Abstract
Background:
HIV viral load suppression (VLS) is the most important indicator of successful antiretroviral therapy. In 2016, Bulambuli District started monitoring HIV patients on ART using viral load tests in an effort to meet the third 90 of the UNAIDS 90-90-90 strategy which is VLS. The objective of this study was to determine the progress in Bulambuli District towards achievement of VLS among HIV infected patients on ART and associated factors that affect this programme.
Methods:
A retrospective cohort study design was used. One thousand, one hundred and one medical records of HIV infected patients on ART who attended HIV clinic at Muyembe Health Centre IV from June 2016 to April 2018 were reviewed. A data abstraction tool was used for data collection. Chi Square was used to determine factors associated with VLS and logistic regression was used to determine the magnitude by which the ART and clinical factors influence VLS. Data were summarized using descriptive statistics for categorical variables and by computing proportions, means and standard deviation for continuous variables.
Results:
Of the patients (n = 944, 85.7%) had attained VLS. Adjusting for known confounders, only adherence to ART was a significant predictor of VLS. Individuals with fair adherence (80%-95%) had 2.667 times the odds of VLS, CI = 1.122-9.370, P-value of <.002 compared to individuals with good (>95%) adherence which was used as the reference while those with poor (<80%) adherence had 4.553 times the odds of attaining VLS, CI = 1.31-13.930, P-value of <.001 compared to individuals with good adherence.
Conclusion:
These findings suggest that Bulambuli District, at 85.7% VLS is on track to attaining the third 90 of the 90, 90, 90 global targets by 2020. It further reveals that adherence is the only significant predictor of VLS in the District.
Keywords
Background
HIV/AIDS is the world’s fifth greatest health challenge according to the Global Burden of Disease Study. 1 According to UNAIDS (2017) there were approximately 36.7 million people worldwide living with HIV/AIDS at the end of 2016. 2 By 2011, Sub-Saharan Africa alone accounted for an estimated 69% of all people living with HIV and 70% of all AIDS deaths in the world. 3 Roosblad reported that by 2014, Uganda had the third-highest number of new HIV infections in Sub-Saharan Africa, behind South Africa and Nigeria. 4 Uganda AIDS Commission estimated that by the end of 2015, about 1.46 million people in Uganda were living with HIV.
Viral load is recommended as the best monitoring method to making a diagnosis and also confirming ARV treatment failure. 5 The Global Health Sector Strategy on HIV recommends that 90% of people living with HIV know their HIV status; 90% of people diagnosed with HIV receive ARV treatment; and that 90% of people living with HIV, who get treatment, achieve viral load suppression. 6 HIV viral load suppression is the most important indicator of successful antiretroviral therapy. 6 It was noted that antiretroviral treatment (ART) aims to improve the prognosis and quality of life for patients living with HIV by reducing the rate of disease occurrence, progression and mortality. 7
There is low viral load suppression among HIV infected individuals on ART in Bulambuli District. According to the Uganda Viral Load dashboard of 2017, Bulambuli District had a viral load suppression level of 74.6%. 8 The Bulambuli district level is significantly below the UNAIDS 90-90-90 target of 90% for viral load suppression by 2020. In spite of the efforts to scale-up of HIV testing, treatment of all those positive, health education of the people on media, massive distribution of condoms and related interventions including making supplies and medicines available and affordable, so little is known about factors associated with viral load suppression among individuals on anti-retroviral therapy in Bulambuli District.
Poor adherence has also been associated with patients who experience side effects to the ART and this affected males more than females. 9 It has also been reported that better ART leads to a significant reduction in disease progression. 10 This implies that there are ART related factors that influence viral load suppression among individuals living with HIV on ART. It was indicated that complexities of the medicines in ART influenced adherence and thus indirectly impact on viral load suppression among individuals on ART. 11 Other studies have found out that viral load suppression is greater for younger patients than for older patients on ART who adhered to the treatment. 12 Another study indicated a significantly higher rate of non-viral load suppression in adolescents compared to young adults when those lost to follow up and the dead were excluded. 13 In peer review 6 studies that reported on viral load suppressions indicated a variation in the proportion of adolescents with viral suppression 12 months after ART initiation between 27% and 89% meaning viral suppression in adolescents was highly variable that needed improved reporting. 14
This study critically looked at clinical factors, ART and socio demographic factors, while controlling for confounders using adequate sample size and a retrospective cohort study design. Though the viral load suppression rate in Bulambuli was found to be 74.6% in 2017 among
HIV infected people, this is bound to change with the various interventions in place and so it could be different at the moment. Failure to achieve and maintain viral load suppression is associated with continued risk of HIV transmission so this study strived to point out specific factors that influence VL suppression in order to help design interventions to the problem.
Methods
Study area
This study was carried out in Bulambuli District, Eastern Uganda and the study site was Muyembe Health Centre IV (HCIV). The District is bordered by Nakapipirit district to the north, Kapchorwa District to the east, Sironko District to the south and Bukedea District to the west. Bulambuli District headquarters are located approximately 32 km (20 miles), by road, northeast of Mbale, the largest city in the sub-region. The District has got 10 Health Centre IIIs and 01 HCIV located at Muyembe. ART services are only accessible at Health Centre III and Health Centre IV so the study site was Muyembe HCIV which is not only centrally placed and easily accessed by most people but also one which is functionally active as far as ART in Bulambuli District is concerned with 2050 enrolled. Among the 2050 only the ones who had a viral load result done (1101) were the ones entered in the study.
Study population
The target population was HIV infected individuals on ART in Bulambuli District while the accessible population was HIV infected individuals on ART attending ART clinic at Muyembe HCIV in Bulambuli District. The study population was HIV infected individuals of all age groups, on ART for at least 6 months, with a viral load test done and attending Muyembe HCIV from June 2016 to April 2018. No records were excluded.
Study design
This was a retrospective cohort study that reviewed patient records.
Minimum sample size calculation
We calculated the minimum sample size using the formula: n = Z 2 (1-α/2)P(1-P)N/(d 2 N + Z 2 (P(1-P)); where: n = Sample size; N = is the total number of patient records in the Muyembe HC IV; Z = is a critical value corresponding to 95% level of confidence with a value of 1.96; P = proportion of patients who don’t attain viral load suppression at 6 months after ART initiation.; and d –Margin of error (precision error) = ±5%. Substituting into the formula, n = 261 (minimum sample size). Though minimum sample size was 261, we reviewed all 1101 records to increase on the precision of our estimates by reducing on the margin of error.
Sampling procedure
All the records of the HIV patients on ART at the health facility with a viral load test result were reviewed.
Study variables
Dependent variable
The dependent variable was viral load suppression status (suppressed/not suppressed).
Independent variables
Independent variables were categorized into 3: Socio-demographic factors, ART related factors and Clinical factors
Data Collection
Data were collected using a data abstraction tool from clinical records. The tool has been deposited in the data repository. 15 Data abstraction was carried out at a single point per patient, and there was no follow up. Patient’s cards were used to evaluate adherence as it has provision of adherence evaluation at every time of patients review by the clinicians and the nurses.
Data Analysis
Data were analyzed using descriptive and inferential statistics using STATA computer software version 14. Categorical variables were summarized using descriptive statistics by computing proportions while continuous variables were summarized using means and standard deviation.
In order to determine the proportion of individuals receiving ART at Muyembe HCIV who attained viral load suppression at 6 months post ART initiation, the proportion was calculated by dividing the number of patients who had achieved viral load suppression (VLS) by the total number of patients enrolled in the study. Similarly, in so as to determine the factors associated with poor viral load suppression among individuals on ART at Muyembe Health Centre IV in Bulambuli District, 2 approaches were used; first through bivariate analysis using chi square statistic and then the P-value less than .05 was taken to be statistically significant. Then all factors included in the bivariate analyses which were ART and clinical related factors were included in the final logistic regression model.
Results
Participant characteristics
One thousand one hundred and one (1101) patient records were reviewed. Of these 767 (69.7%) patients were female and about half of them (48.4%) were 35 years and above. Six hundred nine (55.3%) were married and over 60% (n = 678) lived in urban areas (Town councils of Bulambuli, Kamu, Bulegeni TC and Sironko).
Five hundred fourteen (47.8%) enrolled into care at HIV/AIDS WHO clinical stage two. About half of the patients (n = 542 (49.2%) had a weight above 50 kgs (report underweight instead). One thousand and twenty one patients (n = 1021, 92.7%) did not suffer from opportunistic infections. Fifteen patients (1.4%) had pulmonary tuberculosis. Among those patients (n = 61, 5.5%) were pregnant. About 65% (n = 712, 64.7%) of the patients had been on ART for more than 2 years.
Majority (98.8%) patients on non-protease inhibitors. Majority (96.5%) of the patients were on cotrimoxaxole or dapsone. A good adherence was 79.6% of the patients. One thousand thirteen patients (82%) reported no side effects on ART. Most (62.9%) the patients were taking a single dose which was efervirez based regimen.
Those who received counselling before ART initiation were 85.4%. One thousand and twenty eight patients (93.4%) had a treatment supporter in form of a relative.
The average Cluster of Differentiation 4 (CD4) count of the patients was 210 at ART initiation (SD = 222.3 with a minimum of 15 and maximum of 3561 as shown in Table 1.
Characteristics of the study participants.
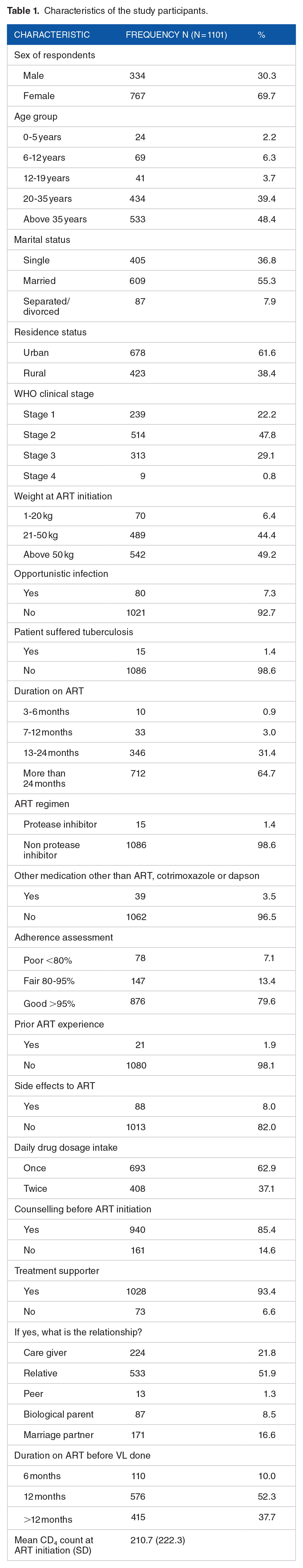
Of 1101 individuals, 944 (85.7%) had attained viral load suppression. Over half (52.4%) had a viral load measured at 12 months post initiation as shown in Table 2.
Viral load suppression at least 6 months post ART initiation.
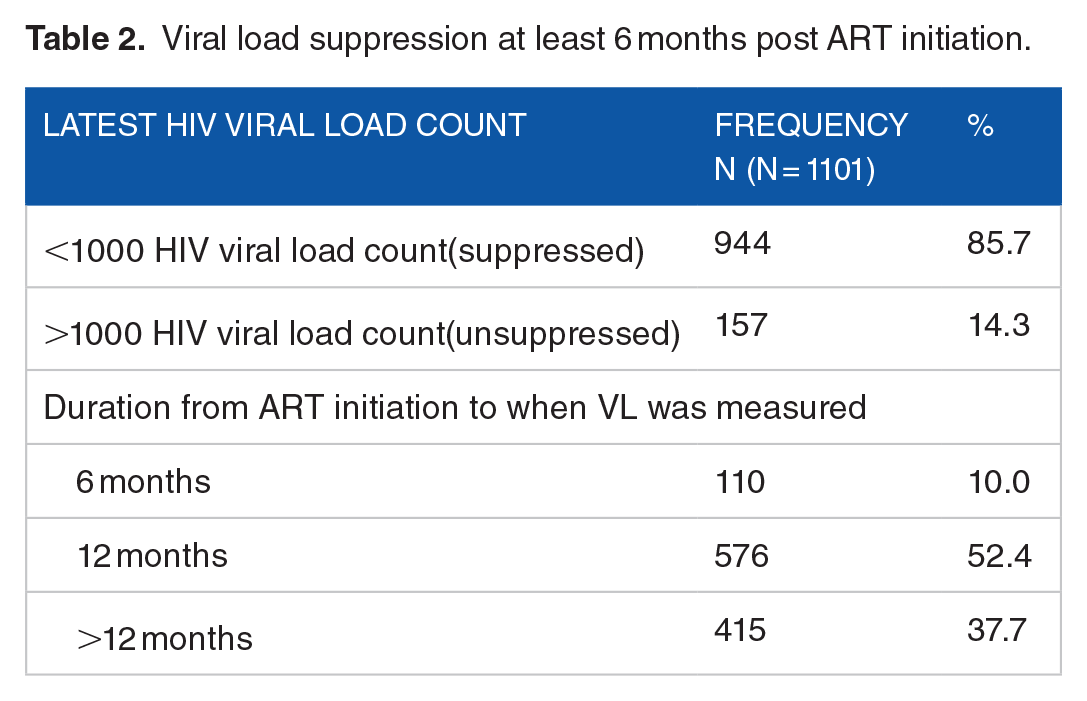
At bivariate analysis using a chi square test the following factors were associated with viral load suppression: age (χ2 = 24.707), marital status (χ2 =15.795), weight at ART initiation (χ2 =4.141), residential status (χ2= 4.401), adherence (χ2 = 37.249) and relation with the treatment supporter (χ2 =11.027) as in Table 3.
Factors related with poor viral load suppression at bivariate analysis.
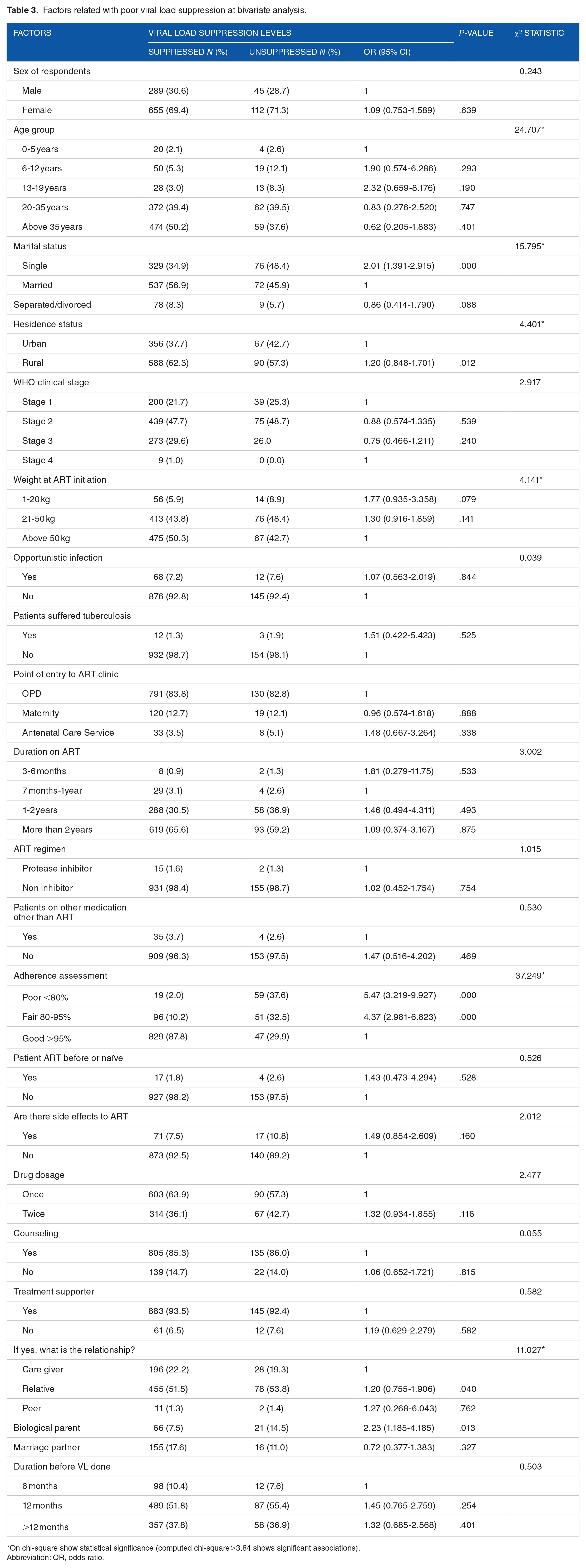
On chi-square show statistical significance (computed chi-square>3.84 shows significant associations).
Abbreviation: OR, odds ratio.
Adjusting for known confounders, only adherence to ART was a significant predictor of viral load suppression, as shown in Table 4. Individuals with fair adherence (80%-95%) had 2.667 times the odds of VLS, CI = 1.122-9.370, P-value of <.002 compared to individuals with good (>95%) adherence which was used as the reference while those with poor (<80%) adherence had 4.553 times the odds of attaining VLS, CI = 1.31-13.930, p-value of <.001 compared to individuals with good adherence.
Multi-variate logistic regression results.
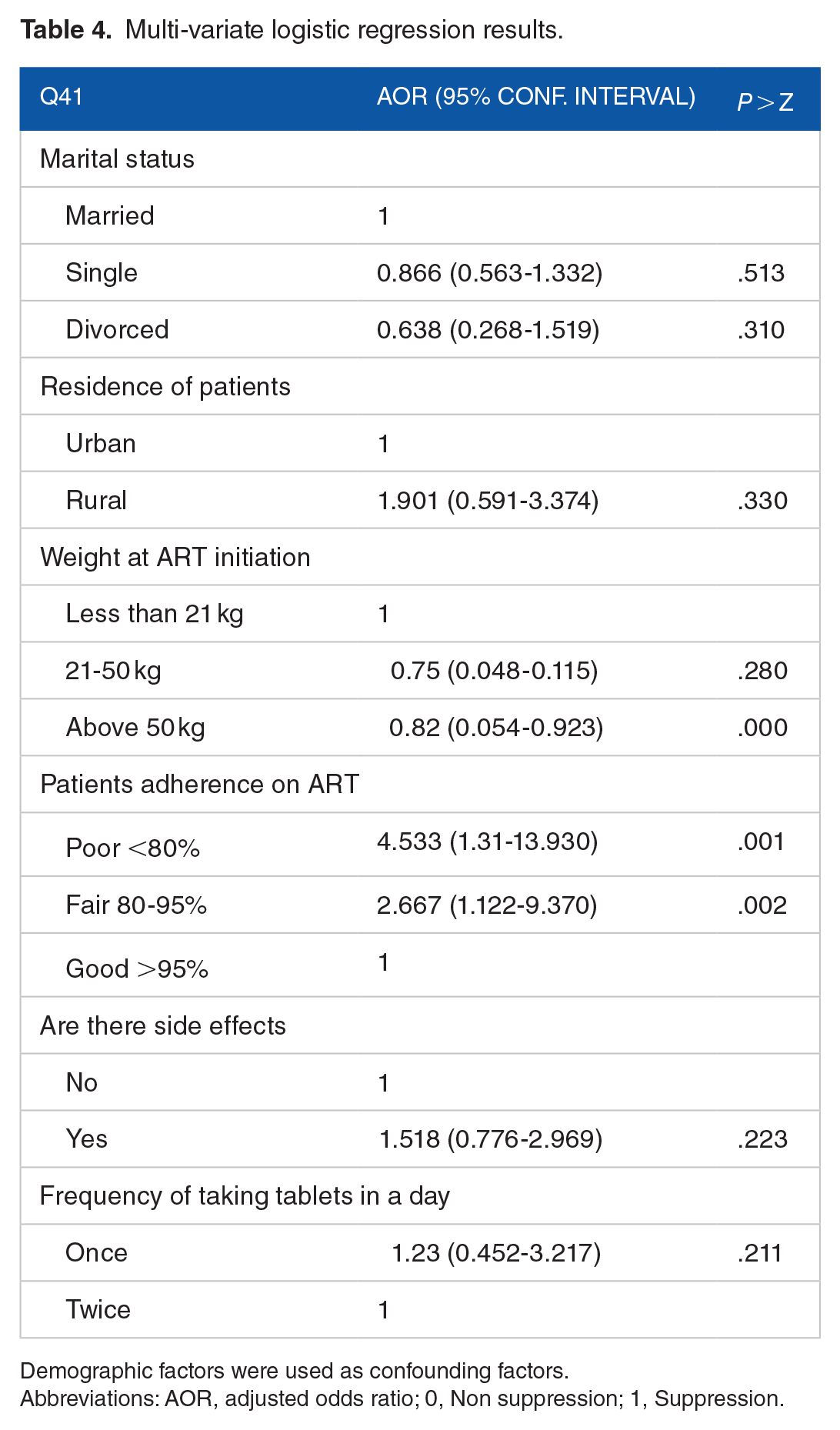
Demographic factors were used as confounding factors.
Abbreviations: AOR, adjusted odds ratio; 0, Non suppression; 1, Suppression.
Discussions
Of the records reviewed 85.7% had attained viral load suppression at least 6 months post ART initiation. Our findings differ from the Ministry of Health viral load dash board that showed the level of viral load suppression level was 74.6%. 8 This could be due to poor reporting at different health facilities and the interventions put in place MOH. Our findings show that for the 576 of patients (52.4%) their viral load was measured at 12 months and beyond and only (n = 110, 10%) were measured at 6 months which is contrary to the WHO consolidated guidelines on viral load testing which recommend that viral load be measured at 6 months after ART initiation. 6
The average CD4 count was 210 (SD = 222) at ART initiation. Initiating ART at low CD4 cell counts does not affect viral suppression but has a two-fold increase in mortality risk compared to people with more robust immune reconstitution. Hence the low CD4 counts at initiation in our study population did not directly affect the level of viral load suppression observed.
In the current study, gender was not associated with VLS. From earlier studies, there were conflicting results reported about the impact of gender on response to ART. 16 Other studies showed further variation in gender ranging from no observed differences between females and males 17 to a more favorable outcome for women. 18 Additionally, since significant differences between males and females were shown regarding tolerability and drug levels of ART, the potential for pregnancy should be considered when prescribing ART in women of childbearing age. 19
The results of this study further indicated that the residence of the patient and viral load suppression had no association meaning that the place where one stays does not significantly affect viral load suppression. These results were found to be in agreement with a growing body of literature that provides evidence that location of where the patient resides in terms of distance from the health facility is not necessarily a barrier that can affect viral load suppression. 20 Sahay and others further indicated that location of the health facility was associated with adherence but not necessarily with viral load suppression. 20
Our findings show that adherence to ART is the only predictor of viral load suppression. Individuals with fair adherence (80%-95%) had 2.667 times the odds of viral load suppression compared to individuals with good adherence (>95%) while individuals with poor adherence (<80%) had 4.553 times the odds of viral load suppression compared to individuals with good adherence. This is in agreement with several other studies which reported significant association of viral load suppression with adherence. It had been reported that poor adherence or non-adherence to ART can lead to rapid replication of the HIV resulting into generation of resistant mutant strains which would no longer be responsive to available antiretroviral drugs,21-23 and this was in agreement with the results of this study. Therefore, while adherence to ART has been pointed out as being very vital, many health care professionals may not accurately be able to predict which clients are more likely to adhere to their regimen, as reported much earlier by Dohrn and colleagues in 2006. 21
It has also been reported that high viral load increases the likelihood of transmission during risky behavior and non-adherent individuals may be more likely to transmit drug resistant strains of virus. However, the prevalence and patterns of non-adherence to antiretroviral drugs remain unclear, largely because of the lack of any gold standard for its measurement. A number of studies have found that 90%-95% of doses must be taken for optimum viral load suppression. In addition suboptimal adherence to highly active antiretroviral therapy has been associated with more rapid disease progression,23,24 which concurs with the findings of this study because both studies found out that adherence was the predictor to viral load suppression and disease progression. There is need to undertake the intensive adherence counselling which can help one know the real cause of nonadherence to the ART which is a main predictor of viral load suppression to enable in addressing the problem of failure to attain viral load suppression. This is because there is no way to predict who of the HIV clients is more likely to adhere to the treatment as reported by Dohrn and colleagues in 2006.
This study found that there was no association between age of the patient and viral load suppression. Our study further found no association between opportunistic infections and viral load suppression (AOR = 1.034, 95% CI = 0.417-2559, P-value = .943) where an opportunistic infection is caused by pathogens that take advantage of the weakened immune system of someone and it is usually due to HIV/AIDS. However another study showed that opportunistic infections such as TB and other conditions like peripheral neuropathy, hepatitis B and anemia, and WHO stage influence the viral load levels and usually make them rise. 25 It was also reported that the risk of developing tuberculosis increased with increasing viral load and therefore recommended HIV viral load monitoring to detect those at high risk of developing tuberculosis but this was independent of the CD4 count. 26 Our study found no association between side effects to the ART and viral load suppression. However, anticipation and fear of side-effects also have an impact on adherence which directly affects VLS. Thus poor adherence has also been associated with patients who experience side effects to the ART and this affected males more than females. 9
Our results indicated that the time a patient had been on ART before a viral load was measured was not associated with viral load suppression however on the contrary other studies showed a variation in the proportion of adolescents with viral suppression 12 months after ART initiation between 27% and 89%. 14 A study in Northwestern Uganda found that at 12 and 24 months, 75% and 72% of patients, respectively, had undetectable viral load (<400 copies/ml).
This study showed no association of counselling at ART initiation with viral load suppression. Where counselling is the process of giving adequate information to the patient about the nature of sickness, expected outcomes when on ART, side effects and what happens when one does not adhere to the treatment however this was not in agreement with a study by Weiser and colleagues who found out that counselling on the need to take ARVs with food, competing demands between food cost and healthcare expenses and forgetting or being unable to take ARVs while working were other factors that influenced adherence and indirectly affected the viral load suppression. 27 This study also revealed that taking other medications other than ART or cotrimoxazole/dapsone was not significantly associated with viral load suppression but this was different from studies by Petersen and colleagues which indicated that complexities of the medicines in ART influenced adherence and thus indirectly impact on viral load suppression among individuals on ART. 11
Our study had some limitations which included missing data and this was handled by taking different denominators “N” for those which had missing variables and this was by taking only those found in the records. This did not affect the study outcome since the sample size was quite big. Specifically, 67 patients had marital status data missing. Since the study did not involve interviewing of participants but rather reviewing of records, this approach could not allow further investigation into some of the information that could have provided more enriched information to the research.
Conclusion
The Bulambuli findings show that their viral load suppression was at 85.7% which was on track to attaining the third 90 of the 90, 90, 90 global targets by 2020. Adherence was the only significant predictor of viral load suppression. Counselling about the importance of adherence is key in management of those patients on ART.
Identifying the causes of poor adherence and systematically addressing them has the potential to support Bulambuli and the country to attain the last 90 targets. Therefore, the study recommends that, more efforts should be focused on strengthening intensive adherence counselling to those who are not suppressing. Capacity building of health workers in adherence counselling and placement of counsellors in ART clinics could have an impact of improving adherence and thereby improving viral load suppression.
Similarly, for further studies, carrying out other studies in all the health facilities of Bulambuli district and other districts is recommended as this will try answer the discrepancy between the ministry of health data and that from the current and other similar studies.
Footnotes
Acknowledgements
This work forms part of PW’s Master of Public Health dissertation at Faculty of Health Sciences, Busitema University, Uganda. The authors therefore wish to thank colleagues and all staff members in the Department of Public Health at the Faculty for their tireless contribution towards the completion of this project. We further thank the research assistants and the technical staff at Muyembe HCIV who rendered their support during the data collection period. Finally, we thank the SURVIVAL Pluss Project for the research grant that enabled successful completion of this work.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the NORHED Project (SURVIVAL-PLUSS), support to Busitema University. The funders only provided funds to facilitate the research approval and data collection process. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Authors’ contributions
This work was collaboratively carried out. Author PW contributed towards the conception, execution, data analysis and work review. Authors YG and JNW supported the supervision, Data analysis, manuscript writing and revision, and reading and confirmation of the final manuscript. All authors were involved in the manuscript preparation and approval of the final version submitted.
Availability of data and materials
All data on which the results, discussions and conclusions of this manuscript are drawn have been deposited accessible in the free Mendeley Data Repository (![]() ).
15
).
15
Ethics approval and consent to participate
The study was approved by the Busitema University Faculty of Health Sciences Higher Degrees and Research Committee as well as the Mbale Regional Referral Hospital Research and Ethics Committee (Ref No. MRRH-REC-IN-COM 081/2018). Permission to conduct the study was further obtained from the Bulambuli District Health Office. Waiver of informed consent was attained because the study involved secondary of existing medical records that were initially collected for purposes of patient care however privacy and confidentiality of personal information was observed. The tool used for data collection provided for numbers not names which ensured that no individual personal data was exposed and the date collected was stored securely to avoid any other people not involved in research from access. The research presented no risk of harm to subjects.
Consent for publication
Not Applicable
