Abstract
Background:
Early detection of post-COVID-19-related lung fibrosis is very important for the early introduction of treatment and to minimize morbidity and mortality. The aim of this study is the early detection and evaluation of post-COVID-19 fibrosis by high-resolution computed tomography (HRCT).
Methods:
This prospective study included 115 patients irrespective of age and sex, who tested positive for the SARS-CoV-2 by nasopharyngeal swab (RT PCR), admitted to the Dhaka North City Corporation (DNCC) dedicated COVID-19 hospital, Dhaka, and discharged after recovery. Patients went through a chest HRCT scan at least once during their hospital stay and another scan during follow-up after hospital discharge and 8 to 12 weeks of negative RT-PCR report.
Result:
Among 100 patients 23 patients had >50% of total lung involvement by visual assessment. Thirty-three patients had 25% to 50% of total lung volume involvement. Twenty-seven patients had less than 25% of total lung involvement, whereas 17 patients had no visual fibrotic change on the follow-up HRCT scan. A statistical association was found between age, gender, smoking, and severe form of lung fibrosis (P < .05). Patients with mild CT severity score (⩽8) had a very good prognosis. Patients who were admitted to the hospital for more than 15 days were more prone to developing moderate and severe forms of fibrosis. Patients who received at least 2 doses of the COVID-19 vaccine had less severe forms of fibrosis as well as more cases of complete radiological recovery. On the HRCT scan, most of the patients had bilateral, peripheral (68%), and predominant mid & lower lobar parenchymal involvement.
Conclusion:
Early detection and HRCT evaluation of post-COVID-19 related lung fibrosis is very crucial for early management and introduction of anti-fibrotic drugs.
Introduction
Coronavirus disease 2019 (COVID-19) is caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which leads to respiratory manifestations that can range from mild flu-like symptoms such as fever, cough, and fatigue to severe respiratory failure requiring intensive care.1,2 The primary risk factors for severe COVID-19 are advanced age, male gender, and comorbidities such as diabetes and hypertension. 3 Due to the ongoing COVID-19 pandemic, there will be an increased number of patients worldwide who survived the COVID-19 disease but still suffer from post-COVID symptoms, raising the importance of managing these COVID-19 sequelae. 4 Pulmonary fibrosis is a recognized sequelae of acute respiratory distress syndrome (ARDS). Its pathogenesis was previously described previously in the literature involving other coronavirus infections. 5 Briefly, it is a combination of virus-induced lung injury, immune response, and activation of a repair process by fibroproliferation. This repair process can result in the repair of affected lung parenchyma or may lead to pulmonary fibrosis with architectural distortion and irreversible lung changes. 5 Pulmonary fibrotic changes occur in the acute stage of infection as the body fights to repair inflamed areas following pulmonary injury. 6 The incidence of fibrotic pulmonary changes following SARS-CoV-2 infection is likely to be high. So, the global burden of fibrotic pulmonary disease will be increasing significantly. 7 Given the huge number of individuals affected by COVID-19, even a less common complication will have major health effects at the population level. 8 Till now, there is no available treatment for post-COVID-19 pulmonary fibrosis. The use of anti-fibrotic in the early acute phase of severe disease with ARDS may reduce fibrosis. 9
The aim of this study is the early detection and evaluation of post-COVID-19 fibrosis by high-resolution computed tomography (HRCT). In addition, the study aims to predict the radiological and clinical risk factors of COVID-19 patients that can lead to pulmonary fibrosis, so that the patients can be managed by early introduction of anti-fibrotic drugs.
Methods
This study included 115 patients irrespective of age and sex who were tested positive for the SARS-CoV-2 by nasopharyngeal swab (RT PCR), admitted to the DNCC dedicated COVID-19 hospital and discharged after recovery. Researchers adopted a convenience sampling method for this study. Patients went through chest HRCT scan at least once during their hospital stay and another one during follow-up after 8 to 12 weeks of negative RT PCR report. However, 5 patients died, and 10 patients were lost to follow-up. So, the final sample size was 100.
Study period - From 01.06.2021 to 31.05.22 (1year).
Inclusion Criteria
Confirmed COVID-19 cases by nasopharyngeal swab- RT-PCR testing.
Hospitalized patients.
Patients who underwent initial HRCT during hospitalization and follow-up HRCT after 8 to 12 weeks of negative RT-PCR report.
Exclusion Criteria
Pregnant females.
Patients with severe respiratory motion artifacts on HRCT images
Patients with a history of chronic interstitial lung disease
CT Scanning Technique
The scan was done with Philips, Ingenuity, 128-slice CT detector without a contrast agent. The scanning parameters were as follows: tube voltage, 120 kVp; tube current, 150 mA; rotation time, 0.8 second; slice thickness, 5 mm; slice interval, 5 mm; pitch, 1.2; matrix, 512 × 512; and breath-holding when fully aspirated.
Case Definition and Image Interpretation
Images were interpreted by 2 certified radiologists. The severity score was done according to Li et al. 10 The abnormalities that were considered significant for the disease included the following: ground glass opacity, consolidation, nodule, reticulation, interlobular septal thickening, crazy-paving pattern, and bronchial wall thickening. Ground-glass opacity (GGO) is defined as an increase in lung density, but the bronchial vascular bundles are still visible. 11 Consolidation is defined as opacification in which the underlying vasculature was obscured. 12
Each lobe was provided a CT score of 0 to 5, depending on the percentage of the involved lobe: score 0—0% involvement; score 1—less than 5% involvement; score 2—5% to 25% involvement; score 3—26% to 49% involvement; score 4—50% to 75% involvement; score 5—greater than 75% involvement. The overall CT score was the sum of the points from each lobe and ranges from 0 to 25 points. Up to a score of 8 was considered a mild disease, a score of 9 to 14 was considered a moderate disease, and a score of more than 14 was considered a severe disease.
Fibrosis was defined as parenchymal bands, irregular interfaces (bronchovascular, pleural, or mediastinal), coarse reticular pattern, traction bronchiectasis, and honeycombing. 13
Lung involvement was classified as 1. No fibrosis 2. Mild fibrosis- <25% parenchymal involvement 3. Moderate fibrosis- 26% to 50% parenchymal involvement 4. Severe fibrosis- >50% parenchymal involvement by visual assessment.
Definition of Smoker
Current smoker: An adult who has smoked 100 cigarettes in his or her lifetime and who currently smokes cigarettes.
Former smoker: An adult who has smoked at least 100 cigarettes in his or her lifetime but who had quit smoking at the time of the interview. 14
Statistical Analysis
Statistical analyses were carried out by using the Statistical Package for Social Sciences version 23.0 for Windows (SPSS Inc., Chicago, Illinois, USA). A descriptive analysis was performed for all data. The mean values were calculated for continuous variables. The quantitative observations were indicated by frequencies and percentages. A “P” value of <.05 was considered as significant.
Ethical Consideration
The aims and objectives of the study along with its procedure, risks, and benefits were explained to the respondents in an easily understandable local language, and then informed written consent was taken from each. It was assured that all information and records would be kept confidential. Ethical approval was obtained from the IRB board of DNCC COVID-19 dedicated Hospital, Dhaka.
Results
Among the study participants 23 (23%) patients had >50% lung fibrosis on follow-up HRCT whereas 33 (33%) patients had 25% to 50% fibrosis, 27 (27%) had <25% lung fibrosis, and finally 17 (17%) did not have any lung fibrosis on follow-up HRCT scan.
Following patterns of distribution of fibrosis in HRCT were observed—pure ground-glass opacity (9%), consolidation (7%), crazy paving (26%), subpleural bands (67%), subpleural interstitial involvement (not honeycomb) (52%), pneumatoceles (9%), and honeycomb (21%) (Figure 1).
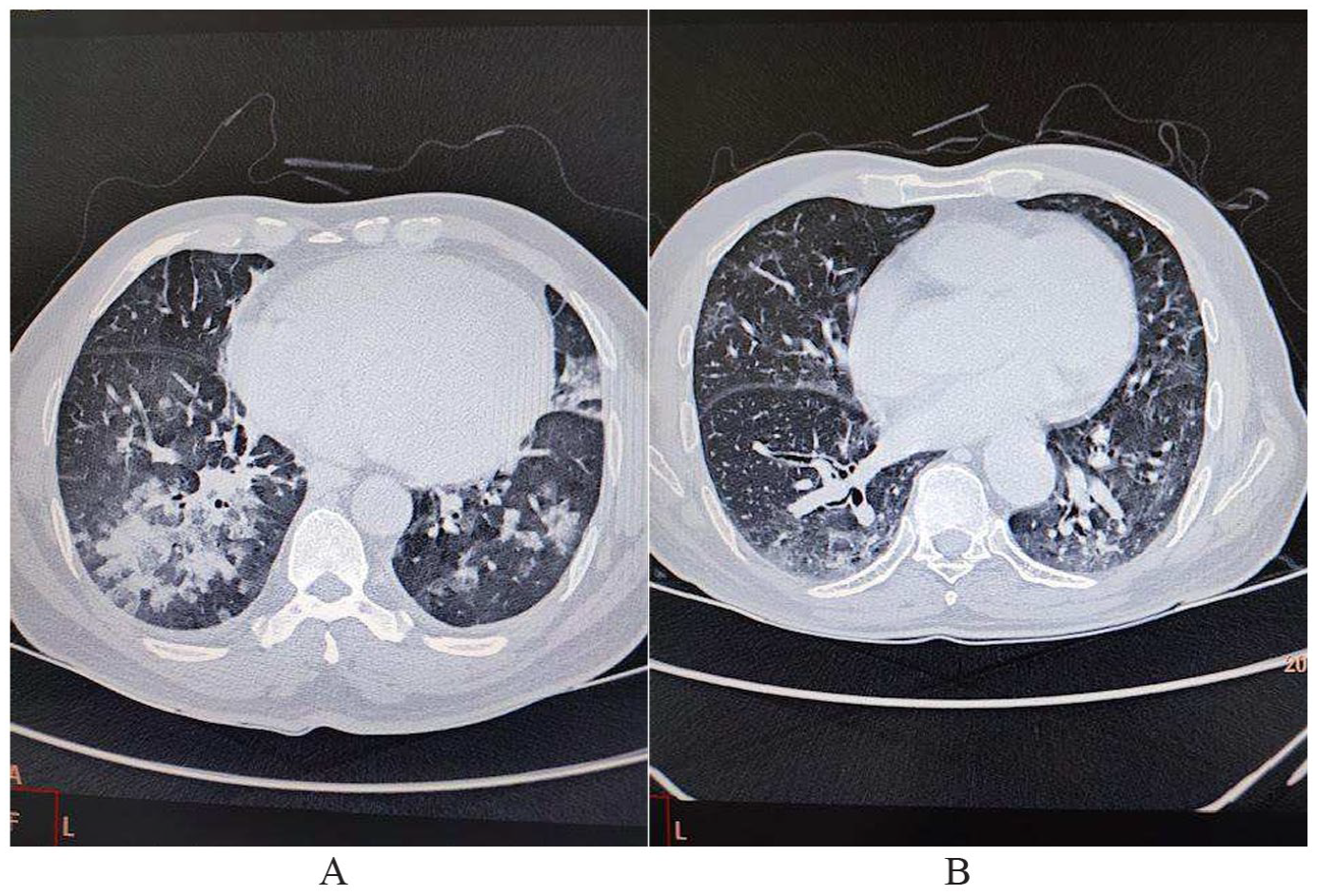
A 49 years old male COVID-19-positive patient presented with fever, cough, and respiratory distress. First HRCT (A) was done on the 11th day of the manifestation of symptoms which shows classic consolidation & mosaic pattern of attenuation in the right lower lobe and ground glass attenuation with scattered consolidations in the left lower lobe & lingular segment of the left upper lobe. Follow-up HRCT (B) was done after 9 weeks, showing regression of consolidation and replacement by ground-glass attenuation, fibrotic bands, and traction bronchiectasis on the right side. In the lingular segment of the left upper lobe, consolidation has completely resolved, whereas in the left lower lobe the initial ground glass attenuation has become coarse. Subtle traction bronchiectasis is also evident in the left lower lobe.
On HRCT 79% of patients were found to have bilateral lung involvement followed by 73% lower lobe, 68% peripheral lung, 48% middle lobe, and 31% upper lobe of lung involvement.
Figure 2 shows a significant association between age and lung fibrosis and parenchymal involvement (P = .0002).
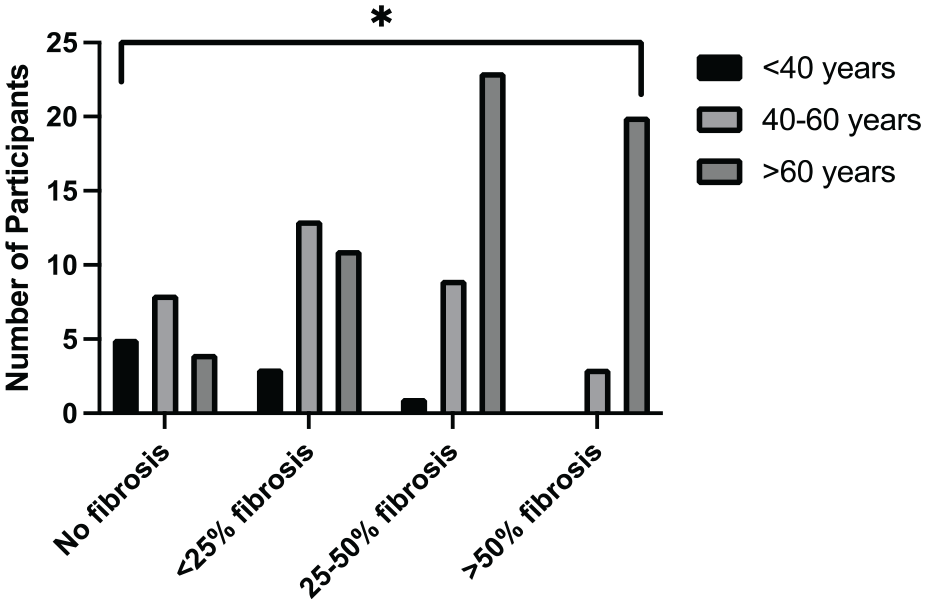
Involvement of lung parenchyma (fibrosis) according to the age of the patients (n = 100).
Figure 3 shows that there is a significant association between gender and lung fibrosis (P = .0004).
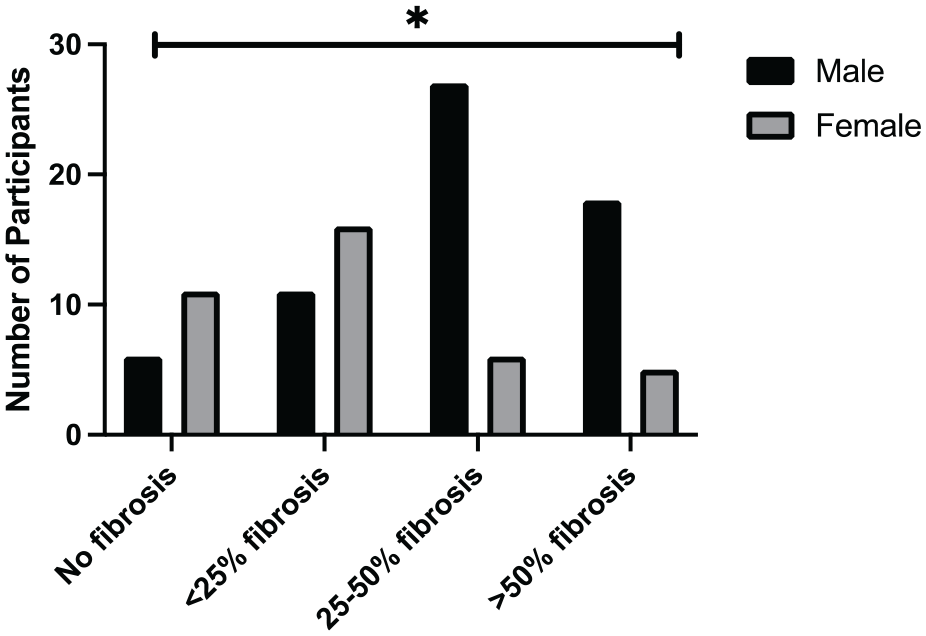
Involvement of lung parenchyma (fibrosis) according to the gender of the patients (n = 100).
Figure 4 shows cigarette smoking had a positive association with lung fibrosis (P = .013).
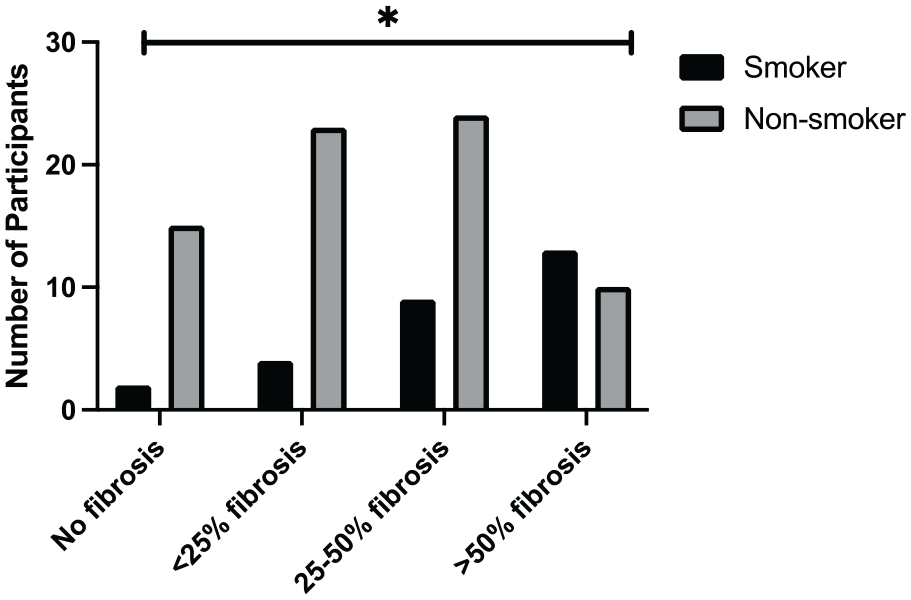
Involvement of lung parenchyma (fibrosis) according to the smoking status of the patients (n = 100).
Figure 5 shows the percentage of patients with moderate and severe CT severity scores had more frequency of development of pulmonary fibrosis even though the association was statistically insignificant (P > .05).
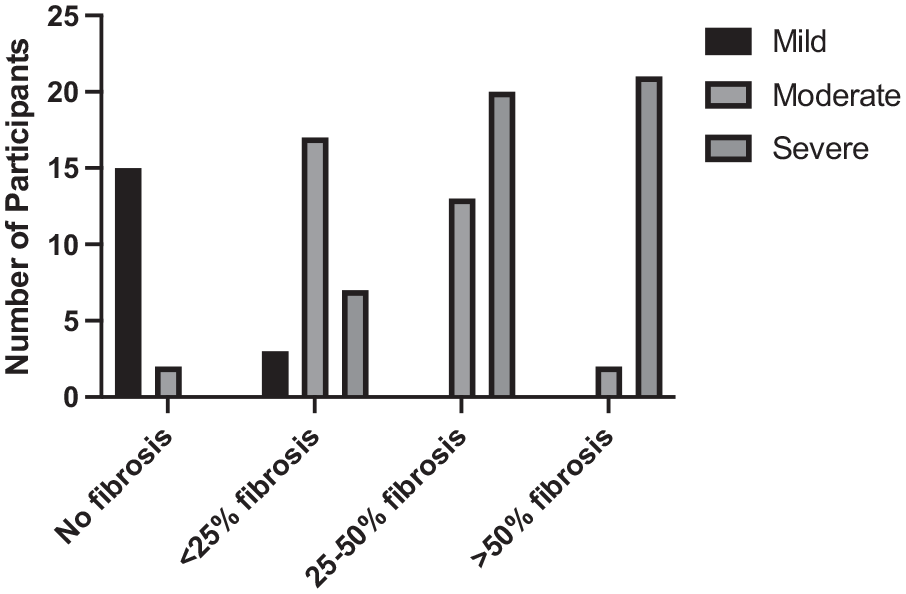
Involvement of lung parenchyma (fibrosis) according to CT severity score on previous HRCT (n = 100).
Figure 6 shows that the percentage of patients who had to stay more than 15 days in the hospital had a more severe form of pulmonary fibrosis, but the association was statistically insignificant (P > .05).
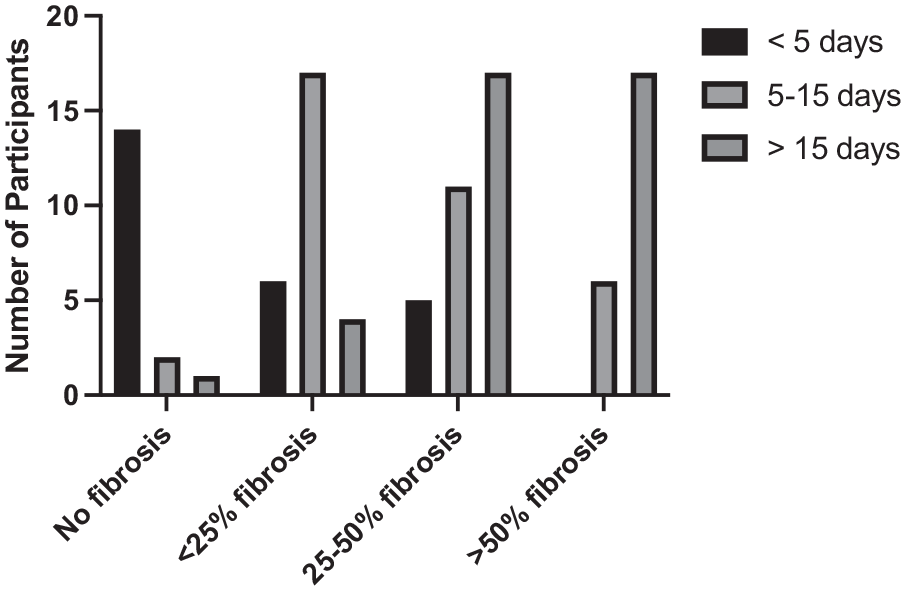
Involvement of lung parenchyma (fibrosis) on HRCT according to hospital stay of the patients (n = 100).
Figure 7 shows that patient vaccination status had no statistical association with the subsequent development of lung fibrosis (P > .05).
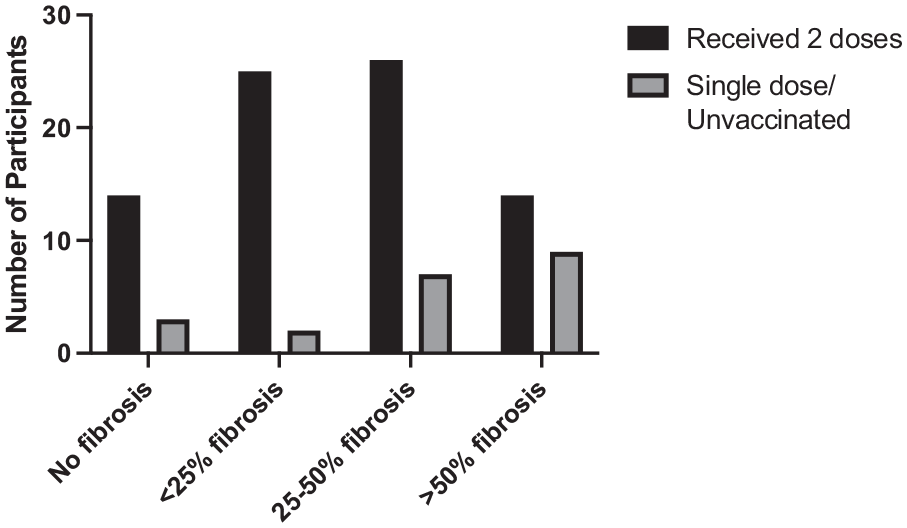
Involvement of lung parenchyma (fibrosis) on HRCT according to the vaccination status (n = 100).
Discussion
More than 50% of the patients (n = 58) were more than 60 years old in our study (Figure 2). Among them, 34.5% (n = 20) of patients had more than 50% of lung involvement. 39.7% (n = 23) patients had 25% to 50% of lung involvement and 19% (n = 11) patients had less than 25% of lung involvement (Figure 2). Whereas, among 58 patients only 6.9% (n = 4) patients had total recovery (no fibrosis) (Figure 2). This data correlates with other studies conducted elsewhere, where researchers found that older patients are more prone to developing fibrosis.15,16 This is largely because older people have underlying medical conditions and weakened immune systems that act as catalysts for severe COVID-19 disease.15,16
We found that patients below 40 years of age had no severe case of fibrosis and out of 9 patients 5 (55.6%) had complete radiological recovery. We also noted that maximum patients of the 40 to 60 year age group had mild (13 out of 33) and moderate (9 out of 33) lung involvement and a significant number of patients (n = 8) recovered completely from COVID-19 pneumonia. This is in line with findings from other studies and anecdotal evidence where young people were found to be less susceptible to COVID-19 complications.15,16
Among 62 male patients 29% (n = 18) patients had severe (more than 50%) parenchymal fibrotic change in contrast to female patients who had only 13.2% (5 out of 38) of severe form of fibrosis. We observed that a significant number of female patients had mild form (less than 25%) of fibrosis (16 out of 38) and complete radiological recovery (11 out of 38) in comparison to male patients (11 and 6 respectively out of 62 patients). Twenty-seven male patients out of 62 had 25% to 50% parenchymal fibrotic(moderate) changes which are significantly higher than female patients (6 out of 38). This may be due to the androgenic effect which promotes the transcription of transmembrane protease, the serine 2 gene that encoded protein primes the spike protein of SARS-Cov-2. This impairs antibody response and facilitates the interaction of the virus and host cells. 17
In our study, about 46% (13 out of 28) of smokers developed a severe form of fibrosis which is significantly higher than nonsmoker patients (about 13%). We also observed that a significant percentage of nonsmoker patients had complete recovery (20.8%) and mild form of parenchymal fibrosis (31.9%) in comparison to smokers (7.1% and 14.3% respectively). Other researchers also found similar types of data in their studies, where the odds of developing fibrosis were higher among smokers compared to non-smokers.15,18
CT severity score is an important factor for the prediction of post-COVID-19 pneumonia-related lung fibrosis. In this study, we found that patients with mild CT severity score (⩽8) had very good prognoses as 83% (15 out of 18) patients showed no sign of fibrosis in follow-up HRCT scans. However, 3 out of 18 patients had a mild form of fibrosis. We noted that a significant number of patients with severe CT severity scores (⩾15) developed moderate (20 out of 48) and severe (21 out of 48) forms of fibrosis in follow-up scans and none had complete recovery. Most of the patients with CT severity scores of 9 to 14 developed mild (50%) and moderate (38%) forms of fibrosis. Our data is supported by other studies where it was shown that CT severity score is correlated to COVID-19 outcome and long-term complications.15,19
In this study, we found that number of days of hospital stay of the patients is directly proportional to the severity of fibrosis. Patients who were admitted to the hospital for more than 15 days were more prone to developing moderate (17 out of 39) and severe (17 out of 39) forms of fibrosis. On the other hand, 56% (n = 14) patients had a complete radiological recovery, and 24% (n = 6) patients had a mild form of fibrosis and had less than 5 days of hospital stay. Whereas the patients who were admitted for 5 to 15 days into the hospital had mostly mild (47.2%) and moderate (30.6%) forms of fibrosis.
In their study, Rahman et al 20 showed that vaccination can significantly reduce the severity of COVID-19 pneumonia both radiologically and clinically. In our study, we observed that patients who received at least 2 doses of the COVID-19 vaccine had less severe forms of fibrosis as well as more cases of complete radiological recovery. Out of 79 patients 14 (17.7%) patients had no sign of fibrosis in the follow-up scan. However, this data is not statistically significant as 14.2% of patients had also complete radiological recovery among 21 non-vaccinated/single-dose vaccinated patients. However, the percentage of severe forms of fibrosis is about twice as in non-vaccinated/single dose vaccinated patients (42.8%) than in completely vaccinated patients (17.7%). We also noted that a significant percentage (31.6%) of completely vaccinated patients had a milder form of fibrosis than the other group (9.5%).
There are several limitations to this study. First, the sample numbers were low compared to the number of positive cases diagnosed. This is because many patients were lost to follow-up and the researchers did not have the resources to contact all the patients after discharge from the hospital. Next, the evaluation of COVID-19 fibrosis is dependent on physicians’ judgment. Hence, there is the risk of bias there even though the researchers tried to mitigate this issue by involving several physicians at each step of evaluation.
Conclusion
Post-COVID pulmonary fibrosis is the major and most important pulmonary complication of post-COVID-19 pneumonia as it causes permanent and untreatable lung destruction. This study evaluated the prevalence of COVID-19 fibrosis among hospital-discharged patients and identified several risk factors for COVID-19 fibrosis. Many of these cases could be prevented by taking care of the risk factors identified in this study. Hence, the findings of this study could be used as a starting guide for policymakers in Bangladesh and lessen the burden on already strained healthcare resources in the country.
Footnotes
Acknowledgements
The authors would like to pay tribute to all the participants who agreed to participate in this study.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Conceptualization: M.T.R; N.U.N; N.A, M.I. Methodology: M.T.R; B.B; M.S; M.M.R.K. Data collection and analysis: M.T.R; N.U.N; N.A; M.I; I.I. Writing first draft: M.T.R; N.U.N; N.A.; M.I. Writing- editing and revision: M.T.R; M.M.A.M. Supervision: B.B; M.S; M.M.R.K; M.M.A.M.
Data Availability Statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
