Abstract
“Open abdomen” is a strategy used to avoid or treat abdominal compartment syndrome. It has reduced mortality both in trauma and non-trauma abdominal catastrophes but also has created a challenging clinical problem. Traditionally, open abdomen is closed in two phases; primarily with a free skin graft and later with a flap reconstruction. A modern trend is to close the abdomen within the initial hospitalization. This requires multi-professional co-operation. Temporary abdominal closure methods, e.g. negative pressure wound therapy alone or combined with mesh-mediated traction, have been developed to facilitate direct fascial closure. Components separation technique, mesh reinforcement or bridging of the fascial defect with mesh and perforator saving skin undermining can be utilized in the final closure if needed. These techniques can be combined. Choice of the treatment depends on the condition of the patient and size of the fascia and skin defect, and the state of the abdominal contents.
In this paper we review the literature on the closure of an open abdomen and present the policy used in our institution in the open abdomen situations.
Keywords
INTRODUCTION
“Open abdomen” (OA) has become a significantly more common intermediate step in the treatment of abdominal emergencies (1). Any insult that results in an acute increase in the volume of the abdominal contents sufficient to cause pressure- related end-organ dysfunction, can lead into abdominal compartment syndrome (ACS). These can include e.g. abdominal trauma, ruptured abdominal aortic aneurysm, retroperitoneal hemorrhage, pancreatitis, extensive burn and sepsis. Low urine output, hypotension and increased ventilator pressures develop as the manifestations of ACS. Open abdomen is used as a strategy to avoid or treat ACS. In addition, the need for re-exploration can be a reason to leave abdomen open.
Using OA strategy can reduce mortality (2–4). It has also created a new group of patients with a complex clinical problem. A variety of surgical methods has been developed for abdominal closure. The traditional policy to make a skin graft on the granulated open abdomen resulted as a giant hernia. The skin graft cannot be removed before 6 months because of the adherence on the bowel surface. Nowadays the aim is to promote definitive closure of OA as quickly as possible within the initial hospitalization. The success in that goal has been shown to be associated with excellent long-term physical and mental health outcome (4).
Several temporary abdominal closure techniques can be used to facilitate definitive abdominal closure (1, 5, 6). These include the Wittman patch™ (Novomedicus, Nokomis, FL), the abdominal re-approximation anchor (ABRA) system (Canada Design Inc., Almonte Ontario, Canada), staged abdominal repair (STAR), negative pressure wound therapy (NPWT) and mesh-mediated traction technique. NPWT alone or combined with mesh-mediated traction technique is further described in this article. Key factor is to keep abdominal wall elastic and mobile by preventing adhesions between the intestines and the abdominal wall and avoid lateralization of the abdominal wall (6). The midline closure of the fascia should be reached. Additional surgical techniques, e.g. components separation (CS) and undermining of the skin, may be needed. Successful re-creation of the linea alba gives dynamic support. Closure should be strong enough to prevent hernia formation. Excessive tension should be avoided because it can lead into necrosis of the skin and fascia. Necrosis, in turn, can lead into infection and wound dehiscence. Sometimes direct closure cannot be obtained and one must settle for compromise. In those situations bridging type of fascia closure methods are considered. Choice of a method also depends on the patient's condition.
In this paper we present methods of closing an open abdomen primarily without a need for distant flaps. In our experience this is usually possible.
BOGOTA BAG
Patients with an open abdomen are often critically ill and are thus treated first in the intensive care unit (1).
Their intestines are swollen and paralyzed. Their haemodynamic status may be unstable. It is common that platelet and hemoglobin levels are low and inflammatory parameters elevated. It is important to wait until the patient's condition stabilizes before finally closing the abdomen. In addition, the nutritional status has to be good enough to ascertain sufficient prerequisites for wound healing. We have noticed major drawbacks in the healing process if the final surgical treatment is too early; additional surgical measures may later be needed.
A Bogota bag can be used as a first-line treatment for temporary abdominal closure. A sterile piece of plastic is sutured to the skin or fascia. Bogota bag prevents evisceration and desiccation. However, it does not prevent adhesion formation between the abdominal contents and abdominal wall and does not help controlling fluid secretion. A Bogota bag also allows progressive retraction of muscular components from each other. This hampers final midline closure of the fascia. This treatment should be used as short period of time as possible and switched to the negative pressure wound therapy (NPWT). NPWT can be started when there is no more need for every day re-exploration of the abdomen, no risk of bleeding and once the inflammatory parameters are declined. NPWT can be started for the majority of the patients within the first week after the OA situation.
NEGATIVE PRESSURE WOUND THERAPY
NPWT is a modern treatment for temporary abdominal closure. This technique provides abdominal coverage, reduction of intra-abdominal pressure and control of exudates. More importantly, it prevents adhesion formation and forms traction between the fascial edges thus facilitating the final fascial closure. In the Barker's technique, negative pressure is applied to the abdomen through surgical towels placed on top of the fenestrated polyethylene sheet (7, 8). French silicone drains are placed on top of the towel and connected to the suction source. Adhesive drape is placed over the towels and drains. Polyethylene sheet is placed between the peritoneum of the abdominal wall and the viscera. This is crucial to prevent adhesion formation. Several commercial equipments are also available. The first to be introduced was abdominal VAC® Therapy™ (vacuum assisted closure, KCI, San Antonio, TX, USA). In this technique, foam covered by a perforated plastic sheet is placed on top of the viscera and between the abdominal wall and viscera. This abdominal dressing is in turn covered by a thick polyurethane sponge placed in the defect between the fascial edges and the skin. An air-tight adhesive film is applied on top of the foams and a drain is connected to the pump.
The NPWT dressings are changed every 2–3 days, and the therapy is continued until the patient's condition is stabilized and a final closure can be done. In some techniques, fascial edges are partially closed superiorly and inferiorly every time the dressings are changed (9). This technique will supposedly increase the linearity of the wound and begins to improve the anatomy and physiology of the abdominal wall (10). NPWT has facilitated the possibility to reach a primary closure of the abdomen. It has been shown that if the treatment exceeds 3 weeks, it is mostly impossible to close the fascia (11, 12).
Sometimes there is longstanding visceral swelling, and a longer treatment period is needed. This can lead into failure of the primary closure of the abdomen. Petersson et al. (13) developed a novel technique for a late closure of the open abdomen. In that technique, VAC® is combined with mesh-mediated fascial traction. Two pieces of polypropylene mesh are sutured to the fascial edges with a running 0 polypropylene suture. The two meshes are sutured to each other in the midline, on top of the foam covered by a perforated plastic sheet, giving traction to fascial edges. A thick polyurethane sponge is then placed on top of the mesh and is further covered by an adhesive film and drain. The meshes are tightened every time the dressings are changed. This technique may have some advantages compared to the technique combining NPWT with partial suturing of the fascia when dressings are changed. NPWT combined with mesh-mediated fascial traction offers the possibility to clean the abdominal cavity, facilitating the reduction of peritoneal fluid and bacteria, every time dressings are changed and mesh tightened. This technique also allows the abdominal wall move freely toward the midline at every dressing change without interference of adhesions between the viscera and abdominal wall.
Abdominal closure is considered when 3–7 cm of separation of the fascial edges remains. VAC® combined with mesh-mediated fascial traction provides a high fascial closure rate after long-term treatment of OA (14).
SKIN GRAFT
The traditional treatment protocol of the OA patients was to wait the intestines to get granulated after which the split-thickness skin graft was applied on the bowel. The inevitable hernia was then later repaired. This method has many disadvantages. The two-staged procedure is costly (4). The risk for an enteroatmospheric fistula is significantly increased. The skin graft is not durable and can thus be ulcerated. The edges of the fascia and muscular components of the abdominal wall are retracted. The lack of mechanical strain causes myofibrotic atrophy and fibrosis (10, 15). Finally, the elastic properties of the muscle are decreased. This increases the transfer of load forces to the midline wound at the time of hernia repair which may contribute to the high laparotomy wound failure rate observed following a hernia repair. In a study by Cheatham et al. (16) it was found that patients awaiting abdominal wall reconstruction demonstrated significantly decreased perceptions of physical, social, and emotional health when compared to the general population. The use of a skin graft in an OA situation should be avoided. It should only be used if other treatment options to achieve same-admission definitive abdominal closure are not possible. If the patient's condition stays poor for a longer period of time not allowing more extensive operations, a skin graft has to be used for a temporary closure of the OA.
FINAL ABDOMINAL CLOSURE
The optimal time for the final abdominal closure after temporary abdominal closure techniques is when the distance between the fascial edges is about 3–7 cm, the patient's condition is stable and his nutritional status is good (14). The fascial edges are closed directly if possible. An important question is whether one should use a mesh to give additional support even though a direct closure is possible. We use mesh reinforcement as augmentation to the fascial closure in order to prevent hernia formation.
Sometimes a fascial defect cannot be entirely closed and different surgical techniques have to be considered. Components separation (CS) can be used to bring fascial edges closer to each other enabling direct closure. CS can be combined with mesh reinforcement. Synthetic and biological meshes can also be used to bridge fascial defects. Extensive skin undermining endangers the circulation of the skin in the midline leading easily to edge necrosis of the flaps. This may lead to exposure of the underlying mesh with further difficult problems. Saving a few perforators arising from the rectus abdominis muscles will preserve the circulation of the undermined skin flaps.
More than one technique may be used in the same patient (Fig. 1 A–C.). The combination of the techniques is selected depending on the condition of the patient, size of the fascial and skin defect, mobility of the abdominal wall structures and how attached the abdominal contents are to the abdominal wall.
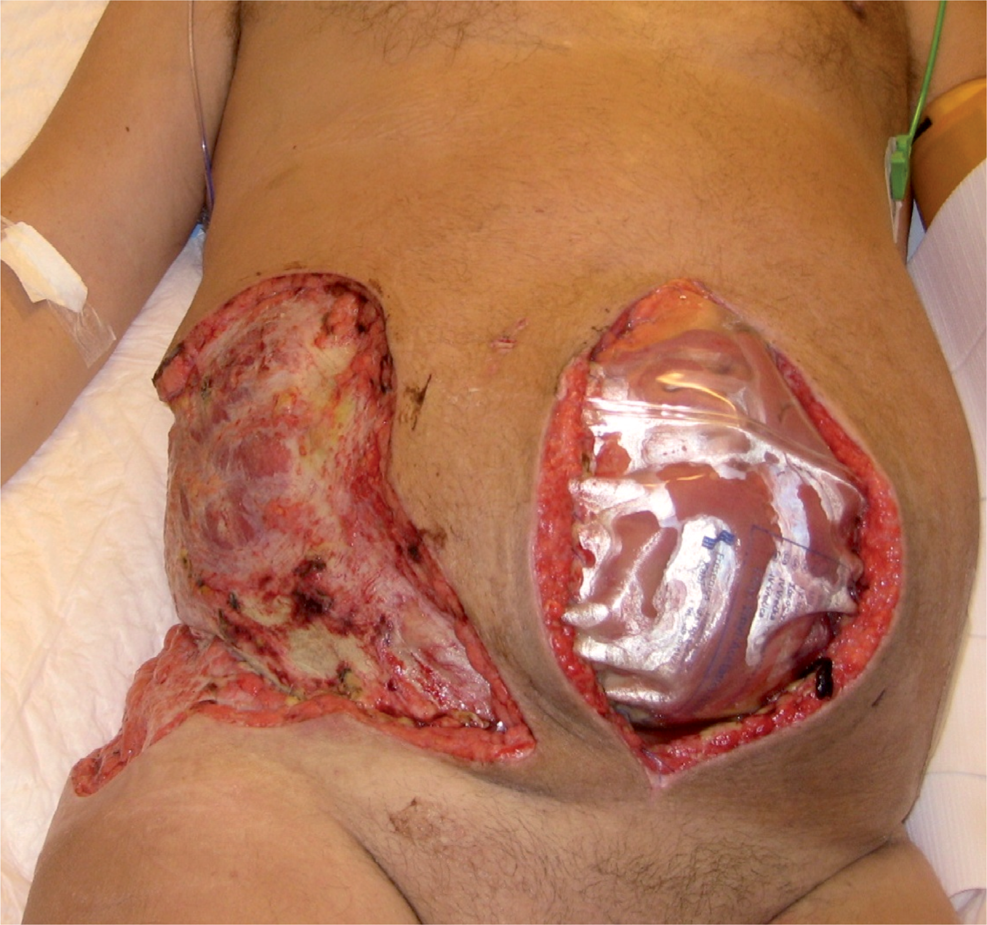
58-year old man had a necrotizing fascitis after an endoscopic radical prostatectomy. The patient was septic and abdominal compartment syndrome was diagnosed. Open abdomen was created and the necrotic tissue was removed 10 days after prostatectomy. A Bogota bag was used for 10 days.
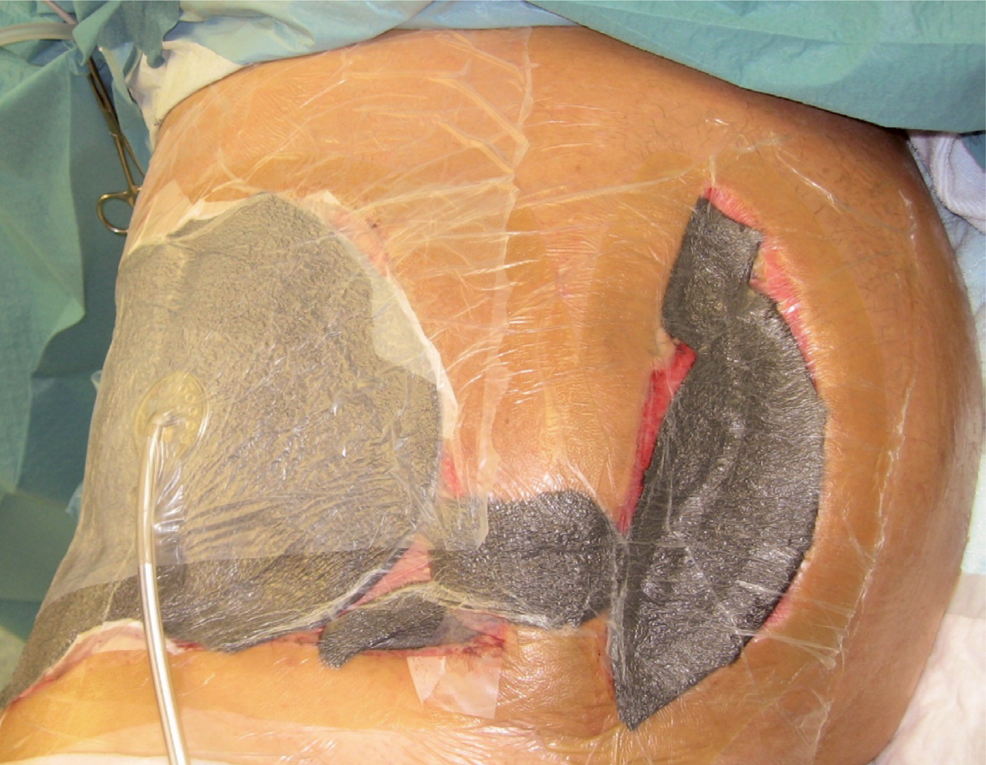
A Bogota bag was changed into negative pressure wound therapy and mesh-mediated fascial traction. NPWT dressings were changed 5 times, and every time the mesh was tightened and the intestines were kept mobile from the inner abdominal wall.
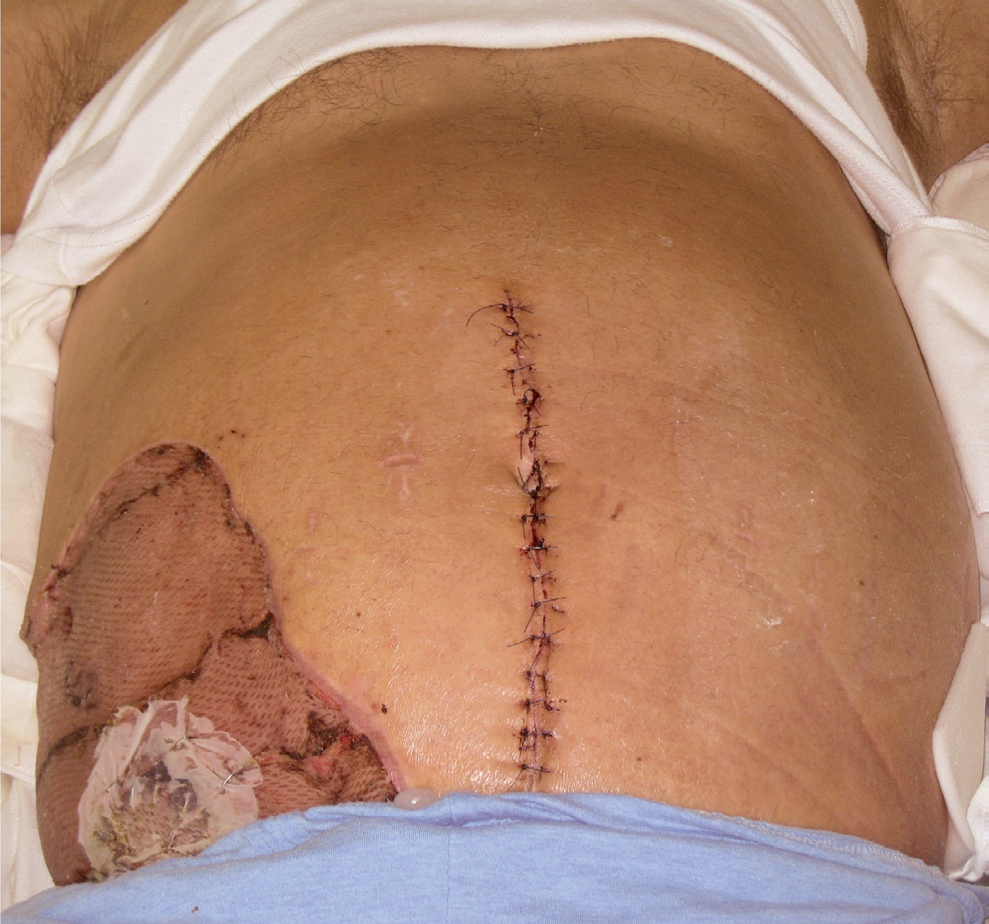
The fascial edges could be reapproximated with the help of a perforator saving components separation on the left side after 26 days of negative pressure wound therapy. The fascial suture line was augmented with an inlay composite mesh. The skin defect in the right flank was covered with a free plit thicknes skin graft. The patient recovered completely.
TRADITIONAL COMPONENTS SEPARATION
The components separation technique was first described by Ramirez et al. (17). The external oblique muscle can be separated from the internal oblique in a relatively avascular plane. The external oblique is divided on both sides vertically about 1–2 cm laterally to the lateral edge of the rectus sheath. The compound flap of the rectus muscle, with its attached internal oblique-transversus abdominis muscle, can then be advanced 10 cm around the waistline. The posterior rectus muscle fascia can also be divided at the middle part of the muscle to further facilitate the mobility of the abdominal wall. The rectus abdominis complex is innervated through intercostal nerves that run deep to the internal oblique muscle fascia. CS thus provides dynamic autogenous reconstruction of massive midline abdominal wall defects. The disadvantage of the technique is that a large area of dissection is needed for proper mobilization of the components. The patients' stable condition and good nutritional state are prerequisites for such extensive surgery.
Some surgeons think that a full CS should not be used to promote fascial closure in patients with OA during the initial hospitalization (1). They consider that this technique should be saved as an option for later abdominal wall reconstruction. On the other hand, one could assume that muscular components of the abdominal wall are more elastic in the primary closure than for example in a secondary hernia repair, and this could support the idea of using components separation in the primary closure. There are no published clinical data or controlled clinical trials reporting the use of CS after OA situation in the primary closure. In our practice, we have used CS with mesh augmentation after OA situation in order to achieve a direct midline closure of the fascia or a direct skin closure after the bridging of the fascial defect. There are some data showing that using mesh reinforcement in components separation seems to improve long-term strength of the secondary hernia repair (18–20). Both single-mesh and double-mesh techniques utilizing synthetic and/or biologic meshes have been used.
PERFORATOR SAVING COMPONENTS SEPARATION
Usually the skin defect is so large that extensive undermining is needed in order to get skin closed in the midline. This could compromise the vascularity of the skin and lead into necrosis and dehiscence of the wound. The ischemia is always much larger in the subcutaneous fat than in the skin. To avoid circulatory compromise of the midline skin we have saved two to three perforators arising from rectus abdominis muscles on each side. We have performed full CS behind the perforators. In OA situations NPWT combined with perforator-saving component separation (PSCS) and mesh augmentation allows usually closure of the midline. In our experience even a large midline defect can be closed without a flap reconstruction with PSCS. CS can be done also mini-invasively or with an endoscopic technique (21, 22). This saves the circulation excellently, but on the other hand, it does not mobilize the skin as efficiently as in an open technique.
BRIDGING OF FASCIAL DEFECTS WITH MESH
Synthetic or biologic meshes can be used for bridging fascial defects if the edges cannot be totally closed after an OA situation (23, 24). Sometimes most of the defect can be closed with components separation and the residual defect can be closed with a bridging mesh. If the abdominal contents are tightly attached to the abdominal wall, a bridging mesh augmentation can be combined with perforator saving subcutaneous undermining to achieve skin closure over the mesh.
Permanent synthetic meshes have a good tensile strength but they also have some disadvantages (25, 26). Scar tissue formation within and around the mesh's fibers may result in dense adhesions to the viscera which can lead into pain, bowel obstruction, perforation, and/or fistula formation. Synthetic materials such as nylon, polypropylene, and polyethylene terephthalate are associated with fistula formation when applied directly over the bowel. Therefore, the use of the composite synthetic materials may be more appropriate if they are applied over the bowel. They contain macroporous and microporous surfaces, one on each side. The microporous surface is nonadherent and can be placed over the bowel. The macroporous surface allows for tissue ingrowth and granulation tissue formation. A synthetic mesh may have to be removed if infected (27). The state of the patient and the site of the infection are considered in the decision-making. Sometimes the mesh can be partially excised, or NPWT can be used, and a complete removal of the mesh is not needed.
The patients must be selected carefully for a synthetic mesh bridging using a skin cover. Synthetic mesh is contraindicated in contaminated or infected cases. In addition, if there are co-morbidities like obesity or diabetes, and/or if patient-related risk factors like smoking, immunosuppressive therapy, poor nutritional status etc. exist, a biologic mesh can be considered. Biologic meshes support tissue regeneration and revascularization. There is minimal risk for adhesion formation, and they do not have to be removed in the case of infection (28). A biologic mesh should be placed with 2–3 cm overlapping of the fascial edge. This removes the tension from the cutting edge of the fascia. There are several biologic meshes available. They can be human- or animal-derived, and either cross-linked or non-cross-linked matrices. There are not sufficient data showing which product would be the best one. The disadvantage of the biologic mesh may be some laxity or bulging observed over time (29). If the biologic mesh is exposed, NPWT can be used on top of it (23). If a direct closure is not possible after NPWT, a formation of granulation tissue allows application of a skin graft on the biologic material.
SUMMARY
“Open abdomen” is a widely adopted treatment in abdominal emergencies. The main goal after the OA situation is to stabilize the patient's condition and achieve primary abdominal closure as soon as possible within the initial hospitalization. Temporary closure methods should be used to prevent adhesion formation between the abdominal wall and viscera and to form traction between the fascial edges. A closure of the OA can usually be achieved during the primary phase of treatment with CS, mesh augmentation and perforator saving skin undermining without a need for a skin graft or a flap reconstruction.
