Abstract
Antimicrobial resistance (AMR) is increasing and it is a serious public health problem worldwide. Nepal is considered as one of the contributors for rising AMR due to the most prevalent irrational use of antibiotics. In this review, we have assessed the practices of antibiotic prescription and dispensing, and antibiotic resistance of commonly encountered bacteria in Nepal. There is exponential increase of therapeutic consumption of antibiotics either without clinician’s prescription or irrational prescription. Almost half of the population in Nepal was found to purchase antibiotics easily from the nearby pharmacies without clinician’s prescription. Irrational prescription is exceeded in remote areas which could be due to lack of access with health posts and hospitals. The third generation cephalosporins, which are considered as the last resort antibiotics were found to be relatively prescribed and dispensed higher as compared to other classes of antibiotics. Despite the existing limited functional surveillance system, antibiotic resistance among bacteria is increasing in Nepal because of irrational prescription, dispensing and consumption of antibiotics without prescription.
Background
The discovery of antimicrobial agents has significantly contributed to controlling infectious diseases by reducing morbidity and mortality among humans and animals. 1 Indiscriminate, inappropriate and inadequate uses of antibiotics are the major reasons for antimicrobial resistance in the world.2-4 The emerging resistance to antimicrobials in South Asia is intertwined with epidemiological, social, cultural and political characteristics of the nations because neither public, private hospitals and health facilities nor antibiotic dispensers are practicing the guidelines properly. In Nepal, National Action Plan on AMR has not been endorsed yet.5-7 Patients use medicines without prescription from medical practitioners. Antibiotic prescription for common infections such as respiratory tract infections, urinary tract infections and typhoid fever by less qualified and unqualified health professionals is more frequent. In developing countries where more than 50% antimicrobials are used without a medical prescription, are most commonly purchased from pharmacies. 5 In developing countries, higher incidence of infectious diseases, inappropriate use of antibiotics in treatments and as growth promoters in animal feed are the contributing factors for antimicrobial resistance.3,8-10
Approximately half of the medicines are prescribed, dispensed or sold inappropriately. Antibiotic prescription practice depends on health professional’s ability to determine the choices of most benefits to the patients. Studies on prescribing patterns are a part of medical audit that help to monitor, evaluate and suggest modification in prescribing practices. 11 Dispensing antibiotics without prescription remain common practice in Nepal and this inappropriate dispensing contribute to antimicrobial resistance. 12 Most commonly dispensed antibiotics in Nepal are cefixime, cefepodoxime, amoxicillin, azithromycin, ciprofloxacin, ofloxacin, cotrimoxazole, and metronidazole. 12 Antimicrobial resistance is a global health issue for both humans and animals. In current time, dominating pathogens such as Escherichia coli, Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumanii, Pseudomonas aeruginosa, Enterobacter spp, Salmonella spp, Pasteurella spp, etc are resisting the action of antibiotics, which has changed pathogenesis and transmission phenomenon in pathogens.13-15 The lack of discovery of new effective antibiotics since last 39 years is further worsening the situation.1,8,16
Nowadays, most of the antibiotics intended to cure people are becoming less effective due to the development of partial or full resistance by bacteria. The studies from Nepal revealed that antibiotics used against bacteria in diseases of infected patients were effective in curing only around 50% of cases whereas the other 50% showed no response.17-19 In some infections, the effectiveness is even less than 50%. For example, amoxicillin, ciprofloxacin and norfloxacin used against E. coli were effective only in less than 40% of the infected people, and effective only in less than 20% in pneumonia caused by Klebsiella spp.20,21 The improper implementation of guidelines to AMR, inappropriate use of antibiotics in treatment, and use of antibiotics as a growth promoter can lead to antimicrobial resistance.22-24 Generation of evidences about antibiotic use and its resistance is one of the top 5 priorities of the Global Action Plan on Antimicrobial Resistance by the World Health Organization (WHO). In this review, we have aimed to explore the data regarding antibiotics prescriptions, dispensing and consumptions in Nepal. Further, we have presented the antibiotic resistance pattern of most common bacteria E. coli and S. aureus most often isolated from clinical specimens. This would help to understand the status of antibiotic prescription, dispensing, consumptions, and resistance in bacteria in Nepal. We collected data from PubMed, scopus, and google scholar using different search terms “antibiotic consumption,” “antibiotic dispensing,” “antibiotic resistant bacterial pathogens” and “Nepal.” The published articles related to objectives of review were selected and assessed independently by authors. From the selected articles, data were extracted in the Excel sheet. In this narrative review, we have provided all relevant data in the tables of the manuscript.
Antibiotics Prescriptions Practices
Antibiotics are one of the mostly prescribed among all drugs and frequently used to treat infections.25-27 Prescribing drugs is done by the physicians at the hospital level and non-physicians (paramedics such as health assistants) at the primary health care level in Nepal.23,28,29 Since the qualifications, training and authorities for prescribing drugs is different among these prescribers, their prescribing practices need to be regularly monitored. 30 In Nepal, antibiotic prescription is regulated by various acts and regulations including Drug Act 1978; however, it has not been found followed by most of the practitioners. 30 This regulatory framework had defined antibiotics as the drug requiring prescription for dispensing. Similarly, a clear guideline has been developed by Nepal Pharmacy Council regarding dispensing of prescribed drugs by registered pharmacists. 31 However, in real practice drug dispensers rarely comply with good pharmacy practice and it is highly unregulated as well.31-34 Various factors influencing the inappropriate prescriptions of antibiotics have been described below:
Unavailability of prescribers
The doctor to population ratio is only 0.17/1000 in Nepal, which is below the WHO recommendation that is, 2.3 per 1000 population. 35 Also, there is higher inequality in distribution of trained human resources between urban and rural areas. So, the people in remote areas of Nepal are compelled to rely on paramedics (health assistants and pharmacists) as a primary source of allopathic health care at the primary health care level. 36 This is an alarming issue since huge proportion of population from the rural area are not having access to quality health care services from the qualified health personnel. Due to the lack of antibiotic treatment guideline, these health workers at the primary care level prescribe antibiotics irrationally. A study conducted in rural areas shows that antibiotic prescribing rate in health care center was 50.4% and health post was 52.2%. 23 The most frequently prescribed antibiotics are second and third generation cephalosporins. These high rate of antibiotic prescription without antimicrobial susceptibility test seems contrary to treatment guideline. 23 A study published in 2020 revealed that increasing trend in consumption of antibiotics from 2006 to 2016 in rural areas including increased antibiotic consumption from 26.6% to 50.3% for the treatment of acute respiratory infections, 20.4% to 32% for fever and 7.7% to 30% for diarrhea. 3 The higher prevalence of multidrug-resistant bacterial strains is not only in the areas close to health centers and hospitals but also have been reported in remote area, which was due to the lack of access with health posts and hospitals and irrational use of antibiotics for the treatment of infections.37,38 This may be due to the knowledge gap and misperception of prescription of the health workers. A positive association between antibiotic prescription and resistance pattern has also been reported.39,40
Irrational prescription practices
Broad spectrum antibiotics are prescribed even when equally effective narrow spectrum antibiotics are available. 26 A hospital based study conducted in Western Nepal shows that second generation cephalosporin was prescribed rather than other narrow spectrum antibiotics. Similarly, studies conducted from 2011 to 2020 revealed that cephalosporin seems to be highly prescribed even the other narrow spectrum antibiotics macrolides and ß-lactams are effective.15,41,42 This signifies a wrong prescription practices by the clinicians and the health workers. Nearly one-third of the prescriptions are inappropriate in a study conducted in Lumbini Medical College, mid-western Nepal. 43 Significantly higher proportions of multidrug resistant bacterial strains have been reported close to health care centers and hospitals due to intense exposure to antibiotics.37,38,44 The study conducted in 1998 showed that 68% and 70% of prescriptions for respiratory infections were treated with antimicrobials and about 97% of medicines distributed for symptoms such as diarrhea were antimicrobials, which may not be necessary in most of the cases. 37 However, study conducted in Nepal between 2006, Nepal between 2016 among children under 5 years of age shows decline in disease prevalence but increase in irrational use of antibiotics. 45 Study conducted in 2020 revealed that antibiotic consumption rate increased from 24% in 2006 to 40% in 2016 for acute respiratory infections, 25% to 35% in fever and 8.2% to 26.2% in diarrhea cases. 45 Therefore, irrational use of antimicrobials is one of the important factors attributing to the development of antimicrobial resistance.37,46
Self-medication
Self-medication (SM) is the practice of consuming medication without the consultation of physicians.24,47,48 It is considered to be associated with inappropriate selection of drugs, their dose and duration of treatment which could lead to prolonged duration of illness favoring the development of resistance.3,49 In Southeast Asia, antimicrobials namely ß-lactams, macrolides, fluoroquinolones, cephalosporins and metronidazole were reported to be highly consumed without prescriptions.42,49,50 Self-medication is an alarming problem in Nepal as 67% to 97% community pharmacies dispense antibiotics without prescriptions.8,36,51 Self-medication could be an important cause of developing resistance by bacteria since the patients lack knowledge about the proper use of antibiotics.
The 20 year trends of antibiotic prescriptions showed that antibiotics belonging to cephalosporin (ceftriaxone) class were the most commonly prescribed antibiotics followed by penicillin (ampicillin) and fluoroquinolones (Table 1). These antibiotics have been prescribed for more than 50% of cases which signifies the over prescriptions of third generation antibiotics despite the availability of other effective antibiotics.
Year wise comparison of commonly prescribed antibiotics (2003-2020).
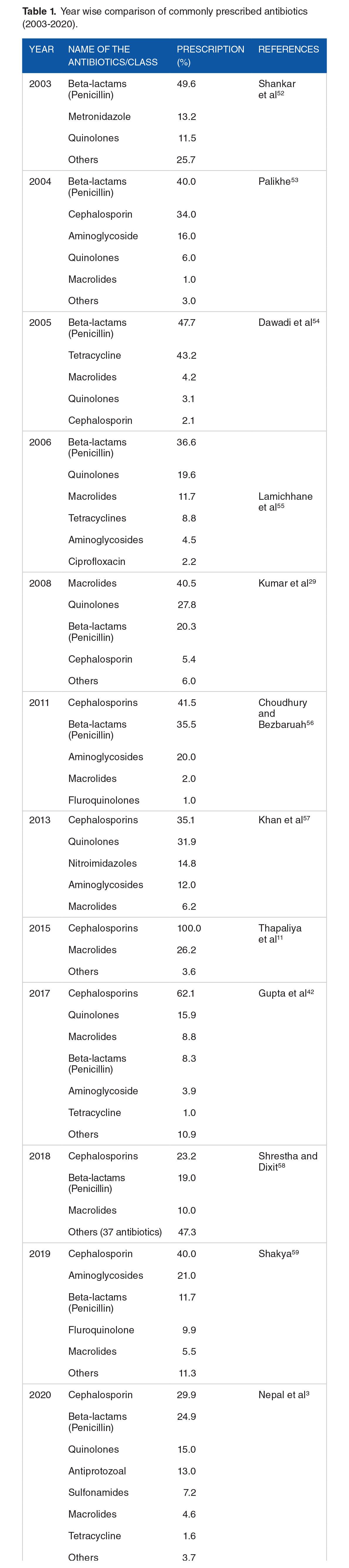
No data is available for the missing years.
Antibiotics Dispensing Practices
Inappropriate use of medicines is a serious global problem leading to increased number of hospitalizations, duration of hospital stay, healthcare costs and mortality rates.4,23,24,46 Dispensing antibiotics without prescription have became common practices especially in low income countries.10,36,60 The over-the-counter dispensing of antibiotics by minimally qualified or unqualified health professionals is a common practice in developing countries like Nepal where 50% of antimicrobials are used without prescriptions and mostly purchased from pharmacies or drug shops. 5 The dispensing of antibiotics without prescriptions is considered as one of the contributors for rise in AMR in Nepal et al.36,61,62
Before 2013, we did not find any data on antibiotic dispensing practices conducted in Nepal. Beta-lactams (Penicillin) was highly dispensed in 2013 but cephalosporins were most commonly dispensed during 2016 to 2020 and macrolides in 2021 (Table 2). The dispensing pattern of antibiotics revealed that cephalosporins are the most frequently dispensed antibiotics, followed by beta-lactams (Penicillin), macrolides, fluoroquinolones, and sulfonamides (Table 2).
Year wise comparison of commonly dispensed antibiotics (2013-2021).
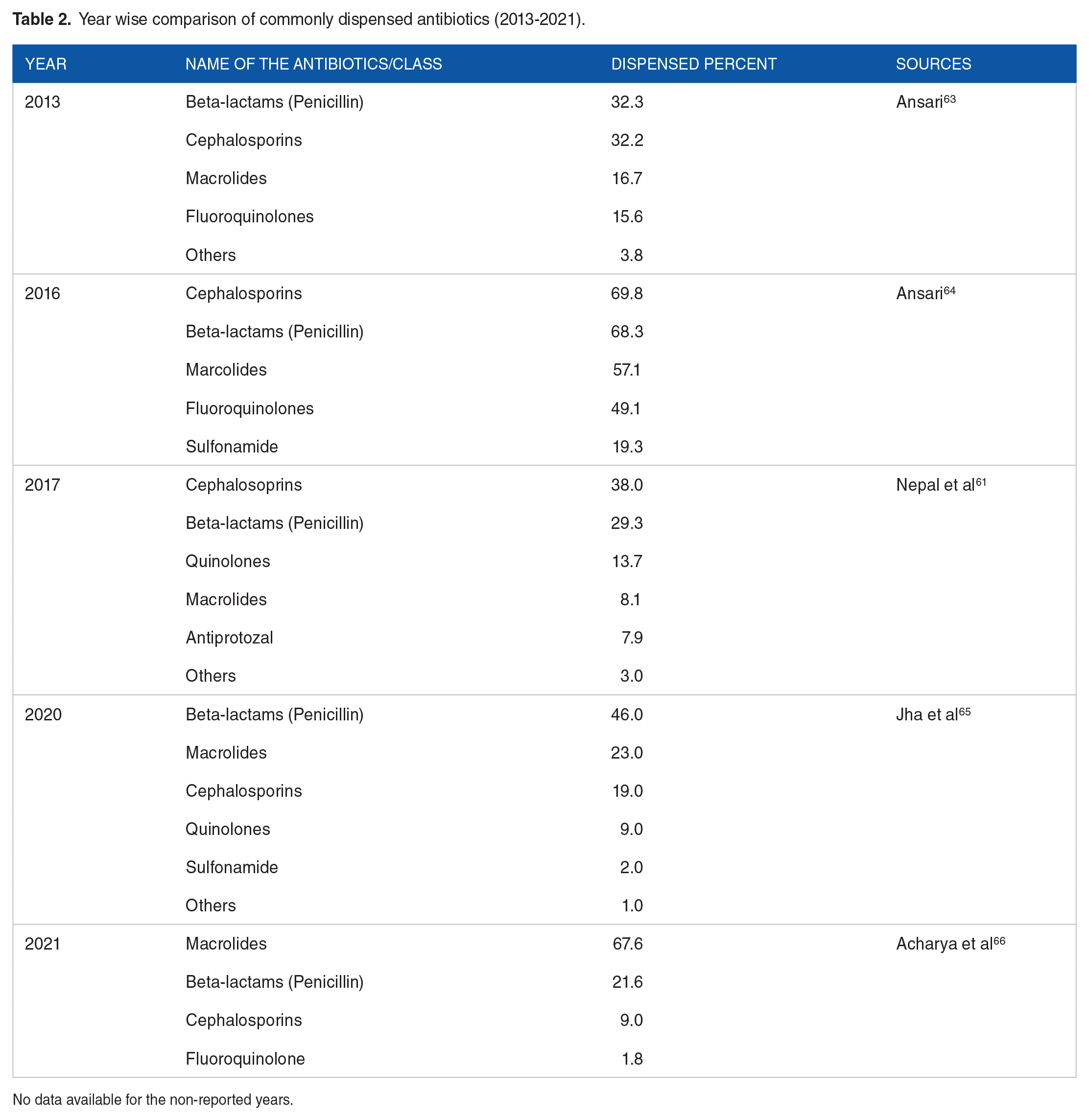
No data available for the non-reported years.
Resistance Pattern
The use of antibiotic has increased since the discovery of penicillin (1943).1,67 In 1950, tetracycline was discovered but just in 9-year difference, tetracycline resistant Shigella was reported. 1 In 1960, methicillin antibiotic was identified but after 2-year methicillin resistant S. aureus was detected. Later on penicillin resistant pneumococcus, vancomycin resistant enterococcus, levofloxacin resistant pneumococcus, and cephalosporin resistant organisms were identified and reported exponential increase in their rates. 68
The hospital based studies showed that common resistant pathogens are E. coli, Vibrio cholerae, S. aureus, Neisseria gonorrhoeae, Salmonella spp., Klebsiella pneumoniae, Streptococcus pneumoniae, Shigella spp., Pseudomonas, and Acinetobacter spp. (Supplemental Table 1). Similarly, National Public Health Laboratory (NPHL) reported E. coli (especially for urinary tract infections) with resistance rate higher than 50% for the entire antibiotics tested. 69 Resistance has been increased significantly from 2006 to 2010. Resistant S. aureus, Klebsiella pneumoniae, Pseudomonas spp., Acinetobacter spp. range from 50% to 100% for different antibiotics.21,68,70,71 The common antibiotics which are resistant by pathogens were reported as ampicillin, cefotaxime, ceftriaxone, imipenem, ceftazidime and piperacillin-tazobactam (Supplemental Table 1).
In the year 2003, high proportion of E. coli isolates were resistant to amoxicillin followed by ampicillin; however, from the years 2011 to 2014, high proportion of E. coli were resistant to second and third generation cephalosporins followed by ampicillin. It has been reported that in 2015, 2016, all ESBL, XDR, and MDR E. coli were resistant to third generation cephalosporins, ciprofloxacin, and ampicillin (Table 3). High proportions of MRSA have been frequently reported as resistant to cotrimoxazole, chloramphenicol, and erythromycin72-74
Antibiotic resistance pattern of E. coli (2003-2019).
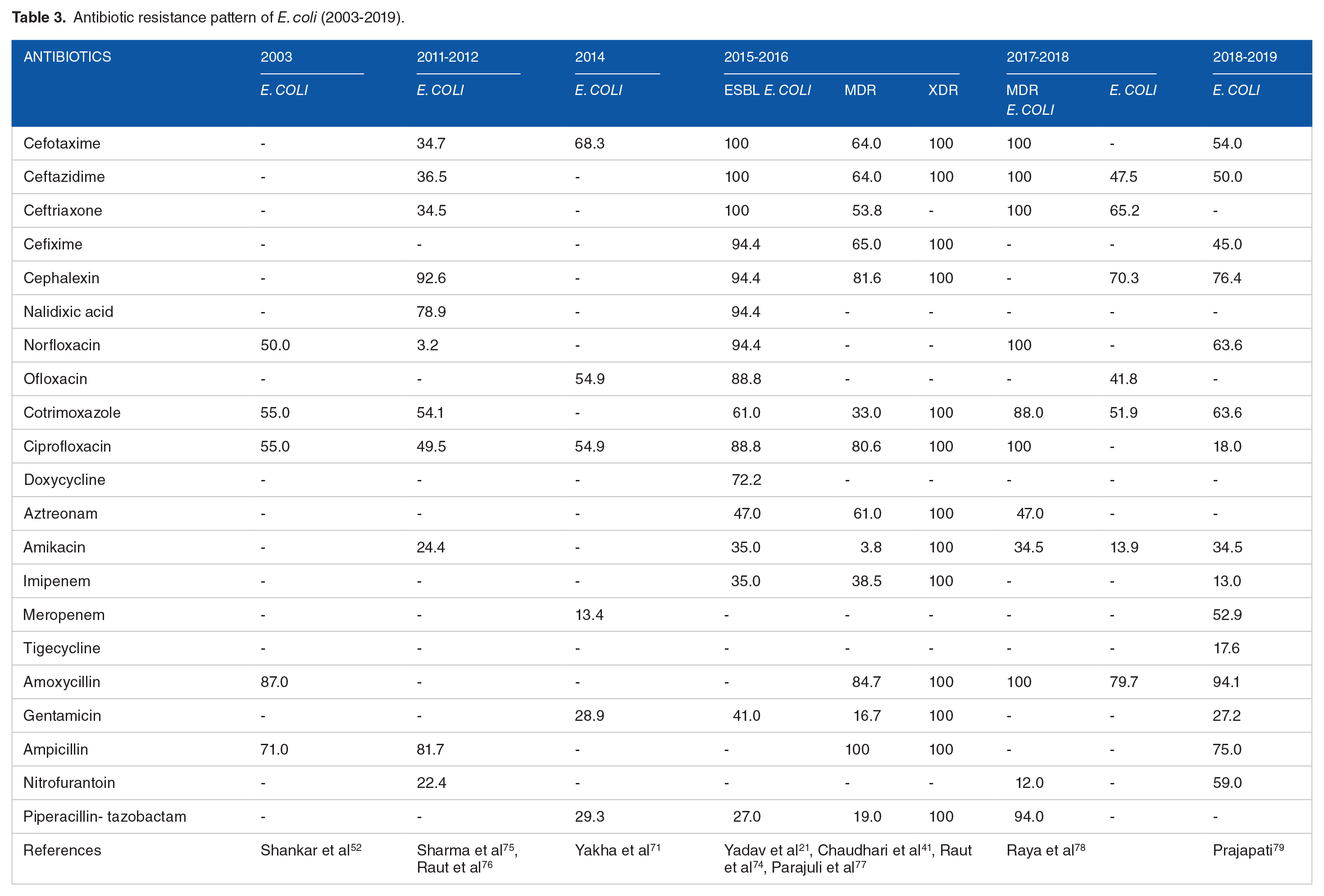
During the years 2003 to 2010, 100% S. aureus were resistant to penicillin and cotrimoxazole followed by amoxicillin. From the year 2005 to 2019, all MRSA, MDR MRSA were resistant to penicillin followed by ampicillin, amikacin, tetracycline and ciprofloxacin (Table 4). Penicillin has been prescribed in high percentage even the resistance pattern of penicillin is high which is due to the gap in knowledge and misperception of prescription practice among the prescribers. Many studies have shown that there is a positive association between antibiotic prescription and resistance pattern of bacteria.39,40
Antibiotic resistance pattern of S. aureus (2003-2019).
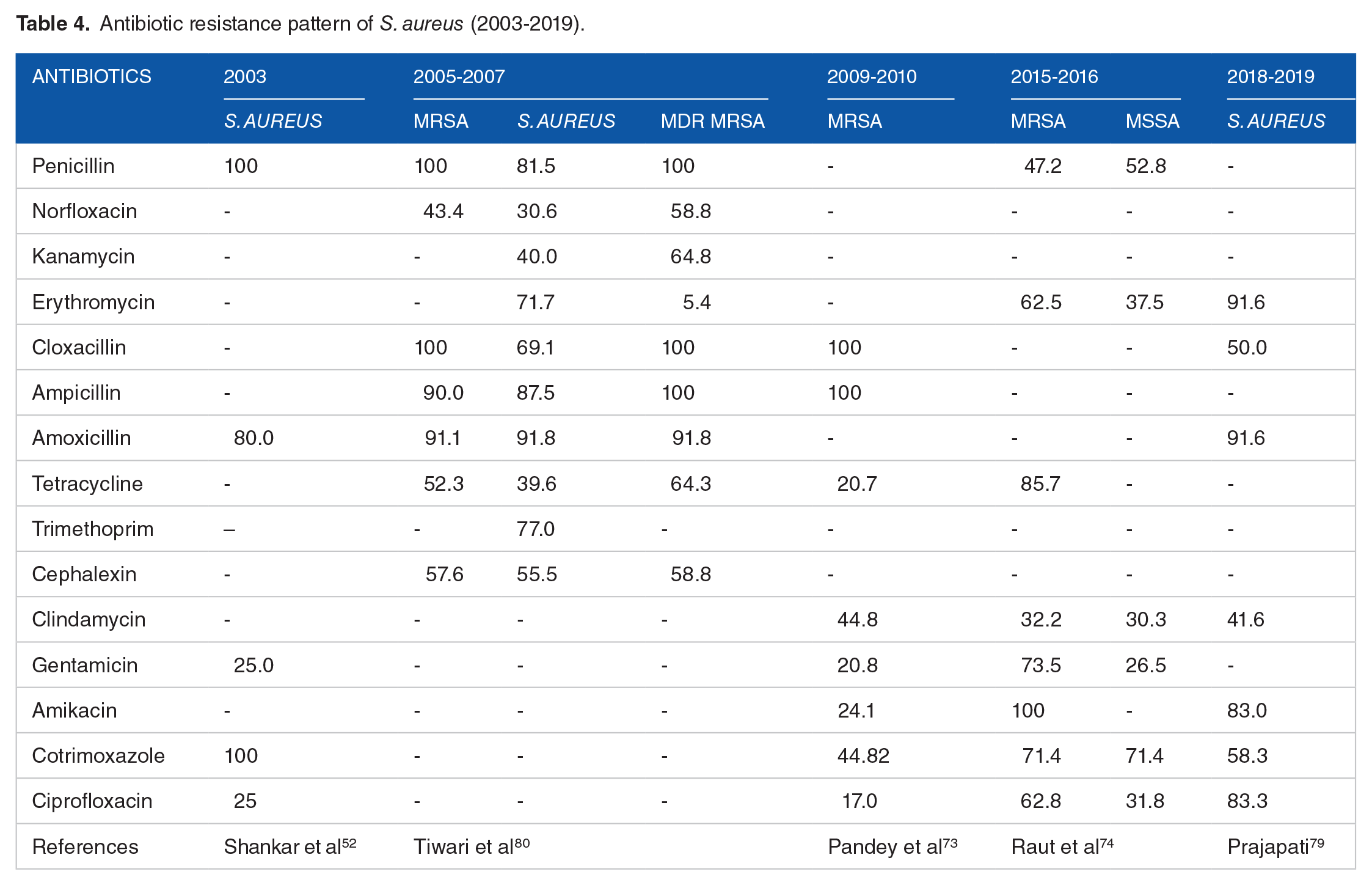
Conclusion
The antibiotic resistance of bacteria in Nepal could be attributed to inappropriate prescription of antibiotics, unavailability of clinicians in remote areas, high proportion of people practicing self-medication, not following the treatment guideline, and the lack of national action plan on AMR. Therefore, to prevent antibiotic resistance the antimicrobial therapy needs to start with first choice and should prescribe the antibiotics after culture and susceptibility test. Unnecessary antibiotic prescriptions, dispensing, and consumptions should be discouraged through raising awareness and implementing regulations. Since the country has limited surveillance on AMR, antibiotic dispensing, and prescriptions in Nepal, nationwide surveillance would support to design proper strategies to contain antimicrobial resistance.
Supplemental Material
sj-doc-1-mbi-10.1177_11786361231167239 – Supplemental material for Antibiotics Prescription, Dispensing Practices and Antibiotic Resistance Pattern in Common Pathogens in Nepal: A Narrative Review
Supplemental material, sj-doc-1-mbi-10.1177_11786361231167239 for Antibiotics Prescription, Dispensing Practices and Antibiotic Resistance Pattern in Common Pathogens in Nepal: A Narrative Review by Kalpana Ghimire, Megha Raj Banjara, Bishnu Prasad Marasini, Pradip Gyanwali, Sudha Poudel, Elina Khatri and Meghnath Dhimal in Microbiology Insights
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Authors Contributions
KG, BPM, and MRB designed the study; KG collected the published paper. MRB and BM supervised the study. KG, SP, and EK analyzed the data; KG, MRB, and EK wrote the original draft. BPM, PG, MD, and MRB reviewed the draft and finalized. All authors read and approved the final review.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
