Abstract
Osteoarthritis is a chronic disease that affects joint cartilage and can cause severe pain and disability. Minor neglected injuries may also result in other diseases that affect daily life. Various attempts have been made to develop wearable auxiliary devices using functional fabrics, but few have simultaneously provided both heat and pressure. Using knitted shape memory alloy (SMA) fabric, a module was manufactured that achieved bending and contraction during operation. An elbow brace that simultaneously provided heat and pressure was developed using this module. Subjective evaluation and measurements of the range of motion (ROM), changes in skin temperature (T sk ), clothing pressure (P c ), and blood flow (F b ) were conducted on the elbow brace while being worn by 10 participants. The multifunctional elbow brace (MFEB) developed in this study generated pressure and heat that increased T sk and P c , ultimately increasing F b . In addition, the ROM of the elbow joint was increased after actuating the elbow brace. Subjective evaluation of the heat and pressure sensation demonstrated its applicability to the human body. We confirmed that the elbow brace had a positive effect on F b and increased the ROM of the joint. These results show the applicability of smart textiles to the development of various wearable devices.
Keywords
Introduction
Osteoarthritis is a chronic disease that affected 330 million people worldwide in 2017. It mainly affects joint cartilage and can cause severe pain and disability.1,2 In particular, minor injuries can lead to osteoarthritis. Neglected injuries can cause persistent pain, tenderness, joint swelling, joint deformation, and can accompany other diseases, affecting daily life.3,4 Use of braces was suggested in addition to providing partial treatment to prevent the aggravation of symptoms in the early stages of pain. 5
Recently, applications ranging from functional clothing to health devices and health clothing have been developed utilizing the various advantages of functional fabrics. Several approaches to compression clothing have emerged. An optimal level of compression for athletic performance was achieved, which was ascertained through EEG analysis while wearing compression pants at various pressures, and high-pressure compression pants had a positive effect on cycling exercise capacity.6,7 Further, Atkins et al. and Engel et al. suggested that compression clothing worn by athletes appropriately affected body temperature during physical activities and had a positive effect on delaying the occurrence of muscle fatigue, which can cause pain in the lower extremities after exercise.8,9 Xiong and Tao described various types of functional compression clothing and their potential applications, which included the management of venous diseases, such as swelling, scar management, joint support, sportswear, and body shaping. 10 They also advocated for research into self-deformable materials and body part pressure standards. In addition, studies related to the thermal function of clothing included analyzing the winter performance of vest and knee protectors that incorporated electrical and chemical heating 11 and clothing capable of infrared radiation using the physical properties of graphene, which could improve skin temperature (T sk ) in a cold environment.12,13
Wearable devices for pain relief have also been developed. These include a wrist-wearable elastic heat exchange-based heater using silver nanowires with a mesh structure with potential application in large range of motion (ROM) human joints 14 and a bandage incorporating polyurethane that could simultaneously provide heat and pressure. 15 Furthermore, studies have been performed on the effect of wearable electronic fibers on knee pain reduction in patients with osteoarthritis, 16 the relief of and recovery from muscle fatigue and pain using far-infrared devices,17,18 and post-exercise muscle pain relief characteristics and joint ROM associated with wearable vibration devices. 19 However, development of fabric-type wearable assistive devices that provide both heat, and pressure is limited.
Shape memory alloys (SMAs) are intelligent materials with structures that transform into a required shape through a phase change owing to temperature changes. This effect has led to the use of SMAs in various applications, including mechanical materials, actuators, and prosthetic medical devices. 20 Early attempts at applying SMAs to wearables were mainly focused on implementing various types of fabric movement through the application of the SMA to woven fabrics.21–23 Since then, various studies on combining the deformation characteristics of SMAs and the characteristics of knitted structures have been conducted. Granberry et al. proposed an orthostatic hypotension prevention support using the gradient structure present in an SMA knitted structure for wearing on the calf. 24 On this basis, they developed a functional SMA knitted actuator that fitted itself according to the flexion of the human body. 25
Recently, various studies have been conducted on muscle strength enhancement devices using SMAs. These include a wrist-worn strength assist device incorporating a polymer tube and an SMA coil spring, 26 an arm muscle assist device equipped with an SMA actuator incorporated into a fabric structure, 27 and an SMA-based wearable ankle aid. 28 Various studies have also been conducted on the actuation characteristics of SMAs, involving approaches such as finite element analysis for SMA-based textiles 29 and deformation prediction of SMA knitted actuators. 30 Additionally, attempts to apply SMAs to functional garments, such as protective garments that provide thermal comfort by creating an air gap between fabric layers when exposed to thermal stimuli, were made.31–33 However, research on the application of fabric-type SMAs to the field of health has been insufficient. Regarding the correlation between T sk , clothing pressure (P c ), and blood flow (F b ), Heinonen et al. suggested that localized heating at the calf can increase muscle temperature and F b in the skeletal muscle. 34 Mitsuno and Kai, and Sun and Song confirmed that P c increased F b and also evaluated appropriate P c for each body part.35,36 In addition, a relationship between appropriate P c and F b to the arm has been suggested.6,37
The current research for human pain relief aids is mainly focused on either applying pressure to the human body or providing heat. In contrast, a close evaluation of the application of SMAs to the human body and the body’s response to the effects of SMA has not yet been performed. Therefore, we propose a fabric-type SMA material design method that utilizes Joule heat and force generated during deformation to increase the T sk by simultaneously providing localized heat and pressure to the human body. Hence, a wearable- type multifunctional elbow brace (MFEB) simultaneously providing heat and pressure, is fabricated, and its effect on F b increase is evaluated. Further, human suitability is reviewed through subjective evaluation to determine whether the joint area exhibits improved ROM.
Method
Experimental assumptions
Previous studies have shown that the T
sk
and P
c
affect F
b
(Figure 1).6,34,36 As the T
sk
and P
c
of a person wearing a wearable device increase, the F
b
exhibits an increasing trend (equation (1)) Experimental assumptions: the expected effect on Fb caused by the Tsk and Pc.
The proposed MFEB simultaneously provides heat and pressure to the wearing area. That is, because the F b increases as T sk increases after actuating the MFEB and the F b increases as Pc increases, we hypothesized that the increase in T sk and Pc has a positive linear relationship with the increase in F b . Thus, this device could induce an increase in F b , as hypothesized (Figure 1).
Materials
Shape memory alloy wire (DYNALLOY, Inc., USA, 55 wt% Ni and 45 wt% Ti, diameter = 200 μm, transformation temperature = 70°C) was used in the module constituting the MFEB. The MFEB was produced by wrapping the SMA textile with ordinary fabric (polyester 100%). The deformation temperature of the SMA used was 70°C, and at that temperature, the SMA showed a 4–5% shrinkage in the axial direction. We showed structural shrinkage of up to 21% by implementing axial shrinkage in a knit structure.
The SMA wire was formed into a textile by a knitting expert using a hand-knitting technique. Knitting produces a fabric by repetition of basic units called loops or stitches. Vertical rows of knitted fabric loops are called wales and horizontal rows are called courses. A knitted fabric with only the face loop on one side is a plain stitch (Figure 2(a)) and that composed of alternating face and back loops in the wale direction is a rib stitch (Figure 2(b)).
38
Figure 2 shows the plain and 1 x 1 rib stitches and knitting directions. Han and Ahn confirmed that when the SMA wire is formed into a knitted structure and heat or current is applied, it forms different shapes according to the loops created in each knitted structure.
39
In the case of a plain knitted fabric, it was observed that the head of each loop was bent toward the leg of the plain knitted pattern because the overall wale possessed the characteristic of bending in that direction. It was confirmed that the rib knitted pattern, in which the front and back sides of the loops cross to form a column, demonstrated the characteristic of shrinking in the course direction. Course and wale of the knitted fabric and knitting direction: (a) plain stitch and (b) rib stitch.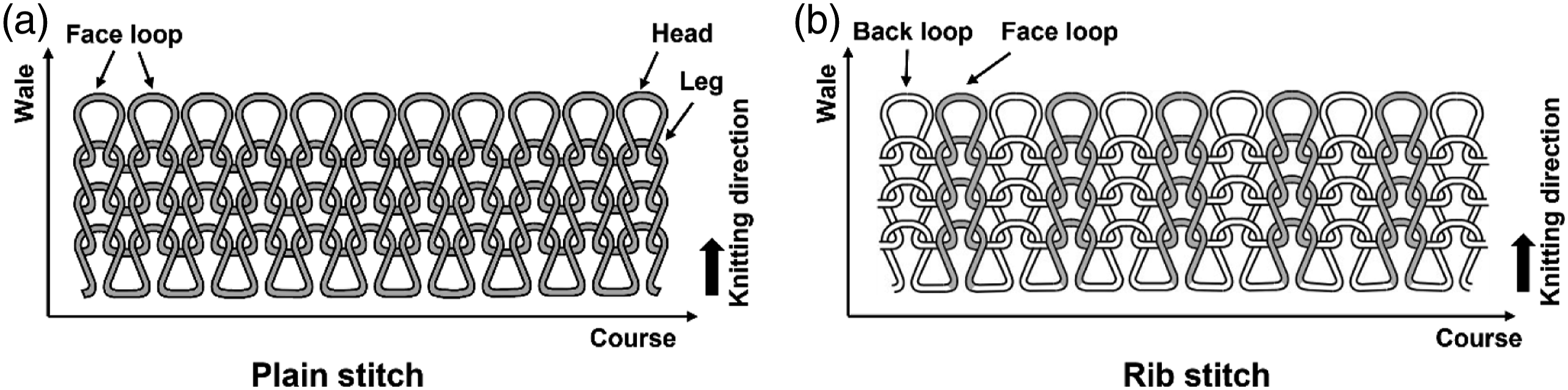
Design and fabrication of MFEB
As the bending and contraction characteristics of the MFEB proposed herein were implemented differently based on the knitting method, a composite module was designed by incorporating different SMA knitted modules to produce a compressive effect on the elbow area. Figure 3 shows the change directions of the knitting modules and the design concept of the knitted SMA composite module to be inserted into the MFEB. The SMA knitted module exerted physical pressure on the area over which it was worn by simultaneously implementing the bending properties of the plain knitted pattern and the shrinkage characteristics of the rib knitted pattern when actuated. Additionally, Joule heating was applied as a thermal effect when the module was deformed at the area on which it was worn. The number of stitches of each knitted module differed according to the application area. The plain knit and the rib knit on the body each incorporated 50 courses and 50 wales, and the plain knit on the straps incorporated 52 courses and 22 wales, whereas the rib knit on the straps incorporated 22 courses and 52 wales. In the body and straps parts, plain and rib knitting modules were inserted in overlapping layers, and the knitting direction of each knitting module is presented in Figure 3(a). Knitted SMA-based MFEB design concept: (a) bending and shrinking directions and (b) composite module.
Figure 4 shows the fabricated MFEB (density = 0.056 g/m2, thickness = 0.41 mm). The outside of the MFEB was covered with neoprene, and the inside (i.e., the area in direct contact with the elbow) was covered with a commercial polyester fabric. The polyester (100% polyester, plain woven, 0.062 g/cm2) was used to cover the module to prevent it from being exposed, and the neoprene (elastic material, elongation = 34.02%, with good recovery) was used to cover the outside of the MFEB because repetitive SMA shape changes may affect the external material. The MFEB was composed of a “body” part that enclosed the elbow area and a “straps” part wrapped around the inner part of the arm (Figure 3(b)). Velcro was attached to the ends of the straps to adjust the MFEB size according to the forearm size (total size of the brace (length × width) was 360 mm × 155 mm, and the size of each strap was 195 mm × 60 mm). Two types of knitted SMA modules were placed in the body and straps. The rib knitted pattern possessing characteristics of shrinking was located at the inner surface of the brace, in the area that made contact with the arm. The plain knitted pattern that possessed the bending characteristic was located at the outer surface of the brace. A power supply control circuit was constructed to electrically actuate the MFEB. A case was manufactured using a 3D printer (FDM 3D Printer, Stratasys F270 (USA)). The completed MFEB (Figure 4(a)) and its actuation by applying a 0.3 A current and 14 V (Figure 4(b)) are shown. Although the SMA has different properties depending on the material combination, the SMA used in this study was able to derive an optimal shape deformation (i.e., actuating force and energy efficiency) when a current of 0.3 A was continuously applied at 14 V. Fabricated MFEB: (a) before actuation and (b) after actuation.
Participants
Demographic characteristics of participants.

SD: standard deviation.
Experimental procedures
The selected participants wore the MFEB, and changes in their biological characteristics were confirmed before and after wearing the device. Before the experiment, participants remained seated for 10 min in a laboratory environment (24°C and RH of 65%) to stabilize the T
sk
and F
b
. The ROM of the elbow before and after the heating and compression actuation of the MFEB was then measured thrice using a digital goniometer (Meloq AB EasyAngle, Stockholm, Sweden) with a position sensor. Figure 5 shows the flexion and extension of the elbow joint, and the ROM is approximately 0°–145°.
40
This method minimized the factors that may interfere with angular measurements made using a passive goniometer.41-43 ROM measurement: (a) measurement angle of the elbow ROM and (b) digital goniometer.
The factors to be evaluated in this study, such as T
sk
, P
c
, and F
b
, were simultaneously measured. Figure 6 shows the experimental setup and the points where the sensors were attached. A wireless thermometry device was used to measure T
sk
(Thermochron iButton® DS1923, Dallas Instrument, USA). The T
sk
sensor was attached to ensure that the MFEB under the upper arm and the inner P
c
sensor two overlapped. For P
c
measurement, a total of four air pack sensors (AMI-3037, Sartorius, Japan) were attached. Two were attached at the center of the areas where each brace was worn on the upper and lower arms. These were based on the elbow joint’s anterior and posterior areas in the joint’s supination state. A non-invasive method that measured the amount of skin F
b
using the laser Doppler effect was employed. The F
b
sensor was attached to the tip of the middle finger of the right hand (MoorVMS-LDF2, Moor Instruments Inc., UK).
44
Experiment setup: (a) participants in the experiment and (b) regions the sensors attached.
Measurements were performed in the following two stages: stage 1, wearing the MFEB; and stage 2, actuating the MFEB (Figure 7). The participants were seated in a comfortable position with their right arm placed on a desk. The six indicators were then monitored for 1 min before wearing the MFEB. Thereafter, the MFEB was worn, and measurements were performed for 5 min before actuation (Stage 1). After actuation, measurements were performed for a further 10 min (Stage 2). Stage 1 is the body vital stabilization time (baseline state), and Stage 2 is the operating time of the MFEB (i.e., the time when the knitted SMA module is fully driven under 0.3 A and 14 V conditions). According to a previous study,
45
we judged that 10 min was an appropriate time to apply thermal therapy. Finally, after removing the MFEB, we measured the ROM of the elbow joint thrice as previously described. The subjective evaluation of heat and pressure effects was conducted by administering a questionnaire 9 min after actuating the MFEB (ISO 10551 2019).
46
We used questions of thermal perception and preference, which are frequently used in subjective thermal evaluations, and added a question on pressure comfort (Table 2). We analyzed the differences between each experimental result with an independent sample t-test using SPSS 25.0 (IBM, Armonk, NY). The significance level was set at p < .05. Experimental procedure. Inquiry and assessment scale for subjective evaluation.

Results
Changes in T sk
Figure 8 shows the changes in the T
sk
of the area where the MFEB was worn during the experiment. For 1 min after attaching the sensor, the average T
sk
was 31.7 ± 0.1°C. It gradually increased from at least 31.9°C to a maximum of 33.2°C for approximately 5 min after wearing the MFEB (stage 1). When the MFEB was being actuated (stage 2), the T
sk
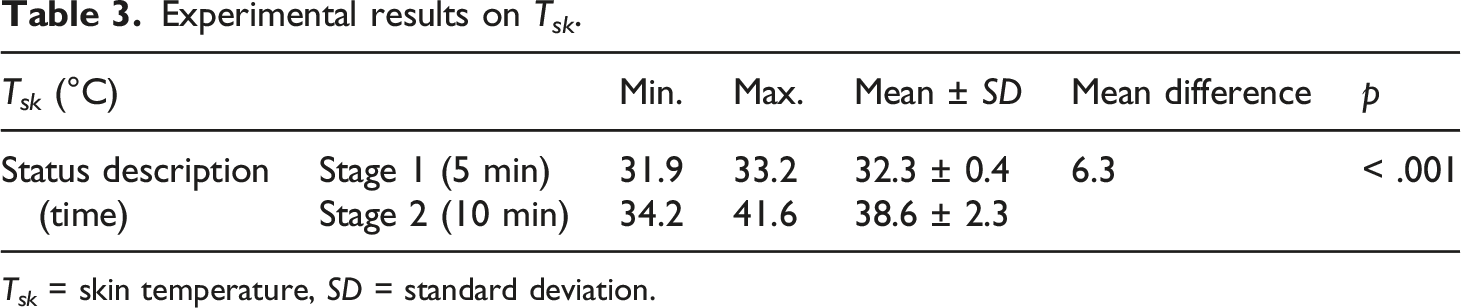
continued to increase up to 41.6°C. Table 3 shows the mean and specific mean differences of stages 1 and 2. A mean difference of 6.3°C was observed between the temperatures when wearing the MFEB and actuating it, which was statistically significant when actuated (p < .001). This indicates that the Joule heating during MFEB actuation raises the T
sk
. Changes in T
sk
during MFEB wearing and actuating experiments. Experimental results on T
sk
. T
sk
= skin temperature, SD = standard deviation.
P c changes
Figure 9 shows the changes in the mean P
c
for each sensor, which was measured as 0 kPa (error range ± 0.06 kPa) for 1 min after attaching the four sensors, which was the stabilization period. After the MFEB was worn (stage 1), the P
c
immediately increased and then decreased again. It can be considered that the increase was as a result of the process of wearing the MFEB and the decrease was as a result of stabilizing after wearing the MFEB. When actuating the MFEB (stage 2), the P
c
of all four sensors increased and the average values of P
c
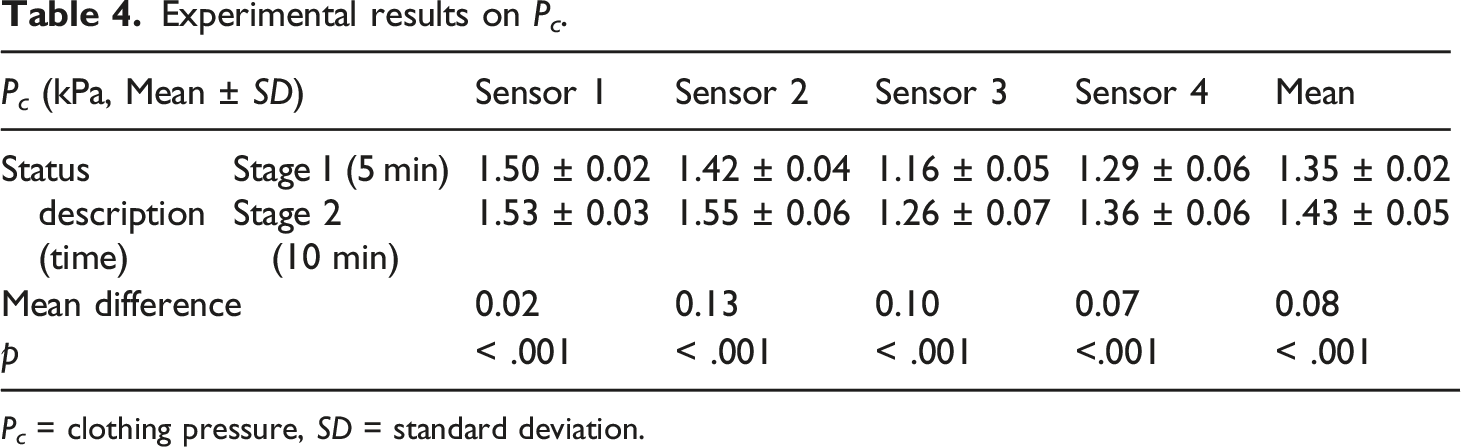
gradually increased by 5.59% (Table 4). We presented the average value of the four sensors because we ultimately tried to determine how the MFEB affects the ROM of the joint. Further, the mean difference of each P
c
between wearing the MFEB and actuating was significant (p < .001). Thus, after actuation, each P
c
increased as the knitted SMA modules in the MFEB shrunk and bent. Changes in the mean Pc during MFEB wearing and actuating experiments. Experimental results on P
c
. P
c
= clothing pressure, SD = standard deviation.
F b changes
The average F
b
was 127.14 ± 8.53 mL/100 g for 1 min after attaching the sensor; however, after wearing the MFEB, it fluctuated for 5 min in the range of 125.10–147.60 mL/100 g (Figure 10). When the MFEB was being actuated, the F
b
fluctuated more vigorously than when simply wearing it (wearing vs. actuating = 15.24% vs. 28.07%); finally, it reached a maximum of 186.54 mL/100 g. An additional increase was also observed as a result of actuating the MFEB. Table 5 shows the specific differences in F
b
at each stage. The average difference between F
b
when wearing and actuating the MFEB is 13.04 mL/100 g, which was statistically significant, that is, the F
b
when actuating the MFEB increased by 8.49%. Thus, it was confirmed that both P
c
and F
b
increased as a result of wearing the MFEB. Changes in F
b
during MFEB wearing and actuating experiments. Experimental results on F
b
. F
b
= blood flow, SD = standard deviation.

ROM and subjective evaluation
Experimental results on ROM.

ROM = range of motion, SD = standard deviation.
Figure 11 shows the results of the heat and pressure related subjective evaluation of each participant approximately 9 min after MFEB actuation, at which the temperature was maintained at the highest level (Table 7). The evaluation score for the thermal perception question “How do you feel about the temperature at this moment?” was 2.30 ± 0.49, which was between “warm” (score = 2) and “hot” (score = 3). Thus, the participants felt that the elbow area was warm or hot when the MFEB was actuated, and seven out of 10 participants perceived it as warm. The score of the question regarding thermal preference “What temperature do you prefer to be at this moment?” was −0.40 ± 0.49, which was between “neutral” (score = 0) and “slightly cooler” (score = −1). Six out of 10 participants answered “neutral,” indicating a preference for the current state of wearing the MFEB or a slightly cooler state. Furthermore, the score for the question regarding pressure comfort “How do you feel about the pressure?” was −1.70 ± 0.46, which was between “comfortable” (score = −2) and “neutral” (score = −1). Seven out of 10 participants answered “comfortable,” while the other three answered “neutral,” indicating a comfortable compression on the elbow area. Thus, even in the subjective evaluation, the heat and pressure applied by the MFEB are acceptable. Subjective evaluation results of each participant: (a) thermal perception, (b) thermal preference, and (c) pressure comport. Experimental results on subjective evaluation. SD = standard deviation.

Assumption verification for Tsk, Pc, and Fb
We normalized the values of T
sk
, P
c
, and F
b
in the states of wearing and actuating the MFEB to a common scale (Figure 12). Figure 12(a) shows the change over the total time measured as a cubic trend line. P
c
gradually decreases after wearing the MFEB and then increases when actuation begins, which is presumably because of the MFEB stabilizing as the SMA module adjusts to fit the body. The T
sk
and F
b
showed a tendency to increase throughout the experiment. Correlation between T
sk
, P
c
, and F
b
: (a) changes in MFEB wearing and actuating experiments and (b) gradient comparison of linear equations during actuating MFEB.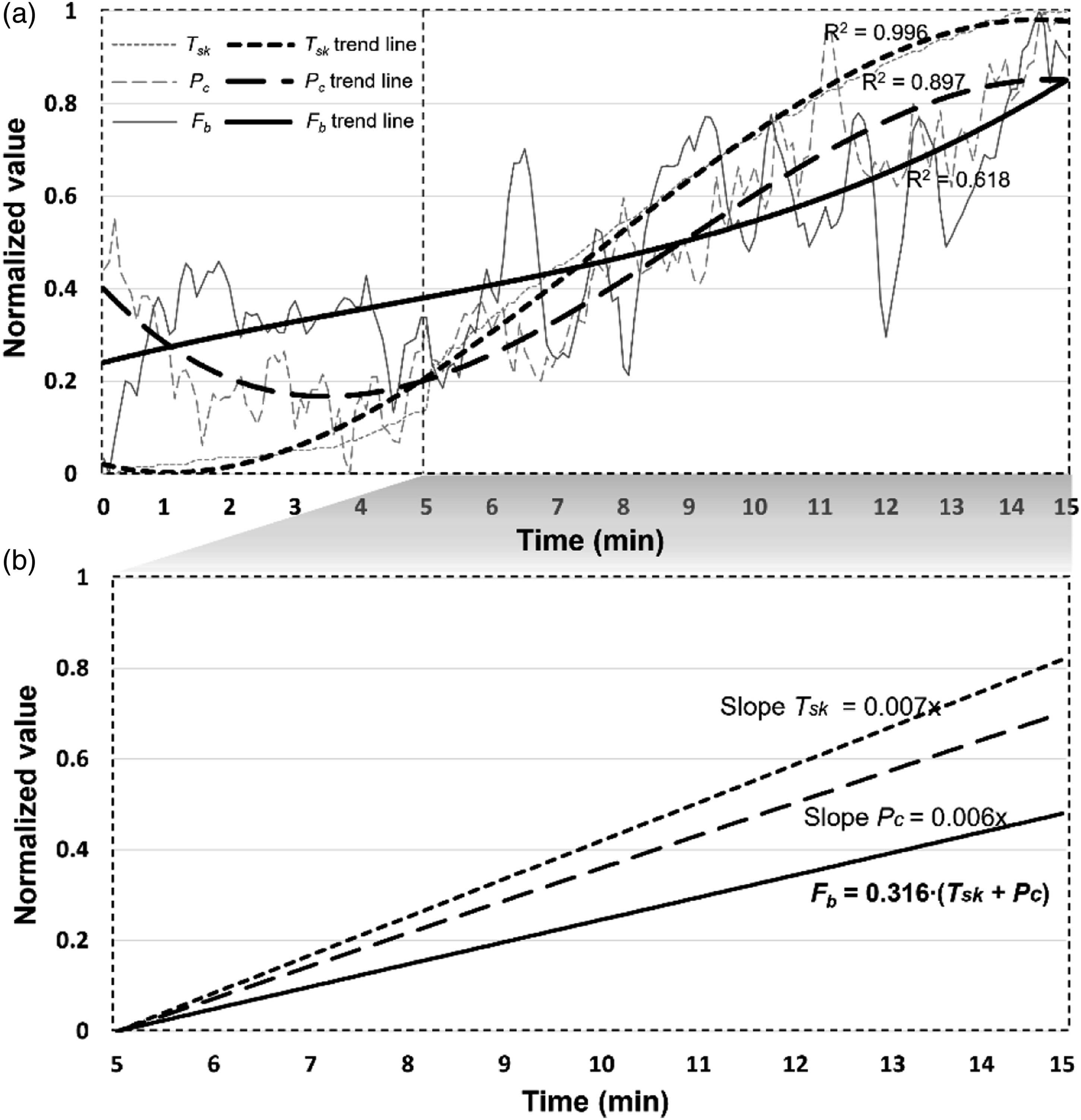
Figure 12(b) represents a reconstruction of the change in the actuating section as a linear equation trend line. The linear increasing trends of T
sk
and P
c
show slopes of 0.007 and 0.006, respectively. Considering equation (1), F
b
can be expressed as equation (2), allowing the correlation of F
b
with the changes in T
sk
and P
c
. Thus, the assumptions set in this study can be accepted
Discussion
Herein, a MFEB was developed using a knitted SMA fabric and applied to the elbow. We confirmed that the bending and contraction deformation and heat generated during actuation of the SMA fabric increased the T sk and P c of the elbow joint and in turn the F b . An appropriate increase in the T sk and P c leads to a positive effect on the human body, suggesting the viability of this knitted SMA fabric as an effective wearable.
The heat generated during SMA actuation increased the T sk , reaching a maximum of 41.60°C during the 10 min period. In terms of pain treatment, 8–30 min is a significant treatment regimen time 14,46,47; thus, we recommend applying the MFEB in the form of heat therapy for 10 min to treat pain. In addition, when the MFEB was actuated, localized heating of the elbow increased the T sk of the arm, which was effective in significantly increasing the F b . These results supported those of Heinonen et al., who suggested that localized heating of the calf can increase skin F b , similar to when the whole body is heated. 34 Further, increased F b through this thermotherapy may relieve joint pain by increasing the delivery of nutrients and oxygen. 48 Recently, the effectiveness of thermal treatment, such as pain reduction by increasing local blood circulation,17,18 has been demonstrated; however, the focus was on proving the effectiveness of heat and not a wearable device.
When the MFEB was actuated, the T sk and F b increased by 16% and 8%, respectively. This indicates that the MFEB can provide effective thermal therapy while serving as a new wearable material for thermal and compression therapy. Although it was not statistically significant, the ROM of the joint slightly increased (approximately 2.40°) after MFEB actuation compared to before actuation. Heat supplied through various methods such as infrared, hot packs, and electric heating pads can increase ROM, serving as an effective adjuvant in therapeutic stretching techniques.14,47,49 As an example of heat therapy, the SMA module in the MFEB represents one of the rehabilitation treatment regimens used for increasing the limited ROM of the joint, which can relax the joint especially in painful areas.
The P
c
immediately increased after wearing the MFEB and appeared to decrease for 5 min after it was worn as the MFEB stabilized. Then, the MFEB was actuated and the P
c
gradually increased. This is because the MFEB is bent slightly inward owing to the bending deformation of the plain stitch and the shrinkage deformation of the rib stitch as the SMA module is actuated. Similar functionality as that of various functional compression clothing items developed in previous studies that increased F
b
in the human body simply by wearing them could be achieved by our MFEB.8–10 Notably, even though the increase in the average P
c
was only 0.08 kPa (1.35 kPa when the MFEB was worn to 1.43 kPa when actuated), the increase in skin F
b
was 8.49%. This was within the appropriate range (1–2 kPa) of the arm region.
35
As such, our study suggests that an elbow brace with multiple functions (i.e., heat and pressure) would be appropriate in terms of the human suitability and safety of healthy people. Furthermore, based on the results of this study, we intend to apply it to people with joint pain of various ages in the future. Figure 13 shows the expected relationship between the ROM and pain reduction due to the effect of the T
sk
, P
c
, and F
b
. Relationship with ROM and pain reduction due to the effects of Tsk, Pc, and Fb.
Furthermore, the results of the subjective evaluation of heat and pressure were also within an acceptable range. Figure 14 shows the gender differences in the subjective evaluation results for thermal perception, thermal preference, and pressure comfort. The optimal temperature for thermotherapy was recommended to be approximately 40–43°C.
46
More women felt “Hot” than men in regard to thermal perception, and more women selected “Slightly cooler” regarding thermal preference. Hwang et al. and Lan et al. (2008) have noted a difference between genders regarding thermal perception and preference, which may be attributed to women being more sensitive to temperature than men.50,51 Thus, it is considered necessary to allow for temperature control based on the wearer. The response to pressure comfort also demonstrated gender differences, and women were slightly more comfortable than men. Gender differences in subjective evaluation results.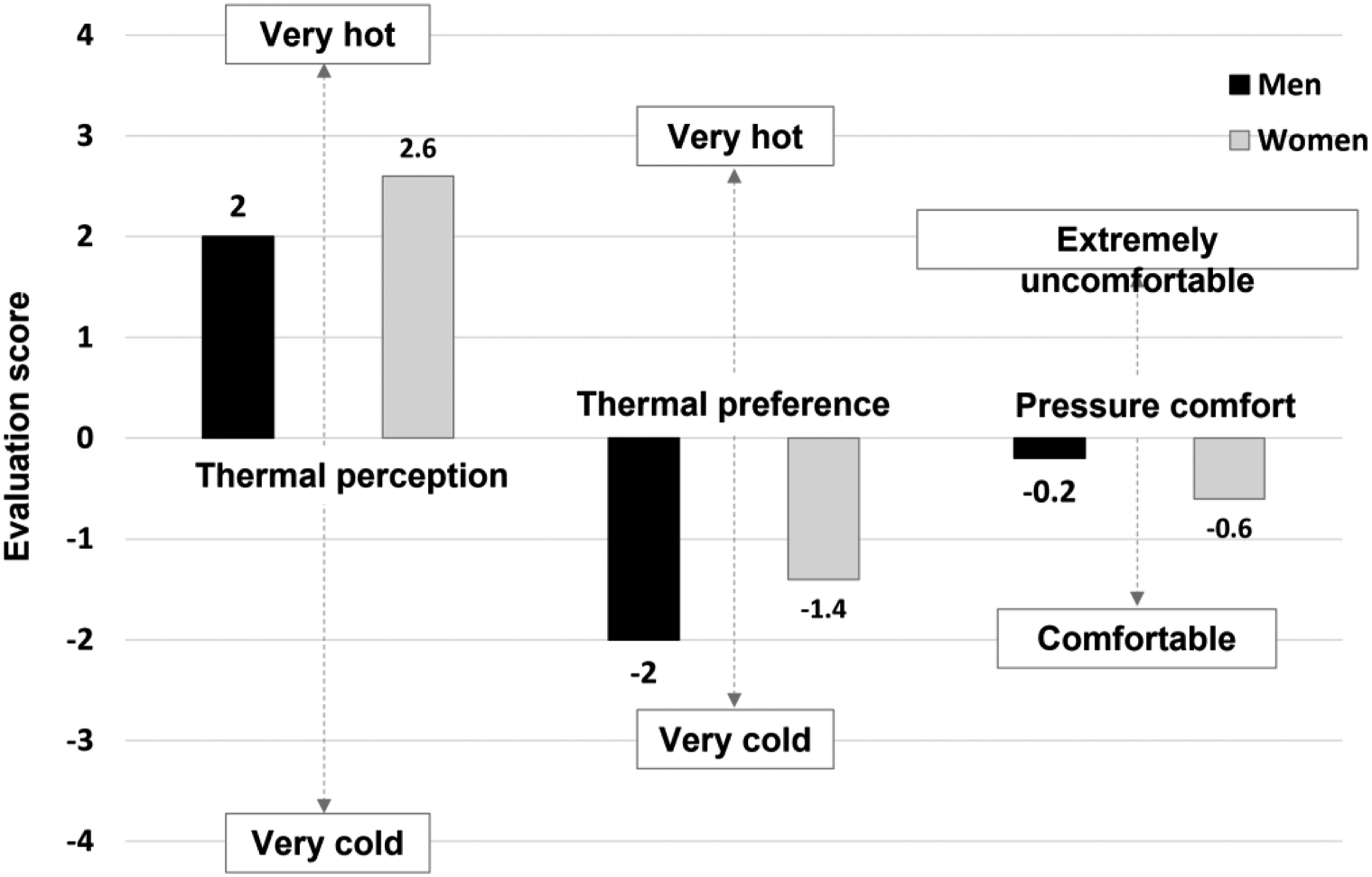
In addition, various factors such as the muscle mass and skin thickness at the application site may affect the results. Appropriate P c at the arm differs from that at other body parts.35,37 Thus, it is necessary to analyze the degree of bending and contraction of the SMA module associated with changing the number and size of knitted loops to produce modules suitable for the body part to which it is applied. Though we performed repeated actuating experiments on the simple actuator using the SMA to verify the continuity of the performance, in future work, we will verify durability by analyzing, for example, washing to increase usability.
Conclusions
We developed a MFEB that can knit modules with different actuation characteristics by simultaneously applying heat and pressure using a hand-knitted fabric incorporating SMA wires. This study suggests that the MFEB can be used as a device for the treatment of pain by providing 0.3 A (14 V) to actuate the SMA; a pressure of approximately 0.12 kPa for 10 min and a thermal effect of 40°C are simultaneously provided to improve F b by 8.49%. We compared the ROM before and after actuating (i.e., before and after applying heat and pressure) in the state of not wearing the MFEB and found that the ROM was increased by approximately 2.4°, which positively affected the improvement. These results can support many previous studies that ultimately show that the MFEB has a positive effect on the body by increasing F b and ROM. In addition, the results of the subjective evaluation were within the range applicable to the body.
This study is the first attempt to evaluate human suitability for the simultaneous effects of heat and pressure in the study of wearable devices using SMA and can provide useful guidance in the design of multifunctional wearable devices using smart textiles that simultaneously implement heat and pressure. In future studies, based on the results of this study, it is expected that the possibility of practical use can be increased through verification of clinical efficacy for osteoarthritis patients in various age groups and analysis of various characteristics and pain treatment effects of MFEB.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korean Government (MSIT) [grant number 2016R1A5A1938472]; and Seoul National University Research Grant in 2021.

