Abstract
Background. The pathophysiology of adductor spasmodic dysphonia (AdSD), like other focal dystonias, is largely unknown. Objective. The purposes of this study were to determine (a) cortical excitability differences between AdSD, muscle tension dysphonia (MTD), and healthy controls; (b) distribution of potential differences in cranial or skeletal muscle; and (c) if cortical excitability measures assist in the differential diagnosis of AdSD and MTD. Methods. Ten participants with adductor spasmodic dysphonia, 8 with muscle tension dysphonia, and 10 healthy controls received single and paired pulse transcranial magnetic stimulation (TMS) to the primary motor cortex contralateral to tested muscles, first dorsal interosseus (FDI), and masseter. We tested the hypothesis that cortical excitability measures in AdSD would be significantly different from those in MTD and healthy controls. In addition, we hypothesized that there would be a correlation between cortical excitability measures and clinical voice severity in AdSD. Results. Cortical silent period duration in masseter and FDI was significantly shorter in AdSD than MTD and healthy controls. Other measures failed to demonstrate differences. Conclusion. There are differences in cortical excitability between AdSD, MTD, and healthy controls. These differences in the cortical measure of both the FDI and masseter muscles in AdSD suggest widespread dysfunction of the GABAB mechanism may be a pathophysiologic feature of AdSD, similar to other forms of focal dystonia. Further exploration of the use of TMS to assist in the differential diagnosis of AdSD and MTD is warranted.
Keywords
Introduction
Adductor spasmodic dysphonia (AdSD) is a neurologically based movement disorder of the laryngeal musculature resulting in a strained, strangled voice quality primarily during speech tasks. 1 AdSD can have a sudden or gradual onset and typically progresses over time leaving those who are afflicted unable to effectively communicate. The effects of AdSD can be devastating to an individual’s identity, occupation, and social engagement.
Results from electromyography (EMG) studies have revealed abnormal, task-specific involuntary movements in AdSD, consistent with other forms of focal dystonia. The pathophysiology of AdSD, however, is largely unknown and hence little advancement has been made in diagnosis or treatment of the disorder. Accurate diagnosis of AdSD is challenging due to similar perceptual features as muscle tension dysphonia (MTD). MTD is thought to be a functional voice disorder characterized by hyperfunction of laryngeal muscles resulting in a strained voice quality similar to AdSD, but a different etiology. There have been reports of patients exhibiting both AdSD and MTD. Past research has explored methods and reported recommendations for differential diagnosis, but there continues to be no gold standard to discriminate between these 2 disorders.2-4 Differential diagnosis is imperative since treatment of these 2 disorders is vastly different. Whereas MTD can be effectively treated with behavioral voice therapy, symptoms of AdSD are not responsive to behavioral voice therapy and are most often treated with injections of botulinum toxin into the thyroarytenoid muscle. Often, a diagnosis of AdSD or MTD can only be confirmed based on the response to treatment. Comparison of neurophysiologic measures such as cortical excitability, offers a novel approach in differential diagnosis which could lead to more effective, efficient treatment of AdSD. A direct comparison of cortical excitability in AdSD and MTD has not previously been reported.
Transcranial magnetic stimulation (TMS) is a noninvasive method of stimulating the cortex to assess cortical excitability and has been used to further advance the understanding of the pathophysiology of other forms of focal dystonia. Past TMS research has revealed reduced cortical inhibition in focal dystonia as measured by differences in short-interval intracortical inhibition (SICI) and shortened cortical silent period (CSP) duration. There have been variable findings in SICI differences in focal hand dystonia.5-8 However, shortened CSP duration has been consistently reported in the region that is responsible for the affected muscle(s) in focal hand dystonia,9-16 cervical dystonia,17,18 blepharospasm,18,19 and oromandibular dystonia. 19 These findings suggest dysfunction of inhibitory interneurons and GABA-ergic mechanisms within the motor cortex may be a pathophysiological feature of focal dystonia. Although the term focal suggests that these cortical excitability differences can be localized to one specific region in the motor cortex, that is, those associated with affected muscles; evidence suggests differences in cortical excitability may be more widespread throughout the primary motor cortex in focal dystonia. Decreased intracortical inhibition, represented by shortened CSP has been reported in unaffected cranial muscles in patients with cranial dystonias such as perioral muscles in blepharospasm18,19 and orbicularis oculi in oromandibular dystonia. 19 In addition, shortened CSP duration has also been reported in cortical hand representation in patients with blepharospasm, 16 cranial dystonia, 20 cervical dystonia, 20 and AdSD 15 without evidence of hand symptoms, suggesting a more generalized disturbance of intracortical inhibition in focal dystonia.
There has been limited assessment of either focal or widespread cortical inhibition in AdSD. The purposes of this study were to (a) compare cortical excitability in AdSD, MTD, and healthy controls; (b) determine if differences in cortical excitability were widespread in the motor cortex, by assessing responses in both cortical spinal and corticobulbar tract muscles; and (c) assess the relationship of excitability measures with perceptual voice assessment. We hypothesized that significant impairment in cortical excitability in both the cortical spinal and corticobulbar tract musculature would be found in AdSD with no differences between MTD and healthy. We also hypothesized that cortical excitability measures, particularly the CSP would correlate with the perceptual voice assessment.
Methods
An a priori power analysis was conducted based on data from previous work comparing cortical excitability as measured by CSP in healthy subjects and those with focal hand dystonia. 13 True difference between the means = 28, Sigma 1 = 22, Sigma 2 = 20.47 with 80% power and an α level of .05 revealed a sample size of 10 subjects per group would be needed to identify a large effect (d = .8). Participants were recruited through the Lion’s Voice Clinic at the University of Minnesota. Each potential participant had been evaluated and diagnosed by an experienced speech-language pathologist and otolaryngologist. Evaluation included a perceptual voice assessment and videostroboscopy. Screening questions were created based on past reports of differential diagnosis of AdSD and MTD4,21 (see the appendix). Exclusionary criteria included: vocal fold pathology, essential tremor, unspecified vocal tremor, neurological condition (other than dystonia), focal hand dystonia or orthopedic hand or wrist dysfunction, denervation surgery and/or chronic gastroesophageal reflux disease. If the participant received botulinum toxin, the last injection must have been ≥3 months prior to participation in the study. Participants in all groups were screened for TMS safety according to published standards including, no history of seizures, other neurologic conditions, metal implanted devices (excluding dental fillings) and pregnancy. 22 One participant (No. 14) had recently been diagnosed by the speech-language pathologist as having AdSD with a possibility of overlying MTD. However, given the participant’s responses to the screening questions, he was placed in the AdSD group.
Participants
Twenty-eight right-handed participants aged 18 to 66 years were enrolled in the study: AdSD (n = 10, mean age 55.62 ± 6.78 years, mean symptom duration 154.5 ± 125.10 months); MTD (n = 8, mean age 52.5 ± 13.84 years, mean symptom duration 53.25 ± 84.75 months) (Table 1); and age- and gender-matched healthy controls (n = 10, mean age 55.37 ± 6.67 years). All participants gave written, informed consent according to the Declaration of Helsinki prior to participation. The study was approved by the University of Minnesota Clinical Translational Science Institute and Institutional Review Board.
Subject Demographic Information for Subjects in the MTD and AdSD Groups.
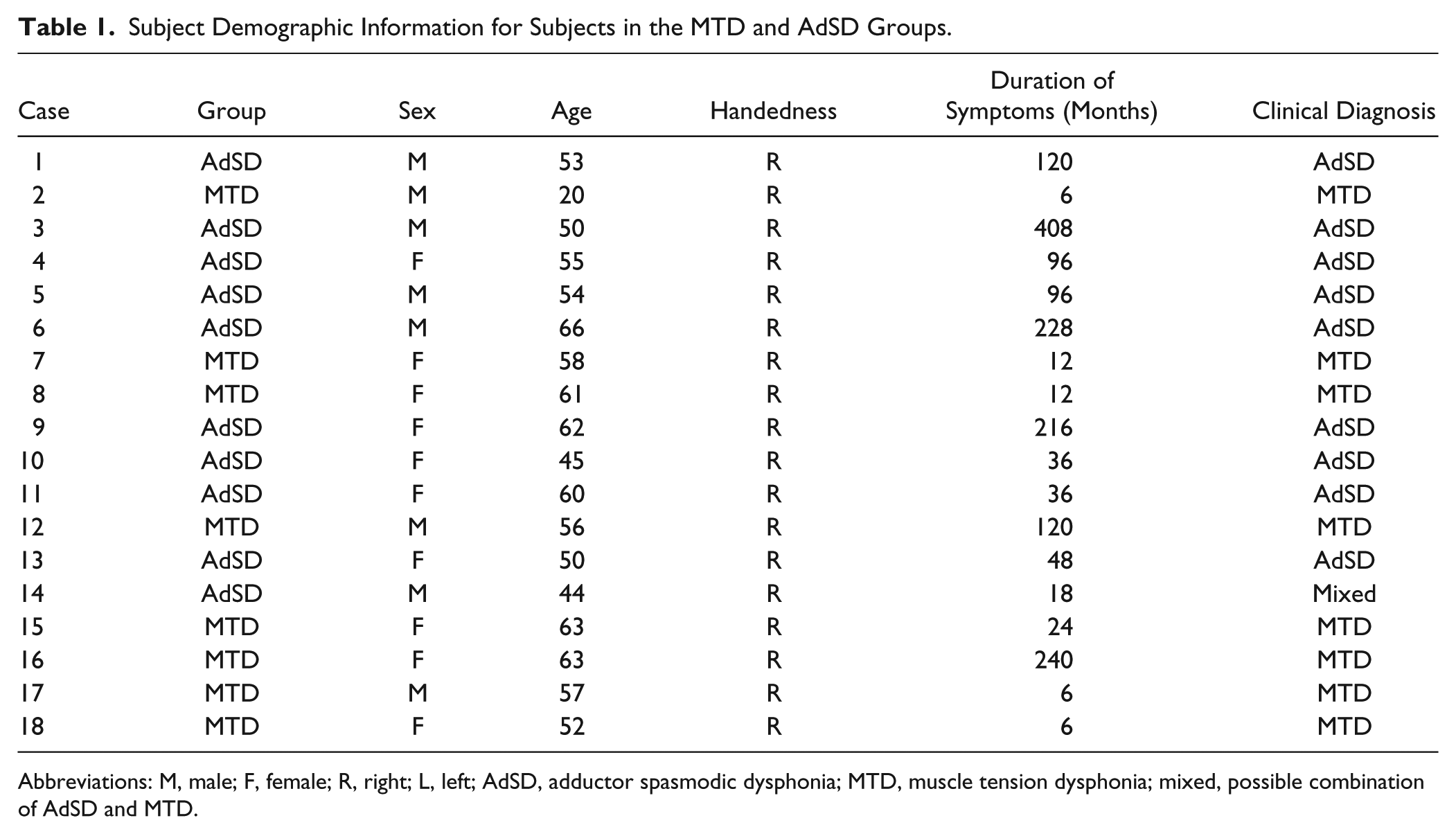
Abbreviations: M, male; F, female; R, right; L, left; AdSD, adductor spasmodic dysphonia; MTD, muscle tension dysphonia; mixed, possible combination of AdSD and MTD.
Clinical Assessment
Each participant was video recorded while being given the Consensus of Auditory Perceptual Evaluation of Voice (CAPE-V) 23 prior to the presentation of TMS. The voice sample included sustained vowels /a/ and /i/, sentence repetition and conversational speech. In addition, each participant repeated a list of 20 adductor phoneme-loaded sentences. 4 The CAPE-V and adductor sentences were assessed by an expert listener, blinded to the participant’s diagnosis. All participants in the AdSD and MTD groups completed the Voice Handicap Index (VHI) to measure of the magnitude of the voice disorder on the participant’s quality of life.
Transcranial Magnetic Stimulation
The TMS stimulus was presented to the left primary motor cortex in all participants. Electromyographic (EMG) traces from masseter (to assess corticobulbar tract) and first dorsal interosseus (FDI) (to assess corticospinal) muscles were acquired using a bandpass filter width of 20 to 2000 Hz (Cadwell Laboratories, Kennewick, Washington). Each participant was seated comfortably in a reclining chair and silver chloride disc electrodes were affixed over the right masseter and right FDI using a belly/tendon montage. The participant was fit with a swim cap to allow cranial landmarks to be first approximated and later confirmed using a 70-mm figure of eight TMS coil (Magstim Co Ltd, Whitland, UK). The optimal location and orientation for the hand region was near the hypotenuse of the markings at 5 cm lateral and 5 cm anterior to the vertex with a 45° posterolateral coil orientation. 13 Optimal masseter motor-evoked potential (MEP) responses were elicited when the coil was approximately 4 to 5 cm lateral to the vertex with an 80° to 100° anterolateral coil orientation.24-26 Resting motor threshold (RMT) and 1-mV threshold for FDI and active motor threshold (AMT) and 0.3-mV threshold for masseter were then determined. Motor thresholds were defined as the lowest stimulus intensity needed to elicit reproducible MEPs of ~50 µV in a resting muscle in 50% of trials (RMT) and ~100 to 200 µV in a slightly contracted muscle in 50% of trials (AMT).27,28 Four measures of cortical excitability were collected: silent period (CSP), short-interval intracortical inhibition (SICI), intracortical facilitation (ICF), and stimulus response curve (SR curve). The FDI was at rest for all measures except CSP and the masseter was in slight isometric contraction for all measures.13,29-31
Cortical Silent Period
The CSP is a measure of intracortical inhibition reflective of GABAB mechanisms. It is a measure of the quiescence when a single pulse, suprathreshold stimulus is delivered during an active isometric contraction.27,28 Ten CSP recordings, with a 15- to 20-second rest interval between each trial, were collected while the participant sustained ~25% of maximum voluntary contraction (FDI) and ~10% of maximum voluntary contraction (masseter). In FDI testing, the average of the 3 maximum contractions was used to calculate 25% of maximal volitional contraction and the participant was directed to contract and sustain this effort to meet the target amplitude provided with visual feedback on a screen situated in front of the participant. In masseter testing, participants used a tongue depressor in a transverse plane (bilateral bite) to perform a contraction. Each participant was asked to bite at maximum force and asked to self-rate the effort required. Then, they were asked to contract and maintain ~10% of that force during the CSP testing. Instructions were “lightly hold this in your teeth, just so I could not pull it easily out.” The CSP onset was defined as the TMS-induced MEP, the offset was identified as the point at which the muscle contraction returned to 50% of the prestimulus average, for FDI 29 and the prestimulus average, for masseter. In masseter, the higher threshold was required due to higher variability of the prestimulus masseter EMG. In masseter, a total of 25 traces (4 from healthy, 13 from AdSD, and 8 from MTD) were considered uninterpretable and excluded from analysis. In FDI, a total of 3 traces were determined to be uninterpretable and excluded from analysis (1 from healthy and 2 from MTD).
Paired Pulse (SICI and ICF)
The SICI is a measure of intracortical inhibition, reflective of the integrity of the GABAA mechanism and is represented by a suppression of a test MEP by a subthreshold condition stimulus 1- to 5-ms earlier.32,33 The ICF is considered to be a test of intracortical facilitation and is demonstrated by facilitation of a test MEP by a subthreshold condition stimulus 10 to 15 ms earlier.27,28 Twenty paired pulse stimuli (10 SICI and 10 ICF) interspersed with single pulse stimuli were presented in a predetermined random fashion while the participant was at rest for FDI and during slight isometric contraction for masseter. The conditioning pulse was set at 80% of RMT (FDI) and AMT (masseter) followed by an interstimulus interval of 3 ms (SICI) and 10 ms (ICF) and test pulse. The ICF and SICI are presented in a ratio, whereby the average peak-to-peak amplitude for the paired pulse stimulus was divided by the average peak-to-peak MEP amplitude of the single pulse stimulus. Calculated responses <1.0 is evidence of inhibition and >1.0, evidence of facilitation.
Stimulus Response Curve
The slope of the stimulus response curve and area under the curve are general measures of cortical excitability. In healthy subjects, the amplitude of the MEP increases as the stimulation intensity increases.27,28 Eight single pulses of each stimulus intensity 110%, 120%, 130%, and 140% of RMT (FDI) and AMT (masseter) were presented in a predetermined random fashion with an interpulse interval between 5 and 10 seconds. MEP responses for the SR curve protocol were analyzed by calculating the average peak-to-peak amplitude for each trial for each stimulus intensity, for each participant. Individual SR curves were plotted for each participant for visual inspection and a mean SR curve for masseter and FDI was plotted for each group. Regression slopes and areas under the curve were then calculated for each muscle in each participant.
Statistical Analysis
After normality assessment determined normal distribution, separate 1-way analyses of variance (ANOVA) were used to identify main effects between groups (healthy, MTD, and AdSD). Participant characteristics including age, gender, and symptom duration were assessed to determine if there was a significant main effect (P = .05) to identify potential covariables to be factored in with each dependent variable. Then, analysis of covariance (ANCOVA) or ANOVA was run as appropriate for each dependent variable (CSP, SICI, ICF, SR curve, area under the curve, and motor thresholds) with significance set at P = .05. Post hoc analysis with Bonferonni correction for multiple pairwise comparisons was used as appropriate to determine difference between groups (P = .025). Pearson product moment correlation coefficient was used to measure the correlation between neurophysiologic measures and clinical severity ratings (P = .05).
Results
Motor Thresholds
There were no significant differences between groups in AMT (df = 2, F = 0.06, P = .94) or 0.3-mV threshold (df = 2, F = 0.026, P = .97) in masseter and no significant differences in RMT (df = 2, F = 0.187, P = .83) or 1-mV threshold (df = 2, F = 0.72, P = .49) in FDI.
Cortical Silent Period
A significant age effect was detected in masseter CSP (P < .001) and FDI CSP (P < .001) and a significant symptom duration effect was detected in FDI (P < .001). As a result, an ANCOVA was conducted with age (masseter and FDI) and symptom duration (FDI) as covariates. Results revealed a significant group effect in both masseter (df = 2, F = 9.92, P < .001) and FDI (df = 2, F = 33.35, P < .001). A post hoc pairwise comparison revealed that participants with AdSD had significantly shorter CSP duration in masseter than participants with MTD (P < .001) or healthy (P = .004). There were no significant differences in masseter CSP duration between healthy and MTD (Figures 1 and 2). In addition, the participants with AdSD also had significantly shorter CSP duration in FDI than participants with MTD (P < .001) or healthy (P < .001). However, the CSP duration in FDI was significantly shorter in MTD compared with healthy (P < .001) (Figures 1 and 3).
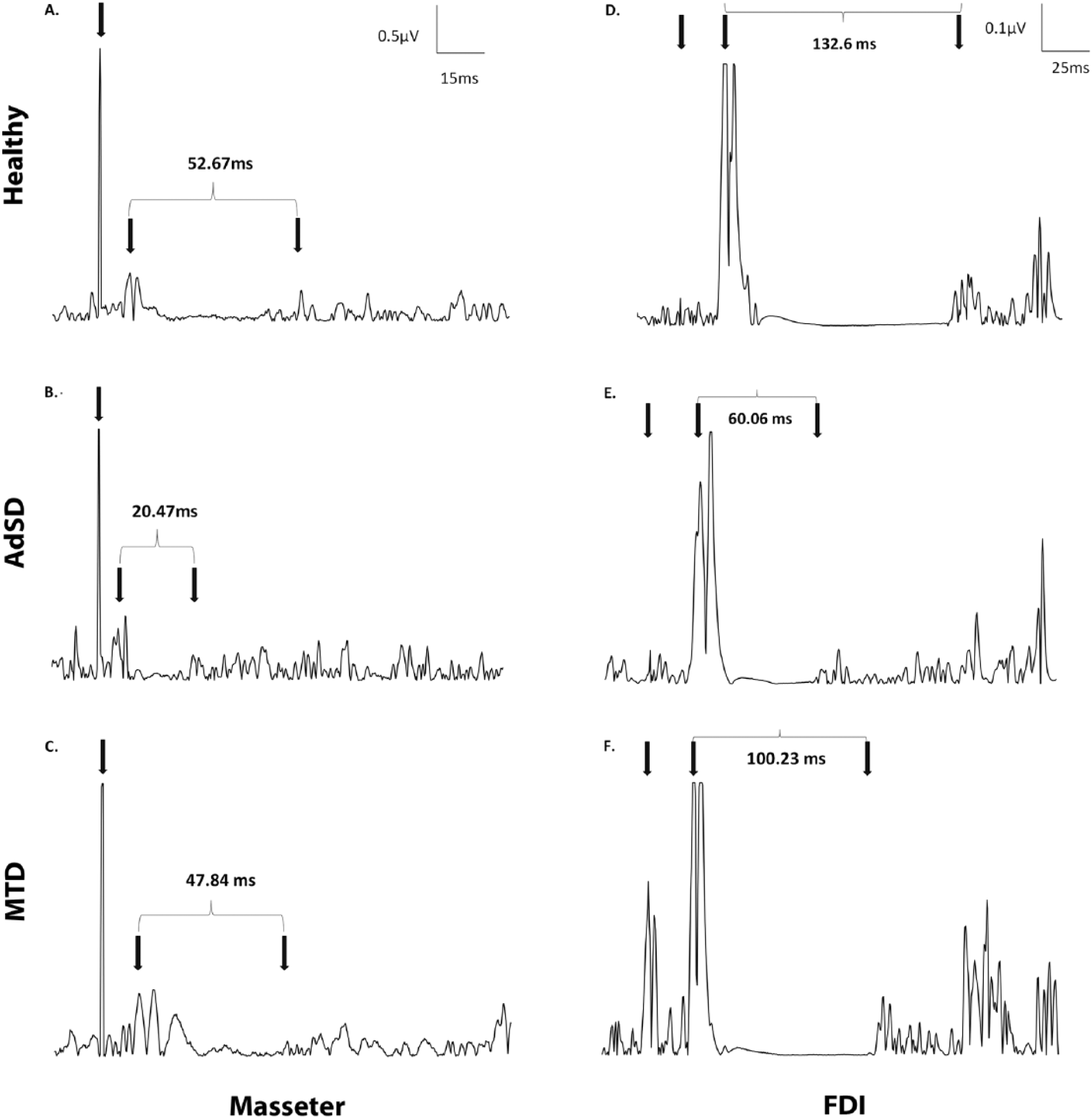
Full wave rectified electromyographic traces of cortical silent period duration in masseter (left) and first dorsal interosseous (FDI; right) from individual subjects: Healthy (A and D), adductor spasmodic dysphonia (AdSD; B and E) and muscle tension dysphonia (MTD; C and F).
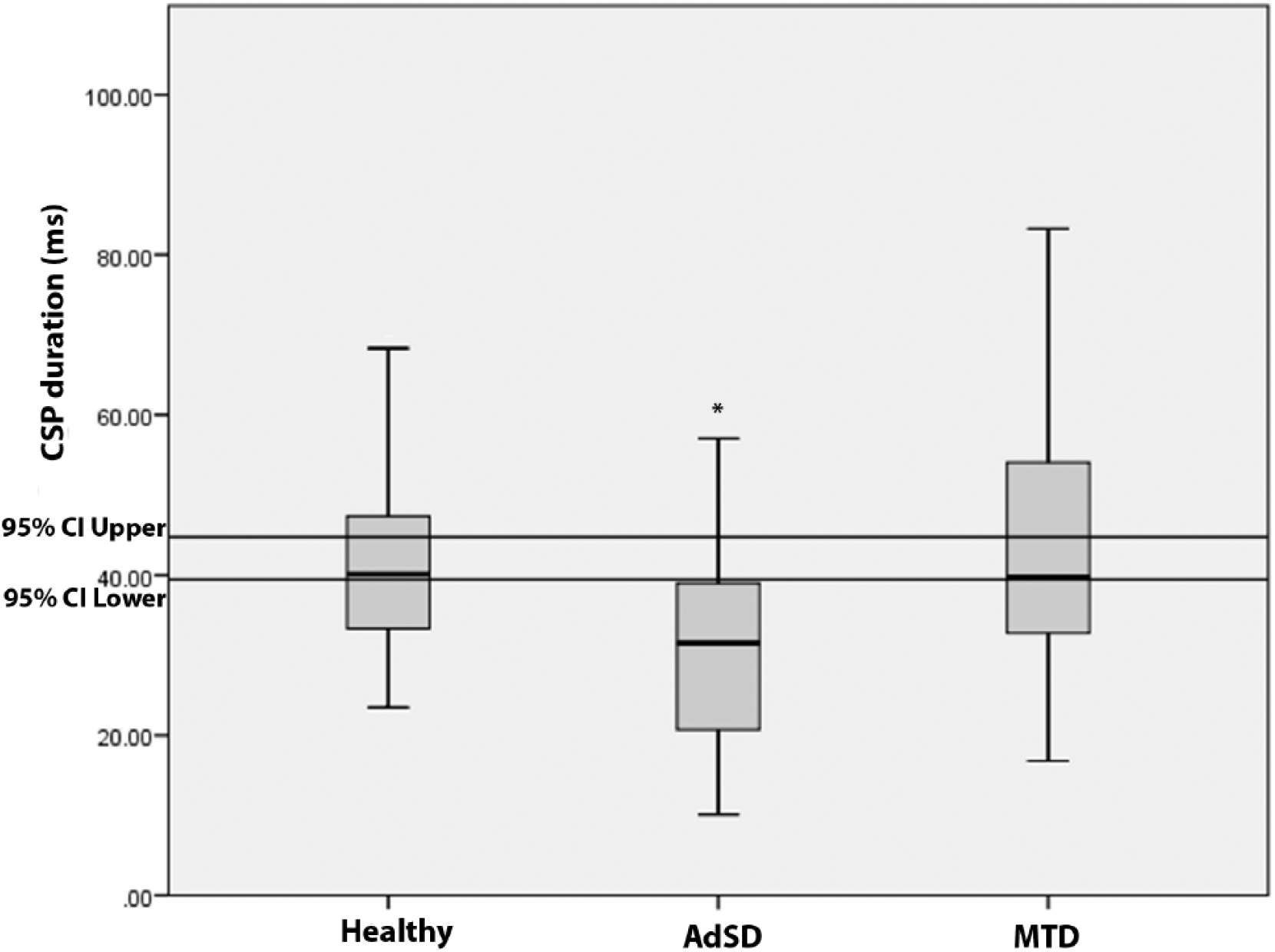
Mean cortical silent period (CSP) duration in masseter across groups. 95% confidence intervals represent healthy controls.
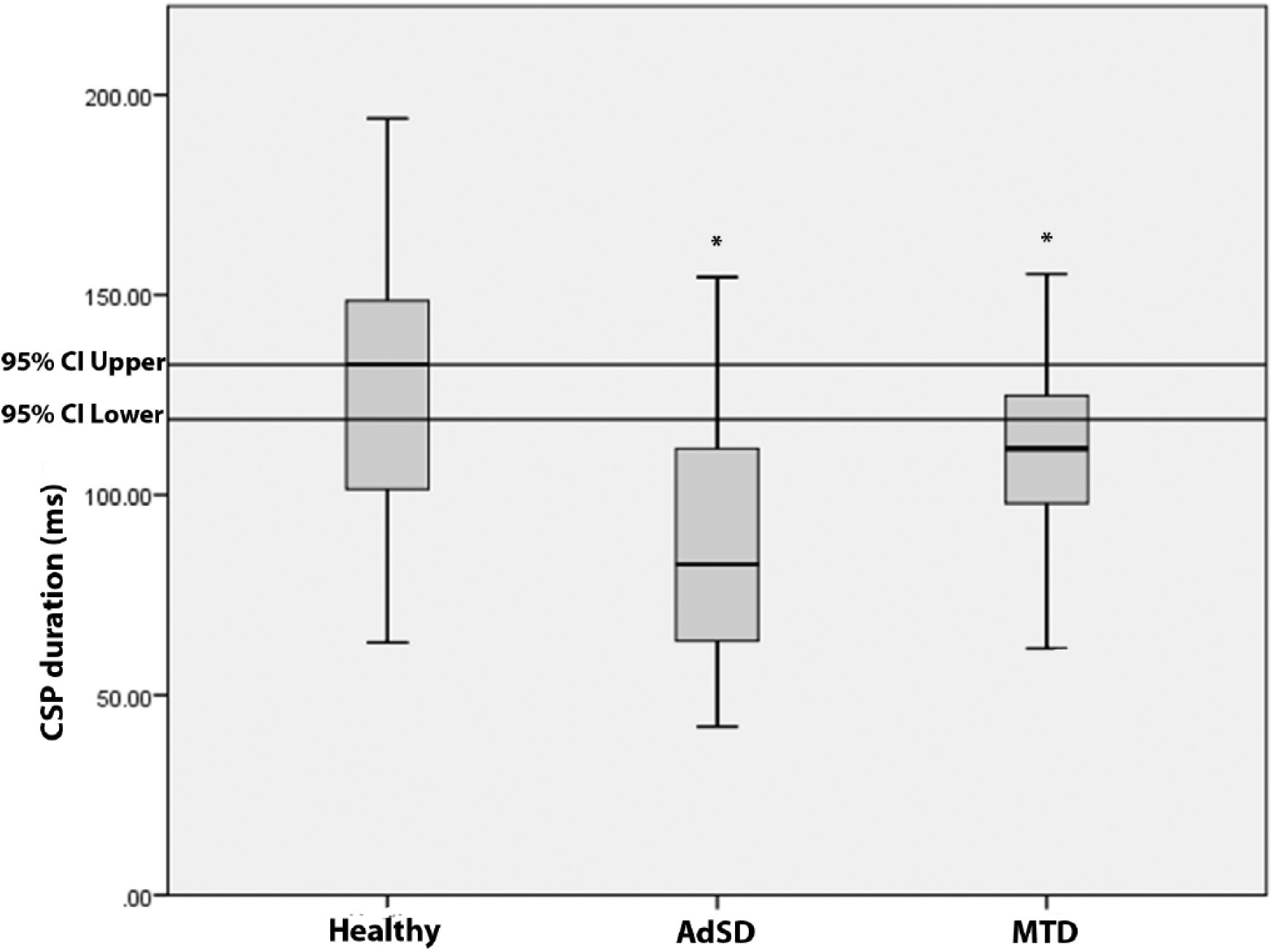
Mean cortical silent period (CSP) duration in first dorsal interosseous across groups. 95% confidence interval based on healthy controls.
Paired Pulse (SICI and ICF)
There were no significant differences in SICI between groups in both masseter (df = 2, F = 0.195, P = .824) and FDI (df = 2, F = 0.859, P = .436). The mean SICI ratios for masseter were >1 across groups indicating no inhibitory effect was observed in the masseter muscle. The mean FDI SICI ratios were <1 across groups indicating an inhibitory effect was observed in each group with both AdSD and MTD demonstrating less inhibition than healthy controls but this difference did not reach significance (Table 2). ANOVA revealed no significant differences in ICF between groups in masseter (df = 2, F = 0.310, P = .736) or in FDI (df = 2, F = .242, P = .0787). Mean ICF ratios were facilitory (>1) across all groups in masseter and FDI (Table 2).
Descriptive Statistics Presented as Mean ± SD (95% CI) for SICI, ICF, and SR Curve Across Groups.
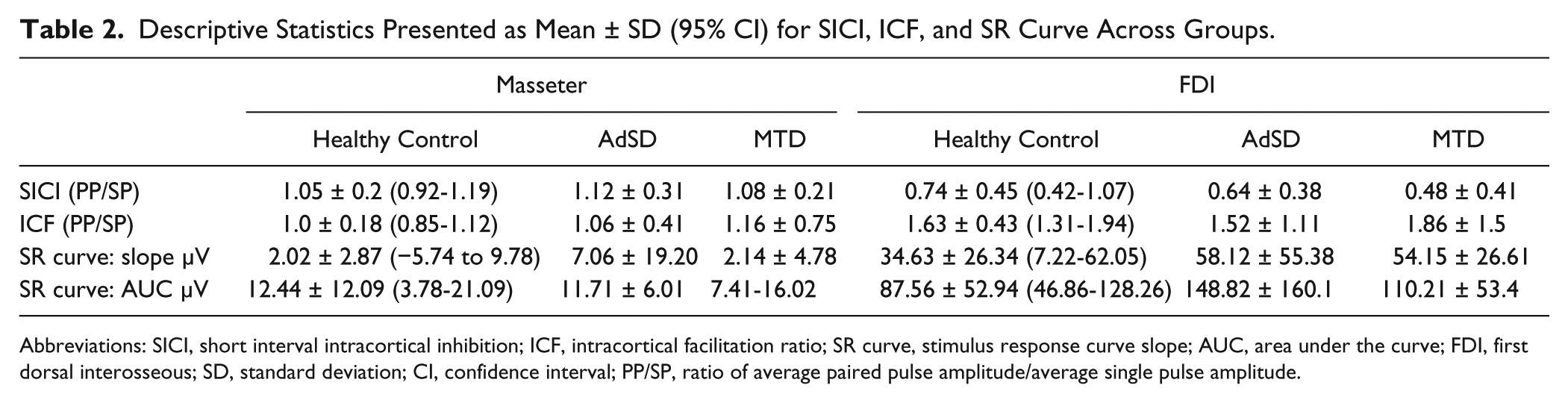
Abbreviations: SICI, short interval intracortical inhibition; ICF, intracortical facilitation ratio; SR curve, stimulus response curve slope; AUC, area under the curve; FDI, first dorsal interosseous; SD, standard deviation; CI, confidence interval; PP/SP, ratio of average paired pulse amplitude/average single pulse amplitude.
Stimulus Response Curve
One-way ANOVA revealed no significant differences in slope between groups for masseter (df = 2, F = 0.539, P = .590) or FDI (df = 2, F = 0.913, P = .415) (Table 2); nor did it reveal significant differences for area under the curve in masseter (df = 2, F = 0.142, P = .869) or FDI (df = 2, F = 0.803, P = .460) (Table 2).
Clinical Assessment
Although a correlation analysis revealed a negative relationship between CSP and CAPE-V, the correlation was weak in strength and did not reach significance in masseter (r = −0.24, P = .35) and FDI (r = −0.23, P = .34). Additionally, none of the cortical excitability measures revealed significant correlations with CAPE-V subtests or total scores. Significant correlations were found between FDI RMT and CAPE-V total scores (r = −0.552, P = .05) and masseter AMT and CAPE-V total scores (r = −0.583, P = .037). This suggests that as the severity of the voice disorder increased, the motor threshold for masseter and FDI decreased. A comparison between AdSD and MTD across CAPE-V subtests revealed no significant differences between groups: breathy (df = 11, F = 0.323, P = .581); rough (df = 11, F = 0.020, P = .890); strain (df = 11, F = 2.403, P = .149); pitch (df = 11, F = 0.006, P = .939); loudness (df = 11, F = 1.146, P = .307); and total CAPE-V score (df = 11, F = 0.902, P = .363) (Table 3). These findings further support that there are similar perceptual features in AdSD and MTD. The number of voice breaks on the adductor phoneme sentence list were calculated and a between group comparison revealed AdSD had a significantly higher number of voice breaks than MTD (df = 17, F = 7.44, P = .015). However, there were no significant correlations between number of voice breaks and CSP duration in AdSD for masseter (r = −0.170, P = .64) or FDI (r = 0.50, P = .41) or MTD for masseter (r = −0.03, P = .94) or FDI (r = −0.60, P = .11) (Table 3).
Descriptive Statistics for CAPE-V Subtests, VHI Total Score, and Number of Voice Breaks During Adductor Sentence Reading.
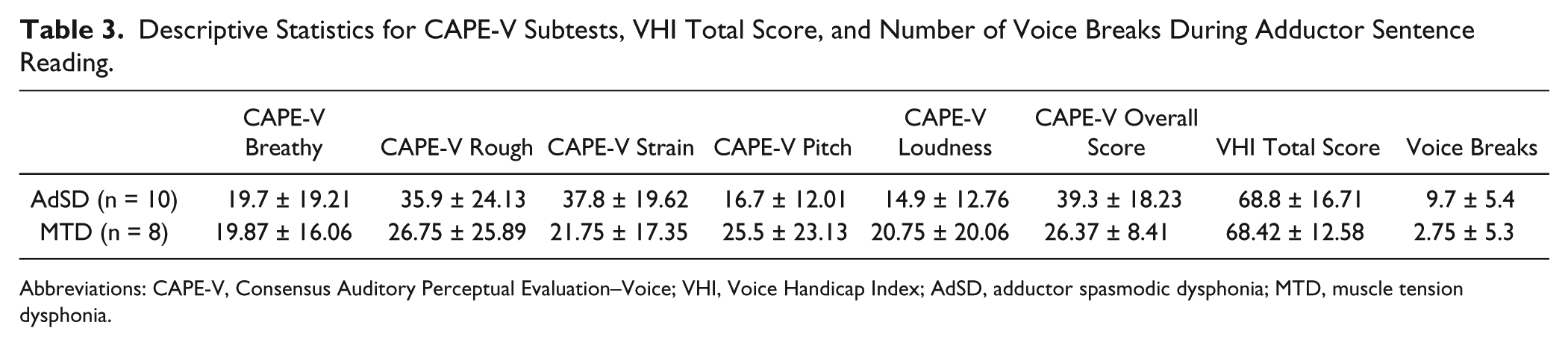

Abbreviations: CAPE-V, Consensus Auditory Perceptual Evaluation–Voice; VHI, Voice Handicap Index; AdSD, adductor spasmodic dysphonia; MTD, muscle tension dysphonia.
Adverse Effects
Two participants reported slight headache during the TMS procedure. The band of the swim cap appeared tight and was cut and the headache subsided. One participant reported a mild headache after the experiment, lasting approximately 2 hours. No other adverse effects were reported.
Discussion
The primary findings of this study revealed individuals with AdSD demonstrated a significantly shorter CSP in both masseter and FDI than the healthy and MTD groups supporting our hypothesis of an impaired intracortical inhibitory mechanism that is not isolated to a focal cortical region or one descending motor system. To the best of our knowledge, this is the first reporting of a potential pathophysiologic marker for AdSD. Contrary to our hypothesis, differences were also found in CSP duration in FDI between MTD and healthy. No other TMS measure revealed differences between groups in either muscle. The finding of shortened CSP duration in AdSD in unaffected muscles is supported by research in other forms of dystonia that have also demonstrated increased cortical excitability in regions responsible for muscles that did and did not have dystonic symptoms.15,18,20
Inhibition and GABA
In the corticospinal system, the CSP can be explained using a segmental level rationale. The initial portion of the CSP is thought to be due to suppression of H-reflexes, due to Renshaw inhibition which is a spinal mechanism.34,35 The latter portion of CSP is thought to be due to suppression of voluntary motor drive by GABAB receptor–mediated inhibition in the cortex. 36 Unlike the spinal motor system, the trigeminal system of the corticobulbar tract has neither Renshaw cells nor axon collaterals to account for the silent period. However, past reports have concluded the CSP in the trigeminal motor system also appears to be segmental, similar to the spinal motor system, with brainstem and cortex accounting for the CSP.25,37-40 The mechanisms that influence CSP in masseter appear to be similar to those in limb muscle; CSP is sensitive to changes to stimulus intensity and coil orientation but not the amount of volitional contraction; providing further evidence that CSP is a cortical phenomenon35,37 and potentially explaining the variability in CSP values across past studies.25,37-39 Masseter CSP duration in healthy individuals in this study was similar to that found by Ortu et al. 25 The duration of CSP reflects postsynaptic GABA-mediated inhibition and is considered a viable method for investigating intracortical inhibition in cranial muscles in health and disease. A shortened CSP indicates a dysfunction in the inhibitory mechanisms, in essence “too little” inhibition. A reduction of CSP duration has been reported in patients with focal dystonia suggesting abnormal GABAergic mechanisms, specifically GABAB receptors, to be a physiologic feature of focal dystonia.11,13,14,17,19,41 The results reported here and other work provide evidence of widespread dysfunction of cortical inhibition suggesting diffuse dysfunction of GABAB mechanisms in dystonia, rather than impairment localized to the affected muscle. SICI is also a measure of the GABAergic mechanism, reflecting the function of GABAA receptors. In some studies, abnormal SICI has been reported in focal hand dystonia6,7 but not in others.5,8 Findings from the current study revealed no inhibitory effect to SICI in the masseter across groups, which may have been influenced by the lack of standardization of muscle contraction during the recording. 30 Although SICI ratios revealed inhibition across groups, there were no significant differences in the amount of inhibition between groups, which may suggest a pathophysiological feature of AdSD is abnormal GABAB-mediated interneurons and not GABAA-mediated interneurons. However, this should be further explored. No differences in ICF across groups found in this study support past findings in dystonia 12 and provide further evidence that deficient GABAergic mechanisms may contribute to AdSD. Reports of the differences in GABA levels within the sensorimotor cortex in focal hand dystonia are conflicting with Levy and Hallett 42 reporting reduced GABA levels and Herath et al 43 reporting no differences in GABA levels in the sensorimtor cortex between patients with focal hand dystonia and controls. Animal research has reported high concentrations of extracellular GABA over an extended period of time influenced inhibitory postsynaptic potentials but did not alter the number of GABA interneurons, receptors or synapses.44,45 Relatedly, the use of GABA antagonist in primates resulted in dystonic-like movements. 46 These findings suggest abnormal GABA concentration levels influence neuroplasticity by altering the inhibitory postsynaptic potential that is reflected in altered CSP duration. Considering aberrant neuroplasticity has been implicated in focal dystonia,20,47 it is feasible to conclude abnormalities in GABAergic mechanisms may play a role in dystonia. Studies have attempted to associate other physiologic findings, such as impaired surround inhibition, with the GABAergic mechanism, but it has been determined that the CSP duration is not related to this phenomenon. 47
Evidence from human pharmacology literature have provided information regarding CSP and GABA receptors that can be used to further our understanding of GABAergic mechanisms in dystonia. Pharmacological GABA reuptake inhibitors or degrading enzymes have been shown to lengthen CSP duration in healthy adults.48,49 There have been few investigations, with variable results, in the use of baclofen, a GABA agonist drug, in dystonia. Some have reported an increase in CSP duration while others have found no effect.50-53 Clozapine, a GABA receptor antagonist, has also reportedly reduced symptoms of oromandibular dystonia and laryngeal dystonia in single case reports.54,55 Because of the limited randomized, controlled trials of the effectiveness of GABA modifying drugs in the treatment of focal dystonia and the inconsistent and unpredictable outcomes, GABA modifying drugs have not been adopted into routine clinical practice.56-58
Neuroimaging
A complimentary tool to TMS in the investigation of the neurophysiology in dystonia is neuroimaging. Differences in cortical and subcortical activation have been identified in focal dystonia; however, there are discrepancies regarding the pattern of these differences (for review, see Zoons et al 59 ). While many studies have reported increased activation of the sensorimotor cortex during symptomatic tasks in focal hand dystonia59,60 and AdSD61,62 suggesting loss of inhibition, reduced activation has also been reported.59,61,63 Although it is counterintuitive, a reduction in activation may actually be observed in people with impaired inhibition due to maladaptive plasticity. That is to say, overuse may cause the cortical map to expand, resulting in reduced intensity of activation due to larger spread. The CSP findings of this study and past evidence of increased activation in the primary motor cortex lend support that multifocal intracortical disinhibition maybe a feature of AdSD.
Perceptual Voice Characteristics and Neurophysiologic Correlates
Contrary to our hypothesis, this study revealed no significant correlation between perceptual voice ratings (CAPE-V and voice break analysis) and CSP duration in either muscle suggesting the severity of the voice disorder does not appear to be reflected in the degree of reduced intracortical inhibition in the primary motor cortex. This has also been documented in focal hand dystonia research. 12 Interestingly, age, not CSP duration or handwriting symptom has been identified as the most significant predictor of response to rTMS intervention in focal hand dystonia. 64 This evidence further supports the consideration that neurophysiological measures may be unable to predict symptom severity; therefore, it is imperative to include perceptual/behavioral measures when investigating focal dystonias.
There were limitations to this study that should be considered. The a priori power analysis was conducted using values from past CSP findings in subjects with focal hand dystonia and therefore resulted in the possibility that other cortical excitability variables were underpowered. A strain gage was used to ensure consistent contraction during CSP recording in FDI, but not in masseter. A bite force load cell was piloted in the early stages of study design, but it required unilateral biting which has been associated with reduced excitability of corticobulbar neurons in the contralateral primary motor cortex 65 and was thus abandoned. We have diminished concern that this was a problem because CSP duration in masseter is not influenced by the amount of muscle contraction, but rather depends on stimulus intensity and coil orientation.25,37 However, not maintaining a standard muscle contraction in masseter may have affected the SICI response in masseter. A bilateral biting task using a strain gage should be considered for examining cortical excitability in the masseter in the future. 65
Another potential limitation was group assignment of the study participants. This is a circular concern, because lack of definitive diagnosis is a central problem in the disorders and a driving factor for this type of study. The finding of shorter FDI CSP duration in MTD compared to healthy controls was contrary to our hypothesis. This finding may have been a result of a mixed diagnosis (AdSD and MTD) or incorrect diagnosis in one or more of the participants in the MTD group. However, this risk was minimized through careful screening of each participant. Although the screening questions (see the appendix) used included the primary perceptual features used by experienced speech language pathologists and otolaryngologists in differential diagnosis, these two disorders are known to have similar perceptual features and therefore, misassignment was possible. The risk of inaccurate group assignment was further mitigated by follow-up communication with participants in the MTD and AdSD groups. Of the 8 participants in the MTD group, 6 responded to follow-up questioning with 5 reporting good benefit from behavioral voice therapy and 1 reporting fair benefit from behavioral voice therapy. Of the 10 participants in the AdSD group, 7 responded to follow-up questions with 6 reporting continued positive effect from botulinum toxin therapy and 1 participant reporting that she had stopped toxin due to bruising and the stress of the procedure. These participants reported no benefit to behavioral voice therapy. Given these considerations, it is highly likely participants were placed in the appropriate group. However, appropriate diagnosis will continue to be a potential limitation in the study of these two disorders as long as there fails to be definitive diagnostic criteria.
This is the first known study investigating intracortical mechanisms in AdSD using TMS or neurophysiological measures to compare AdSD and MTD. The results support our hypothesis of widespread impaired inhibition in AdSD across both corticobulbar and cortical spinal tracts, reflected in shortened CSP duration in asymptomatic muscles, providing valuable evidence to further elucidate the pathophysiology of AdSD. In addition, these findings suggest CSP duration may be used to assist in the differential diagnosis of AdSD, and provides the foundation for future studies in cortical excitability in this population which may lead to novel treatment protocols that target and facilitate balance in cortical excitability.
Footnotes
Appendix
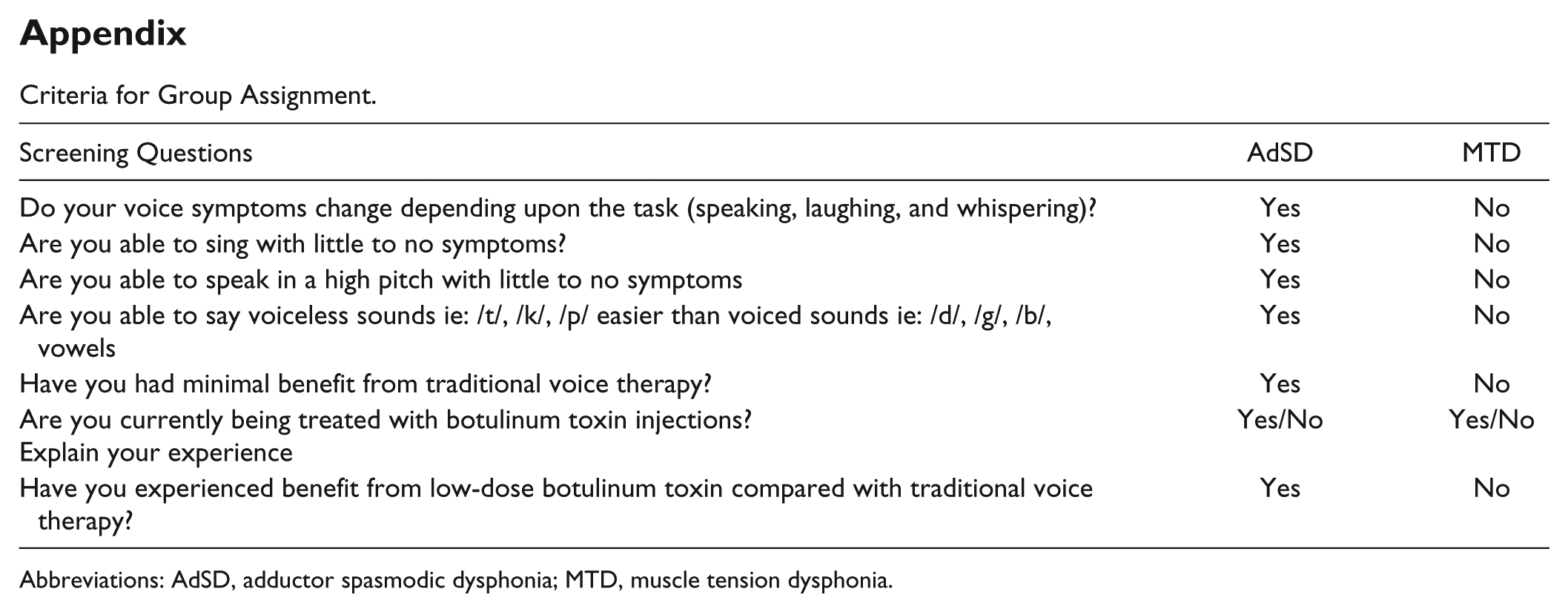
Criteria for Group Assignment.
| Screening Questions | AdSD | MTD |
|---|---|---|
| Do your voice symptoms change depending upon the task (speaking, laughing, and whispering)? | Yes | No |
| Are you able to sing with little to no symptoms? | Yes | No |
| Are you able to speak in a high pitch with little to no symptoms | Yes | No |
| Are you able to say voiceless sounds ie: /t/, /k/, /p/ easier than voiced sounds ie: /d/, /g/, /b/, vowels | Yes | No |
| Have you had minimal benefit from traditional voice therapy? | Yes | No |
| Are you currently being treated with botulinum toxin injections? Explain your experience |
Yes/No | Yes/No |
| Have you experienced benefit from low-dose botulinum toxin compared with traditional voice therapy? | Yes | No |
Abbreviations: AdSD, adductor spasmodic dysphonia; MTD, muscle tension dysphonia.
Acknowledgements
The authors gratefully acknowledge the efforts of George “Shep” Goding, MD, Deirdre Michael, PhD, CCC-SLP, and Lisa Butcher, MS, CCC-SLP.
Authors’ Note
The content of this article is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Research reported in this publication was partially supported by the National Center for Advancing Translational Science of the National Institutes of Health Award Number UL1TR000114 and The American Association of University Women.
