Abstract

Keywords
Toe–brachial indices (TBI) are being integrated into international guidelines1,2 due to their utility as an adjunct test for peripheral artery disease (PAD), particularly in diabetes populations.3,4 The addition of an exercise protocol has been demonstrated to improve diagnostic accuracy of the traditional ankle–brachial index (ABI). 5 However, there has been limited investigation of the effect of exercise on the accuracy of TBI. Therefore, this pilot study aimed to determine the diagnostic test accuracy of the TBI for PAD following an exercise protocol in participants with suspected PAD.
This prospective cross-sectional study ran between 2019 and 2020 in a private vascular laboratory in Newcastle, Australia. Adults exhibiting signs or symptoms consistent with PAD were recruited. Exclusion criteria included inability to adhere to testing protocol (e.g., treadmill walking), conditions preventing toe or brachial pressure measurement (e.g., vasoneural disorders, connective tissue disorders, hallux wound or bilateral mastectomy). Informed written consent was obtained, and ethics approval was in place (H-2010-1230). One limb per participant was included in the study – the symptomatic limb, or where both limbs were symptomatic, the right limb. One vascular sonographer conducted all assessments, with inter-rater reliability previously determined to be acceptable. 6 All measurements were taken in a temperature-controlled clinical room (23–25°C). Pretesting participant protocols and the measurement procedure for pressure measurements for the vascular laboratory are consistent with current guidelines and as previously described.1,4 A Hadeco Smartdop 45 (Hadeco, Kawasaki, Japan) with a photoplethysmography probe was used to measure systolic toe pressure (TP). Participants walked on a treadmill at a maximum of 3 km/hour and a 10° incline for up to 5 minutes. If the participant experienced excessive lower extremity discomfort, angina, or dyspnoea, exercise was ceased. Toe, ankle, and brachial pressures were then immediately recorded in a supine position. Subsequently, visualisation of arteries and peak systolic velocities were obtained from the distal aorta to the foot via colour duplex ultrasound (reference standard) and were completed in the same session. Velocity ratios for grading of stenoses have previously been reported. 6
Descriptive statistics and measures of sensitivity, specificity, and positive and negative likelihood ratios with 95% CIs were calculated for TBI for detecting PAD – defined as one or more lower limb arteries with stenosis of ⩾ 50%. 7 The diagnostic threshold for PAD using TBI was considered to be < 0.70. Interpretation of postexercise TBI was evaluated firstly by using the diagnostic threshold of < 0.70 for PAD, and secondly, if the postexercise value was > 20% lower than the resting TBI. A receiver operating characteristic (ROC) curve was performed for TBI and postexercise TBI (online Supplementary file) and the area under the curve (AUC), calculated using IBM SPSS statistical software, Version 24 (IBM Corp., Armonk, NY, USA).
Participant characteristics, vascular testing results, and diagnostic accuracy results are presented in Table 1 (n = 50). ABI mean values fell within a normal range for resting and postexercise (1–1.3). TBI mean values were lower postexercise compared to resting values (mean TBI: 0.66 resting, 0.55 postexercise), which is similar to a previous study. 8 Using a diagnostic threshold of < 0.70 for PAD, AUC values for postexercise TP (0.88, 95% CI 0.78 to 0.97) and TBI (0.95, 95% CI 0.88 to 1.02) were higher than for resting measures (TP: 0.76, 95% CI 0.62 to 0.90; TBI: 0.83, 95% CI 0.69 to 0.97). The negative likelihood ratio for postexercise TBI (0.05, 95% CI 0.01 to 0.37) was important, 9 indicating a 20-fold decrease in the odds of having PAD in a patient with a negative result. Sensitivity of postexercise TBI (96.3, 95% CI 81.03 to 99.91) was higher than resting TBI (80.77, 95% CI 60.65 to 93.45). Specificity values were comparatively lower in resting TBI (73.91, 95% CI 51.59 to 89.77) and postexercise TBI (69.57, 95% CI 47.08 to 86.79). Interpreting postexercise TBI using a > 20% decrease relative to resting values had lower sensitivity (69.23, 95% CI 48.21 to 85.67), but higher specificity (87.50, 95% CI 67.64–97.34) than using the < 0.7 threshold for PAD.
Descriptive statistics and diagnostic test accuracy.
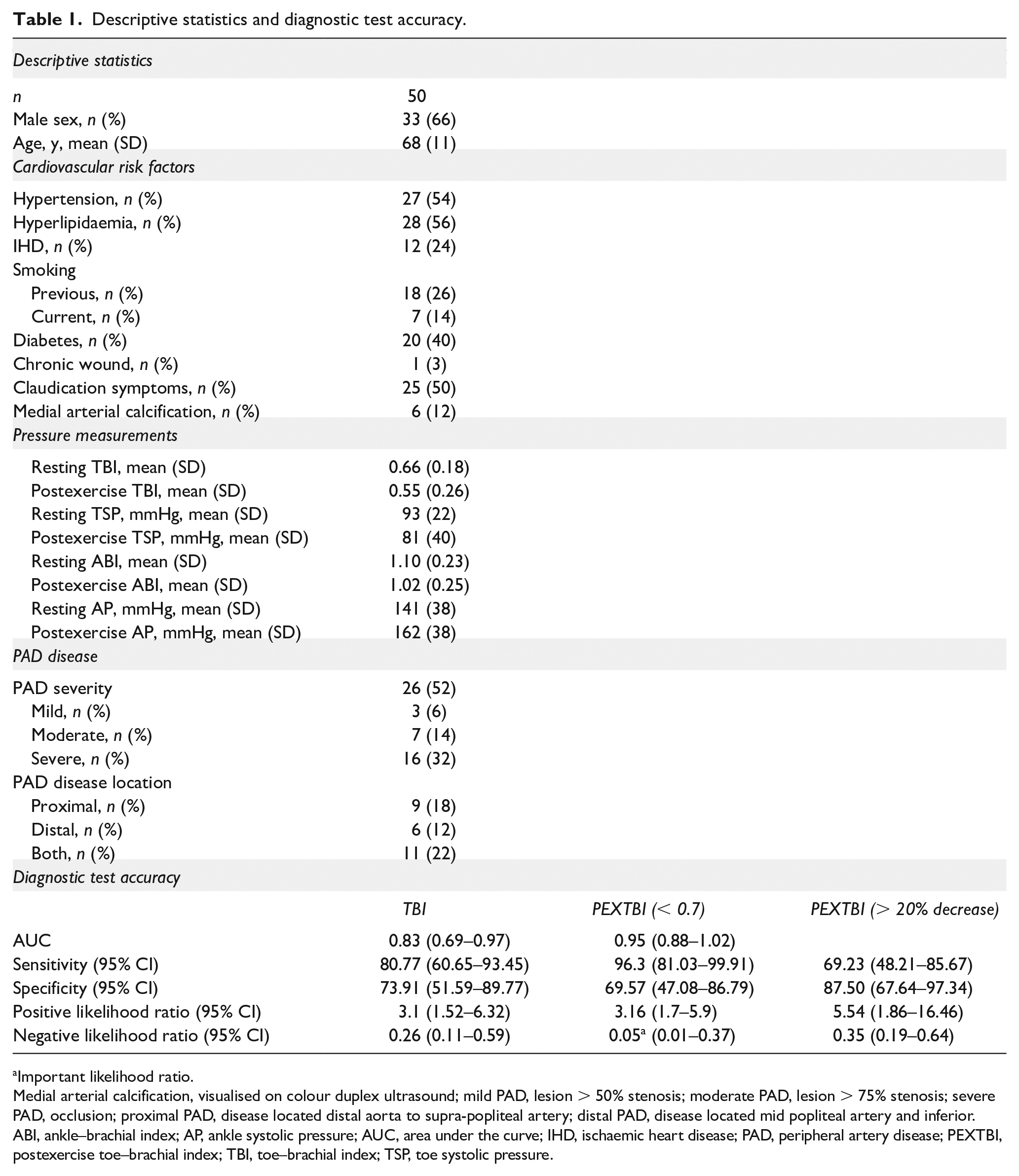
Important likelihood ratio.
Medial arterial calcification, visualised on colour duplex ultrasound; mild PAD, lesion > 50% stenosis; moderate PAD, lesion > 75% stenosis; severe PAD, occlusion; proximal PAD, disease located distal aorta to supra-popliteal artery; distal PAD, disease located mid popliteal artery and inferior.
ABI, ankle–brachial index; AP, ankle systolic pressure; AUC, area under the curve; IHD, ischaemic heart disease; PAD, peripheral artery disease; PEXTBI, postexercise toe–brachial index; TBI, toe–brachial index; TSP, toe systolic pressure.
Similar to previous studies in ABI, adding an exercise protocol increased the sensitivity and overall accuracy of TBI for detecting PAD, but low levels of specificity were demonstrated in both resting and postexercise TBI. This indicates false positives are likely using resting TBI, but more so in postexercise TBI. Mean postexercise TBI values were lower than resting measures, consistent with a previous study in healthy participants. 10 Healthy participants normally show a mild drop in postexercise ABI – with ankle pressures increasing, but less than brachial pressure, due to the vasodilation effect in exercising limbs. 11 A 20% difference between resting and postexercise ABI values is currently considered indicative of pathology, but it is unknown whether the same difference applies to TBI. The lower specificity of the postexercise TBI found in this present study may reflect a reduction in TBI that is a normal physiological response to exercise, which has been demonstrated in another small study of 27 nonpathological limbs. 12 Further investigation of normal values for postexercise TPs and TBI is required to quantify thresholds to determine pathological response. The varying degrees of sensitivity and specificity across different testing methods also highlights the need for clinicians to use a variety of testing methods, in conjunction with the clinical picture, to guide ongoing management.
Notable limitations included the lack of blinding (although risk of bias is limited as the index testing was completed first), the subjective nature of both testing methods, and potential order effect due to lack of randomisation. Other limitations include the possibility of measurement error (unlikely given the previously established reliability of the tester) and a small sample size given the pilot nature of the study.
The results of this pilot study suggest the postexercise TBI may be useful as an adjunct test to help identify PAD in patients with suspected disease. Postexercise TBI is worthy of further large-scale studies to comprehensively establish diagnostic accuracy.
Supplemental Material
sj-pdf-1-vmj-10.1177_1358863X211039548 – Supplemental material for Diagnostic accuracy of postexercise toe–brachial index for identifying peripheral artery disease (PAD): A pilot study
Supplemental material, sj-pdf-1-vmj-10.1177_1358863X211039548 for Diagnostic accuracy of postexercise toe–brachial index for identifying peripheral artery disease (PAD): A pilot study by Peta Ellen Tehan, Richard Rounsley, Mathew Sebastian and Vivienne Helaine Chuter in Vascular Medicine
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplementary material
The supplementary material is available online with the article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
