Abstract
Background
Steatosis hepatis is of outstanding clinical importance. The aim of this study was to apply the new parametric method “Ultrasound Derived Fat Fraction” (UDFF) to monitor changes of liver fat in obese patients undergoing weight loss measures.
Methods
In 53 obese patients BMI, absolute body fat, waist circumference and UDFF were measured before and after a three-month weight loss intervention. UDFF measurements were performed using a Siemens ultrasound system (DAX, 1.0–3.5 Mz). We analysed the correlation of change in BMI (≥−1 vs < −1), body fat (≥−2 kg vs < −2 kg) and waist circumference (≥−10 cm vs < −10 cm) with the change in UDFF (≥−30% vs < −30%) (significance level: p < 0.0167).
Results
At baseline, mean BMI was 39.2 (range: 29.8–63.6), body fat 51.3 kg (range: 29.9–111.7), waist circumference 120.2 cm (range: 95–164) and UDFF 26% (range: 7–41%). 54.7% of patients lost at least 2 kg of body fat. These patients were significantly more likely to have a reduction in UDFF of at least 30% (≥2 kg fat: 58.6% vs. < 2 kg fat: 20.8%; p = 0.011). For BMI and waist circumference changes no significant correlation with UDFF was observed.
Conclusion
This study underlines that UDFF could be a promising, non-invasive tool to monitor changes in liver fat.
Introduction
Obesity is a complex chronic disease in which excess body fat (adiposity) impairs health, increases the risk of long-term medical complications (e.g. steatosis hepatis) and reduces lifespan. 1 Among several comorbidities steatosis hepatis is a risk factor for the development of liver cirrhosis. 2 A quarter of the world's population is affected by steatosis hepatis and the prevalence is increasing.2,3 Many guidelines therefore recommend screening for steatosis hepatis in the presence of metabolic syndrome2,4,5 and new ultrasound based parametric techniques are available to monitor these patients.6–9 For all patients with Metabolic Dysfunction-associated Steatosis Liver Disease (MASLD) lifestyle modification (e.g., dietary changes, physical exercise) is advised by guidelines (e.g. the EASL guideline). 4
The degree of fatty liver can be assessed accurately by liver biopsy, but this procedure is not suitable for screening or surveillance due to its invasiveness and complexity.10–12 An alternative non-inverse method is MRI proton density fat fraction (MRI-PDFF). 13 However, this procedure is not widely available and is expensive. Therefore, in clinical routine, liver fat is frequently assessed sonographically by comparing the echogenicity of the liver parenchyma in B-Mode with the right kidney. However, this non-parametric method is limited in sensitivity, particularly in cases of low-grade hepatic steatosis4,14,15 and depends on the sonic conditions into the retroperitoneum. 15 An increase in the echogenicity of the liver parenchyma is only seen when around 30% hepatocytes accumulate fat droplets. 16 The sensitivity and specificity of ultrasound at detecting moderate to severe steatosis, using histology as reference standard, are 80–89 and 87–90%, respectively.17,18 The sensitivity and specificity drops to 65 and 81%, respectively, when all grades of steatosis are considered. 17
Several parametric methods have been developed to determine the fat content of the liver by measuring the attenuation of ultrasound waves in liver tissue.9,19 These include ‘Controlled Attenuation Parameter’ (CAP) and ‘Attenuation Imaging’ (ATI), both of which showed a correlation with the degree of fatty liver by measurement of the attenuation of sound waves.11,20,21 Recently, the two promising parametric techniques TAI (Tissue Attenuation Imaging) and TSI (Tissue Scatter Distribution Imaging) have shown good results, with TAI achieving higher diagnostic accuracy than TSI. 22 The accuracy of these procedures is limited in obese patients due to attenuation by more subcutaneous fat. Therefore, the UGAP (Ultrasound-Guided Attenuation Parameter) method was developed, which is less susceptible to a deterioration in diagnostic accuracy in obese patients. 23 Recently, Siemens has developed another new method called ‘Ultrasound derived fat fraction’ (UDFF). 24 In addition to the attenuation of the ultrasound waves, this method analyses the backscatter coefficient in the liver parenchyma. The microstructure of the tissue influences the backscatter coefficient which has been shown to correlate with the amount of intrahepatic fat.8,25–27 This combined measurement as well as the deeper penetration depth due to the lower frequencies used 28 could improve the measurement in obese patients. UDFF is measured in a few minutes and the results are expressed as fat fraction in percent. Most recently, UDFF was found to have a better correlation with MRI-PDFF than both CAP and the hepatic/renal echogenicity ratio. 29 UDFF was also shown to be a reliable and accurate method for the quantification and classification of hepatic steatosis, with strong agreement to MRI-PDFF. The UDFF cut-off values of 5.5%, 15.5%, and 17.5% provide high sensitivity and specificity for the detection of mild, moderate, and severe hepatic steatosis, respectively. 30
The aim of this study was to evaluate the potential usefulness of UDFF for monitoring intrahepatic fat in obese patients following a standardized lifestyle modification. Already available methods such as sonographic assessment based on B-mode imaging are not sensitive enough, and validated MRI-based methods are only available to a limited extent. Furthermore, the CAP used in a weight reduction study before 31 is presumably more susceptible to measurement errors in obese patients than UDFF.32,33 We selected obese patients in particular because of their reduced prognosis and life expectancy. Moreover, this enables analysis of possible changes in steatosis hepatis after weight loss. We now present our first results of an ongoing clinical trial.
Methods
Patients
The present pilot study included data from 57 patients with obesity participating in a randomized controlled, prospective trial on lifestyle interventions, conducted by the Department of Medicine 1 at the University Hospital Erlangen, Germany. All patients were obese with obesity defined as a BMI greater or equal 30 kg/m2 and/or a waist circumference exceeding sex-specific reference cut-offs (80 cm for females, 94 cm for males). Patients fulfilling all criteria were subsequently enrolled in the study.
The intervention included dietary counseling for weight loss in accordance with clinical guidelines, combined with exercise recommendations based on WHO standards. This comprised a mediterranean diet regime with a net energy deficit of 500 kcal in relation to usual energy requirement 34 and interval ergometer training. 35 The patients did not take any weight-reducing medication.
All patients of the intervention study were included in our analysis after checking the exclusion criteria. Two patients were excluded from the study due to sonographic evidence of liver cirrhosis. This condition is discussed as a possible confounding factor affecting the UDFF measurement due to structural transformation. 36 Furthermore, two patients with an initial UDFF value of < 6.3% were excluded because this value rules out fatty liver disease. 37 Thus, data of a total of 53 patients were analyzed before and after three months of intervention (Figure 1). The vascularization of the liver was regular.
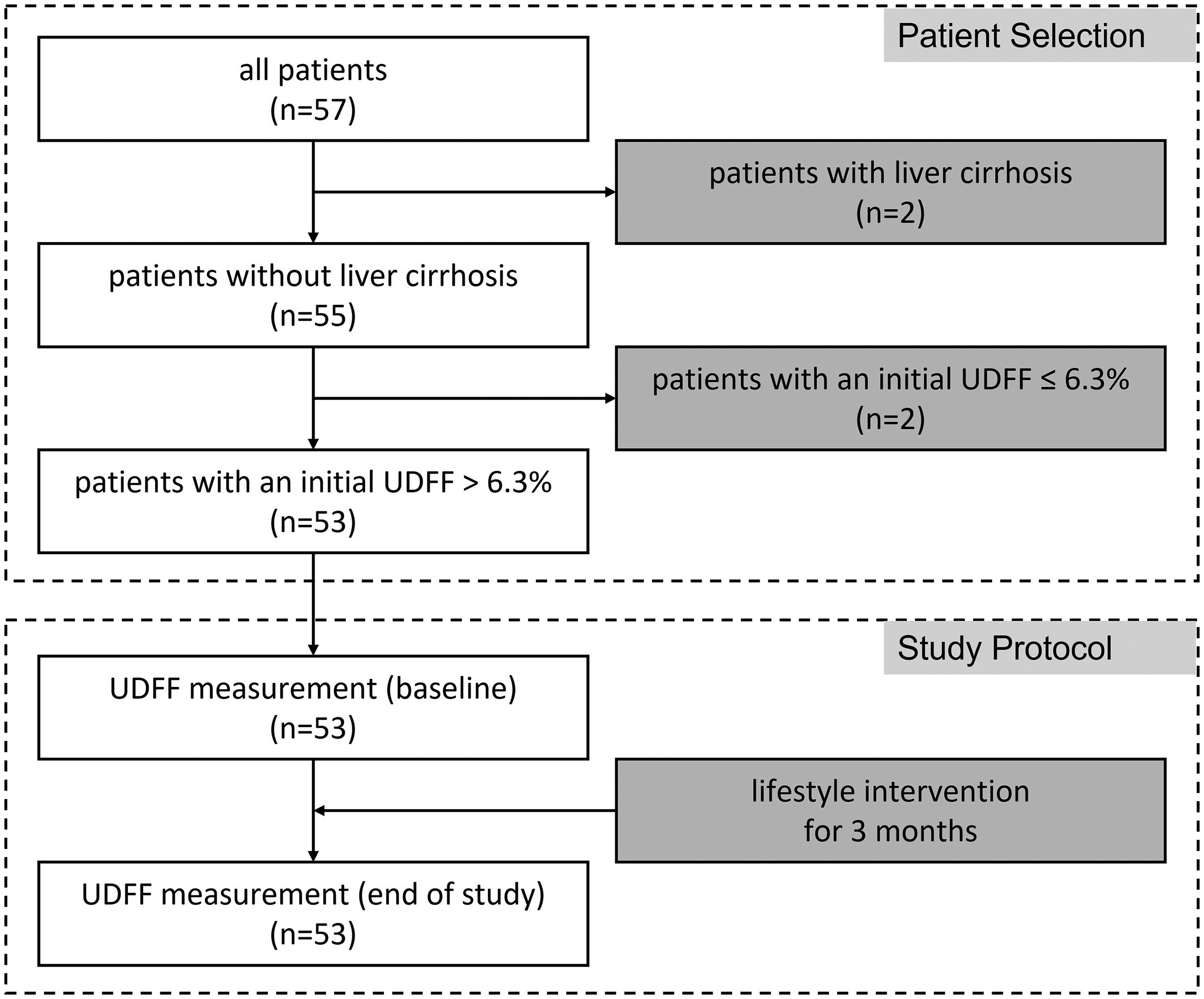
Flowchart - Patient selection and study protocol.
Lifestyle intervention and measurement of body fat
Body composition was measured using bioelectrical impedance analysis (BIA) with the InBody 970 device, following the manufacturer's instructions. BIA estimates body fat by measuring the resistance of body tissues to a small electrical current, since fat tissue conducts electricity less efficiently than lean tissue. Participants were required to fast for at least 8 h and sit for at least 5 min prior to the measurement.
The absolute body fat (in kg) was determined by multiplying the percentage of body fat by the body weight (in kg) and dividing the result by 100 (e.g., 150 kg body weight×50% body fat /100 = 75 kg body fat). Finally, the difference between the values for the absolute body fat before and after the intervention was calculated.
All participants received dietary counselling on the mediterranean diet and exercise recommendations based on WHO standards
UDFF measurements
UDFF was measured at the start and end of the intervention using a deep abdominal transducer (DAX, 1.0–3.5 MHz) on a Siemens ACUSON Sequoia ultrasound device according to the manufacturer's specifications. In addition, the recommendations of the World Federation for Ultrasound in Medicine and Biology were taken into account. 9 Patients were in a supine position, abducting their right arm and holding their breath shortly during each measurement. The measurement was taken in the right lobe of the liver using an intercostal approach, perpendicular to and 1.5 cm below the liver capsule (Figure 2). The result is given as a percentage value. Afterwards, a median was derived for each visit based on five repeated measurements per patient. Finally, it was investigated whether the UDFF was reduced by at least 30% (relative). This threshold value was based on a meta-analysis of MRI studies on hepatic steatosis with analysis of histological changes (see Discussion for details).
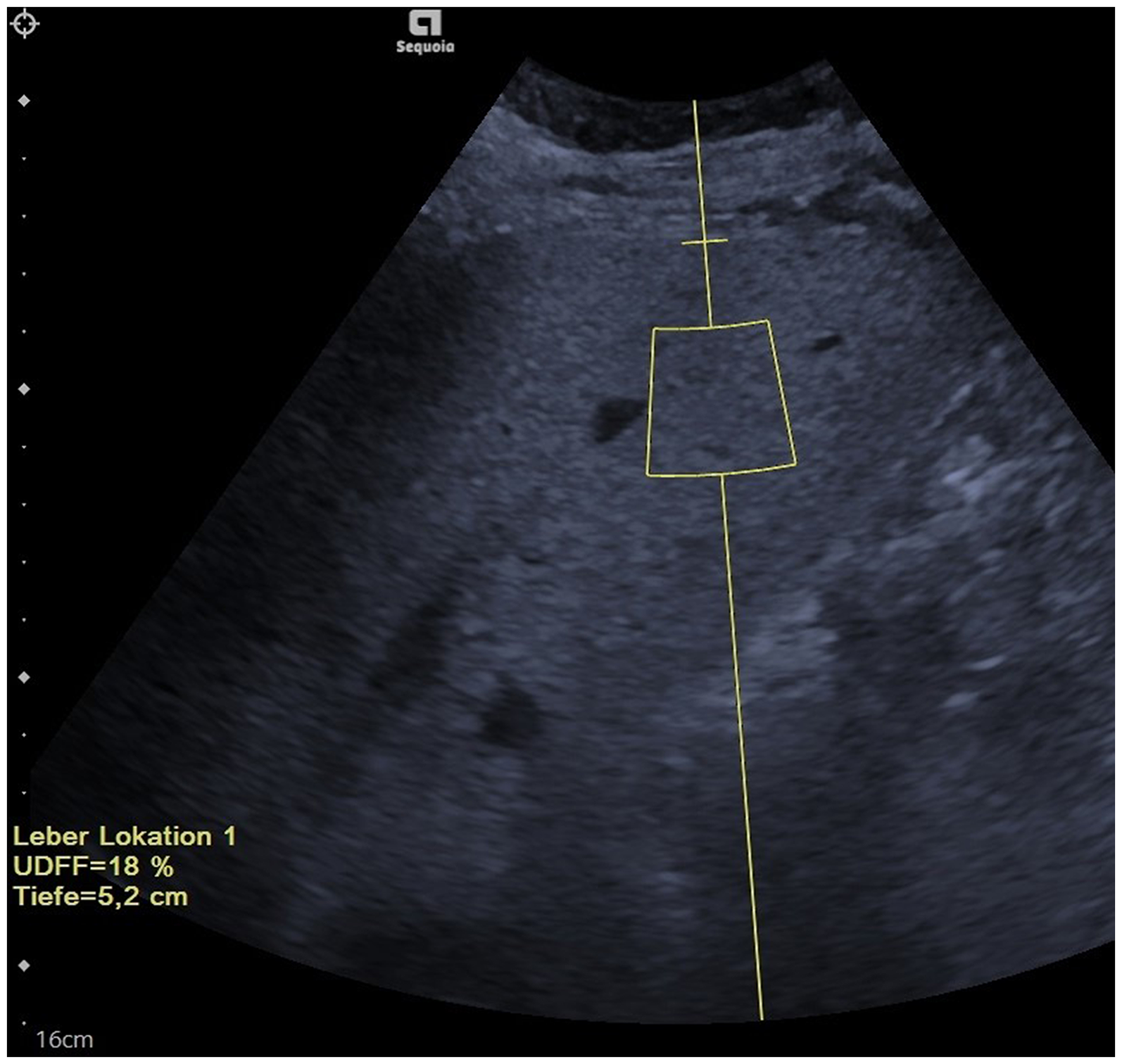
Exemplary UDFF measurement in a patient.
Statistics
The statistical analyses were conducted using the software RStudio (Version 1.4.1106; R Version 4.2.1). For the analysis of the impact of BMI, body fat change and waist circumference on UDFF the Fisher's exact test was employed (cut off: 30% relative reduction of UDFF). The significance level was adjusted according to the Bonferroni correction for multiple testing (p < 0.05/3 = <0.0167 was considered to be significant).
Ethics
This study was approved by the Ethics Committee of the Medical Faculty of the Friedrich-Alexander-University Erlangen-Nuremberg (application number: 22-60_2-B).
Results
Patient characterization
The patients were on average 50.7 years old and predominantly female (71.7%). All patients were obese (baseline mean BMI of 39.2; range: 29.8–63.6). The initial average UDFF was 26%. The average skin-liver distance during the initial UDFF determination was 31.6 mm (Table 1).
Patient characteristic. Results are displayed as means. The square brackets additionally include the range and the round brackets comprise the standard deviation or shares (gender).
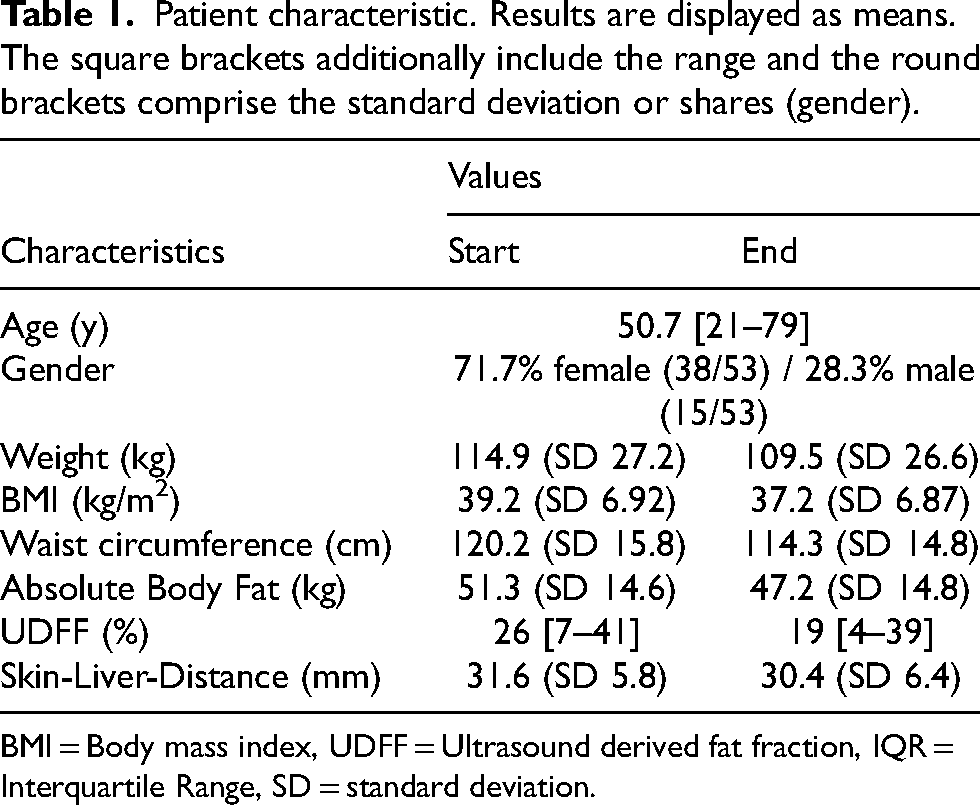
BMI = Body mass index, UDFF = Ultrasound derived fat fraction, IQR = Interquartile Range, SD = standard deviation.
Development of BMI, body fat and waist circumference
Over the course of three months, 47.1% of patients were able to lose at least 5 kg of total body weight and 62.3% were able to reduce BMI by at least one point. During the observation period, 22.6% of the patients decreased their waist circumference by at least 10 cm and 54.7% were able to lose at least 2 kg of body fat (Figure 3).
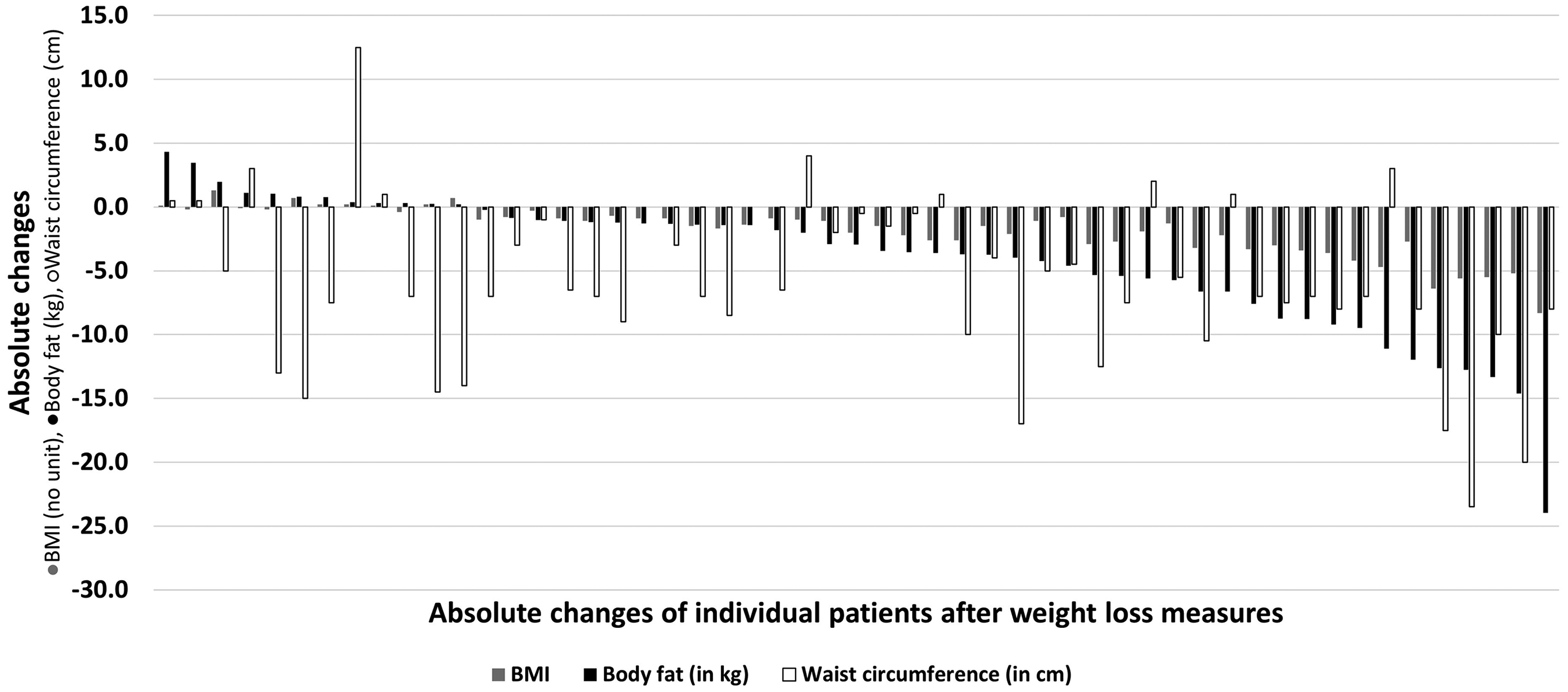
Absolute changes to the BMI (grey columns), body fat in kg (black columns) and waist circumference in cm (white columns) of individual patients after weight loss measures. A value of 0 indicates that the values for this patient were the same before and after the intervention. Patients are ordered according to the change in their body fat, from the greatest increase to the greatest decrease.
Impact of change in BMI, body fat and waist circumference on steatosis hepatis
A reduction in BMI of at least one point was associated with a clear trend towards an improve of UDFF. However, the difference concerning the amount of patients with a relative UDFF reduction of at least 30% was not statistically significant (BMI reduction ≥ 1: 54.5% vs BMI reduction < 1: 20%; p = 0.02) (Figure 4(a)). Patients who lost at least 2 kg of body fat were significantly more likely to achieve a relative reduction in UDFF of 30% or more, compared to those with less body fat reduction (58.6% vs. 20.8%; p = 0.011) (Figure 4(b)). However, a reduction in waist circumference of at least 10 cm compared to patients with less or no reduction did not correlate with a reduction in UDFF (50.0% vs. 39.0%; p = 0.52) (Figure 4(c)).
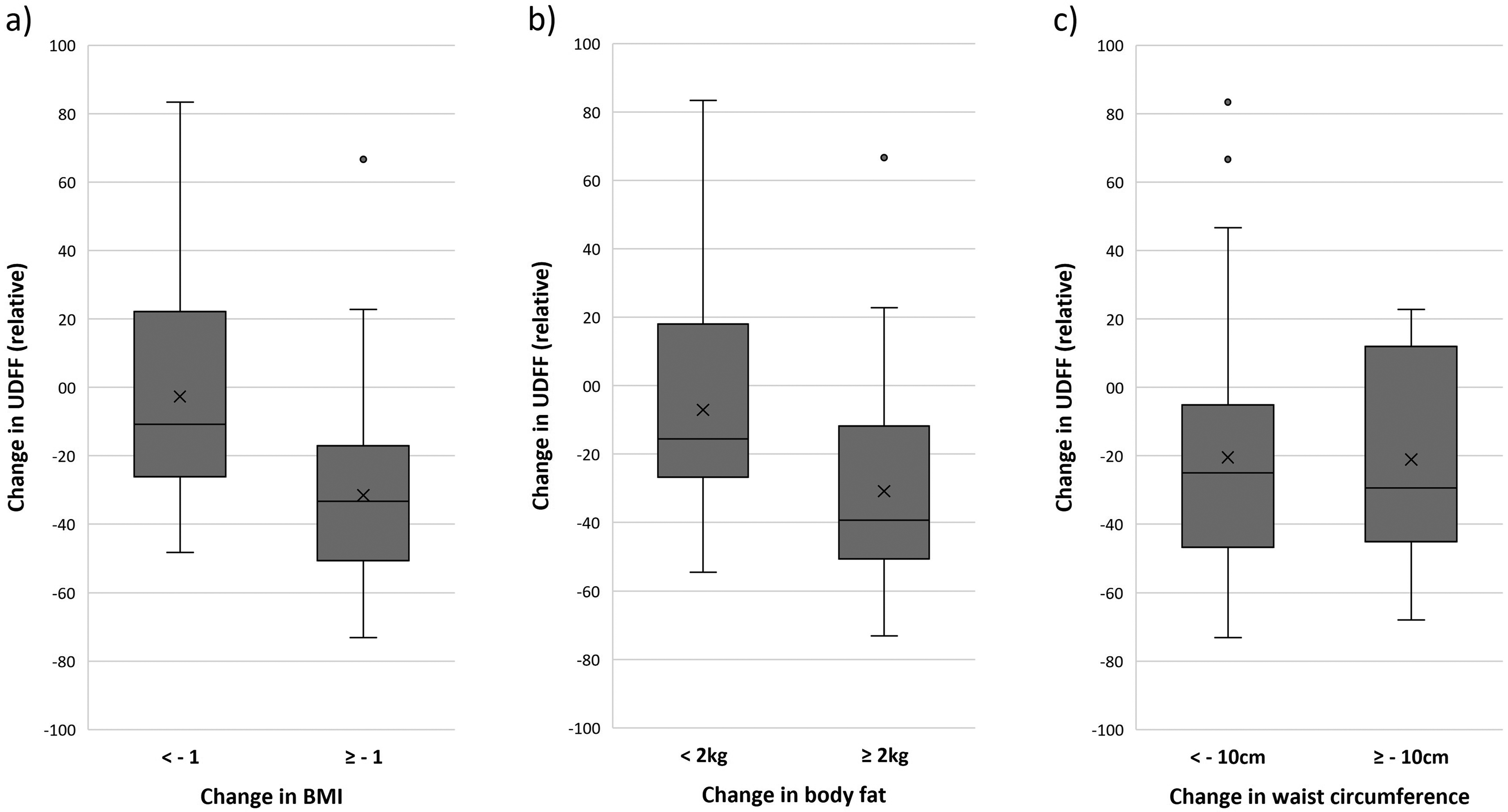
Change in relative UDFF during intervention in dependence on the change of BMI (a; p = 0.02), body fat (b; p = 0.011 [significant]) and waist circumference (c; p = 0.52).
Discussion
Steatosis hepatis is a relevant risk factor for the development of liver cirrhosis. Risk groups (e.g., obese patients) for steatosis hepatis should be screened in this regard.
The gold standard for the assessment of steatosis hepatis is liver biopsy, which should not be used routinely due to its complexity and invasiveness. With regard to non-invasive procedures, the most accurate data exist for MRI-PDFF. 13 With regard to the detection of steatosis hepatis (S0 vs S1-3) in comparison to histology, an excellent AUROC of 0.98 was found. 38
However, MRI-PDFF is also complex, expensive and availability for a broad clinical use is limited. In clinical practice, the comparison of the echogenicity of the liver and renal parenchyma by B-mode ultrasound is therefore used most often. This method is highly available and fast. Although, the sensitivity of this method is low, particularly in regard to mild steatosis hepatis. An increase in the echogenicity of the liver parenchyma is only seen in advanced stages of steatosis. 16 Furthermore, the inter-observer variability is high.4,14 One more advanced method that has been used for more than a decade is the computerised measurement of the hepatorenal index (HRI), which uses computer software to compare the brightness of the liver and kidney parenchyma in the B-mode image.8,9 Studies using HRI have produced mixed results on the exact cut-off for detecting liver steatosis.39,40
Hepatic steatosis also leads to changes in liver perfusion. Therefore, attempts have been made to detect hepatic steatosis by vascular changes. Doppler sonography is the most commonly used imaging technique to visualise haemodynamic flow changes. However, setting the correct Doppler parameters depends on the experience of the investigator. Difficult acoustic conditions in obesity present a challenge to the use of Doppler parameters for therapeutic monitoring. However, the new multimodal capabilities of new high-end ultrasound systems (e.g., HiFR CEUS or SR CEUS) may allow a definitive diagnosis of morphological, vascular and tumour changes in the liver. 41
Several parametric sonographic methods have been developed in recent years with the aim of detecting and grading steatosis hepatis quickly and reliably. Moderate to good results have been achieved with CAP and ATI. 20 In a recent study, CAP achieved an AUC (area under the curve) of 0.69 compared to MRI-PDFF in the differentiation of S0 vs S1-S3 and 0.95 compared to histology. ATI showed in the same study an AUC of 0.86 compared to MRI-PDFF and 0.92 compared to histology. 42 Another study using histology as a reference was able to show that ATI and CAP can detect steatosis hepatis with at least 33% liver fat similarly reliable as MRI-PDFF. 43 The sensitivity to detect at least 5% liver fat appears to be better for MRI-PDFF and ATI than for CAP. In addition, new ultrasound technologies to assess hepatic steatosis, such as liver viscosity, are showing promising results. 44 The accuracy of ATI and CAP is particularly limited in obese patients due to attenuation by pronounced subcutaneous fat. Furthermore, the UGAP (Ultrasound-Guided Attenuation Parameter) method was developed, which also estimates steatosis hepatis via the attenuation of ultrasound waves. However, it uses a reference phantom for calibration and is therefore less susceptible to a deterioration in diagnostic accuracy in obese patients. 23 However, this method also reaches its limits with a BMI of > 40 kg/m2. 45 In a non-extremely obese population (average BMI 26.3 kg/m2), it achieved a sensitivity of 86.7% and a specificity of 82% for the detection of steatosis hepatis. 23
Another promising method appears to be UDFF from Siemens.29,46–48 The combined measurement of attenuation and the backscatter coefficient as well as the deeper penetration depth due to the lower frequencies used 28 could improve the measurement in obese patients. Several studies have demonstrated a high diagnostic accuracy for UDFF. In comparison with MRI-PDFF, a high AUC (0.9) was observed for the detection of low-grade steatosis hepatis (6%). 46 The intra-observer (ICC [intraclass correlation coefficient] = 0.96) and inter-observer (ICC = 0.94) variabilities are excellent. 47 Another study using MRI-PDFF as a reference investigating differentiation between S0 and S1-S3 showed a better AUC (0.99) for UDFF than for CAP (0.92) and the comparison of echogenicity of liver parenchyma to kidney parenchyma (0.87). 29 Most recently, the first systematic review and meta-analysis, including nine studies of UDFF in comparison to MRI-PDFF demonstrated that UDFF exhibits high sensitivity and specificity in detecting hepatic steatosis, with a pooled sensitivity of 90.4% (95%CI:84.0–94.4%) and pooled specificity of 83.8% (95% CI: 75.1–89.8%) and a AUROC of 0.93 (95%CI: 0.83–0.95). 49
Based on the promising data on UDDF, we used this technology to monitor steatosis hepatis in an ongoing interventional trial.
Two patients were excluded because of liver cirrhosis, and its unclear effect on UDFF measurement. Two patients were excluded due to a low UDFF value and therefore a probable absence of steatosis hepatis. This cut-off has not yet been uniformly determined. We used the value from the study by Labyed et al. (6.3%), 37 as this only included patients with a high probability of steatosis. A total of 4 out of 57 patients were excluded in our study, meaning that 93% of all initially screened patients were finally analysed.
We observed in patients with a reduction in BMI of at least one point, a trend towards more frequent relevant reduction of UDFF (−30%), but this was not statistically significant. However, a loss of 2 kg of body fat was significantly more likely to result in a UDFF reduction of at least 30%, compared to patients with less body fat loss. Absolute body fat was used as the criterion for a relevant decrease, as it is independent of changes in body water volume, in contrast to BMI and relative body fat. With regard to the change in waist circumference, we did not observe any differences with respect to the UDFF. We attribute this to known unavoidable measurement inaccuracies for this method. 50
Others have already been able to show that weight reduction improves CAP values. 31 For MRI-PDFF, it has been shown that a reduction of at least 30% is more likely to result in histologic response (51 vs 14%) and NASH resolution (41 vs 7%). 51 For parametric ultrasound we did not find such data. Therefore, we used this 30% cut-off for a relative reduction in UDFF in our study.
A special feature of this study is that we were able to examine only obese patients before and after a weight-modifying intervention. However, there are also limitations. One relevant limitation of our study is the lack of correlation with histology or MRI-PDFF. Although, it is important to note that previous studies have demonstrated a strong correlation between UDFF and histology or MRI-PDFF.29,46,47 Since we are convinced that the high diagnostic quality of UDFF has already been sufficiently proven, we have focused on the changes in UDFF over the course of the study and have dispensed with additional histology or MRI-PDFF. However, confounding by metabolic processes in the liver during weight loss cannot be completely ruled out as a factor affecting the measurement of UDFF in follow-up tests, although this seems unlikely. Our study primarily focused on the potential of UDFF to sensitively detect short-term changes in steatosis hepatis. Another limitation is the relatively small sample size. Nevertheless, even within this limited group, we were able to demonstrate a clear effect of body fat reduction on UDFF. Based on these promising results, we feel encouraged to use UDFF in an ongoing interventional trial. In addition to detecting structural changes, new sonographic methods have been developed to estimate liver function. For example, the “rise time” parameter extracted from CEUS could contribute to a rough assessment of liver function.52,53
In summary, we observed that a greater reduction in body fat leads to a greater decrease in UDFF and thus possibly to an improvement in steatosis hepatis. Therefore, UDFF could represent a promising non-invasive and fast method for monitoring the course of steatosis hepatis. However, further studies are needed to verify this effect, possibly by additional correlation with MRI.
Footnotes
Ethical Considerations
This study was approved by the Ethics Committee of the Medical Faculty of the Friedrich-Alexander-University Erlangen-Nuremberg (application numbers: 22-60_2-B).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data underlying this study are available from the authors upon reasonable request.
