Abstract
Background:
Lower urinary tract symptoms are common and can significantly impact quality of life, especially in men with co-morbidities and end-stage renal disease. The presence of lower urinary tract symptoms affect the quality of life of patients on hemodialysis.
Objectives:
The purpose of this study is assessing the presence and severity of lower urinary tract symptoms among male patients on hemodialysis. Factors that may exacerbate lower urinary tract symptoms were assessed and studied. The impact of lower urinary tract symptoms on quality of life was also identified.
Methods:
A prospective, multi-central, and cross-sectional study of male patients on hemodialysis was conducted. Demographics, clinical data, and core lower urinary tract symptoms score questionnaire were all collected. A correlation has been made between all variables.
Results:
One hundred forty-five patients were enrolled. Eighty-seven percent of hemodialysis patients had at least one storage symptom, and 85% had at least one voiding symptom. The prevalence of storage symptoms (frequency, nocturia, urgency, and urgency incontinence) was found to be 3%, 70%, 44%, and 12%, respectively. The voiding symptoms were mainly weak stream, straining, and incomplete emptying, which were found in 60%, 43%, and 36%, respectively. Fifteen percent of the cohort had a negatively significant impact on their quality of life. The absence of voiding symptoms was statistically linked to a better quality of life (
Conclusion:
Storage and voiding lower urinary tract symptoms are common among hemodialysis male patients with a minor impact on their quality of life. Age, smoking, and obesity are major risks of exaggerating such symptoms.
Introduction
Lower urinary tract symptoms (LUTS) are common and hidden morbidity among a different cohort of patients and diseases according to several local and international studies.1–6 LUTS are a broad category of symptoms that may directly affect the quality of life (QoL), especially in men with other co-morbidities.7,8 Recently, subjective and objective evidence has been evolving to show that the lower urinary tract function is affected by the status of end-stage renal diseases.9,10 Therefore, the presence of LUTS don’t not only affect the QoL of patients on hemodialysis (HD) but also may harbor a risk to the proposed renal transplant if not adequately addressed and treated. 11 Several factors play a role in developing LUTS among male patients on HD. For instance, age, duration of dialysis (DoD), and concomitant prostatic enlargement are potential risk factors for developing LUTS.9,12 However, the evidence is still weak regarding the presence and severity of LUTS, risk factors, and the impact on QoL among HD patients.
LUTS, composed of both storage and voiding symptoms, can vary among different patient cohorts.6,13 Storage symptoms such as nocturia, urgency, and urgency incontinence (UUI) can significantly affect the QoL of HD patients especially causing sleep disturbance.14,15 However, given the complex co-morbidities of these patients, such storage symptoms might be overlooked by treating physicians. 16 Furthermore, there is limited data on LUTS in HD patients. Therefore, we believe there’s a knowledge gap regarding LUTS and their impact on QoL in HD patients that this article aims to address. Poor QoL in HD patients may lead to negative impact and increase the morbidity and mortality of such vulnerable group.17,18 Identifying this issue and its impact will guide treating physicians to screen for LUTS in HD patients early on, leading them to the appropriate investigations and treatments, ranging from simple bladder diaries to complex invasive urodynamic testing. 19 Therefore, this study aims to analyze LUTS among HD patients across different institutions. This study enrolls patients on HD as a result of End-stage renal disease (ESRD) to analyze their storage and voiding symptoms and their impact on QoL. Factors such as, obesity, smoking, and diabetes are evidently linked to developing LUTS among different cohorts.20,21 Thus, these variables are also analyzed to assess their impact on developing LUTS.
Methods
Study design and population
This multicentral, cross-sectional study enrolled male patients with HD. This study includes three main dialysis centers in Palestine. The data were prospectively collected and analyzed between October 2021 and January 2022. The study employed a convenient sampling method, inviting all HD patients from three dialysis centers who met the inclusion criteria to voluntarily participate in the study and fill out a questionnaire. Male patients over 18, with a dialysis duration of more than 12 months, were included. Patients with symptomatic urinary tract infection, an underlying functional or anatomical urological problem, or no urine output were excluded.
Data collection
A simple frequency-volume chart was used to assess the urine production among males with HD. Demographics and clinical data were collected. Age, body mass index (BMI), smoking, diabetes mellitus (DM), and dialysis duration in months were considered. The core lower urinary tract symptom score (CLSS) questionnaire was used. 22 The Arabic version of the questionnaire was prepared and evaluated by a group of experts in the fields of urology and biostatisticians, the clarity of the questionnaire was pretested in a pilot study of 15 patients. This questionnaire measures LUTS severity and the impact on QoL. CLSS recognizes storage and voiding symptoms and the value of CLSS is linearly correlated to the severity of symptoms. There is a separate section about the impact of LUTS on QoL, which uses zero as delighted and six as terrible. The questionnaire has a total of 11 questions. The primary outcome was the detailed description of LUTS, which includes storage and voiding symptoms, risk factors for each category, and the impact on QoL.
Statistical analysis
The analysis was carried out using the IBM Statistical Package for Social Sciences (SPSS) program (version 21, developed by IBM Corporation). Descriptive analysis was employed to present participant characteristics, utilizing frequencies and percentages for categorical variables and mean ± standard deviation for continuous variables. Bivariate analysis was conducted using the Pearson chi-squared test to explore potential associations between demographic and clinical variables and storage and voiding symptoms. Additionally, this analysis aimed to uncover the relationship between LUTS and QoL among male HD patients. The significance level was set at
Ethics approval and consent to participate
The study was conducted according to the ethical standards of the Human Experimentation Responsible Committee (institutional and national) and the Helsinki Declaration. Patients were invited to participate voluntarily, with a detailed explanation of the study’s purpose, objectives, and potential risks. To ensure confidentiality, no personal information was collected, and patients were identified by codes instead of names. Access to the collected data was restricted to the research team, exclusively for research purposes. Additionally, all patients provided verbal informed consent before participating in the study. The study protocol, including patient clinical data access and usage as well as conducting patient interviews and obtaining verbal informed consent, received approval from the Institutional Review Boards of An-Najah National University (Reference No: Med, Sep, 2021/8).
Results
Patients’ demographics and clinical data
One hundred forty-five patients were enrolled, with 74 (51%) being under the age of 60 years, 86 (61%) having a BMI of 25 or higher, 58 (41%) being smokers, 84 (58%) being diabetic, and 70 (48%) being on dialysis for more than 24 months. The median amount of urine output/24 h was 120 mL. Table 1 shows the demographics and clinical data.
Demographics and clinical data in male hemodialysis patients (

Storage symptoms
Frequency, urgency, and nocturia are common among the cohort, 5 (3%), 64 (44%), and 101 (70%), respectively. Stress urinary incontinence (SUI) and UUI are less prevalent in comparison to overactive bladder (OAB) symptoms as they appeared in 7 (5%) and 17 (12%), respectively. One hundred twenty-six (87%) had at least one storage symptom. Table 2 shows the frequency of both storage and voiding symptoms among HD patients.
Frequency of LUTS among male hemodialysis patients (

Voiding symptoms
Weak stream, straining, and incomplete emptying were found in 87 (60%), 62 (43%), and 52 (36%), respectively. Eighty-five percent of the participants had at least one voiding symptom. Table 2 shows the frequency of both storage and voiding symptoms among HD patients.
Correlation between demographics and storage symptoms
Frequency significantly correlated to smoking and DoD of fewer than 24 months 9% and 7% (
Correlation between demographics, clinical data, and storage symptoms among male hemodialysis patients (
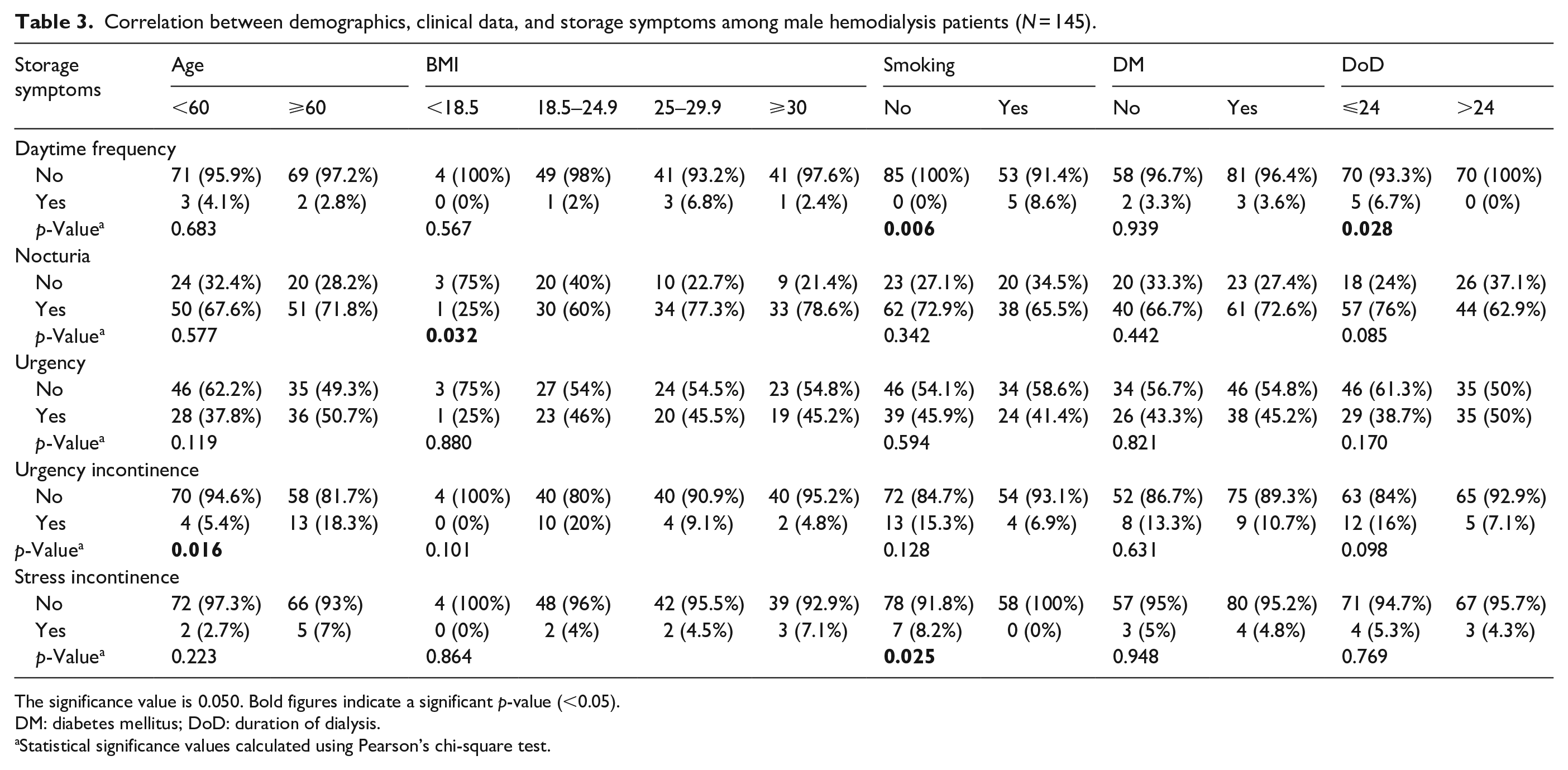
The significance value is 0.050. Bold figures indicate a significant
DM: diabetes mellitus; DoD: duration of dialysis.
Statistical significance values calculated using Pearson’s chi-square test.
Correlation between demographics and voiding symptoms
Bladder pain significantly correlates to the dialysis duration of more than 24 months (
Correlation between demographics, clinical data and voiding symptoms among male hemodialysis patients (

The significance value is 0.050. Bold figures indicate a significant
DM, diabetes mellitus; DoD, duration of dialysis.
Statistical significance values calculated using Pearson’s chi-square test.
Impact of LUTS on QoL
One hundred twenty-four (86%) were satisfied with their storage and voiding symptoms. Twelve (8%), 8 (6%), and 1 (1%) “mostly dissatisfied,” “unhappy,” and Terrible feeling about their symptoms. Table 5 shows the impact of LUTS on QoL.
Impact of LUTS on quality of life among male hemodialysis patients (

Correlation between LUTS and QoL
The absence of voiding symptoms was statistically linked to a better QoL (
Correlation between LUTS and quality of life among male hemodialysis patients (

The significance value is 0.050. Bold figures indicate a significant
Statistical significance values calculated using Pearson’s chi-square test.
Discussion
Our results show that OAB is common among male patients with ESRD and being on regular HD. Underlying structural changes in bladder may be seen in ESRD. 23 Surprisingly, nocturia as a mono symptom was found in 70% of the cohort. The presence of nocturia rather than nocturnal polyurea in such a group of patients raises the question regarding the underlying pathophysiology and treatment.24–26 Moreover, nocturia and sleep deprivation may negatively affect the mental health of such a vulnerable group of patients.27–30 Thus, a bladder diary in HD has to be collected regularly as it is a simple tool that may early raise awareness about a potential lower urinary tract dysfunction (LUTD) and can differentiate between nocturia and nocturnal polyuria. 31
Moreover, BMI is significantly associated with nocturia, according to our results. This is supported by the evidence that higher BMI and waist circumference are significantly associated with LUTS.32,33 Thus, weight reduction strategies and regular exercise should be encouraged in this group of patients to help with LUTS.34,35
UUI and SUI are not that common among male patients on HD. However, 87% of the cohort in our study complained of at least one storage symptom. Thus, a screening questionnaire about the storage LUTS is mandatory, especially since the treatment strategies for OAB are mostly lifestyle modification and medical treatment in the early phase, which are feasible and successful.36–39 Furthermore, age, smoking, and high BMI are significantly related to different variable storage symptoms, according to our results. Thus, strategies such as lifestyle modification, smoking cessation, and regular physical activity may help to improve the overall storage symptoms. 40
Voiding symptoms are also a prominent feature in males on HD, higher than in the population-based study. 41 Eighty-five percent of the cohort had at least one voiding symptom. Poor stream is the most prominent feature among this cohort of patients. It is not apparent whether it is related to the HD, poor urine output per stream, or even underlying bladder outlet obstruction. 12 However, such a problem has to be identified in order to reverse any underlying problem, such as benign prostatic enlargement or urethral stricture. Early identification may also help avoid unnecessary bladder damage secondary to high voiding pressure or consequent poor compliance, which harbor a risk to the potential transplanted kidney in the future.42,43 Moreover, the poor flow may represent an underactive urinary bladder which has to be cleared by an objective test such as cytometry or video urodynamics. 44 Thus, we do believe that if the screening LUTS questionnaire raises the possibility of avoiding problem, a urinary flow test is a reasonable screening test prior to proceeding with further invasive tests. 45
Fifteen percent of the cohort had a negative impact on their QoL secondary to LUTS. Although it is a minority, it is significant as those patients are not willing to pursue with their life in such conditions. Several previous studies among different cohort of patients show a negative impact of LUTS on QoL.2,46 Thus, actions should be taken to improve the HD QoL as it is already threatened by being connected to the dialysis machine most of the time. 47 Moreover, this study shows that the absence of voiding symptoms is positively correlated to a better QoL.
The study establishes that both voiding and storage LUTS are prevalent among HD patients, corroborating existing evidence. 16 The findings reveal that LUTS significantly impair the QoL of these patients. It is well recognized that QoL in HD patients is influenced by various factors, including sleep disturbances, depression, and frailty.48–50 The identification of LUTS as an additional factor exacerbating the difficulties faced by these patients represents a significant insight, highlighting the need for further attention in this area.
Addressing LUTS through various The International Continence Society (ICS) validated questionnaires can aid in their management.19,22,51 Some patients might require more invasive diagnostics such as uroflowmetry and invasive urodynamics to ascertain the underlying issues prior to administering definitive treatments.52,53 Looking ahead, future research could benefit from prospective and invasive studies that might include methodologies such as uroflowmetry or urodynamics. Such studies are poised to enhance our understanding of LUTDs in males undergoing HD, providing a foundation for improved diagnostic and treatment strategies.
Strength and limitation
This is the first study in Palestine to analyze LUTS among males on HD in three different centers in a prospective manner. Nevertheless, some limitations should be acknowledged. The absence of objective assessments such as urinary flow test and invasive urodynamics makes it difficult to draw major recommendations. LUTS is broad category of symptoms that required subjective and objective assessment to understand the pathophysiology and unmask major LUTD. 19 Therefore, the addition of adjunctive tests such as uroflowmetry and invasive urodynamics is required in few occasions to properly evaluate LUTD according to the ICS. 54 Mainly, invasive urodynamics help to differentiate between underactive bladder and bladder outlet obstruction in case of poor flow, especially that the urine volume is decrease in HD.55,56 Therefore, this article serves as an early call to conduct screenings for LUTS in HD patients, provide suitable noninvasive evaluations and treatments, and, in certain instances, recommend more invasive diagnostic procedures such as uroflowmetry and urodynamics. Moreover, future studies should aim to investigate more detailed information on relevant variables such as co-morbidities, medication usage, and socioeconomic status, thus enhancing the comprehensiveness of the research findings. Additionally, the use of a convenient sampling method without a formal sample size calculation is a limitation of this study.
Conclusion
LUTS represents a noticeable morbidity among HD patients that necessitates attention and treatment. Regular screening for LUTS among HD patients is advisable, with subsequent provision of suitable diagnostic measures and management strategies tailored to the severity of LUTS and its effects on QoL.
Supplemental Material
sj-docx-1-smo-10.1177_20503121241263302 – Supplemental material for Lower urinary tract symptoms among male patients on hemodialysis: Prospective and multi-central cross-sectional study
Supplemental material, sj-docx-1-smo-10.1177_20503121241263302 for Lower urinary tract symptoms among male patients on hemodialysis: Prospective and multi-central cross-sectional study by Faris Abushamma, Enas Zidan, Zainab E Douglass, Anas Jaber, Zaher Nazzal, Zakaria I Hamdan, Mahfouz Ktaifan and Hashim Hashim in SAGE Open Medicine
Footnotes
Acknowledgements
The abstract of this article was accepted as an oral presentation at the 20th Urological Association of Asia Congress 2023 which was held in United Arab Emirates from September 28, 2023 to October 1, 2023.
Author contributions
FA and ZN contributed to the conception of the idea, designed the study, and supervised the team in the data collection and analysis process in addition to participation in writing and finalization the article. EZ, ZED, and AJ conducted data collection, literature search, data analysis, and helped in writing the article. ZIH provided critical review and helped in the article final version. MK assisted in data analysis and article writing. HH contributed to the conception of the idea, reviewing and finalizing the article. All authors consented to the submission of the article to the journal after revising and approving the final version.
Availability of data and materials
The data from our surveillance are not available on the public domain due to privacy and ethical restrictions, but anyone interested in using the data for scientific purposes is free to request permission from the corresponding author.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
All aspects of the study protocol, including patient clinical data access and usage as well as conducting patient interviews, received approval from the Institutional Review Boards of An-Najah National University (Reference No. Med, Sep, 2021/8). The study was conducted according to the ethical standards of the Human Experimentation Responsible Committee (institutional and national) and the Helsinki Declaration.
Informed consent
Verbal Informed consent was obtained from all patients after detailed explanation of the study’s purpose and objectives, The IRB of An-Najah National University Approved verbal informed contest.
Trial registration
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
