Abstract
Keywords
Introduction
Among persons with cervical spinal cord injury (SCI), restoration of hand function is a key priority. 1 Various therapies, surgical interventions, and devices have been proposed to improve hand function in individuals with C4-C7 tetraplegia. Among these interventions, functional electrical stimulation (FES) devices have shown promising results. 2 Some FES systems for grasping, also known as neuroprostheses for grasping, have been successfully commercialized and are typically intended for routine daily use. 3,4 During a power grasp, the object is held in a clamp formed by partly flexed fingers and the palm; counterpressure is applied by the thumb lying more or less in the plane of the palm. 5 Precision grip of small objects is generated by flexing the fingers and opposing the thumb. 5
Anecdotal accounts over the past 30 years have reported that individuals with C4-C7 tetraplegia who frequently use their FES systems for grasping may have experienced improved carryover in function that persists even when the device is not in use. 6-10 Neurological mechanisms for the carryover effect were proposed by Rushton in 2003. 11 We published the results of a phase I randomized controlled trial that examined this carryover effect. 12 Although that study was not powered to determine treatment efficacy, its results suggested that short-term use of FES therapy (FET) for grasping has the potential to improve hand function in individuals with both complete and incomplete subacute C4-C7 SCI.
The objective of this study was to determine if FET is an effective means of improving voluntary hand function in adults with incomplete subacute (<6 months postinjury) tetraplegia (C4-C7, AIS B-D). We hypothesized that individuals with tetraplegia who undergo FET may have greater improvements in voluntary hand function, in particular grasping, when compared with individuals who receive a similar volume and duration of conventional occupational therapy (COT) during subacute rehabilitation.
Methods
Consenting adult subjects who met inclusion criteria were randomized to either the control group or the intervention group. They received either 1 hour of COT plus 1 hour of FET daily (intervention group) or 2 hours of COT (control group) on weekdays, for a total of 10 hours of therapy per week for 8 weeks. Outcome assessments were performed by staff blinded to the study intervention and group allocation. The study was approved by Toronto Rehabilitation Institute’s research ethics board and registered on www.clinicaltrials.gov (ClinicalTrials.gov ID NCT00221117). We certify that all criteria for the ethical conduct of clinical trials were met.
Subjects
Eligible subjects were identified through staff referrals, poster campaign, and local advertisements during their initial inpatient rehabilitation following traumatic SCI.
Inclusion criteria
(
Exclusion criteria
(
Study Protocol and Randomization
Subjects were randomized using 2 sets of sealed envelopes. Each unmarked envelope contained a single sheet of paper with a printed number in the range of 1 to 40. A second set of envelopes was marked with numbers from 1 to 40 and contained a single sheet specifying the group allocation. The randomization schedule was done using the
Interventions
Conventional occupational therapy
COT pertaining to hand function
12
represents the current best practice activities against which the FET was compared. The COT included the following: (
FES therapy
The FET began by designing stimulation protocols to generate power (circular grip and lateral pinch) and precision (opposition with 2 and 3 fingers) grasps on demand. The stimulation sequence (protocol) for power and precision grasps was developed for each patient individually using the Compex Motion electric stimulator. Compex Motion is a fully programmable transcutaneous (surface) stimulator that uses self-adhesive surface electrodes. 13
The power grasp was used for grasping bigger and heavier objects such as water bottles and coffee mugs (see Figure 1). Lateral pinch was used for grasping smaller and thinner objects such as keys and paper. Precision grip was used for grasping smaller objects such as dice and popcorn. Power grasp was generated by partly flexing the fingers and the thumb in flexion and slight opposition. Lateral pinch was generated by fully flexing the fingers followed by the thumb flexion. Precision grip was generated by first forming opposition between the thumb and the palm, which was followed by index finger and thumb flexion. Muscles that were stimulated during therapy were the following:

Examples of object manipulation during the functional electrical stimulation therapy.
The FET protocol used in this study allowed individuals who did not have any voluntary movement or contraction in the wrist and fingers to be included. This factor makes FET unique when compared with alternative therapy forms. In the early stages of FET all the movements were performed with the help of FES. Subjects were asked to imagine a particular movement and then try to execute it voluntarily. The occupational therapist would allow the subject to struggle while trying to perform the desired movement. Ten to 20 seconds after attempting a desired task, the therapist activated the FES sequence and helped the subject perform the desired movement. As soon as an individual showed signs of recovery of either voluntary extension or flexion in a stimulated muscle group, he/she was encouraged to make an effort to produce the movement voluntarily, which was previously facilitated by FES. As the subject demonstrated improved strength and range of motion, the FES for those muscle groups were phased out and refocused on other muscle groups that were still weak and needed to be “reactivated.” The order in which muscle groups were sequentially “reactivated” was subject dependent. In later phases of FET the use of FES was reduced considerably and was used only to help a subject carry out particular components of the movement that he/she was still unable to do.
In all cases FET was delivered while the individual was performing functional tasks, such as grasping a mug, writing his/her name, playing table tennis, and so on. Use of FET as part of a functional training was an essential component of this therapy. FET was not used for muscle strengthening; instead, it was used to retrain the neuromuscular system to execute tasks it was previously unable to carry out voluntarily. Movements were performed against gravity and sometimes against light manual resistance. The number of repetitions was determined based on subject’s strength and endurance. In general, the subject spent at least 45 minutes out of the 60 minutes of daily FET performing various tasks common in ADLs while being assisted by FES system for grasping. In the later stages of therapy the therapists allowed the subject to control the triggering of the stimulation sequences. The key element in this therapy, besides FES, is that the subject was fully engaged in the therapy process and that he/she paid attention to the tasks being performed. That is why the focus of our FET was execution of as many diverse functional tasks as possible during the therapy sessions.
The stimulation parameters used were the following: (
Therapy Dose
All subjects received therapy daily, 5 days per week, for the duration of 8 weeks (total of 40 sessions). On “therapy days” all subjects received a total of 1 hour of COT between the right and left hands and 1 hour of either FET (intervention group) or additional 1 hour of COT (control group) between the right and left hands. The 2 hours of therapy were performed with at least a 2-hour break in between. Both groups received 1 dose of COT irrespective of their group allocation to ensure that they received the best practice upper limb therapy for tetraplegic patients available at the time of this study within the medical rehabilitation program at Toronto Rehab. Subjects in the control and intervention arms of the study received equal amount of therapy and attention.
Outcome Measures
Primary outcome measure
The Functional Independence Measure (FIM) 15 was employed to measure the degree of disability for daily self-care.
Secondary outcome measures
The Spinal Cord Independence Measure (SCIM)
16
is a disability scale that has been specifically developed to evaluate the degree of disability in patients with traumatic and nontraumatic SCI. The SCIM assesses function in 3 core areas: (
The Toronto Rehabilitation Institute Hand Function Test (TRI-HFT) 17 evaluates gross motor function of unilateral grasp (also referred to as the Rehabilitation Engineering Laboratory Hand Function Test). Hand functions that are assessed with TRI-HFT include the following: lateral or pulp pinch and palmar grasp. The TRI-HFT consists of 3 components. The first evaluates the power grasp, the lateral pinch, and precision grip, whereas the second and third components evaluate the strength of both power and lateral grasps. The scoring system for TRI-HFT (scale 0-7) is as follows:
0 = No movement elicited, that is, subject unable to reach for the object
1 = Subject able to reach for the object but unable to grasp the object
2 = Subject able to reach and grasp (using passive grasp) but unable to lift the object successfully off the supporting surface
3 = Subject able to reach and grasp (using active grasp) but unable to lift the object successfully off the supporting surface
4 = Subject able to reach, grasp, and lift the object (using passive grasp) but unable to manipulate the object
5 = Subject able to reach, grasp, and lift the object (using active grasp) but unable to manipulate the object
6 = Subject able to reach, grasp, lift, and manipulate the object (using passive grasp) appropriately
7 = Subject able to reach, grasp, lift, and manipulate the object (using active grasp) appropriately
This scoring system was developed specifically for individuals with SCI in distinction to another system 12,17,18 for stroke.
Statistical Analysis
The subject’s impairment and demographic characteristics were analyzed using descriptive statistics for parametric and nonparametric data. The baseline outcome data of the intervention and control groups were compared using Fisher exact test (for categorical variables) and Mann–Whitney
Results
Figure 2 shows the CONSORT diagram for screening and entries. One subject in the intervention group and 1 control dropped out. Data for 1 subject in the intervention group was corrupted before the analysis was preformed, which left 21 subjects (9 in the intervention group and 12 in the control group) with full baseline and therapy completion data. Demographics and neurological descriptors are shown in Table 1. Out of these 21 subjects who successfully completed the therapy and had complete data sets at baseline and therapy completion, only 5 were willing and able to participate in the 6-month follow-up assessment session (4 in the intervention group and 1 in the control group). Because of very poor response of the subjects in taking part in the 6-month follow-up assessment session, only data collected at baseline and therapy completion phases of the study were analyzed.
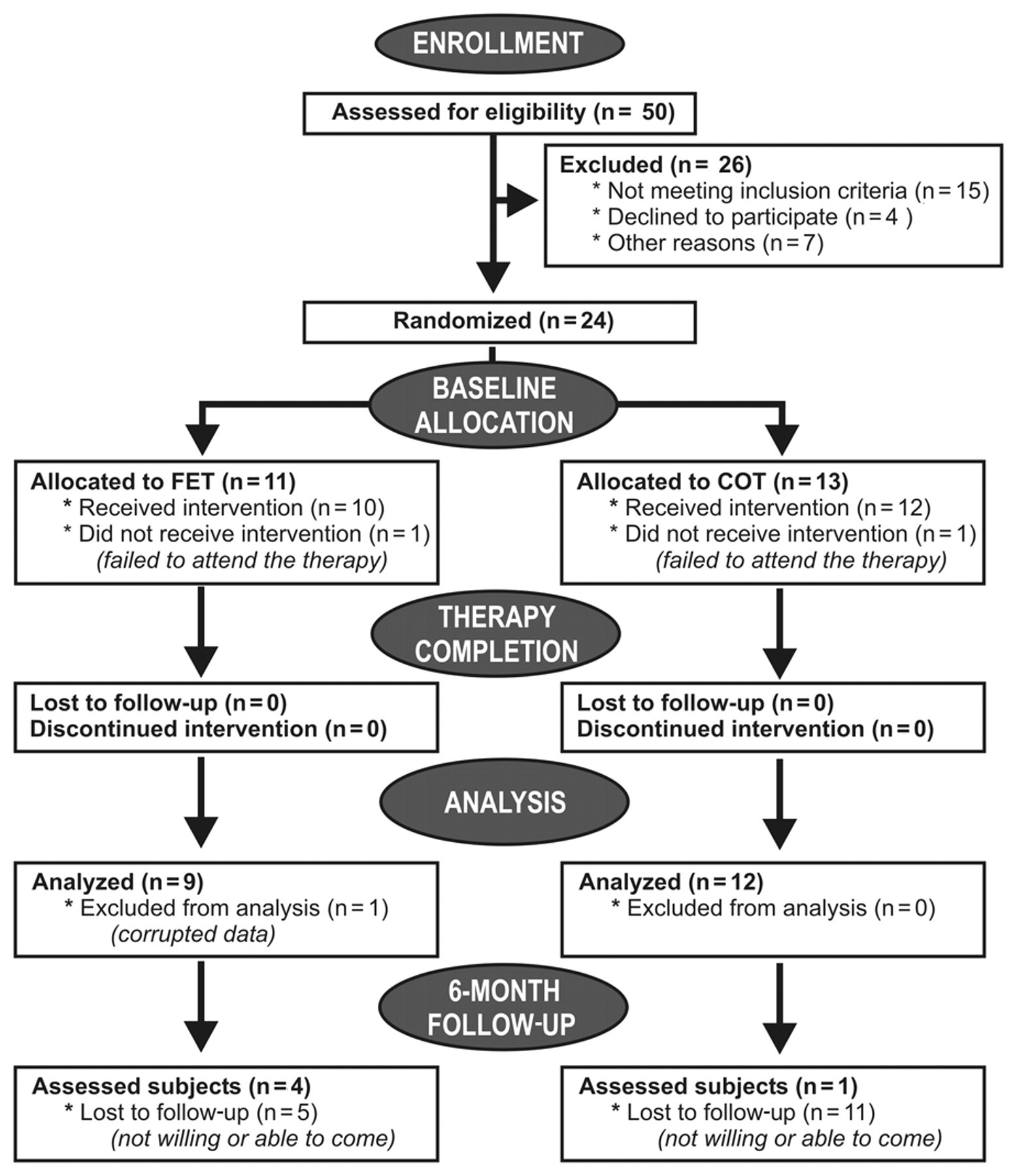
CONSORT diagram showing the recruitment process and the recruitment numbers Abbreviations: FET, functional electrical stimulation therapy; COT, conventional occupational therapy.
Subjects’ Demographic and Neurological Data
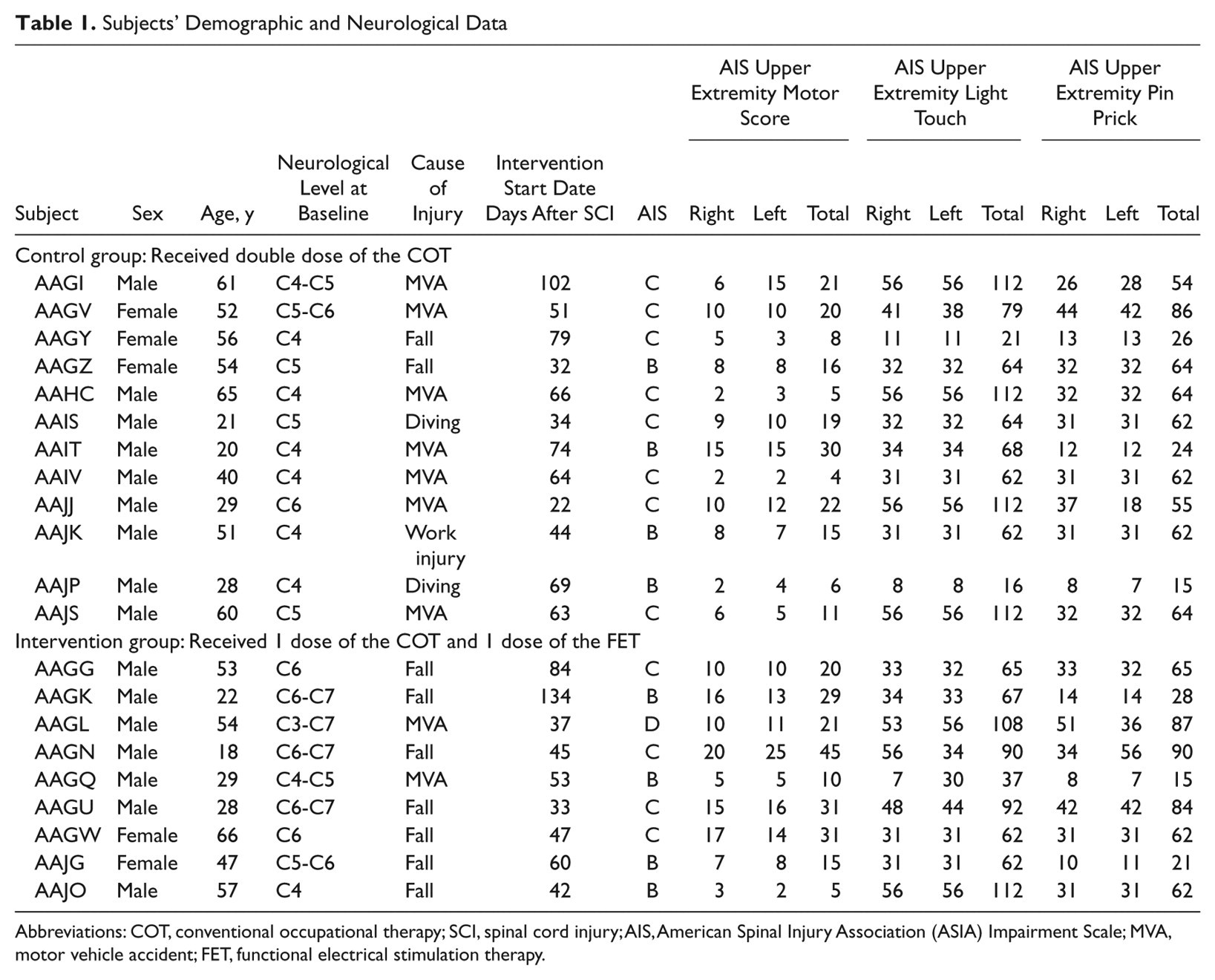
Abbreviations: COT, conventional occupational therapy; SCI, spinal cord injury; AIS, American Spinal Injury Association (ASIA) Impairment Scale; MVA, motor vehicle accident; FET, functional electrical stimulation therapy.
At baseline there was no clinically significant difference between the groups (Table 2). At completion, both intervention and control groups improved (Table 3 and Figure 3). However, the FET group improved more (Table 4). Statistically significant improvements were observed in FIM self-care subscores, SCIM self-care subscores, TRI-HFT instrumented cylinder scores, and TRI-HFT credit card scores (Figures 4 and 5). Trends with repeated-measures testing were found for the TRI-HFT total score for manipulation of objects 1 to 10
12,17,18
(
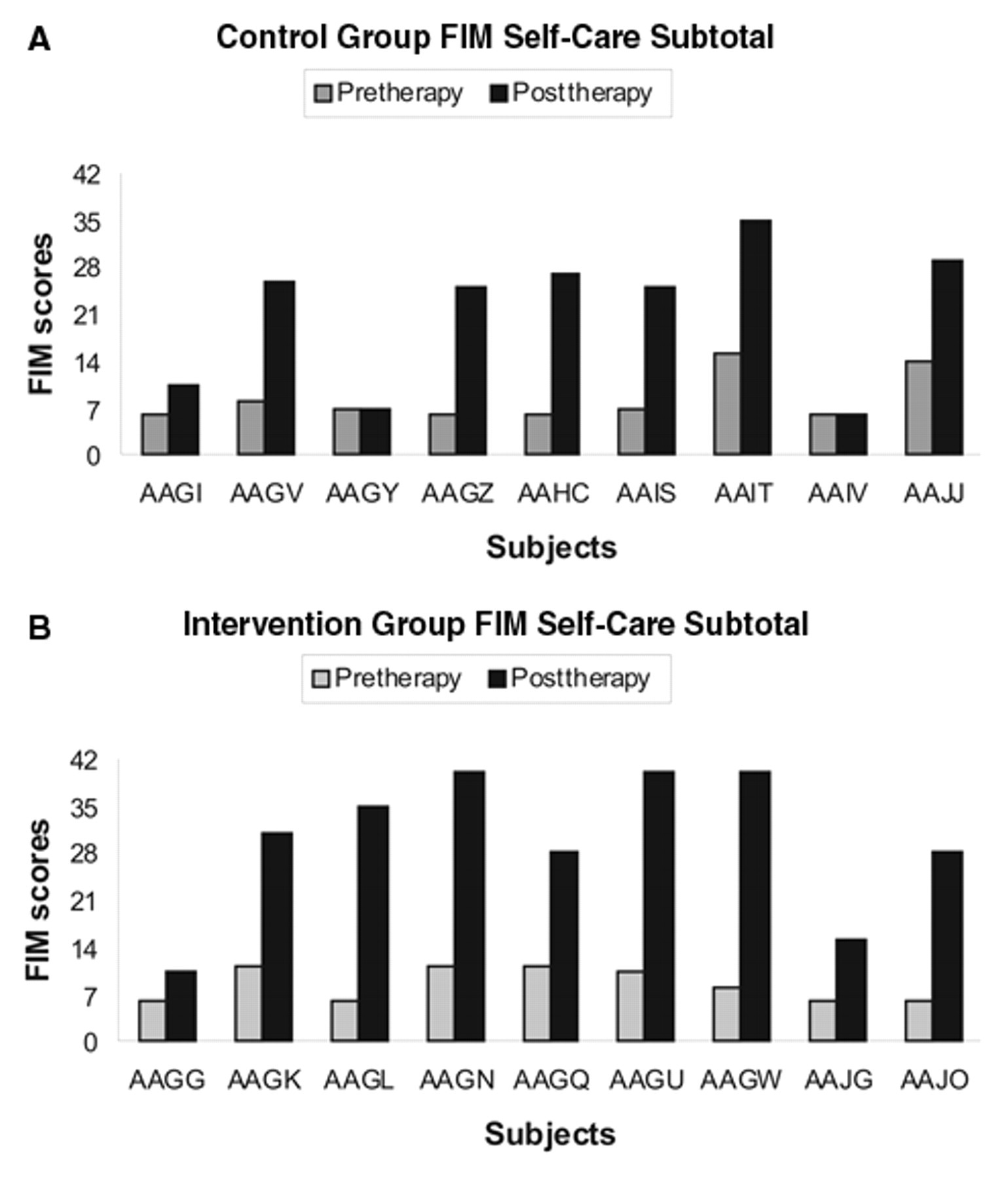
(A) Subjects’ Functional Independence Measure (FIM) Self-Care subscore before and after therapy for the control group. (B) Subjects’ FIM Self-Care subscore before and after therapy for the intervention group.
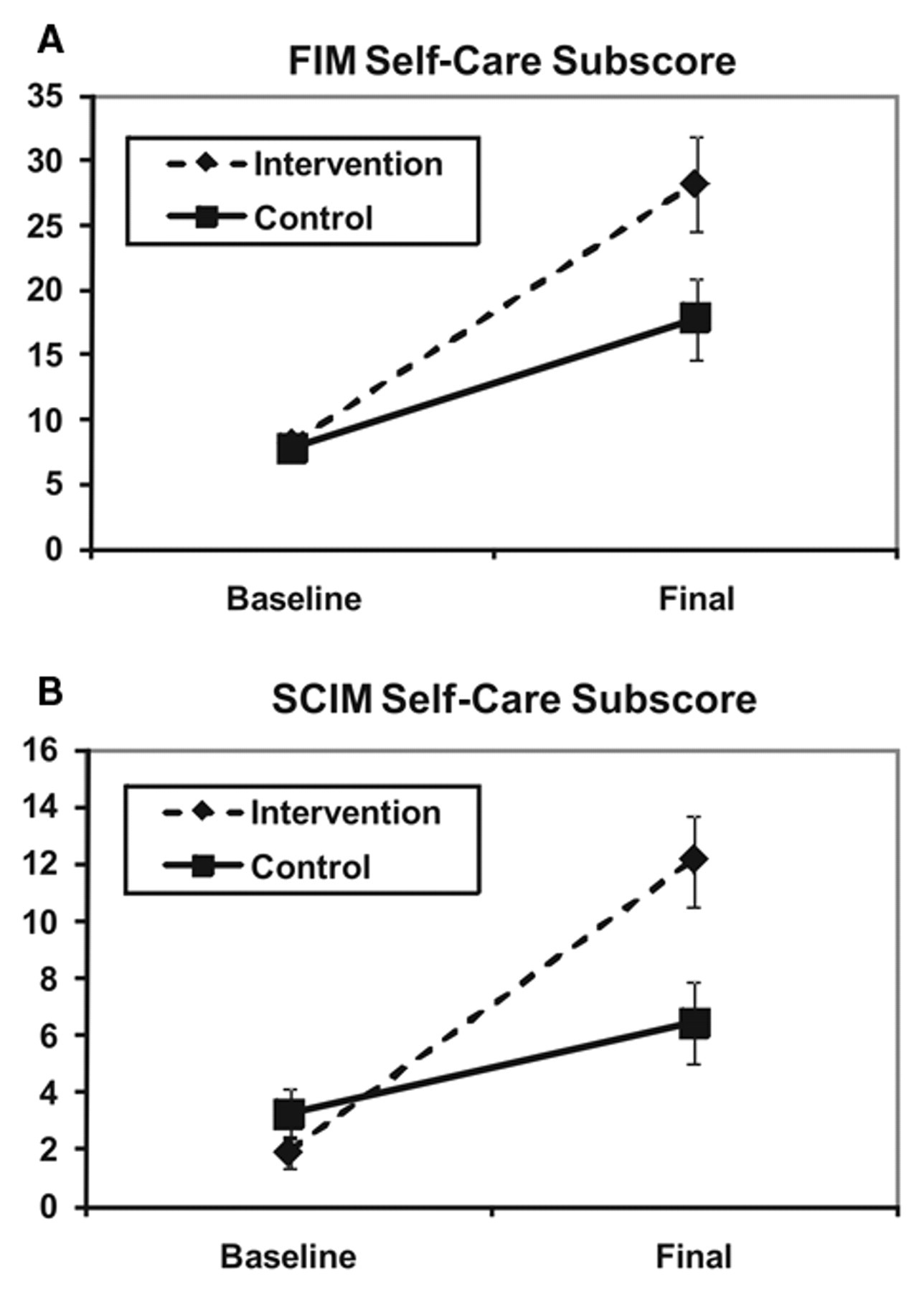
(A) Functional Independence Measure 9FIM) self-care subscores at baseline and after therapy completion for the controland intervention groups (mean ± standard error of mean). (B) Spinal Cord Independence Measure (SCIM) self-care sub-scores at baseline and after the therapy completion for the control and intervention groups (mean ± standard error of mean).
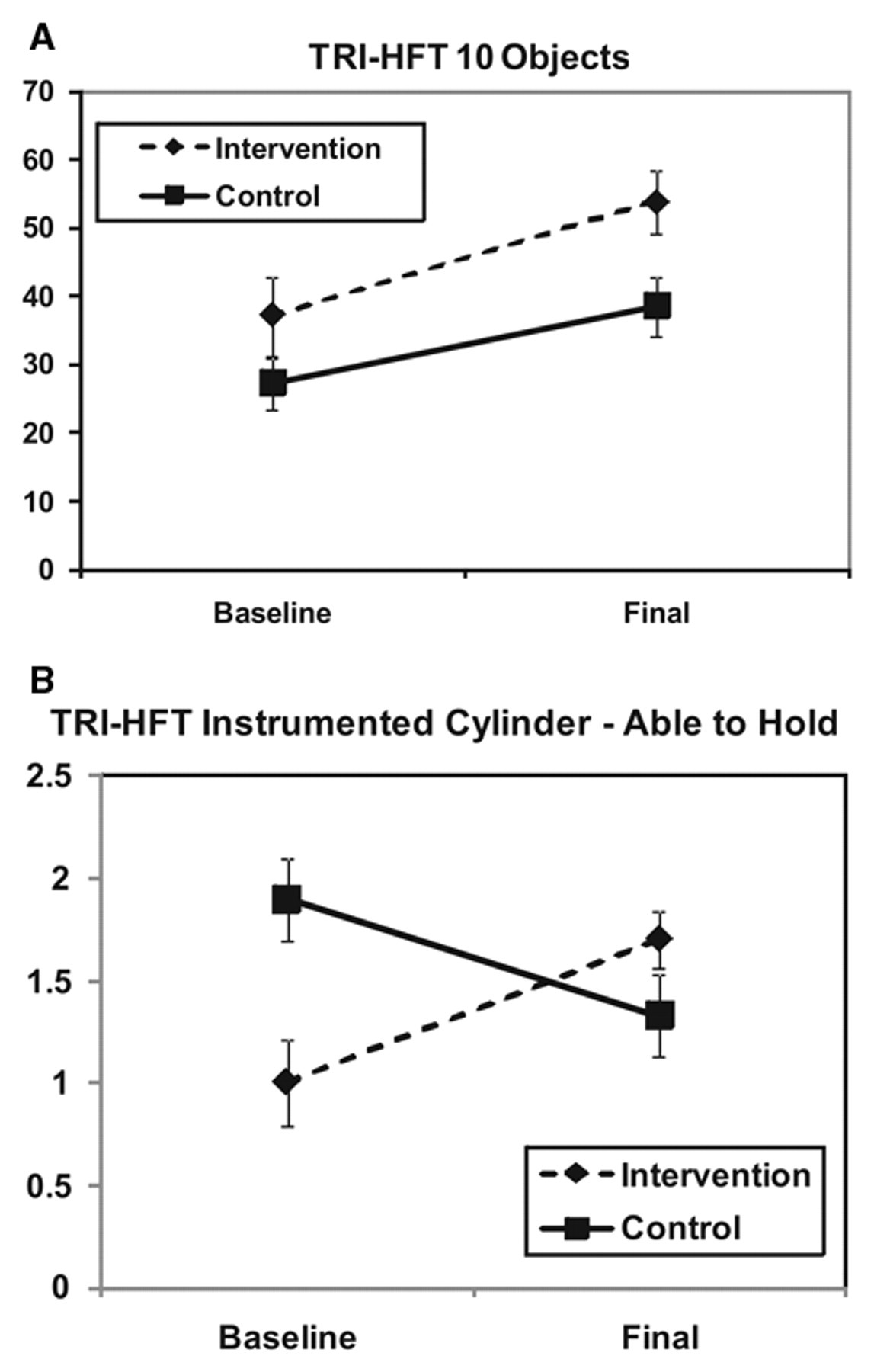
Toronto Rehabilitation Institute Hand Function Test (TRI-HFT) 10 objects (objects 1 to 10 in Refs [12, 17, 18]) total score at baseline and after therapy completion for the control and intervention groups (mean ± standard error of mean). (B) TRI-HFT Instrumented Cylinder—Able to Hold (object 12 in Refs [12, 17, 18]) score at baseline and after therapy completion for the control and intervention groups (mean ± standard error of mean)
Baseline Data Comparisons Between Control and Intervention Groups
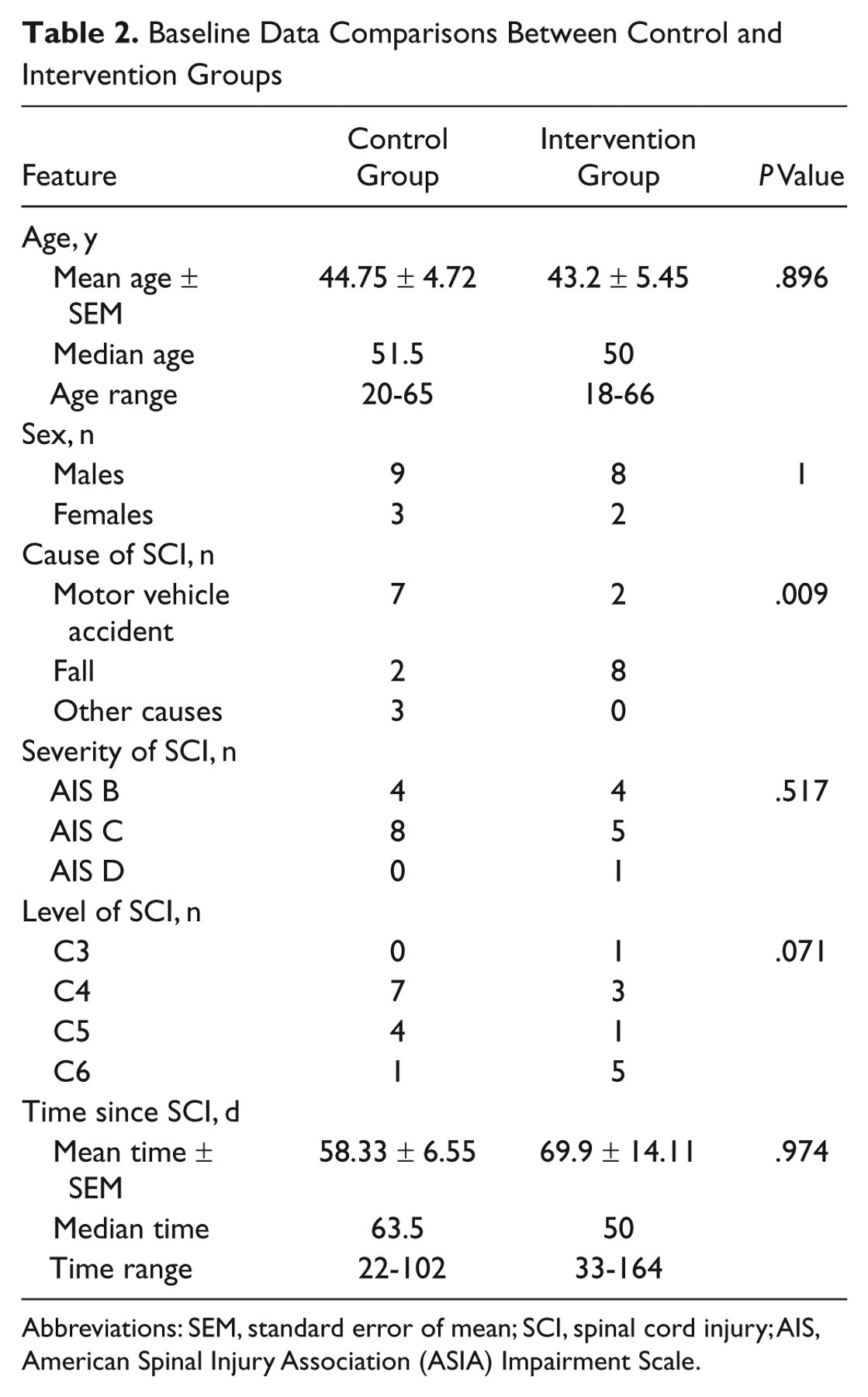
Abbreviations: SEM, standard error of mean; SCI, spinal cord injury; AIS, American Spinal Injury Association (ASIA) Impairment Scale.
Individual Subjects’ FIM Self-Care, Sphincter Control, and Motor Subscores for the Intervention and Control Groups
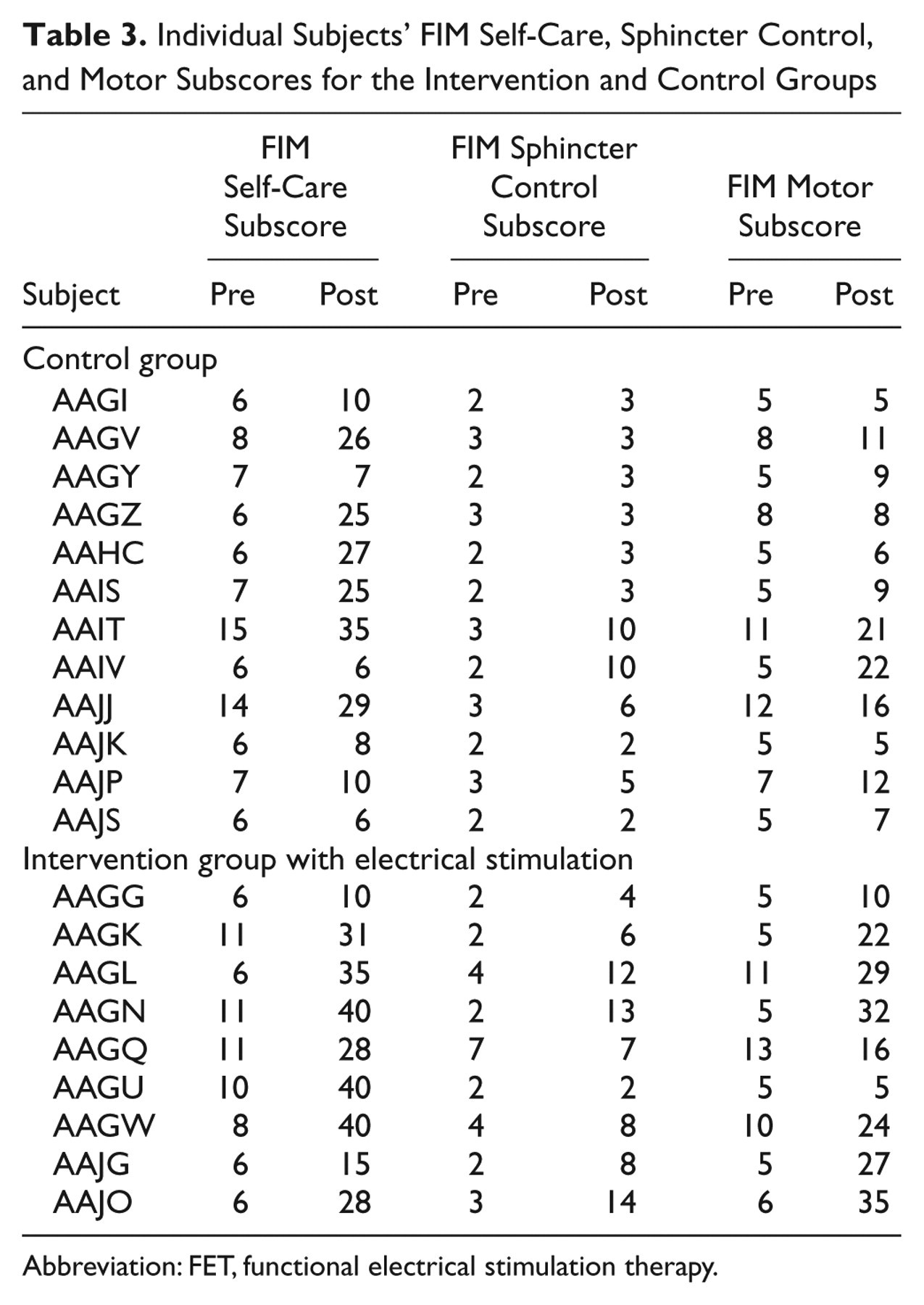
Abbreviation: FET, functional electrical stimulation therapy.
Summary of the Mean Test Results for the Control and Intervention Groups at Baseline (Before) and on Completion of the Therapy (After), With Corresponding
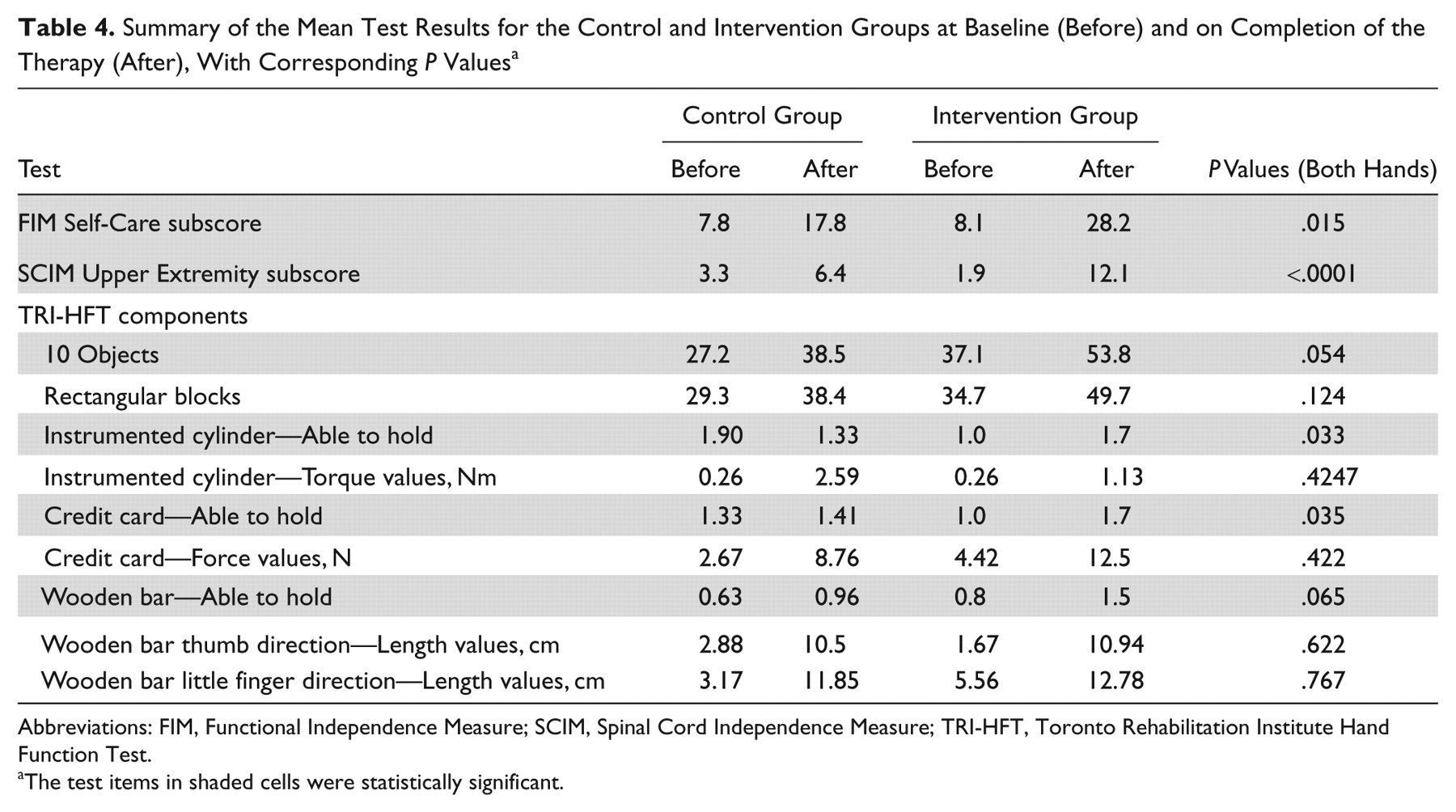
Abbreviations: FIM, Functional Independence Measure; SCIM, Spinal Cord Independence Measure; TRI-HFT, Toronto Rehabilitation Institute Hand Function Test.
The test items in shaded cells were statistically significant.
Discussion
This is the first randomized controlled trial evaluating the efficacy of FET in individuals with subacute incomplete tetraplegia after SCI. Statistically significant differences in hand function were found in favor of the FET intervention despite a small sample size (12 in the control group and 9 in the intervention group) and large variability.
The results suggest the efficacy of a surface FET intervention that can be tailored and adjusted to patients’ needs on a daily basis and can evolve as patients improve their function. Furthermore, our findings suggest that if a subject who attempts to execute a grasping task is assisted with the FET to carry out that task, he/she is effectively voluntarily generating the motor command. FET is providing afferent feedback (
The results are quite different from those reported in the study where FET was applied to patients with severe hemiplegia. 17,18 Stroke subjects did not experience dramatic improvements in FIM scores. This finding is explained by the typical bilateral disability of persons with SCI, which is not the case in individuals with hemiplegia. Individuals with hemiplegia, with time and intensive therapy, learn how to reach and grasp objects using the least affected arm, without engaging the more affected arm in ADLs. Hence, in these subjects, improving the function in the disabled arm does not produce significant changes in FIM scores. However, in the individuals with SCI, who typically have bilateral disability, even small improvements in hand function may produce measurable improvements in the FIM and SCIM scores. The results suggest that FET applied to hand function in individuals with SCI positively affects performance in ADLs and increases independence measured by the FIM and SCIM.
What is unique about this study is that we provided 1 dose of COT (1 hour of therapy) daily to both the intervention and control groups, followed by 1 dose of either COT or FET. The study design intentionally put FET in a possibly less favorable position compared with the double dose of the task-related COT.
A limitation of this study is that despite considerable effort we failed to attract the subjects to take part in a 6-month follow-up assessment. This can be explained by the fact that the majority of the subjects were discharged home or to long-term care facilities that were far from the study site.
The positive results, as well as results of our preceding study, 12 suggest that individuals with SCI would benefit from FET for grasping and voluntary hand function. We recommend at least 40 one-hour sessions of FET to try to improve upper limb function. Only after the patient has not shown signs of improvement should other invasive procedures be considered, such as implanted neuroprostheses for grasping and tendon transfers.
We have trained more than 30 occupational therapists, physiotherapists, and biomedical engineers to administer the FET. Most of the physiotherapists and occupational therapists already knew how to use electrical stimulation systems, so minimal additional training, up to 2 hours, was needed. Donning and doffing the system requires no more than 5 minutes. From a logistics perspective, FET may be easily integrated into existing occupational therapy programs without requiring additional treatment hours or funds beyond those needed to purchase a programmable FES system.
Footnotes
Acknowledgements
The authors would like to acknowledge the valuable assistance of Kieva Richards, Jennifer Holmes, Suzanne Iafolla, Tamara Schultz, Melanie Alappat, Farhana Jaffer, Grant Murray, Sylvia Haycock, and Abdul Kadir Bulsen, who helped with delivering the therapy and performing the assessments.
The author(s) declared no potential conflicts of interest with respect to the authorship and/or publication of this article.
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: The work presented in this article was supported by grants from The Physicians’ Services Incorporated Foundation (PSI Grant #05-06) and Christopher and Dana Reeve Foundation (TA1-0706-2). Additional financial support for this study was received from the Toronto Rehabilitation Institute and Ontario Ministry of Health and Long-Term Care.
