Abstract
Background: During the COVID-19 pandemic, office workers were displaced from their places of employment. This situation caused a heightened interest in understanding viral disease transmission in indoor spaces including offices. Although data has been published on the survival of various coronaviruses including SARS-CoV-2 on a variety of surfaces, most related to impermeable materials common to healthcare environments. Methods: We studied two typical contract fabrics (polyester and wool) and cotton for HCoV-OC43 (ATCC #VR-1558) persistence up to 24 h using a modified ISO 18184 test protocol. Results: We found that HCoV-OC43 was undetectable after 12 h on cotton fabric, 24 h on polyester fabric, and was reduced by 93 +/− 6% within 24 h on wool fabric compared to an inoculum-only control. Differences in droplet-fabric contact angles were observed for the three fabrics, and absorption correlated with virus inactivation. Conclusions: Polyester and wool exhibit virus-inactivating properties similar to cotton, although the degree of inactivation is different between the three materials. Liquid absorption is likely a key factor involved in the inactivation process. When the results are extrapolated to real-world environmental temperature and relative humidity conditions, commonly used fabrics in interior offices spaces are determined as unlikely sources of human coronavirus transmission.
Keywords
Introduction
SARS-CoV-2 pandemic
The COVID-19 pandemic hit the world by surprise with huge costs in terms of lives lost, financial burdens, family isolation and worldwide disruption. For months or longer, most people throughout the world experienced some version of “sheltering in place”, and most “non-essential” offices and businesses were temporarily forced to cease operations, becoming unoccupied.
Even with vaccinations being rolled out in 2021, the occurrence of variants continues to affect the timing and return of employees to office spaces and traditional working environments. Workplaces in the United States have conformed to national guidance from the Centers for Disease Control and Prevention (CDC) 1 and Occupational Health and Safety Administration (OSHA) 2 as they developed to keep workers safe. These organizations provide critical guidance to employers on the specific strategies and procedures to allow employees back to the office.
In the Autumn of 2021, the demand for office spaces appears to have hit an inflection point and is beginning to rise. As of September 2021, approximately 40% of all global office workers have returned to the office, and some conclude most workers are predicted to return to the office in the first quarter of 2022. 3
Even with clarified guidance and increasing plans to return to the office, there are still unanswered questions about how specific indoor environments, particularly interior office environments and their associated materials of construction, play a role in disease transmission. How and when a worker will return to the office has been a complex choice driven partially by the type of work, employers’ demands and the employee comfort level. To the extent that the office space can be made as safe and healthy as possible, it is incumbent on employers, designers, engineers, facilities managers, and all others involved in designing, constructing and managing an office space to understand potential pathogen transmission in these spaces and methods for mitigation. Over time, research has proven that COVID-19 is primarily transmitted via air in the form of droplets (in close proximity) or particles (at a distance from the exhaler), rather than through touch transmission via fomite surfaces. 4 Nevertheless, understanding how SARS-CoV-2 virus, and viruses in general, interact with various workplace surfaces is essential for understanding our workplace material environment, potential for disease transmission and methods of mitigation.
Indoor office built environments
According to the last Commercial Buildings Energy Consumption 5 survey conducted in 2018 by the U.S. Energy Information System, there were 5.9 million commercial buildings in the U.S. of which 940,000 were office buildings. These office buildings contained 16.5 billion sq. ft. (1,532,900,160 m2) of office floorspace, second only to floorspace used for warehouses and storage. There were over 88 million professionals in the U.S. in 2020, 6 who likely worked in some kind of office space.
Categories of typical furnishings in an office and their materials of construction.

aA variety of fabric fibres is used in contract furniture applications, including primarily polyester, wool, nylon, blends of these fibres and coated fabrics.
As shown in Table 1, there is quite a variety of materials of construction for offices in the built environment. In general, the materials can be divided into two groupings: structural and surface. This distinction is important since the user of the furniture touches the surface of the product. Note that some materials are both structural and surface materials since they are made of solid materials.
Surface materials can be further divided into hard and soft surfaces. Soft surfaces consist primarily of fabrics, whereas hard surfaces consist of painted surfaces, laminates and veneers. Specialized fabrics are engineered for “contract” applications to be durable to withstand rugged use in semi-public spaces. All contract fabrics are designed for aesthetics, since people prefer to work in beautiful environments. Other categories of performance criteria for contract fabrics include flammability, wet and dry crocking, colorfastness to light, abrasion and physical properties such as breaking strength and pilling.
In offices, fabrics are primarily used for seating and panels. The total U.S. market for contract textiles for 2019–2021 has been estimated at $6 billion. 8 For the U.S. interior design industry, 39% of projects were for corporate offices, by fees. 8 This is in comparison to other interior built environments such as hospitality, healthcare, government, residential, education and retail.
Fabrics in the contract textile market are constructed of several yarn types as well as yarn blends. A large proportion of these textiles are made of polyester, and a smaller amount is made from wool. Cotton is generally not used for a variety of reasons including lack of both durability and fire resistance in panel and drapery use.
Fabrics, the indoor office work environment and the pandemic
Early in the COVID-19 pandemic, surface materials received much scrutiny for their ability to withstand vigorous disinfection routines for which they typically had not been designed or selected. This was also a time when the mode of SARS-CoV-2 transmission had not been clarified as primarily airborne. For high touch surfaces primarily in the case of SARS-CoV-2, and for any other virus that may be transferred via touch and fomite surfaces, disinfecting soft surfaces without causing unintended damage is a challenge. There are very few disinfectants determined to be effective and appropriate for use on standard contract fabrics such as those made with polyester, wool and/or cotton. As of November 2021, of the 580 disinfectants on EPA’s List N-COVID-19 Disinfectants, only 10 were listed as effective on porous, non-launderable surface types. 9
Because of our collective experiences, we learned about both the resistance of surface materials to the main families of disinfectants (bleach, sodium hypochlorite, alcohol, hydrogen peroxide and quaternary ammonium), as well as which technologies can help deactivate viruses and be implemented as components of the contract fabric itself. Active ingredients to control microbes (such as those based on silver and copper) are used in fabrics typically for non-public health purposes, such as to control odours. Inhibiting viral disease transmission had not been as much of a concern or necessity until the SARS-CoV-2 pandemic. To our knowledge, no contract fabric had been designed to withstand or otherwise deter virus persistence on their surface or to inhibit disease transmission until the COVID-19 pandemic. Worth noting is that the use of antiviral or antimicrobial substances in the built environment is a debated topic, and many organizations persistently avoid use. 10 Therefore, the inherent ability of contract textiles to inhibit viruses without the use of antimicrobial additives is an important topic of concern to those interested in the indoor built environment.
Virus persistence data on various surfaces including cloth and cotton
To understand the possible role that surface materials could have on SARS-CoV-2 transmission, we conducted a “rapid review” literature search in April 2020 about SARS-CoV-2 and surfaces. We justified this rapid process because of the urgency of the need for the review. We relied primarily on published reviews in the clinical literature as well as expert guidance (such as the CDC and WHO). This process was supplemented by retrieving key references found through searching PubMed or in citations in the review articles. We prioritized information on SARS-CoV-2, but since the amount of information was limited, we also reviewed the literature on other human coronaviruses such as SARS-CoV-1, HCoV-229E and HCoV-OC43.
van Doremalen et al. 11 published the first paper addressing SARS-CoV-2 persistence on a few surfaces (better known as fomites in healthcare). These included copper, cardboard, stainless steel and polypropylene plastic. Others12,13 reviewed the literature on the persistence of human coronaviruses (HCoV) in general on a wide variety of surfaces. A few studies 14–19 published results on a variety of surfaces that included soft, porous surfaces such as “cloth” and cotton in their experiments.
While conducting this review, we noticed that cotton fabric samples exhibited shorter viral persistence than other hard, nonporous materials tested (excluding copper). This was interesting considering that many specifiers for the office built environment had shied away from soft porous surfaces due to their incompatibility with harsh disinfectants and the perception that soft surfaces were less hygienic.
We were particularly interested in whether shorter viral persistence on cotton materials would apply to other contract fabrics made from different yarn types. However, the only data we found on fabrics was for cotton-based materials. Other fabric-like materials that were tested were those found in a hospital (including disposable gowns and Personal protective equipment (PPE) masks). 14 However, the exact material composition was not explicitly described. Additionally, due to variations in experimental methods, it was difficult to compare results from different studies. The major variations included the volume, concentration and composition of inoculant; ageing conditions such as temperature and humidity; and whether the samples were dried before testing.
Methodological testing conditions and human coronavirus persistence on “cloth” or cotton.
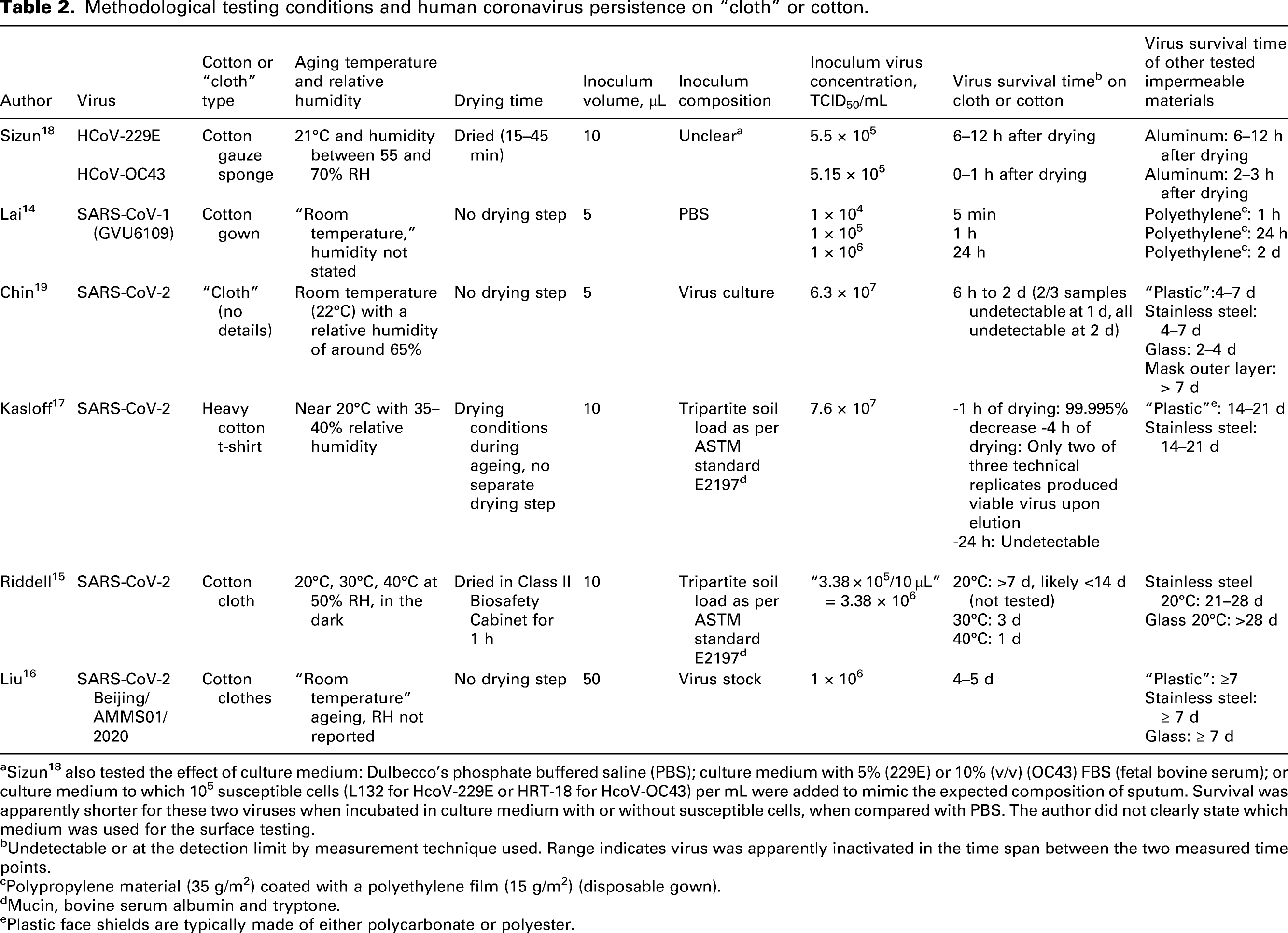
aSizun 18 also tested the effect of culture medium: Dulbecco’s phosphate buffered saline (PBS); culture medium with 5% (229E) or 10% (v/v) (OC43) FBS (fetal bovine serum); or culture medium to which 105 susceptible cells (L132 for HcoV-229E or HRT-18 for HcoV-OC43) per mL were added to mimic the expected composition of sputum. Survival was apparently shorter for these two viruses when incubated in culture medium with or without susceptible cells, when compared with PBS. The author did not clearly state which medium was used for the surface testing.
bUndetectable or at the detection limit by measurement technique used. Range indicates virus was apparently inactivated in the time span between the two measured time points.
cPolypropylene material (35 g/m2) coated with a polyethylene film (15 g/m2) (disposable gown).
dMucin, bovine serum albumin and tryptone.
ePlastic face shields are typically made of either polycarbonate or polyester.
The exact lifetime of human coronavirus on surfaces is variable, which is expected considering that the authors used a variety of experimental methods. However, all studies show shorter virus persistence on cotton (or “cloth”) than impermeable materials (aluminium, stainless steel, glass and various plastics).
The data show promise for cloth and cotton fabrics to have an inherent virus-inactivating property without the presence of antiviral or antimicrobial active ingredients. Our goal is to explore the possibility of an inherent virus-inactivating property by first understanding if it was generalizable to fabrics made from other yarn types, particularly those prevalent in the contract fabric markets used in office built environments.
Common indoor contract fabrics knowledge gap
There is a gap in knowledge about the persistence of viruses on fabrics besides cotton. The data on cotton fabrics showed an interesting trend in that virus persistence was noticeably lower on these materials than impermeable surfaces (excluding copper 11 ). Researchers speculated porosity was the reason for decreased viral persistence on cotton fabrics. Riddell et al. 15 cited the process of drying down as being a significant factor, as well as adhesion of the virus to the yarn, which hinders the recovery of the virus during testing. Kasloff et al. 17 noted the possible effect of the increased surface area changing the drying phenomena as being responsible for lower virus persistence on cotton and possibly other porous materials. This downplays the virus-surface adhesion theory as the sole mechanism for decreased active viral recovery from cotton fabric.
Yet basic questions remain as to whether all porous fabrics exhibit low persistence, or if uniquely cotton fabrics have this property. Knowledge of the virus persistence on fabrics other than cotton would not only help to understand materials highly prevalent on furnishings in office environments but also establish the underlying physical and chemical mechanisms of virus survival in microenvironments that undergo both drying and absorption at the surface–air–water interface. We aim to fill the gap of knowledge of virus persistence on fabrics other than cotton.
Experimental methods
Choice of fabrics for testing
We chose three commercially available fabric products for the study. Each fabric product was made with 100% polyester, wool or cotton yarns. All materials were contract or upholstery grade, which signifies greater durability than other grades of fabric. We based our choices on a balance of relevancy of the results to our end use application (indoor offices) and the ability to draw scientific conclusions from the results. No stain-repellent or other finishes were applied to the polyester or wool; however, the cotton fabric had a silicone softener on its surface.
Choice of virus
We chose to use human coronavirus HCoV OC43 (ATCC #VR-1558) as a surrogate for SARS-CoV-2. Although use of the SARS-CoV-2 virus itself would provide the most relevant data, the ability to obtain the virus and the need for BSL3 to handle the virus hindered progress. We also considered coronavirus HCoV 229E as our surrogate, but instead opted for OC43 because it is a beta coronavirus, and therefore more similar in structure to SARS-CoV-2.
Virus–fabric persistence test methods
We conducted a survey of standardized test methods that existed for studying viral persistence on fabrics. Many tests were found that could be adopted for our interests, such as ASTM E2197. 20 However, ISO 18184 21 was most closely aligned with our interests since it was specifically designed for testing viral persistence on fabrics and other porous materials.
According to ISO 18184, the viruses were deposited onto a specimen. After specific contact time, the remaining infectious virus was counted, and the reduction rate was calculated by the comparison between the antiviral product test specimen and the control specimen by common logarithm. There are two methods to quantify the infectious virus titer. One method is the plaque assay and the other is the TCID50 method. The selection of the method depends on the convenience and experience of the testing organization.
The following is a more detailed description of the methods employed: 1. Each fabric is cut into 0.40 g ± 0.05 g pieces of approximately 20 mm by 20 mm in size. 2. Each sample is inserted to form a cup shape at the top of a 50 mL tube as shown in Figure 1(a). 3. Each fabric swatch is inoculated with 200 μL virus inoculum of approximately 2.83 × 107 FFU/mL (for an initial virus inoculation of around 5.66 × 106 FFU/sample) suspended in a solution of Dulbecco’s Modified Eagle Medium (1x), with 2% Fetal Bovine Serum, Non-Essential Amino Acids (1x), Penicillin–Streptomycin (1x) and 0.5% 1M HEPES (4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid) (no artificial saliva components added) as shown in Figure 1(b). Note that depending on the fabric hydrophilicity/hydrophobicity, the inoculum may absorb immediately or after a few minutes. The inoculum was always thoroughly in contact with the fabric throughout the designated contact time. 4. Samples are capped and incubated at 35°C, 5% CO2 in a high humidity (>90%) incubator as shown in Figure 1(c). The maximum temperature deviation in the incubator is +0.1/−0.4°C that can occur when the chamber is opened to remove samples for testing. Relative humidity could dip to 50% for up to an hour during these events. 5. After specified incubation time at 0, 1, 2, 4, 12 and 24 h (+/−10 min), samples are removed from the incubator and recovered in 20 mL of modified SCDLP buffer. The composition of the specific SCDLP Buffer used is 17 g/L casein peptone, 3 g/L soybean peptone, 5 g/L sodium chloride, 2.5 g/L dextrose (glucose), 2.5 g/L dipotassium phosphate, Penicillin–Streptomycin (1x), and 0.1% BSA in DPBS. 6. Samples are vortexed for 1 min to fully recover virus from the fabric sample. Note that recovery is checked through confirmation testing at t = 0 for each sample. 7. Samples are dilution plated on Rhabdomyosarcoma cells (ATCC #CCL-136) in 24-well plates with an agarose plug placed on the top and then incubated for 24 h. 8. After incubation, samples are fixed with a 1:1 acetone/methanol mixture to prevent further growth, and the agarose plugs are removed. 9. Once fixed and dried, samples are stained with the Vectastain ABC mouse IG kit using mab 542-71 to develop foci. 10. Foci units are counted and calculated to determine the FFU/per sample, averages, outliers and log and percent reductions. Note that only viable viruses are detected by this method. (a) Fabrics prepped and placed inside tubes. (b) Virus inoculum pipetted onto fabric surfaces. (c) Fabrics aged at controlled temperature and humidity inside the incubator during contact time.

The methods of ISO 18184 were utilized as written with the exceptions that we (1) incubated at temperature of 35°C, (2) because of the nature of the question we were asking (in that no antiviral or antimicrobial treatments were used), we chose to use a virus inoculum of the same volume as that was used on the tested fabrics (with contact with no other surface except the container (polypropylene 50 mL tube)) as our control, and (3) we used the Focus Forming Assay to quantify the active virus.
Virus quantification: Focus forming assay
Although ISO 18184 specifies the use of TCID50 or plaque forming assays to measure the infectability of viruses after the exposure, we used focus forming assay which is an immunostaining technique and a variation of the viral plaque assay. Instead of detecting the plaque formation after virus-induced cell lysis, these assays detect infected host cells and infectious virus particles before a plaque is formed. 22 This technique is superior to other techniques because it is easier to detect than plaques due to their dark appearance in contrast with light, less susceptible to misinterpretation as cell monolayer damage over a viral unit, and the plates incubate for a shorter period of time, providing results more quickly.
Results
Fabric characterization
The fabric samples were characterized by optical microscopy as shown in Figure 2. Although all fabrics were woven, they had different weave constructions. Fabrics as observed by microscopy showing their constructions.
Droplet–Fabric Surface Interactions
The interaction of a droplet of water with each fabric surface was investigated to get a basic understanding of the capillary action, contact angle and surface energy of the three test fabrics as shown in Figure 3. Water droplet–fabric interactions by optical microscopy showing immediate absorption or hydrophobicity. Note that all drops are absorbed completely over time.
Although polyester completely and immediately absorbed the water droplet, cotton and wool did not. However, during the viral tests, all fabrics absorbed the virus inoculant within 10 min.
Virus persistence results
Figure 4 shows the average viral dose recovered from each fabric after exposure to the virus inoculum at each time point for each of the fabrics. Average viral dose recovered at various time points up to 24 hours for the fabric samples.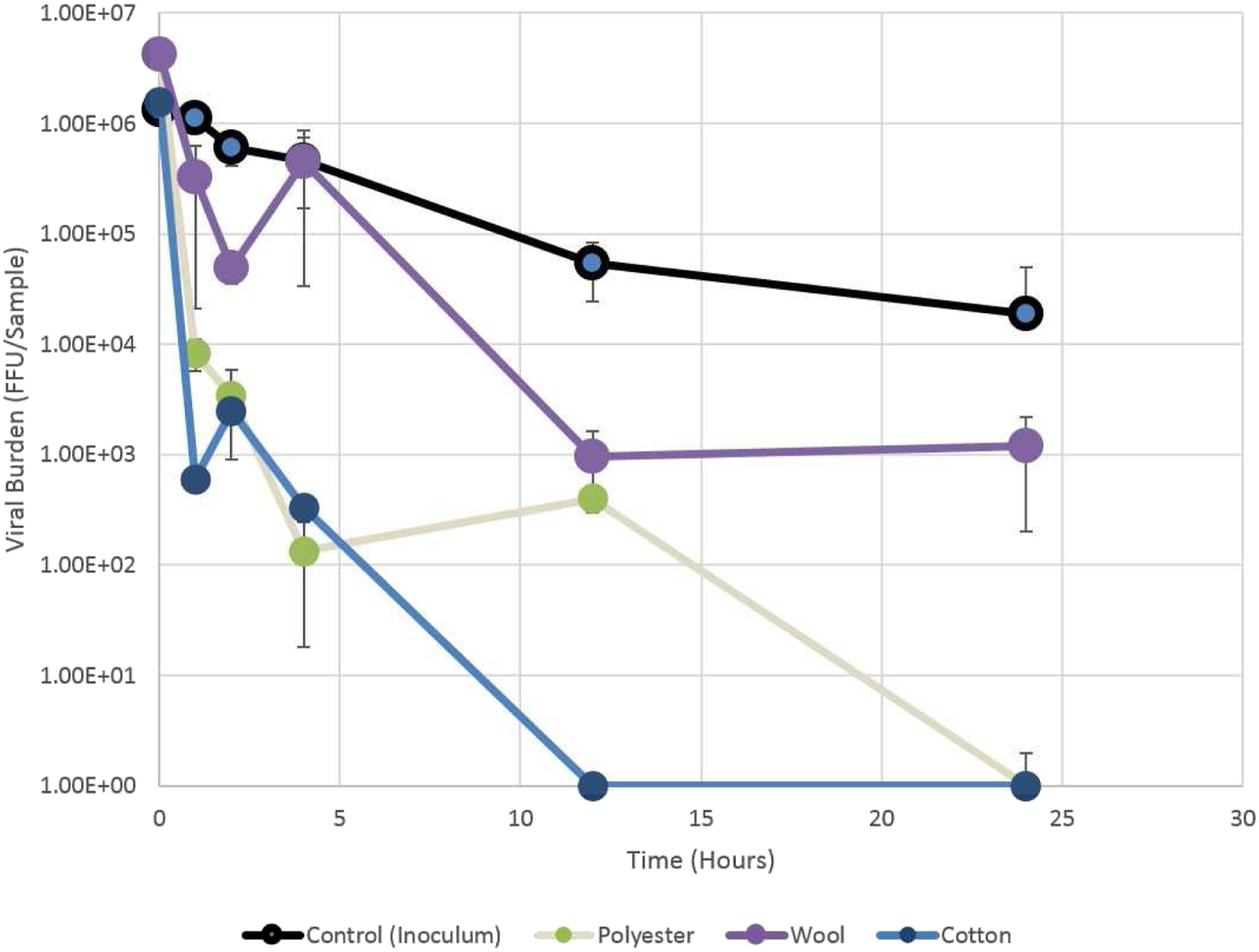
The recovered virus concentration was between 1.34 × 106 FFU/sample and 4.27 × 106 FFU/sample at t = 0, showing the same order of magnitude of virus recovery as virus inoculation.
Although the viability of the virus in the inoculum (with no surface contact) decreases to some extent over the 24-h period, the virus in contact with all fabrics showed a larger and faster decrease in viable virus dose recovered over time.
The fabric results can be summarized as follows: 1. Cotton fabric showed the shortest viral persistence (no virus detected at 12 h) and fastest inactivation. 2. No virus was detected on the polyester fabric by 24 h. 3. Virus persistence on the wool sample was reduced by 93 ± 6% at 24 h compared to the inoculum control and did not become undetectable within the experimental time frame.
Discussion and generalizability
Effect of fabric fibre type on virus persistence
Anecdotally, “naturally” derived wool and plant fibre–based fabrics are often reported to have innate antibacterial properties, and some scientific studies on wool components 23 and plant-based fibre components 24 have confirmed antibacterial properties. Cotton without antimicrobial treatments 25 is not found to be antibacterial to our knowledge. However, whether fibre components, fibres, or fabrics made with these various materials exhibit virus-inactivating properties is largely unknown except for the results summarized on cotton herein.
We confirmed that cotton fabric exhibits an inherent virus-inactivating property as has been reported in the literature, reaching undetectable recoverable virus dosage at 12 h in our test conditions. However, wool was not found to share this virus-inactivating property to the same degree, never reaching an undetectable recoverable dose within 24 h. It must be remembered, however, that there are no antiviral or antimicrobial treatments on any of these fabrics, so even an average 93% inhibition rate compared to the control is quite beneficial.
We were surprised to learn that polyester exhibited a virus-inactivating property, reaching undetectable recoverable dose by 24 h, and better performing in this respect than wool.
Thus, porous fabric materials all have a virus-inactivating effect, although there are differences in the degree of inactivation based on (at least) the fabric fibre type. The “natural” versus synthetic origin of the fabrics was not found to be a determining factor.
Role of environmental conditions (temperature and humidity) on virus persistence
The stability of coronaviruses decreases with increasing temperature (between 10°C and 40°C).13,26 The effect of relative humidity (RH) is not linear and exhibits a U-shape, with the lowest stability between 40 and 65% RH. 26 The complex relationship between coronavirus stability, temperature, and RH has been studied mechanistically, and can be explained by basic chemical kinetic principles such as reactions proceeding faster at higher temperatures and higher solute concentrations. 26 Our situation has the added complexity of including an absorbing and not inert surface that provides another route for virus deactivation besides temperature and drying kinetics.
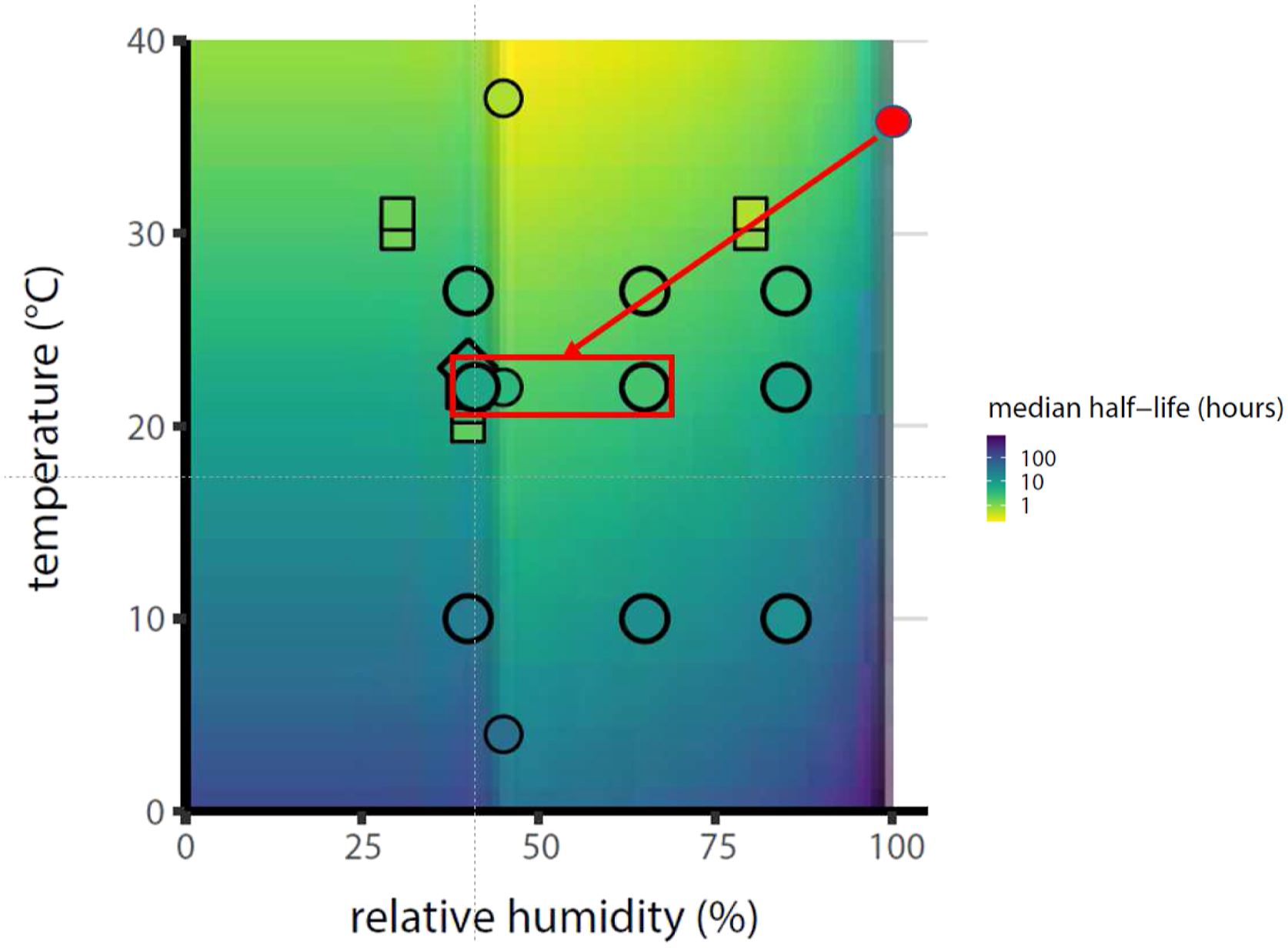
In Figure 5, we compare the conditions of our testing (35°C and 100% RH) to those of a suggested indoor environment (22°C, 40–65% RH)
27
by overlaying these conditions on Figure 3(c) of Morris et al.,
26
which is a heatmap showing posterior median predicted virus half-lives (results from their study and others) as a function of temperature (T) and RH. The red dot at the right side of the figure represents the testing conditions, and the red arrow points to a red box showing the range of T and RH for office environments. Note that the virus shows more stability in the lab testing conditions than the office conditions, indicating our results likely over-estimate the time of survival and length of persistence in real-world office conditions. Overlay of our lab testing conditions (red dot) and real-world suggested office environments (red box) onto human coronavirus stability according to temperature and relative humidity. Adapted from Morris et al.
26
Role of drying on virus persistence
Chatterjee 28 reported on why viruses are less persistent on porous, permeable surfaces than impermeable surfaces. Their explanation relies heavily on the role of droplet drying, and the competing effects of diffusion-limited evaporation from impermeable surfaces versus capillary absorption and droplet spread on permeable surfaces. When a virus-laden droplet soaks into the fabric, it is spread over a large surface area of fabric yarns and fibres, creating a thin film. Thin films of water evaporate more quickly than thick films; therefore, viruses are less stable on porous, permeable materials like fabrics than impermeable materials.
The explanation of drying per se may not be applicable to the results of this study, because the samples were never dried. They did experience differences in absorption due to different capillary forces, however. With our results, we have unlocked new questions relating to understanding deeper questions about how fabric properties, such as absorption, might influence virus persistence.
Role of absorption by porous, permeable materials (fabrics) on virus persistence
Spontaneous mobility of liquid droplets in fibrous substrates has been studied. 29 There are clear relationships between the size of pores and absorption behaviour, capillary force, droplet shape and wetted area. The contact angle of the liquid on the surface is predictive of the ease of liquid penetration and is dependent on fibre diameter and spacing between fibres.
Capillary action or wicking of performance fabrics has been studied. 30 There are differences in fibre–water interactions between cellulosic fibres (which absorb water, swell and dry slowly) versus synthetic fibres (which do not absorb water, wick water along their surfaces and dry quickly). Capillary forces arise from wetting, and the degree of absorption is a balance between the cohesive and adhesive forces of the water–fiber system. When adhesion is greater than cohesion, fluids flow.
To understand if absorption played a role in virus inactivation in our studies, we measured the absorption capacity of our three fabrics using a Gravimetric Absorbency Testing System (GATS). This system measures the demand wettability of the test fabrics. This test indicates the lateral wicking ability of the fabric, or the ability of the sample to take up liquid spontaneously in the direction perpendicular to its plane. Figure 6 shows the results. Demand wettability (absorption) of the fabrics. C = cotton, P = polyester, W = wool.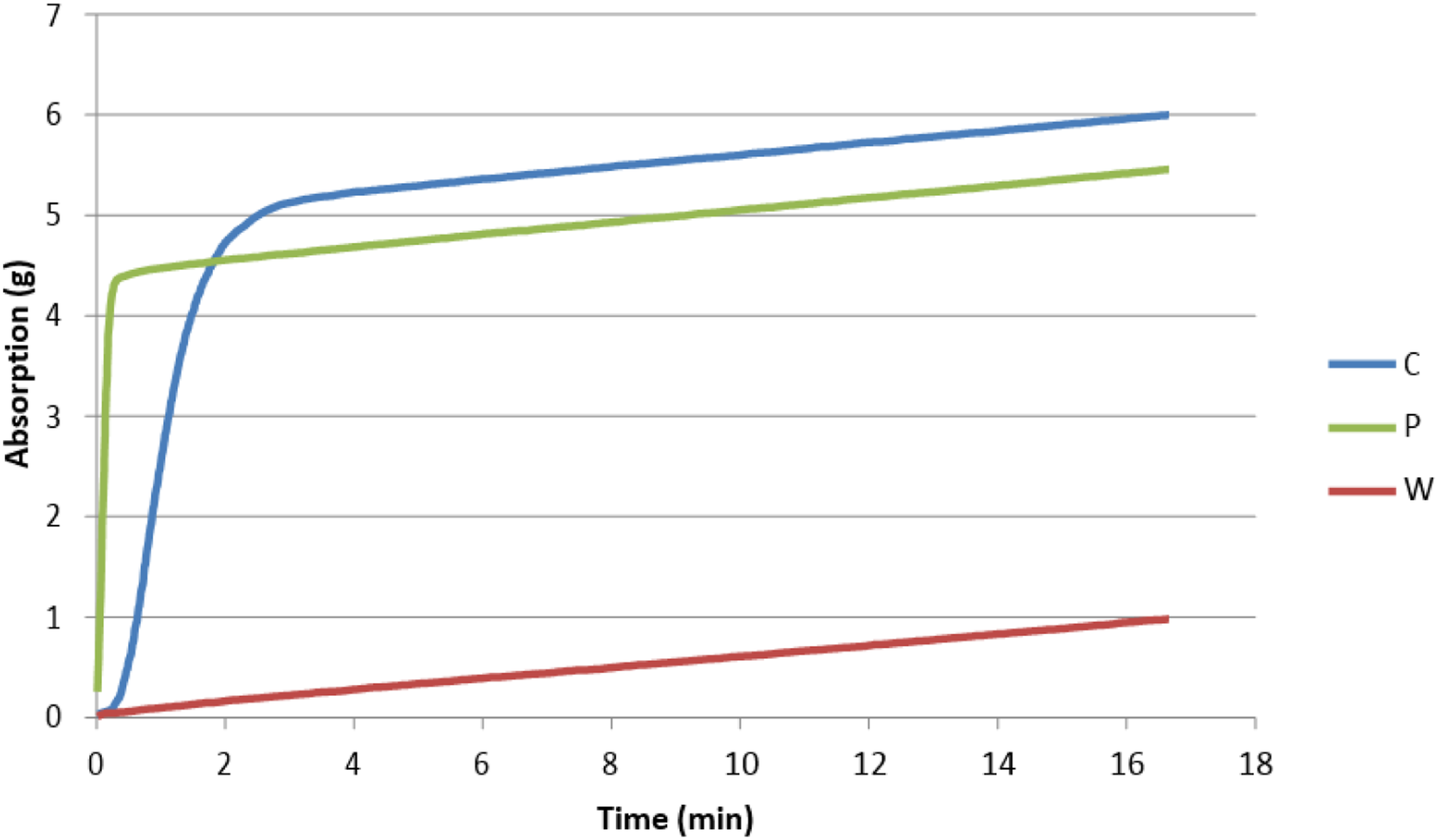
The results show a correlation between absorption capacity and virus stability, that is, the fabric with highest absorption capacity (cotton) had the fastest virus inactivation, polyester was second and wool last.
Clearly, differences in absorption propensity exist between porous, absorptive fabrics of different physical and chemical compositions. It is likely that these differences may cause viruses to destabilize to different degrees and at different rates, which may lead to controllable virus inactivation properties.
Role of virus adhesion to fibre surfaces on results
The simple explanation of virus adhesion to the high amount of surface area on fibres in fabrics does not seem to be the sole explanation of the lack of active virus recovery from the fabrics (leading to the conclusion of virus inactivation on fabrics), since our results showed the same order of magnitude of recovered virus at the 0 time point from all fabrics in comparison to the inoculated concentration. This check does not rule out the possibility of time-dependent adsorption of virus to the fabric surface, but it does provide evidence against purely adsorption to fibres in the fabric as a reason for the decrease in active virus recovery over time.
Discussion summary
Our data shows that the fabric’s absorption propensity has the most likely bearing on virus persistence (higher absorption correlates with shorter persistence). The yarn/fibre type has some bearing in so far as it enhances rather than diminishes absorption. Enhanced drying cannot be the sole reason for shorter persistence of coronaviruses on permeable fabrics versus impermeable surfaces. Measurement error due to experimental limitations of virus adhesion inside the fabrics is also not supported.
Potential limitations to extrapolating these findings to real-world office environments include the difference in the coronavirus survival in real respiratory fluids versus simplified fluids used in laboratory experiments. Data show that basic chemical principals apply to understanding virus survival as it relates to T + RH, and the exact detailed knowledge of identities and quantities of non-virus reactants may not be necessary. 26
We need to be cautious when extrapolating a simplified, testable experiment to real-world scenarios. Even though we conducted our study on HCoV OC43, we suggest that we can extrapolate findings to SARS-CoV-2 as well as influenza viruses. This is because viruses can generally be classified according to a disinfection hierarchy model, and that medium-sized enveloped viruses can generally be considered in the same class when it comes to disinfection.31,32
Our study has simplified the complex “real world” environment into a study of one temperature, one drying condition at one relative humidity, and focused on measuring the effect of a combination of real-world fabrics (with different porosity, structures and single fiber types) to begin to understand virus persistence on common materials in indoor environments such as offices. Our hope is to create learnings that will provide designers and specifiers the information needed to limit transmission of disease-causing viruses, and HCoV specifically, in office environments. Although our conclusions are based on laboratory studies, we are cautiously optimistic that they can be extrapolated to real-world office conditions because of existing knowledge as described in previous sections.
Conclusions
These results indicate that typical contract fabrics like polyester and wool exhibit a coronavirus-inactivation property in a similar way to that shown for cotton fabrics, as confirmed in this study, and shown in a variety of studies in the literature. We found that HCoV-OC43 was undetectable at 12 h on cotton, 24 h on polyester, and reduced by 93 +/− 6% within 24 h compared to the control on wool. Fabric absorption capacity is a key physical property correlated with virus inactivation. Typical contract fabrics in office environments (at conditions of 22°C and 40–65% RH) are not likely fomites supporting coronavirus transmission.
Footnotes
Acknowledgments
We thank Melissa Hart and Sherrie Willson of Steelcase for their help in selecting the most relevant fabrics for study of the indoor office environment. We would also like to thank Allan Smith, James Ludwig, Derek Ludwig, Terry Lenhardt, Jody Hanson, and Kurt Heidmann for supporting funding this work at Steelcase, Inc. We would also like to thank Sophie Guevel from the Textile Protection and Comfort Center from the Wilson College of Textiles at the North Carolina State University for the GATS testing and data.
Author contributions
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by Steelcase, Inc. ST and CD are employees. NV and MH were contracted through ResInnova to perform the antiviral lab testing and analysis.
