. Information regarding smoking, alcohol consumption, social and civil status, and physical activity, as well as use of medications may also be important.
Perspectives
Based on current findings and a recent study by Hwang et al. (2015) reporting that men with hypertension are more likely to have severe LUTS, a systematic identification and assessment for LUTS, ED, and QoL in poststroke men is recommended. Alternatively, there may be a “hidden” health problem requiring attention.
In cases, where urologists see younger men with a history of sudden LUTS (urgency and nocturia) or severe ED with poor QoL, he might consider potential risk for stroke and advise the patients to seek a cardiovascular evaluation (Miner et al., 2014).
Wehrberger et al. (2011) reported an association between severe LUTS and cardiovascular diseases and stroke, but not as a cause–effect relationship. Bouwman et al. (2015) explained this association by the fact that they share risk factors such as obesity, diabetes, hypertension, smoking, and aging. However, this association may be the subject for another study.
Using available validated and reliable screenings as subjective tools, it is possible to identify and assess these symptoms. In future studies, questions needs to be asked are the following: (a) Why do health care professionals, for example, primary care physicians, not ruinously identify assess or offer evidence-based treatment to poststroke men with LUTS? (Booth, Kumlien, Zang, Gustafsson, & Tolson, 2009; Dumoulin, Korner-Bitensky, & Tannenbaum, 2005) and (b) Why do poststroke men with LUTS and ED not seek help from health care services?
In addition, the use of screening assessment should not replace deeper urological diagnostic and assessments in severe cases.
Furthermore, knowledge of the frequency of LUTS and ED in poststroke men compared with healthy age-matched men may be necessary for establishing what can be considered as “normal” in the general population; this is important in diagnostics and, particularly, also in the context of therapeutic studies.
Reference values for LUTS, ED, and QoL need to be established in comparable up-to-date and age-matched population due to the major demographic changes in population, economics, and lifestyle.
Conclusion
In this group of poststroke men with stroke-related LUTS and >55 years, the frequencies of severe LUTS and ED were higher than for healthy controls with LUTS, while QoL were significantly lower in comparison.
In the age group ≤55 years, poststroke men with stroke-related LUTS had a trend of significantly higher frequency of severe LUTS and ED than the healthy controls with LUTS, while QoL were significantly lower in comparison.
It is recommended to identify and assess older poststroke men for LUTS and ED and to establish up-to-date, age-matched, and reference values of LUTS, ED, and QoL.
Footnotes
Acknowledgements
The authors want to thank all the participants for their contributions, as well as all the staff at the Departments of Neurology, Herlev and Glostrup Hospitals and at the Department of Occupational Therapy and Physiotherapy Therapy, University of Copenhagen, Glostrup, Denmark.
Declaration of Conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by grants from the Association of Danish Physiotherapists’ Research Foundation and Practise Foundation, the Foundation of 17.12.1981, Lykkefeldts Grant, the Foundation of Lundbeck (UCSF) and the Department of Physiotherapy and Occupational Therapy Glostrup Hospital, University of Copenhagen, Glostrup, Denmark.
