Abstract
Introduction
Prostatectomy for localized prostate cancer (PCa) has a high 10-year survival rate of 90%1,2; however, it negatively affects quality of life (QOL) and is associated with short- and long-term morbidities. 3 We4,5 and others6-8 have shown that physical exercise as an intervention strategy can reduce many adverse effects of cancer treatments such as hormone suppression and radiotherapy. Exercise is now recommended by the American College of Sports Medicine 9 and the American Cancer Society 10 to enhance cardiovascular and musculoskeletal function in cancer survivors, including that for PCa.
For a range of different surgical procedures, exercise prior to surgery is associated with fewer postsurgical complications and shorter hospitalization,11-16 leading to improved health outcomes and reduced health care costs.16,17 To date, the role of exercise prior to prostatectomy has centered on the role of pelvic floor exercises to reduce incontinence. Results from these studies support pelvic floor exercise training prior to prostatectomy,18,19 although incontinence is still a troublesome affliction. 20 However, pelvic floor exercise training does not address other adverse effects such as the loss of muscle mass and reduction in physical function that accompanies surgery and the postsurgical period. Indeed, the decline in muscle mass and physical performance may be quite problematic for those men with already poor physical function prior to surgery. We recently reviewed the literature regarding presurgery exercise training interventions in cancer patients and found that although the majority of studies indicated beneficial effects on function and physical capacity, no studies had been undertaken in PCa patients. 13
Therefore, the purpose of this study was to determine the feasibility of a supervised presurgical exercise program consisting of resistance and aerobic training for men with PCa. Specifically, the primary outcome was to investigate the effects of presurgical exercise on muscle strength 6 weeks following surgery with secondary outcomes of physical performance, body composition, and incontinence.
Methods
Patient Recruitment
A total of 16 patients with localized PCa, not undertaking androgen deprivation therapy (ADT) and scheduled to undergo prostatectomy, were referred between October 2010 and June 2012 to participate in the study. Patients were referred by invitation from their attending specialist at a hospital in Perth, Western Australia, and interested patients then contacted the chief investigator (FS) for further information. Prior to entry into the study, patients were screened by an accredited exercise physiologist. The eligibility criteria included at least 7 weeks between diagnosis of cancer and surgery date to allow time for assessments and 6 weeks of exercise; absence of any acute illness or any musculoskeletal, cardiovascular, or neurological disorder that could inhibit them from exercising; and medical clearance from their general practitioner. Of these 16 patients, 2 men did not meet the inclusion criteria, resulting in 14 eligible patients being invited to participate. Four declined to participate in the study citing traveling from their residence to the University exercise clinic, where training and assessments would take place, as a barrier to participation. The remaining 10 men entered the exercise program and completed all aspects of the study. The study was approved by the University Ethics Committee, and all participants provided written informed consent. Patients completed assessments undertaken at baseline, prior to surgery, and at the 6-week postsurgery follow-up.
Exercise Intervention
Patients undertook two 90-minute supervised sessions per week at the university’s exercise clinic. A home-based activity log sheet was also provided at baseline, and this was monitored weekly throughout the exercise intervention. Patients were encouraged to exercise more than the recommended amount, 9 though this was not enforced. Sessions commenced with a 5-minute warm-up consisting of moderate-level aerobic exercise and stretching. This was followed by a progressive resistance training program that targeted the major upper- and lower-body muscle groups and included the chest press, seated row, latissimus pull-down, leg press, leg extension, and leg curl exercises. Participants performed 2 to 4 sets per exercise at 6 to 12 repetition maximum (RM) intensity (6-12 repetitions per set). Sessions also included 3 trunk stabilizing exercises: plank (all front abdominal muscles), reverse bridge on a Swiss ball (erector spinae muscles), and side plank (both oblique muscles), 21 consisting of 3 sets of 10 to 30 s, with a rest of 30 to 60 s between sets, and the training load increased progressively. 22 Aerobic exercise was undertaken for 20 minutes at an intensity of 60% to 80% of estimated maximum heart rate and included activities such as walking or jogging on a treadmill, and cycling or rowing on a stationary ergometer. The session concluded with a cool-down period of stretching activities. All sessions were conducted with one-on-one supervision by an accredited exercise physiologist who ensured safety and adherence to correct lifting techniques.
Muscle Performance
Dynamic muscle strength for the seated row, chest press, leg press, and leg extension exercises was assessed using the 1-RM method, which is the maximal weight that can be lifted once with correct technique. 23 To assess muscle endurance, the maximal number of repetitions performed at 70% of the baseline 1-RM of chest press and leg press were used. 24 Muscle endurance scores for presurgery and postsurgery assessments were determined using the baseline load. Both muscular testing protocols have been shown to be reliable and valid. 25
Physical Performance
A battery of tests was used to assess physical performance 26 and included usual and fast 6-m walk, 6-m backward walk, repeated chair rise, stair climb, and 400-m walk as a measure of cardiorespiratory fitness. Tests were performed in triplicate, except for the 400-m walk, which was performed once.
Body Composition
Total body lean mass (LM), fat mass (FM), and percentage fat were assessed by dual-energy X-ray absorptiometry (Hologic, Discovery A, Waltham, MA). In addition, regional tissue composition was determined by manipulation of the segmental lines according to specific anatomical landmarks, 27 with appendicular skeletal muscle calculated from the sum of upper- and lower-limb LM. 28
Incontinence
The definition of urinary incontinence was according to the International Continence Society guidelines 29 and defined as a total increase of 8 g or more in one or more pad(s) during a 24-hour pad test. This test is based on the normal value ranges in older men who had not undergone any urological procedure, as detailed by Moore et al, 30 and has been used in a number of clinical investigations.31,32 The 24-hour pad test was conducted at the postsurgery time point, with the weight of urine loss calculated (Used pads − Preweighed pads). The International Consultation on Incontinence Modular Questionnaire (ICIQ) for men was used to self-assess urinary incontinence. 33 The severity of urinary incontinence—slight (1-5), moderate (6-12), severe (13-18), and very severe (19-21)—was based on the work by Klovning et al. 34
Other Measures
Height and body weight were measured using a stadiometer and electronic scales, respectively, and body mass index (BMI) calculated as weight in kilograms divided by height in metres squared (kg/m2). Total cholesterol, high-density lipoprotein, low-density lipoprotein, and triglyceride levels were measured commercially by an accredited Australian National Association of Testing Authorities Laboratory (Pathwest Diagnostics, Western Australia) as standard baseline measures. Self-reported physical activity was assessed with the Leisure Score Index of the Godin Leisure-Time Exercise Questionnaire. 35
Statistical Analysis
Data were analyzed using the IBM SPSS statistical package (PASW v 19, SPSS, Chicago, IL) and included standard descriptive statistics, paired Student’s t-tests, and repeated-measures ANOVA. An intention-to-treat approach was used with a last-observation-carried-forward procedure for any missing data. 36 Post hoc Bonferroni adjustment was used to locate the source of significant difference. The effect size (ES) was calculated as ES = [(MeanPost − MeanPre)/SDPre] and defined as small (d = 0.2), medium (d = 0.5), and large effect (d ≥ 0.8). 37 We aimed to detect a medium standardized effect. Tests were 2-tailed, with an α level of P ≤.05 required for significance.
Results
Patient Characteristics and Adherence
Baseline characteristics are presented in Table 1. The men were aged 59 to 77 years old, with a prostate-specific antigen (PSA) level of 2.1 to 13 ng/mL. Mean time for the 10 patients from diagnosis to surgical resection and to postsurgery follow-up was 176 ± 196 days and 42 ± 7 days, respectively. The long presurgery waiting period was largely driven by one patient’s waiting time of 708 days resulting from a medical costing issue. Consequently, the median time between diagnosis to resection was 114.5 days. Adherence to the exercise program was moderate, with half the patients completing more than 80% of the 12 training sessions and only 1 missing more than 6 sessions. There were no adverse effects or health problems noted.
Patient Characteristics (n = 10).
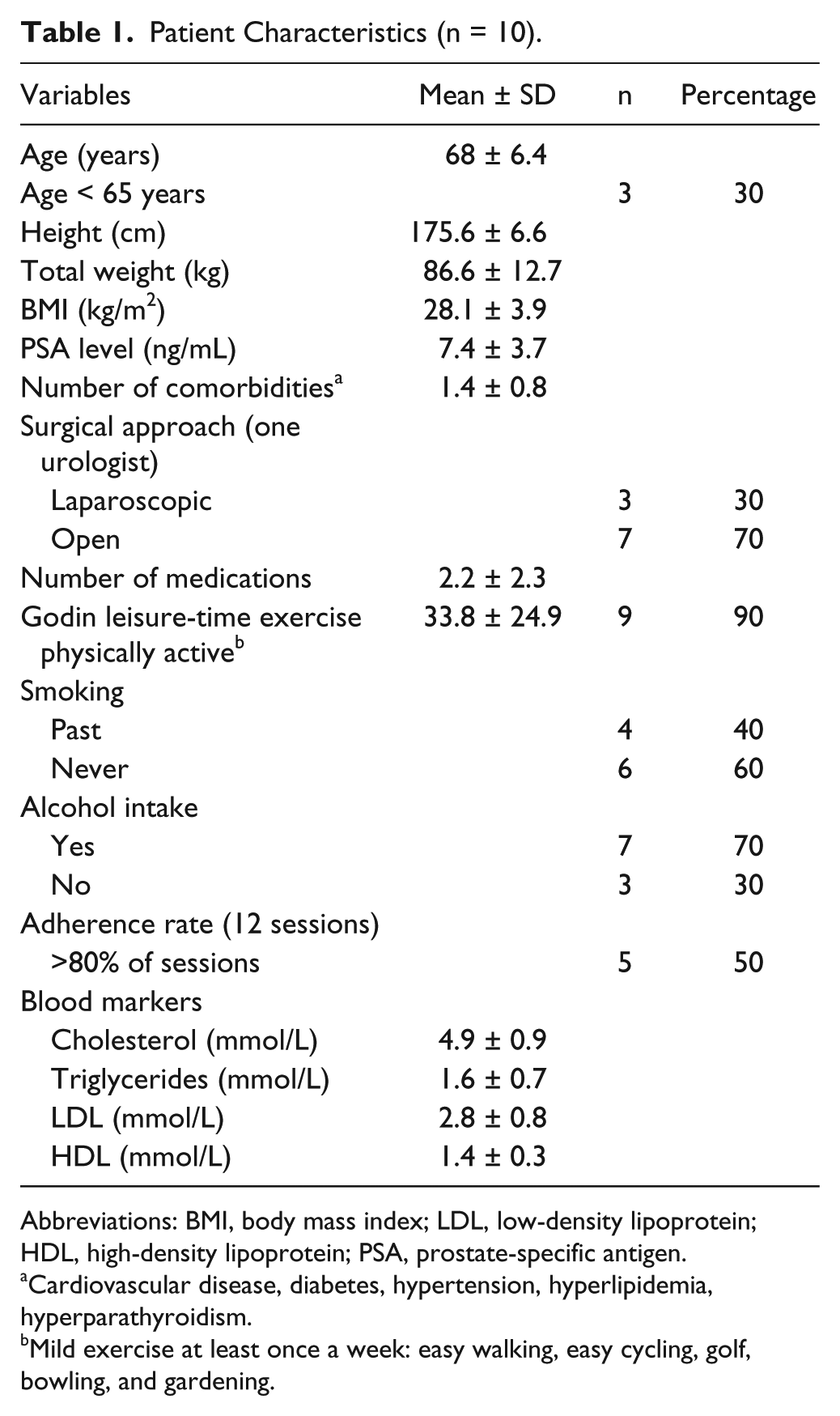
Abbreviations: BMI, body mass index; LDL, low-density lipoprotein; HDL, high-density lipoprotein; PSA, prostate-specific antigen.
Cardiovascular disease, diabetes, hypertension, hyperlipidemia, hyperparathyroidism.
Mild exercise at least once a week: easy walking, easy cycling, golf, bowling, and gardening.
Muscle Performance
Patients significantly increased muscle strength (P < .05) for all resistance exercises from baseline to presurgery (Table 2). However, between presurgery and postsurgery, muscle strength decreased for the seated row and leg press (P < .05), such that postsurgical values did not substantially differ from baseline values. There was some improvement in muscle endurance presurgery, although it was not statistically different from baseline, and postsurgery values did not substantially differ from baseline.
Muscle Function and Physical Performance Absolute Values and Change Over the Presurgical and Postsurgical Study Period.
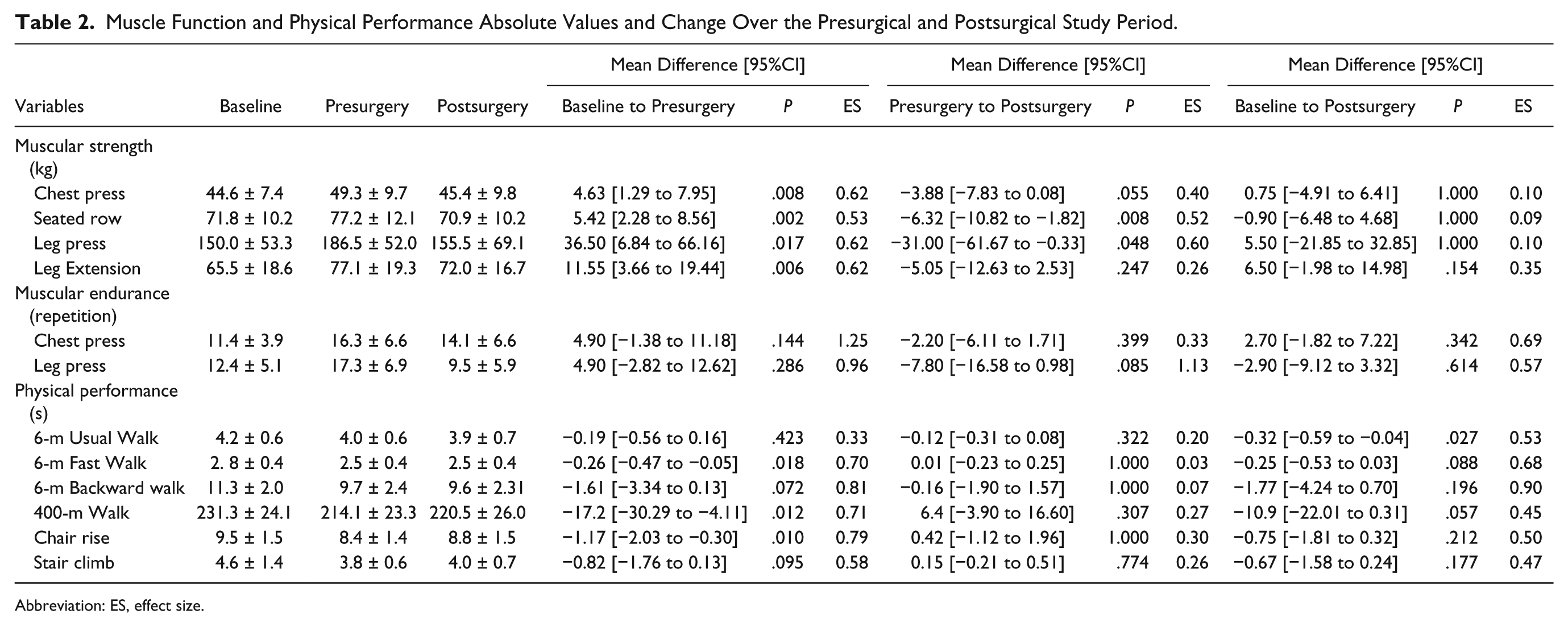
Abbreviation: ES, effect size.
Physical Performance
Following the 6-week training period, there was a significant improvement (P < .05) in the 6-m fast walk, 400-m walk, and repeated chair rise test, whereas change in the 6-m backward walk and stair climb approached significance (P < .10; Table 2). Improvements in physical performance prior to surgery were largely maintained postsurgery, with no significant difference for any test. When compared with baseline, postsurgical performance values were not statistically different except for the 6-m walk, which remained significantly faster (P = .027; Figure 1).

Comparison of walking speed (m/s) at baseline, presurgery, and postsurgery. *Significantly different from baseline; P < .05.
Body Composition
There was no change in whole body or regional LM and FM prior to surgery; however, LM significantly decreased by 2.7 kg following surgery (P = .014), and this was significant for both the upper and lower limbs and, consequently, appendicular skeletal muscle (Table 3). Similarly, when compared with baseline, all postsurgery LM results were significantly reduced (P < .05), with no significant change for whole body or regional FM.
Body Composition: Absolute Values and Change Over the Presurgical and Postsurgical Study Period.
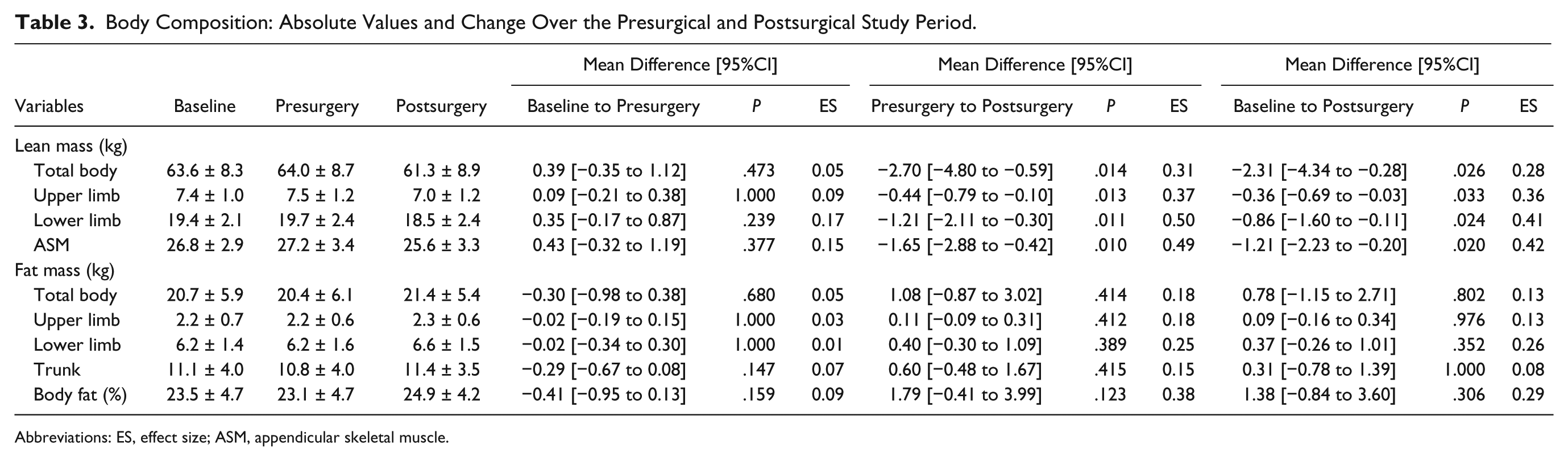
Abbreviations: ES, effect size; ASM, appendicular skeletal muscle.
Incontinence
Mean urinary loss at 6 weeks postsurgery was 226 ± 343 g. Based on the ICIQ, 1 patient had slight urinary incontinence at baseline while at presurgery, 1 had slight and 1 had moderate severity of incontinence. However, at postsurgery the number of men with slight, moderate, and severe self-reported urinary incontinence was 4, 3, and 3, respectively.
Godin Leisure-Time Exercise Questionnaire
There were no significant differences for any of the Godin leisure-time scales across the study (Table 4).
Self-reported Physical Activity at Baseline, Presurgery, and Postsurgery.

Abbreviation: ES, effect size.
Godin leisure-time exercise questionnaire.
Discussion
This study was undertaken to examine the potential feasibility of presurgical exercise in men with PCa scheduled to undergo prostatectomy. We found that it was possible to recruit men with localized PCa to undertake a short-term program of aerobic- and resistance-based exercise prior to surgery and that the program could be undertaken with a moderate adherence rate (half of the men completed all prescribed exercise sessions) and without any adverse effects. Moreover, as a result of training, we observed 2 important findings: (1) the primary outcome muscle strength was substantially enhanced prior to surgery and (2) the benefits of presurgical training, especially for physical performance, were largely maintained 6 weeks postsurgery despite a significant loss in LM, so that even though patients were in the postsurgical recovery period, their physical performance was comparable to or better than what it was several weeks prior to surgery.
Reduced physical activity among surgical patients represents a considerable health risk38,39; therefore, it is reasonable to assume that increasing physical reserve capacity prior to admission would be associated with an elevated level of physical capacity after surgery compared with if no exercise training had been undertaken. Interestingly, several recent reviews have emerged on the potential of prehabilitation and its ability to not only effectively improve patient outcomes but also contribute to the health economy by reducing length of stay in hospital and readmission rates.16,17,40,41
The prehabilitation time period between diagnosis and surgical resection may be a principal limitation in implementing such interventions for a variety of reasons, including the urgency of the prostate cancer condition, operating facilities, and surgeon availability. It is acknowledged that there will be cases where patients may have a shorter time period between diagnosis and surgery than in the current study. In such cases, implementation of this program may not be feasible. However, in the present study, the median waiting time from diagnosis to surgical resection was 114.5 days. This time period between diagnosis and surgery is an opportunity to introduce targeted exercise programs. Our intention with this protocol was to evaluate the feasibility and benefit of adding an exercise program during this waiting period to enhance their postsurgical functional capacity.
As expected and consistent with our previous work in older adults23,24 and men with PCa undertaking ADT or with prior exposure to hormone and radiation therapy,25,26,42 appropriately prescribed exercise had a beneficial effect on enhancing muscle strength and improving physical performance of patients prior to surgery. Following only 6 weeks of twice-weekly training, muscle strength significantly improved by ~8% to 24% depending on muscle group. Given that there was no significant change in regional or whole body LM, the improvements in muscle strength were most likely the result of neural adaptations to training.11,15 Postsurgery, muscle strength decreased; however, it must be noted that strength values remained comparable to those at baseline, despite patients being in the postsurgical period (accompanying bed rest and reduced physical activity) and losing ~2.5 kg of LM.38,39 Given the loss of LM postsurgery and the loss of strength that accompanies reductions in muscle mass, the effect of exercise prior to surgery is to increase the patients’ reserve capacity, thereby, providing a buffer to the detrimental effects of surgery and the postsurgical period.
Importantly, improvements in muscle strength prior to surgery were accompanied by improvements in physical performance, such as chair rise ability and 400-m walk time, and these improvements in performance were maintained 6 weeks postsurgery. The improvements in physical performance following training are comparable with previous research in healthy older adults23,24 and in men with PCa undertaking ADT.25,26 However, retention of these benefits 6 weeks following prostatectomy is an important finding and highlights the potential beneficial role of presurgical exercise or prehabilitation in the maintenance of a minimum level of functional ability postsurgery compared with that expected in nonactive persons.38,39 This may be especially important for men who are close to the functional thresholds for performing activities associated with independent living, thereby prolonging independence and maintaining QOL.
From presurgery to 6 weeks postsurgery, there was a substantial reduction in regional and whole-body LM and an increase in FM, albeit not significant, such that the patients lost approximately 1.5 kg of body weight. The alterations in body composition may be attributed to the combination of bed rest and lack of moderate to strenuous physical activity in the 6 weeks following surgery and, possibly, dietary changes, although this was not tracked. It has been recommended that a presurgical exercise intervention may be an effective way to attenuate and combat this loss in LM. 13 Indeed, with longer duration resistance exercise in community-dwelling older adults, we have found increases of ~1 to 1.5 kg in LM following 6 months of training23,43 as well as modest increases in muscle thickness 26 and LM accretion 25 in men with PCa on ADT following 12 to 20 weeks of training. Taking into consideration the adverse effects of surgery, patients who do not engage in any form of prehabilitative exercise may be disadvantaged in comparison with those who do in the postsurgery period, which may affect their recovery and longer-term functioning.
Prostatectomy is frequently associated with urinary incontinence that has persistent long-term effects. 44 Despite undergoing some form of exercise, incontinence was still prevalent at 6 weeks postsurgery, although 3 of the 10 patients reported only slight incontinence. Biofeedback from exercising and strengthening the muscles of the pelvic floor has been used to develop control and reduce incontinence. 45 Studies have shown that the incidence of incontinence can be reduced through pelvic floor muscle training, which is recognized as a noninvasive treatment for postprostatectomy incontinence18,19,32 and which our participants also undertook as part of their standard care. Although previous research found that isolating the pelvic floor muscles and eliminating abdominal muscle activity was the most effective way to perform these exercises, 46 there is controversy, with some researchers suggesting that to activate the pelvic floor muscles, it is necessary to also activate the abdominal muscles, which may result in higher-intensity pelvic floor muscle contractions.47-49 Therefore, to increase the likelihood of continence in the current study, we included exercises for all the trunk stabilizer muscles. However, given the lack of a control group, we cannot draw definitive conclusions as to the potential beneficial effect of adding resistance training and trunk stabilizer strengthening activities to the standard care of pelvic floor exercises, and this specific area awaits further investigation.
To our knowledge, this is the first study examining the effects of supervised resistance and aerobic exercise prior to prostatectomy. Nevertheless, our study has several limitations that are worthy of comment. First, this feasibility study did not use a randomized controlled trial design, which would have provided the best level of evidence. However, it is important to note that some of the patients suggested that they would not have complied with the study if they had been requested to participate in a control group, citing the importance for them to actually exercise. Second, our participants were volunteers for an exercise trial and, as such, are not representative of all men scheduled to undergo a prostatectomy. However, compared with the general population of men of a similar age residing in the same geographical area, 50 they were comparable in terms of BMI and physical function. Moreover, all but one of the participants were physically active based on our classification of undertaking mild exercise at least once a week, with activities such as easy walking, easy cycling, golf, bowling, and gardening; however, they did not meet the recommended guidelines for either vigorous or moderate physical activity. 9 Third, we did not include a long-term follow-up to determine if the benefits of exercise persisted over time, such as 6 months or longer. Fourth, we only had a moderate adherence rate because of the fact that recruitment of these patients was done at a clinic in a hospital that was a 45-minute drive away from the main training facility. Clearly, time spent traveling to an exercise facility is not only a barrier to participation but also a barrier to exercise program adherence. Strategies to counter this need to be incorporated in the design of future exercise programs for this population. In a similar fashion, participation in the program may be enhanced by having a research nurse or study representative on site at the clinic or hospital to discuss the program and answer questions from interested patients. Finally, our feasibility study included a relatively small sample size and the multimodal nature of the program makes it somewhat difficult to disentangle the contribution of each to the study outcomes. Nevertheless, we found that a relatively brief program of supervised resistance and aerobic exercise can be undertaken prior to prostatectomy with a number of improvements primarily in physical function maintained 6 weeks postsurgery. It is important to note that the time period between diagnosis and surgery may be a principal limitation in implementing such interventions. However, this intervening time could provide the ideal window of opportunity to introduce targeted exercise programs.
Conclusions
In conclusion, we found that a relatively brief presurgical exercise program had a significant beneficial effect on muscle strength and physical performance prior to surgery, with benefits in physical performance maintained 6 weeks postsurgery. It would appear that a prehabilitation program in men scheduled for prostatectomy is feasible and may be particularly beneficial for those who are deconditioned and close to thresholds for performance of daily activities by enhancing their reserve capacity. Further study investigating the role of presurgical exercise in a larger cohort of PCa patients that incorporates a control group is warranted to substantiate and extend our findings.
Footnotes
Acknowledgements
There were no external sources of funding or competing interests. The authors would like to thank and acknowledge all participants for their time and contribution.
Authors’ Note
Trial registration: ACTRN12615000731594. Registered June 30, 2015.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
