Abstract
Background. Neurorehabilitation studies suggest that manipulation of error signals during practice can stimulate improvement in coordination after stroke. Objective. To test visual display and robotic technology that delivers augmented error signals during training, in participants with stroke. Methods. A total of 26 participants with chronic hemiparesis were trained with haptic (via robot-rendered forces) and graphic (via a virtual environment) distortions to amplify upper-extremity (UE) tracking error. In a randomized crossover design, the intervention was compared with an equivalent amount of practice without error augmentation (EA). Interventions involved three 45-minute sessions per week for 2 weeks, then 1 week of no treatment, and then 2 additional weeks of the alternate treatment. A therapist provided a visual cursor using a tracking device, and participants were instructed to match it with their hand. Haptic and visual EA was used with blinding of participant, therapist, technician-operator, and evaluator. Clinical measures of impairment were obtained at the beginning and end of each 2-week treatment phase as well as at 1 week and at 45 days after the last treatment. Results. Outcomes showed a small, but significant benefit to EA training over simple repetitive practice, with a mean 2-week improvement in Fugl-Meyer UE motor score of 2.08 and Wolf Motor Function Test of timed tasks of 1.48 s. Conclusions. This interactive technology may improve UE motor recovery of stroke-related hemiparesis.
Keywords
Introduction
New technology offers opportunities to hemiparetic stroke survivors who frequently have the potential for recovery long after their course of therapy has ended. 1 Therapy is often terminated because third-party payers incorrectly associate a tendency to plateau in motor recovery with a similar plateau in functional improvement. Emerging interventions include intensive repetitive practice, 2 task-specific training, 3 and interactive robotic technology4-6 to restore upper-extremity (UE) motor ability and function. Although these methods might offer benefits, the wide variety of technology-facilitated interventions need to be clearly evaluated and distinguished from therapist-guided repetitive practice. Recent work studying neuroplasticity during movement control supports methods that leverage the natural adaptive nature of the nervous system. 7 Specifically, the manipulation of error signals during practice appears to stimulate improvement in coordination for individuals with or without a history of stroke. 8 This article also speculated that such learning was implicit through repetition. Although the mechanisms for these improvements are not yet known, we speculate that the nervous system reacts to and learns more from larger errors. 9 Here we implement these ideas in a clinical intervention that uses visual display and robotic technology, which can deliver augmented error signals during training.
Error augmentation (EA) has shown promise because it isolates and enhances movement errors and promotes changes in movement control. 9 This feedback is sometimes counterintuitive and differs greatly from the current standard level of care—seldom does a therapist try to amplify a patient’s mistakes. However, such error-driven learning processes are believed to be central to neuroplasticity and reacquisition of skill in human movement.10,11 Brewer et al 12 used deceptively small visual feedback of force to encourage stroke survivors with persisting motor deficits to push harder than their original capability. Rossetti et al 13 showed a therapeutic benefit using prisms to shift the visual field in stroke survivors with hemispatial neglect. Our group showed improvement in stroke survivors’ movement straightness using training forces that amplified the original errors in movement. 7 Several approaches have also addressed the related idea of elevating resistive forces as long as the participant remains capable of moving.6,14 Whereas this approach can amplify error, resistances did not directly depend on error, as we propose in the present study.
Here we hypothesized that during therapist-directed treatment, EA would lead to greater functional recovery over repetitive practice alone. Individuals with chronic stroke received both standard and EA treatment in a blinded, randomized crossover design.
Methods
Participants
This was a quadruple-blind, crossover design, registered at ClinicalTrials.gov, number NCT01574495. In all, 27 adults with chronic stroke agreed to participate in the study (12 male, age range = 36-88 years, mean age = 57.92 years). Study participants were recruited from a registry of poststroke individuals or from those who contacted the lab with interest in participating as a result of postings in the Chicago area. This study was approved by the Northwestern University Institutional Review Board. All participants provided informed consent according to the Declaration of Helsinki prior to commencing the study. A total of 26 individuals completed all phases of the study, and only 1 participant, who dropped out for reasons that did not pertain to the study, was excluded from analysis (Figure 1). Eligible participants were all adults aged 18 years or more who had suffered a single cortical stroke and were at least 6 months poststroke. Participation also required some recovery of proximal strength in the hemiparetic limb, as confirmed by an UE Fugl-Meyer score of 15 to 50. Exclusion criteria included multiple strokes, bilateral paresis, severe spasticity or contracture, severe concurrent medical problems, severe sensory deficits, cerebellar strokes resulting in severe ataxia, significant shoulder pain, focal tone management with botulinum toxin (Botox) injection to the hemiparetic UE within the previous 4 months, depth perception impairment (<3/9 on Stereo Circle Test), visual field cut, cognitive impairment (Mini Mental State Examination < 23/30), or severe aphasia, affective dysfunction, or hemisensory neglect that would influence the ability to perform the experiment or provide informed consent. Participants were also excluded if they received any other skilled UE rehabilitation in a clinical setting. We discovered that 1 participant (participant 14) received outpatient therapy during his entire enrollment. We included this person in our analysis to rigorously adhere to our randomization procedure for data analysis according to the intention-to-treat approach15,16 and also because of the crossover nature of our design. See Table 1 for participants’ demographics and lesion characteristics.
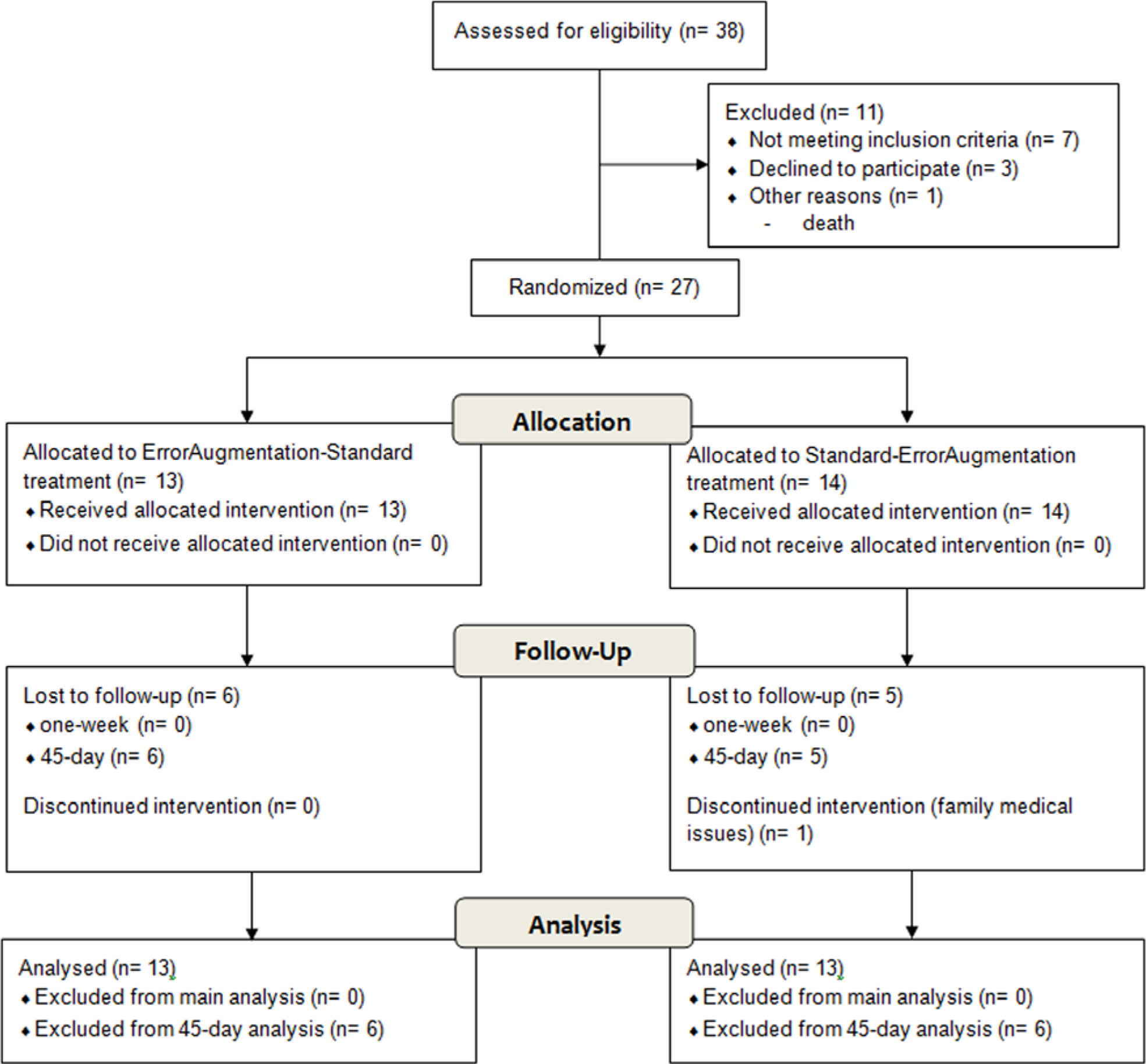
Participant recruitment flow diagram.
Baseline Demographic and Clinical Characteristics.
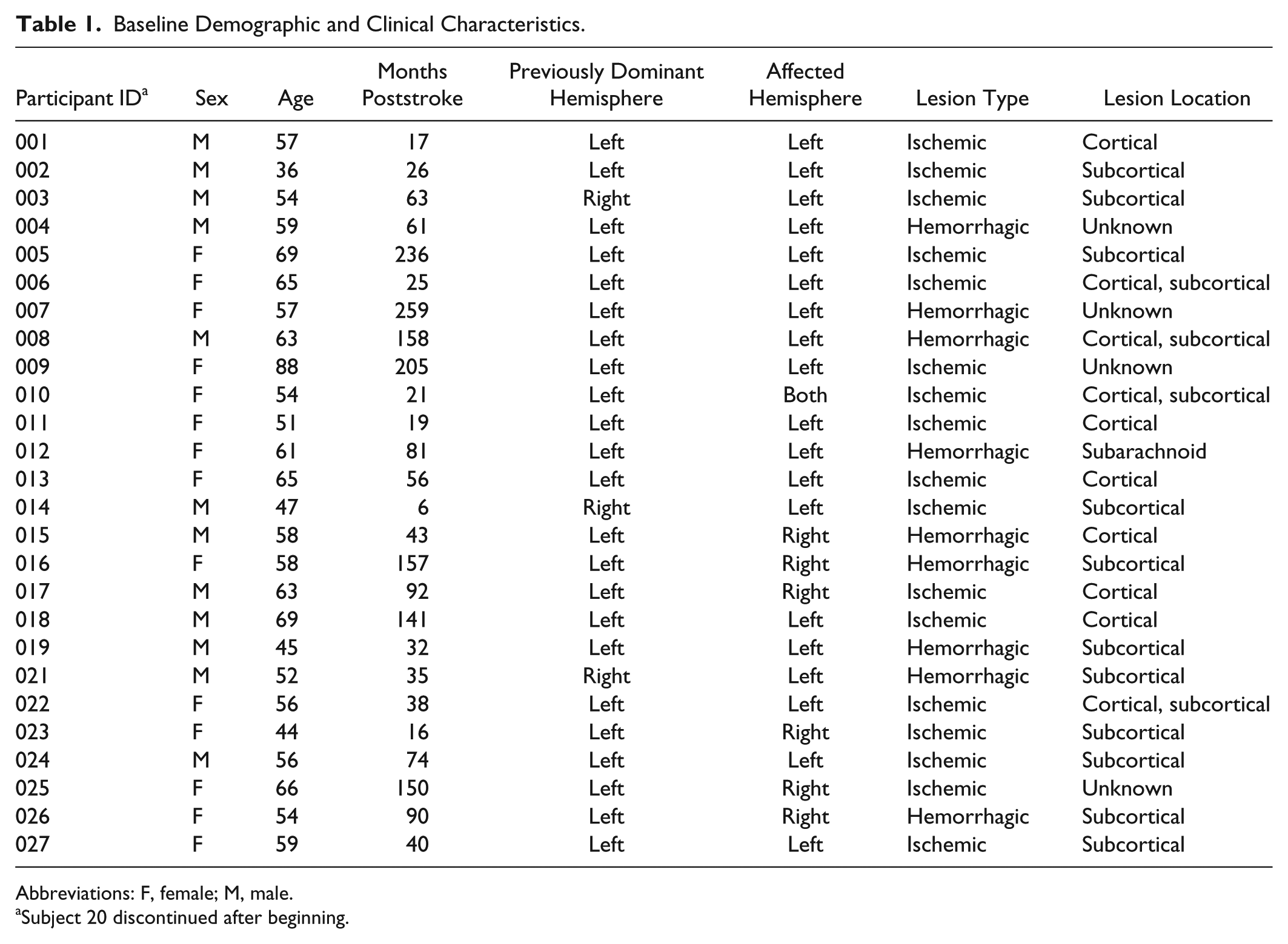
Abbreviations: F, female; M, male.
Subject 20 discontinued after beginning.
Study Setting
The study took place solely at the Robotics Laboratory at the Rehabilitation Institute of Chicago from January 2007 to April 2012. We used a 3-dimensional haptic/graphic system called the Virtual Reality Robotic and Optical Operations Machine (VRROOM). 17 StereoGraphics liquid crystal shutter glasses separated left and right eye images, and Ascension Flock of Birds sensors tracked head motion for appropriate display of perspective. A SensAble Technologies Phantom Premium 3.0 robot interfaced with the participant’s impaired wrist (Figure 2). A Wilmington Robotic Exoskeleton (WREX) provided antigravity arm support. 18
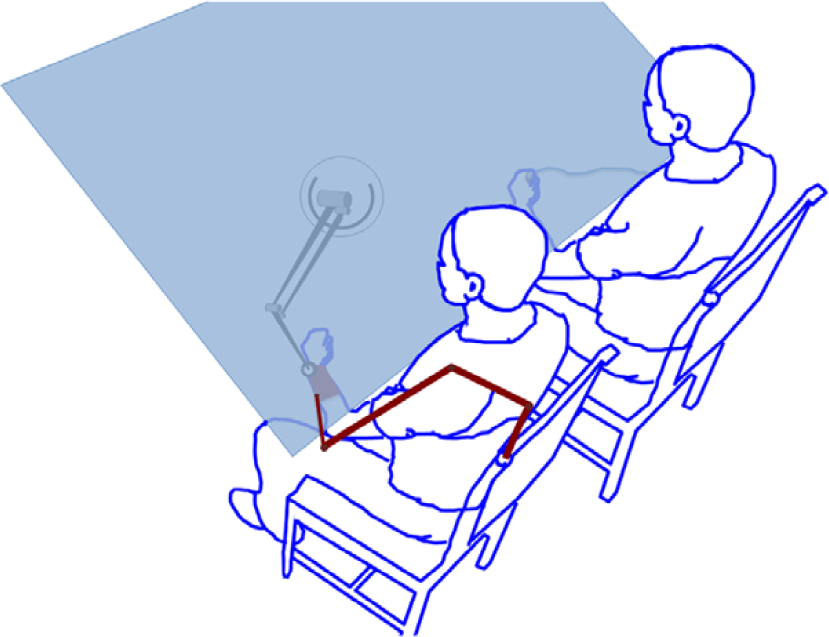
Experimental setup: therapist (right) and participant (left) sat side by side in front of the virtual display. The robot handle is attached to the participant’s hand, and the therapist holds a position tracker. Projected image of a hand (controlled by the therapist) and a green cursor representing the participant’s hand position were projected onto a back projection screen and 2 mirrors, thus giving the illusion of an interactive 3-dimensional environment.
Experimental Protocol
A computer-generated list of random numbers allocated each participant to 1 of 2 groups. We tested 2 experimental robotic-assisted treatments in a crossover design: each participant received either a control treatment of repetitive practice with no EA, called the standard treatment phase, or a treatment with the same amount of practice plus combined visual and haptic error augmentation, called the error augmentation treatment phase. Each phase consisted of 2 weeks of training with participants receiving three 60-minute sessions per week (6 sessions per experimental phase). After a week of rest, each group experienced the other treatment type for another 2 weeks.
Each session began with 5 minutes of passive range-of-motion (ROM) exercises, followed by 10 to 15 minutes of setup of the participant and therapist within the VRROOM, then six 5-minute blocks of movement training with 2-minute rest periods between each treatment block (Figure 3). The treatment protocol included the practice of standardized movements for all participants (consisting of forward and side reaching, shoulder-elbow coupling, and diagonal reaching across the body), in addition to customized movements. The customized treatment blocks targeted specific areas of weakness determined by the therapist based on the previous standardized 5-minute block. This allowed the clinician to customize the therapeutic approach, focusing on what was most critical for a particular participant’s recovery. Between the 2 phases of treatment, participants received a 1-week rest where there were no UE interventions. Quantitative assessments were performed at the beginning and end of each treatment phase (pre and post) as well as 1 week after post (follow-up) and 45 days after the end of the final postassessment. During this 1-week and 45-day retention period also, there were no UE interventions.
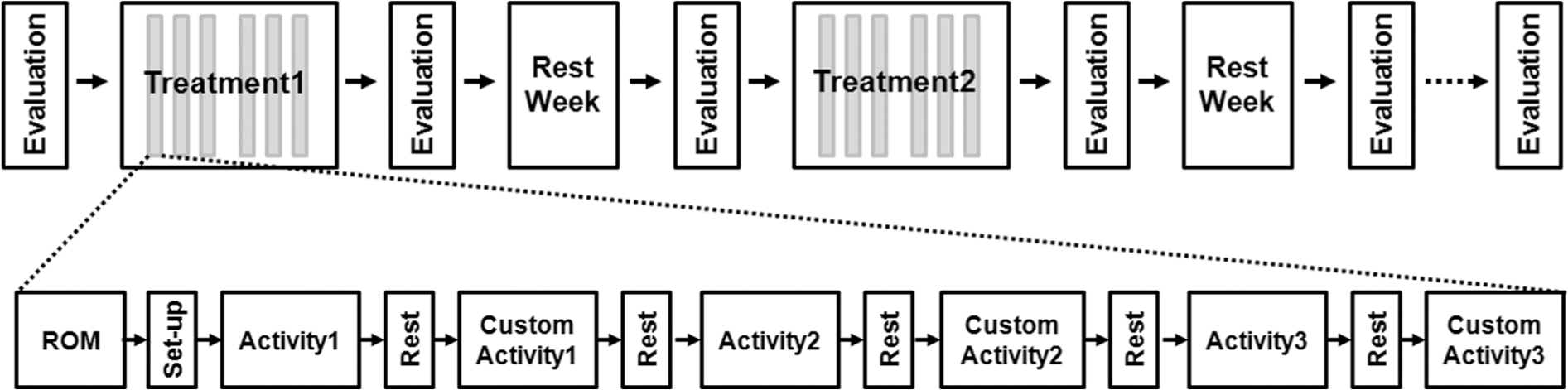
Study layout (top), session layout (bottom).
During all therapy sessions, participants were comfortably seated in a chair with the hemiparetic arm supported by the WREX gravity-balanced orthosis. The hemiparetic hand was placed in an exotendon glove that included a wrist splint, which assisted with hand opening and neutral wrist alignment to allow for a more functional hand and wrist position. Because holding a handle is not necessarily the same as free-hand motion, 19 we connected the robot near the wrist to allow the hand to open freely as well as to allow free pronation and supination of the forearm with the WREX swiveling wrist support. The PHANTOM robot was attached to the forearm with the center of the handle located above the radiocarpal joint. Forces were only applied by the robot during the EA treatment phase; however, the robot was attached during both phases to assist in blinding the participant and treating therapist as well as to provide feedback regarding location within the 3D workspace. It is difficult to determine if these responses reflect any true failure of blinding, 20 and there were also known compromises in our attempt at blinding.
During training, participants were only able to see 2 cursors within the virtual environment with the view of their arms being blocked. One cursor was manipulated by the treating therapist, whereas the other was controlled by the participant. Participants were instructed to follow the exact path of the therapist’s cursor as closely as possible by superimposing their cursor over the therapist’s cursor as it moved throughout the workspace. During the EA treatment phase, the error vector e, defined as the instantaneous difference in position between the therapist’s cursor and the participant’s hand was visually magnified by a factor of 1.5 as part of the EA. Additionally, we applied an error augmenting force of 100 N/m, pushing the participant’s hand further away from the target controlled by the therapist in the virtual environment. For safety purposes, this force was designed to saturate at 4 N. To determine the sample size, we chose to measure the improvement in the Fugl-Meyer clinical score as the main outcome—an improvement of at least 3.5 is commonly believed to be clinically meaningful. 21 Based on a power >80%, 2-sided type I error of 0.025 (adding to 0.05), and an estimated variance of 2.5, 9 we obtained a sample size of 11 patients per group, which was increased to 13 to account for factors of safety and a possible drop-out rate of 10%.
Evaluation Procedure
Participants were evaluated inside the VRROOM with the ROM test and outside the VRROOM with the clinical measures immediately prior to the start and again at the end of each treatment phase. Follow-up testing was performed at 1 week and at 45 days after the end of the second treatment phase. The follow-up evaluation for the treatment received in the first 2 weeks overlapped with the evaluation of the start of the second treatment. A blinded evaluator administered all outcome measures, including our primary outcome, the arm motor section of the Fugl-Meyer (AMFM) to measure impairments,21,22 as well as our secondary outcome measures, which included the Wolf Motor Function Test (WMFT) for functional ability23,24 and the Box and Blocks assessment as an indicator of manual dexterity.22,25 ROM was also evaluated in successive reaches from a neutral point on their lap to 9 evenly spaced targets placed at the extent of the reachable workspace (randomly presented with each target repeated 3 times). From this, we calculated and averaged the fraction of full arm-extension in the direction of each target. Finally, to assess perception of the experience, participants completed the Intrinsic Motivation Inventory (IMI) questionnaire, 26 which consists of 25 questions in 4 categories (interest/enjoyment, perceived competence, motivation/effort, and perceived value).
Statistical Analysis
To examine for treatment-related change, outcomes were analyzed using a repeated-measures analysis of variance (ANOVA), with factors of evaluation day (pre vs post), treatment type (EA vs standard), and treatment order (EA first vs EA second). To examine for retention, a second-repeated measures ANOVA was performed with factors of evaluation day (post vs follow-up), treatment type (EA vs standard), and treatment order (EA first vs EA second). Finally, for each treatment type, a paired t test was used to evaluate participants’ changes in performance at 45 days relative to the final post time point. All statistical tests were evaluated using an α level of .05.
Results
The primary analysis was EA treatment effect and involved all patients who were randomly assigned. Our main outcome measure, AMFM, in an overall analysis, showed significant improvement over the 6 weeks (paired t test, t = 4.077, df = 25, P < .001), such that the average gain was 2.23 ± 2.79 points. Further detailed analysis (repeated-measures ANOVA) showed a significant interaction effect between treatment type and evaluation day: F(1, 24) = 4.261, P < .050. The treatment type by evaluation day interaction indicated that within the 2-week training phases, the EA treatment showed significantly better performance than the standard treatment. As shown in Figure 4 (left), over the first phase of training, the EA treatment group showed a change in 2.08 points (pre to post), whereas the standard treatment group rose only 0.69. As can be seen in the same figure, during the second phase of training where each group swapped training types, although not significant, the group that received EA training showed larger improvements than the group who received standard training. As a result, EA treatment provided a therapeutic advantage that further improved the average gains by 1.00 AMFM point over repetitive practice alone. The treatment-type by treatment-order interaction—F(1, 24) = 5.933, P < .025—indicated that there was significant improvement in the second 2-week period, relative to the first. There was also a significant main effect in evaluation day showing that participants improved an average of 1.12 ± 2.48 points for each 2-week treatment phase over the course of training: F(1, 24) = 7.013, P = .014. These improvements were unchanged after 1 week of rest: F(1, 24) = 0.00, P = 1.00. With the 15 participants for which we were able to obtain data at a 45-day follow-up, the AMFM showed an overall improvement averaging 2.93 ± 3.37 points from the first evaluation to the 45-day follow-up evaluation (paired t test, t = 3.372, df = 14, P < .005).
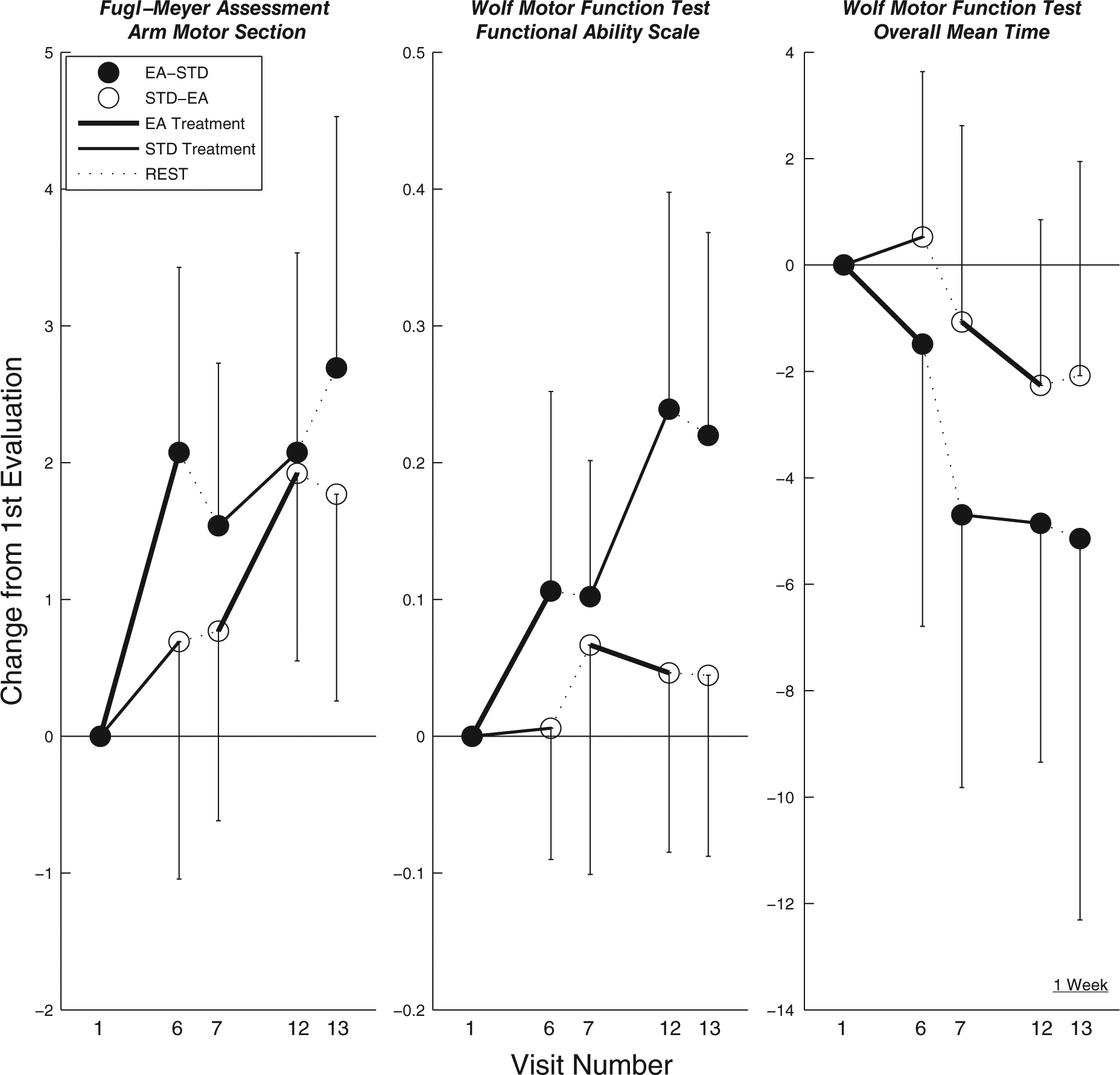
Clinical score changes from the first visit: AMFM score (left), WMFT score (middle), WMFT time (right). Thick line shows the EA treatment, thin line is the standard treatment, and dashed lines are the rest periods. Each group is shown in a different color.
When we examined the final outcome of each group, as seen in Figure 4, the group that started with EA treatment showed an improvement of 2.69 ± 3.07 points, whereas the other group showed an increase of 1.77 ± 2.52 points. Interestingly, this trend was also found at the 45-day follow-up where the group receiving EA treatment first showed a total improvement of 4.13 ± 4.05 points and the second group showed a total improvement of 1.57 ± 1.81 from the first visit. These overall gains from the beginning of the training to the end of the study occurred despite a drop in performance after returning from a 1-week break, such that there was no significant difference in AMFM scores for the groups training with and without EA prior to starting the second phase of the training.
We found similar treatment-related results in our secondary measures. Although variable, the WMFT Functional Ability Scale (FAS) improved significantly, with an overall average of 0.13 ± 0.24 points over 6 weeks (paired t test, t = 2.735, df = 25, P < .012). This score also showed a significant interaction effect between treatment type and order of treatment—F(1, 24) = 7.416, P < .012—indicating that there was higher gain in the second 2-week period relative to the first (Figure 4, middle). This effect was unchanged after 1 week of rest: F(1, 24) = 3.149, P > .088. The same trend was also seen in the WMFT time measure, where the significant interaction between treatment type and treatment order—F(1, 24) = 7.860, P < .010—indicated a shorter time to complete task items in the second 2-week period (Figure 4, right). These improvements were unchanged after 1 week of rest: F(1, 24) = 3.123, P > .088. Finally, at the 45-day follow-up, the WMFT showed overall improvements averaging 0.21 ± 0.36 points with the FAS from the first evaluation to the 45-day follow-up evaluation (paired t test, t = 2.272, df = 14, P < .040).
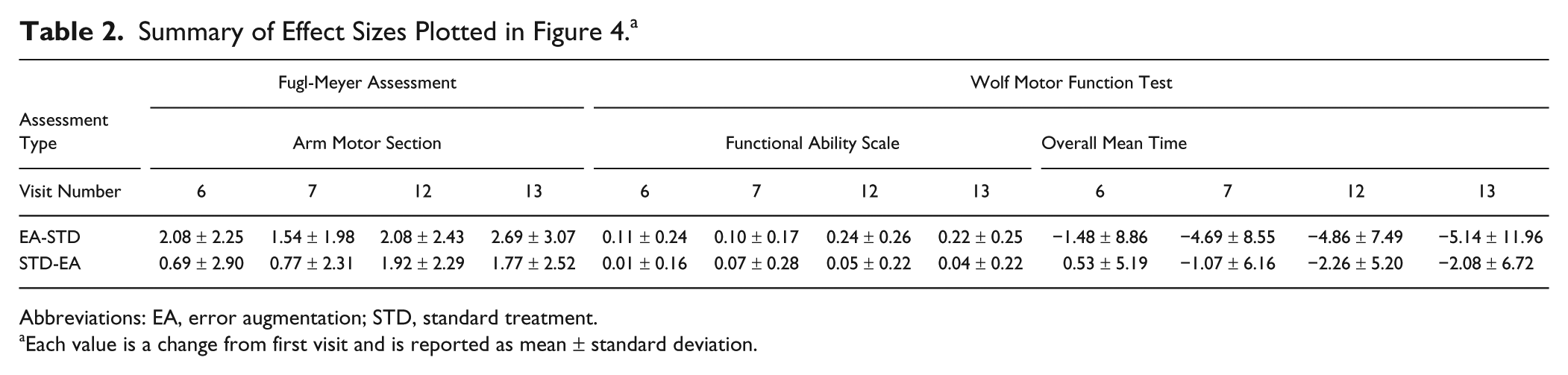
The measure we constructed, ROM, appears to be less sensitive to change. We failed to detect significant treatment-related effects in ROM and Box and Blocks assessments. A summary of all the effect sizes reported above is shown in Table 2.
Abbreviations: EA, error augmentation; STD, standard treatment.
Each value is a change from first visit and is reported as mean ± standard deviation.
Perceived value and enjoyment of the overall experience was evident in the IMI questionnaire results. The highest scores were associated with questions such as, “I would be willing to do this again because it had some value to me.” Generally, all results were more in agreement with the positive questions and more in disagreement with negative questions (see the online appendix). The lowest scores were reported in questions related to the perceived competence subscale, such as, “I think I did pretty well at this activity, compared to others.” The groups of IMI questions were averaged and then compared with the overall clinical outcome scores, but the series of 24 pairwise correlations revealed no significant relationships higher than R2 = 0.45.
Discussion
This blinded, randomized crossover study revealed a benefit of repetitive practice with EA over repetitive practice alone. The AMFM, WMFT FAS score, and WMFT Functional Ability Scale (FAS) time showed significant EA-related improvements when compared with standard care. Although this study does not firmly establish the clinical efficacy of such interventions, it does shed light on a family of future methodologies for improving motor function after stroke.
Although the effect sizes were modest and could be considered not quite clinically meaningful, 27 we argue that such gains might continue for longer treatment courses. In contrast to this study, typical robotic interventions include a training duration of at least 6 weeks or more.6,28-30 In the literature, constraint-induced movement therapy utilized 2-week periods, with each day including 6 hours of training1,31,32; others included 2 to 3 hours of training. 33 Our study matched several other studies in weekly dosage (1-hour treatment sessions 3 times per week).6,29,30 However, our study had a shorter duration of 2 weeks per treatment phase, whereas the aforementioned studies lasted 6 to 8 weeks. Because EA showed significant improvements during just 2 weeks of treatment, larger effect sizes might be obtained with higher treatment dosages or durations. Participants also reported improvements in function such as increased use of the involved extremity in daily life and improved self-care independence, which were not captured in any of the outcome measures. This could be a result of the measures not being sensitive enough to these changes. In future studies, it may be beneficial to include a self-report questionnaire such as the Motor Activity Log. 34
This study builds on several other studies that highlight the prospect of augmenting error in order to enhance the learning process and supports EA as an effective option over regular, repetitive practice for therapy. Such work has been shown to be effective in reshaping movements in individuals with stroke, 9 altering the rate and amount of adaptation in locomotion training, 14 and encouraging more force output in rehabilitation tasks. 12 Our work here joins other mounting evidence supporting EA approaches for speeding up or enhancing learning in both healthy and brain-injured individuals.
Whereas EA can be considered a form of antiassistance, it is important to distinguish it as neither assistive 35 nor resistive in the manner that weight training resistance exercise impedes motion to foster hypertrophy, bone density, and motor unit recruitment. 36 EA may actually push in any direction relative to the direction of motion, depending on locations of the cursor and target.
It is still not clear what underlying neurological mechanisms might be the reason individuals respond to EA. It may be that the impaired nervous system neither reacts to nor learns from smaller errors, and the EA approach might promote learning by making errors more noticeable. Moreover, models of learning suggest that at least one mechanism of learning is driven by error.10,11 The approach might also simply heighten motivation and/or attention or simply intensify the signal-to-noise ratio for sensory systems, making errors more noticeable.
One insight may come from how results differed between ability (AMFM) and function (WMFT). WMFT (Figure 4, middle and right-hand side plots) did not significantly improve when applied in the second phase (weeks 4 and 5). These data suggest that the intervention had greatest impact on motor ability and may have diminishing effects on functional ability. It may be that more functionally relevant tasks in the presence of EA can lead to continued gains in functional scores. Moreover, Figure 4 suggests that if EA is performed in the second 2-week period, performance increases may be more difficult to detect, perhaps because of an order effect.
Although the IMI revealed a positive experience overall, some participants did not find the repetitive nature of the intervention particularly engaging. There were no gaming elements or scores for success, and the only motivational mark for success was their own view of the cursor and target in real time. Several complained about the mundane, repetitive nature of the experiment, expecting a more “exciting” experience using virtual reality. However, positive changes in clinical scores were seen even without an engaging interface. It remains to be seen whether more creative elements can be used to enhance the involvement of the participants’ attention to optimize clinical outcomes or whether such elements might serve as a distraction from rigorous deliberate practice. 37
Although helpful in assisting arm posture, the WREX gravitational assistance device and hand-opening glove may have increased setup time and restricted movement at the extremes of the reachable workspace. Participants with less impairment may have also benefited from less inhibited reaching without this equipment. It remains to be seen whether an alternative approach could improve results, with a clinical cutoff for supplementing with such assistive devices.
This study provides practical clinical evidence that points to future studies that can improve arm motor recovery. The techniques associated with EA may be easily added to the repertoire of possible strategies for rehabilitation, likely to be most effective if combined with other rehabilitation strategies. In the search for optimal training methods, the evidence presented here points to possible future research that makes use of feedback technology to leverage the error-based adaptive tendencies of the nervous system to improve motor recovery and possibly functional reaching ability.
Footnotes
Acknowledgements
We thank Sylvester Vijay, Assaf Pressman, Felix Huang, Kathy Stubblefield, Meghan Buell, Amit Shah, Sarah Housman-Gunderson, Leland Wilkinson, and Derek Kamper for their excellent technical and clinical assistance and advice on this project.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by National Institute of Disability and Rehabilitation Research (H133E0700 13) and National Institute of Health (R01 NS053606), the summer internship in neural engineering (SINE) program at the Sensory Motor Performance Program at the Rehabilitation Institute of Chicago, and the Falk Trust. For additional information see <![]() >.
>.