Abstract
Background. A thorough understanding of the presence of different upper-limb somatosensory deficits poststroke and the relation with motor performance remains unclear. Additionally, knowledge about the relation between somatosensory deficits and visuospatial neglect is limited. Objective. To investigate the distribution of upper-limb somatosensory impairments and the association with unimanual and bimanual motor outcomes and visuospatial neglect. Methods. A cross-sectional observational study was conducted, including 122 patients within 6 months after stroke (median = 82 days; interquartile range = 57-133 days). Somatosensory measurement included the Erasmus MC modification of the (revised) Nottingham Sensory Assessment (Em-NSA), Perceptual Threshold of Touch (PTT), thumb finding test, 2-point discrimination, and stereognosis subscale of the NSA. Upper-limb motor assessment comprised the Fugl-Meyer assessment, motricity index, Action Research Arm Test, and Adult-Assisting Hand Assessment Stroke. Screening for visuospatial neglect was performed using the Star Cancellation Test. Results. Upper-limb somatosensory impairments were common, with prevalence rates ranging from 21% to 54%. Low to moderate Spearman ρ correlations were found between somatosensory and motor deficits (r = 0.22-0.61), with the strongest associations for PTT (r = 0.56-0.61) and stereognosis (r = 0.51-0.60). Visuospatial neglect was present in 27 patients (22%). Between-group analysis revealed somatosensory deficits that occurred significantly more often and more severely in patients with visuospatial neglect (P < .05). Results showed consistently stronger correlations between motor and somatosensory deficits in patients with visuospatial neglect (r = 0.44-0.78) compared with patients without neglect (r = 0.08-0.59). Conclusions. Somatosensory impairments are common in subacute patients poststroke and are related to motor outcome. Visuospatial neglect was associated with more severe upper-limb somatosensory impairments.
Introduction
The somatosensory system allows us to interpret somatosensory stimuli received from receptors located in the joints, ligaments, muscles, and skin. 1 Somatosensory information such as pain, pressure, or joint position sense, is then processed in different brain regions to modulate incoming sensory information. 1 Key brain regions involved in processing somatosensory information are the primary and secondary somatosensory cortex, the thalamus, insula, posterior parietal cortex, and the cerebellum. 2 Within the somatosensory system, a classification in exteroceptive, proprioceptive, and higher cortical somatosensation can be identified.3,4 Each of these categories includes a set of somatosensory modalities such as light touch and pain within exteroceptive somatosensation, position and movement sense within proprioceptive somatosensation, and somatosensory discrimination sense within higher cortical somatosensation. 3 Deficits of these somatosensory modalities are common after stroke, with prevalence rates ranging from 11% to 85%.5-7 Variability is attributed to differences in definition, study populations, somatosensory modalities tested, and assessment method used. 5 To date, most studies concentrated on identifying deficits in a single somatosensory modality such as light-touch perception or joint position sense. Therefore, a thorough understanding of the prevalence and distribution of deficits in different exteroceptive, proprioceptive, and higher cortical somatosensory modalities in the subacute phase poststroke is lacking.
Along with upper-limb somatosensory impairments, approximately 70% of patients poststroke experience motor impairments in the affected upper limb. 8 Our recent systematic review 9 investigating the impact of somatosensory deficits on outcome after stroke showed that different somatosensory impairments are negatively associated with motor recovery in the upper limb. Despite these results, the review highlighted the need for large high-quality cohort studies that combine somatosensory measures of different modalities to determine the relationship with both unimanual and bimanual motor performance with more accuracy.
It is well known from previous literature that visuospatial neglect, a neuropsychological disorder often encountered poststroke, negatively affects recovery.10-16 Unilateral visuospatial neglect has been defined as the inability to detect, respond to, and orient toward novel and significant stimuli occurring in the hemispace contralateral to a brain lesion. 17 The reported incidence of neglect ranges between 10% and 80% in stroke survivors.18,19 Variability among studies is again believed to be related to participant selection, nature and timing of the assessment, and differences in definitions of this complex phenomenon. 20 It was recently shown that the time course of recovery of visuospatial neglect mimics the recovery patterns of other neurological impairments such as motor or functional outcome, with large improvements in the first weeks poststroke and with the recovery reaching a plateau around 3 months poststroke. 21 Visuospatial neglect is known to increase length of hospital stay, 11 may hinder response to therapy, 11 and is negatively associated with performance in activities of daily living. 12 Nijboer et al 13 showed that on admission to the rehabilitation center, patients with visuospatial neglect have significantly worse functional performance compared with patients without neglect, as measured with the Barthel Index and Functional Independence Measure. 13 A detailed analysis of the different domains of the Functional Independence Measure showed that on average, patients with neglect scored significantly lower on self-care, transfers, and locomotion compared with the nonneglect patients, whereas no differences were found between groups for sphincter control and cognition. 13
Furthermore, visuospatial neglect is linked to poor motor performance13,15,16 and has a suppressive effect on upper-limb motor recovery, mainly during the first 3 months poststroke when spontaneous neurological recovery is taking place. 14 Despite the shared neuroanatomy between somatosensory processing and the presence of visuospatial neglect in areas of the parietal cortex,22,23 only a few studies13,14,24-27 reported the relationship between visuospatial neglect and somatosensation in the upper limb. The presence of visuospatial neglect seems to be associated with more severely affected limb position sense in the arm13,14,25-27 and is predictive for impaired limb movement sense. 24 However, information on the association between visuospatial neglect and exteroceptive or higher cortical somatosensory deficits after stroke is lacking.
The primary objectives of this study were therefore (1) to map the prevalence and distribution of different exteroceptive, proprioceptive, and higher cortical somatosensory impairments in the upper limb and (2) to study the association between different somatosensory impairments and unimanual as well as bimanual motor function poststroke. A final objective was to investigate whether the presence of neglect is associated with the occurrence (3a) and severity (3b) of somatosensory impairments and whether the association between somatosensory impairments and unimanual as well as bimanual motor outcome is different for patients with and without visuospatial neglect (3c). The primary hypothesis was that, in line with the previous literature,5-7 upper-limb somatosensory deficits are common and that from the group of somatosensory impairments, higher cortical somatosensory deficits are most prevalent. This hypothesis is driven by the fact that for higher cortical sensation such as discrimination of different objects, an intact exteroceptive sensation (ie, touch and pressure) as well as higher cortical discriminative function is required. 6 Second, based on a recent systematic review completed by the investigators, 9 it was hypothesized that somatosensory impairments are moderately associated with unimanual and bimanual motor function. Third, based on the closely related neuroanatomy,2,22,23 it was further hypothesized that visuospatial neglect is highly associated with the prevalence and severity of exteroceptive, proprioceptive, and higher cortical somatosensory deficits. Finally, based on the previously completed systematic review, 9 we expect that somatosensory deficits are moderately associated with unimanual and bimanual motor function, equally in patients with and without visuospatial neglect.
Methods
Participants
Inclusion and Exclusion Criteria
For this cross-sectional observational study, 122 patients were assessed between October 2013 and August 2014 in 7 neurorehabilitation units in Belgium (n = 102) or in the home environment of the patient (n = 20). Patients assessed in the home environment all completed inpatient rehabilitation and were still enrolled in outpatient physical therapy. The inclusion criteria were the following: (1) first-ever stroke as defined by the World Health Organization (WHO) 28 ; (2) assessed within the first 6 months after stroke; (3) motor and/or somatosensory impairment in the upper limb, using outcome measures as described below; (4) minimally 18 years old; and (5) substantial cooperation to perform the assessment. Patients were excluded if they had the following: (1) a prestroke Barthel index 29 score of <95 out of 100; (2) other neurological impairments with permanent damage, such as multiple sclerosis or Parkinson’s disease; (3) a subdural hematoma, tumor, encephalitis, or trauma that led to symptoms similar to that of a stroke; and (4) serious communication, cognitive, or language deficits, which could hamper the assessment. Participants signed a written informed consent form prior to participation. Ethical approval was obtained from the Ethics Committee of the University Hospital of Leuven and all participating centers.
Patients were assessed in a single test session. One trained researcher performed the data collection. Patients’ baseline characteristics were assessed, including age at stroke onset, gender, comorbidities (Cumulative Illness Rating Scale 30 ), hand dominance, time poststroke, lateralization, and type of stroke.
Outcome Measures
Somatosensory Assessment
Exteroceptive somatosensation
The Erasmus MC modification of the (revised) Nottingham Sensory Assessment (Em-NSA) 31 assesses light touch, pressure, and pinprick. Light touch was applied with a cotton wool, pressure with the index finger, and pinprick with a toothpick at predefined points. Scores for each modality range from 0 (loss of somatosensory function) to 8 (intact somatosensory function). A cutoff score of <7 indicates the presence of somatosensory impairment. The Em-NSA has good to excellent intrarater and interrater reliability. 31
The Perceptual Threshold of Touch (PTT) 32 is the minimal stimulus level of touch that is detectable. A transcutaneous electric nerve stimulation (TENS) was applied with a portable device—the CEFAR Primo Pro (Cefar Medical AB, Sweden). Round electrodes, with a diameter of 3 cm, were applied to the index finger and bulb of the thumb. A high-frequency constant current of 40 Hz with single square pulses of 80 µs pulse duration was applied. The amplitude was gradually increased in increments of 0.5 mA until a tingling sensation was perceived at the index finger. Good psychometric properties are established for the PTT. 32 To evaluate PTT impairment, individual scores were compared with age- and gender-matched cutoff norm values. 33
Proprioceptive somatosensation
The Em-NSA 31 assesses proprioception by passively moving predefined joints of the upper limb. Scores range from 0 (loss of proprioceptive function) to 8 (intact proprioceptive function). A cutoff score of <7 indicates the presence of proprioceptive impairment (movement sense). The Em-NSA has good to excellent intrarater and interrater reliability. 31
The thumb finding test (TFT) 34 was used to evaluate proprioception because it examines the ability to locate the thumb of the affected limb in space. The scoring ranges from 0 (no difficulty) to 3 (severe difficulty). A cutoff score of >0 indicates the presence of impaired proprioception (position sense).
Higher cortical somatosensation
The Em-NSA 31 assesses sharp-dull discrimination by alternating sharp (toothpick) and dull (finger) stimuli, at predefined points. Scores range from 0 (loss of discriminative function) to 8 (intact discriminative function). A cutoff score of <7 indicates the presence of higher cortical somatosensory impairment. The Em-NSA has good to excellent intrarater and interrater reliability. 31
During the stereognosis assessment of the original NSA, 35 patients need to identify 11 everyday objects by touch and manipulation in the affected hand, while blindfolded. Assistance to manipulate the objects in the hand is given by the assessor, when needed. For each object a score from 0 (failed to recognize object) to 2 (recognized object) is given. A cutoff score of <19 indicates the presence of stereognosis impairment. The stereognosis section of the NSA shows a moderate to good test-retest reliability in patients with stroke. 36
Two-point discrimination (2PD) 37 was assessed at the fingertip of the index finger. Distance between the points was gradually reduced from 15 mm until the patient incorrectly felt only 1 point. The last correct answer was recorded as the result. The 2PD threshold in healthy controls has a mean of 3.5 mm (±SD = 1.7). 38 Those with a 2PD threshold higher than 5 mm were classified as having impaired 2PD. Good reliability has been found for the 2PD assessment. 37
In summary, based on the different assessments, exteroceptive somatosensation included the measures of light touch, pressure and pinprick (of the Em-NSA), and the PTT. Proprioceptive somatosensation was assessed using the TFT and the proprioception subscale of the Em-NSA. Finally, higher cortical somatosensation comprised sharp-dull discrimination, stereognosis, and 2PD.
Assessment of Visuospatial Neglect
The Star Cancellation Test (SCT) 39 from the Behavioural Inattention Test (BIT) 40 was used to assess the presence of visuospatial neglect. A previous study 41 found the SCT to be the most sensitive paper-and-pencil measure of visuospatial neglect. Different stimuli are presented on a piece of paper, including large stars, letters, short words, and small stars. The test page is placed at the patient’s midline. The task is to locate and cross out all small stars using their hand of choice. A cutoff score of <44 (out of 54 stars) indicates the presence of visuospatial neglect. 42 A lateralization index was calculated from the ratio of stars cancelled on the left of the page to the total number of stars cancelled, according to Halligan et al. 43 Laterality scores range from 0 to 1, with values near 0.5 suggesting unbiased performance, between 0 and 0.46 indicating visuospatial neglect in the left hemispace, and between 0.54 and 1 indicating visuospatial neglect in the right hemispace. Interrater reliability of the SCT is found to be high. 44
Motor Assessment
The Fugl-Meyer Motor Assessment Upper Extremity (FMA-UE) 45 is a reliable and valid measure for overall motor impairment, with a total score between 0 and 66. The Action Research Arm Test (ARAT) 46 measures motor performance in 4 different subscales: grasp, grip, pinch, and gross movement, with a maximum score of 57. Reliability 47 and validity 48 are established for the ARAT. The arm section of the motricity index (MI) 49 is a reliable measure of muscle strength during pinch grip, flexion of the elbow, and abduction of the shoulder. Total scores vary between 0 and 100. The Adult Assisting Hand Assessment Stroke (Ad-AHA Stroke), a Rasch-based performance scale, measures how effectively the affected hand is spontaneously used during performance of a bimanual task. Performance of the semistructured present task was videorecorded. A total of 19 test items, describing different object-related hand actions, are scored on a 4-point scale rating the quality of performance. The raw scores are then converted through the Rasch analysis to logit scores varying between 1 and 100, with higher scores indicating higher bimanual ability levels (unpublished results). 50
Statistical Analysis
Patients’ clinical and demographic characteristics are displayed as frequencies with percentage, mean with SD, and median with interquartile range (IQR). The prevalence and distribution of deficits in different somatosensory modalities such as light touch, position sense, or stereognosis were calculated using frequencies with percentages according to the presence of exteroceptive, propriocepive, or higher cortical somatosensory problems. Therefore, the different somatosensory variables were dichotomized according to the presence of a deficit or normal functioning based on the above-mentioned predefined cutoff values. Furthermore, associations between somatosensory and motor impairments were assessed using Spearman rank correlation coefficients. For this analysis, the full score range of the somatosensory and motor variables was used. Strength of the relation was interpreted according to Munro’s correlation descriptors 51 : very low, r = 0.01-0.24; low, r = 0.25-0.49; moderate, r = 0.50-0.69; high, r = 0.70-0.89; and very high, r = 0.90-1.00.
To study the relation with neglect, first, all clinical and baseline characteristics from patients with visuospatial neglect were compared with those of patients without visuospatial neglect by using the Wilcoxon rank sum test and χ2 tests. Second, the prevalence of somatosensory deficits in patients with visuospatial neglect was compared with the prevalence in patients without visuospatial neglect by using χ2 tests. Severity of different somatosensory impairments was compared between patients with and without visuospatial neglect, using the Wilcoxon rank sum test. Finally, using the Fisher r-to-z transformation, it was tested whether the correlation coefficients for the association between somatosensory and motor impairments found in the patients with and without neglect were significantly different. P values were considered statistically significant at the .05 level. All statistical analyses were performed using SPSS, version 22.
Results
A total of 122 patients were assessed once between 12 days and 6 months poststroke (median = 82 days; IQR = 57-133). Table 1 shows the patient characteristics, presented for the total group, for the patients with visuospatial neglect (n = 27, 22%) and without visuospatial neglect (n = 95, 78%). For the total group, median age at stroke onset was 67 years (IQR = 59-76), and 63% of the patients were male. The majority of patients suffered from ischemic stroke (88.5%). A total of 48 patients (39%) showed right-sided hemiparesis and 73 patients (60%) left-sided hemiparesis; 1 patient had symptoms on both sides of the body.
Patient Characteristics.
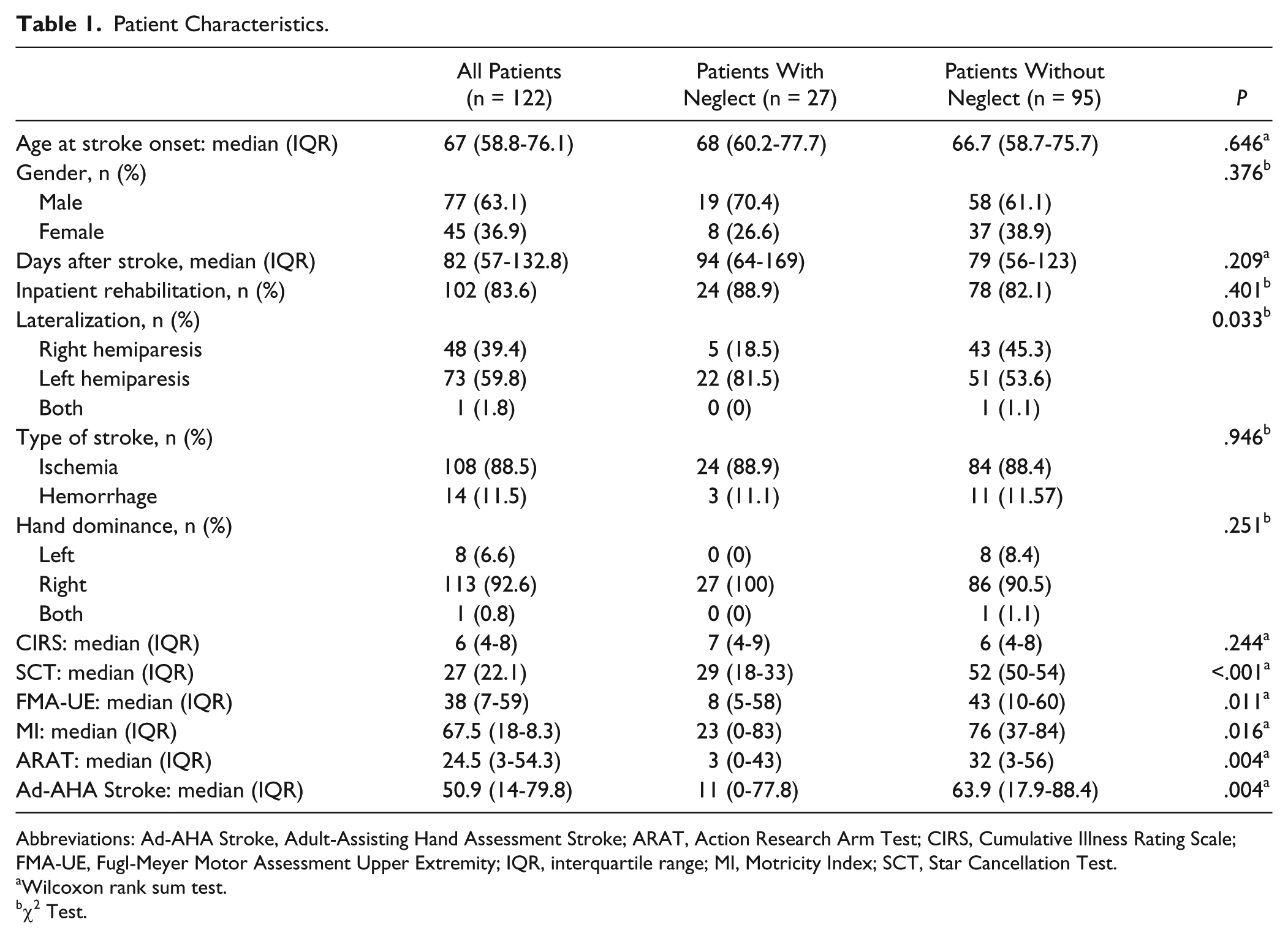
Abbreviations: Ad-AHA Stroke, Adult-Assisting Hand Assessment Stroke; ARAT, Action Research Arm Test; CIRS, Cumulative Illness Rating Scale; FMA-UE, Fugl-Meyer Motor Assessment Upper Extremity; IQR, interquartile range; MI, Motricity Index; SCT, Star Cancellation Test.
Wilcoxon rank sum test.
χ2 Test.
Total Group
Objective 1: Map Prevalence and Distribution of Different Somatosensory Impairments
In the total group, exteroceptive impairments (light touch, pressure, pinprick, light-touch threshold) were present in 21% to 37% of the patients, with the PTT revealing the highest frequency (37%) of exteroceptive dysfunction. Proprioceptive impairment (position sense, movement sense) was diagnosed in 23% of the patients when using the Em-NSA, whereas 54% of the patients showed proprioceptive impairment using the TFT. Finally, deficits in higher cortical somatosensation (sharp-dull discrimination, stereognosis, 2PD) were present in 43% to 50% of the patients (Figure 1, panel A). Panel B shows the distribution of somatosensory impairments according to the presence of unique (pure) exteroceptive, unique proprioceptive, or unique higher cortical somatosensory impairments or a mixture of these deficits. This shows that only 16% of the patients presented without somatosensory impairment and that approximately 50% of the patients experienced a mixture of somatosensory impairments. Therefore, only a minority of patients had unique exteroceptive (14%), unique proprioceptive (9%), and unique higher cortical somatosensory (13%) impairments.
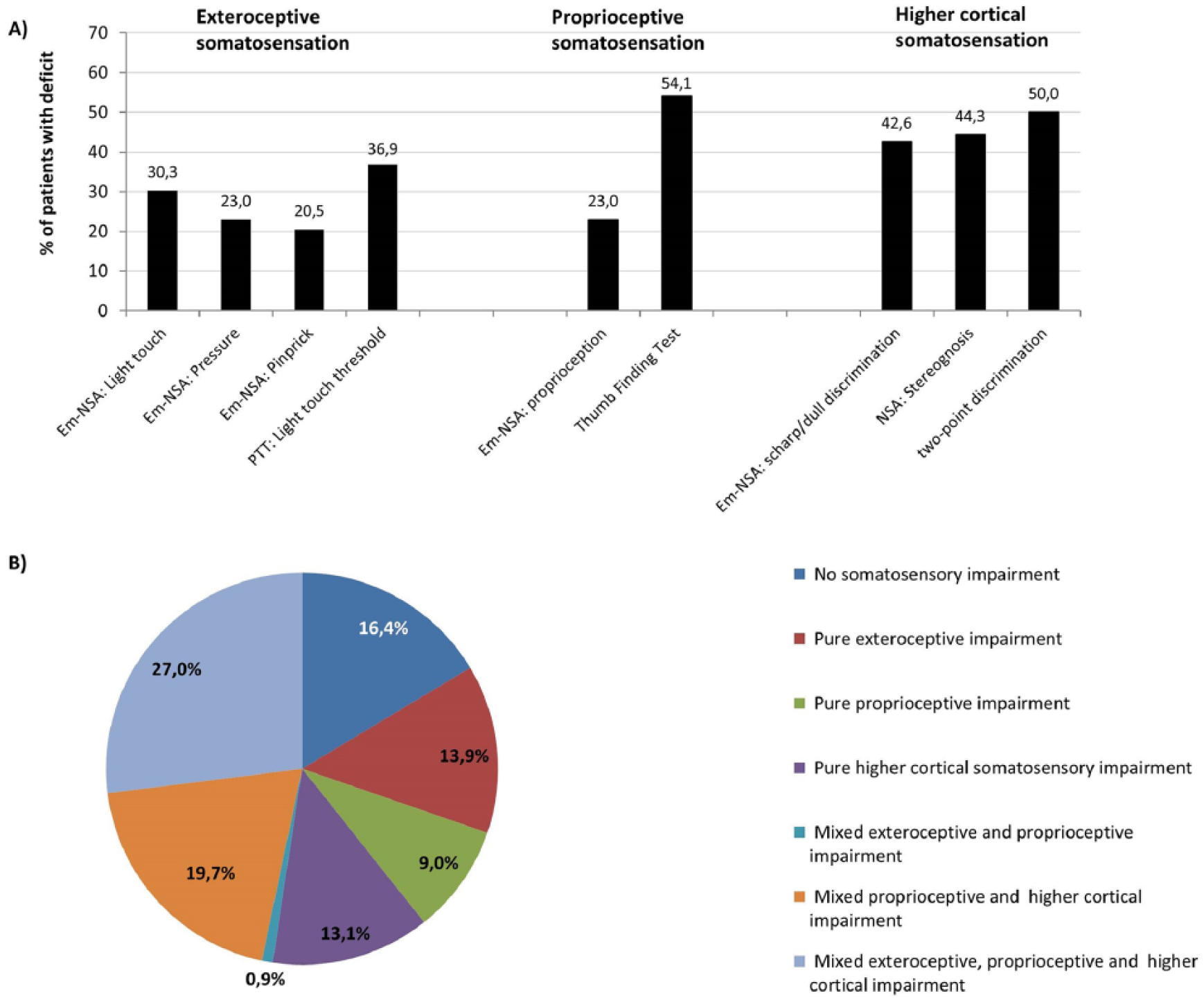
A. Prevalence of exteroceptive, proprioceptive, and higher cortical somatosensory deficits in the upper limb after stroke in all patients. B. Distribution of somatosensory deficits: unique (pure) and mixed somatosensory impairments in all patients.
Objective 2: Study Sensorimotor Associations
Table 2 shows results of the correlation analysis between somatosensory and unimanual (FMA-UE, MI, ARAT) and bimanual (Ad-AHA Stroke) motor assessment for the total group. Overall, low correlations (r = 0.22-0.44) were found between somatosensory and motor deficits, except for the PTT and stereognosis, which showed moderate correlations with motor function (r = 0.51-0.61). For each of the somatosensory variables, comparable results were found for the association with unimanual and bimanual motor function.
Spearman ρ Correlation Coefficients for Association Between Somatosensory and Motor Impairments in All Patients (n = 122). a
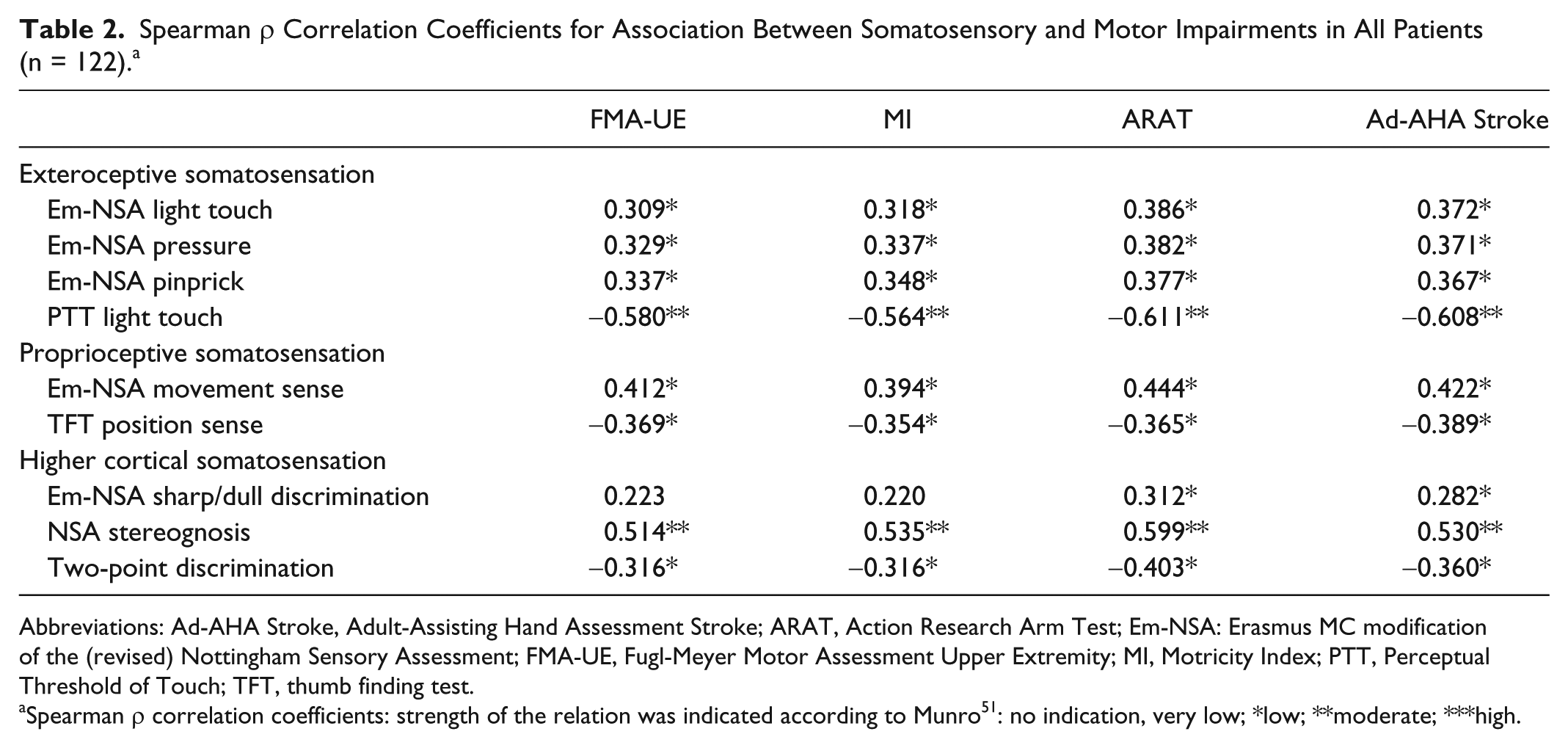
Abbreviations: Ad-AHA Stroke, Adult-Assisting Hand Assessment Stroke; ARAT, Action Research Arm Test; Em-NSA: Erasmus MC modification of the (revised) Nottingham Sensory Assessment; FMA-UE, Fugl-Meyer Motor Assessment Upper Extremity; MI, Motricity Index; PTT, Perceptual Threshold of Touch; TFT, thumb finding test.
Spearman ρ correlation coefficients: strength of the relation was indicated according to Munro 51 : no indication, very low; *low; **moderate; ***high.
Between-Group Differences in Patients With and Without Visuospatial Neglect
Objective 3a: Map Prevalence and Distribution of Somatosensory Deficits
In total, 27 patients had visuospatial neglect, with a median score on the SCT of 29 (IQR = 18-33); 20 patients had visuospatial neglect in the left hemispace and 4 in the right hemispace, and 3 had nonlateralized visuospatial neglect. As seen in Table 1, patients with visuospatial neglect had right-hemisphere lesions significantly more often and had significantly more severe unimanual (FMA-UE, MI, ARAT) and bimanual (Ad-AHA Stroke) motor scores compared with patients without neglect. Figure 2 shows the prevalence (panel A) and distribution (panel B) of somatosensory impairments for patients with and without visuospatial neglect. Patients with neglect have somatosensory impairments (prevalence 41% to 78%) significantly (P < .05) more often (Figure 2, panel A) compared with patients without neglect (prevalence 15% to 47%). The distribution analysis presented in panel B showed that in the neglect group, 7.4% had no somatosensory impairment, which is considerably less compared with the non neglect group (18.9%). Furthermore, 74.1% of the patients with visuospatial neglect presented with mixed exteroceptive, proprioceptive, or higher cortical somatosensory impairments, whereas only 40% presented with mixed impairments in the non neglect group.
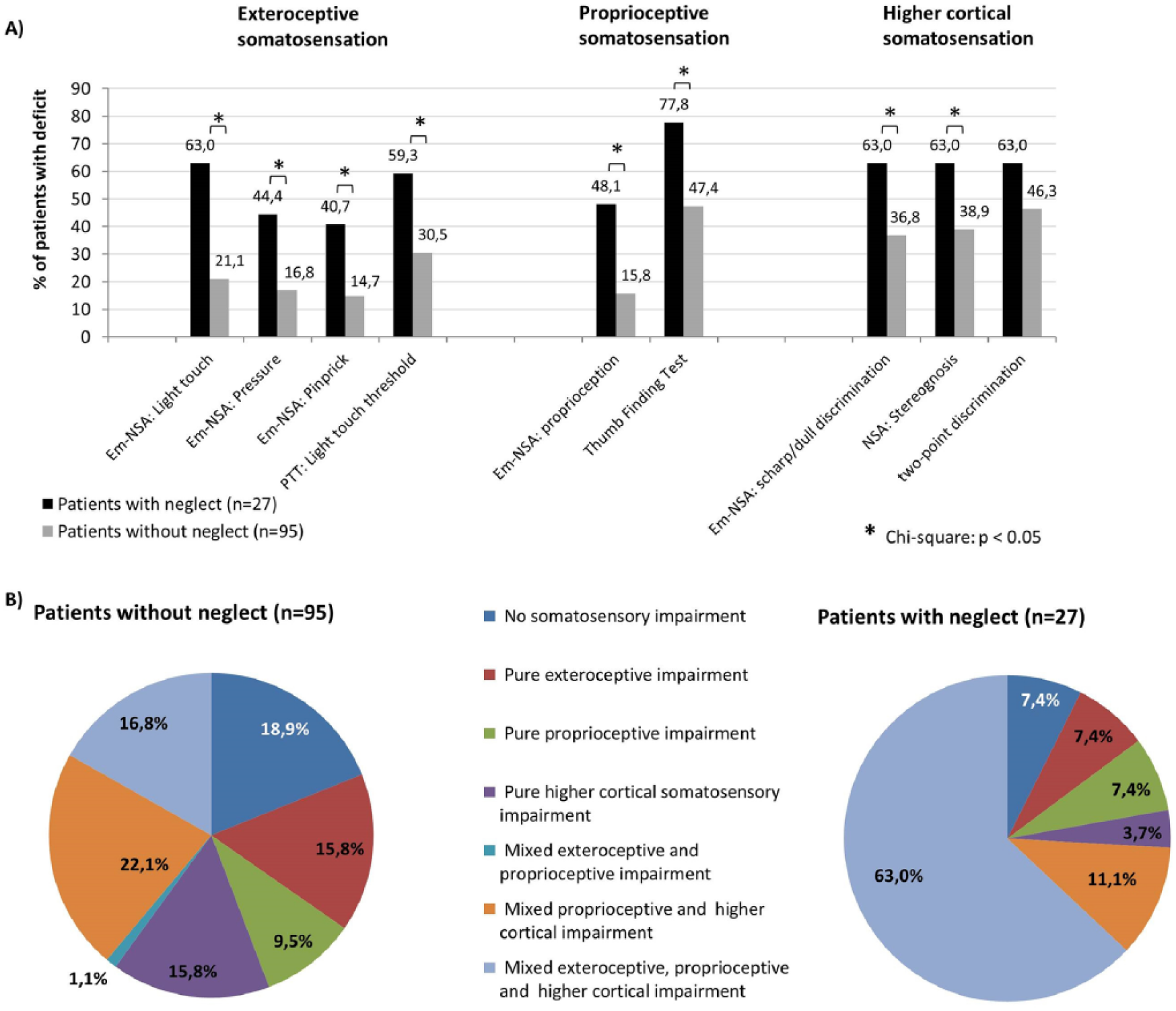
A. Prevalence of exteroceptive, proprioceptive, and higher cortical somatosensory deficits in the upper limb after stroke in patients with and without visuospatial neglect. B. Distribution of somatosensory deficits: unique (pure) or mixed somatosensory impairments in patients with and without visuospatial neglect.
Objective 3b: Assess Severity of Somatosensory Impairments
Significant between-group differences in severity of the different somatosensory impairments are shown in Table 3. Exteroceptive (light touch, pressure, pinprick, light-touch threshold), proprioceptive (position sense, movement sense), and higher cortical somatosensory (sharp-dull discrimination, stereognosis, 2PD) functions were significantly (P < .05) more severely affected in patients with visuospatial neglect.
Differences in Severity of Somatosensory Impairments in Patients With and Without Visuospatial Neglect.
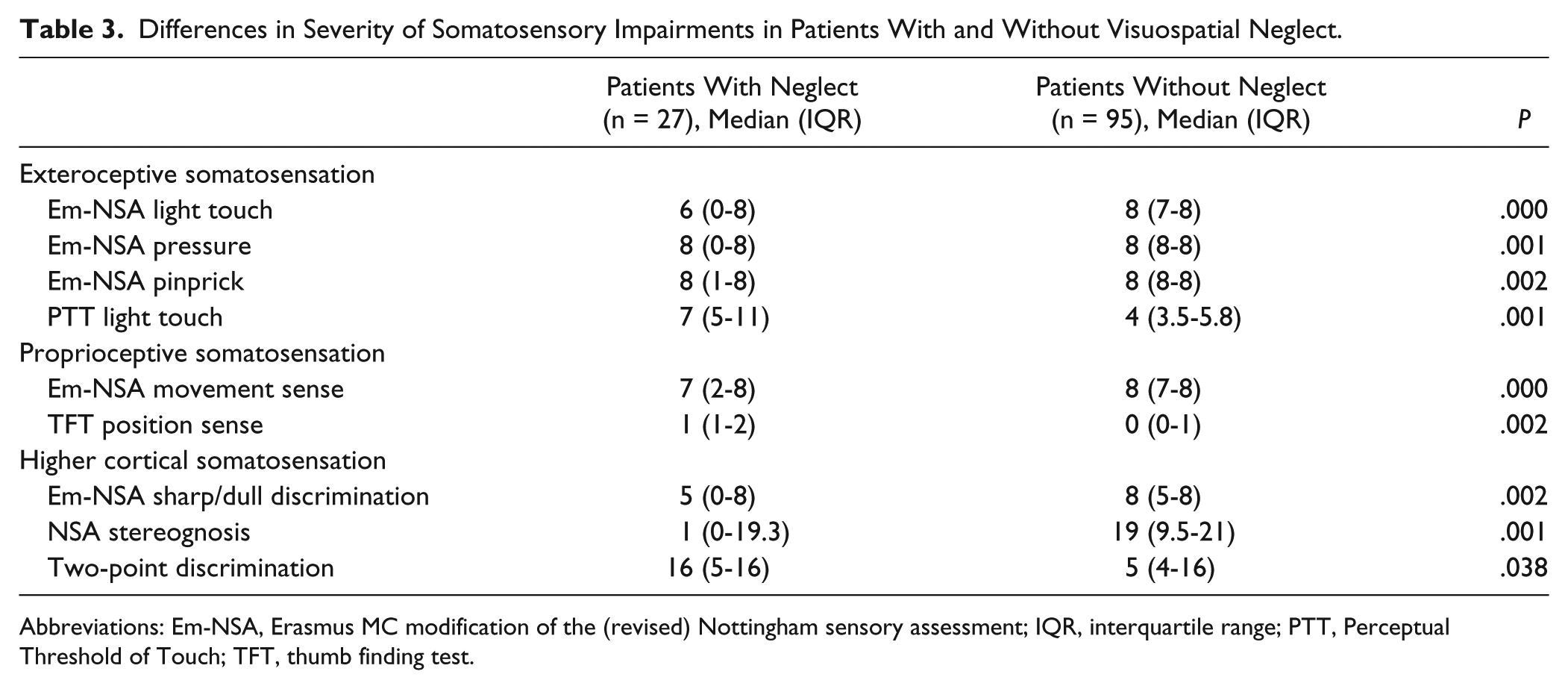
Abbreviations: Em-NSA, Erasmus MC modification of the (revised) Nottingham sensory assessment; IQR, interquartile range; PTT, Perceptual Threshold of Touch; TFT, thumb finding test.
Objective 3c: Study Sensorimotor Associations
The correlation analysis between somatosensory and unimanual and bimanual assessment in patients with and without visuospatial neglect (Table 4) revealed overall stronger correlations in the neglect group (r = 0.44-0.78) compared with the non neglect group (r = 0.08-0.59), with statistically significant between-group differences for the correlation of all motor scores (except for the ARAT) with stereognosis and pressure. On the other hand, the correlation between the PTT and all 4 motor outcomes was comparable for patients with neglect (r = 0.46-0.55) and without neglect (r = 0.55-0.59). Furthermore, the association between somatosensory deficits and unimanual outcome (ARAT, FM-UE, MI) was comparable to the association with bimanual outcome (Ad-AHA Stroke). Finally, the highest values in correlation coefficients were found for the association between stereognosis and motor function in patients with neglect (r = 0.72-0.78) as well as without neglect (r = 0.40-0.51).
Spearman ρ Correlation Coefficients for Association Between Somatosensory and Motor Impairments in Patients With and Without Visuospatial Neglect. a
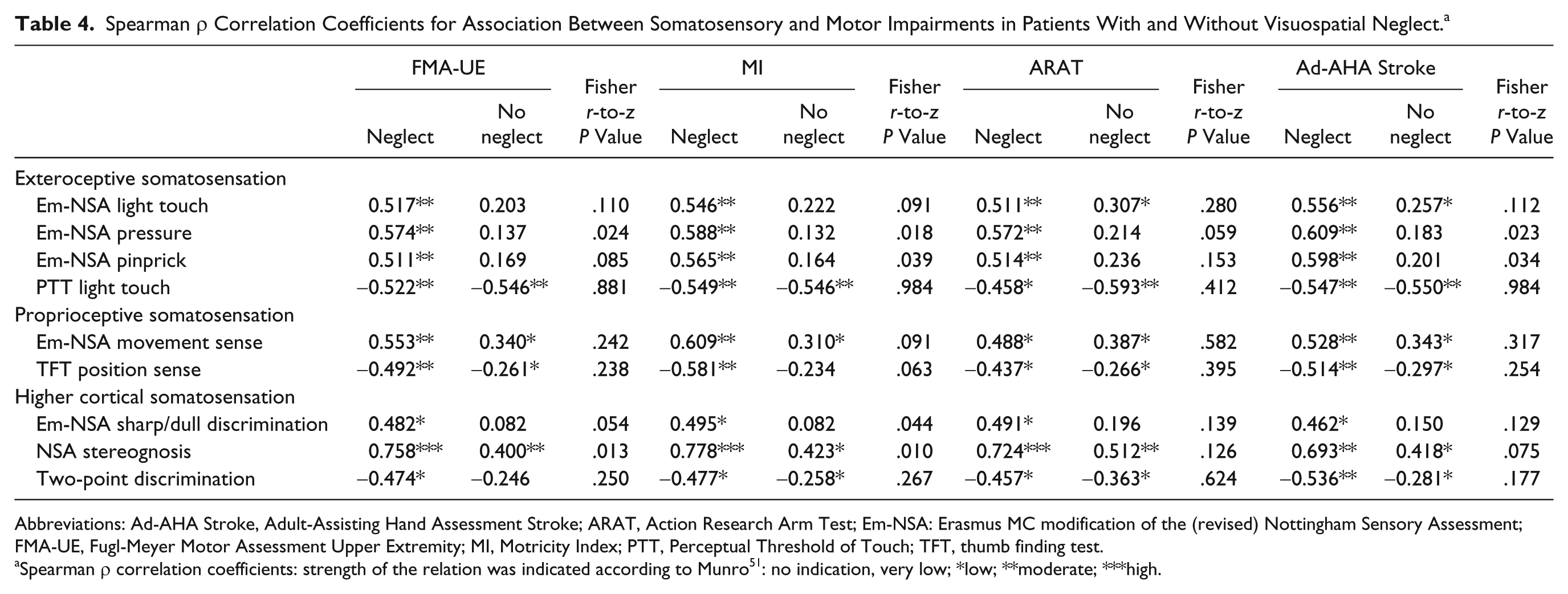
Abbreviations: Ad-AHA Stroke, Adult-Assisting Hand Assessment Stroke; ARAT, Action Research Arm Test; Em-NSA: Erasmus MC modification of the (revised) Nottingham Sensory Assessment; FMA-UE, Fugl-Meyer Motor Assessment Upper Extremity; MI, Motricity Index; PTT, Perceptual Threshold of Touch; TFT, thumb finding test.
Spearman ρ correlation coefficients: strength of the relation was indicated according to Munro 51 : no indication, very low; *low; **moderate; ***high.
Discussion
Results of this study showed that deficits in upper-limb somatosensation are common in patients in the subacute phase poststroke and that these deficits are associated with unimanual and bimanual motor performance. It was shown that patients with neglect have more combined and more severe exteroceptive, proprioceptive, and higher cortical somatosensory deficits compared with patients without neglect. Furthermore, this study showed that in patients with neglect, consistently stronger associations exist between somatosensory impairments and unimanual and bimanual motor performance when compared with patients without neglect.
Results of the study regarding the prevalence of somatosensory deficits are in line with those of previous studies. Connell et al 6 reported that 23% to 47% experienced exteroceptive impairments in the upper limb and 43% to 63% proprioceptive impairments; stereognosis was affected in 31% to 89% of the patients on admission to the rehabilitation center. Tyson et al 7 reported that in a group of patients 2 to 4 weeks poststroke, 55% had exteroceptive dysfunction, whereas only 22% had proprioceptive dysfunction in the upper limb. This result might be explained by the inclusion solely of patients with an anterior circulation stroke, resulting primarily in deficits in the lower limb. Furthermore, the proprioceptive integration areas, located in the posterior parietal lobe in the brain, 52 were probably not affected by lesions in the anterior circulation. Interestingly, this study showed a large difference in prevalence of proprioceptive deficits when using the TFT (54%) compared with the proprioception subscale of the Em-NSA (23%). This latter result might be explained by the difference in assessment methods. During the TFT, position sense of the whole upper limb is assessed, which might be more difficult compared with selective assessment of movement sense in separate joints in the Em-NSA.
As expected from our recent systematic review, 9 this study showed that different somatosensory deficits are associated with motor impairments in the upper limb, especially the PTT and stereognosis, which showed moderate correlations with motor function. For each of the somatosensory variables, comparable results were found for the association with unimanual and bimanual motor function.
As hypothesized, the study showed that patients with visuospatial neglect present with more mixed somatosensory impairments and significantly more severe somatosensory impairments, compared with the non neglect group. This finding could be explained by the extent of the lesion because larger lesions will affect motor, somatosensory, and attention areas in the brain. Patients with neglect had indeed, besides worse somatosensory outcomes, consistently worse motor outcomes. This might provide indirect evidence of larger brain lesions in patients with visuospatial neglect. Brain regions important in somatosensory processing are also in close proximity to brain regions responsible for neglect. In a study by Ptak and Schnider, 23 visuospatial neglect was associated with damage to the temporal-parietal junction, the middle frontal gyrus, and the posterior intraparietal sulcus, whereas Yue et al 53 showed that lesions in the inferior frontal gyrus, precentral and postcentral gyrus, superior and middle temporal gyrus, the insula, and surrounding white matter were more frequent in patients with visuospatial neglect compared with patients without neglect. These regions are in close proximity to the brain areas responsible for the processing of different somatosensory inputs such as the primary and secondary somatosensory cortex, insula, and posterior parietal cortex. 2
We acknowledge that the presence of visuospatial neglect might interfere with the assessment of somatosensory functioning because of the attention deficit. Therefore, the fact that patients with neglect have more mixed and more severe somatosensory impairments might also be attributed to the attention deficit. However, neglect was assessed using the SCT, a test for visuospatial extra-personal neglect, which is distinct from personal neglect,22,54-56 of which the latter plausibly more strongly interferes with somatosensory testing. Furthermore, the sample group included patients with visuospatial neglect without any somatosensory deficit, which supports the idea that somatosensory function in patients with visuospatial neglect can be tested. Future research could use an integrative approach, combining different measures of neglect to capture all the different dimensions of personal and extra-personal neglect using different paper-and-pencil tests and an extensive behavioral assessment such as the Catherine Bergego Scale to study neglect during activities of daily living.55-57
Interestingly, the study also showed that in patients with neglect, the association between somatosensory and unimanual and bimanual motor outcome is moderate to strong, compared with only low to moderate in the non neglect group, with significant between-group differences for stereognosis and pressure perception. These findings may be important when delineating rehabilitation strategies because patients with neglect might benefit from other types of treatment. Somatosensory function was shown to be equally associated with both unimanual and bimanual motor performance. Finally, stereognosis was shown to have the strongest association with motor function. This last finding is in accordance with results of a study by Connell et al, 6 where upper-limb performance was found to be a significant predictor of stereognosis impairment. This correlation is not surprising because the recognition of objects relies on manual exploration to derive meaningful knowledge about the characteristics of the object. Assistance to manipulate the objects in the hand is given by the assessor; however, it remains unclear whether patients derive the necessary perceptions by this method. Future studies are needed to gain insights into the validity of the stereognosis assessment in patients with severe hand paresis.
The strength of the current study is that it included the use of a combination of reliable and valid assessment methods for different somatosensory modalities of exteroceptive, proprioceptive, and higher cortical functioning in a large cohort of subacute stroke patients. Furthermore, besides the pure clinical assessment methods, an increased objective measure to assess the exteroceptive function was included—namely, the PTT. 32 PTT measures the threshold of light touch in a more sensitive way by using high-frequency TENS, which activates cutaneous receptors of light touch and their accompanying large myelinated Aβ fibers. 32 The clinical score of light touch and the PTT scores were significantly correlated (r = −0.63), but our results suggest that the PTT assessment was able to identify more light-touch deficits. This might have contributed to the finding that correlations between PTT and motor performance were the same for patients with and without visuospatial neglect. This highlights the potential of PTT as a measure of exteroceptive function in patients poststroke, both for research purposes and the clinical setting.
Some limitations of the study need to be recognized. First, patients were assessed in different settings: 84% of our patients were assessed in 7 different rehabilitation centers, and 16% were assessed at home but were still enrolled in outpatient physical therapy. Recruitment of patients was not performed consecutively but was conducted in the different rehabilitation centers, upon eligibility on predefined assessment days. A flowchart cannot be provided because there are no data available on patients who were ineligible for participation in the study. The specific content and frequency of the treatment were not documented, and therefore, we were not able to control for treatment provided. Second, detailed information on localization and extent of the lesion would have been useful in exploring the shared neuroanatomy between brain areas responsible for the outcomes of the study. Third, measurement of visuospatial neglect with solely the SCT might be seen as limited to assess this complex phenomenon. Yet the emphasis of this study was on the somatosensory and motor functioning, with visuospatial neglect as an influencing factor. Future research is necessary to replicate these findings with a more extended test battery for personal and extra-personal neglect, using a combination of different paper-and-pencil tests as well as behavioral assessment such as the Catherine Bergego Scale to assess neglect in daily activities. 57 Furthermore, we were not able to control for hemianopia as a confounding factor during the assessment of neglect, which could have influenced the results of the SCT because of a possible interfering visual impairment. Finally, subacute patients were assessed between 12 days and 6 months after stroke, which covers a broad time window for inclusion of the patients. Of our sample of 122 patients, 57% were in the early subacute phase (up to 3 months poststroke) and 43% in the late subacute phase (between 3 and 6 months poststroke). Because these groups were not comparable based on the different demographic and clinical characteristics, between-group analyses were not indicated. Future studies should report on repeated assessments at fixed time points.
Conclusions
The novel findings from this large cross-sectional study are that somatosensory deficits are frequently seen in the subacute phase poststroke and are related to motor outcome. The presence of visuospatial neglect is associated with the presence and severity of somatosensory deficits. Second, in patients with neglect, somatosensory impairments have a stronger association with motor impairments when compared with patients without neglect. Therefore, recommendation for practice includes the screening of visuospatial neglect from the early stage poststroke. This might imply that patients with neglect need different intervention strategies for sensorimotor rehabilitation. Furthermore, because this study showed that somatosensory deficits are common after stroke, we suggest the clinical use of reliable and valid measures of somatosensory deficits. Additionally, quantitative measures such as the PTT can be helpful in clinical practice.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: They received financial support from the Promobilia Foundation, Sweden (research grant number 15060) and from the Foundation Van Goethem-Brichant, Belgium.
