Abstract

What are compression socks and who needs to wear them?
Compression socks (also called compression stockings or compression hose) are snug-fitting, elastic garments that can help treat the symptoms of multiple medical conditions related to the veins and the lymphatic system, including varicose veins, 1 post-thrombotic syndrome, 2 lymphedema, 3 and more.
Compression socks are often called ‘graduated’ compression because the highest pressure is applied near the ankle and gradually decreases as it goes further up the leg. The squeezing action of the compression sock helps to force the blood in the leg veins to return to the heart, taking fluid that has been trapped in the tissue with it.
What are the options for compression socks?
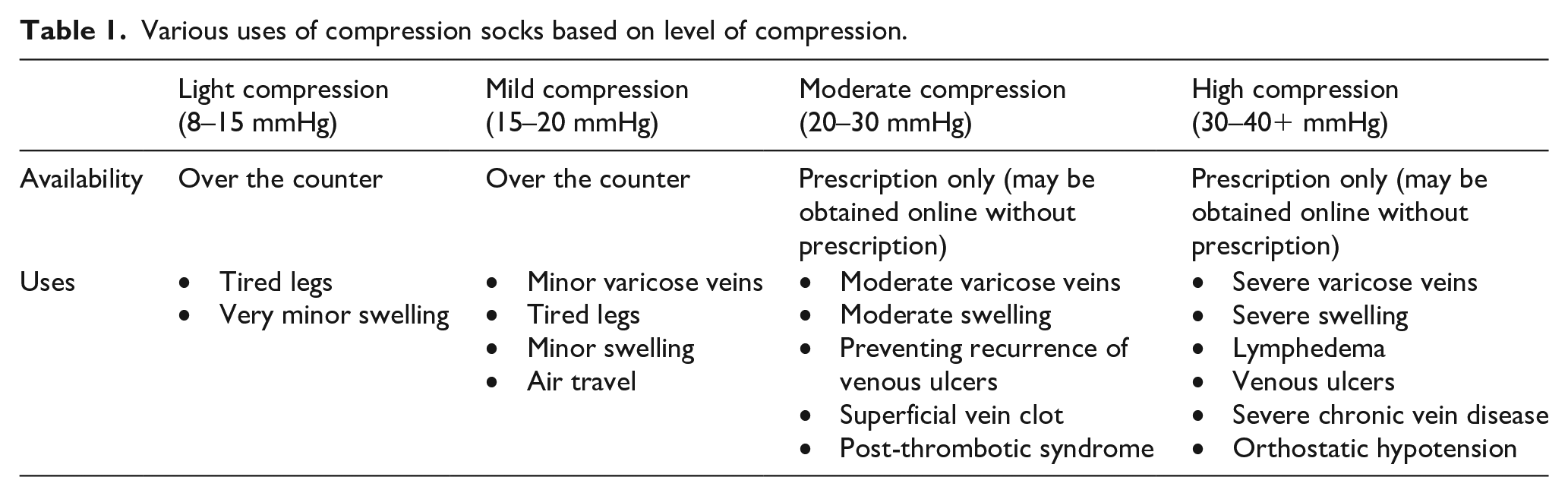
The strength of compression socks is measured in millimeters of mercury (mmHg), similar to a blood pressure cuff. This number tells the amount of pressure or compression the socks will apply to the leg. The higher the number, the stronger the degree of compression. Table 1 shows the different options for compression and typical uses.
Various uses of compression socks based on level of compression.
Compression socks come in different sizes. Each person should have their legs measured to ensure that the size is correct. Otherwise, the socks may not be comfortable. If the socks are too loose, then they may not relieve the symptoms or treat the swelling. If the socks are too tight, then blisters may occur or they may restrict the blood flow too much. If the size of the leg changes (e.g. due to weight gain, weight loss, or significant improvement in leg swelling), then the person may need to be re-measured. Measurements should be taken in the morning, when the legs are the least swollen.
Compression socks come in various lengths, including knee-high, thigh-high, and waist-high (tights or pantyhose). They also come in many different fabrics, colors, and patterns. The longer the sock, the more difficult it may be to don (put on), so knee-high socks tend to be the most commonly prescribed. Patients with painful varicose veins in the thighs may benefit from thigh-high stockings. With varicose veins behind the knee, thigh-high stockings or tights may be more comfortable, as the band or gripper of a knee-high sock may put pressure directly on the bulging veins. Zippered compression socks are available. Some patients may find that these are easier to put on.
Compression socks come in open-toe and closed-toe varieties, and in most cases, the patient chooses the style. Patients who wear stronger compression socks may find that the open-toe style allows for easier donning using a donning aid, which is a device that assists in pulling the sock over the foot and calf. For patients whose feet and toes swell, open-toe socks may increase the swelling of the uncovered toes.
When should compression socks be worn?
For the best results, compression socks should be put on first thing after getting out of bed and worn until the end of the day. The socks help to fight gravity because sitting with the legs down or standing can worsen swelling, discomfort, or other symptoms in patients with vein and lymphatic disorders. For those who have rapid onset of swelling once they are in an upright position, it may be helpful to lie down for a few minutes with the legs elevated above the level of the heart after showering and before putting on socks, or to shower in the evening. Patients who know they are going to be sitting or standing for long periods without moving around—for example, on a long plane flight—should make sure they wear their compression socks.
When should compression socks not be worn?
Compression socks are a relatively safe treatment, but some patients should avoid them. For patients with severe peripheral artery disease (PAD), the compression socks could further restrict blood flow into the leg. (To learn more about PAD, read the relevant Vascular Disease Patient Information Page 4 .) However, most patients with PAD can safely wear compression socks for other conditions after thorough evaluation by a vascular specialist. Compression socks are often a critical part of treatment for venous ulcers, which are open wounds on the legs that are related to blood that flows poorly out of the leg. But for some patients with wounds, compression socks may be difficult to get over bandages and dressings, so the treating team may elect for a different type of compression garment.
Compression socks are not usually worn while sleeping because they could bunch up and restrict blood flow, which could be dangerous. Also, for most patients who sleep in a bed with the legs at least level with the heart, swelling naturally improves overnight.
Should compression socks be worn during exercise?
Some athletes wear compression socks during exercise to improve the blood flow from the legs back to the heart and lungs (‘venous return’) and to prevent the blood in the veins from pooling in the lower legs. In general, some people feel better wearing compression socks during exercise and notice less swelling afterwards. However, some people find wearing compression socks during exercise to be hot or uncomfortable. Fortunately, the calf muscles help to push the blood back toward the heart when walking, which helps to do the same job as the socks.
What can help with putting compression socks on?
Compression socks can be difficult to put on. Donning compression socks requires proper technique, as shown in Figure 1. Videos are also available online to assist with the application of the socks. Many people instinctively bunch or roll their socks up before putting their foot in, but then the bunched layers of sock create higher compression that can be difficult to squeeze the foot through. Wearing textured rubber gloves, such as the kind used for washing dishes, can be helpful to pull up the sock and smooth out any wrinkles. Compression sock manufacturers also make gloves to aid with donning.

Steps for putting on knee-high compression socks.
For most venous and lymphatic conditions, moisturizing the skin is an important part of treatment. However, this should be done in the evening after taking off compression socks. Moisturizing before putting compression socks on makes them more difficult to don. Some patients may wish to use powder or cornstarch prior to donning socks, which can help the sock slide across the skin. Patients who lack grip strength or who are unable to reach their feet because of musculoskeletal issues, obesity, or other concerns, may wish to ask a family member or caregiver to assist.
Several donning devices can also help with putting on compression socks. These devices are available at medical goods retailers and online.
What is the difference between TED hose and compression socks?
TED stands for ‘thromboembolic deterrent’, which means that the socks are meant to decrease the risk of blood clots. These socks are often white and open-toe, and they are used in hospitalized patients who are not able to walk around, especially after surgery. The level of compression is typically 20 mmHg or less, and they are designed to last approximately 3 weeks. Typically, the compression in TED hose is static, not graduated—in other words, the amount of pressure is the same throughout the length of the stocking, unlike a compression sock, whose higher compression at the ankle helps push blood out of the leg.
Graduated compression socks are designed for people who are able to walk around, and they are more durable than TED hose. Compression socks that are properly cared for will last the equivalent of being worn every day for about 4 to 6 months. Eventually the socks will lose their elasticity and no longer control symptoms. Many experienced wearers of compression socks can tell when their socks are worn out because they become much easier to put on due to being stretched out.
Do compression socks help to prevent blood clots?
Research has shown that compression socks may help prevent blood clots from forming in the deep veins of the legs, a condition known as deep vein thrombosis (DVT). Health care practitioners often recommend wearing compression socks during air travel to help prevent DVT and to control leg swelling that sometimes occurs when seated for long periods. DVT is uncommon among travelers on flights shorter than 5 hours.
Are compression garments covered by insurance?
Depending on the plan, some private insurers will cover a portion or all of the cost of compression garments. Medicare generally only covers compression socks for the treatment of a venous leg ulcer. If medically necessary, the cost may be reimbursable with a health care flexible spending account.
What can make the compression socks last longer?
Following the laundry instructions is important to prolong the life of the socks, which should be washed daily. Some can be machine washed and/or dried, whereas some require hand washing and/or air drying. A mild detergent and warm or cold water should be used. Woolite®, bleach, and fabric softeners should not be used because they break down the elastic. The socks should always be dried on low heat if using a dryer, but air drying may be preferred, as it will lengthen the sock’s useful life even if it is rated for machine drying. A mesh lingerie bag can prevent the material from snagging or getting stretched out by tangling with other clothes. If a snag occurs in the sock fabric, clear nail polish can help to prevent it from becoming a hole.
Are there any options for compression other than socks/stockings?
Occasionally the health care team may choose alternative compression garments, either because compression socks are too difficult for the patient to don or because of the condition being treated, the shape of the patient’s legs, or other factors. One option is compression bandages, which come in different strengths and degrees of stretch and may be changed daily or every several days, depending on the type and the reason they are used. Some patients may be prescribed a compression stockinette, which is a tube of elastic fabric that is cut to fit the leg and is pulled on like a sock and typically has a lower strength of compression than a sock. Other patients may be prescribed a stretchy sleeve with a hook-and-loop (Velcro) closure that allows for easier donning and adjustment of compression.
Patients with extremely large or small legs or whose calf is much larger than the ankle may need custom socks, but most people are able to find off-the-shelf socks that fit.
Some patients with lymphedema and other conditions may be prescribed an electric compression pump that is worn for several hours each day while seated or lying down. These devices can be helpful while they are being worn, but without a compression garment, swelling often recurs rapidly in the course of the day.
What else can be done to help reduce leg swelling?
Most patients with venous and lymphatic conditions who are prescribed compression garments are also encouraged to exercise. This exercise should ideally use the calf muscles, such as walking. Contraction of the calf muscles helps to push blood out of the leg and may improve swelling. Water-based exercise including swimming, water walking, or water aerobics may be helpful in improving swelling, with the advantage of being easier on the joints.
Anyone diagnosed with a venous or lymphatic disorder should work to maintain a healthy weight. The veins and lymphatic vessels must drain through the pelvis and abdomen to get back to the heart, and excess weight can make drainage more sluggish and contribute to leg swelling.
Some people may be sensitive to the effects of dietary salt (sodium), and if so, they should aim to reduce salt intake. Salt is added to most processed foods including deli meats and cheeses, soups, and frozen meals.
Leg elevation may help to control swelling and other symptoms. Patients should elevate their legs when possible during the day. The higher, the better. Using a stool when seated at a desk or stacking up pillows on the sofa can help. Swelling is typically better upon awakening after lying flat with the legs level with the heart overnight. On the other hand, patients who sleep in chairs or recliners may find that their swelling does not get better when they sleep, because their legs are below the level of the heart.
Summary
Compression socks are prescribed to treat many different venous and lymphatic disorders to help control leg swelling and other symptoms. Patients who are prescribed compression socks must be measured to ensure they get the right size sock for their leg shape. Donning aids can help patients who have difficulty putting on their socks, and sometimes doctors will prescribe alternative forms of compression, like sleeves or bandages. Exercise, weight maintenance, and leg elevation are important additional treatments to help with leg swelling.
The ‘Vascular Disease Patient Information Page’ is a regular feature of Vascular Medicine. All articles in the collection are available for free online at http://journals.sagepub.com/vmjpatientpage
The Vascular Disease Patient Information Page is provided for educational purposes only and is not a substitute for medical advice.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
