Abstract
Integrative Oncology (IO) programs are increasingly emerging at cancer centers and universities worldwide; often these include some combination of clinical service, research, and/or training. However, one gap that often occurs is in moving research results into practice, due to complexities and differences between research and service delivery models and priorities. We recently created the ACTION (Alberta Complementary Therapy and Integrative Oncology) Centre with the goal of partnering with the provincial public health service to promote and facilitate evidence-based integrative oncology care throughout Alberta. The Centre bridges the silos of academia and clinical care by embodying 3 core principles, to be (1) Patient-oriented, (2) Collaborative, and (3) Evidence-based. The ACTION Centre oversees the implementation of clinical research and academic training, and supports the development of clinical services, as well as patient and provider education. The ACTION Centre has five components which include: (1) Patient and healthcare provider education; (2) Individualized IO consultation and treatment planning; (3) Supporting access to complementary therapies; (4) Clinical trials of IO interventions, and; (5) Student training through the TRACTION (Training in Clinical Trials and Integrative Oncology) program. We offer this model of shareholder collaboration in the hopes that other IO programs may be able to use it as a template to further their own progress, working collaboratively toward the ultimate goal of advancing evidence-based, comprehensive, integrative healthcare to improve the lives of people affected by cancer.
Comment on: Carlson LE, Zelinski EL, Speca M, et al. Protocol for the MATCH study (Mindfulness and Tai Chi for cancer health): A preference-based multi-site randomized comparative effectiveness trial (CET) of Mindfulness-Based Cancer Recovery (MBCR) vs. Tai Chi/Qigong (TCQ) for cancer survivors. Contemp Clin Trials. 2017;59:64-76. doi:10.1016/j.cct.2017.05.015
In celebration of 20 years of the publication Integrative Cancer Therapies, an important vehicle for sharing evidence-based research on integrative oncology (IO) interventions and approaches, we wanted to share our approach to the integration of complementary modalities with conventional care through the ACTION (Alberta Complementary Therapy and Integrative Oncology) Centre, the first program to successfully integrate IO modalities and consultation into a public, provincial cancer care agency in Canada. This piece serves as a commentary regarding the larger model and structure supporting our ACTION Centre clinical trials; specifically the MATCH study, which utilizes a novel pragmatic, preference-based design to compare a mindfulness-based cancer recovery program to a taichi/qigong program for a wide range of distressed cancer survivors. 1 The study was designed to emulate real-world program delivery and support future implementation efforts. In this case we are attempting to specify for which symptoms each of these interventions are optimally helpful; with this information clinicians can provide more specific guidance to patients who are interested in mind-body modalities, and clinical programs can choose to add modalities that best address concerns common to their clients. For a study like this to be successful, infrastructure supporting stakeholder engagement needs to be in place to enable future dissemination and implementation efforts.
Our objective is to provide a local example of how different institutions and stakeholder groups have collaborated within this model, which might provide a template for others to help implement the structures necessary to successfully integrate complementary therapies within existing cancer care delivery models and operational budgets.
The core philosophy of IO is contained in the official Society for Integrative Oncology (SIO) definition as: “a patient-centered, evidence-informed field of cancer care that utilizes mind and body practices, natural products, and/or lifestyle modifications from different traditions alongside conventional cancer treatments. Integrative oncology aims to optimize health, quality of life, and clinical outcomes across the cancer care continuum and to empower people to prevent cancer and become active participants before, during, and beyond cancer treatment.” 2 Keeping this philosophy and definition in mind, the ACTION Centre operates under 3 core principles: it is (1) Patient-Oriented; (2) Collaborative, and; (3) Evidence-based. There are five components to the ACTION Centre which span the spectrum of research, education, and informing direct clinical care, the key triumvirate necessary to ensure rapid discovery incorporates education of trainees and seamless transition of evidence-based and operationally feasible interventions into clinical care. This sounds simple, but in reality these areas (research, training, professional/patient education, and clinical care) usually operate in silos, with different budgets, different administration, different funding sources and formulas, different policies, different personnel, different priorities, completely different buildings, etc. . .—rendering translation of research results into everyday practice prohibitive.
The ACTION Centre was designed to overcome these barriers by bringing together programs and stakeholders from all these areas to work together toward common goals. It is collaborative in that the Centre is a partnership between the University of Calgary (U of C; research and training) and the provincial health authority which delivers all clinical cancer care (Alberta Health Services-AHS, and within AHS Cancer Care Alberta-CCA). The ACTION Centre works with CCA stakeholders to address knowledge and service gaps in the provision of evidence-based complementary therapies (CTs). Hence, the ACTION Centre is the hub of IO innovation, increasing access to evidence-based CTs, and supporting the translation of IO research into clinical care through strong partnerships. It is patient-oriented in that half of the steering committee consists of patient and family advisors, and the steering committee determines priorities across all five components. The remainder of the steering committee consists of representatives from AHS CCA, including administration, pharmacy, nutrition, supportive care (psychosocial and rehabilitation oncology), medical oncology, radiation oncology; from the University of Calgary (researchers and trainees), as well as local not for profit community-based organizations which support and advocate for cancer survivors, and fundraising bodies including local cancer foundations.
The ACTION Centre oversees the implementation of research and academic training, and develops, evaluates, and improves IO clinical interventions and education across the five components:
Patient and Healthcare Provider IO Education: The ACTION Centre collaborates with CCA to enhance knowledge of the evidence base for the efficacy of CTs and improve patient-provider communication about CTs; programs are delivered in person and online. An evaluation project of one such program has recently been published, showing a simple 3-module online program was effective in improving oncology health care providers’ attitudes and knowledge toward CTs. 3
IO Consultation Service: We are evaluating the provision of an IO consultation service through a grant-funded study. It aims to provide high needs patients undergoing conventional treatment for cancer with an individualized patient-centered, safe, culturally sensitive, evidence-based integrative oncology plan which may include recommendations for specific CTs. It also aims to promote safety and quality in the use of complementary therapies, as well as determining the feasibility and sustainability of incorporating this clinical service into routine practice. The service is led by a medical oncologist trained in IO. Referrals for this service are accepted from any oncology provider (medical/radiation/surgical oncologist, pharmacist, nursing etc.) and consultation is provided free of charge within the cancer centre.
CT Provision: Patients currently have access to a number of evidence-based CTs through publicly funded psychosocial and rehabilitation oncology, nutrition, and pharmacy services within AHS, grant-funded research studies (including within the ACTION Centre) through the University of Calgary, and through non-profit community-based cancer support organizations such as Wellspring (eg, yoga, meditation, support groups, relaxation/hypnosis/imagery, exercise programs, lymphatic massage, nutrition education and counseling, taichi/qigoing), where we have partnered to train providers in evidence-based programs.
IO Clinical Trials Unit: This program is funded largely through operating grants administered by the U of C, and involves trainees in graduate and postdoctoral programs and full-time academic staff. The objective is to enhance the evidence base for CTs in cancer care, focusing on further investigating promising CTs patients are interested in but that lack adequate evidence to fully support integration into practice. The focus is on using patient-oriented and pragmatic research methods.
The TRACTION Program (Training in Research and Clinical Trials in Integrative Oncology): This is a federally funded training program through the Canadian Institutes of Health Research Strategy for Patient-Oriented Research, which trains up to 20 fellows each year across disciplines, programs, and levels (Honors undergrad to postdoc) in IO and patient-oriented methods. These trainees then go on to focus on program development, evaluation, and implementation in a variety of research and clinical settings.
The ACTION Centre organizational structure is presented in Figure 1. As shown, there is also an external Scientific Advisory Board consisting of experienced researchers and clinicians from a range of successful IO programs across North America. This board advises the Steering Committee on matters regarding scientific issues, as well as implementation and education strategies from their own extensive experience. The collaborative nature of the program can be seen in the different colors; primarily U of C (research/training) components are in red; AHS (clinical care) components in green. There is a sub-committee comprised of a mix of steering committee members from both U of C and AHS advising each component, so that even when a component is administered by one entity, the committee overseeing it has members from both. This is essential to assure a good flow of communication and help with translation of research programs and results into routine clinical care.
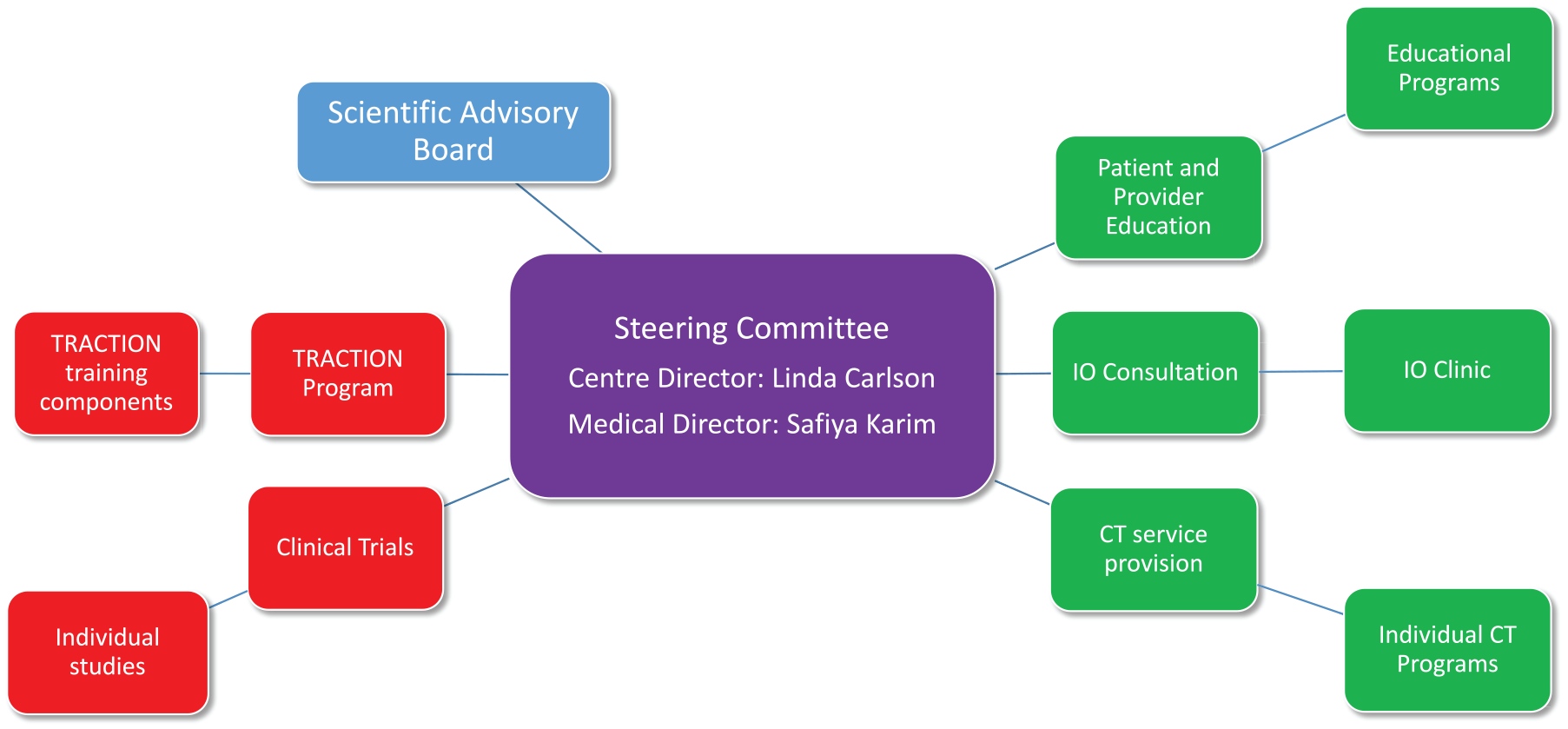
ACTION Centre organizational structure.
For example, in addition to the MATCH study, some research studies currently underway exemplify this approach of designing and evaluating interventions that address clinical gaps or needs, and are operationally efficient and sustainable. ACTION Centre researchers collaborate with operational (clinical) leaders to select study design features and outcome measures that are feasible, clinically meaningful, and inform impact analyses considering the operational costs/benefits for future implementation. Interventions need to be scalable and sustainable, and findings generalizable to broad clinical populations. Some current examples include:
(1) Group acupuncture for cancer pain. We evaluated whether delivering group acupuncture treatments would be as effective as individual administration for treating cancer pain, and what the cost-savings would be. 4 It turned out that group administration was just as effective as individual sessions for pain reduction, at less than half the cost. The next step is to co-develop a business plan for implementation of group acupuncture for cancer pain as part of routine care.
(2) Mobile and online mindfulness programs. In the SEAMLESS study, the ACTION Centre partnered with industry and developed a mindfulness app based on our in-person evidence-based Mindfulness-Based Cancer Recovery (MBCR) program, and are testing it in cancer survivors. 5 If helpful, it could easily and inexpensively be made widely available to cancer survivors across the country. In the ONE-MIND study, we partnered with an online mindfulness company and developed a synchronous video-conferencing adaptation of the MBCR program, and are currently testing whether it can be successfully used by people currently undergoing chemotherapy to prevent the development of common chemotherapy-related side-effects. 6 If successful it could also be made widely available from people’s own homes. The next step if the study shows benefit would be to increase awareness of and access to these programs so they can be integrated into existing models of psychosocial oncology care within Alberta and beyond.
In summary, we believe developing a structure to formally bridge the gaps between academic and publicly funded health care institutions and collaboratively work toward common goals across research, education, and clinical care is a critical step in moving promising evidence-based interventions into practice. Taking direction from patient partners and clinical decision-makers, and involving them in decisions about which CTs to study, and in what modality, further supports implementation and knowledge translation into the community. The ACTION Centre can serve as a model of one way to successfully achieve these ends.
Footnotes
Author Contributions
LEC wrote the first draft of the manuscript; SK and LL edited.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: LEC receives royalties from New Harbinger Publications and American Psychological Association books for book sales, and eMindful.com for online MBCR program sales.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The SEAMLESS study, group acupuncture, and the ONE-MIND study were funded by the Enbridge Research Chair in Psychosocial Oncology, co-funded by the Canadian Cancer Society Alberta/NWT Division and the Alberta Cancer Foundation, held by LEC. The MATCH study is funded by the Lotte and John Hecht Memorial Foundation. The TRACTION program is funded by a CIHR SPOR Mentorship Chair in Innovative Clinical Trials held by LEC. The ACTION centre is partly funded by the Charbonneau Charitable Gift Foundation and the Daniel Family Leadership Chair in Psychosocial Oncology.
