Abstract
The presence and increase of challenges to eHealth in today’s society have begun to generate doubts about the capability of technology in patient empowerment, especially within the frameworks supporting empowerment. Through the review of existing frameworks and articulation of patient demands, weaknesses in the current application of technology to support empowerment are explored, and key constituents of a technology-driven framework for patient empowerment are determined. This article argues that existing usage of technology in the design, development and implementation of patient empowerment in the healthcare system, although well intentioned, is insufficiently constituted, primarily as a result of fragmentation. Systems theory concepts such as holism and iteration are considered vital in improving the role of technology in enabling patient empowerment.
Introduction
Technology is arguably an integral part of modernity. The potential of technology to facilitate the activities of modern society is well recognised, 1 and there is hardly any facet of contemporary society that is devoid of modern technology. The relevance of technology to patient empowerment was readily apparent from the early advocacy of eHealth in health systems. The nexus between technology and patient empowerment is such that the latter could not be imagined without the former. Patient empowerment, being a product of the modern age, is not sustainable without technology, although technology in and of itself is also not a panacea to empowerment facilitation. 1 The requirements for patient empowerment such as vast access to health information and knowledge, 2 self-management programmes, 2 new health policy construction for patient involvement 3 and the use of mobile and wearable devices 3 cannot be harnessed and efficiently managed without effective technology. However, the presence and increase of challenges to some technological utilities like health information technologies (HIT) have begun to generate doubts about the capability of information and communication technologies (ICT),1,2,4 especially with regard to patient empowerment.
Facilitating patient empowerment is integral to any modern healthcare system and corresponds to developments towards a greater level of liberty. 20 Progress has been made with the conceptualisation and development of models and frameworks aimed to support the delivery of the empowered patient. 1 Technological products are being extensively utilised and integrated in the design, development and implementation of these frameworks. Nevertheless, some patient empowerment frameworks and models have concealed their expansion and strength through disconnected elements 4 and are showing signs of age in an increasingly technological healthcare environment. 5 Additionally, the vast application of technology in both the discourse and modelling of patient empowerment is yet to deliver the prized goal of an empowered patient. 6
This article discusses patient empowerment and critiques the application of technology in the design, development and implementation of infrastructure to support it. The contribution of the article is to suggest a more sustainable technology-driven framework of patient empowerment. Patient empowerment as a concept is discussed and existing patient empowerment frameworks are critically analysed. Limitations highlighted within these frameworks coupled with an understanding of their strongest features are used in the development of a new model of patient empowerment, as presented in section ‘A unified technology-driven framework of patient empowerment’ (Figure 1). This new model draws on aspects of systems thinking such as holism, and iteration, to propose a new approach to thinking about the impact of technology on patient empowerment. The final section of the article concludes by describing next steps and further work.
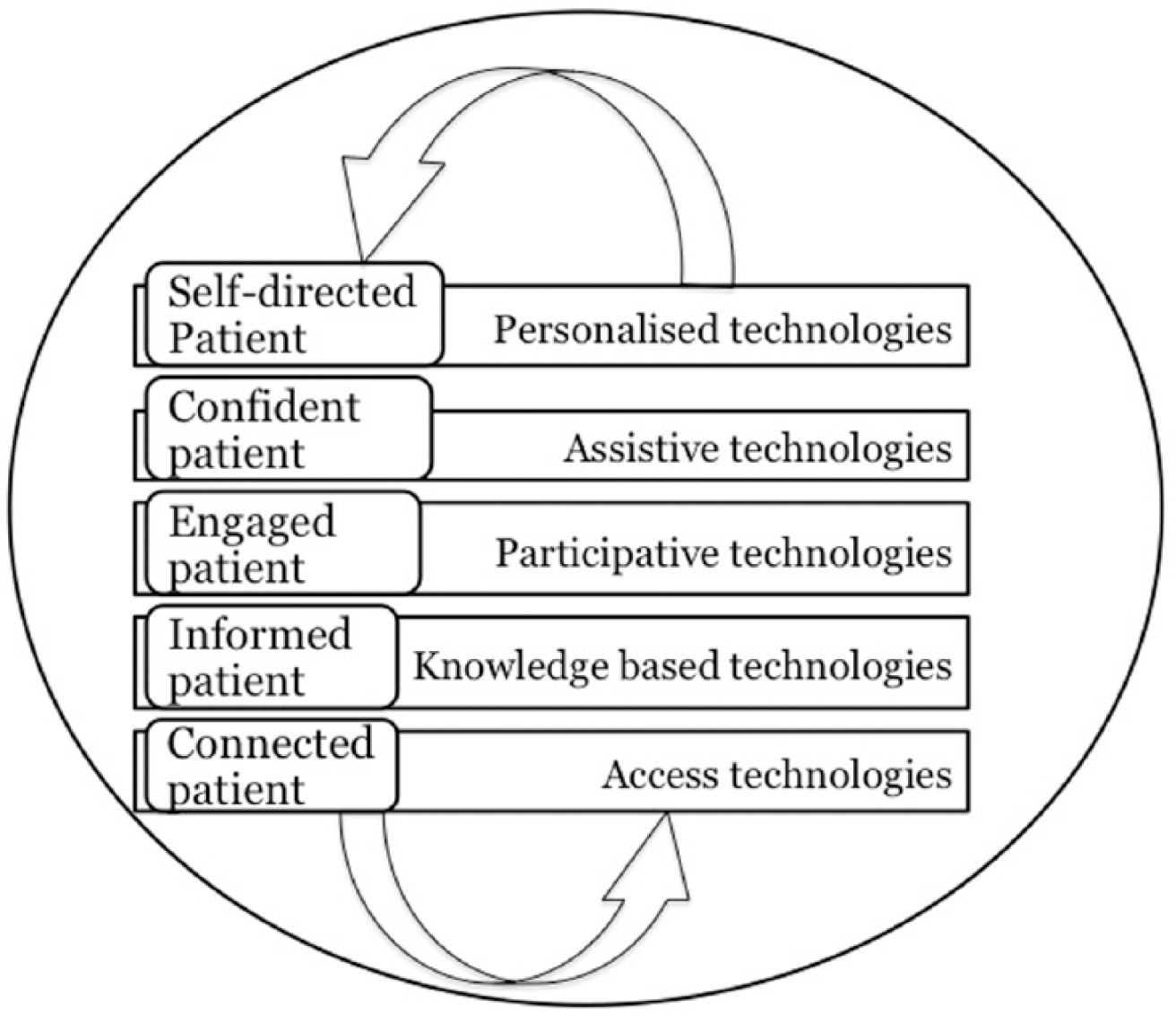
Unified technology-driven (UTD) framework.
Patient empowerment and patient empowerment frameworks
Today, there exists many definitions of patient empowerment, but essentially patient empowerment is about patients taking control or responsibility over their health, illness and treatment care, 4 as well as the ability to participate in the consultation and decision-making process. 5 Patient empowerment also encourages adherence, with the expectation of a patient to follow treatment guidance. This contrasts with traditional doctor–patient relationships, which accept the concept of ‘compliance’ in which patients are required to do as they are told. 5 Here, we find the hallmark of patient empowerment as a non-paternalistic approach to healthcare services. Thus, the majority of literature in the effort to explain patient empowerment stresses the difference between ‘adherence’ and ‘compliance’.4,5,7,8 Adherence connotes partnership 8 with this contrasting with compliance, which denotes subservience. 9
Anderson and Funnell, 9 in a study about patient empowerment and its common misconception, reconsidered patient empowerment as an interactive process that may be facilitated by healthcare providers, designed to yield positive results. In their case, this involved helping patients make self-selected changes related to physical activity. Similarly, Schulz and Nakamoto 10 assert that patient empowerment is the continuous active participation of the citizen in his or her health and care pathway, with the interactive use of information and communication technology. In these contexts, patients are responsible drivers of their own health, in which the healthcare system values them as partners. Thus, these view patient empowerment as a product of provider–patient interaction, a process of communication and the sharing of knowledge through partnership, with the use of technology for a range of different purposes. Regardless of differences among definitions, a unifying theme is present in all the descriptions of empowerment throughout the healthcare literature. This unifier is ‘self-determination’ characterised by the need to change a prevailing situation. Patient empowerment, however, is also linked to many functional elements such as information access, knowledge development, technology support, partnership work and self-management.
Existing frameworks regarding patient empowerment are often constructed in relation to a multitude of different terms and aims. 23 For example, frameworks exist related to community empowerment 4 for health purposes, the empowerment of carers, 5 family health empowerment, 7 provider empowerment 8 (described as doctors as facilitators of empowerment), patient centric 11 viewing the patient as the most crucial element) and disease management4,7 for long-term condition care. Patient empowerment frameworks and models can be regarded as a philosophy in patient care, 4 describing approaches (rooted in different care practices and ideologies) to structuring healthcare systems in order to provide better patient care, through a belief that empowered patients lead to enhanced health and well-being. 5 Frameworks and models help to advance patient empowerment action through identification of requirements to enable such empowerment to occur. 5 Thus, it can be argued that frameworks and models improve the scalability and effectiveness of patient empowerment implementation. 12
In a number of existing frameworks, patient empowerment is guided through a focus on psychological assumptions 9 and the doctor–patient relationship. 12 This emphasis on how healthcare providers could help patients be more confident and involved in their healthcare and treatment plan5,7,11 through understanding patients as experts in their own lives.
Role of technology in patient empowerment
Technology is by far the most prominent tool concerning the development of an approach to patient empowerment. 6 Many patient empowerment frameworks and models are designed, developed and implemented with the aid of various technologies. 6 Technology has proven to be extremely useful to patient empowerment not only as a tool to aid the empowerment process but also as a facilitator of learning about patient empowerment. 19 The delivery of an empowered patient is increasingly becoming contingent on technology being used to facilitate communication, access provision, interpret data, provide real-time connectivity, enable co-production between patients and health providers, and so on. For example, technological means to aid effective communication between all healthcare stakeholders can increase knowledge generation and exchange between all stakeholders in the healthcare system. Another important point is the use of technology for collaboration among patients and providers. 27 Indeed, technology in relation to patient empowerment allows patients to share ideas about health information with different groups of people. Technology-driven frameworks for patient empowerment are being constructed in which the most crucial elements profoundly depend on technology. Conversely, technologies in some frameworks may also be arranged such that their role in delivering patient empowerment is obscured. This could result in today’s patient empowerment models not being effective in the near future, 22 as technologies such as mobile devices and social networks are rapidly changing patient expectations of involvement in their own healthcare.
Technology-driven frameworks and concerns
More complex approaches to the delivery of empowered patients rely on technology and the way it is utilised. 10 There are a wide number of technologies empowering patients. For example, web services have been used for information sharing, interactive portals and remote data access.6,10 Another technology, which is growing in usage, is mobile applications both on mobile phones and tablets applied to ease communication among healthcare stakeholders (i.e. providers, patients and systems). Some of these mobile apps include the MedXCom app, 6 which lets patients request appointments, enables them to store and manage all of their health information, and instantly share important data and updates with their doctors; 13 and Apple’s health apps 14 which allow patients to put all their health data in one place and enable data from a patient’s health app to be automatically shared with their doctors. An interesting technology applied in empowering patients is the use of forums, blogs and social networks for online support. These are suitable tools to convert support groups from physical life to the electronic world, thus generating knowledge and a community including healthcare stakeholders and other patients, which then strengthens the continuity of care beyond treatment.
Technology-driven frameworks have been used primarily in reference to the application of technological tools to support patient empowerment. 6 These technological tools (i.e. Internet, mobile applications, web portals, social networks and many more) are increasingly being integrated in the design and implementation of some patient empowerment frameworks. This has the effect of portraying technology-driven frameworks as a technical effort, which guides patient empowerment through a focus on the potential of technology to deliver personal healthcare management. 13 With this growing acceptance of the application of technology in patient empowerment, some medical scholars and health organisations have proposed technology-focused frameworks, 24 which can be broadly classified thus: access frameworks, knowledge-based frameworks, participative frameworks and assistive frameworks. In the sections below, these four significant categories of technology-driven patient empowerment frameworks will be reviewed.
Access frameworks
Access frameworks can be broadly defined as a collection of technology-driven frameworks that guide patient empowerment through a focus on access. Access frameworks see the problem of patient empowerment as that of inaccessibility. Consequently, technology models are framed to address this problem. Various strategies are thus devised to present pathways and points of contact through which patient empowerment could be attained. The issues of interfaces and connectivity form key elements of access frameworks. 14 Access frameworks offer many benefits such as enabling patients and communities to use appropriate healthcare services in promotion of their medical services needs. 3 However, these frameworks fail to aid a greater sense of health ownership in patients, and collaborative working practices in practitioners. 28 Furthermore, their emphasis on access as the major impediment to the realisation of an empowered patient can oversimplify the problem of patient empowerment. 25
Knowledge-based frameworks
Knowledge-based frameworks recognise the value of knowledge to patient empowerment. Information is conceived as being singularly important within healthcare systems to enable patients to understand their own health. 7 Within this framework, an important criterion of successfully empowering a patient is the awareness of health information that directly aids their needs. 15 Technology is thus utilised chiefly to address the issues of knowledge and information. Examples of technological devices and apps used within the knowledge-based framework are SGH Diabetes Pal and Patient Pal, which seek to provide necessary knowledge to patients. Nonetheless, a knowledge framework alone cannot guarantee positive results, as access to knowledge is not an end in itself.
Participative frameworks
The key concept behind participative frameworks is on enabling the patient support process. Participative frameworks seek to do this through promoting participation in the patient empowerment goal with patients. This idea offers many benefits, which include encouraging and enabling patients to be more actively involved in managing their own health through the use of technology to exchange ideas and information with other patients and/or providers. It also offers significant productivity improvements in the development and implementation of patient empowerment. 21 This can encourage patient to be active in helping others to understand their health through sharing their experience, but at the same time, there is a risk as these patient perspectives on health management may overrule providers’ expert.
Assistive frameworks
Assistive frameworks direct patient empowerment to achieving a balance of technology support in line with health needs. 16 These are generally centred on utilising assistive technologies to provide greater independence by enabling a patient to perform tasks outside practitioner’s intervention. Assistive frameworks open avenues for continuous readily accessible healthcare and can help to facilitate self-monitoring. 6 However, there is a lack of comprehensive understanding of how the various assistive technologies available can fit together to provide a patient with complete independence.
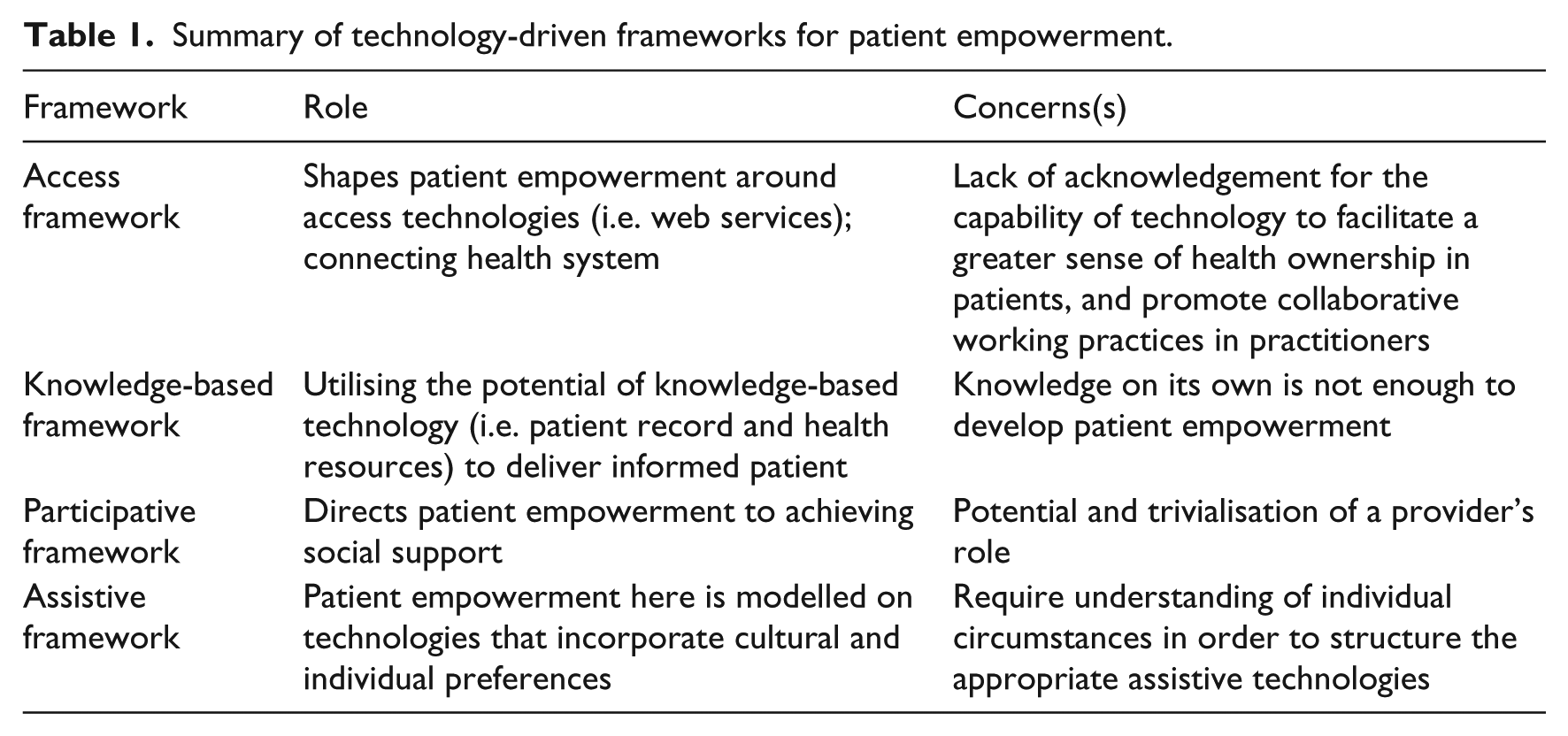
Table 1 shows a summary of existing technology-driven patient empowerment frameworks. Models and frameworks open avenues for better understanding of the efficacy of technology in the implementation of patient empowerment.
Summary of technology-driven frameworks for patient empowerment.
A unified technology-driven framework of patient empowerment
Current technology-driven frameworks already allow for the establishment of initial steps towards the delivery of an empowered patient.6,10 However, while a wide number of technology-driven frameworks have claimed to support patient empowerment, the misapplication of technology in the design, 26 implementation and development of these has lead to results not forthcoming from the current usage of technology.15,26 Therefore, it is apparent that if technological roles were to be assigned differently, positive results may occur. This section proposes one single unifying model that articulates the role of technology in patient empowerment.
Building on the existing models and frameworks for patient empowerment, this section presents a unified technology-driven (UTD) framework (Figure 1) of patient empowerment. The proposed framework focuses on the aspects of technologies empowering patients and their effect on patient attitudes towards empowerment. In this framework, patient empowerment is appreciated as an iterative process whereby every step in the empowerment process is repeated, to understand the system as a whole, and to arrive at a desired result. Furthermore, the proposed patient empowered technology framework brings together disparate elements of existing technology-driven frameworks, offering a more comprehensive account of the role of technology in delivering an empowered patient. More importantly, the framework highlights the role that technology plays in every phase of the empowerment process. In this regard, technology is a useful tool, which can make the practical implementation of patient empowerment possible. The model presented in Figure 1 also highlights the impact related to the promotion of empowerment for all healthcare stakeholders.
One of the distinguishing characteristics of the proposed technology-driven framework is its employment of the principle of holism, which broadens the scope of the patient empowerment process to include as many stakeholders and technological roles as possible. Some patient empowerment models exclude some patient groups, often leaving them unable to get a greater sense of health ownership. For example, models that do not concentrate on groups of patients who are not chronically ill, or who use health services infrequently. The UTD framework, which has the most general purpose, supports empowerment to diverse patient groups who otherwise would be virtually invisible to the mainstream healthcare system.
Components of UTD framework
The proposed framework identifies five roles where technology will be critical to improvement and change in the patient empowerment model. Over the last 5 to 10 years,6,15 there has been a significant amount of effort put into the application of technology to empower patients, although little attention is paid on its role in patient empowerment. 21 Based on review of the patient empowerment literature, there are five overlapping themes in the literature that can be considered key classes of technologies involved in the empowerment of the patient; these are as follows: access technologies, knowledge-based technologies, participative technologies, assistive technologies and personalised technologies.
Access technologies
Access technology is one of the key mechanisms used for empowering patients. Its application covers several approaches such as interface(s), computerised patient records, formatting (i.e. document structures), health card applications, summary care records and many more. Access technology covers the electronic provision of health and treatment information to all healthcare stakeholders (providers, patients, etc.). For example, the summary care record provided by the NHS in the United Kingdom interacts with databases searching for suitable information to connect providers at emergency wards. This effort is based on data management, which is a means that enables data storage and sharing between all healthcare stakeholders. Access technologies also allow patients and healthcare providers to access health information and services. For many, access technologies play an important role in delivering the empowered patient, while for others, access alone is not adequate to empower a patient. True patient empowerment requires that patients are not just recipients of information but also partners who can also generate and process information. The role access technology plays here is in connecting to the healthcare system as a whole including all stakeholders (patients, providers, etc.). However, existing frameworks are not designed to enable patient input, 26 as they do not automatically have access or editing rights for their records. 7 The proposed framework includes patient access at its core, expecting patients to be connected in the first stage of the process of patient empowerment. This is considered to allow the establishment of the connected patient and can be used in achieving the next stage of the empowerment process through an iterative process, thus establishing a connected healthcare system (i.e. national, cross-national and global).
Knowledge-based technologies
Knowledge-based technologies allow the collection and displacement of useful health information to healthcare stakeholders such as patients and providers for reading, viewing, study or reference. 29 Knowledge-based technology includes health portals, knowledge banks, health libraries, Web Information Systems, email and many more. The main functions of these technologies are to provide resources and inquiry support for patients, providers and other healthcare stakeholders. Thus, knowledge-based technology is crucial in the delivery of the empowered patient. The importance of knowledge-based technology in patient empowerment has also been recognised by many health organisations such as the World Health Organization (WHO), which initiated free and open access to medical literature through the Health InterNetwork Access to Research Initiative (HINARI). However, there is the case of ‘dangerous knowledge,’ which means that having unlimited health knowledge may lead patients to act on unproven science. 8 For example, a patient with high blood pressure could access health information, which concludes that caffeine is not a risk factor for cardiovascular disease. Acting on such information alone could lead to the patient’s continued use of coffee. However, other research into the effects of coffee on human health may have provided a contrary result. Thus, knowledge-based technology in this context may not automatically yield absolute positive results, which are important for patient empowerment. In the proposed framework, knowledge-based technologies are recognised specifically for their ability to deliver informed patients. Informed patients are enlightened about their own health and their negotiating agents 12 whose health responsibility is both a matter of increasing knowledge 10 about everyday experience as part of a reflexive plan and a matter of locating this plan within a broader informational environment.
Participative technologies
Participative technologies allow patients to get and share information easily and give them straightforward access to knowledge traditionally held by doctors, but that does not inherently empower patients. 6 This involves social media (i.e. Skype, Twitter and Facebook), web portals, health forums, dialogue construction, email and many more. For example, suppose a patient with mental issues joined a social media group such as Depression Alliance for peer support, visits 10 top online health forums to discuss their health problem and has a video chat on Skype with their doctor for clarification of the information they received from other sources. Is that patient empowered? This will no doubt transform the paternalistic relationship between a patient and the healthcare system into a partnership care process. Partnership care is one of the central mechanisms available to support the development of patient empowerment 13 and is essential for the delivery of the empowered patient with a high quality of healthcare diagnosis and treatment of disease, thus providing patients with an opportunity to get involved and take an active role in their own healthcare. The application of participative technologies in the proposed framework is argued as a means through which inherent problems in empowering patients (including supporting the asymmetry between healthcare stakeholders and their willingness to share information) can be solved through a developed approach that leads to patients who are more involved in their care.
Assistive technologies
One of the technologies that best facilitate the implementation of patient empowerment is assistive technologies. 6 This encompasses a range of devices from mobile to wearable devices. It may involve the following: mobile phones with installed health apps; memory aids such as reminder messages, medication aids, clocks and calendars; sensors around the home to detect situations that can be potential hazards such as patient absence from a bed; and other technologies associated with illnesses such as dementia. Assistive technologies may not necessarily place the patient in the control seat. 10 However, they may help the patient with everyday living, enabling patients to perform tasks that they would otherwise be unable to do, or increase the safety with which the task can be done. 16 For example, a person who is a sleepwalker could trip over breakable or harmful objects, and be injured, or could open the door and leave the home without knowing, but with assistive technology, a sensor could raise an alarm in such a situation, thereby waking the sleepwalker or others. Therefore, assistive technologies can help to promote independence for patients and to promote liberty. Thus, this would help create patients’ general feeling of confidence in managing and treating their own health. In this regard, the proposed framework appreciates the role of assistive technologies in empowerment to deliver or enhance a confident patient.
Personalised technologies
Inclined to the level of complexity of personal healthcare management in modern healthcare system and the differences in patients (whether they be caused by variation in disease, lifestyles or preferences), personalised technologies are becoming increasingly necessary in healthcare and a vital element in the patient empowerment model. Personalised technologies are tools or approaches that may be designed to meet an individual patient’s requirements, preferences and needs. This may involve self-diagnosis, personal alert management, self-monitoring, self-care, self-treatment, self-protection, self-assessment, self- efficacy and self-management. Personalised technologies may help patients prevent some disease (diabetes, heart disease, kidney disease or heart failure) or reduce the risk of having one. For example, the NHS health and symptom checker app allows patients to check symptoms if feeling unwell, 30 which will then automatically provide them with assessment, information about their condition and advice on how to look after their own health. This may help spot early warning signs and help prevent a condition getting worse. In addition, this may help patients make beneficial choices that are more relevant to their own circumstances and preferences. 17 The proposed framework understands personalised technologies as self-health, which allows patients to modify, control their own health to individual expectations. This can help patient take more control over their health, well-being and treatment plan; promote personal initiative; and provide a greater sense of health ownership in patients. Furthermore, the ultimate desired goal of patient empowerment is not limited to any single aspect such as connected, informed, engaged, confident or self-directed patient, but rather all ingredients working together as one whole system.
How the proposed framework, UTD, overcomes the concerns identified in section ‘Technology-driven frameworks and concerns’
The UTD integrates all the key technology-driven frameworks and focuses on core patient empowerment elements. Patient empowerment approaches involve multiple elements that cannot be explained by their component parts alone. There is a need for a unified application of a homogeneous technology to support patient empowerment. The proposed framework, UTD (Figure 1), recognises the five technology roles (access, knowledge-based, participative, assistive and personalised) across various different forms as core to successful patient empowerment development while understanding that there are other elements that can be utilised to improve empowerment outcomes. The recognition of these five technological roles can help to overcome the concerns stated in section ‘Technology-driven frameworks and concerns’. For example, all the elements in the UTD interact with one another systematically to deliver an empowered patient. This increases the chances to acknowledge the role of technology in facilitating a patient’s sense of health ownership. In addition, the UTD minimises the trivialisation of any health stakeholders’ role making the role of doctor and patient equally important. Most importantly, through connected, informed, engaged, confident and self-directed patients, the distribution of health information and apps can be open to diverse groups of patients in relation to their needs. Therefore, the UTD may lessen the retrieval of ‘dangerous knowledge’. Overall, the UTD understands that the traditional technology-driven frameworks complement each other and understanding them as a whole can help minimise the presented concerns.
Iterative process
Iteration is vital in the development of empowerment processes, which require frequent monitoring of progress. As seen in Figure 1, the idea of an iterative process is inherent in the proposed framework. The framework suggests that activities in the empowerment process will need to be repeated over time as a patient’s condition changes and their experience develops. Each repetition of the process is expected to produce a result that can be used as the starting point for the next iteration. For example, access technologies can aid to deliver a ‘connected patient’ (i.e. practitioner, provider, patient, hospitals, general practitioners (GPs) and organisations), which could be used as a starting point to guide the use of knowledge-based technologies to produce a more ‘informed patient’. In addition, the framework emphasises that there is no starting point or end point during the process. An iterative process allows repeating component elements of the empowerment process to generate a targeted or desired result. This makes the UTD framework not a static model but a continuous process leading to new experiences. The UTD uses iterations to increase the patient experiences and understanding of his or her condition, or increase patient understanding of new conditions. The framework also enables a patient to be at different levels of empowerment dependent on different aspects of their health condition. For example, patients may feel completely empowered in managing a condition they have experienced for a long period of time, but be at lower levels of the framework for conditions they have only recently acquired.
Conclusion and future work
As our healthcare systems move to patient-centred care models, there is a tendency that a patient’s role will change from a paternalistic to a more adherence focused approach. 7 There is a clear quest in the effort to understand patient empowerment methods for the delivery of empowered patients, and the development of models for patient empowerment have been an on-going global research issue over the past few decades. 6 With the emergence of eHealth services, most of the recent research assumed that any push for technology should focus on access to health information 10 and services, to enable partnership care 14 and for knowledge development 18 in order to yield patient empowerment. 18 However, the slight misunderstanding of technology in the design, development and implementation of some of the current models of patient empowerment has underrated the strength of the role that technology can play in helping to deliver the empowered patient and as such results have not been forthcoming.6,16 The presented technology-driven framework of patient empowerment in this article could successfully cope with the demands of a patient-empowered technology system, as in this framework, the role of technology is re-designed to take into account holistic perspectives and an iterative process. In this regard, re-application of the role technology presently has in the effort to deliver empowered patients in accord with the proposed framework (Figure 1) as the potential to yield positive results. In the patient empowerment approach, all its properties cannot be determined or explained by their component parts alone. Thus, the entire system should be considered as a whole. Therefore, there is a need for the unified application of homogeneous technology in patient empowerment. Iteration is vital in empowerment processes, which require frequent monitoring of progress.
Further work will focus on developing additional support for the framework through healthcare stakeholder analysis, including exploration through a qualitative questionnaire to have a complex, holistic picture, and detailed views of information around patient empowerment principles. This will enable a further level of complexity to be analysed and taken into consideration. The proposed framework of patient empowerment recognises access across various different forms as a core to successful patient empowerment development, while understanding that there are other elements that can be utilised to greater improve empowerment outcomes. The UTD framework proposed in this article does not just have the potential to be integrated into the UK health system, it also has the potential to be integrated on an international scale into other environments. Some of the aspects of the framework could also be applied to a health information application, service or design. The literature identifies a number of barriers, which may hinder such an implementation process. If the barriers of the implementation are identified early, then actions can be taken to overcome these barriers. Some possible barriers that may be encountered are administrative practice and perhaps the availability of software, but through knowledge and awareness, these can be overcome.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
