Abstract
Introduction:
The simplified Pulmonary Embolism Severity Index (sPESI) is a validated tool for risk stratification in acute pulmonary embolism (PE). It incorporates heart rate (HR) ⩾ 110 beats per minute (bpm) as a prognostic factor; however, recent evidence suggests that lower HR thresholds may also be clinically relevant. This study evaluated the prognostic performance of sPESI-based models using varying HR cut-offs and assessed the incremental value of adding right ventricular dysfunction (RVD).
Methods:
We conducted a retrospective cohort study of 696 outpatients with objectively confirmed PE between 2014 and 2019 in a Canadian health region. sPESI models were recalculated using HR thresholds of ⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm. The addition of imaging-confirmed RVD was also examined. Outcomes included 30- and 90-day all-cause mortality. Model performance was assessed using logistic regression, area under the curve (AUC), Youden’s Index and net reclassification index (NRI).
Results:
Lowering the HR threshold improved event detection and reclassification. HR ⩾ 100 bpm provided the most balanced performance for 30-day mortality (AUC 74.7%, Youden Index 0.414), and HR ⩾ 90 bpm offered greater sensitivity. Adding RVD modestly improved model discrimination, with sPESI + RVD at HR ⩾ 80 bpm achieving the highest sensitivity (92.9%) and negative predictive value (> 99%) for 30-day mortality. The strongest association with mortality was observed for sPESI alone HR ⩾ 100 bpm (OR 2.06; 95% CI: 1.47–2.92). Findings remained consistent in a hospitalized-only sensitivity analysis.
Conclusion:
Modifying HR thresholds within the sPESI model, particularly at ⩾ 100 bpm, and incorporating RVD meaningfully improves short-term mortality prediction in acute PE. These refinements may enhance clinical decision-making, especially in selecting patients for safe outpatient management.
Keywords
Introduction
Pulmonary embolism (PE) is the third leading cause of cardiovascular death worldwide.1,2 PE is linked to significant morbidity and mortality even with advancements in diagnostic techniques and treatment. A key determinant of early prognosis is right ventricular dysfunction (RVD). Clinical indicators of RVD (e.g., sustained hypotension, right ventricular dilation on imaging, and elevated cardiac biomarkers) have been consistently associated with increased early mortality.3,4
Obstruction of the pulmonary arteries leads to elevated pulmonary vascular resistance and right ventricular wall stress, which in turn prompts a compensatory rise in heart rate (HR) to maintain cardiac output.5,6 HR, a simple and rapidly accessible clinical parameter, is a key prognostic indicator in normotensive patients with acute PE. 7 It is incorporated into most validated risk assessment tools, including the Pulmonary Embolism Severity Index (PESI) and its simplified version (sPESI) and aids the identification of patients at low risk for adverse events who might be safely treated with outpatient management.8–12 This is particularly relevant given the expanding use of direct oral anticoagulants (DOACs), which facilitate home treatment without the need for parenteral agents.13,14
sPESI is a widely used guideline-recommended score that predicts the risk of 30-day mortality in patients with acute PE.15–17 It allocates one point for each of six clinical features: age > 80 years, cancer history, chronic cardiopulmonary disease, systolic blood pressure (SBP) < 100 mmHg, oxygen saturation < 90%, and HR ⩾ 110 beats per minute (bpm). 8 This HR cut-off was derived from the original PESI model, where HR ⩾ 110 bpm was identified as an independent predictor of 30-day mortality. 18 Alternative risk scores, such as the Functional Assessment Staging Tool (FAST) score, have suggested that lower HR cut-offs (e.g., 100 bpm) may also have prognostic significance.7,11,19–21
Despite the established role of HR in the risk stratification of acute PE, the optimal threshold for prognostic assessment remains unclear. Clinical practice guidelines recognize elevated HR as a risk marker but do not define a specific cut-off value.15,16 Recent evidence suggests that even minimal HR elevation may be associated with increased mortality and adverse clinical outcomes in acute PE.5,6,19,20,22 The potential prognostic value of alternative HR cut-offs has also been highlighted in larger registry studies and real-world populations, where it appears that HRs of 80–100 bpm can still carry significant risk.5,6,19,20,22 Consequently, adjusting the HR cut-off within the sPESI could optimize its predictive value, especially in normotensive patients where clinical management decisions regarding early discharge or outpatient treatment rest on accurate risk stratification.
Given the growing emphasis on early discharge and outpatient care for selected patients with acute PE, there is a need to optimize risk stratification tools that support safe and efficient clinical decision-making in this context.15–17 The sPESI is endorsed by contemporary guidelines—including those from the 2020 European Society of Cardiology (ESC) guidelines and the 2016 American College of Chest Physicians (CHEST) Antithrombotic Therapy for Venous Thromboembolic (VTE) disease guidelines—as a practical tool for identifying patients at low risk of early mortality who may be considered for outpatient management.15–17 Its ease of use, real-world applicability, and alignment with ambulatory workflows have led to widespread clinical adoption.7,11,13,20 The original PESI, although more granular, is less feasible for rapid bedside decision-making in acute care. As such, we sought to evaluate whether modifying the HR threshold (⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm) within the sPESI framework—and incorporating imaging-confirmed RVD—could improve prognostic performance and enhance early risk stratification for outpatient PE management.
Methods
Study design and setting
We conducted a retrospective cohort study of outpatients with acute PE in a Canadian health region serving ~250,000 adults. Approval was obtained from the Newfoundland and Labrador Health Research Ethics Board and the institutional Research Proposals Approval Committee.
Study population and data sources
The cohort included adults (⩾ 18 years) with objectively confirmed acute PE between June 1, 2014 and May 31, 2019. Charts with positive PE imaging were reviewed. Data were collected from electronic health records up to 90 days postdiagnosis. Exclusions were missing PE or HR data, an untraceable health number, or death at diagnosis.
Data collection
Data were collected via chart review from the Newfoundland and Labrador Health Services (NLHS) Eastern Zones’ electronic records up to 90 days after the diagnosis of acute PE by trained research assistants, and included medication data, patient-specific characteristics, and healthcare utilization. Patient characteristics included demographic data, the diagnostic testing modality used, and components of sPESI on initial presentation. We collected data on vital signs, laboratory tests, diagnostic imaging, comorbidities, treatment, and mortality within 90 days of acute PE diagnosis. Mortality status was determined through review of electronic medical records across healthcare facilities in the Eastern Zones of the NLHS. This process ensured comprehensive capture of in-hospital deaths and minimized the likelihood of missing mortality data. In-hospital mortality was captured with accuracy, but cause-of-death data were inconsistently recorded. As such, PE-specific mortality could not be reliably ascertained across the cohort. To avoid misclassification bias, analyses were limited to all-cause mortality, a clinically relevant and commonly used endpoint in prognostic studies of acute PE.
Variables and definitions
The primary outcome was all-cause mortality at 30 and 90 days. Exposures included HR, sPESI, and RVD. HR was recorded following hospital presentation and prior to the initiation of treatment for VTE. In cases where multiple HR values were documented, the first recorded HR at the time of presentation—before anticoagulation was administered—was used for analysis. sPESI variables included: age > 80 years, cancer, chronic cardiopulmonary disease (heart failure [HF] or chronic lung disease), HR ⩾ 110 bpm, SBP < 100 mmHg, and oxygen saturation < 90% at the time of diagnosis.8,18,23 HF was defined as prior hospitalization for HF, symptoms of HF (New York Heart Association functional class ⩾ 2) or left ventricular ejection fraction < 40%. Chronic lung disease included asthma, chronic obstructive pulmonary disease, or restrictive lung disease. RVD was based on computed tomography (CT) reports in accordance with the Canadian Association of Radiologists’ national practice guidelines on investigations for acute PE (right ventricular to left ventricular diameter ratio ⩾ 1.0). 24 Covariates included demographics, comorbidities, and diagnostic modality.
Statistical analysis
Patients were stratified by HR < 80 bpm versus ⩾ 80 bpm to compare baseline characteristics. Continuous variables were summarized using mean (SD) or median (IQR), and categorical variables using frequencies and percentages. Differences in continuous variables were assessed using one-way ANOVA for normally distributed data and the Kruskal–Wallis test for nonnormally distributed data. Categorical variables were compared using chi-squared or Fisher’s exact tests, as appropriate.
The prognostic performance of multiple sPESI-based models for predicting 30- and 90-day all-cause mortality was evaluated. Predictor variables included dichotomous and continuous sPESI representations, with modified HR thresholds (⩾ 80, ⩾ 90, and ⩾ 100 bpm), the original threshold (⩾ 110 bpm), and extended models incorporating RVD. Predictors were analyzed as categorical and continuous measures where applicable. Model performance was assessed using sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), false positive rate (FPR), and false negative rate (FNR), each with 95% CIs via the Wilson method. Discrimination was measured by area under the curve (AUC) with 95% CIs using DeLong’s method, 25 and receiver operating characteristic (ROC) curves were generated for visual comparison.
Clinical utility was examined using the net reclassification index (NRI) with the original sPESI as reference, calculated separately for events (deaths) and nonevents (survivors). Prognostic relevance of sPESI models at varying HR thresholds was further tested with univariate logistic regression, with results expressed as odds ratios (OR) and 95% CI.
To evaluate the discriminative performance of risk stratification models at varying HR thresholds, we calculated the Youden Index (J), defined as J = Sensitivity + Specificity – 1. This metric provides a single statistic that captures the optimal trade-off between sensitivity and specificity, aiding in the identification of the threshold that maximizes overall diagnostic accuracy. A higher Youden Index indicates better model performance, with values ranging from 0 (no discriminatory ability) to 1 (perfect accuracy). The index was computed for each sPESI-based model with and without RVD, across different HR cut-offs (⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm), and for both 30-day and 90-day mortality outcomes.
Missing HR data were excluded from analysis to preserve the exposure–outcome relationship.26,27 Missing sPESI data were imputed via chained equations, 28 generating 20 datasets, with pooled results via Rubin’s rules. 29
We performed a sensitivity analysis excluding patients with baseline SBP < 90 mmHg—a marker of patients with high-risk PE due to its association with hemodynamic instability, vasopressor use, and increased in-hospital mortality. 15 An additional sensitivity analysis was performed including only patients who were hospitalized during the index PE encounter. Analyses were conducted in R, version 4.2.2 (R Foundation for Statistical Computing), with statistical significance set at p < 0.05 (two-sided).
Results
A total of 696 adult outpatients with objectively confirmed PE were included in the analysis; 89 patients were excluded due to missing HR data. The mean age was 65.1 ± 16.3 years, 42% were men, the mean weight was 91.4 ± 30.2 kg, and the mean HR was 97.8 ± 21.7 bpm. Of these, 136 (19.5%) had a HR < 80 bpm and 560 (80.5%) had a HR ⩾ 80 bpm. Patients with a HR < 80 bpm were older (69.6 vs 64.0 years, p < 0.001), had higher oxygen saturation (96.1% vs 95.0%, p = 0.005), and had less hypoxemia. The group with a HR < 80 bpm had lower RVD prevalence (9.6% vs 13.4%), lower sPESI (0.9 vs 1.2, p = 0.0001), and a greater proportion of sPESI = 0 (44.9% vs 27.5%, p = 0.0003). DOAC use was higher in the HR < 80 bpm group (51.5% vs 33.4%), whereas patients with a HR ⩾ 80 bpm more often received parenteral anticoagulation or vitamin K antagonists; thrombolysis was exclusive to the HR ⩾ 80 bpm group (3.4% vs 0%, p = 0.022). Hospitalization was less common (57.4% vs 76.4%, p = 0.00012) and the length of stay shorter (median 1 vs 3 days, p < 0.0001) in the HR < 80 bpm group. Rates of subsequent hospitalization, emergency room visits, bleeding, recurrent VTE, and short-term mortality were similar. Thirty-day mortality was 4.0%, and 90-day mortality was 7.9% (Table 1).
Baseline characteristics and initial presentation of patients with acute PE stratified by heart rate.
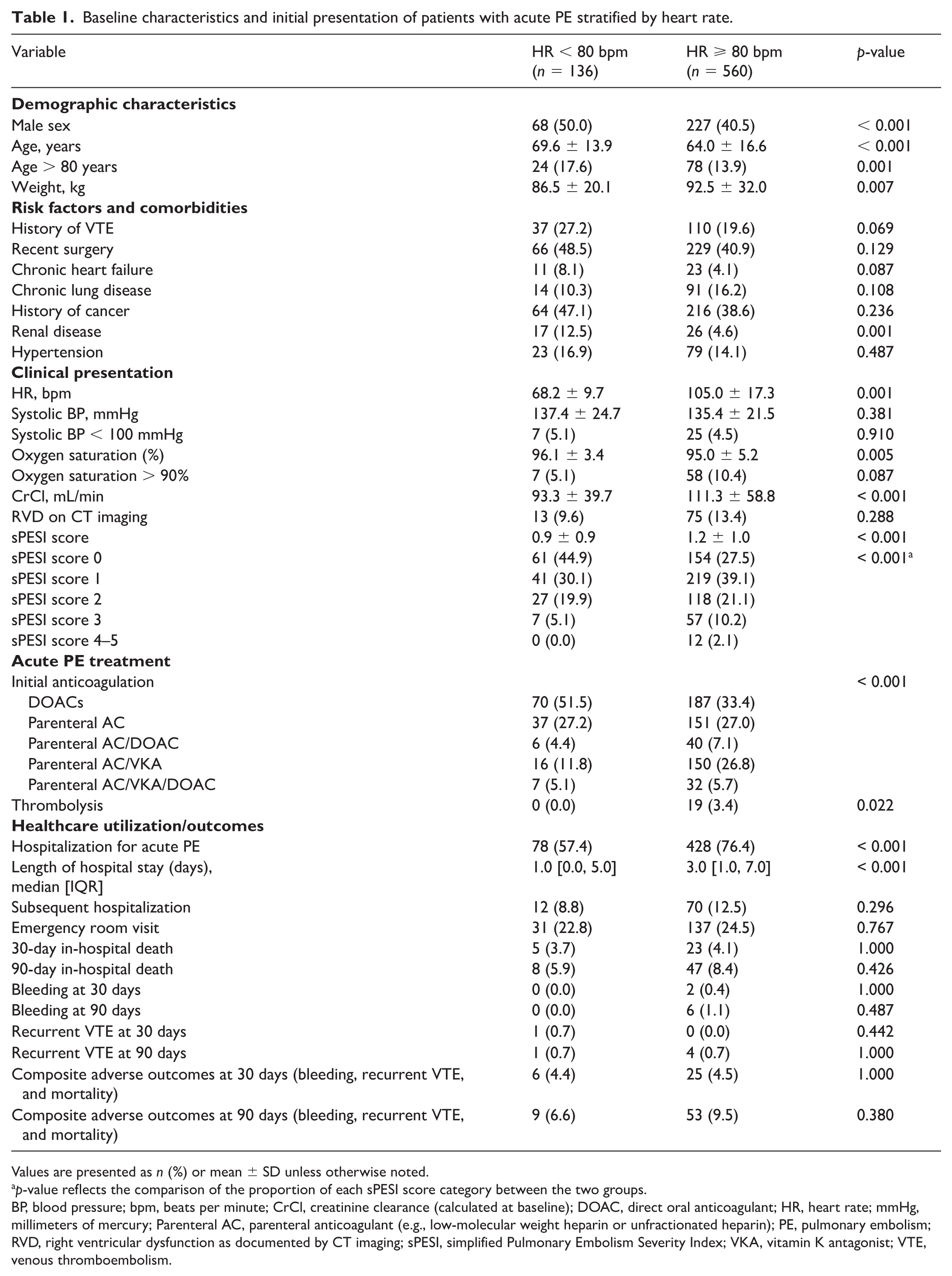
Values are presented as n (%) or mean ± SD unless otherwise noted.
p-value reflects the comparison of the proportion of each sPESI score category between the two groups.
BP, blood pressure; bpm, beats per minute; CrCl, creatinine clearance (calculated at baseline); DOAC, direct oral anticoagulant; HR, heart rate; mmHg, millimeters of mercury; Parenteral AC, parenteral anticoagulant (e.g., low-molecular weight heparin or unfractionated heparin); PE, pulmonary embolism; RVD, right ventricular dysfunction as documented by CT imaging; sPESI, simplified Pulmonary Embolism Severity Index; VKA, vitamin K antagonist; VTE, venous thromboembolism.
Supplemental Table S1 shows trends across the full HR spectrum: higher HR, particularly ⩾ 110 bpm, was associated with younger age, lower oxygen saturation, greater RVD prevalence, higher sPESI scores, increased use of parenteral anticoagulation and thrombolysis, and higher hospital admission and bleeding rates. Mortality and recurrent VTE varied less, and no deaths occurred at 30 or 90 days in patients with sPESI = 0.
Model performance of simplified Pulmonary Embolism Severity Index (sPESI) variants
In the overall cohort, the prognostic performance of sPESI models varied significantly by HR threshold. The modified sPESI model using a threshold of HR ⩾ 100 bpm demonstrated the most favorable balance between sensitivity and specificity, achieving the highest Youden’s Index score for both 30-day (0.414) and 90-day (0.467) mortality, alongside robust AUC values (74.7% and 78.5%, respectively). This threshold outperformed the conventional HR ⩾ 110 bpm cut-off, which yielded slightly lower Youden’s Index values and AUCs. Although an HR threshold of ⩾ 90 bpm achieved excellent sensitivity (92.9%) for 30-day mortality, this came at the cost of markedly reduced specificity (42.4%), limiting its discriminatory value.
The NPVs remained consistently high across all HR-based models (95.7–99.3%), whereas PPVs were low (6.3–18.3%) due to the low event rate (Table 2).
Prognostic performance of sPESI models with varying heart rate thresholds for predicting 30- and 90-day mortality in acute pulmonary embolism.
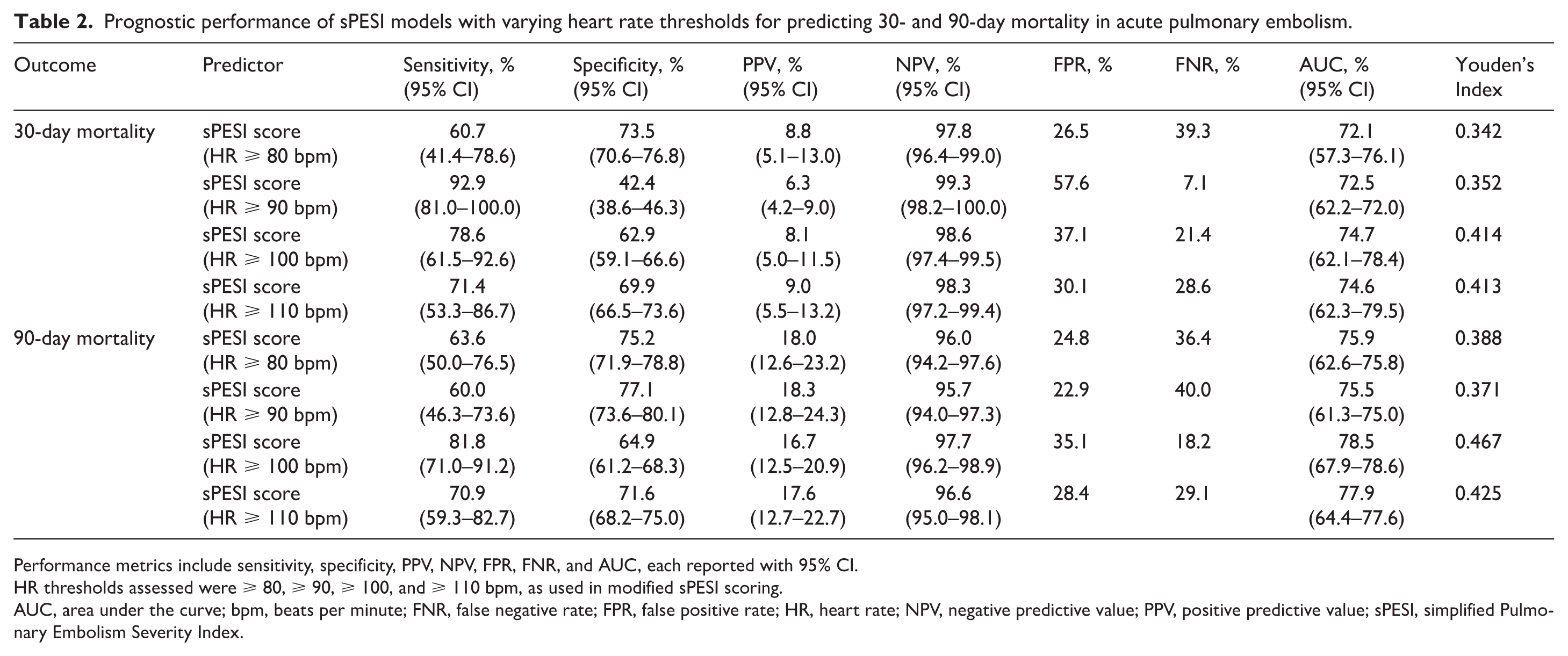
Performance metrics include sensitivity, specificity, PPV, NPV, FPR, FNR, and AUC, each reported with 95% CI.
HR thresholds assessed were ⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm, as used in modified sPESI scoring.
AUC, area under the curve; bpm, beats per minute; FNR, false negative rate; FPR, false positive rate; HR, heart rate; NPV, negative predictive value; PPV, positive predictive value; sPESI, simplified Pulmonary Embolism Severity Index.
Using the original sPESI score at HR ⩾ 110 bpm as the baseline, the HR ⩾ 80 bpm and HR ⩾ 90 bpm models improved risk classification for 30-day mortality. The highest NRI was observed for sPESI at HR ⩾ 80 bpm (NRI = 0.23), primarily driven by improved event classification (NRI events = 0.39), despite reduced specificity (NRI nonevents = −0.16). Similar findings were noted for 90-day mortality (NRI = 0.13). The sPESI score at HR ⩾ 90 bpm also yielded meaningful reclassification (NRI = 0.18 for 30-day mortality). Models with higher HR thresholds (HR ⩾ 100 bpm and ⩾ 110 bpm) showed minimal or no reclassification benefit (Table S2).
The addition of RVD to the sPESI model (sPESI + RVD) marginally improved overall sensitivity across all HR thresholds of ⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm but led to a modest trade-off in specificity. Notably, the sPESI + RVD model with HR ⩾ 90 bpm yielded the highest Youden’s Index (0.436) among all models for 30-day mortality, suggesting a potential benefit in combining physiologic and imaging parameters to enhance early mortality risk stratification in patients with acute PE (Table 3). NRI analysis demonstrated that lowering the HR threshold in sPESI-based models improved classification accuracy for both 30-day and 90-day mortality. Compared to the baseline sPESI and sPESI + RVD models using the conventional HR threshold of ⩾ 110 bpm, modified models with lower HR cut-offs demonstrated improved classification of short-term mortality events. The greatest reclassification benefit was observed with the HR ⩾ 80 bpm model, particularly for 30-day mortality (NRI = 0.23 for sPESI, NRI = 0.19 for sPESI + RVD), primarily driven by more accurate identification of deaths (NRI events = 0.39 and 0.29, respectively) (Tables S2 and S3). For 90-day mortality, reclassification gains persisted with HR ⩾ 80 bpm but were more modest (NRI = 0.13 and 0.11, respectively). Models with HR cut-offs of ⩾ 100 bpm or higher provided minimal or no incremental improvement in event classification. These results support the potential value of lower HR thresholds in risk stratification tools, particularly for guiding decisions about early discharge or outpatient management.
Prognostic performance of sPESI-based models with right ventricular dysfunction using varying heart rate thresholds for 30- and 90-day mortality in acute pulmonary embolism.
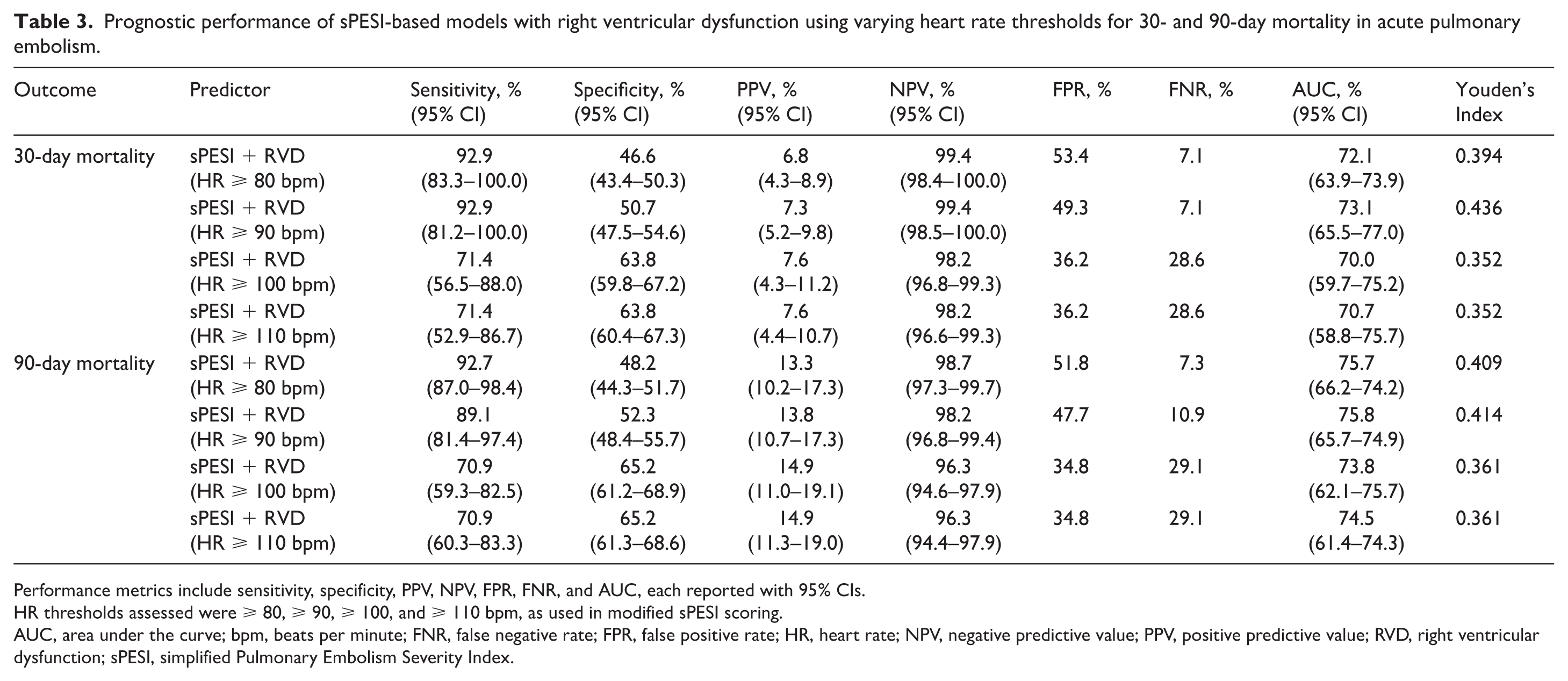
Performance metrics include sensitivity, specificity, PPV, NPV, FPR, FNR, and AUC, each reported with 95% CIs.
HR thresholds assessed were ⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm, as used in modified sPESI scoring.
AUC, area under the curve; bpm, beats per minute; FNR, false negative rate; FPR, false positive rate; HR, heart rate; NPV, negative predictive value; PPV, positive predictive value; RVD, right ventricular dysfunction; sPESI, simplified Pulmonary Embolism Severity Index.
Logistic regression analysis
The logistic regression models revealed associations between sPESI at varying HR thresholds and mortality at 30 and 90 days. Similar associations were seen between sPESI with RVD at varying HR cut-off values and mortality at 30 and 90 days. The logistic regression analyses confirmed that sPESI alone showed the strongest association with 30-day mortality at HR ⩾ 100 bpm (OR 2.06, 95% CI 1.47–2.92) and with 90-day mortality (OR 2.54, 95% CI 1.95–3.38). When RVD was included, the strongest associations shifted to HR ⩾ 90 bpm for 30-day mortality (OR 1.82, 95% CI 1.33–2.50) and to HR ⩾ 80 bpm for 90-day mortality (OR 2.19, 95% CI 1.70–2.84) (Table 4).
Univariate logistic regression of sPESI-based risk models with varying heart rate thresholds for predicting 30-day and 90-day mortality in patients with acute pulmonary embolism.
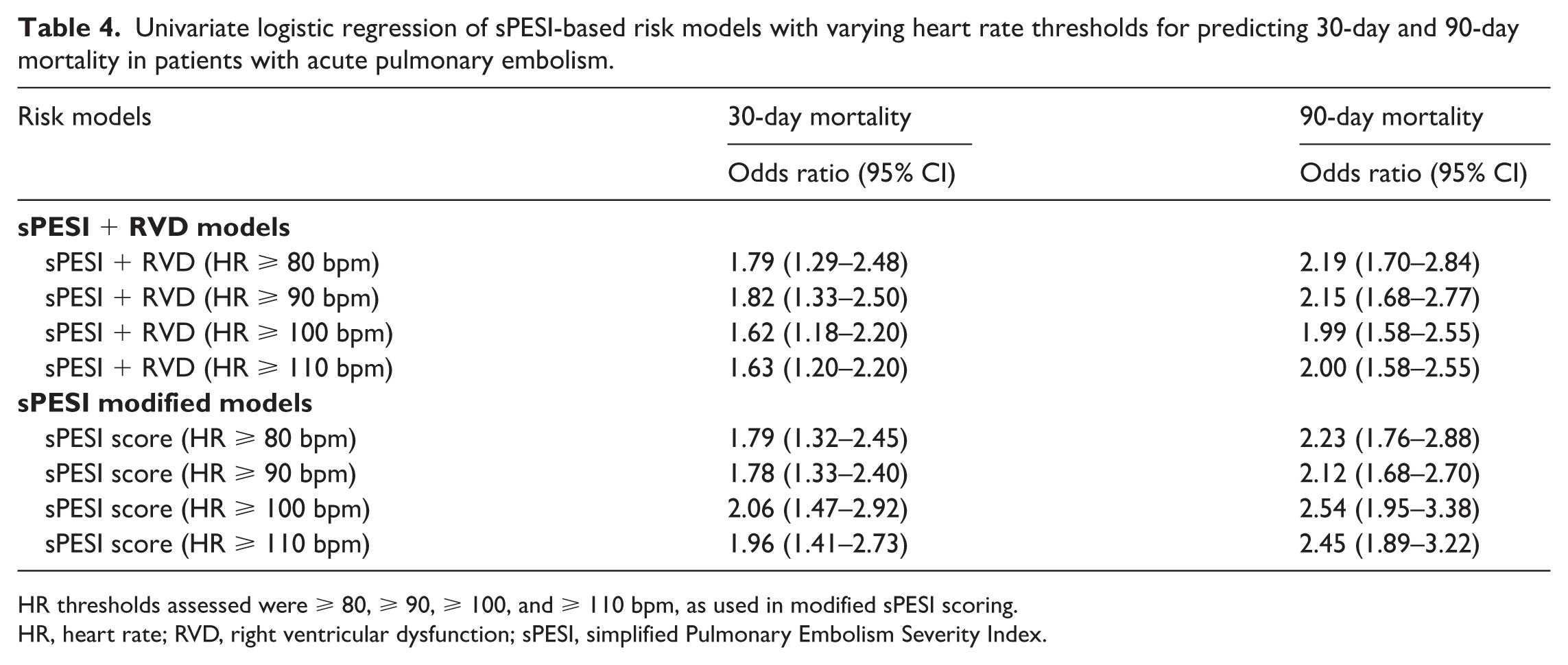
HR thresholds assessed were ⩾ 80, ⩾ 90, ⩾ 100, and ⩾ 110 bpm, as used in modified sPESI scoring.
HR, heart rate; RVD, right ventricular dysfunction; sPESI, simplified Pulmonary Embolism Severity Index.
Sensitivity analyses
After patients with shock were excluded, the sensitivity analysis showed results which were consistent with primary results (Tables S4–S7; Tables S11 and S12). In analyses restricted to hospitalized patients with acute PE (N = 506), findings were consistent with the main cohort, but the overall discriminatory performance was modestly higher. For 90-day mortality, the sPESI model with HR ⩾ 100 bpm demonstrated the highest Youden’s Index (0.533) and strong sensitivity (91.3%), affirming its utility in identifying patients at elevated risk during inpatient care. At 30 days, the HR ⩾ 110 bpm model yielded the highest Youden’s Index (0.484), though the HR ⩾ 100 bpm model performed comparably well (0.424), with slightly lower specificity. Incorporating RVD into the sPESI framework improved sensitivity at all thresholds but lowered specificity, especially at lower HR cut-offs. The sPESI + RVD model with HR ⩾ 90 bpm offered the best trade-off for 90-day mortality in this subgroup (Youden’s Index 0.443), aligning with the trend observed in the full sample (Tables S8 and S9). Logistic regression confirmed that both sPESI and sPESI + RVD models maintained significant associations with short-term mortality, with the HR ⩾ 100 bpm threshold yielding the highest ORs (Tables S10, S13, and S14). These results reinforce the relevance of HR refinement and RVD integration for risk stratification in hospitalized patients, with implications for inpatient monitoring and care.
Discussion
In this retrospective cohort study of outpatients with acute PE, we found that adjusting the HR threshold within the sPESI framework had a meaningful impact on the model’s ability to discriminate between risk levels and improved overall classification performance. Notably, the use of lower HR thresholds, particularly ⩾ 90 bpm and ⩾ 100 bpm, improved the sensitivity and NRI for short-term mortality compared to the conventional cut-off of ⩾ 110 bpm.
This study specifically focused on the sPESI score, rather than the original PESI, for several reasons. First, sPESI is the preferred tool in current clinical guidelines for risk stratification in normotensive patients with acute PE who may be eligible for home treatment or early discharge.14,17 Second, several components required for calculating the full PESI, such as altered mental status and functional impairment, are often incompletely documented in electronic medical records, particularly in real-world ambulatory settings, which can compromise model validity. Third, many prior investigations that have evaluated the role of HR thresholds or additional prognostic markers, such as RVD, have done so using sPESI rather than PESI.5,6,10 As such, the use of sPESI in our analysis allowed for consistency and comparison with the broader evidence base. Finally, the sPESI model’s ease of use and practicality in emergency and outpatient environments make it a relevant tool for real-time decision-making, supporting its continued refinement and clinical applicability.
Our study builds on previous evidence emphasizing the important role of HR in early risk stratification for acute PE.5,6,13,17–19,30,31 In the PESI and sPESI models, HR ⩾ 110 bpm was included as a prognostic variable due to its association with increased early mortality.8,18 However, this threshold has been questioned in recent years, with emerging evidence indicating that even moderately elevated HR (80–110 bpm) may be linked to worse outcomes.16,17 These findings have prompted renewed interest in whether the sPESI might benefit from recalibrating the HR cut-off to improve its predictive accuracy.
Our results affirm that modifying the HR threshold meaningfully alters the sPESI score’s ability to predict patient outcomes. Specifically, models using HR cut-offs of ⩾ 100 bpm provided the most balanced sensitivity and specificity for predicting 30-day mortality, with an AUC of 74.7%. Notably, lower thresholds (HR ⩾ 80 or ⩾ 90 bpm) offered higher sensitivity but at the expense of specificity. This finding is consistent with the RIETE registry and the FAST score validation studies, which reported improved risk classification using HR cut-offs below 110 bpm.3,4,11,19,20 Similarly, recent real-world data by Jaureguízar et al. 5 and Yamashita et al. 6 showed that HR ⩾ 90 bpm was independently associated with higher 30-day mortality in normotensive patients with PE.
The ROC and NRI analyses provided clearer detail on the models’ ability to discriminate and reclassify risk. Although sPESI models with lower HR thresholds improved event classification (i.e., better identification of patients who died), the trade-off was reduced specificity due to more false positives. This trade-off carries practical implications. The consistently high NPV across all models suggests that patients classified as low risk were unlikely to experience early mortality—a critical consideration when evaluating patients for outpatient management. 14 However, the low PPV underscores the limited standalone prognostic utility of HR-based sPESI modifications. This supports the importance of incorporating additional clinical variables, such as imaging-confirmed RVD or biomarkers, into more comprehensive risk stratification strategies.3,4,9,15,16
Incorporating RVD into the sPESI framework resulted in a modest yet consistent improvement in prognostic performance across both 30- and 90-day mortality outcomes. The sPESI + RVD model using a HR threshold of ⩾ 80 bpm achieved the highest sensitivity (92.9% and 92.7%, respectively) and NPV (> 98%), reinforcing its potential to safely identify low-risk patients. These findings align with prior studies highlighting the added prognostic value of imaging-confirmed RVD in acute PE risk stratification.3,4,7,10 However, this gain was relatively modest compared to the improvement observed with HR recalibration alone, suggesting that HR threshold optimization accounts for the bulk of prognostic refinement. Consistent with our central observation, approximately 70% of the performance improvement appears attributable to HR adjustment, with the remaining 30% linked to the addition of RVD. Logistic regression analyses further reinforced these findings. When RVD was included, the optimal threshold shifted slightly lower, with HR ⩾ 90 bpm demonstrating the best predictive value. These results support earlier work suggesting that even moderate HR elevation may reflect early hemodynamic compromise in acute PE.16,17
The results were consistent in sensitivity analyses excluding patients with SBP < 90 mmHg—a group at risk for hemodynamic instability—confirming the robustness of our findings. Furthermore, although our primary focus was 30-day mortality, similar performance patterns were observed for 90-day mortality. Models using an HR threshold of ⩾ 100 bpm demonstrated the strongest discriminative ability (Tables S6 and S7). This finding suggests that early physiological imbalances, particularly elevated HR, may carry sustained prognostic significance beyond the acute phase. This aligns with prior research linking persistent right heart strain to adverse outcomes later in the disease course.6,32,33
As a second sensitivity analysis, we repeated all prognostic performance and regression analyses in the subgroup of patients hospitalized for the index PE event. Findings from the hospitalized cohort were consistent with the primary analysis. Lower HR thresholds continued to demonstrate improved discrimination for both 30- and 90-day mortality, with the highest Youden Index values observed at HR ⩾ 100 bpm and ⩾ 110 bpm, reflecting a more favorable balance between sensitivity and specificity in this higher-risk population. Incorporation of RVD again provided incremental gains in sensitivity and negative predictive value, particularly for 90-day mortality, but these improvements remained modest relative to those achieved through HR recalibration alone. The direction and magnitude of ORs in univariate logistic regression were similar to those observed in the overall cohort, supporting the robustness of our findings and suggesting that the prognostic relevance of optimized HR thresholds and RVD integration extends to patients requiring hospitalization at presentation.
The primary clinical implication of our findings relates to early risk stratification for outpatient management. As contemporary guidelines increasingly support early discharge in selected patients with acute PE, there is a need for pragmatic and reliable tools to identify individuals at low risk for short-term mortality.15,16 Given that the sPESI score is primarily used to guide outpatient treatment decisions, optimizing the HR threshold may improve the safety of selecting patients who truly fall within a low-risk profile. Our results suggest that modest elevations in HR—even below the conventional 110 bpm threshold—carry clinically relevant risk, particularly in normotensive ambulatory patients. These findings indicate that refinement of HR thresholds could enhance the ability of clinicians to identify appropriate candidates for outpatient care, rather than guide selection for advanced PE therapies. Because sPESI was originally developed to predict all-cause 30-day mortality rather than to guide advanced PE interventions, our findings should be interpreted in the context of outpatient triage and early discharge decisions rather than escalation to advanced therapies. Prospective validation of these modified models is warranted to support their integration into clinical decision-making pathways.
Strengths and limitations
This study represents one of the largest real-world analyses to systematically evaluate the prognostic impact of varying HR thresholds in sPESI-based models for acute PE. The inclusion of a well-defined outpatient cohort with objectively confirmed PE enhances the applicability of findings to contemporary clinical practice. We employed multiple robust statistical techniques (e.g., ROC analysis, logistic regression, NRI) to comprehensively assess model performance. Additionally, incorporating RVD as an imaging-based marker provided valuable insights into the utility of combining clinical and imaging risk stratification approaches.
However, several limitations warrant consideration. The retrospective design introduces the potential for residual confounding and selection bias. HR was captured at a single time point, which may not fully reflect dynamic physiological changes. RVD assessment was based on standard imaging interpretations and did not include echocardiographic or functional parameters. Moreover, the study was conducted within a single Canadian health region, which may limit the generalizability of findings to other healthcare systems.
Also, beta-blocker use, which may blunt the HR response and impact scoring in heart rate-dependent models such as sPESI, could not be reliably assessed in this study. Medication data were incompletely captured in the health records and therefore excluded to minimize the risk of misclassification bias. This represents a potential confounder that should be addressed in future prospective studies.
Next, our analysis focused on all-cause mortality rather than PE-specific mortality or long-term functional outcomes. Mortality in this study was classified as all-cause rather than PE-specific, as the retrospective design and limitations in available documentation did not permit reliable attribution of death directly to PE. This approach was taken to avoid misclassification bias, recognizing that cause-of-death details were often unclear. Although this limits our ability to isolate the direct impact of PE on mortality, all-cause mortality remains a clinically meaningful endpoint that captures the overall burden of illness in this population. Future prospective studies with adjudicated cause-of-death data are warranted to more accurately assess PE-specific mortality.
Finally, mortality data were obtained from electronic medical records, with deaths primarily captured through review of medical records across healthcare facilities within the Eastern Zone. As a result, deaths that occurred outside hospital settings and not recorded in the provincial electronic medical records may not have been captured. However, given the centralized structure of healthcare delivery in Newfoundland, the likelihood of missed deaths is expected to be minimal.
Conclusion
In this retrospective cohort study of outpatients with acute PE, we found that modifying the HR threshold within the sPESI framework significantly influenced the model’s prognostic performance. Lower thresholds, particularly HR ⩾ 90 and ⩾ 100 bpm, improved sensitivity and risk reclassification for 30- and 90-day mortality, suggesting that even modest elevations in HR carry meaningful prognostic information. Incorporating RVD further enhanced model discrimination, though to a lesser extent than HR recalibration alone. These findings support the refinement of sPESI-based risk stratification by integrating optimized HR cut-offs and imaging markers. Future prospective studies are warranted to validate these results and inform updates to clinical guidelines, particularly for identifying patients suitable for outpatient management.
Supplemental Material
sj-docx-1-vmj-10.1177_1358863X261420329 – Supplemental material for Optimizing sPESI with heart rate threshold adjustments for risk stratification in acute pulmonary embolism: A retrospective cohort study
Supplemental material, sj-docx-1-vmj-10.1177_1358863X261420329 for Optimizing sPESI with heart rate threshold adjustments for risk stratification in acute pulmonary embolism: A retrospective cohort study by Kwadwo O Bonsu, Stephanie W Young, Tiffany A. Lee, Hai V Nguyen and Rufaro S Chitsike in Vascular Medicine
Footnotes
Data availability statement
Access to the de-identified data used in this study is restricted and may be made available upon reasonable request, subject to approval by the Human Research and Ethics Board and Digital Health, Newfoundland and Labrador Health Services. Requests for data access may be directed to:
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Kwadwo Osei Bonsu received a postdoctoral fellow salary from an unrestricted grant provided by Sanofi Canada. Stephanie Young and Rufaro Chitsike have received unrestricted research grants from Sanofi Canada and Bayer Canada for research and clinical activities outside of this work. Rufaro Chitsike received speaking honoraria from Pfizer Canada. Tiffany A. Lee has received investigator-initiated, unrestricted research funding from Shoppers Drug Mart, Inc., unrelated to this work. Hai V Nguyen has no conflicting interests.
Funding
The development, implementation, and evaluation of the former NLHS Eastern Zones Thrombosis Service, including this study, was supported by an unrestricted grant from Sanofi Canada and Bayer Canada.
Supplemental material
Supplemental material for this article is available online.
