Abstract
Introduction
Intensive case management is an essential component of community mental health care system for people with severe mental illness. We examined the association of service types with previous and future functioning and hospital admissions using a longitudinal data, to clarify the case managers’ activity.
Methods
The study included baseline assessment, recording and analysis of services, and follow-up assessment. At the baseline and follow-up assessments, we examined functioning (ie, Personal and Social Performance Scale: PSP) and hospital admission of users for past periods. For recording and analysis of services, we recorded services provided by case managers over 2 months, and five core services were used for the analyses: regular face-to-face contact, outreach services, hospital-based (outpatient) services, and easy contacts and coordination.
Results
Outreach services were significantly associated with hospital admissions at baseline and follow-up assessments. Hospital-based services were significantly associated with lower PSP scores and hospital admission at follow-up assessment. Easy contacts and coordination were associated with lower PSP scores at follow-up assessment.
Conclusion
In Japan, most services are provided in the outpatient department of hospital, and outreach services are relatively time consuming for case managers; thus, the indications for providing outreach services need to be carefully considered. Therefore, we suggest that case managers provide flexible services to users according to the circumstances in Japan.
Introduction
Intensive case management (ICM) is an essential component of the community mental health care system for people with severe mental illness. 1 While several packages of ICM services are implemented according to regional conditions, such as Assertive Community Treatment (ACT),2,3 ICM packages generally have common service structures. For example, in ICM programs, the caseload is restricted to a low number ( ≤ 20); case managers coordinate the services offered, directly provide services, and outreach services are sometimes provided. 1 Indeed, past studies have provided a large body of evidence for the effects of structured ICM programs on reducing hospitalization-related outcomes in economically developed countries. 1 Implementation and dissemination of ICM is globally widespread and was first applied in Japan in the 2000s. 4
In addition to the effects and service structures of ICM packages, service contents have been also examined.5-9 Based on the responses to open-ended questions and discussion with case managers, Fiander and Burns 6 suggested 10 categories of ICM services: housing, finance, daily living skills, criminal justice system, occupation and leisure, engagement, physical health, caregivers and significant others, specific mental health intervention or assessment, and medication. A recent network analysis on case management services also proposed 5 types of core service: regular face-to-face contact, outreach services, hospital-based (outpatient) services, and easy contacts and coordination. 5 In ICM packages, case managers provide a wide variety of services including these contents.
Whereas the basic services provided by case managers are becoming clearer based on previous findings,5,6 the intensity and contents of services are individually different among users in the actual service setting. For example, longer duration of outreach services appears to be related to lower functioning in people with mental illness. 5 Vocational services were more frequent in younger users, and physical health services were more frequent in older users. 10 These findings suggested that the intensity and contents of services are determined at least in part based on users’ individual conditions as evaluated before services are provided. In addition, people with mental illness have high relapse rate 11 and are frequently readmitted to hospital. 12 That is, the symptoms and conditions of users are always changing, and some of these changes lead to future deterioration of function and hospital admission. We speculated that case managers provide flexible services to cope with future risks.
Taken together, the previous findings suggested that case managers determine services contents based on both users’ previous conditions and future risks. Past studies have examined the association of service types with users’ previous conditions as evaluated before providing services5,10; however, few studies have addressed whether services were provided according to individual future conditions. Therefore, the present study was conducted to examine the association of service types with previous and future functioning and hospital admissions in ICM users, using longitudinal data.
Method
Data Acquisition
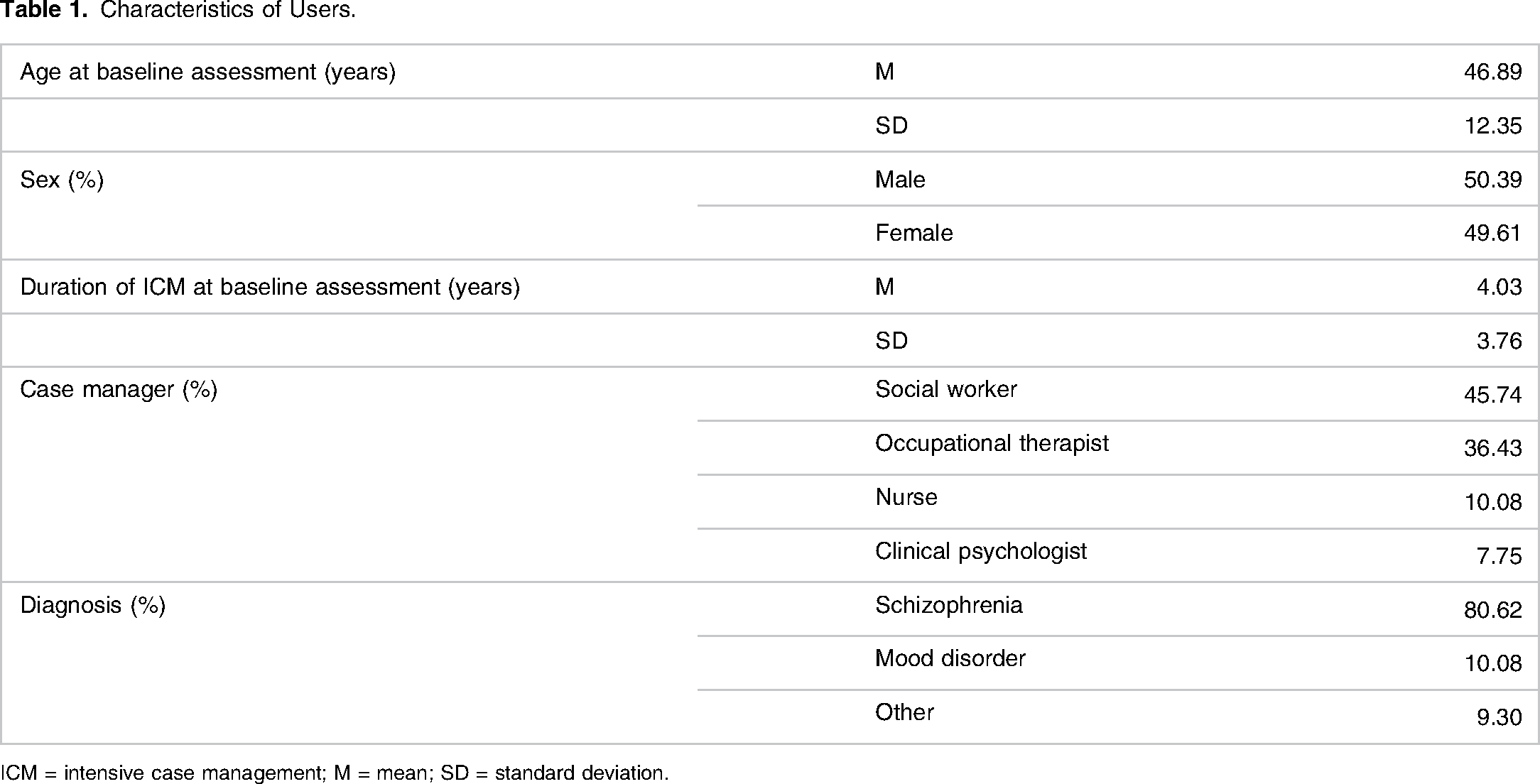
This study consisted of baseline assessment, recording and analysis of services, and follow-up assessment (see Figure 1). A portion of the data for baseline assessment and recording of services was taken from our previous studies.5,13-15 Firstly, we recruited patients who received psychiatric outpatient services, psychiatric day care, or outreach services in Asahi General Hospital as study participants (n = 744). The following inclusion criteria were set for baseline assessment: age over 20 years; continuous use of services for at least 6 months at the participating medical institution or a total duration of mental health service use of at least 12 months; and diagnosis codes from F10 to F99 in the International Statistical Classification of Diseases and Related Health Problems, 10th revision (ICD-10). We also set the following exclusion criterion: utilizing residential care facilities for the aged and disabled, except for group home care. A total of 520 patients were eligible, and five of them declined to participate. Among the participants, the 144 ICM users at baseline assessment were recruited for recording and analysis of services, and six of these ICM users declined to participate. In the follow-up assessment, we could not follow 9 participants. Finally, data from 129 ICM users were used for this study Table 1. Written informed consent was obtained from all participants for baseline assessment, recording and analysis of services, and follow-up assessment. All procedures involving human participants were approved by the ethics committee at Asahi General Hospital (2016092001). Flowchart of participants. Characteristics of Users. ICM = intensive case management; M = mean; SD = standard deviation.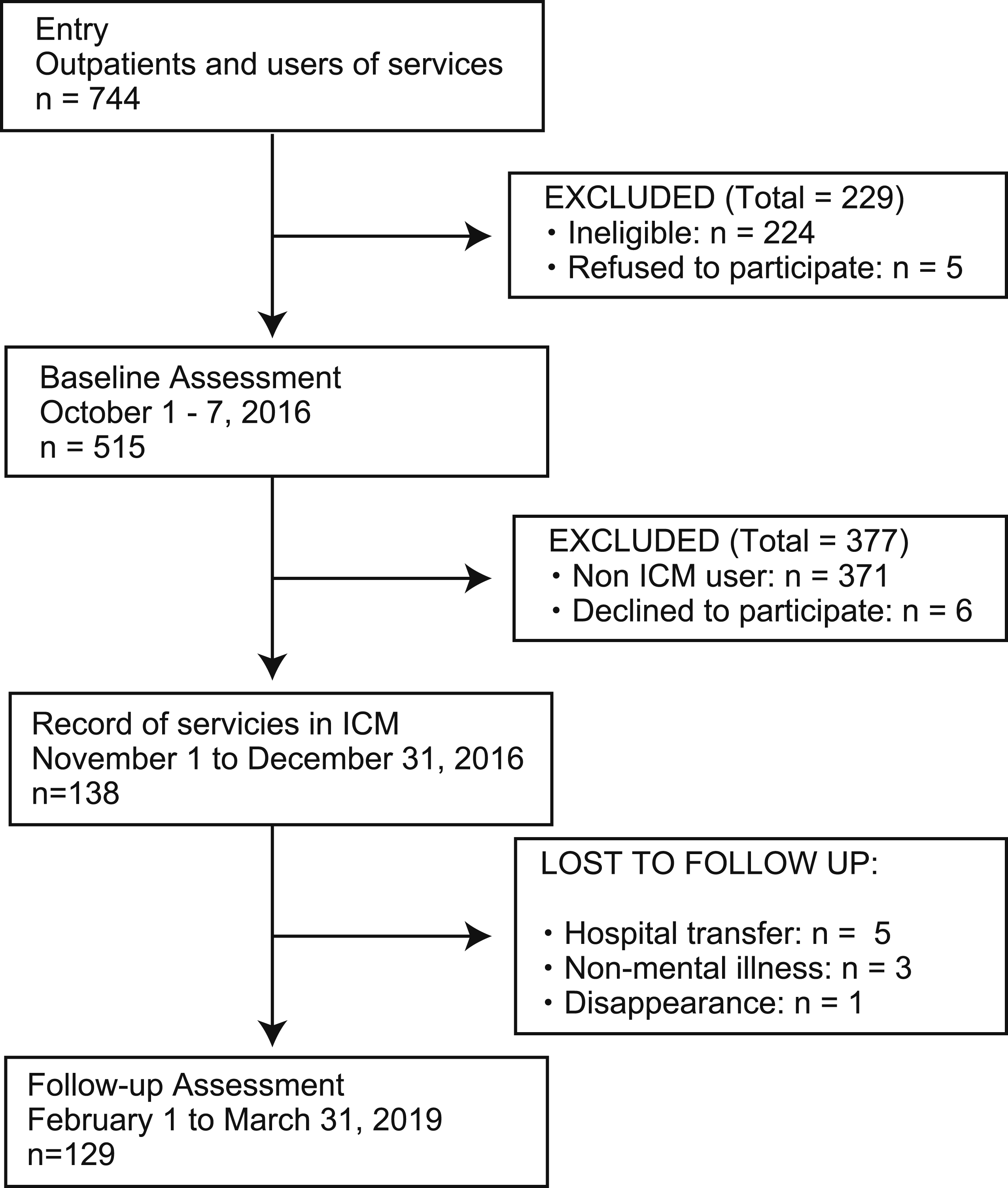

Baseline and Follow-up Assessments
Functioning in each participant was evaluated using the Japanese version of the Personal and Social Performance Scale (PSP). 16 The attending doctor performed PSP at baseline assessment, and the case manager performed PSP at follow-up assessment. PSP consists of the following four domains: socially useful activities, personal and social relationships, self-care, and disturbing and aggressive behavior. 17 PSP scores range from 0 (ie, low functioning) to 100 (ie, high functioning).
In the baseline assessment, case managers were asked to report the number of hospital admissions for the past year in each participant. In the follow-up assessment, they were asked to report the number of hospital admissions for the past 2 years.
Record of Services
The case manager recorded the services provided for each participant for 2 months. The services were classified into 16 categories: Intake, assessment or creation of a care plan; Coordination of services with other institutions; Coordination of services in the medical institution; Care meeting; Counseling; Support for self-care activity; Support for social life; Support for interpersonal relationships; Support for housing; Support for job seeking or entering school; Support for accompanying the user to a psychiatric hospital; Support for accompanying the user to other hospitals; Support for mental health medication; Support for medication for other problems; Support for the user’s family; and Other. We further classified the services into three settings for communication: Hospital-based (outpatient) service; Outreach service; and Telecommunication, based on a service process survey. 18 In our previous study, 5 we identified 5 types of core ICM services: regular face-to-face contact (ie, hospital-based counseling), outreach services (ie, outreach support for mental health medications), hospital-based services (ie, hospital-based support for mental health medication), easy contacts (ie, counseling via telecommunication), and coordination (ie, hospital-based coordination of services in the medical institution, and coordination of services with other institutions via telecommunication). In Japan, most mental health professionals belong to hospitals, and most services are provided in the outpatient department of hospital. Hence, hospital-based service reflected services provided by case manager in the outpatient department of hospital. In this study, we used the number of the 5 services provided for 2 months as the indices of amounts of services. The percentages of users who received services were 48.02% for regular face-to-face contacts, 36.43% for outreach services, 7.75% for hospital-based services, 17.05% for easy contacts, and 44.19% for coordination.
Statistical Analysis
The difference in PSP scores between the baseline and follow-up assessments was assessed by a paired t-test, and the difference in the percentage of users admitted to hospital was assessed by a chi squared test. Pearson’s correlation was used to examine the relationship between PSP scores at baseline and follow-up assessments. Because about 20% of users were admitted to hospital for both surveys, the number of hospital admissions was binarized for the analysis (ie, zero: 0, and one or more: 1). Then, we performed a multiple logistic regression analysis predicting hospital admission at follow-up assessment from the PSP score and hospital admission at baseline assessment. Kendall’s correlations were used to examine the relationships between PSP scores and types of services. The percentage of users who received each service was lower than 50%. Thus, the number of services was binarized for the analysis (ie, zero: 0, and one or more: 1), and we performed multiple logistic regression analyses. In the stepwise multiple logistic regression analyses, we added age, sex (female = 0, male = 1), and PSP scores and hospital admissions at the baseline and follow-up assessments to the first model. The analyses were performed using R 3.5.2. 19
Results
Characteristics of Users
Table 1 shows characteristics of users. Mean duration of ICM at baseline assessment was 4.03. Over 80% of users were diagnosed as schizophrenia. Over 80% of case managers were social workers or occupational therapist.
Functioning and Readmission at Baseline and Follow-up Assessments
Personal and Social Performance Scale and Percentages of Users Admitted to Hospital at Baseline and Follow-up Assessments.
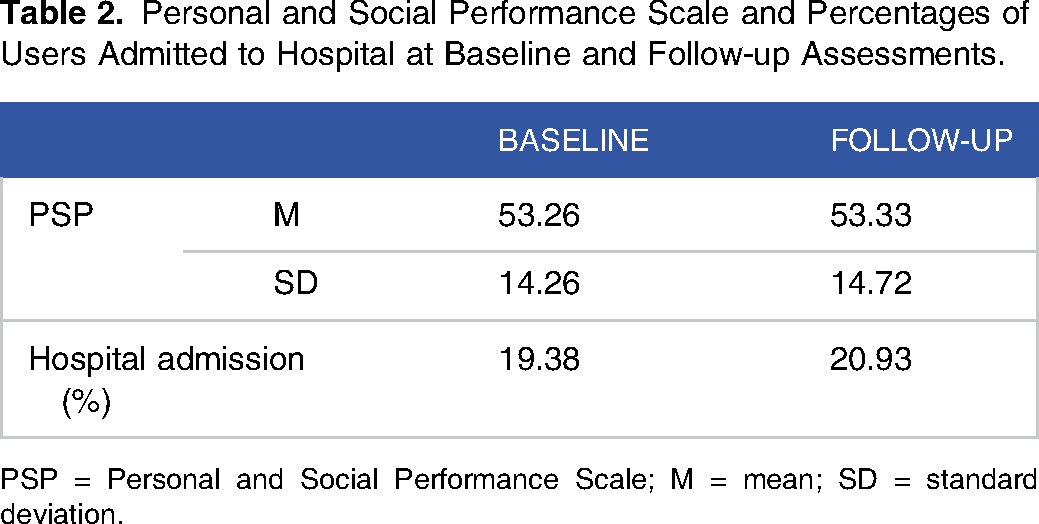

PSP = Personal and Social Performance Scale; M = mean; SD = standard deviation.
Association between functioning and types of services
Relationship Between Personal and Social Performance Scale (PSP) and Types of Services (Kendall’s Rank Correlation Coefficient).

Results of Stepwise Logistic Regression Analyses for the Association of Service Types With Previous and Future Functioning and Hospital Admissions.
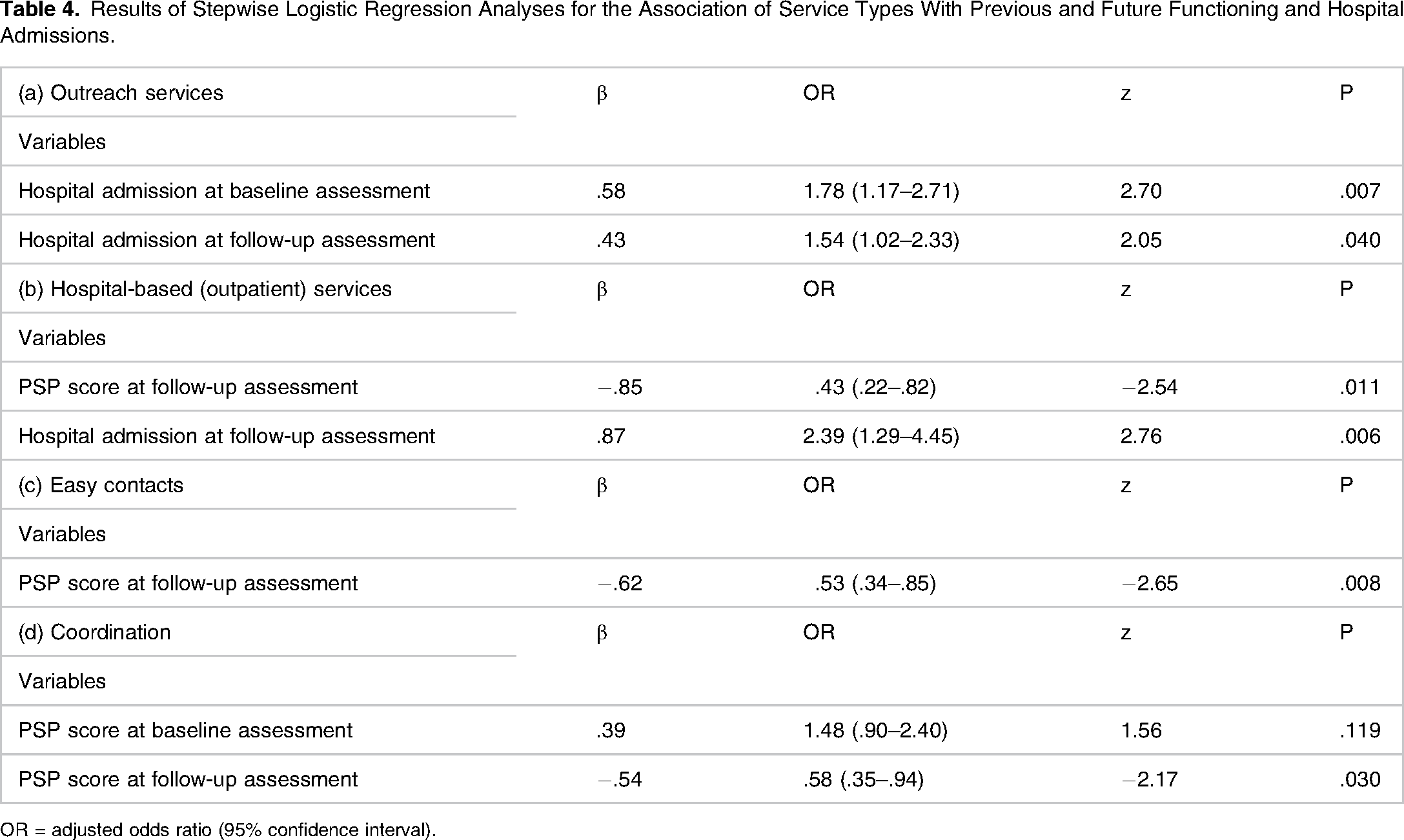
OR = adjusted odds ratio (95% confidence interval).
Discussion
The study aimed to examine the association of hospital admission and service types with participants’ functioning at baseline assessment or follow-up assessment using longitudinal data. The previous studies5,10 suggested that case managers of ICM programs determined their service contents based on both users’ previous conditions (eg, previous hospital admission) and future risks (eg, risk assessment of future admission) that were only evaluated before providing services. Since this study assessed the service types and participants’ functioning before and during providing case management, it augments existing evidence.
Regular face-to-face contact (ie, hospital-based counseling) was not significantly associated with any variables. In our previous study, regular face-to-face contact was the most frequently provided type of service. 5 Maintaining contact with users is one of the basic functions of case management. 1 We thought that regular face-to-face contact was a reflection of basic functions of ICM. It is possible that regular face-to-face contact was provided to users independent of symptoms and conditions.
Outreach services (ie, outreach support for mental health medications) were associated with hospital admissions at baseline assessment. Outreach services are a central component of ICM programs; for example, in Canada, most case management services were reported to be provided outside of the office. 20 In Japan, most services are provided in the outpatient department of hospital. 5 In such circumstances, it was considered that outreach services were time consuming for individual case managers. Therefore, we suggest that outreach services were mainly provided to users who had a risk to avoid attending a hospital, that is, users admitted to hospital. In addition, there was a significant association between outreach services and hospital admission at follow-up assessment. ICM services aim to keep people with severe mental illness living in the community, that is, the prevention of hospital admission is important for case managers. Thus, outreach services might be provided to prevent users from being admitted to hospital.
Hospital-based services (ie, hospital-based support for mental health medication) were significantly associated with lower functioning and hospital admission at follow-up assessment. Hospital-based service reflected services provided by case manager in the outpatient department of hospital. Users at risk of deteriorating functioning and admission to hospital need to receive services. 21 In Japan, most services are provided in the outpatient department of hospital. 5 Users frequently received hospital-based support for mental health medication for medical adherence when they attended to hospital to receive several types of services. Thus, hospital-based support for mental health medication was associated with the opportunity of receiving hospital-based services. 5 Hence, we suggested that the opportunity to attend the hospital is increased for users at risk of deteriorating functioning and admission to hospital. In Japan, case managers also belong to hospital, and ICM is performed as hospital-based services. The findings showed that the hospital-based ICM is convenient for Japanese mental health system.
Easy contacts (ie, counseling via telecommunication) were significantly associated with lower functioning at follow-up assessment. Symptoms, situation, and characteristics of mental illness are always changing.11,12 Telecommunication was considered convenient for flexibly coping with urgent changes. Therefore, case managers seemed to make contacts with users via telecommunication for urgent changing.
Coordination (ie, hospital-based coordination of services in the medical institution and coordination of services with other institutions via telecommunication) was significantly associated with lower functioning at follow-up assessment, whereas the association of coordination with lower functioning at baseline assessment was not significant. Coordination is a core content of case management services to arrange for services to be delivered. 22 Baseline assessment was performed during October 1–7, 2016, and recordings of services started form November 1, 2016, that is, there was about-one-month-duration from baseline assessment to recordings of services. We considered that coordination had performed for users with lower functioning at baseline assessment in the about-one-month-duration. On the other hand, it seemed that coordination for new services was needed to prevent risk of deteriorating functioning. We suggested that the timing of performing coordination was related to the findings about the association between coordination and functioning.
In a previous study, positive associations between higher functioning and services were interpreted as indicating the effectiveness of the services. 10 In this study, some types of services were associated with lower functioning and hospital admission in follow-up assessment, which might mean that these services were associated with deterioration of users. There were no differences in functioning or hospital admissions between baseline and follow-up assessment. In this study, users received ICM services for a long time (over 4 years; see Table 1). The findings indicated that symptoms of mental illness were relatively stable with ICM services. Therefore, we believe that the associations between lower functioning and hospital admission did not reflect deterioration because our sample was relatively stable and the effects of ICM services had already appeared at baseline assessment.
Strengths and Limitation
There were several limitations of this study. Although core services were proposed by a network analysis, 5 there were too many types of services. Thus, our results did not reflect all features of ICM. We used data from only one institution. Hence, the findings were strongly related to the environment of that institution and may not reflect the general features of ICM. The number of users who received hospital-based services and easy contacts was small, which might have distorted the statistical results. Although we suggested that services were determined based on future risks, our findings were the associations of services with functioning and hospital admission at follow-up assessment. Thus, it is possible that services influence functioning and hospital admission at follow-up assessment.
The present study also has some strengths. Typically, it is effortful to record ICM services in detail. Moreover, the implementation of ICM differs among regions 2 and only one previous study 10 examined the association between types of services and future outcomes of users. In addition, we followed up over 90% of the study participants for 2 years and 6 months. Therefore, our study is considered valuable in light of recording ICM services in detail and longitudinal study.
Conclusion
We examined the association of service type in ICM with previous (ie, baseline assessment) and future (ie, follow-up assessment) functioning and hospital admission using longitudinal data. Outreach services were significantly associated with previous and future hospital admissions. Hospital-based services were associated with future lower functioning and future hospital admission. Easy contacts and coordination were also significantly associated with lower functioning at follow-up assessment. In Japan, most mental health services are provided in hospital, and outreach services are relatively time consuming for case managers; therefore, the indications for providing outreach services need to be carefully considered. Our findings showed that case managers may provide flexible services to users according to such Japanese circumstances.
Footnotes
Acknowledgments
This work was supported by Health Labor Sciences Research Grants (19GC2003) from the Ministry of Health, Labour and Welfare of Japan. We would like to extend special thanks to staff of Asahi General Hospital.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
