Abstract
Schwannoma corresponds to a benign neurogenic tumor, derived from neural crest cells. It accounts for approximately 5% of all benign soft tissue tumors. These are the most common cause of peripheral nerve neoplasms of the oral cavity and oropharynx representing 1%. Isolated or solitary neurofibromas of the oral cavity usually involve the tongue or the labial mucosa. They appear as soft, painless, slow-growing masses that are tender to depression or palpation. The case of a 40-year-old woman is studied because of the presence of painless swelling, slow, and progressive growth of the oral language. Complete removal of the lesion was performed and primary closure was performed. It had a satisfactory evolution, maintaining adequate sensory and sensory mobility and innervation.
Introduction
Schwannomas are benign neurogenic tumors, derived from neural crest cells, specifically from cells of the peripheral nerve sheath called Schwann cells.1-3 They represent approximately 5% of all benign soft tissue tumors. These may occur in any peripheral nerve, cranial nerve (with the exception of the olfactory nerve and optic nerve), cutaneous nerves of the head, and neck and flexor surfaces of the extremities. They are the most common cause of peripheral nerve neoplasms of the oral cavity and oropharynx representing 1%. Solitary neurofibromas in the oral cavity rarely become sarcomas; however, 15% of those with Von Recklinghausen disease develop malignancy.
Computed axial tomography and magnetic resonance imaging (MRI) are useful for its detection, with MRI being the study of choice. The ideal treatment is complete trans-oral excision. The trans-oral approach via anterior midline glossotomy seems to be a good option because it is safe, has a low index of vascular and nervous lesion, and has a rapid recovery. When surgery is chosen, there is a relatively low risk of complications and recurrences.
Case Report
This is the case of a 40-year-old woman, with a history of eclampsia during her pregnancy 6 years ago, a benign thyroid nodule, and left benign breast disease. She attends the Otolaryngology and Head and Neck Surgery presenting a painless, slow, and progressive growing tumor of the oral tongue with a discreet margin at the tip of the tongue. She has slurring of words and dysphagia for approximately 1 year. In the physical examination of the oral cavity, a smooth, nonpainful, firm, submucosal mass with regular borders and of approximately 6 cm × 5 cm is felt behind the tip. The mass includes the dorsal and ventral part of the tongue surpassing the lingual V. Mobility of the tongue is preserved. No fasciculations or atrophy of the tongue was observed (see Figure 1). There are no palpable lymph nodes. There are no pathological findings in the chest X-ray. A computed tomography is requested where an encapsulated, well-delimited nodular image is reported at the lingual area (see Figure 2).
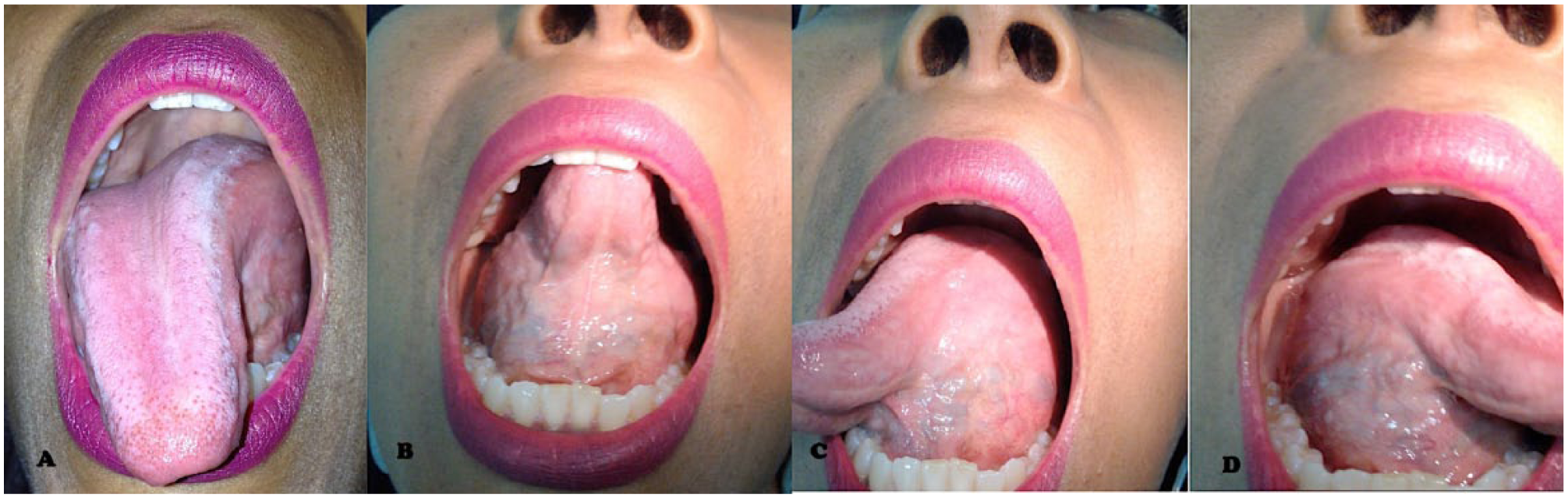
(A-D) Lesion in different positions of the tongue; note that despite the large size of the lesion, lingual mobility is preserved.
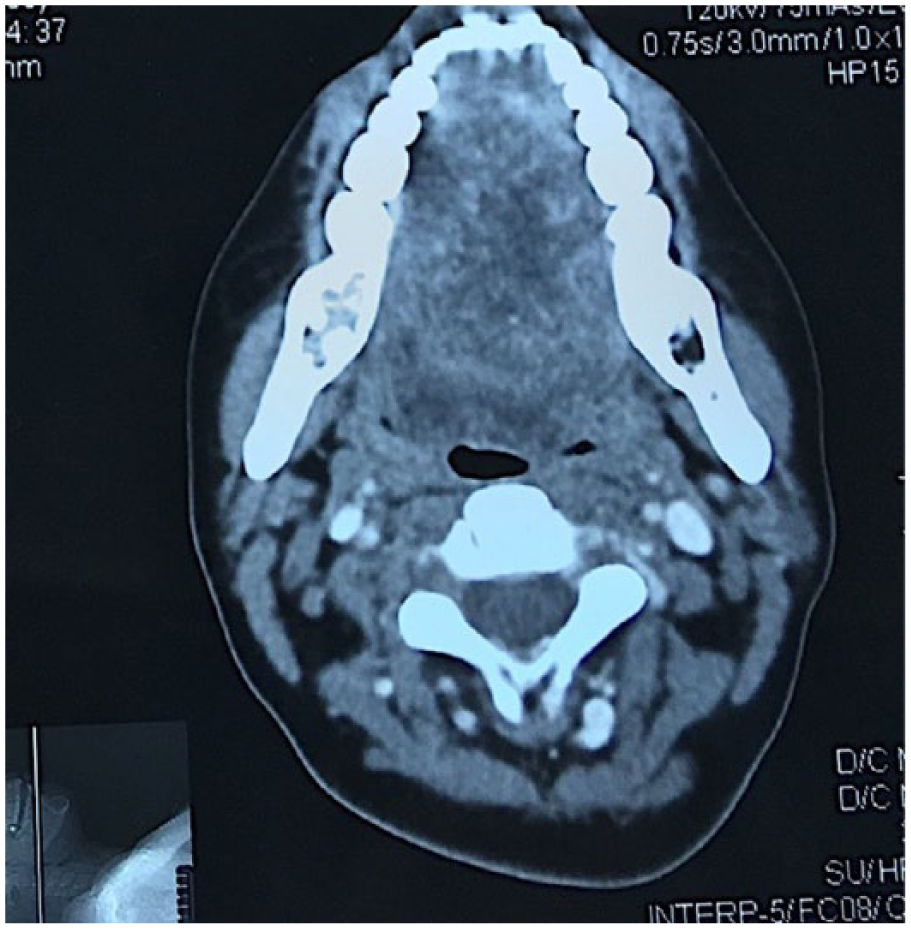
Computed tomographic scan showing well-defined oral and base tongue lesion.
It was decided to perform an anterior midline glossotomy approach with total excision and primary closure. A temporary tracheotomy was performed because of the tumor size, involvement of the base of the tongue, the risk of edema, and/or postoperative bleeding. The tracheotomy tube was withdrawn at 3 days post-op. An approximately 6 cm × 4 cm encapsulated tumor with regular borders and firm consistency was removed. There were no mishaps during or after surgery. On the first day post-op, the patient was put on a liquid diet and was sent home. Histopathologic examination revealed a schwannoma (see Figures 3 and 4).
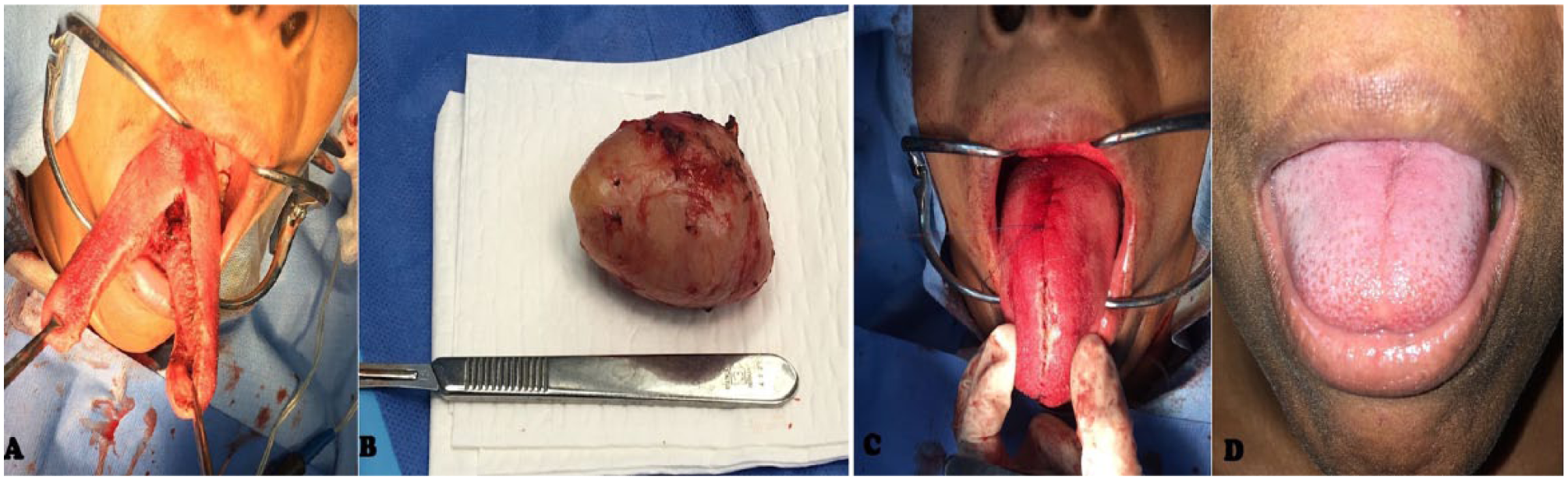
(A) Anterior glossotomy approach, (B) surgical specimen, (C) primary closure after resection, and (D) 6 months postoperative.
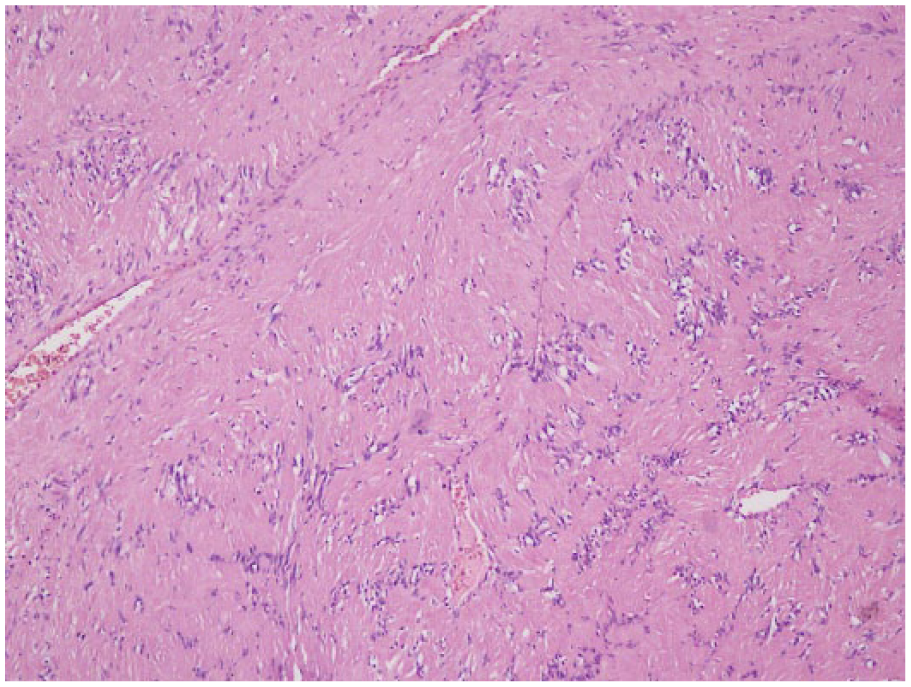
Microscopic image of the schwannoma showing Verocay bodies. 20x, Haematoxylin and eosin stain.
Discussion
Schwannomas are benign neurogenic tumors, derived from neural crest cells, specifically from cells of the peripheral nerve sheath called Schwann cells.1-5 These may occur in any peripheral nerve, cranial nerve (with the exception of the olfactory nerve and optic nerve), cutaneous nerves of the head and neck, and flexor surfaces of the extremities. A predilection of sensory nerves has also been reported. It represents approximately 5% of all benign soft tissue tumors; 25% to 40% located in the head and neck, of which 90% are located at the level of cranial nerve VIII6-9 and only 1% in the oral cavity and oropharynx. 10 Isolated neurofibromas of the oral cavity usually involve the tongue but can also be found in the palate, floor of the mouth, oral mucosa, mandible, and labial mucosa. 11 As they are rare lesions, they are not among the main differential diagnoses of tumors of the oral cavity. It is difficult to determine precisely which nerve gave origin to the lesion, especially if it comes from a small nerve. 8 According to the literature and reported cases, this tumor has no gender preference, and it can appear at any stage of life7,12,13 being more frequent between the second and fourth decades, appearing at the average age of 27 years.
Two types of schwannoma can be seen in the oral cavity. The most common is the submucosal type, which presents itself as well defined, encapsulated, with firm consistency, and cyst-like appearance. The other is the nonencapsulated type, located below the basal layer of the mucous membrane. The histologic characteristics that allow the diagnosis are the presence of a mixture of cell populations called Antoni Type A and Type B cells with Verocay bodies and a hypocellular zone with hyalinized vessels. 14 In the immunohistochemical analysis, most tumor cells react positively to the S-100 protein.14,15
They appear as a painless and slow-growing mass. The most common symptoms are odynophagia and dysphagia. In a minority of the cases, otalgia and sleep apnea can occur. The average size of these tumors is 2 cm. 16 The patient previously commented had a tumor size 3 times more than the average. About 25% of patients may be asymptomatic.
It has been determined that oral cavity schwannomas may be associated with Von Recklinghausen neurofibromatosis, specifically if there are multiple lesions. About 70% of all cases of Von Recklinghausen have schwannomas in the oral cavity. Solitary neurofibromas in the oral cavity rarely become sarcomas. The risk of malignancy varies from 8% to 10% between cases but increases up to 15% in patients diagnosed with Von Recklinghausen neurofibromatosis. 17
As for the diagnosis, a detailed clinical history and a thorough physical evaluation that include palpation of the tongue and evaluation of the motor and sensory functions are paramount. Computed tomography, ultrasonography, and MRI are useful for its detection, allowing us to estimate the size and margins of the tumor, its composition, and whether there is infiltration into the surrounding structures. Of these imaging studies, nuclear magnetic resonance is preferred, showing a well-defined, hyperintense, and homogeneous nodulation in T2 and isointense in T1.12,18
Differential diagnosis should be made with other types of lesions such as lipomas, lingual thyroid, lymphangiomas, hemangiomas, leiomyomas, and benign salivary gland tumors. 18
The ideal standard treatment is complete surgical excision. The trans-oral approach is preferred in 80% of the cases,12,15,18 because those presented in solitary way can be removed with relatively little risk of recurrence, however, in those involving tongue base. The trans-cervical approach was used. In our case, we prefer the anterior medial glossotomy because we consider a safe approach, with few complications and that allows the resection of both the oral part and the base.
Conclusions
Lingual schwannomas are rare tumors whose diagnosis should be suspected when there is a solitary, well-delimited, nonpainful, and slow-growing oral lesion and slurring of words with or without involvement of its base. The trans-oral approach via anterior midline glossotomy seems to be a good option because it is safe, has a low index of vascular and nervous lesion, and has a rapid recovery.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
JD and PC conceived of the presented idea. PC developed the theory and performed the computations. JD verified the analytical methods. JD encouraged SS to investigate the histology findings and supervised the findings of this work. All authors discussed the results and contributed to the final manuscript.
