Abstract
Men, particularly minorities, have higher rates of diabetes as compared with their counterparts. Ongoing diabetes self-management education and support by specialists are essential components to prevent the risk of complications such as kidney disease, cardiovascular diseases, and neurological impairments. Diabetes self-management behaviors, in particular, as diet and physical activity, have been associated with glycemic control in the literature. Recommended medical care for diabetes may differ by race/ethnicity. This study examined data from the National Health and Nutrition Examination Surveys, 2007 to 2010 for men with diabetes (N = 646) from four racial/ethnic groups: Mexican Americans, other Hispanics, non-Hispanic Blacks, and non-Hispanic Whites. Men with adequate dietary fiber intake had higher odds of glycemic control (odds ratio = 4.31, confidence interval [1.82, 10.20]), independent of race/ethnicity. There were racial/ethnic differences in reporting seeing a diabetes specialist. Non-Hispanic Blacks had the highest odds of reporting ever seeing a diabetes specialist (84.9%) followed by White non-Hispanics (74.7%), whereas Hispanics reported the lowest proportions (55.2% Mexican Americans and 62.1% other Hispanics). Men seeing a diabetes specialist had the lowest odds of glycemic control (odds ratio = 0.54, confidence interval [0.30, 0.96]). The results of this study suggest that diabetes education counseling may be selectively given to patients who are not in glycemic control. These findings indicate the need for examining referral systems and quality of diabetes care. Future studies should assess the effectiveness of patient-centered medical care provided by a diabetes specialist with consideration of sociodemographics, in particular, race/ethnicity and gender.
Background
In the United States, 9.3% of the population, 29.1 million people, have diabetes. Diabetes was the seventh leading cause of death in the United States in 2010 and is likely to be underreported as a cause of death (Centers for Disease Control and Prevention [CDC], 2014). A greater percentage of men have diabetes (13.6%) as compared with women (11.2%; CDC, 2014). Moreover, race/ethnicity disparities exist in the age-adjusted percentage of people in the United States, with American Indians/Alaska natives having the highest (15.9%) followed by non-Hispanic Blacks (NHB; 13.2%), Hispanics (12.8%), Asian Americans (9.0%) and non-Hispanic Whites (NHW) having the lowest (7.6%; CDC, 2014).
Critical to diabetes care is receiving national standardized diabetes self-management (DSM) education and support (American Diabetes Association [ADA], 2014). Ongoing DSM education and support are essential components to prevent the risk of complications such as kidney disease, cardiovascular diseases, and neurological impairments (eye and peripheral nervous system damage; ADA, 2014). The effectiveness of DSM education may be a factor of health care utilization. Medical care for individuals with diabetes should include seeing a diabetes specialist (diabetes nurse practitioner, physicians’ assistant, or dietitian certified in diabetes education) qualified to administer DSM education (ADA, 2014).
Diabetes standards of care have shifted focus from self-monitoring blood glucose (SMBG) toward strategies to improve blood glucose and diabetes outcomes. Diet is a major strategy to prevent diabetes-related complications and the American Diabetes Association (ADA) recommends that all individuals with diabetes receive individualized medical nutrition therapy from a registered dietitian (ADA, 2014). There are several dietary patterns that evidence suggests improvements in glycemic and cardiovascular disease risk factors such as the Mediterranean, low-fat, low-carbohydrate, and vegetarian (Wheeler et al., 2012), as well as the Dietary Approach to Stop Hypertension diet (ADA, 2014). The common elements of these diets are sufficient dietary fiber (from whole grains, fruits, and vegetables) and low saturated fat. According to Standards of Medical Care in Diabetes—2014, saturated fat and fiber recommendations for persons with diabetes are the same as those for the general population: 14 g/1,000 kcal of fiber and no more than 10% of daily calories from saturated fat (ADA, 2014).
Other components of DSM are physical activity, eye examinations, and foot care. Regular exercise has been demonstrated to improve glycemic control, reduce cardiovascular risk factors, support weight loss, and improve quality of life and mental outlook (ADA, 2014). The recommendations for adults with diabetes correspond to that of the general population: 150 minutes per week of aerobic activity (50% to 70% of maximum heart rate), spread over at least 3 days per week with no more than 2 consecutive days without exercise (ADA, 2014). Physical resistance training should be performed at least twice per week unless contraindicated (ADA, 2014). Annual examinations for retinopathy and patient education for self-foot care are important components of diabetes care (ADA, 2014). A factor often considered in DSM is SMBG when used a guide to DSM; however, SMBG frequency and timing is largely a factor of patients’ goals (ADA, 2014).
Having diabetes may influence quality of life, which may affect self-assessment of health (Vadstrup, Frølich, Perrild, Borg, & Røder, 2011). Self-rated health (SRH), as an ordinal question asking individuals to rank their health (World Health Organization, 2002), has been established as a marker of morbidity (Sheldon, Kaplan, & Salonen, 1999) and a determinant of the population’s well-being throughout the literature (DeSalvo, Fan, McDonnell, & Fihn, 2005; Idler & Benyamini, 1997; Jylhä, 2009; Tsai, Ford, Li, Zhao, & Balluz, 2010).
Diabetes care depends on continuous support and health care utilization is a necessary component to patient-centered treatment. It has been well-documented that men have lower rates of health care utilization compared with women; however, few studies compared genders for health care utilization for persons with diabetes. Men with diabetes had fewer appointments with primary care physicians and specialist as compared with women with diabetes, despite access to health care in Israeli (Shalev, Chodick, Heymann, & Kokia, 2005) and German cohorts (Krämer et al., 2012).
Purposes and Hypotheses
The purpose of this study was to examine DSM differences between race/ethnicity in men with diabetes and the relationships among glycemic control, type of medical care, and SRH. This article explores racial/ethnic differences in glycemic control for men with diabetes. There are racial/ethnic differences in glycemic control for both males and females, with Mexican Americans (MA) having the lowest percentage of glycemic control (A1C < 7.0): 40.5% followed by NHB: 51.8%, and NHW: 52.2%, for U.S. adults ages ≥40 years (Agency for Healthcare Research and Quality, 2013). Although there were no significant differences in glycemic control between NHB and NHW, based on this report, racial differences have been identified for A1C between NHW (7.4 ± 1.7) and African Americans (8.1 ± 2.5) from an urban setting, even when adjusting for clinical, demographic, and diabetes-related psychosocial factors (Hansmann, Ren, & Sevick, 2010).
Some disparities may be due to unequal treatment across race/ethnicity in health care even when health care status, age, income, and disease state are comparable (Nelson, 2002). For individuals with diabetes, type of medical care may reflect quality: Seeing a diabetes specialist may represent a higher level of care than those persons not referred to a diabetes specialist. According to a patient survey, DSM and nutrition education, interpersonal care, and a skilled health care team are vital elements for diabetes care (Fleming et al., 2001). DSM education and training that includes healthy eating, SMBG is recommended for individuals with diabetes (CDC, 2014). Medical care that helps DSM may improve perceived health.
Method
Source of Data
Data for this study were from appended 2-year cycles of data sets from the National Health and Nutrition Examination Survey (NHANES) 2007 to 2008 and 2009 to 2010 (National Center for Health Statistics, 2015). NHANES is a program of studies designed to assess the health and nutritional status of adults and children in the United States by combining interviews and physical examinations. The sample for the survey is selected to represent the U.S. population of all ages. Persons 60 years and older, African Americans, Asians, and Hispanics are oversampled to produce reliable statistics. NHANES uses a complex, multistage probability sample design to obtain representative samples of the noninstitutionalized, civilian U.S. population.
Description of Sample
This study acquired data for males ≥21 years of age with self-reported diabetes from four out of five racial/ethnic categories: MA, OH, NHB, and NHW. The classification “other races” (Asian and mixed races) was excluded, since numbers in this category were not sufficient for multiple comparisons. The final sample size with complete data for hemoglobin A1c (A1C) and DSM variables was N = 646 (MA = 121, OH = 69, NHB = 159, NHW = 297).
Ethical Considerations
The data used for this study were publically available. Prior to public release, the study protocols (continuation of Protocol No. 2005-06 for both data sets) were approved by the National Center for Health Statistics Research Ethics Review Board (2015). Separate informed consent forms were signed by participants for the interview and health examination, or just the interview. Participants for this study read, understood, and signed informed consent forms for the interview and health examination. Detailed information concerning the data collection procedure for the surveys is found at the website (National Center for Health Statistics, 2015).
Study Design
For this study, a population was categorized as having diabetes based on diagnosed diabetes. Several questions were considered for the construction of the variable “diagnosed diabetes”: (1) “The next questions are about specific medical conditions. Other than during pregnancy, have you ever been told by a doctor or health professional that you had diabetes or sugar diabetes?”; (2) “How old were you when a doctor or other health professional first told you that you had diabetes or sugar diabetes?”; and (3) “When was your diabetes diagnosed?” Each question was by self-report and subject to recall bias. Since there were missing values for Questions 2 and 3, construction of the variable, “diagnosed diabetes,” was based on Question 1. A variable for years with diagnosed diabetes was created by subtracting age at diagnosis from current age.
Diabetes Self-Management Variables
Indicators of a healthy diet recommended saturated fat and dietary fiber were constructed based on the first 24-hour recall. The second dietary recall was not used due to missing values and difference in how the data were collected between the two recalls. The first recall was an in-person interview and the second recall was by telephone. Fiber was constructed as g/1,000 kcal and converted to a binary variable: inadequate/adequate fiber intake. Inadequate fiber intake was considered <14 g/1,000 kcal, based on the dietary guidelines for Americans (Institute of Medicine, 2002-2005). Adequate fiber was formed for ≥14 g/1,000 kcal. Saturated fat was based on percentage of calories using 9 kcal/g.
Hemoglobin A1c (A1C) ≤8.5 was considered having glycemic control; the cutoff value is based on the less-stringent goal of A1C between 7 and 8 (ADA, 2014) and the Department of Veterans Affairs and the Department of Defense (2010) recommendation of <9 for older adults, as well as the estimated marginal means of the study population.
SMBG was formed using variables for frequency and unit. Unit of measure was converted to weeks, then multiplied by frequency. The frequency table was interpreted and collapsed, based on percent responses and clinical significance. The descriptive variable for SMBG consisted of four levels: never, less than once per week, once per week, and more than once per week.
Frequency of checking feet for sores was calculated using two variables: frequency and unit. Unit of measure was converted into weeks and mutliplied by frequency. The descriptive variable for checking feet was collapsed to three levels: never, less than once per week, and more than once per week, based on participant response and clinical significance.
Eye care was based on having or not having retinal damage. Hypothesis test were conducted with binary outcomes for adequate DSM behaviors. SMBG and checking feet were considered adequate at once per week or more versus inadequate behavior at less than once per week or never. Performing physical activity was a positive response to moderate to vigorous recreational activity and/or work-related physical activity.
Major Independent Variables and Covariates
This study compared men from four race/ethnicity categories as the major independent variable for DSM behaviors as dependent variables. Covariates chosen were based on their clinically known confounders of health behavior and their availability in the data set. Age, currently smoking (yes, no), obesity (yes, no), education level, poverty level, marital status, glycemic control, health insurance, and seeing a diabetes specialist were the major adjustment variables. Age was used as a continuous variable in years. Smoke status was generated from two variables about ever smoking 100 cigarettes in a lifetime or not and still smoking. The new variable, currently smoking, was considered as answering “yes” or “no” to currently smoking. Body mass index, calculated as weight in kilograms divided by the square of height in meter, was used to form a binary variable “obesity/no obesity” with body mass index ≥ 30 kg/m2 as the cutoff for obesity. Education level was collapsed into four levels: less than high school, high school, some college, college degree or higher. The poverty level was formed, based on the ratio of family income to poverty, where a score of 1 or lower represented poverty versus >1 as above the poverty level. According to the Office of the Secretary of Planing and Evaluation, poverty levels for 2007 to 2010 were approximately $21,000 to $22,000 per year for a family of four and $24,000 to $26,000 per year for a family of five (U.S. Department of Health & Human Services, 2015). Marital status was converted into a binary variable: considered living with a partner or married versus other. Ever seeing a diabetes educator/specialist (was coded as “yes” and never seeing a diabetes specialist was coded as “no,” based on the last time the participant saw a diabetes nurse educator or dietitian or nutritionist for their diabetes. Two participants reporting “don’t know” were coded as missing. Having health insurance in the past 12 months was considered affirmative with a positive response and a negative responses was considered not having health insurance (there were less than 1% answering “not sure” and they were coded as not having heath insurance in the past 12 months). SRH was reported as one of five responses: excellent, very good, good, fair, or poor. A binary variable was created with good to excellent versus fair or poor.
Data Analysis
All data were analyzed with the Statistical Package for Social Sciences (SPSS, Version 22) with the module for complex design analysis. The sample weights for the first 24-hour dietary recall were computed using the average of the 2-year sample weights for each cycle, as per guidelines set by NHANES. The sample weights used were based on the data file with the smallest sample size (C. L. Johnson et al., 2013). All analysis took into account differential probabilities of selection and the complex sample design, with SPSS, using the Taylor series linearization. A p value of less than .05 (two-sided) was considered statitically significant. Participants’ characteristics were presented as frequency and percentage by race/ethnicity and were performed with cross-tabulations and tested with the chi-square test. Logistic regression models for complex sample analysis, reduced (adjusted for age and race/ethnicity), fully adjusted (age, race/ethnicity, smoking status, obesity, education, poverty, marital status, health insurance, SRH, ever seeing a diabetes specialist/educator), and final models (most clinically important variables retained to achieve significant models) were performed to test the differences across race for DSM behaviors.
Results
The demographics of the study population are presented in Table 1. Hispanics and Blacks were significantly younger than NHW. Mexicans and OH had a higher proportion married or partnered as compared with NHB and NHW. Compared with NHW, MA were the least educated. Minority groups had the lowest percentage covered by health insurance as compared with NHW. NHB had the highest proportion “ever seeing a diabetes specialist/educator” (85%) followed by NHW (75%), whereas Hispanics had a considerably lower proportion of reporting visiting a diabetes specialist (OH, 62% and MA, 55%). There were no significant differences by race/ethnicity for obesity, smoking, and glycemic control.
Characteristics of U.S. Population of Men With Diabetes by Race/Ethnicity.
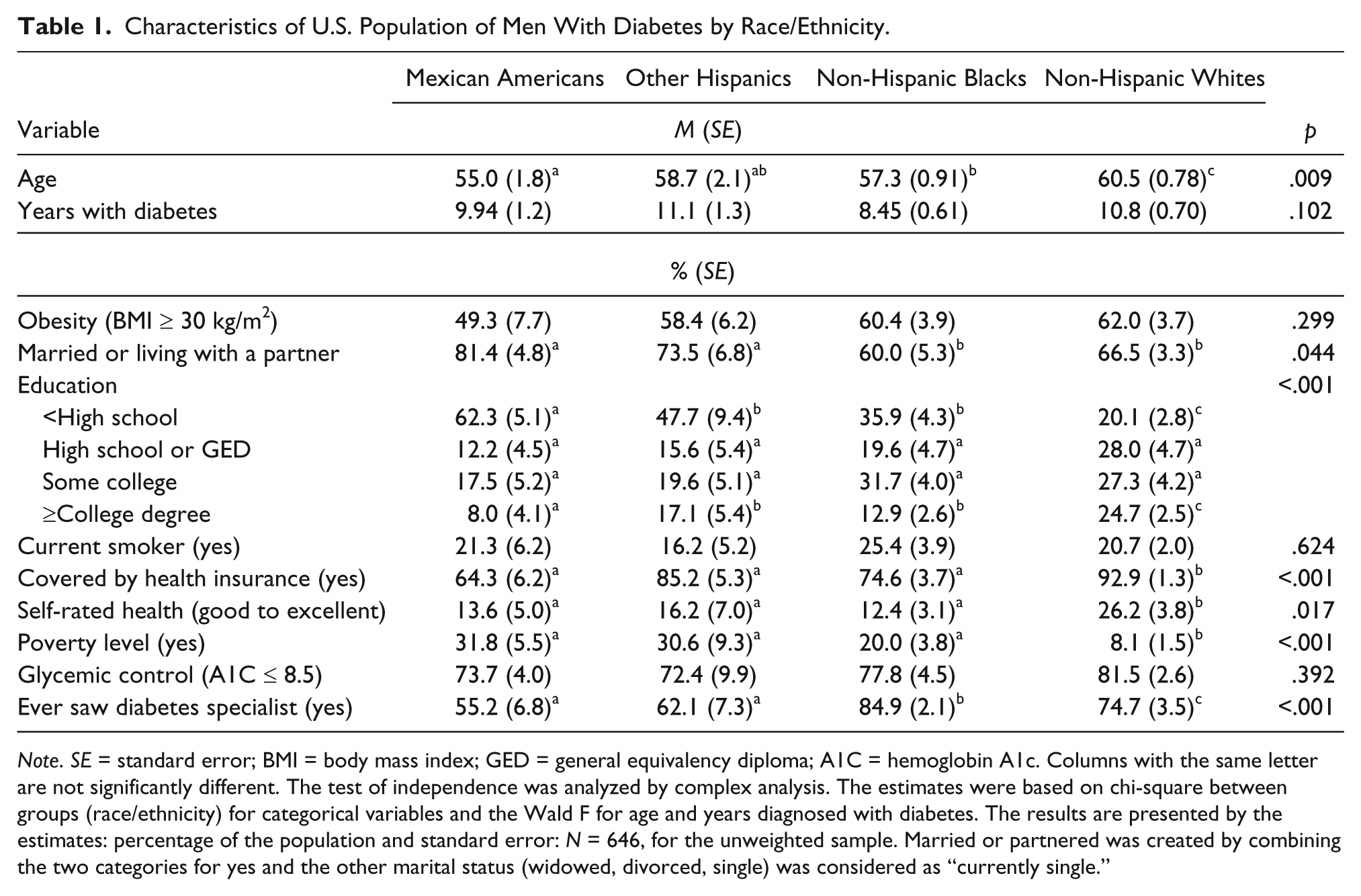
Note. SE = standard error; BMI = body mass index; GED = general equivalency diploma; A1C = hemoglobin A1c. Columns with the same letter are not significantly different. The test of independence was analyzed by complex analysis. The estimates were based on chi-square between groups (race/ethnicity) for categorical variables and the Wald F for age and years diagnosed with diabetes. The results are presented by the estimates: percentage of the population and standard error: N = 646, for the unweighted sample. Married or partnered was created by combining the two categories for yes and the other marital status (widowed, divorced, single) was considered as “currently single.”
Effect of Diet and Physical Activity on Glycemic Control (Hypothesis 1)
The reduced and final adjusted models for the odds of glycemic control with dietary factors and physical activity are presented in Table 2. A model with all the proposed adjustment variables could not be fit. The list of covariates were ordered by clinical importance: age, race/ethnicity, smoking status, obesity, health insurance, education, poverty, marital status, ever seeing a diabetes specialist/educator, and SRH and removed by least importance one at a time until a fit model could be achieved. The final model included the adjustment variable age, race/ethnicity, smoking status, obesity, and health insurance. The consumption of adequate fiber increased the odds of having glycemic control: odds ratio (OR) = 4.22, confidence interval (CI) [1.77, 10.10], reduced model; OR = 4.31, CI [1.82, 10.20], final model. There were no significant differences in glycemic control with following the recommendations for adequate saturated fat (p = .501, reduced model; p = .797, final model) and for performing physical activity at work and/or for recreation (p = .884, reduced model; p = .601, final model).
Logistic Regression Analyses Assessing Dietary Factors and Physical Activity With Glycemic Control (A1C ≤ 8.5).

Note. OR = odds ratio; CI = 95% confidence interval; Dependent variable = glycemic control (hemoglobin A1c ≤ 8.5). The reduced model was adjusted for age (p = .009). The full model was adjusted for age (p = .084), obesity (p = .340), smoking (p = .823), and health insurance (p = .134).
Diabetes Self-Management Skills in Men With Diabetes Across Race/Ethnicity (Hypothesis 2)
There were significant differences by race/ethnicity for consumption of higher than adequate saturated fat (p < .001), checking feet (p = .024), physical activity (p = .002), and SMBG (p = .007). The results indicated that NHW has the lowest percentage of adherence to saturated fat recommendations (<10% of calories from saturated fat). NHB had the lowest adherence to fiber guidelines (7.3%); albeit, the differences were not significant (p = .085). NHW had the highest percentage reporting performing physical activity at work and/or for leisure as compared with other ethnicities. NHB, followed by NHW had the lowest percentage of reporting “never checking feet” (17% and 20%, respectively). NHB had the highest percentage (70%) of adhering to the guidelines (checking feet at least once per week). Table 3 depicts the estimate (percentage) and standard error (percentage) for each skill.
Diabetes Self-Management Skills in Men With Diabetes Across Race/Ethnicity.
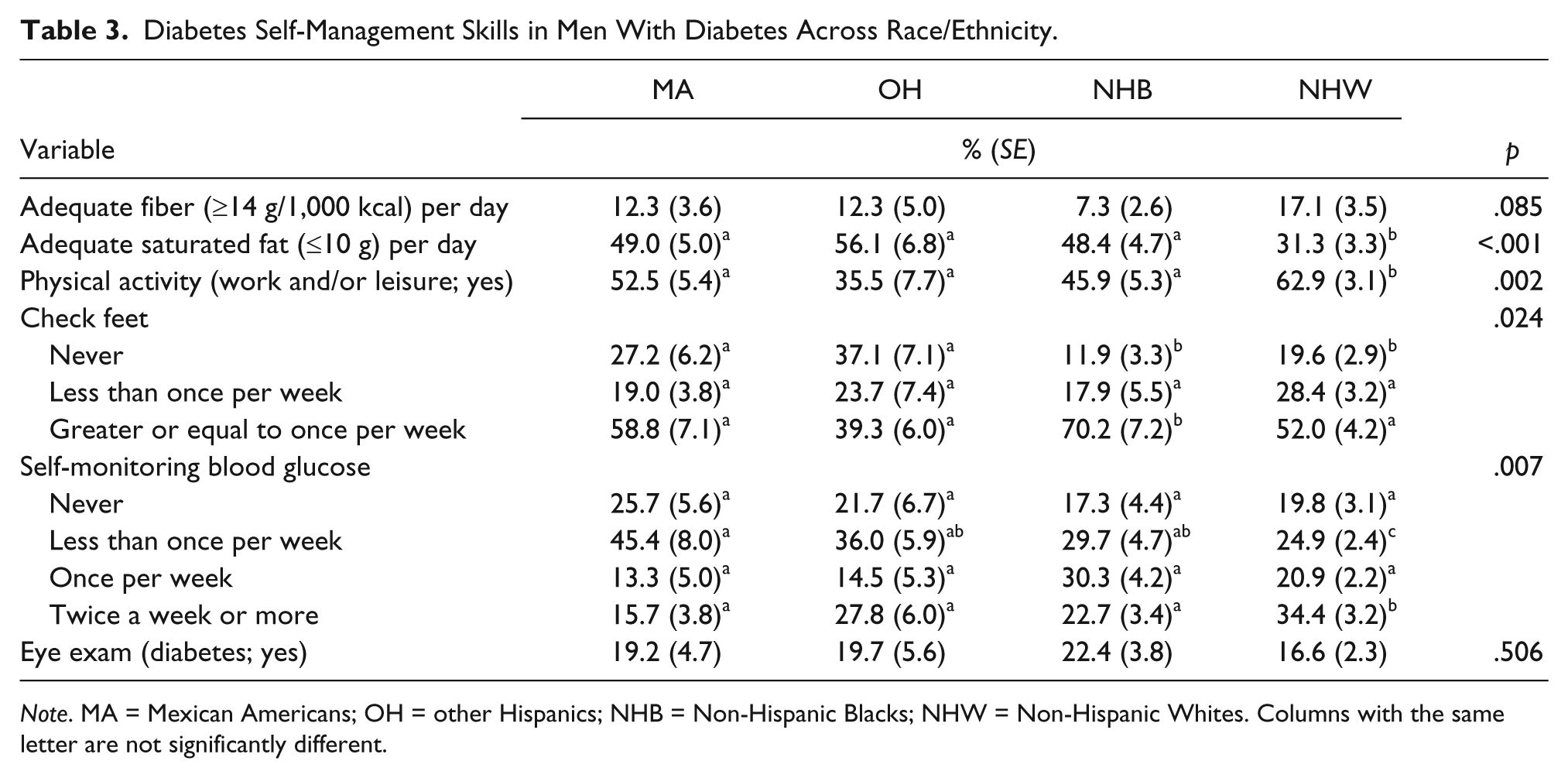
Note. MA = Mexican Americans; OH = other Hispanics; NHB = Non-Hispanic Blacks; NHW = Non-Hispanic Whites. Columns with the same letter are not significantly different.
Self-Rated Health, Seeing a Diabetes Specialist, and Glycemic Control (Hypothesis 3)
A model could not be fit for “ever seeing a diabetes specialist” with the odds of good to excellent SRH (p = .104; Hypothesis 3a). SRH and glycemic control were not significantly associated (p = .297). The logistic regression models for “seeing diabetes specialist” and glycemic control (Hypothesis 3b) are presented in Table 4. Model 1 was adjusted by age (p = .152), health insurance (p = .087), and smoking (p = .583). Model 2 was adjusted by years with diagnosed diabetes (p = .043), health insurance (p = .016), and smoking (p = .311).
Logistic Regression Analysis Assessing Seeing a Diabetes Specialist and Glycemic Control (Hemoglobin A1c ≤ 8.5).

Note. OR = odds ratio; CI = confidence interval. Model 1 adjusted by age (p = .152), health insurance (p = .087), and smoking (p = .583). Model 2 adjusted by years with diagnosed diabetes (p = .043), health insurance (p = .016), and smoking (p = .311).
In contrast to the proposed hypothesis, odds of having glycemic control was less for those who reported “ever seeing a diabetes specialist” (OR = 0.57, CI [0.34, 0.98], Model 1; OR = 0.54, CI [0.30, 0.96], Model 2). There were no significant differences in reporting “ever seeing a diabetes specialist” by race/ethnicity.
Discussion
Health determinants for men with diabetes assessed by race/ethnicity in this study were obesity, marital status, education level, smoking status, health insurance status, SRH, poverty level, glycemic control, ever seeing a diabetes specialist, and DSM behaviors. NHW had higher odds of protective health determinants as compared with Blacks and Hispanics for higher education, above poverty level, having current health insurance, reporting good to excellent SRH and SMBG. Hispanics had higher odds of currently living with a partner or being married but lower odds of reporting ever seeing a diabetes specialist as compared with NHB and NHW. NHB had the highest odds of reporting ever seeing a diabetes specialist. Both NHB and NHW had higher odds of frequently checking feet as compared with Hispanics. Hispanics and Blacks had higher odds of saturated fat intake at or below the recommendation as compared with NHW. There were no significant differences in obesity, physical activity, and fiber intake across race/ethnicity; however, adequate fiber and performing physical activity were associated with glycemic control across race/ethnicity.
DSM behaviors, in particular, as diet and physical activity, have been associated with glycemic control in the literature. For this population, adequate fiber intake was associated with lower A1C; however, regulating saturated fat and performing physical activity were not significantly associated with glycemic control. In contrast, Barnard et al. (2006) reported that individuals randomized to the low-fat vegan group (10% of energy from fat) consumed less saturated fat and had a greater reduction in A1C as compared with those randomized to the group following the omnivorous ADA diet after 22 weeks, while physical activity did not differ between groups. Barnard et al. (2006) adjusted for medication use; however, medication use may be a confounder in saturated fat intake and glycemic control by race/ethnicity in the current study.
SRH was not associated with glycemic control for the current study population. The current results of no significant relationship between A1C and SRH were in agreement with an earlier study of a primarily NHW patients with type 2 diabetes (Blaum, Velez, Hiss, & Halter, 1997) and for a German cohort with type 2 diabetes (Boehme, Geiser, & Renneberg, 2014). Higher A1C was associated with poorer SRH for patients with diabetes from a primary care facility in Denmark (Nielsen, Gannik, Siersma, & Olivarius, 2011). The disagreement in the literature may be due, in part, to the association of poorer health for persons with diabetes. Persons with diabetes were more likely to report fair to poor SRH as compared with persons without diabetes for an African American and Hispanic cohort (Huffman et al., 2013) and a MA sample (Otiniano, Du, Ottenbacher, & Markide, 2003). Persons with diabetes who reported poor SRH consistently over a 4-year interval were more likely to have comorbidities as compared with those whose SRH decreased from good to poor over the same interval (Schmitz et al., 2013). Diabetes complications may be a confounder for SRH and glycemic control (Nielsen et al., 2011). Higher SRH measured by a visual analog scale was associated with lower risk of diabetes complications for a large New Zealand/Australian cohort (Hayes et al., 2008).
Medical care is an important factor in DSM behaviors and outcomes for men with diabetes. In this study, those who reported ever seeing a diabetes specialist/educator had less odds of glycemic control as compared with those reporting never visiting a specialist across racial and ethnic groups. These findings suggest that physicians may selectively recommend diabetes education, based on glycemic control as a basis of the patient’s DSM. In agreement with the Agency for Healthcare Research and Quality (2013), there were no racial/ethnic differences in glycemic control; however, in this study, NHB had the highest odds followed by NHW, and Hispanic had the lowest odds of reporting ever seeing a diabetes specialist. In contrast, the ADA (2014) recommends ongoing diabetes education by specialist for all persons with diabetes, regardless of their A1C levels. Improvements in glycemic control made by patients with a physician–nurse practitioner team as compared with treatment with a physician were lost on termination of the team intervention (Litaker et al., 2003). The relationship between seeing a diabetes specialist/educator and glycemic control could not be established as causal. The literature indicates better glycemic outcomes for patients seen by a diabetes specialist (Healy, Black, Harris, Lorenz, & Dungan, 2013; Rothman et al., 2005; Wexler et al., 2012). Treatment by an intense intervention with clinical pharmacists and a diabetes educator reduced A1C by 1.7% as compared with treatment with a diabetes physician (Rothman et al., 2005). One-time care session from a pharmacist followed by usual care from a primary care provider reduced A1C by 0.8% in a 12-month study of patients with type 2 diabetes and poor glycemic control (A1C > 8.0; Rothman et al., 2005). Glycemic control was improved after 12-month follow-up in a randomized control trial of adults with type 2 diabetes and A1C ≥7.5% for the group receiving diabetes education by specialists (enhanced treatment) as compared with the group receiving usual care (control group; Wexler et al., 2012). For their study, usual care included nonspecialist physicians administering diabetes education and dietitians (not certified in diabetes education) providing nutrition counseling (Wexler et al., 2012). The enhanced treatment group received 60 to 90 minutes of diabetes education provided by a certified diabetes educator (Wexler et al., 2012). Healy et al. (2013) reported that formal diabetes education for patients with poorly controlled diabetes was associated with reduced odds of hospital readmission by 34% for 30 days and 20% for 180 days. These studies indicate improvements in diabetes outcomes and support the need for diabetes education in the management of diabetes.
Limitations
There were several limitations of this study. Cause and effect could not be established by this study since the data were comparing groups from a single time point. There may have been subject bias in some of the variables. Whether or not the treatment received was patient-centered and identified useful by the participants was not available in this secondary analysis. Similarly, the frequency and duration of diabetes education counseling was not indicated. It is not clear whether some men were not referred or that they chose not to comply with the recommendation to see a diabetes specialist. Despite the limitations, a major strength of this study was the use of a national database (NHANES), which has specialized in collecting health data by race/ethnicity.
Implications for Clinical Practice and Future Research
The results of this study suggest that diabetes education counseling may be selectively given to patients with high A1C; albeit, glycemic control can fluctuate between physician’s visits and may not be a definitive marker of DSM. Glucose-lowering drugs may lose their effectiveness for persons not following dietary and physical activity recommendations. Several studies indicated that lower A1C could be achieved by a combination of medication and lifestyle factors that reduced obesity and helped prevent diabetes for those at risk (Knowler et al., 2002; Kosaka, Noda, & Kuzuya, 2005; Ramachandran, Snehalatha, Mary, Mukesh, & Vijay, 2006; Tuomilehto et al., 2001). Continued change of lifestyle factors after follow-up identified prevention or delay in diabetes for a Finnish cohort after 7 years (Lindström et al., 2006) and a Chinese cohort after 20 years (Li et al., 2008).
The complex dynamics of interpersonal relationships makes assessment of “culturally sensitive and collaborative,” patient-centered treatment difficult. Moreover, few studies have investigated whether the message was received in the manner it was intended for men with diabetes and if race/ethnicity affected the communication process. Several studies have indicated health disparities by race/ethnicity have occurred in patient-centered, participatory provider–patient relationships (Cooper-Patrick et al., 1999; DiMatteo, Murray, & Williams, 2009; R. L. Johnson, Roter, Powe, & Copper, 2004). There is some evidence that improvements in diabetes outcomes may not occur for minority patients, even when physicians are made aware of racial disparity in diabetes care and outcomes (Sequist et al., 2010). Patient-centered medical care may improve glycemic control in older adults with diabetes (Heisler, Cole, Weir, Kerr, & Hayward, 2007). Targeting diet and physical activity for those at risk for or with diabetes by diabetes education counselors with a patient-centered approach is supported by the literature. Future studies should assess the effectiveness of patient-centered medical care provided by a diabetes specialist with consideration of sociodemographics, in particular, race/ethnicity and gender.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
