Abstract
Introduction
Nurses play a critical role in hospitals by continuously monitoring patients and responding promptly to emergencies, with most working within a three-shift rotation system, 1 often facing understaffing, excessive workloads, and irregular schedules. 2 Irregular schedules are linked to fatigue, obesity, sleep disturbances, infertility, and miscarriage,3,4 and may disrupt work-life balance and nurse-patient interactions, potentially compromising patient safety.2,5,6 Well-structured schedules, in contrast, improve nurses’ health, job satisfaction, and work-life balance,7–9 enhancing both care quality and nurses’ quality of life. 10 The American Nurses Association emphasizes the importance of equitable workloads and healthy scheduling to ensure safe, high-quality patient care. 11
Nursing scheduling involves planning and allocating work hours to maintain safe staffing and optimal care delivery. 12 Nurse managers must balance staffing levels, competencies, fairness, and organizational needs.13,14 However, perception gaps often exist between schedulers and staff, as personality, family status, and individual preferences make it challenging to satisfy all nurses. Misuse of scheduling authority can lead to perceptions of unfairness, dissatisfaction, and lower morale. 15 Furthermore, inappropriate scheduling has been associated with anxiety, stress, burnout, and sleep disorders, while fatigue and drowsiness reduce concentration, worsen work-life balance, and negatively affect patient safety.2,6,16 Thus, hospitals should regularly monitor scheduling practices and intervene proactively when problems arise.
Efforts to develop equitable and efficient scheduling systems have been reported domestically and internationally. In South Korea, Jeon et al. proposed a scheduling model incorporating various constraints, 17 while Song developed an automated scheduling system using a web-based interface to reflect nurse preferences. 18 Internationally, preference-based scheduling systems in Egypt and India have demonstrated economic and operational benefits by reducing overtime and shortening scheduling time.19,20 Nonetheless, most automated systems still rely on rule-based or preference-matching approaches, requiring substantial manual adjustments and limiting scalability and workflow integration. 21 Many commercial systems operate as standalone applications, making real-time linkage with hospital information systems challenging and thus limiting dynamic schedule updates. 22
Artificial intelligence (AI) and robotic process automation (RPA) remain underutilized in nurse scheduling. RPA automates repetitive tasks, enhancing fairness and accuracy, 23 reducing manager workload, and improving satisfaction. 24 Moreover, integrating RPA directly into hospital information systems can substantially reduce administrative task time and errors. 22 Compared to traditional automated or preference-matching approaches, RPA provides clear advantages, including direct data extraction, automated staffing-guideline checks, schedule generation without extensive system redevelopment, reduced administrative burden, and easier integration with existing hospital workflows. 22
In South Korea, the Ministry of Health and Welfare has implemented policies to improve shift work conditions, including the “Night Nurse Pay” program and the “Guidelines for Nurses’ Night Work.” 25 The Nurse Shift System Improvement Pilot Project, initiated in 2022, requires hospitals to implement predictable shift schedules and meet specific staffing requirements for night-duty nurses, with financial support provided based on compliance. 26 These policies highlight the importance of adhering to scheduling criteria and the need for research on effective implementation strategies.
Given the complexity of nurse scheduling and ongoing efforts to improve working conditions, this study aims to develop and implement an RPA-based nurse staffing program directly integrated into routine workflows. Building on previous systems’ limitations, this study evaluates the program’s impact on nurses’ work characteristics, health status, and work-life balance, providing foundational evidence to inform future workforce strategies.
Research hypotheses
• Hypothesis 1: There is no significant difference in work characteristics between the experimental group, where the nurse staffing program using RPA is implemented, and the control group. • Hypothesis 2: The experimental group working in a unit where the nurse staffing program using RPA is implemented shows better health status compared to the control group. • Hypothesis 3: The experimental group working in a unit where the nurse staffing program using RPA is implemented shows better work-life balance compared to the control group.
Methods
Design
This interventional study employed a non-equivalent control group pretest-posttest design to develop a nurse staffing program using RPA, implement it among nurses, and evaluate its effects on work characteristics, health status, and work-life balance.
Study sample
The study was conducted at a general hospital, participating in the Integrated Nursing Care Service Wards and the Nurse Shift System Improvement Pilot Project. Two general wards, two Integrated Nursing Care Service Wards, and two Intensive Care Units (ICUs) were randomly selected from six general wards, six Integrated Nursing Care Service Wards, and four ICUs. Nurses from these wards were recruited via convenience sampling and assigned to experimental or control groups. Data were collected from November 15, 2023, to June 30, 2024. The sample size was calculated using G*Power 3.1, based on Cohen’s formula for paired t-tests with a medium effect size of 0.5, significance level α = 0.05, and power of 0.95. The minimum required sample size was 54 per group, totaling 108. To meet this, 134 participants were recruited.
Inclusion criteria were nurses with at least 6 months of work experience in general wards, Integrated Nursing Care Service Wards, or ICUs, who were directly involved in patient care. Exclusion criteria were less than 6 months of work experience, assignment to non-clinical roles, extended leave, departmental transfer or resignation during the study period, or incomplete/invalid responses. Consequently, 102 nurses remained and were evenly allocated to the experimental (n = 51) and control (n = 51) groups. Cooperation with the study was facilitated by co-researchers affiliated with the hospital.
Ethical considerations
This study was approved by the Institutional Review Board of the affiliated hospital on August 9, 2023 (IRB No.: MJH 2023-06-048). Participants provided written informed consent after being briefed about the study purpose, confidentiality, voluntary participation, and right to withdraw.
Instruments
A structured questionnaire comprising 72 items was used in this study: 7 on general characteristics, 6 on work characteristics, 30 on health status, and 29 on work-life balance. The tools were used with original authors’ permission.
Work characteristics
Survey questions were developed based on monitoring indicators from the Nurse Shift System Improvement Guidelines (April 2022) and the Guidelines for Nurses’ Night Work (May 2022).25,26 The questionnaire included items on the maximum number of consecutive workdays, total monthly shifts, leave provision after excessive night shifts, number of night shifts per month, rest after night shifts, and consecutive night shifts per cycle. Specifically, it assessed whether consecutive workdays were limited to five or fewer, whether 1 day of leave was granted when designated night shifts exceeded seven, whether at least 48 h of rest was ensured after two or more consecutive night shifts, and whether the number of consecutive night shifts was limited to three or fewer.
Health status
Health status was measured using the 30-item Health Status Scale, developed by Kim, 27 based on the health questionnaire from the University of Tokyo’s Department of Public Health, and later adapted into the Korean version of the Todai Health Index by Lim. 9 The scale includes 10 for the physical domain, 7 for the psychological domain, 3 for the spiritual domain, and 10 for the social domain. Each item was rated on a 5-point Likert scale ranging from 1 (“strongly agree”) to 5 (“strongly disagree”). All items were negatively worded and reverse-coded, with higher scores indicating a better health status. Cronbach’s alpha was .87 in Lim’s study 9 and .91 in the present study.
Work-life balance
Work-life balance was measured using the Work-Life Balance Scale developed by Kim and Park. 28 This scale comprises 29 items: 8 on harmony between work and family, 8 on harmony between work and leisure, 9 on harmony between work and personal growth, and 4 on general evaluation of life. Each item was rated on a 5-point Likert scale ranging from 1 for (“strongly agree”) to 5 (“strongly disagree”). As all items were negatively worded, reverse coding was applied during statistical analysis, with higher scores indicating higher levels of work-life balance. Cronbach’s alpha was .93 in Kim and Park’s study 28 and .95 in the present study.
Research procedure
Development of the nurse work scheduling program using RPA
Assessment of the current nurse scheduling process
Although the hospital used an information system, each nursing unit had distinct, non-standardized scheduling rules. Nursing department staff, co-researchers, and the system developer held meetings to identify challenges. Nurse managers entered into the system manually created rosters based on preferences and constraints. This delayed distribution and created undesirable sequences (e.g., E→D), conflicting with national guidelines. Privacy concerns arose as requests were visible to colleagues. Junior nurses felt pressured when preferences conflicted with senior staff. The developer conducted a 2-week observational study in three units to identify workflow patterns and constraints for automation.
Development of the nurse staffing program utilizing RPA
An RPA bot was developed to automate monthly schedules based on nurse manager preferences and ward rules. The bot generated schedules, submitted them for review, and registered final versions in the system. Nurses’ perspectives were incorporated during development through unit meetings and informal consultations, during which nurses provided feedback on fairness concerns, workflow issues, and preferred scheduling rules. Their input was used to refine constraint settings and request procedures, ensuring that end-user needs were reflected in both system design and the interpretation of study outcomes. (1) Setting Document – Users selected functions (automatic generation or preference-based), periods (1–3 months), and registration options (upload or Excel file). Documents were Excel-based and linked to system. (2) Google Sheet for Nurses – Nurses submitted requests via Google Sheets shared through KakaoTalk. After submission, editing privileges were restricted to view-only. (3) Google Sheet for Nurse Managers ① Nurse Information – HR data (e.g., groups, employment dates, shift types) were synced with the nurses’ sheet. Staff were grouped by tenure and shift type. ② Duty Setting – Shifts included Day (07:00–15:30), Evening (14:00–22:30), Night (22:00–07:30) and fixed D2 (08:30–17:30). Monthly schedules reflected a 40-h workweek. Public holidays were recorded on a yearly sheet. ③ Constraints – Based on national guidelines: Staffing Numbers - Minimum staffing requirements were set for each group and shift. Day shifts included D and D2. Consecutive Shifts - Maximum 5 consecutive workdays, 3 consecutive night shifts, and rest days after 2 night shifts. Shift transitions like E→D or N→E were prohibited. Shift Limits - Monthly caps for D/E/N matched individual preferences. Blank fields triggered default logic. ④ Requests – Nurses entered preferences and days off. Nurse managers added vacations and events, then reset sheets monthly. When nurse preferences exceeded staffing limits or violated constraints, the RPA bot used a simple conflict-resolution process. Preferences were prioritized based on staff group and submission order; if conflicts remained, the bot reassigned shifts using default rules that complied with national guidelines. Nurse managers could make targeted manual adjustments through an override function before finalizing the schedule.
Pre-test
Before implementation, both groups completed surveys—collected within three days—on demographics, work, health, and work–life balance.
Application of the RPA program
From January 1 to May 30, 2024, the RPA system was applied to the intervention units on a monthly basis. • Nurse managers updated staffing data by the 30th. • Nurses submitted input by the 5th. • Reviews were completed by the 9th. • The Bot generated and registered schedules by the 10th. • Managers finalized and published schedules by the 11th (Figure 1). Application of nurse work scheduling program using RPA. Note. NRS, nurse rostering system.

Post-test
From June 10 to 26, 2024, post-tests were conducted using the same procedure. Data were collected within 5 days.
Data analysis
Data were analyzed using SPSS WIN 22.0 program. Descriptive statistics (frequency, percentage, mean, and standard deviation) analyzed general characteristics and research variables. Group homogeneity was assessed using independent t-test and Chi-squared tests. Program effectiveness was evaluated using Chi-squared or paired t-tests following normality tests.
Results
General characteristics
Homogeneity test on general characteristics of participants (N = 102).
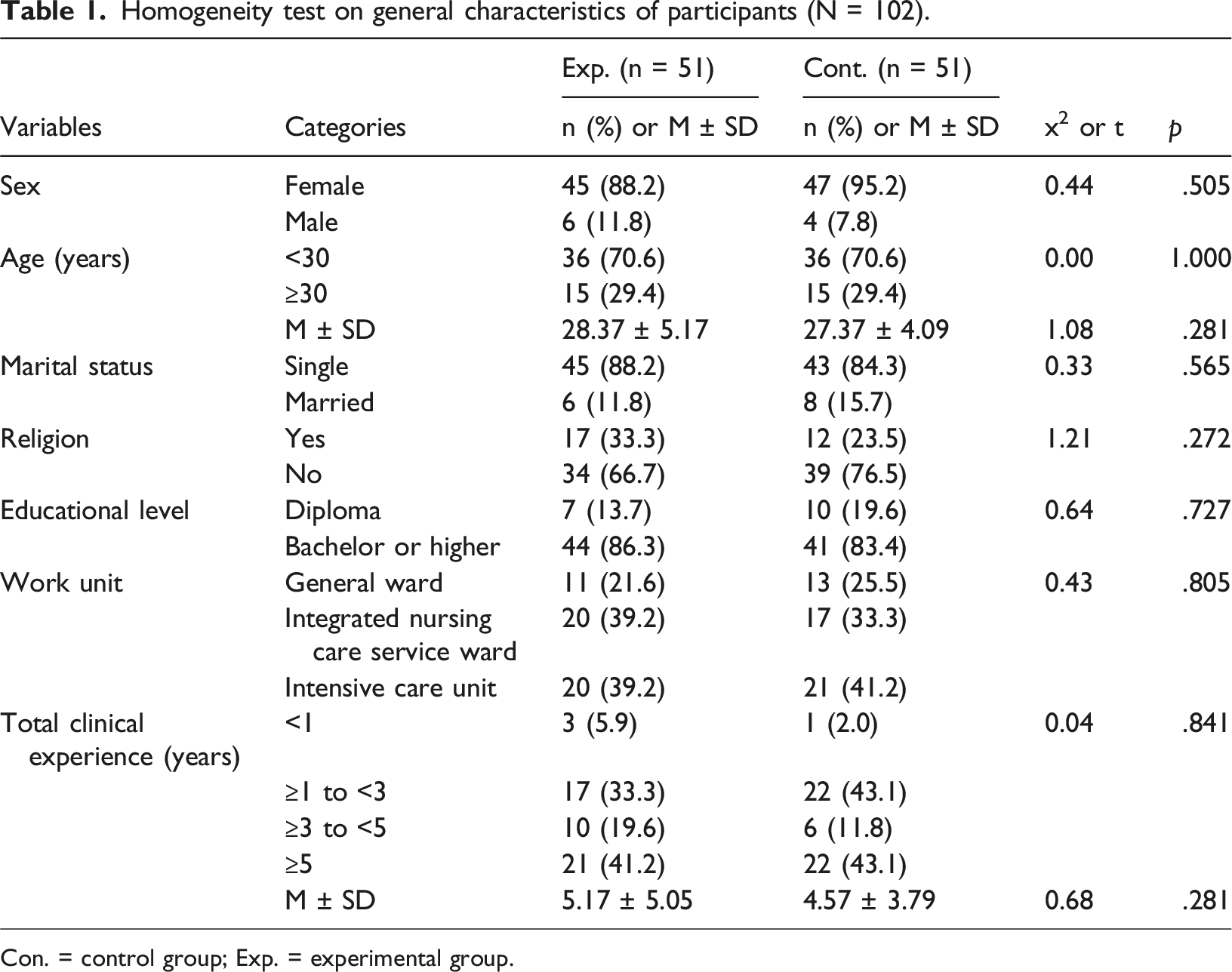
Con. = control group; Exp. = experimental group.
Homogeneity test for dependent variables between experimental and control groups before intervention
Homogeneity test on main variables between groups (N = 102).
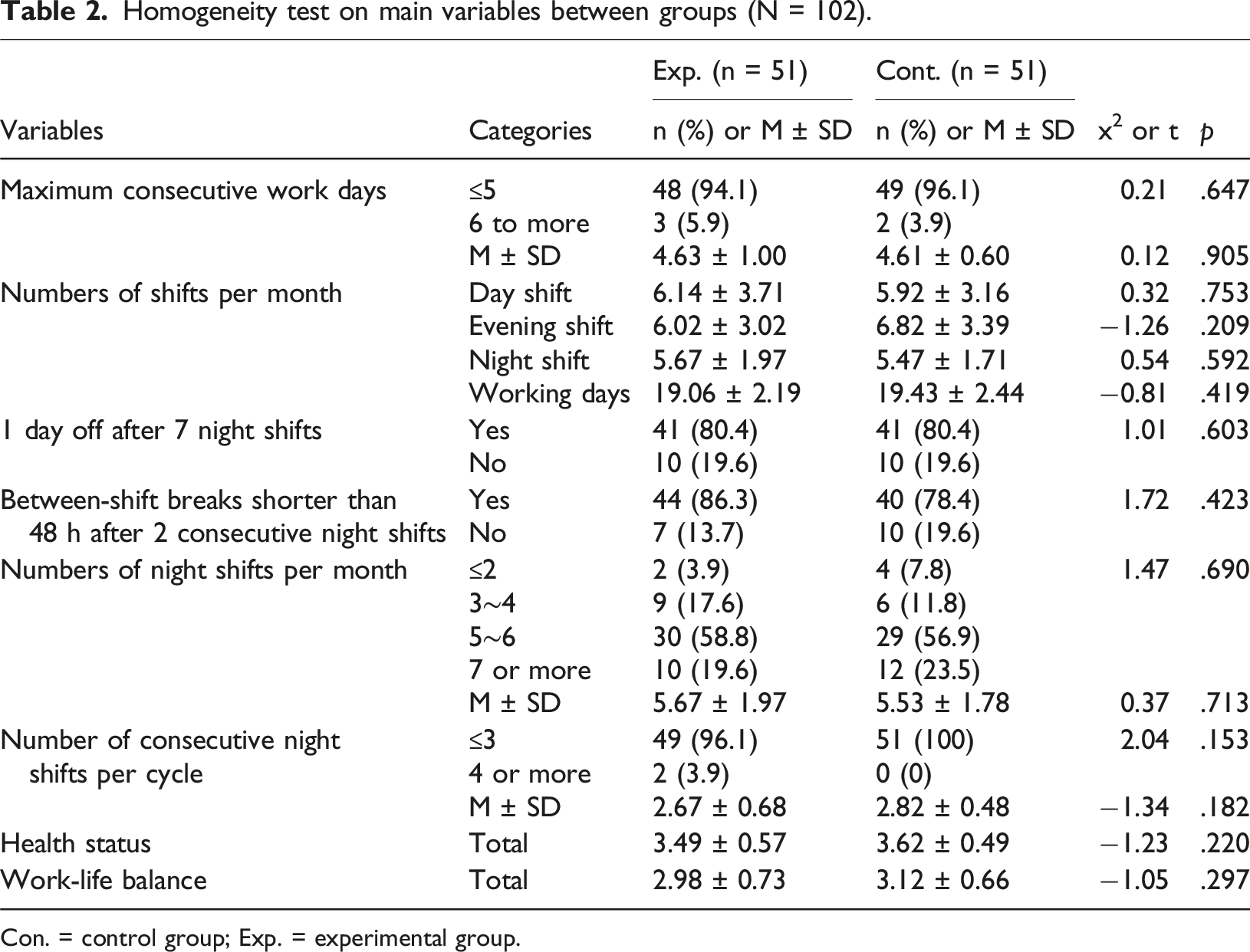
Con. = control group; Exp. = experimental group.
Effect of the nurse work program applying RPA for participants
Hypothesis 1 test
Comparison of work characteristics, health status, work-life balance between groups (N = 102).
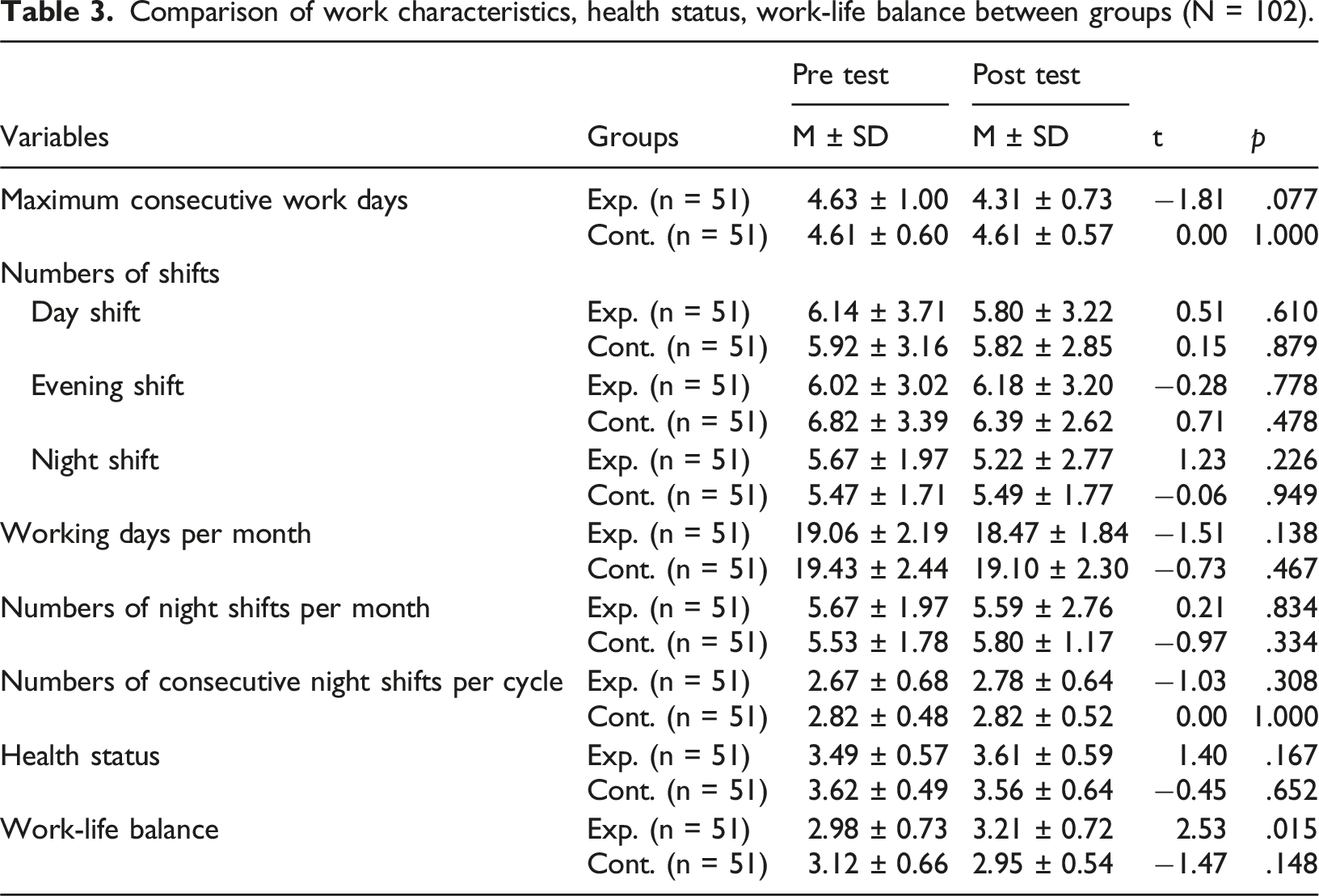
Comparison of work characteristics between groups (N = 102).

aFisher’s exact test; Con. = control group; Exp. = experimental group.
Differences in main variables between groups (N = 102).

aFisher’s exact test; Con. = control group; Exp. = experimental group.
Hypothesis 2 test
Hypothesis 2, which predicted that the experimental group working in a unit where the nurse staffing program using RPA is implemented would have better health status than the control group, was rejected. Paired t-test results comparing nurses’ health status before and after the RPA program showed an increase in the experimental group from 3.49 ± 0.57 to 3.62 ± 0.49, which was not statistically significant (t = 1.40, p = .167). In the control group, health status decreased from 3.62 ± 0.49 to 3.56 ± 0.64, also showing no significant difference (t = −0.45, p = .652) (Tables 3 and 4). The difference in change between the two groups was not significant, with the experimental group at 0.12 ± 0.62 and the control group at −0.05 ± 0.85 (t = 0.19, p = .236) (Table 5).
Hypothesis 3 test
Hypothesis 3, which predicted that the experimental group working in a unit where the nurse staffing program using RPA is implemented will show better work-life balance than the control group, was supported. The paired t-test comparing nurses’ work-life balance before and after the RPA program showed a significant increase in the experimental group from 2.98 ± 0.73 to 3.21 ± 0.72 (t = 2.53, p = .015). In the control group, work-life balance decreased from 3.12 ± 0.66 to 2.95 ± 0.54, but this difference was not statistically significant (t = −1.47, p = .148) (Tables 3 and 4). Additionally, the difference in change scores between the two groups was statistically significant, with the experimental group showing 0.23 ± 0.65 and the control group −0.17 ± 0.81 (t = 2.72, p = .008) (Table 5).
Discussion
This study aimed to develop a nurse staffing program using RPA and to evaluate its effects on work characteristics, health status, and work-life balance among nurses. The results supported Hypothesis 1, showing no statistically significant differences in work characteristics between the experimental group and the control group, reflecting that both groups followed the Nurse Shift System Improvement Guidelines and the Guidelines for Nurses’ Night Work. However, the experimental group showed higher compliance with key scheduling criteria. No nurses exceeded three consecutive night shifts; only 2.0% in the control group did so, both reflecting improvements compared to the 8.3% reported by Park et al. 29 Approximately 80% of nurses in both groups received at least 48 h of rest after two or more consecutive night shifts, which exceeds the 32.0% reported by Hong et al., 1 with higher compliance in the experimental group.
Inappropriate nurse scheduling may increase the risk of treatment errors and mortality rates. 30 Nurse managers involved in the Nurse Shift System Improvement Pilot Project reported difficulties in manually creating 3-month schedules, particularly when considering individual preferences and institutional constraints.19,29,31 The RPA-based scheduling system offers a practical and scalable solution for addressing the complexities of nurse staffing while supporting healthcare workforce digital transformation. By efficiently generating fair, guideline-compliant rosters, it enhances operational performance and nurse well-being, suggesting strong potential for broader adoption. Although further research is warranted to evaluate its scalability and adaptability across diverse healthcare settings.
The results did not support Hypothesis 2, indicating no statistically significant difference in health status between nurses in the experimental and control groups. Although health status scores increased in the experimental group and declined in the control group, the difference was not statistically significant. These findings are consistent with a study conducted at a Danish psychiatric hospital, which found no significant differences in behavioral, cognitive, or somatic symptoms when a work schedule reflecting individual preferences was implemented. 32 This suggests that shift work itself, rather than the implementation of an automated staffing system, may be a contributing factor to the decline in nurses’ health. Shift work disrupts circadian rhythms, increasing the risk of gastrointestinal disorders, sleep disturbances, fatigue, and musculoskeletal symptoms. 33 Shift-working nurses report poorer sleep quality and higher fatigue compared to those with fixed shifts. 34 Moreover, they are significantly more likely to experience work-related incidents, compromising patient safety and the quality of care. 35
Improving health outcomes among shift-working nurses requires systemic and policy-level interventions, including minimizing long consecutive shifts, ensuring sufficient rest periods, offering flexible scheduling options, and recognizing the inherent physiological challenges posed by shift work. A comprehensive approach that prioritizes nurse health is essential to maintaining a sustainable and safe healthcare workforce. While the RPA-based scheduling system improved reflection of nurse preferences, enhanced scheduling fairness, and promoted work-life balance, statistically significant health improvements were not observed. This may be because the system primarily focuses on operational efficiency and fairness, rather than direct health-related factors, such as fatigue recovery, mental well-being, or sleep quality.36,37 Therefore, improving nurses’ health requires additional organizational measures, including adequate staffing, guaranteed rest periods, and resilient shift rotations, along with national policies limiting night shifts and consecutive working days.38,39
The results supported Hypothesis 3, showing that nurses in the experimental group experienced significantly better work-life balance than those in the control group. Work-life balance scores increased in the experimental group but declined in the control group, a difference that reached statistical significance. This finding aligns with a study conducted at a Danish psychiatric hospital, where nurses reported improved work-life balance when schedules reflected individual preferences. 32 Irregular and unpredictable work schedules, such as night shifts and weekend duties, negatively affect nurses’ work-life balance and overall well-being.32,40 Allowing nurses to choose shift patterns suited to their needs can reduce fatigue and improve sleep quality. 31
In this study, although staffing constraints limited the degree of shift options, the RPA-based program allowed rosters to be finalized by the 15th of each month and planned 1 to 3 months in advance. This increased predictability likely gave nurses greater control over their work hours, contributing to enhanced work-life balance. These improvements support nurses’ health and job satisfaction while contributing to workforce retention and patient safety. Sustaining such benefits will require organizational and governmental support, including adequate staffing levels and scheduling models that align with the Korean healthcare context.
This study is the first in South Korea to develop and implement an RPA-based nurse scheduling system and assess its impact on workforce outcomes. The findings suggest that RPA may not only improve work-life balance and potentially enhance perceived fairness in scheduling, but also lessen nurse managers’ administrative burden by automating complex scheduling tasks. Nevertheless, several limitations should be acknowledged. The study was conducted at a single site using self-reported data, limiting generalizability. The effectiveness and acceptability of RPA may also vary depending on hospital size, workforce density, digital infrastructure, and institutional policies, indicating the need for further research to evaluate the system’s applicability and scalability across diverse healthcare settings.41–43 Operational performance indicators such as scheduling efficiency, time saved, and user satisfaction were not assessed; future studies should include these objective metrics to fully capture the system’s broader value. Additionally, the work characteristics survey contained descriptive items similar to demographic questions, making reliability testing inappropriate; this was acknowledged as a limitation.
Successful implementation and wider adoption of RPA within healthcare organizations require consideration of technology acceptance perceptions. According to the technology acceptance model and the unified theory of acceptance and use of technology, perceived usefulness and perceived ease of use are critical determinants of successful technology adoption.44,45 Future research should quantitatively or qualitatively assess how RPA was perceived during the nurse scheduling process, including satisfaction, perceived usability, and trust among frontline nurses and nurse managers. In this context, RPA should not be viewed as a standalone solution but rather as one component of a comprehensive strategy that includes nursing workforce policies, organizational culture reform, and policy-level interventions to ensure health, fairness, and efficiency.
Conclusion
This study developed and evaluated a nurse staffing program using RPA to improve scheduling efficiency, work-life balance, and compliance with staffing guidelines. As the first empirical study in Korea to implement and assess an RPA-based nurse scheduling system, it demonstrated practical benefits in clinical settings. Although no statistically significant change was observed in health status, work-life balance significantly improved in the experimental group, highlighting the value of predictable and flexible scheduling.
Publishing rosters 1–3 months in advance enhanced schedule predictability, supported personal planning, and reduced work-home conflict. The system produced fair, guideline-compliant schedules, reduced administrative workload of nurse managers, and increased transparency. It also alleviated junior nurses’ discomfort when their requests conflicted with those of senior staff.
By incorporating individual preferences while adhering to national guidelines, RPA provides a scalable, efficient solution to persistent scheduling challenges. Given the relationship between poor scheduling, nurse well-being, and patient safety, healthcare organizations should consider adopting automation technologies. Successful implementation will require institutional support, ongoing evaluation, and engagement from both leadership and frontline staff. Future implementation efforts should consider nurses’ acceptance of technology, organizational readiness, and alignment with workforce policies for ensuring sustained adoption and maximizing system’s benefits.
Supplemental Material
Supplemental Material - Development of a nurse scheduling program using robotic process automation in Korea
Supplemental Material for Development of a nurse scheduling program using robotic process automation in Korea by Sun Young Jung, Hyung-Eun Seo, Sung Hwa Hong, Eun-Young Doo in Health Informatics Journal.
Footnotes
Acknowledgements
The authors thank all the survey participants.
Ethical considerations
This study was approved by the Institutional Review Board of Myongji Hospital (IRB No.: MJH 2023-06-048).
Consent to participate
Participants provided written informed consent after being briefed about the study purpose, confidentiality, voluntary participation, and right to withdraw.
Author contributions
Conception and design, data acquisition, and data analysis and interpretation: SYJ, HES, SHH, and EYD. Manuscript drafting and revision: HES and EYD. Final approval of the manuscript and public responsibility for appropriate portions of the content: SYJ, HES, SHH, and EYD. Agreement to be accountable for all aspects of the work: SYJ, HES, SHH and EYD.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: this research was supported by Myongji Hospital (grant number 2301-04-01).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
