Abstract
This study aims to investigate healthcare practitioner behaviour in adopting Health Information Systems which could affect patients’ safety and quality of health. A qualitative study was conducted based on a semi-structured interview protocol on 31 medical doctors in three Malaysian government hospitals implementing the Total Hospital Information Systems. The period of study was between March and May 2015. A thematic qualitative analysis was performed on the resultant data to categorize them into relevant themes. Four themes emerged as healthcare practitioners’ behaviours that influence the unsafe use of Hospital Information Systems. The themes include (1) carelessness, (2) workarounds, (3) noncompliance to procedure, and (4) copy and paste habit. By addressing these behaviours, the hospital management could further improve patient safety and the quality of patient care.
Introduction
Health information technology (HIT) is the overarching term applied to various information and communication technologies used to collect, transmit, display, or store patient data. 1 HIT, which includes hospital information systems (HIS), electronic health record (EHR), computerized physician order entry (CPOE), electronic prescribing (e-prescribing), clinical decision support systems (CDSS), and bar-coded medication administration (BCMA), has been widely implemented in healthcare organizations to support healthcare services. HIT is expected to increase the quality and safety of healthcare services by improving communication, patient delivery time, and documentation. Despite the benefits, HIT could also introduce consequences when it is poorly designed, implemented, and used. Problems related to HIT can disrupt healthcare delivery, harm patients, and even cause death. For instance, a retrospective analysis of all reported safety events from 2005 to 2011 under the Clinical Safety of England’s national programme for information technology (IT) found that three deaths were linked to software-use errors and pending test result from previous hospitalization record that was not visible to the relevant clinicians. 2 A more recent study on EHR-related medication errors in two ICUs (intensive care units) revealed that 34 per cent of the medication events included orders with omitted information and duplicated orders. 3 These EHR-related errors had greater chances of harming the patients and they occurred more frequently at the ordering stage compared with other events. In addition, the human–computer interaction problem was the most frequently reported, associated with HIT-related patient safety incidents. 4
Previous studies have looked at the sociotechnical factors affecting safety including people, technology, tasks, organization, and the environment. Hautamäki 5 reported usability issues such as information on multiple views, the reliance on healthcare practitioners’ memory to execute daily tasks, and issues with patient identification caused usage errors that led to patient safety incidents. Moreover, the results from the system’s literature review and interviews with medical doctors showed that knowledge, system quality, information quality, service quality, training, organization resources, teamwork, task-related stressor, physical layout, and noise as the sociotechnical factors influencing the safe use of HIT.6,7 However, little is known about the specific nature of healthcare practitioner behaviours affecting unsafe use of HIS in clinical settings. Hence, this study addresses the question: How do healthcare practitioners use HIS that pose risk to patient safety and quality of care? The aim of this study is to identify healthcare practitioner behaviours that influence the unsafe use of HIS. Medical doctors who have adequate experience in using HIS in Malaysian government hospitals participated in the semi-structured interview. This study believes in the safe use of HIS as the prevention of errors, accidental patient harm, and adverse events within the care process by using HIS.
Methods
Semi-structured interviews were conducted to identify healthcare practitioner behaviours that influence the unsafe use of HIS. Details of the research methods used for this study are explained in the following sections.
Sample and setting
Semi-structured interviews were conducted in three Malaysian government hospitals located within Federal Territory and the Selangor state. The hospitals were selected based on their experience with HIS implementation, hospital size, and working environment. These selected hospitals implement Total HIS (THIS) to support their healthcare services. THIS integrates various hospitals subsystems such as Laboratory Information System (LIS), Pharmacy Information System (PIS), Radiology Information System (RIS), and Picture Archiving Communication System (PACS). All the chosen hospitals had implemented the same version of THIS. Therefore, the design and implementation of THIS follow a similar standard. Both Hospitals A and B had completely implemented THIS in December 2007, whereas Hospital C implemented it 2 months after Hospitals A and B. At the time of data collection, Hospital A, a national reference centre for haematology patients, had 562 beds. Hospitals B and C shared the same number of beds at 620. Therefore, it is anticipated that all the three hospitals have a similar working environment and experience of THIS implementation.
This study primarily focused on doctors who are also THIS users. Considering their important role in patient-care delivery and their routine use of the THIS, they can be considered crucial research subjects. THIS use is mandatory to all doctors in the selected hospitals. Moreover, THIS training was also provided to all the doctors. Purposeful sampling was adopted to select the suitable candidates to participate in the interview, because the aim was to provide rich information in context. The criterion for the sample selection was a minimum of 1-year experience in using THIS. According to the statistic obtained from the human resource department of each hospital, the total number of doctors working in the three hospitals was 770 in December 2014. In total, 31 medical doctors participated in the interview, in which 10, 9, and 12 doctors are from Hospital A, B, and C, respectively. About 58 per cent of the participants were female doctors. The participants were attached to various departments, including emergency and trauma, medical, general surgery, paediatric, obstetrics and gynaecology, orthopaedic, otorhinolaryngology, ophthalmology, cardiology, nephrology, neurosurgery and neurology, haematology, psychiatric, and rehabilitation. Their experience in using THIS was between 1.5 and 10 years.
Data collection
Semi-structured interviews with 31 medical doctors at the three hospitals were held between March and May 2015. An ethics approval from Malaysia’s Ministry of Health Medical Review and Ethics Committee (MREC) and the participated hospitals were obtained prior to the data collection. A semi-structured interview guide was designed to manage the discussion with the medical doctors (Appendix 1). The interview questions contained neutral and open-ended questions to avoid eliciting socially desirable responses. New questions were permitted to arise as a result of the discussion. The data collection method used an interview protocol developed by Hesse-Biber and Leavy. 8 Potential participants were approached at their workplace to get their agreement to participate in the interview. They were given a brief explanation about the study and the interview. Once they agreed to participate, face-to-face interview was conducted at the participants’ workplace on a date and time that were convenient for them. A mix of both English and Bahasa Malaysia languages were used throughout the interview. The interview questions consist of neutral and open-ended questions. The interview sessions were audio-recorded, except for two sessions which were manually recorded because the participants were reluctant to audio-record their discussion. Each interview session took around 15–20 min, and the total duration of all the interviews was approximately 14 h.
Data analysis
The analysis of the interview data was conducted according to the steps suggested by Creswell. 9 First, recorded audio data and handwritten notes from the interviews were transcribed to word processor text. Transcripts of interviews were then presented to the interviewees for validation purposes to ensure the interviewer had captured the respondents’ intended meaning. Then, the interview transcripts were organized into sections for easy retrieval. Subsequently, the transcribed interviews were then coded using the qualitative data analysis software, ATLAS.ti. The interview transcripts were divided into text segments and these segments were labelled with the codes. Table 1 presents an example of codes applied to a short segment of data. The transcripts were read repetitively to highlight parts of the text and to emphasize the sections and issues that appeared to be significant and relevant. Deductive coding was used for the analysis.
Example of data extracted with codes applied.

The coded data were studied to detect areas of similarity and overlap between codes. All overlapping and redundant codes were removed. Finally, similar codes were grouped together under theme or category to form a major idea. Codes that appeared to share some unifying feature were clustered into a theme. 10 Thematic maps were used as the visual representations to help sort the different codes into themes. Figure 1 shows the thematic map that shows the relationship between themes (shown as circles) and codes (shown as rectangles) deduced from the thematic analysis. All the themes were reviewed and discussed among the team members to confirm that the themes meaningfully capture the important and relevant elements of the coded extracts and the entire data set. Any variance in interpreting the findings was fixed through discussions until consensus was reached. Themes that were deemed not relevant were discarded.
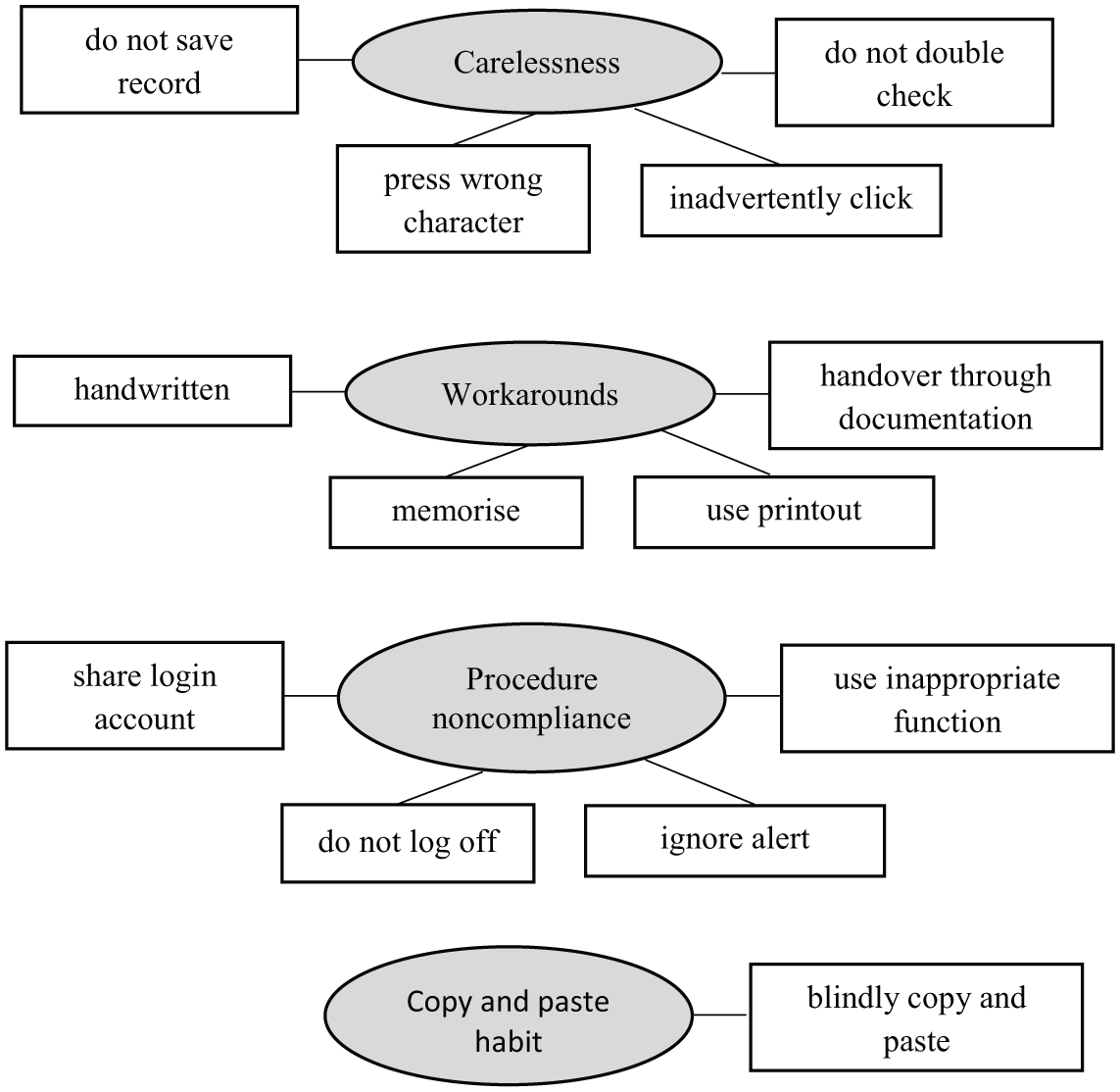
Thematic map.
Results
The interview sessions revealed four themes that emerged as healthcare practitioner behaviours that influence the unsafe use of HIS. The themes include (1) carelessness, (2) workarounds, (3) noncompliance to procedure, and (4) copy and paste habit.
Carelessness
From the interview, the respondents stressed that being vigilant by double-checking everything is very important to avoid errors while using HIS. This is because HIS does not have error-check feature. Therefore, healthcare practitioners need to double-check their own work. The points are highlighted as follows:
It is essential for healthcare practitioners to double-check patient names because there may be patients with similar names. Carelessness can possibly cause the healthcare practitioners to inadvertently select or enter notes on the wrong patient. Respondents explained their views as follows:
The respondents also remarked that errors can possibly happen due to an inadvertent click on the wrong item from the option lists. For instance, the healthcare practitioners might click the wrong medication, dosage, or patient record. Besides, healthcare practitioners are also prone to press the wrong characters on the keyboard. Hence, healthcare practitioners are advised to always double-check before signing notes and make corrections after committing any mistake. Respondents expressed this inference in the following ways:
Moreover, some healthcare practitioners forgot to save notes entered in HIS. Hence, they need to retype the unsaved record. This problem will cause problems for other doctors viewing the notes or the patient-care plan. Respondents highlighted the issues by saying:
Workarounds
Based on the interview, it was revealed that healthcare practitioners do not immediately enter or update patient-care plan on HIS during the ward round. Instead, they would transcribe the information into HIS after the ward round. All information is temporarily handwritten while the ward round is being conducted. It is possible to make mistakes when transcribing the information such as wrong ordering, and wrong data entry for the patients’ record. Respondents emphasized their views as follows:
Some of the respondents expressed that the ward round is carried out fast, thus constituting to the reason that some healthcare practitioners prefer to enter notes or plan after the round. Moreover, healthcare practitioners do not have sufficient time to immediately key in the notes during the ward round. Therefore, they write down the necessary information on a paper before transcribing it into HIS. Respondents expressed their views by stating that:
The presence of too many patients is another reason for healthcare practitioners to transcribe the patients’ notes from paper into HIS afterwards. There is a possibility that the healthcare practitioners might miss or forget to key in some information into the patients’ notes as they are all transcribed into the systems after the ward round. Respondents pointed out their views as follows:
Besides that, the interview findings show that memorizing is another workarounds strategy to overcome the problems or constraints associated with HIS usage. For instance, healthcare practitioners memorize the information to be entered due to the problem of entering notes. Apart from that, healthcare practitioners memorize patients’ information before the ward round. Sometimes, it could lead to error because the information is not presented during the ward round. Respondents expressed their views as follows:
However, some healthcare practitioners choose to printout the information from HIS for their reference during the ward round, but HIS is still not used during those times. In this situation, the printed paper may be misplaced, and consequently exposing the patient’s information to others. In addition, notes are not entered immediately during the ward round. Therefore, it could result in some missing information. Respondents explained this view as follows:
Some of the healthcare practitioners also sometimes write notes on the printout due to the rush in ward round. The data entry for all patients will be done afterwards. Transcribing notes from handwritten documents into the HIS is proven to double the healthcare practitioners’ work. A respondent explained the view:
In addition, it was revealed that sometimes, discussion among doctors from different departments regarding referral patients is done through HIS. The notes or plan is handed over merely through documentation. Hence, verbal communication does not happen. Conversely, if the referred doctor meets the corresponding doctor to verbally discuss about the case based on the manual approach, the referred doctor immediately writes down the notes into a file after the meeting. However, through HIS, the corresponding doctor only refers to the plan that is sometimes submitted late on HIS. Respondents expressed this inference in the following way:
Procedure noncompliance
For the best use of HIS, it is essential for healthcare practitioners to follow the appropriate HIS procedure. The interview findings show that some healthcare practitioners shared their HIS login account or used their colleague’s account. This will make it difficult to trace back to the responsible person when problems occur if a healthcare practitioner let their colleague use their account. Hence, it causes problem and delay to patient delivery. For instance, a pharmacist detects a wrong medication order and confirms it with the doctor based on the logged account, but often times the doctor would not admit the mistake. Respondents conveyed this view as follows:
Besides, a respondent stated that some specialists simply give their authorized account’s password to doctors for making order. However, it may turn out to be a problem if the doctors misuse the password for other unrelated orders:
The respondents also pointed out the need to always immediately log out from HIS account to avoid other healthcare practitioners from using it. Respondents expressed this view in the following ways:
Ignoring alert is another issue related to the noncompliance to procedure discovered from the interviews. In most cases, healthcare practitioners tend to ignore the alert or do not read the alert carefully because the alert frequently shows up and is always unnecessary. Respondents reported this view as shown below:
Moreover, some healthcare practitioners tend to use inappropriate functions to perform a particular task on HIS. For instance, a healthcare practitioner uses progress notes function to enter new patients’ notes. However, in practice, healthcare practitioners actually have to enter the new patient’s notes under clerking notes function, but they avoid using it because it is time-consuming to enter lengthy information. This comment was made by respondents who stated that:
Copy and paste habit
From the interviews, it was also revealed that the copy and paste habit contributes to the unsafe use of HIS. Copying and pasting have become the habit and trend among HIS users. In this case, respondents remarked that copy and paste is not a problem as long as healthcare practitioners understand the case and do not copy and paste blindly, as shown below:
Patients’ medical status may change after a long stay in the ward. However, some healthcare practitioners do not update the initial progress according to the current status. They merely copy the initial progress notes and simply add new progress notes to it. Eventually, other doctors who refer to the notes may not understand it. A respondent expressed this by saying:
A respondent also highlighted that copy and paste without updating the necessary information could result in lengthy documents:
The act of copying and pasting blindly without double-checking the information may repeat the error done by others. This implication was highlighted by a respondent below:
Discussion
The qualitative study had successfully identified the significant healthcare practitioner behaviours in adopting HIS that possibly affect patient safety and quality of care. The unsafe behaviours include carelessness, workarounds, noncompliance to procedure, and copy and paste habit. The themes are consistent to the systematic literature review carried out by Salahuddin et al. 6 It is important to note that vigilance is able to prevent mistake while using HIS. Wrongs in patient’s record, data entry, selection from dropdown menus, and file uploads were the most commonly reported mistakes that led to clinical errors such as assigning the wrong dose and wrong instructions.5,11 Similar to Ash et al. 12 study, carelessness resulted in healthcare practitioners to inadvertently click on the wrong item and misspelling when performing data entry. Selection errors were found to be the most frequent errors in using HIT, especially electronic prescribing.13,14 Healthcare practitioners did not perform any confirmation on the default value or forgot to delete or change auto-populated information that may cause patients to receive wrong medication dosage. The healthcare practitioners did not double-check and, subsequently, commit errors due to performing tasks urgently to meet the organizational demand as well as the time pressure. There is also a possibility for healthcare practitioners to forget to enter the patients’ notes.
The workarounds are associated with memorizing or writing down notes before transcribing them into HIS, writing notes on HIS printout, and completely relying on HIS for information handover. In accordance with the findings of Or et al., 15 healthcare practitioners wrote down all related data on paper and re-transcribed the data into the system later due to inconvenient access of the system at the patients’ bedside. Occasionally, the healthcare practitioners were unable to recall some of the details when entering the data into the system as well as having delayed data entry. Niazkhani et al. 16 identified that lack of mobile computer devices, time-consuming process of order entry, busy work schedules of physicians, and lack of adequate coordination between team members were the factors of workarounds. The workarounds resulted in physicians relying merely on their memory, handwritten notes prior to transcribing into HIT, and delayed order entry. Reliance on memory resulted in healthcare practitioners not recording necessary information in the system or recording a wrong medication dose, unit, administration route, or schedule into the system. 5 Moreover, very similar to Saleem et al.’s 17 study, healthcare practitioners used the printout of information from HIS for their reference and also wrote notes on the printout to make up for the restraints of the HIT implementation. Workarounds manifested when HIT failed to support physicians in their work. 18 Our qualitative data indicates that the workarounds can cause undesirable negative effects on patient safety and quality of care.
Simply by using others’ HIS account, the habit of not logging off, ignoring alert, and using inappropriate function, these acts can be identified as misconducts of the working procedure. Login and alert features are the primary designed for safety purposes. However, healthcare practitioners may get annoyed with these features and, consequently, bypass these features when they are poorly integrated with their workflow. Wentzer et al. 19 revealed that time-consuming login procedure and systems did not adequately support the mutual dependencies of physicians and nurses’ workflow, which had led some of the physicians to share their login account with nurses. Besides that, many healthcare practitioners used other healthcare practitioners’ accounts that are already logged in during previous sessions instead of using their own account when attending to the urgency in providing medical care due to a time-consuming login procedure.20,21 Moreover, the pop-up alerts call for healthcare practitioners’ attention to carefully consider whether a process could be harmful. The sheer numbers of alerts, inconsequential alerts, and the way these alerts are designed have influenced the way healthcare practitioners respond to alerts. 22 Practitioners distracted by too much irrelevance alerts may ignored the alerts. This sometimes causes an important alert to be missed, which potentially can endanger patient’s safety.20,23 Misconduct of the working procedure may indicate that the procedures to perform tasks using HIT were lacking, impractical, or poorly understood. 24
In addition, the copy and paste habit may result in errors, outdated information, and lengthy documents. Similarly, copy and paste habit issues have been addressed in a study carried out by Holden, 25 who reported that copied and pasted notes do not provide new information, contain redundant copy-pasted information, and made it difficult to know what colleagues were thinking because notes became less meaningful. Hence, copy and paste reduced the quality of notes entry. Aita and Belvedere 26 revealed that a new prescription order generated as copy of previous prescription resulted in errors of over/under dosage, due to failure in updating the dose. Therefore, the copy and paste habit becomes a constraint in the implementation of HIS by posing risks to the safety and quality of patient care. In a more recent study, Tsou et al. 27 showed that 66 per cent to 90 per cent of clinicians regularly use copy and paste. Copy and paste can cause internal inconsistencies, error proliferation, and documentation in the wrong patient chart.
The results from this study are valuable for providing in-depth knowledge of how healthcare practitioner behaviours can influence patient safety and quality of care. However, this finding is characterized by a number of limitations, which need to be considered when interpreting this work. The qualitative data is only from the viewpoint of doctors. Other groups of HIS users, for example, nurses and pharmacists were not considered in this study. Their inclusion may provide broader and more in-depth information to the study. Besides, the findings of this study are purely based on the views of HIS users. No hospital records or evidence of safe practices or patient outcomes was investigated in this study. A combination of observation and document review analysis are suggested for future study to gain in-depth understanding and stronger evidence concerning the healthcare practitioner behaviours towards safe HIS use.
Conclusion
This study provides important practical examples of how healthcare practitioner behaviours could result in unintended consequences of the HIS. The findings of this study help illuminate current challenges to the HIS implementation and provide a platform to better design HIS that is integrated with clinical needs and workflow to support healthcare practitioners in the delivery of quality and safe patient care. Moreover, insights into these contextual issues can help healthcare organizations, healthcare practitioners, and HIS implementers to understand the in-situ operation of HIS in its usage context, and help to design strategies to lessen the number of unsafe HIS adoption and their possible negative consequences.
Footnotes
Appendix 1
Acknowledgements
The authors would like to thank the 31 medical doctors who gave their time to participate in the interviews and the officers of the clinical research centres for their assistance in conducting the interviews.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Universiti Teknikal Malaysia Melaka (UTeM) and the Ministry of Higher Education (MOHE) Malaysia.
