Abstract
Purpose
To review the role of artificial intelligence powered chatbots in diabetes self-management.
Methods
This narrative review examines the role of chatbots in type 2 diabetes self-management. A comprehensive literature search was conducted across PubMed, Science Direct, and Google Scholar (2020–2025), guided by a health informatics specialist. Studies were screened using predefined inclusion and exclusion criteria, with selection visualized through a PRISMA flowchart. Data extraction focused on study characteristics, participant demographics, chatbot interventions, and outcomes related to glycemic control and patient engagement. Lastly, the findings were then organized and interpreted according to the six domains of the Chronic Care Model.
Findings
Twelve studies examined chatbot applications in diabetes self-management, highlighting improvements in patient engagement, adherence, and glycemic control. Several studies reported significant HbA1c reductions and enhanced self-care confidence. Review studies confirmed chatbots’ role in education and chronic disease management, while AI-driven interventions showed potential for optimizing inpatient glucose control. Despite their effectiveness, concerns remain regarding the reliability and accuracy of AI-generated medical information, emphasizing the need for further validation and refinement in clinical practice.
Conclusion
Chatbots improve diabetes self-management, engagement, and glycemic control. Further research is needed to enhance reliability and integrate them into clinical practice.
Introduction
Diabetes is a chronic condition characterized by elevated blood sugar levels, resulting from disruptions in insulin activity and β-cell function. 1 As of 2021, approximately 536.6 million people worldwide were living with diabetes, and it is projected that this number will rise to 783.2 million by 2045. The global prevalence of diabetes among adults aged 20 to 79 was estimated at 10.5%, with comparable rates between men and women, and the highest prevalence observed in those aged 75–79. 2
Effective diabetes management is essential for maintaining optimal health outcomes and preventing the onset of complications associated with the disease. 3 Individuals with type 2 diabetes (T2D) can potentially prevent or delay the onset and progression of diabetes-related complications. They can achieve this by managing their blood glucose levels stringently, which helps prevent complication such as cardiovascular event, cerebrovascular accidents, renal failure, visual impairment, and neuropathy. 4 Traditional diabetes self-management education has been delivered in person, but it faces challenges such as high costs and limited scalability. 5
Clinical guidelines recommend regular self-monitoring of blood glucose (SMBG) for individuals with type 1 diabetes and those with type 2 diabetes using insulin, typically testing at least four times daily. 6 However, Despite its importance, many people do not adhere to recommended testing frequencies, and some do not test at all. 7 In this context, Digital therapeutics, including AI-powered chatbots, offer an innovative solution by providing personalized and accessible interventions. 8
A chatbot function as a virtual robot that engages in conversations, providing users with answers to their queries. By simply sending messages to chatbot services, users can easily access the information they need without the hassle of launching apps or visiting websites. 9 Consequently, Chatbots have great potential for patient education and self-care management. 10 In comparison to static character images or text-only displays, the interactive and conversational communication methods employed by chatbots have the potential to enhance engagement by offering extra motivational and emotional support.11,12 Furthermore, chatbots provide patients with the convenience of receiving assistance at any time through smartphone apps or online platforms. 13 Moreover, they have the potential to enhance patient education, empower self-management, and improve glycemic control by providing guidance on diet, exercise, medication, and blood glucose monitoring.10,14 Additionally, AI chatbots have shown strong alignment with clinical protocols in insulin dosing, outperforming traditional medical prescriptions. This suggests chatbots can improve diabetes management by enhancing treatment adherence and optimizing insulin therapy. 15
By leveraging AI, natural language processing, and machine learning, chatbots can engage in conversational interactions with users. They adapt based on past interactions to provide personalized support. 16 Accordingly, this narrative review aims to explore the current state of chatbots in blood glucose self-monitoring and insulin management, highlighting their potential benefits and future directions in diabetes care.
Methods
This narrative review explores the role of chatbots in self-management of patients with type-2 diabetes. Methodological adjustments were designed to address the unique challenges of emergency and triage nursing, enabling a more thorough evaluation of chatbot applications. Accordingly, a comprehensive literature search was conducted using PubMed, Science Direct, and Google Scholar to identify relevant studies. A health informatics specialist was consulted to design an effective search strategy that combined natural language and Medical Subject Headings (MeSH) terms. Since most recent AI-related studies have been published in the last few years, filters were applied to include research published between 2020 and 2025.
Search strategy
Searching strategies in relevant databases.

Study selection
The search found 647 potential studies. Studies were included if they discussed patient centered chatbot or AI tool applications in diabetes management, particularly in type-2 diabetic patients, based on their title, abstract, or keywords. Exclusion criteria included studies conducted on different diabetes types, research involving AIs other than chat bots, opinion pieces lacking empirical evidence, and non-English publications. A PRISMA flowchart was used to independently show the selection process (Figure 1). PRISMA flowchart for study selection.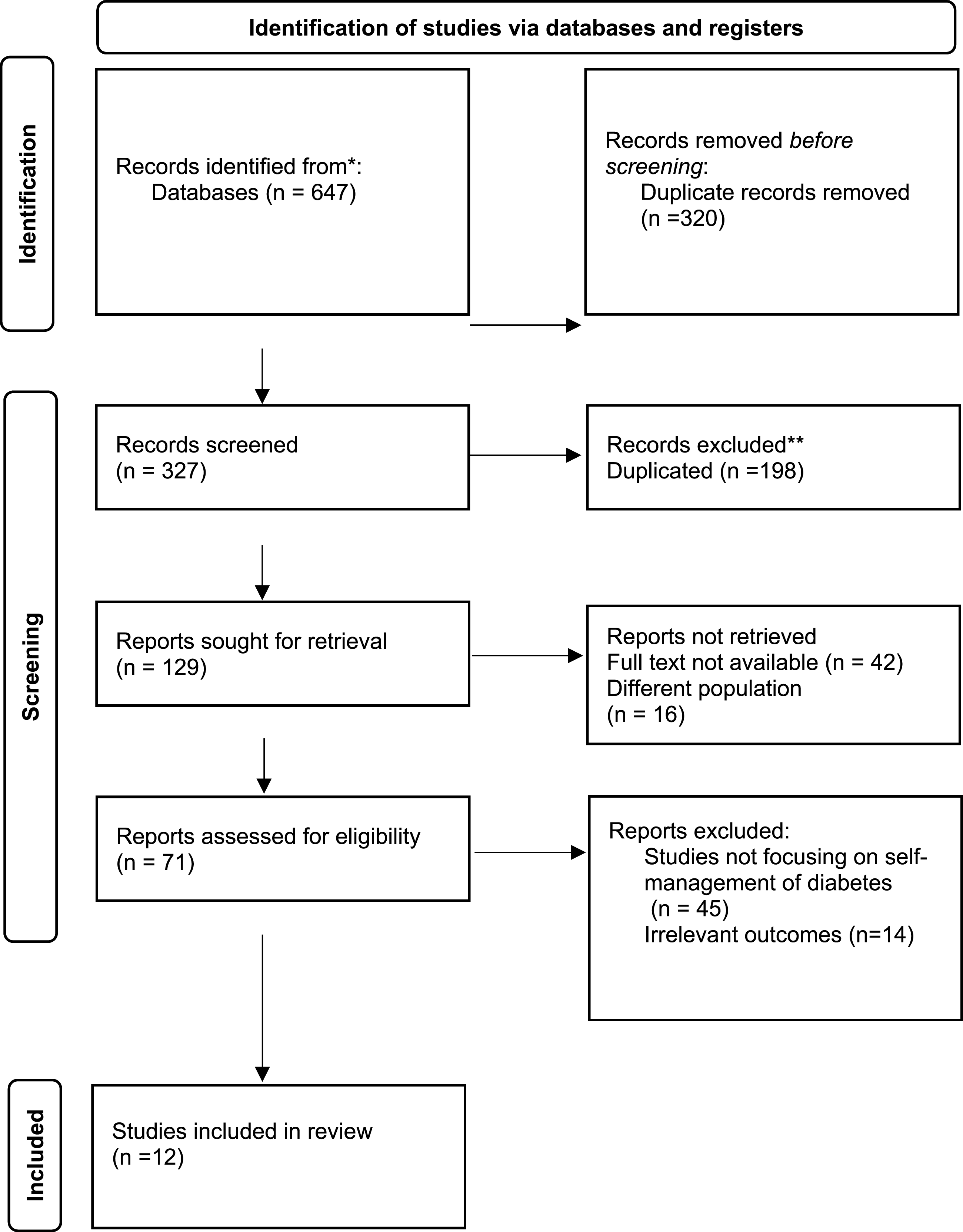
Data extraction
A standardized data extraction process was employed to ensure the accuracy and consistency of the collected data. Two independent reviewers (M.M and H.MT) conducted the data extraction, and any discrepancies were resolved through discussion with a third reviewer (M.S) to minimize bias and enhance reliability. The extracted data included key elements such as study characteristics, participant demographics, intervention details, outcome measures, and results.
Study characteristics included the author(s), year of publication, country of origin, study design (e.g., randomized controlled trial, cross-sectional, cohort study), and sample size. Participant characteristics such as the type of diabetes (focusing on type 2 diabetes), age, gender, and other relevant demographic details were also collected.
Intervention details were carefully recorded, including the type of chatbot used (e.g., AI-powered, rule-based), the primary function of the chatbot (e.g., blood glucose monitoring, dietary guidance, medication adherence), and the frequency and duration of chatbot use. The AI features employed, such as natural language processing and machine learning capabilities, were also noted.
Outcome measures focused on key aspects of diabetes self-management, including improvements in blood glucose levels, medication adherence, lifestyle modification, patient engagement, and satisfaction. Clinical outcomes, such as reductions in HbA1c levels, were recorded alongside psychological outcomes, including reductions in diabetes-related distress. Key findings related to the effectiveness of chatbots in diabetes self-management, along with any reported statistical significance, were documented. All extracted data were compiled into a structured table to facilitate analysis and synthesis.
Data synthesis
Findings from the 12 selected studies were synthesized narratively. Key insights related to chatbot applications in emergency nursing were categorized and summarized. The narrative analysis connected theoretical insights with real-world applications, focusing on development, implementation and effectiveness of Chatbots in diabetes self-management.
Integration of theoretical framework
In this review, the Chronic Care Model (CCM) was applied as a guiding framework to organize and interpret the findings. The CCM was chosen because it provides a comprehensive structure for evaluating chronic disease management interventions, emphasizing six key components: self-management support, delivery system design, decision support, clinical information systems, health system/organization of care, and community resources and policies. By mapping the included studies onto these components, this review highlights how chatbots contribute to strengthening each dimension of chronic care, ranging from enhancing patient self-management to improving system-level efficiency and continuity of care. 17
Results
Summary of studies on Chatbots in Type 2 diabetes self-management.

Chatbot studies mapped to the Chronic Care Model (CCM) domains.

Chatbot development and implementation
Several studies focused on the development and implementation of chatbots for diabetes self-management. For example, Echeazarra et al. (2021) developed “TensioBot,” a chatbot designed for self-managed blood pressure monitoring, providing real-time feedback and advice based on user data, which improved patient engagement and adherence to treatment. 18 Similarly, Mash et al. (2022) evaluated the “GREAT4Diabetes” WhatsApp chatbot during the COVID-19 pandemic, reporting enhanced patient engagement and understanding of diabetes self-care. Additionally, the chatbot helped reduce physical visits to healthcare facilities, ensuring patient safety and maintaining service efficiency during the pandemic. 19 Nassar et al. (2023) assessed a diabetes education chatbot for T2D, noting positive behavioral and clinical outcomes, with improved patient knowledge and engagement. 20
Effectiveness of chatbots in diabetes management
The effectiveness of chatbots in diabetes management was a key focus in several studies. Wu et al. (2024) 14 conducted a systematic review and meta-analysis of 25 studies, finding that chatbot use in diabetes self-management led to improved blood glucose levels, although evidence for weight reduction was limited. Lee et al. (2023) performed a randomized controlled trial involving 294 participants, demonstrating that an AI-based dietary management system improved HbA1c levels and facilitated weight loss over 48 weeks in T2D patients, with the AI platform yielding better outcomes than routine care, highlighting the enhanced efficacy of combining AI tools with professional guidance. 21 Magee et al. (2022) conducted a study that demonstrates patient acceptability and satisfaction, suggesting improvements in A1C levels and self-care confidence among a primary care population. Combined with the evaluation of a personalized diabetes chatbot for adults with type 2 diabetes (T2D), early results indicate enhanced user engagement and self-management outcomes. 22 In a review of eleven studies conducted by Hani et al. (2023), the significant impact of achieving diabetes self-management through information technology (IT) using natural language processing (NLP) methods was confirmed. These methods included deploying a semi-automated interactive system in real-time to interpret patients’ biological data, physical activity, and calculated dietary content derived from messages sent by patients to enhance their self-management. 23
Review and comparative studies
Several review studies provided insights into the broader application of chatbots in chronic disease management. Jiang et al. (2024) conducted a scoping review of 36 studies on embodied conversational agents (ECAs) in chronic disease management, concluding that ECAs were effective in promoting screening and self-management, with high acceptability and effectiveness. 24 Lu et al. (2024) reviewed the “DiaLOG” AI platform, which integrates risk assessment and personalized education for diabetes self-management, with early-stage findings suggesting improved patient engagement and outcomes. 25 Shriyal (2024) reviewed healthcare chatbot applications for diabetes, highlighting benefits in patient education, self-monitoring, and improving adherence to treatment plans. 26
AI chatbots and clinical accuracy
The accuracy and reliability of AI chatbots in providing diabetes-related information were also examined. Nakhleh et al. (2023) assessed ChatGPT’s accuracy in answering diabetes knowledge questions, finding potential for AI in diabetes education but highlighting the need for improved reliability. While ChatGPT demonstrated clear and understandable responses, concerns were raised about its lack of referencing and sourcing, emphasizing the importance of validating AI-generated information in medical contexts. 27 Rojas-López et al. (2024) compared an AI chatbot to physicians in managing in-hospital glucose levels in T2D patients, reporting comparable effectiveness, suggesting that AI chatbots may aid inpatient diabetes care. 15
Quantitative outcomes of Chatbot interventions in diabetes management
A number of included studies reported quantitative outcomes that help clarify the clinical significance of chatbot interventions. In a systematic review and meta-analysis of 25 studies, Wu et al. (2024) found that chatbot-supported diabetes self-management significantly reduced HbA1c by an average of 0.30% (95% CI 0.04–0.55; p = .02), although no significant effect was observed on body weight (MD = 1.41 kg; 95% CI –2.29 to 5.11; p = .46). 14 Similarly, in a large randomized controlled trial involving 294 participants, Lee et al. (2023) demonstrated that an AI-based dietary management chatbot improved both HbA1c and weight loss over 48 weeks compared with routine care, underscoring the added value of AI-enhanced guidance, although exact mean differences were not reported. 21
Evidence from smaller trials further supports these findings. For instance, Magee et al. (2022) described improvements in A1C levels and greater self-care confidence in a primary care population using a personalized diabetes chatbot, though quantitative details were limited. 22 In the inpatient setting, Rojas-López et al. (2024) found that an AI chatbot achieved glucose control outcomes comparable to physicians, suggesting the potential for safe application in hospital care, even though effect sizes were not explicitly provided. 15
Conclusively, anchoring your results within the Chronic Care Model shows that chatbots do not just provide isolated technological support they touch all dimensions of chronic care delivery. They strengthen self-management, support clinicians, optimize health systems, and can even extend care into the community (Table 3).
Discussion
The aim of this narrative review was to examine the role of AI-based chatbots in diabetes self-management, particularly in blood glucose monitoring and insulin management. Results indicated that chatbots are effective tools for these tasks, enhancing patient engagement through personalized support and continuous access to information.
Glycemic outcomes
Studies show that chatbots improve blood glucose control and adherence to treatment plans by offering instant feedback, and tailored nutritional guidance. 21 Stanford University’s study 28 on the application of chatbots in diabetes management demonstrated significant improvements in insulin adherence and blood sugar control among users of this technology. The results highlighted reduced time to achieve optimal insulin dosage and decreased stress related to disease management in patients. These findings underscore the potential of chatbots for specific populations, such as the elderly or individuals with limited access to medical services. However, the study’s limitations include its short duration (2 months) and reliance on fasting blood sugar instead of A1C as an evaluation metric, indicating the need for long-term research and comparisons with other digital systems.
Another study 29 demonstrated that the ease of use and rapid access to information via chatbots enhanced patient satisfaction in dietary planning. These systems, by providing diverse medical resources, address a broad spectrum of patient educational needs; however, in certain instances, limitations in available information have resulted in dissatisfaction. These findings underscore the necessity of developing more advanced algorithms to deliver accurate and up-to-date information.
Implementation barriers
Despite their potential advantages, significant challenges remain. Accuracy and reliability are major concerns, as highlighted by studies like Nakleh et al. (2023), 27 which emphasized risks associated with inaccurate or clinically inconsistent information leading to poor patient decisions. Additionally, disparities in digital literacy and access to technology may limit effective use among certain populations. Long-term sustainability of chatbot interventions is also unclear, necessitating further research through randomized controlled trials (RCTs) to strengthen evidence. Beyond these factors, the absence of emotional intelligence in chatbots represents a significant limitation in their application to diabetes self-care. Additionally, limited digital literacy and unequal access to technology may restrict use among older adults, rural populations, or those with socioeconomic disadvantages.30,31 Privacy and data security concerns also pose challenges, as patients may hesitate to share sensitive health information through AI systems. 32 Furthermore, language barriers and cultural differences can affect usability and patient engagement, particularly in global or multilingual settings.14,33 Integration with existing healthcare workflows remains another obstacle, as clinicians may perceive chatbots as disruptive or duplicative without clear guidelines and interoperability with electronic health records. Addressing these barriers is essential to ensure equitable, safe, and sustainable implementation of chatbot interventions in real-world diabetes care. 34 Integration with healthcare systems is another priority, ensuring chatbots complement traditional care rather than replace it. Future studies should evaluate broader outcomes such as psychological well-being, quality of life, and cost-effectiveness to assess the overall impact on patient health. 27
Ethical considerations and policies
The implementation of chatbots requires rigorous ethical considerations to mitigate algorithmic biases. System design must adhere to principles of equitable access and avoid exacerbating existing health inequities. Furthermore, integration of these technologies into electronic health record (EHR) systems and healthcare provider training programs is critical for optimal utilization. 35 Accordingly, to improve feedback, we should educate patients on how to use chatbots effectively, ensuring better patient-reported outcomes. While chatbot-based education implementation depends on national policies.
Cost-effectiveness of chatbots
Although few studies provided formal economic evaluations, the reviewed evidence suggests that chatbots offer operational efficiencies and potential cost benefits. For example, the GREAT4Diabetes WhatsApp chatbot reduced in-person clinic visits during the COVID-19 pandemic, 34 while primary care–integrated chatbots improved HbA1c and patient satisfaction without increasing provider workload. 14 Platforms such as DiaLOG and TensioBot demonstrate scalability, leveraging existing digital infrastructure for broader population reach. 18 By automating patient education, monitoring, and routine counseling, chatbots may also optimize workforce utilization and reduce clinician burden, although oversight is necessary to ensure accuracy.32,33 Overall, these findings indicate that chatbot interventions could enhance efficiency, scalability, and workforce effectiveness in diabetes care, highlighting the need for future studies to include formal cost-effectiveness analyses.
Future researches
While preliminary evidence demonstrates promise, substantial aspects of chatbot applications in patient support remain underexplored. Additional research is warranted to assess the efficacy of these systems across diverse populations including individuals with limited health literacy or comorbid conditions and to conduct comparative analyses with conventional methodologies. Investigating the operational impacts of these technologies within real-world clinical settings constitutes a priority for future investigation. Chatbots show promise for managing diabetic self-care,14,26 but the current evidence base is limited. Further research, including randomized controlled clinical trials, is required to strengthen the evidence.
At last, while AI-based chatbots cannot replace healthcare professionals, they can serve as valuable tools to alleviate workload pressures, especially during crises like pandemics 19 where access to in-person care is limited. However Continuous monitoring of information accuracy and patient education on effective usage are crucial for maximizing their benefits.
Limitations
The methodology of this narrative review presents several limitations that must be acknowledged. The selection of PubMed, Science Direct, and Google Scholar, CINAHL and Embase as the primary databases, while comprehensive, may have resulted in the exclusion of relevant studies indexed in other databases such as IEEE Xplore or Scopus, potentially limiting the breadth of the literature reviewed. The restriction to studies published between 2020 and 2025 ensures the inclusion of recent advancements but may have overlooked earlier foundational research that could provide essential context. Additionally, despite the structured search strategy developed with input from a health informatics specialist, the reliance on specific keywords and MeSH terms may have inadvertently omitted studies employing alternative terminologies to describe chatbot interventions in diabetes self-management. The inclusion of only English-language publications introduces a language bias, potentially excluding valuable findings from non-English sources and limiting the generalizability of the results.
Furthermore, although study selection was conducted independently by two researchers, subjective judgment was involved in determining the relevance of articles based on titles and abstracts. While a third reviewer was consulted to resolve discrepancies, the potential for selection bias remains. The heterogeneity of included studies, encompassing diverse research designs, sample sizes, and chatbot intervention methodologies, complicates direct comparisons and limits the synthesis of consistent conclusions. Additionally, the absence of standardized outcome measures across studies poses challenges in evaluating the overall effectiveness of chatbot applications in diabetes self-management. On the other hand, without systematic risk of bias assessments or quality grading, the strength and reliability of the evidence cannot be fully established. Many included studies varied in design, sample size, and outcome reporting, which may introduce heterogeneity and affect the generalizability of findings. Additionally, several studies lacked detailed methodological information or did not report effect sizes, limiting the ability to compare results across interventions. Future reviews should incorporate structured quality assessments. Lastly, the predominance of studies with short follow-up periods restricts insights into the long-term effectiveness and sustainability of chatbot interventions. Addressing these methodological limitations in future research will be essential for improving the robustness and applicability of findings in this domain.
Conclusion
Within the framework of the Chronic Care Model, AI-based chatbots show promise in improving diabetes self-management by enhancing education, engagement, and system efficiency. However, current evidence is limited, and further rigor is needed. Future work should include randomized controlled and hybrid implementation–effectiveness trials, with attention to equity for elderly, rural, and low-literacy populations. Strengthening accuracy, data security, and integration with electronic health records will be essential. Aligning chatbot development with CCM principles can help establish them as scalable, equitable, and sustainable tools in chronic disease care.
Footnotes
Acknowledgments
Hereby, we express our sincere gratitude to all the experts who helped us with the present study.
Author contributions
Hooman Mohammad Talebi: Supervision, Data Curation, Conceptualization, Revision, Methodology. Mehdi Safarabadi: Supervision, Data Curation, Conceptualization, Revision. Marzieh Mousivand: Data curation, Writing Original Draft, Investigation. Aref Zarei: Data curation, Writing Original Draft, Revision. Mohammad Sadegh Fakhari: Data curation, Writing Original Draft, Revision
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data would be available via sending formal request to the corresponding author.
