Abstract

Keywords
What is venous thrombosis at unusual sites?
Thrombosis is the formation of blood clots within a blood vessel. Veins are the blood vessels responsible for returning blood from the brain, arms, legs, and organs back to the heart. Deep vein thrombosis (DVT) is the abnormal formation of blood clot(s) inside any deep veins of the body, causing a narrowing or blockage within the affected vein(s).
The veins of the legs or arms are the two most common locations where DVT occurs. 1 Less commonly, DVT may develop in other locations. Blood clots that form within the deep veins of the legs or arms may break off and travel through the bloodstream until they reach the lungs. This event is called a pulmonary embolism (PE).
The term ‘venous thrombosis at unusual sites’ refers to a DVT in any deep veins other than in the legs or arms. These less common locations where DVT may occur include the deep veins (and venous sinuses) of the brain; the retinal veins inside the eyes; the veins of any major organ inside the abdomen including liver, spleen, kidneys, and intestines; the gonadal (ovarian or testicular) veins deep in the pelvis; and the inferior vena cava (IVC). The IVC is the largest vein deep inside the abdomen, carrying the blood coming from the legs, pelvis, and abdomen back to the heart.
What are the features and risk factors for venous thrombosis at unusual sites?
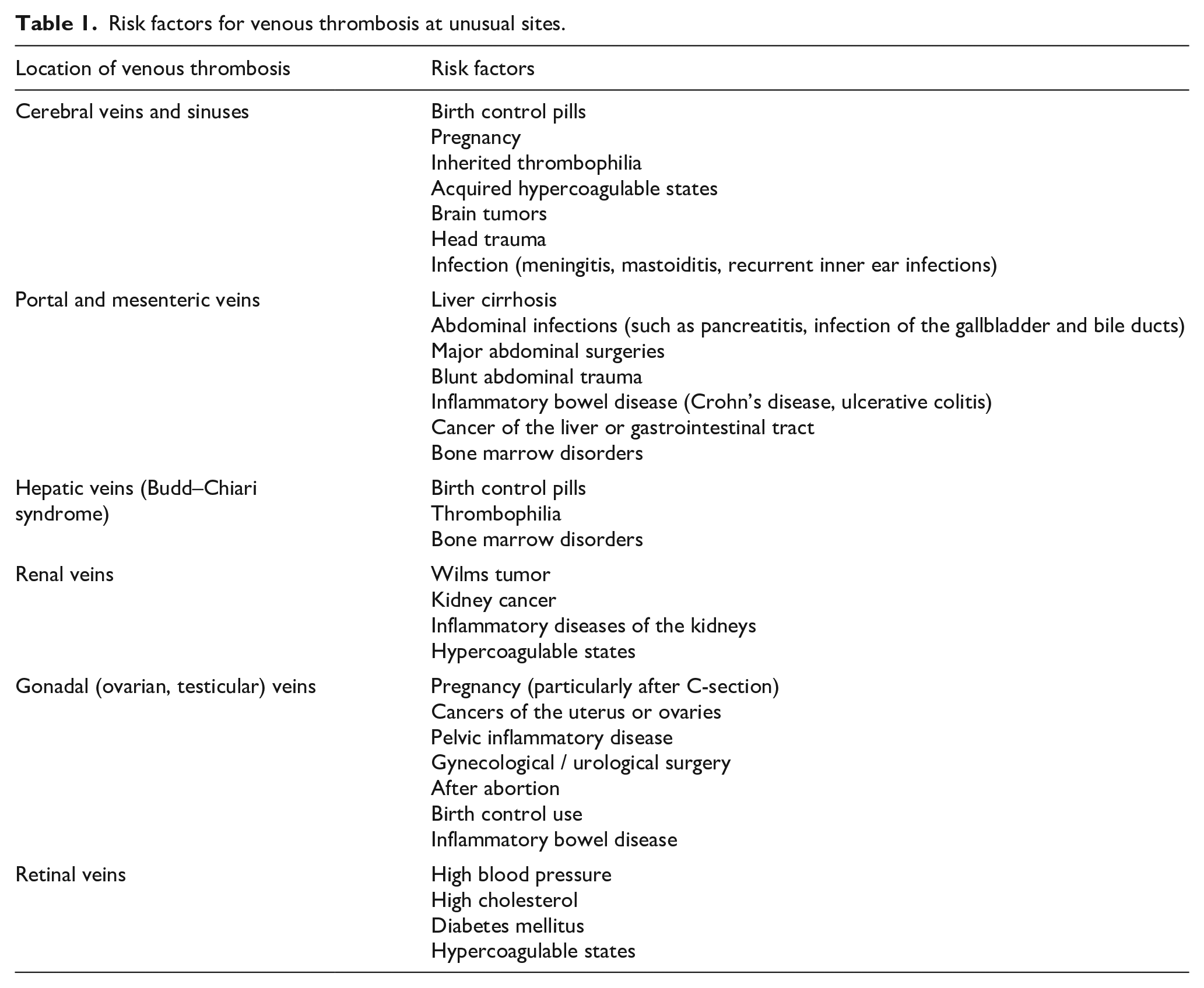
The risk factors associated with venous thrombosis in an unusual site vary depending on the location in the body (Table 1).
Risk factors for venous thrombosis at unusual sites.
When a DVT occurs in a deep vein of the brain, it is called ‘cerebral venous sinus thrombosis’ (CVST) (Figure 1).2–4 In CVST, the arterial blood flow into the brain is normal, but the pressure within the brain may build up because of poor blood drainage out of the brain. CVST occurs in between 1 in 100,000 and 1 in 500,000 individuals each year.2,3 This condition is more common in young adults (younger than 45 years), and especially in young women. The most common risk factors for CVST include birth control pills, pregnancy, and the presence of inherited (genetic) or acquired predispositions to clotting (also called ‘hypercoagulable states’). 5 More recently, very rare cases of CVST have been reported as a complication of certain COVID-19 vaccines. 6
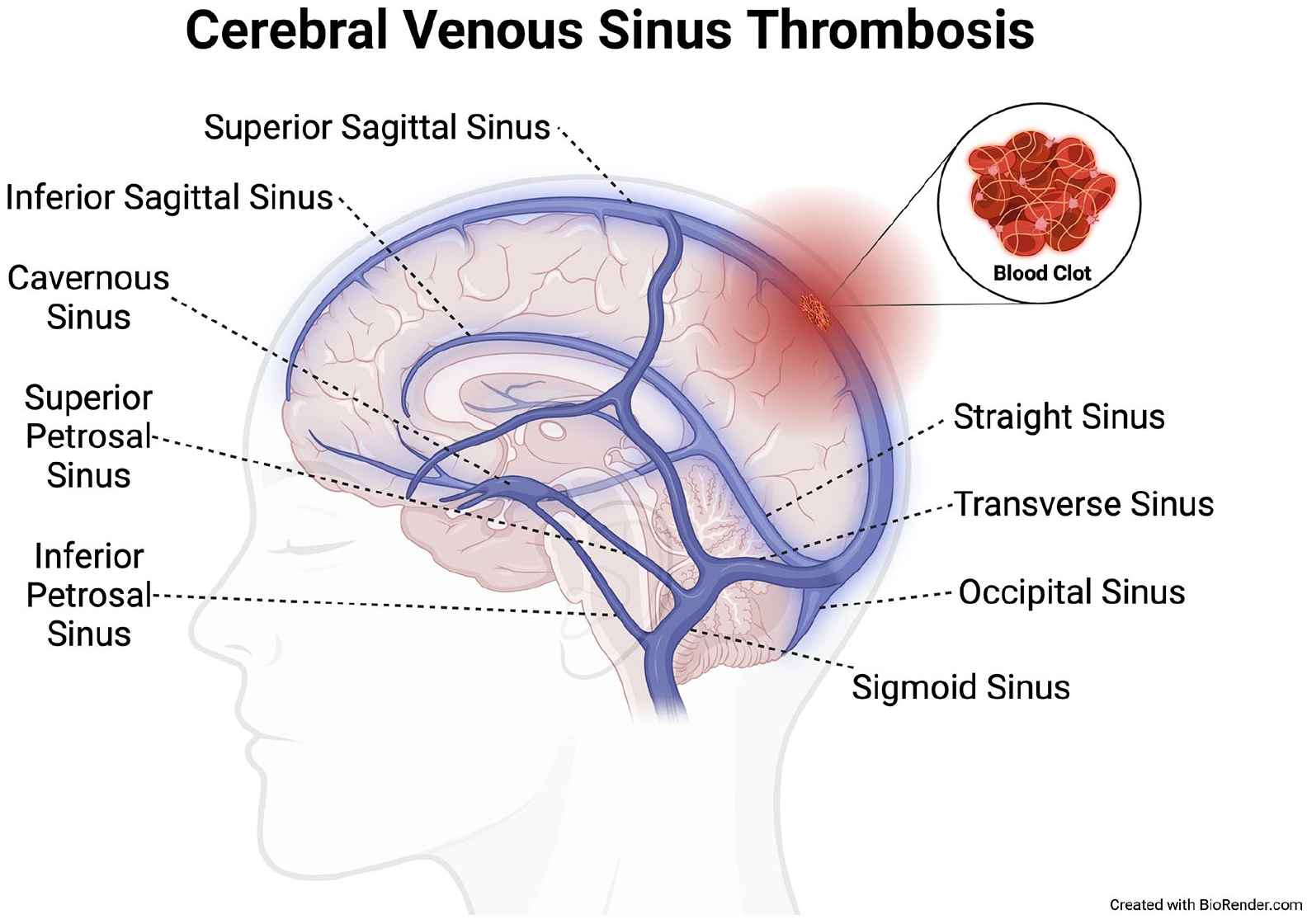
Blood clot formation (‘thrombosis’) in veins of brain causing cerebral venous sinus thrombosis.
Portal vein thrombosis (PVT) affects the portal vein of the liver, which receives blood from the spleen and intestines and then goes into the liver (Figure 2). 7 PVT occurs in approximately 1 in 100,000 individuals each year, but it is much more common in patients with liver cirrhosis. 8 The mesenteric veins receive blood from the small and large intestines. Mesenteric vein thrombosis (MVT) is less frequent but shares most of the risk factors that cause PVT. Splenic vein thrombosis refers to blood clots forming in the vein that receives blood from the spleen. This DVT is almost always found in combination with PVT and/or MVT. Indeed, it is common for a patient to have clots in the portal, mesenteric, and splenic veins simultaneously. Isolated splenic vein thrombosis has been described in patients with chronic pancreatitis and other pancreatic diseases, as well as in those with conditions that cause enlargement of the spleen.
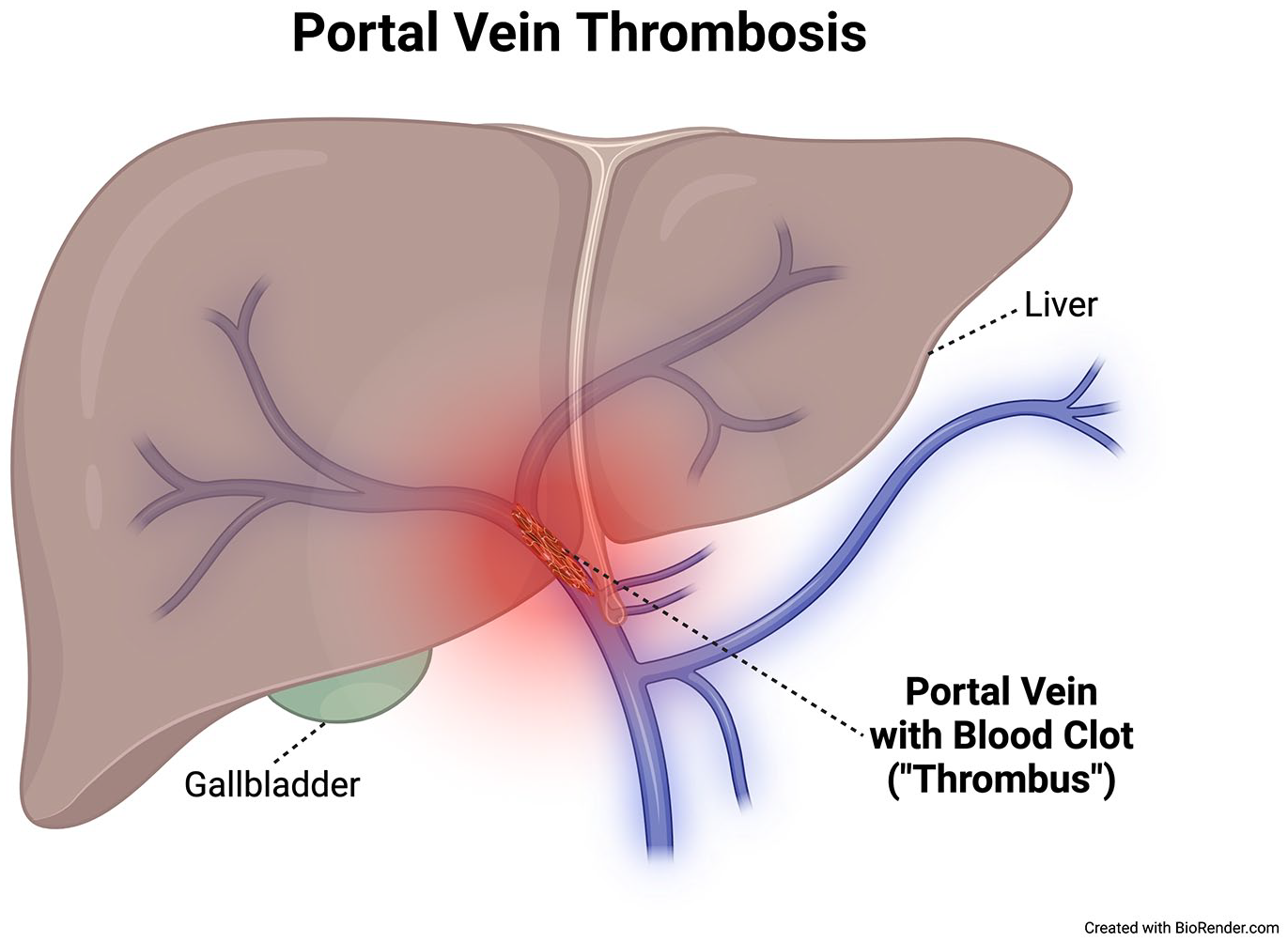
Blood clot formation (‘thrombosis’) in veins of liver causing portal vein thrombosis.
Budd–Chiari syndrome is a rare, unusual site of DVT affecting between 1 in 500,000 and 1 in 1 million individuals each year.8,9 This syndrome refers to DVT in the hepatic veins (which drain blood from the liver into the IVC), sometimes extending into the IVC. Budd–Chiari syndrome is more common in young adults and in young women.
Renal vein thrombosis refers to DVT involving the veins that drain blood from the kidneys (Figure 3). 10 This condition can occur rarely in infants who require hospitalization for serious infections, as well as with rare childhood cancers that start in the kidneys (Wilms tumors). In adults, the most common causes are kidney cancer, inflammatory diseases of the kidneys, and hypercoagulable states.
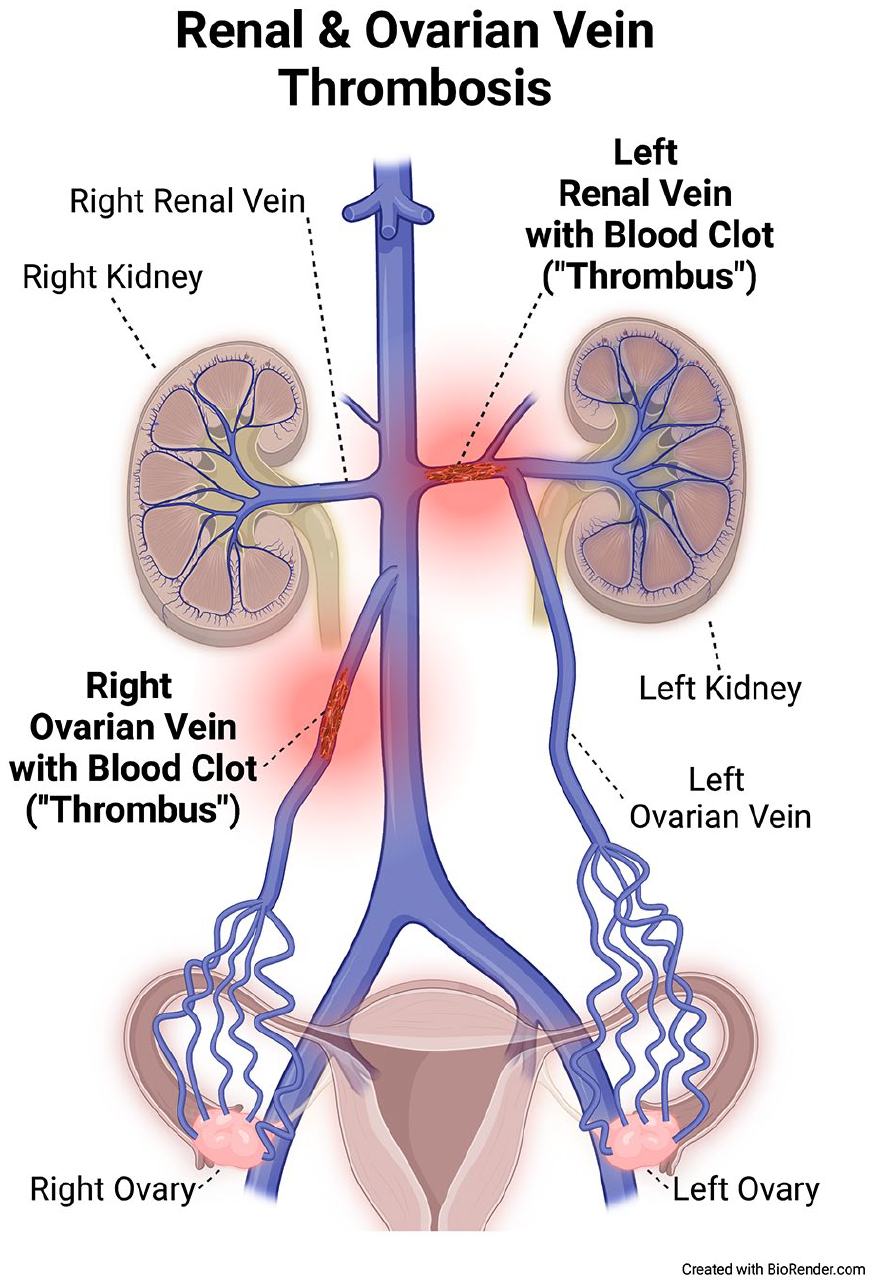
Blood clot formation (‘thrombosis’) in veins of kidneys and ovaries causing renal vein thrombosis and ovarian vein thrombosis, respectively.
Gonadal vein thrombosis refers to veins that drain the pelvic/sex organs, usually the ovarian veins in women (Figure 3), 10 and less commonly the testicular veins in men.
Retinal vein thrombosis (or occlusion) refers to blood clots that block a vein deep in the back of the eye (retina), leading to partial or total vision loss in the affected eye. Unlike other locations for thromboses at unusual sites, this condition is most associated with the same risk factors that cause heart disease, stroke, and peripheral artery disease, such as high blood pressure, high cholesterol, and diabetes. Rarely, it can be caused by underlying inherited or acquired hypercoagulable states.
What are the signs and symptoms of venous thrombosis at unusual sites?
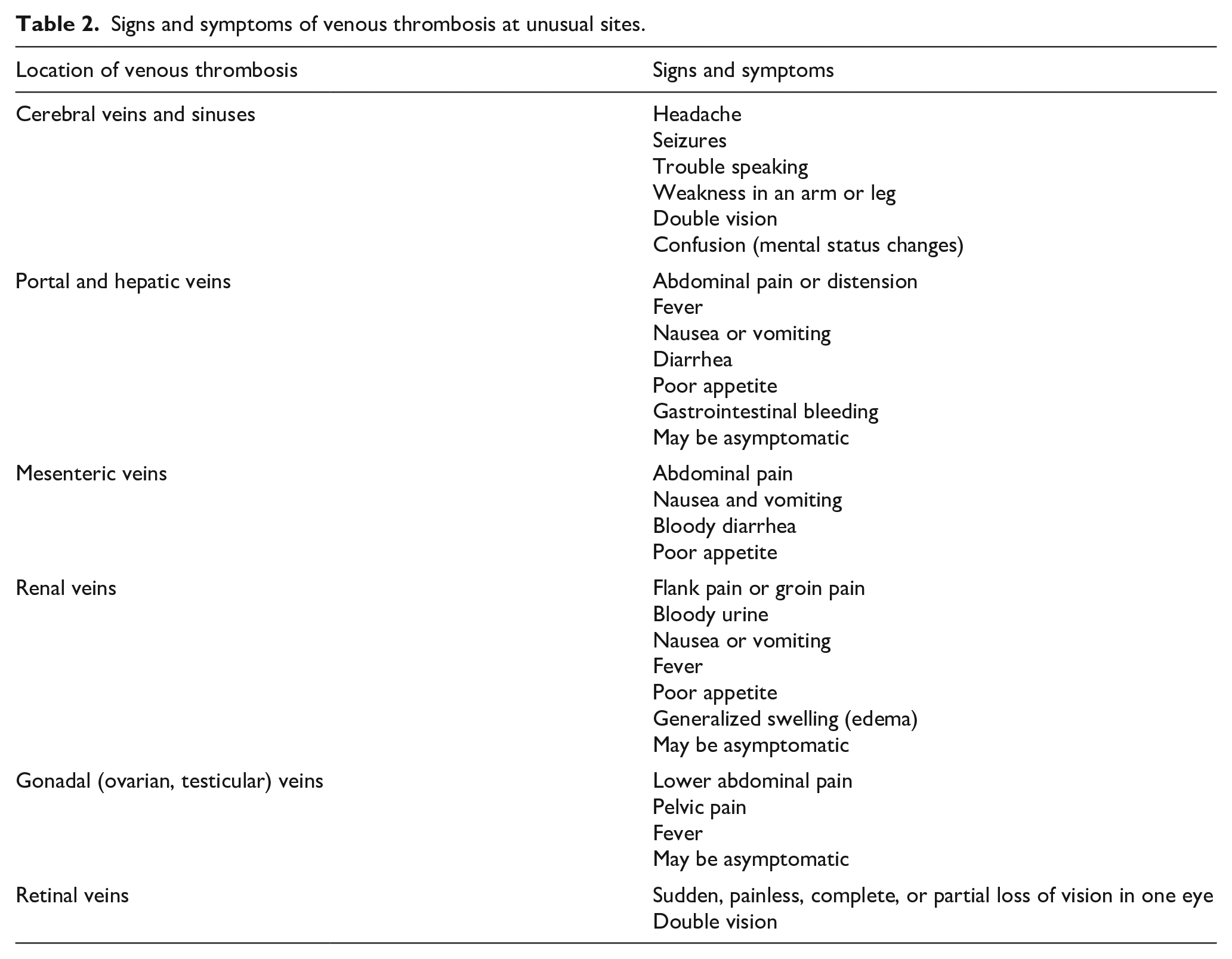
The most common symptoms seen with thrombosis at unusual sites are shown in Table 2. The signs and symptoms associated with venous thrombosis at unusual sites vary according to the location where they occur. Sometimes these thromboses may cause no symptoms and may be found when a computed tomography (CT) scan or magnetic resonance imaging (MRI) is done to investigate unrelated symptoms. But they may also present as a medical emergency, particularly when the DVT involves the mesenteric veins in the abdomen or the cerebral veins. Unlike DVT of the legs and arms, CVST, retinal vein thrombosis, and splanchnic vein thromboses do not pose a risk of PE. However, DVT involving the renal veins, the gonadal veins, and/or the IVC may lead to PE and cause symptoms of chest pain, shortness of breath, fast heartbeat, or coughing up blood.
Signs and symptoms of venous thrombosis at unusual sites.
How is venous thrombosis at unusual sites diagnosed?
Although DVT of the legs and arms can almost always be diagnosed using vascular ultrasound, 11 venous thrombosis at unusual sites typically requires a CT scan or MRI to confirm or rule out the diagnosis. Although vascular ultrasound can visualize the IVC and the portal, hepatic, and ovarian veins, CT and MRI are more accurate in establishing a diagnosis of thrombosis in those locations. Likewise, CT or MRI are the diagnostic tests of choice for CVST, mesenteric, and splenic vein thrombosis.
Retinal vein thrombosis is diagnosed by fundoscopy, an exam in which an ophthalmologist uses a magnifying lens coupled with a bright light to look inside the retina (back of the eye).
Once a thrombosis in an unusual site is diagnosed, additional blood tests may be ordered to help understand why the clot occurred. 5
What is the treatment for venous thrombosis at unusual sites?
Except for retinal vein occlusion, anticoagulation therapy (blood thinners) is the mainstay of treatment for DVT in unusual locations. Treatment is usually started with either intravenous heparin infusion or a type of heparin called low-molecular-weight heparin, which is administered by injections once or twice daily under the skin. After an initial period of anticoagulation with injectable or intravenous blood thinners, patients usually must continue anticoagulation – typically with an oral medication (‘blood thinner pill’) – for at least a few months, and perhaps indefinitely. Duration of anticoagulation therapy will vary from person to person: a shorter duration (a few months) is appropriate if the blood clot was caused by transient risk factors, whereas indefinite therapy may be necessary in cases with ongoing risk factor(s).
In patients with CVST who have life-threatening intracranial hypertension (brain swelling due to complete blockage of the veins by blood clots), catheter-based vascular procedures may have to be performed. With ‘mechanical thrombectomy’, a catheter is threaded into the veins inside the brain with the goal of removing clots. In severe cases, clot busting medications (thrombolytics) may also be infused into the clot. In rare instances, patients may require brain surgery.
In patients with mesenteric vein thrombosis who have serious mesenteric ischemia (a medical emergency in which the intestines suffer from lack of blood flow due to clotting and severe swelling), emergency surgery with or without catheter-based vascular procedures may be necessary.
What are the long-term effects of thrombosis at unusual sites?
The most common long-term symptom associated with CVST is frequent headaches, which often do not have any correlation with how much the blood clots dissolve. In patients with retinal vein thrombosis, the initial partial or complete visual loss may become permanent. Patients with portal or mesenteric vein thrombosis, or thrombosis of the renal veins, usually do not have any long-term symptoms related to the DVT itself; symptoms are typically related to the underlying illness that caused the DVT in the first place. In patients with IVC thrombosis in which the vein becomes significantly narrowed or blocked, patients may go on to develop chronic, intermittent leg pain, swelling, and redness (‘post-thrombotic syndrome’). 12
How can venous thrombosis at unusual sites be prevented?
There are no lifestyle measures known to prevent venous thrombosis at unusual sites, which typically are triggered by conditions outside one’s control. Hospitalized patients typically receive low doses of blood thinners to prevent DVT of the legs and PE, but it is not known if this strategy can prevent venous thrombosis at unusual sites as well. If the blood clots were caused by a specific risk factor which can be treated (such as infection, medication, or tumor), treating that underlying risk factor will be the best way to help determine the optimal duration of blood thinner treatment and to minimize or prevent future blood clots in those unusual locations.
Summary
Venous thrombosis at unusual sites refers to blood clots in the deep veins of the body other than the legs or arms. Blood clots may form in the veins of the brain, the eyes, the organs in the abdomen and pelvis, and the inferior vena cava. Symptoms depend on the site in which the blood clots develop. Diagnosis can sometimes be made with ultrasound, but more often with advanced imaging like CT or MRI scans. A thorough work-up to identify the underlying cause(s) is of utmost importance to determine duration of treatment with blood thinner medications.
The `Vascular Disease Patient Information Page' is a regular feature of Vascular Medicine. All articles in the collection are available for free online at http://journals.sagepub.com/vmjpatientpage.
The Vascular Disease Patient Information Page is provided for educational purposes only and is not a substitute for medical advice.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
Dr Alexandra Solomon currently holds the position of Anticoagulation Forum Ansell Fellow at Boston Medical Center. Boston Medical Center received an Anticoagulation Forum Ansell Fellowship Award, which was supported by an unrestricted educational grant from Janssen Biotech, Inc., administered by Janssen Scientific Affairs, LLC.
