Abstract

Keywords
Postthrombotic syndrome (PTS) affects 25–40% of patients within 1 year after deep vein thrombosis (DVT) and results from increased venous pressure due to obstruction or valvular incompetence. The risk of this complication increases with proximal thrombus extension.1–4
The Villalta score is the gold standard for diagnosing PTS but is limited by its subjective clinical assessment and lack of objective diagnostic criteria. Other scores, such as the Venous Clinical Severity Score (VCSS), are primarily used for chronic venous disease (CVD) and are not specific for PTS.5,6 Duplex sonographic reflux time (SRT) in the popliteal vein is an established functional test that may indicate venous abnormality and the Marder score quantifies residual thrombotic material by ultrasound. 7 Light reflection rheography (LRR) is a photoplethysmographic method used to measure venous refill time (VRT) after calf muscle activation and is commonly applied in CVD diagnostics. 8 The German S2k guideline recommends LRR as a supplementary measurement method for PTS; however, evidence supporting its diagnostic validity is lacking. 9 Therefore, this study aimed to evaluate the diagnostic value of LRR in detecting venous insufficiency after DVT and its correlation with the Villalta score, the VCSS, the Marder score, and SRT.
This cross-sectional, single-center study included patients with a first unilateral DVT between April and December 2016. Data were collected 12–18 months after the index event. Inclusion criteria were (i) lower-extremity DVT; (ii) ability to adhere with study procedures and guideline-based anticoagulation and compression therapy; (iii) age ⩾ 18 years; (iv) written informed consent from patient; and (v) sufficient compliance to conduct the study. Exclusion criteria were (i) peripheral arterial disease (PAD) Fontaine stage III or IV; (ii) bilateral DVT; (iii) recurrent DVT; and (iv) advanced varicose veins (visible diameter > 3 cm, sonographic varicose vein diameter > 5 mm). The study was approved by the local institutional ethics committee.
Demographic and thrombosis-specific data were recorded. Thrombosis was classified as distal (popliteal and crural veins) or proximal (including iliac and femoral veins). All assessments were performed on the affected limb. Clinical symptoms were evaluated using the Villalta score 5 and the VCSS. 6 Residual thrombotic material was quantified using the Marder score (0–28 points). 7 SRT was performed in a seated position after manual calf compression, with values > 1000 ms indicating venous reflux. LRR was performed with the patient seated, and a VRT < 25 seconds was defined as pathological.
Continuous variables are presented as median (IQR). Differences between two cohorts were analyzed using the two-sided Mann–Whitney U-test. Associations between measurement methods were assessed by Bravais–Pearson correlation analysis.
A total of 62 patients (median age 64.5 years, 32 women) were included. According to the most proximal thrombus extension, 46.7% had a distal DVT and 53.2% had a proximal DVT. The mean interval between the index event and the study exam was 509 days (SD ± 46), with a median of 441 days (IQR 422–471).
As shown in Table 1, the Villalta score identified PTS in 22 patients (35.4%), with a median score of 3.5 (IQR 2–5.25); 19 of these patients had only mild PTS. The Marder score was 0 in 39 of 61 patients, indicating no residual thrombotic material. One patient was missing SRT and LRR data due to an acute deep vein thrombosis at follow-up. The SRT was pathological in only six of 61 patients (9.8%). LRR was abnormal in 41 participants (67.2%), indicating venous incompetence. The median VRT was 19 seconds (IQR 14–28). No correlation was found between the Villalta score and apparatus tests. The VCSS was significantly higher in patients with abnormal LRR (p = 0.003), correlation was weak (r = 0.362). Abnormal LRR was not associated with more thrombotic material or sonographic reflux.
Comparison of patients with and without postthrombotic syndrome, SRT, and LRR (VRT).
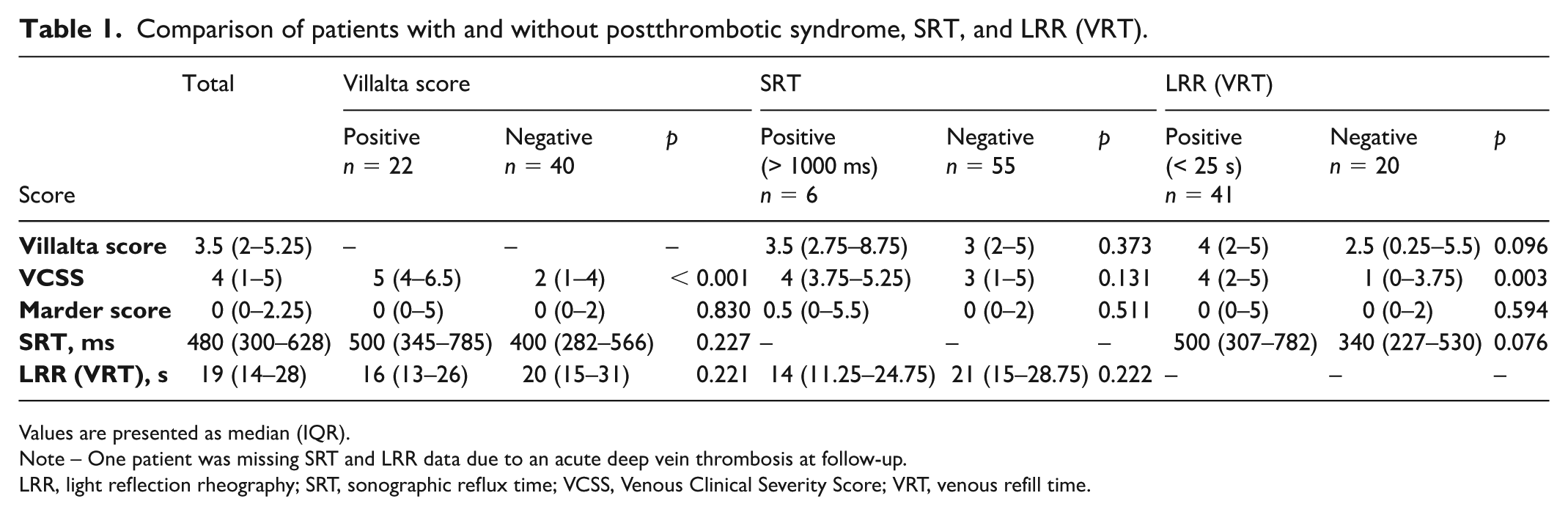
Values are presented as median (IQR).
Note – One patient was missing SRT and LRR data due to an acute deep vein thrombosis at follow-up.
LRR, light reflection rheography; SRT, sonographic reflux time; VCSS, Venous Clinical Severity Score; VRT, venous refill time.
Among patients with PTS, 75% had an abnormal and 25% had a normal LRR. Accordingly, LRR showed a sensitivity of 75% but a specificity of only 37.5% in diagnosing PTS. Patients with proximal DVT had a significantly higher Marder score and more reflux, but no significant differences in clinical scores and LRR results compared to distal DVT. LRR is feasible and noninvasive but shows poor concordance with the Villalta score and other methods. Contrary to our expectations, proximal DVT showed no significant LRR abnormalities, further limiting its diagnostic value. We identified a correlation between the VCSS and LRR, indicating a potential link to clinical severity. Future research is needed to clarify why the VCSS is correlated and the Villalta score was not.
This study demonstrates a gap between clinical and instrumental PTS assessments. Limitations include small sample size and single-center design, particularly with respect to statistical power. Based on our findings, we conclude that the guideline-recommended use of light reflection rheography in PTS diagnostics should be critically re-evaluated, as our data indicate a risk of substantial overdiagnosis of PTS when relying on this parameter.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
