Abstract
Background:
Although there is a high burden of HIV in sub-Saharan Africa (SSA), studies on mental health issues among people living with HIV are scarce. The study addressed the transition to “test and treat” guidelines for HIV, which makes it unique regarding its evaluation of psychological distress amongst newly initiated people living with HIV in the test and treat era.
Methods:
We conducted a cross-sectional survey of 689 people newly diagnosed with HIV. Symptoms of psychological distress were measured using the Kessler-10 psychological distress assessment scale. Factors associated with psychological distress were captured using interviewer-administered questionnaires. Ordinal logistic regression analyses were employed to identify predictors of psychological distress.
Results:
The magnitude of psychological distress was 58.63% (95% CI = 55.2%-62.3%). The severity of the psychological distress of which, 17.42% had severe distress. Psychological distress was observed more among female patients (β = 0.47, AOR = 1.59, 95% CI = 1.12, 2.27), patients presented with opportunistic infections (β = 0.50, AOR = 1.65, 95% CI = 1.03, 2.66) and being non-working functional status (β = 0.99, AOR = 2.70, 95% CI = 1.64, 4.45). Moreover, patients who were malnourished (β = 0.46, AOR = 1.58, 95% CI = 1.09, 2.26), having good level of knowledge on HIV prevention (β = 0.59, 95% CI = 0.55, 0.39, 0.78), presented with sexually transmitted infection (β = 0.48, AOR = 1.61, 95% CI = 1.01, 2.58), history of alcohol use (β = 0.44, AOR = 1.55, 95% CI = 1.09, 2.21), perceived stigma (β = 0.08, AOR = 1.09 95% CI = 1.04, 1.15) and treated in health centers (β = 0.55, AOR = 1.74, 95% CI = 1.25, 2.41) had higher odds of psychological distress.
Conclusion:
The large majority of newly diagnosed HIV patients suffered from psychological distress. An increased vulnerability was observed among females, those with opportunistic and sexually transmitted infections, those having poor functional status and malnourished. Furthermore, HIV patients treated in health centers, those who had history of alcohol use and patients with high level of HIV related stigma are more negatively affected by the HIV diagnosis. Hence, all intervention strategies should target all the identified predictors.
Introduction
Mental health problems are known to be common among people living with HIV in Africa. 1 In sub-Saharan Africa (SSA), the burden of depression among people living with HIV (PLWH) ranges between 9% and 32%. 2 More than 1.57 million disability-adjusted life years (DALYs) are lost among people with depression and HIV in Sub-Saharan Africa in general and about 30 000 DALYs are lost in Ethiopia in particular. 1 Although there is a high burden of both HIV and mental health problems in SSA, there is scarce research on mental health issues among HIV positive people.3-5
The concept of psychological distress includes a range of emotional states with symptoms of depression and anxiety. 6 Mental health problems are higher among both people vulnerable to acquiring HIV and PLWH, compared with the general population.1,7 Given the strong evidence for the contribution of mental health and behavioral problems to poor HIV health outcomes, there is an obvious need for universal mental health screening and the provision of mental health treatment integrated into ongoing HIV care. 7 However, most of the studies conducted in Africa among HIV patients do not use validated tools in the study areas. 1
In Ethiopia, expansion and strengthening ART care and treatment activities are supported by the process of task shifting: training of nurses and community health agents in prevention, treatment, care, and support activities which further strengthen community linkages and ensure availability of standard minimum packages of HIV services at primary health care level. 8 Additionally, due to insufficient mental health specialists to close the enormous treatment gap for mental disorders among HIV patients, “task-shifting” (training and supporting non-specialist health workers to deliver mental healthcare) 5 may also be implemented in the HIV clinic. Moreover, screening for and managing mental health problems and substance use is one of the key elements of chronic HIV care in Ethiopia. 8
Newly diagnosed PLWH are exposed to multiple stressors. These include concerns of confidentiality, discrimination/stigmatization, disclosure, and fear of infecting others. 9 On the other hand, the 2017 revised World Health Organization (WHO) guidelines for managing advanced HIV disease and rapid initiation of antiretroviral therapy (ART), 10 indicated that there is a research gap on the psychological readiness of newly diagnosed HIV positive individuals. Psychological distress is a major barrier to timely ART initiation.5,11 HIV positive people with uncontrolled depressive symptoms are more likely to have poor adherence to ART 8 and to have poor health-related quality of life. 12 Hence, documenting the magnitude, severity, and predictors of psychological distress among newly HIV diagnosed people could guide the test and treat strategy.
Previous studies on the burden of psychological distress among HIV infected people have reported a value of 33% in SSA, 1 11.2% in Dilla-Ethiopia, 13 7.8% in North Shewa-Ethiopia 14 and 37.6% of HIV infected people were reported to experience mild/moderate while 29.5% experienced severe psychological distress in Oromia-Ethiopia. 15 Moreover, 24.3% of patients had common mental disorders in Debre Markos referral hospital-northwest Ethiopia 16 and 24.5% of HIV positive people suffered from co-morbidity of depression and anxiety in Addis Ababa, Ethiopia. 17 Similar findings were reported in SSA with 15.3% experiencing major depressive disorder, 1 in rural Tanzania 15.5%, 3 32.6% of depression in Nigeria, 18 13.8% of depressive symptoms in Kenya 19 and 36.5% depressive symptoms in Africa in general. 4 These previously published studies mostly used small sample sizes, conducted in a single clinical settings, use arbitrary dichotomizations of the outcome variables and surveyed among HIV positive patients who are already on treatment. However, our study tried to address gap from the previous studies. This study included multiple clinical sites with large number of newly HIV diagnosed people and data were analyzed using ordinal logistic regression analysis.
At the time of HIV diagnosis, the level of psychological distress among newly identified HIV patients is high. 9 But it decreased over time due to an individual positive thinking and other coping behaviors. 20 Mental health affects both HIV patients’ treatment uptake and clinical outcomes. 21 Hence, investigating the level of psychological distress among newly diagnosed HIV patients in the test and treat era added new information in the literature.
Factors associated with psychological distress are being female, illiterate, current use of alcohol, low social support, low socioeconomic status, immunosuppression, and perceived stigma.2,9,13,14,22,23 Other factors associated with the level of anxiety are perception of side effects, ART drug regimen and duration on treatment.19,24 Severe psychological distress was highly prevalent among those who were recently diagnosed and who initiated ART late.15,25 Furthermore, concerns of confidentiality, disclosure, emotional distress, fear of infecting others, and excessive attention to physical functions were the most common source of stressors among newly diagnosed HIV positive people. 9 On the other hand, there is growing evidence that PLWH with sustained HIV viral suppression cannot transmit HIV through sex. 26 This may allow optimized messaging of undetectable = untransmittable (U = U) that will build hope in the community and contribute to a lessening of HIV-related stigma. Ultimately, this has the potential to reduce psychological distress among PLWH and their sex partners. 7 Measuring the current level of psychological distress could provide timely information to guide public health intervention along with the changing guidelines. Therefore, the aim of this study was to investigate the magnitude and predictors of psychological distress among newly diagnosed HIV positive people in northwest Ethiopia.
Methods
Design
This was a cross-sectional survey of newly diagnosed people living with HIV.
Study setting
The study was conducted in 3 administrative zones of Amhara regional state, northwest Ethiopia. These are: Bahir Dar City administration, East Gojjam zone, and West Gojjam Zone. The study period covered from December 1st, 2018 to July 30, 2019. We have recruited newly diagnosed HIV patients from 23 selected health facilities rendering ART services. Of which 2 are referral hospitals (Debre Markos and Felege Hiwot), 7 are primary hospitals and the remaining 14 are health centers. In all health facilities, integrated mental health services were available. At least 1 staff member of the HIV clinic had received training in the screening and management of common mental health disorders.
Study participants
The 3 administrative zones were selected purposefully. Then health facilities (both hospitals and health centers) were selected based on patient case load. Accordingly, those ART rendering health facilities with average monthly new patient flow of minimum 3 cases were included in the study. For this purpose, we have conducted secondary data analysis from the health facility’s previous 3 months report. Study participants were recruited from health facilities that on average diagnosis 3 to 5 new HIV patients per month. All adults newly diagnosed to be HIV positive were consecutively enrolled in the study. Data were collected within 30 days of HIV diagnosis irrespective of ART initiation. Those patients who interrupted their treatment previously and re-initiated during the study period were excluded from the study.
Sample size determination
The patients enrolled for this study were part of a cohort study. The sample size was thus calculated to ensure adequacy of the sample to investigate the psychological distress and its correlations. Sample size was determined using Epi-Info (7) a total of 689 patients were required for the cohort study and we used all enrolled for this study.
Sampling technique
All newly diagnosed HIV positive individuals who intended to continue their HIV treatment in the same health facility where the diagnosis is made or those who were referred to the study health facilities from other health facilities within 7 days of diagnosis were invited to participate in the study. All eligible patients were enrolled until the required sample size was reached.
Data collection tools and procedures
Data collection tools were developed by reviewing literature in the field. The tools measured socio-demographic characteristics, clinical characteristics, behavioral and psychological characteristics. The psychological distress tool was adopted from the Kessler-10 scale 27 which has been validated in Ethiopia.15,25 Data was collected using interviewer administered questionnaires. Data collectors were nurses working in the ART clinic. The client exit interviews were conducted in a separate quiet room.
Variables and measurement
The dependent variable was psychological distress measured using the Kessler Psychological Distress Scale (K10). 28 The K10 is a 10-item, 5-level response scale. K10 values range from 10 to 50. The outcome variables were measured using 10 questions each containing 5-point Likert scales (1 = never, 2 = a small part of the time, 3 = some of the time, 4 = most of the times, 5 = all of the time). Values less than or equal to 19 were categorized as not clinically significant distress (well), scores between 20 and 24 as mild distress, 25 to 29 as moderate distress, and 30 to 50 as severe psychological distress. 29
The independent variables included socio-demographic variables (age, sex, religion, ethnicity, marital status, educational status, employment status, occupation, residence) wealth status calculated based on world food program guidelines to wealth index calculation, 30 health facility related characteristics (types of health facility and distance from health facility), baseline clinical variables (opportunistic infections, body mass index—BMI, functional status, any current health complaints, and WHO clinical stage), behavioral variables (substance use, serostatus of sexual partner and HIV test history, number of sexual partner/s, condom utilization, and alcohol use. HIV and ART related Knowledge, history of STI). Level of perceived HIV-related stigma was assessed using 4 item questions with a Cronbach’s alpha value (α = 0.896), which had adequate reliability score to measure HIV-related stigma.
Data management and analyses
Data were entered into Epi-Data version 3.5 and exported to STATA version 14 and SPSS version 24 for further analysis. Descriptive analysis such as frequency and percentage was carried out. We used ordinal logistic regression analysis to predict factors associated with the outcome variable. The outcome variables were in 4 scales based on disease severity (well, mildly distressed, moderately distressed, and severely distressed). Each independent variable was fitted in the model separately and check for the assumptions of ordinal logistic regression. We excluded those independent variables with empty cells and those with small in frequency from the cross-tabulation. Then those that passed the assumptions of the model were fitted altogether to predict the outcome variables. The assumptions for ordinal regression which assuming that the effect of the independent variables is the same for each level of the outcome variables was checked via test of parallel lines. Values for the final model assumptions were as follows; model fitting information (Chi-square = 155.691,
Finally, the results were presented using parameter estimates (β) and adjusted proportional odds ratio (AOR). The statistical significance was declared at
Ethical approval and consent
The proposal was approved by the joint University of Ibadan/University College Hospital, Ibadan Institutional Review Board (IRB) of the University College Hospital (UCH), University of Ibadan, Nigeria (reference number UI/EC/18/0463). It was also approved by IRB at Debre Markos University (reference number HSC/30/02/2011). We obtained permission from Amhara Public Health Institute. Moreover, we obtained written informed consent from each study subject.
Results
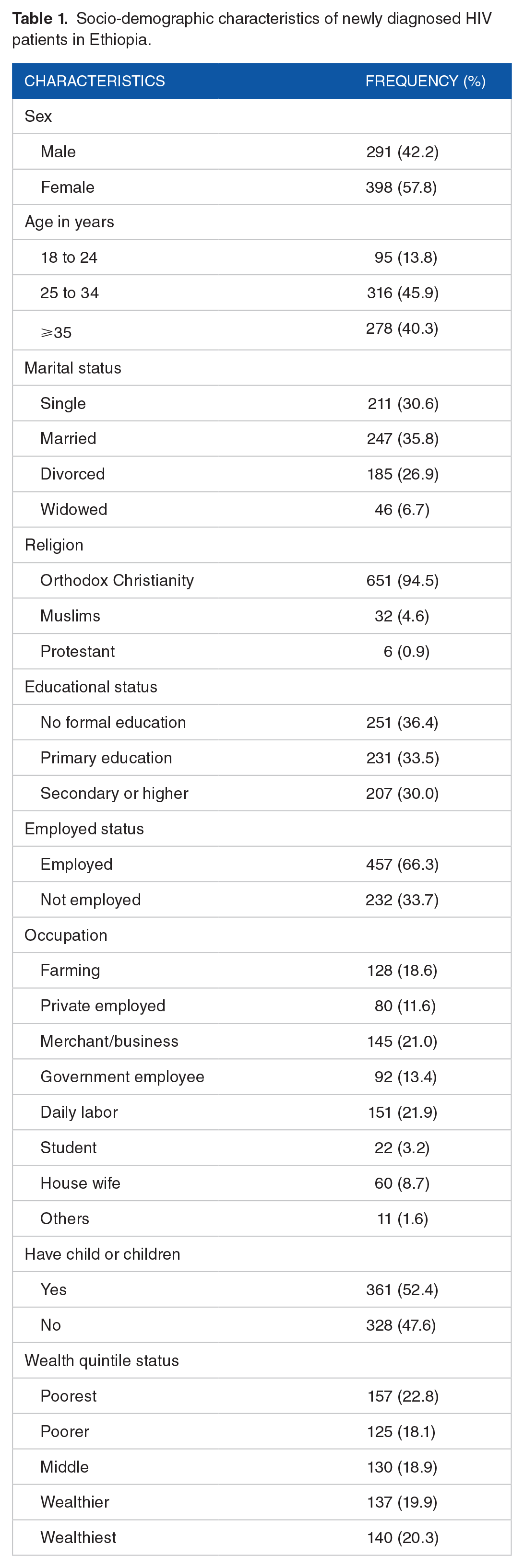
A total of 689 newly diagnosed HIV patients were included in this study. Three hundred ninety-eight (57.8%) were females. The mean age of study participants was 33 ± 9.17 years and 316 (45.9%) were in the age group of 25 to 34 years. The majority (651, 94.5%) were Ethiopian Orthodox Christian by religion. Four hundred fifty-seven (66.3%) were employed and 282 (40.9%) were in the poorest or poorer wealth quintile (Table 1).
Socio-demographic characteristics of newly diagnosed HIV patients in Ethiopia.
Health facility-related characteristics of study participants
Two hundred eighty-four (41.2%) of the study participants were from East Gojjam zone, 165 (23.9%) from West Gojjam zone and 240 (34.8%) were from Bahir Dar City administration. Attendance in the health facilities showed that 352 (51.1%) attended hospitals and 337 (48.9%) within health centers. The majority (531, 77.1%) were urban residents and 540 (78.4%) of them were located less than 1-hour walking distance from the health facility. Similarly, 490 (71.1%) were residing within the catchment area of the health facility.
Clinical characteristics of study participants
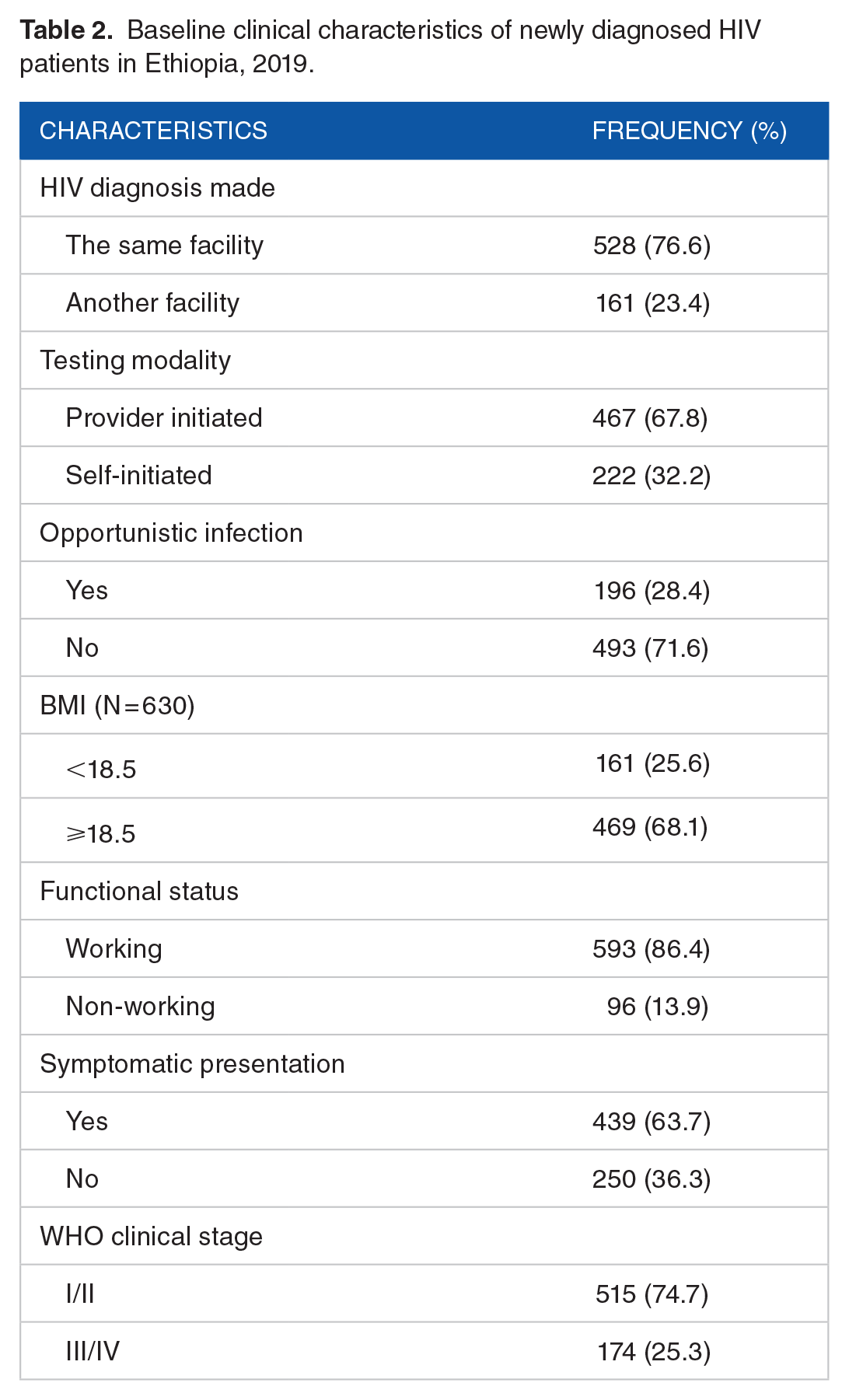
The majority (528, 76.6%) were diagnosed with their HIV status in the same health facility in which they were linked for ART service. HIV test was initiated by health care providers in 467 (67.8%) of study participants. About 196 (28.4%) had opportunistic infections at enrollment. The stages of majority (593, 86.4%) of participants were at working functional status while 515 (74.7%) were at WHO clinical stage I/II. Forty-two (6.1%) women were pregnant (Table 2).
Baseline clinical characteristics of newly diagnosed HIV patients in Ethiopia, 2019.
Behavioral characteristics
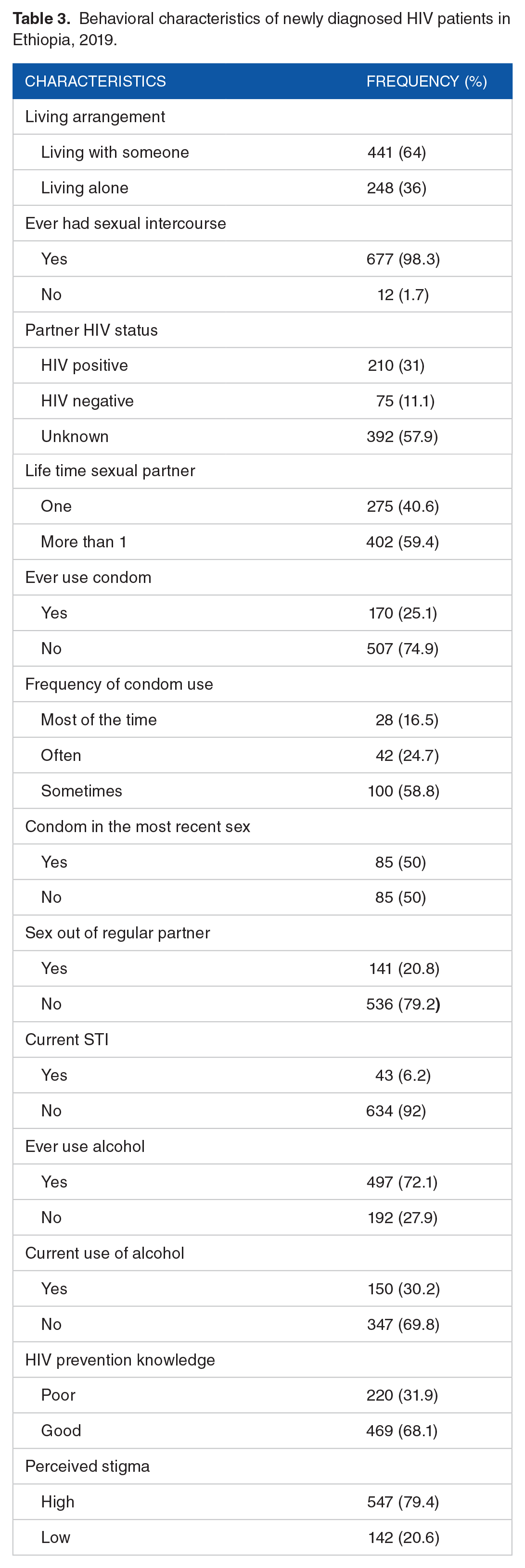
The majority (677, 98.3%) had sexual experience and 402 (59.4%) had more than one-lifetime sexual partner. One hundred seventy (25.1%) reported ever use condom while 85 (50%) of them reported condom use in the most recent sexual activity. Three hundred ninety-two (57.9%) of participants reported that they did not know the HIV status of their sexual partners (Table 3).
Behavioral characteristics of newly diagnosed HIV patients in Ethiopia, 2019.
Magnitudes of psychological distress
About 404 out of 689 patients (58.64%, 95% CI = 55.2%-62.3%) had different level of psychological distress symptoms. These included: mildly distressed (23.07%), moderately distressed (18.14%), severely distressed (17.42%) and 41.36% were well or not distressed.
Predictors of psychological distress
Before conducting ordinal logistic regression, we checked the frequency of each variable and excluded those with empty cells and those with small frequency using cross-tabulations. Ordinal logistic regression fitted with each independent variable and the outcome variables to test the assumption of the model. Then all independent variables were fitted into ordinal logistic regression. Proportional adjusted odds ratio and parameters estimates (coefficients) were reported to indicate the strength and directions of association.
HIV patients attending their treatment in health centers, we would expect 0.55 increase on the odds of having psychological depressive symptoms compared to those in hospitals, (β = 0.55, AOR = 1.74, 95% CI = 1.25, 2.41). Psychological depressive symptoms among females increased by 0.47 compared with male counterparts (β = 0.47, AOR = 1.59, 95% CI = 1.12, 2.27). Presence of opportunistic infections at enrollment to care increase by 0.50 (β = 0.50, AOR = 1.65, 95% CI = 1.03, 2.66). Similarly, baseline non-working (ambulatory or bedridden) functional status a 0.99 increase in the odds of having psychological depressive symptoms (β = 0.99, AOR = 2.70, 95% CI = 1.64, 4.45). Moreover, patients who were malnourished (β = 0.46, AOR = 1.58, 95% CI = 1.09, 2.26), having good level of knowledge on HIV prevention (β = 0.59, 95% CI = 0.55, 0.39, 0.78), presented with STI symptoms (β = 0.48, AOR = 1.61, 95% CI = 1.01, 2.58), history of alcohol use (β = 0.44, AOR = 1.55, 95% CI = 1.09, 2.21) and perceived stigma (β = 0.08, AOR = 1.09 95% CI = 1.04, 1.15) had higher odds of psychological depressive symptoms (Table 4).
Ordinal logistic regression on predictors of psychological depressive symptoms among newly diagnosed people living with HIV in Northwest Ethiopia, 2019.
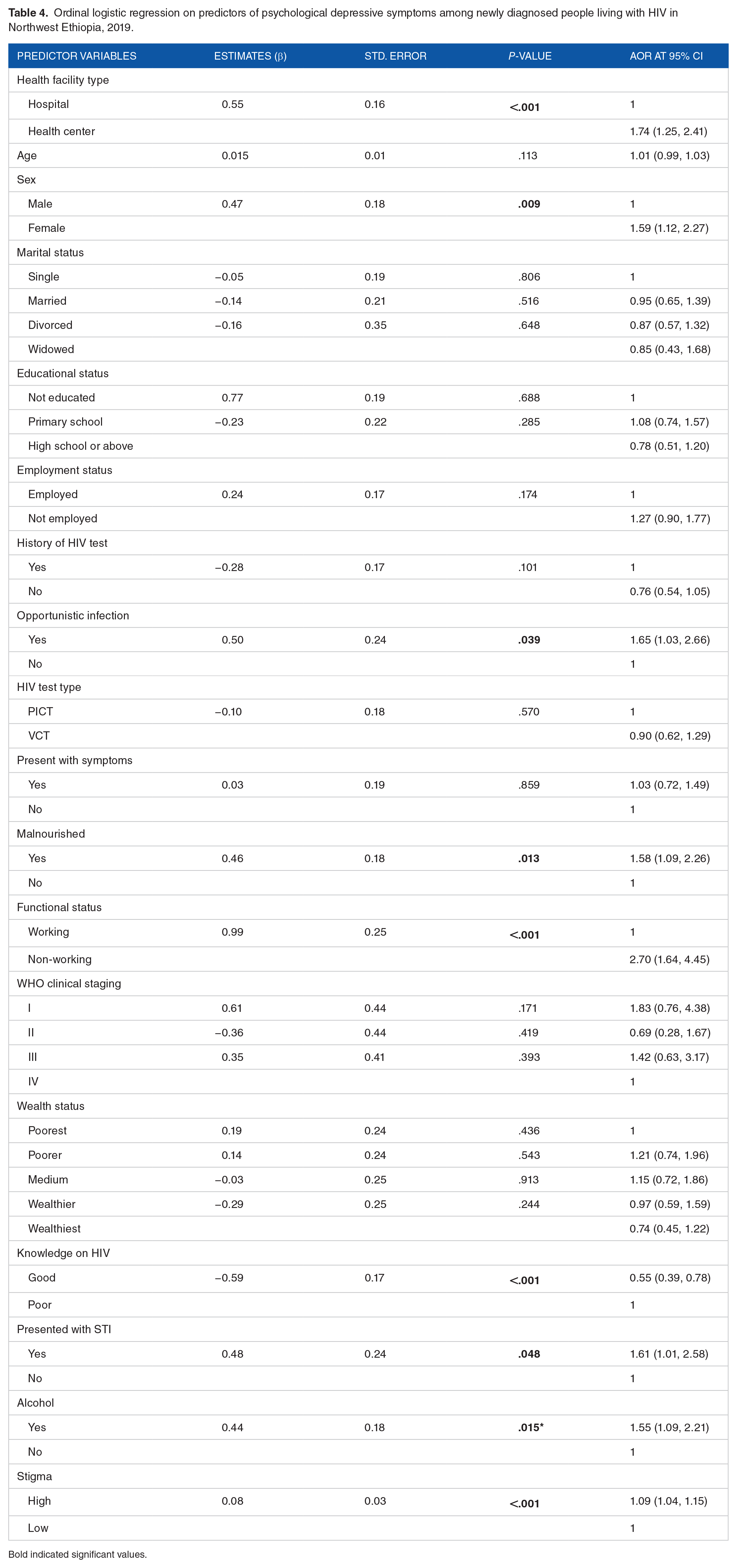
Bold indicated significant values.
Discussion
This study aimed to examine the magnitude of psychological distress and predictors among newly diagnosed persons living with HIV in northwest Ethiopia.
The large majority of newly diagnosed HIV patients suffered from psychological distress. An increased vulnerability was observed among females, those with opportunistic and sexually transmitted infections, those patients having poor functional status and malnourished. Furthermore, HIV patients treated in health centers, those who had history of alcohol use and patients with high level of HIV related stigma are more negatively affected by the HIV diagnosis. The prevalence of psychological distress (58.6%) among newly diagnosed HIV positive people was similar to some studies in Ethiopia.11,15 But much higher than other studies in Ethiopia.13,14 The discrepancies may be attributed to the difference in tools used to assess psychological distress. The latter 2 studies used self-reported questionnaires (SRQ-20) and Hospital Anxiety and Depression Scale (HADS) tools, respectively while the current study used the Kessler-10 psychological distress scale to measure the level of psychological distress. Several tools are used to screen different mental health problems among people living with HIV and in the general population.2,28,31 Validating the most accurate tools according to the population of origin (language, education) as well as ART status is necessary. 2 This finding implies that there is a need to a nationally validated mental health screening tools for both research and public health intervention purpose in Ethiopia. Moreover, the current finding (58.6%) was higher than a value (33%) reported in systematic review and meta-analysis in Sub-Saharan Africa. 1 Such differences may be attributed to inter-scale variations in the measuring of psychological distress.
In the current finding, the severity of psychological distress symptoms was lower than previously published reports in Ethiopia15,25 but higher than a study in Malawi. 32 In addition to the tool differences used among the studies, the current study was conducted among newly diagnosed HIV positive patients may be with profound concerns of confidentiality, disclosure, emotional distress, and fear of infecting others. 9 This was supported by previous literature in which HIV patients who were stable and on ART may have benefited from intervention by healthcare workers that lead to decreased HIV related stressors over time.9,15,32,33 Indeed, it is necessary to provide ongoing mental health monitoring of HIV patients at different levels of the healthcare intervention, and special emphasis is recommended for those newly identified HIV positive people.
As we compare females with males, the odds of severity versus the combined mild and moderate level of psychological distress was increased among females. This result was in agreement with the previous findings from Ethiopia,13,14,17,34,35 Houston-Texas 22 and elsewhere in SSA2,23 in which females had higher odds of psychological distress and or depression. The gender disparity may be attributed due to females’ greater reactivity compared with men’s has been attributed to gender differences in biological responses, self-concepts, masculinity issues, and coping styles.36,37 So that, clinicians working in HIV clinics should considered gender-sensitive care.
This study deepens the knowledge on the influence of HIV related stigma on the development of psychological distress. Thus, one-unit increase in a score of perceived HIV related stigma scale, 1.09 times greater in experiencing psychological distress. The finding was in agreement with many studies in the field.9,11,14,16,17,19-21,34,36,38,39 Stigma and discrimination are major barriers to testing, treatment uptake, and adherence. 40 Patients who suffered from depression as a result of stigma are more likely to experience worsening disease states and, thus, poorer health outcomes.41,42 The finding further reinforces policymakers, clinicians and people living with HIV to consider high impact interventions against discrimination and stigma based on HIV positive test result.
Patients who had good knowledge of HIV prevention were less likely to develop psychological distress. This may be due to improved understanding of HIV treatment and prevention. 7 Furthermore, the odds of having psychological distress among those patients with a history of alcohol use was increased compared with their counterparts. The finding was supported by previous studies that reported patients who use alcohol were affected by depressive symptoms.5,14,43 However, due to the cross-sectional nature of the study design, we could not provide the causal associations between depression and alcohol use. A similar study reported that patients had increased alcohol use when they are experiencing higher depressive symptoms than usual, while those with higher average depressive symptoms over time report less alcohol use. 44 So that does the psychological distress caused an increased alcohol uptake or alcohol use caused the psychological distress is not answered by this study. Nevertheless, prevention of alcohol consumption should be continued as 1 arm of intervention in the HIV care, support and treatment services. Hence, restriction of alcohol use among people living with HIV should be strengthened.
Baseline clinical characteristics of people living with HIV were found to be the predictors of psychological distress. Of these, non-working functional status (ambulatory or bedridden), being malnourished, presented with opportunistic infection and sexually transmitted infections. This was in line with previous studies in Ethiopia and Sub-Saharan Africa.2,14,19,38,45,46 Such findings can be explained as physical and or functional changes as a result of a disease process may cause stressful events 9 which in turn caused a significant level of psychological distress. This implies clinicians should give focus to treat physical health conditions in addition to HIV treatment. Provisions of prophylaxis against opportunistic infections and treating sexually transmitted infections should be integrated with mental health interventions. A recent study on the impact of micronutrients on the psychological well-being of HIV infected individuals revealed that supplementing of a micronutrient can reduce the experience of distress, anxiety, and depression among HAART naïve HIV infected patients. 47 This is important to understand the 3 critical junctions of service integrations among HIV, mental health, and nutritional interventions which would enhance the HIV treatment outcomes.
In addition to those predictors from socio-demographic, behavioral, and clinical characteristics of HIV patients, healthcare settings were also known to be one of the contextual predictors of psychological distress. In this study, the odds of psychological distress symptoms were higher among HIV patients who were attending their treatment at primary healthcare settings compared to those treated in hospitals. This may be due to lack of integrated mental health services at lower primary care level.4,48 Therefore, training of healthcare workers on mental health services integration with HIV care, support and treatment in the primary healthcare settings should be a policy priority.
Limitations of the study
Though the study was the first to investigate the magnitude and predictors of psychological distress using ordinal logistic regression analyses in Ethiopia, there were limitations inherited to the study design and data collection tools. The Kessler psychological distress scale (K-10) is not 100% sensitive and specific. The sensitivity and specify of the tool was 86% and 83% respectively. 49 Hence, this may underestimate the magnitude of the problem. Due to the nature of the study design we did not know whether or not the present distress was triggered by HIV diagnosis. Moreover, we did not use a validated social support scale to measure the level of social support.
Conclusion
The magnitude of psychological distress was high among newly diagnosed people living with HIV. Predictor variables emerged from socio-demographic factors (being female), behavioral factors (perceived HIV related stigma, HIV related knowledge and alcohol use), clinical factors such as being in non-working functional status, being malnourished, having opportunistic, and sexually transmitted infections. Furthermore, contextual factors of the healthcare setting played an important role in predicting the level of psychological distress. Hence, all intervention strategies should target the 4 layers of challenges.
Footnotes
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Pan African University (PAU), a continental initiative of the African Union Commission (AU), Addis Ababa, Ethiopia, as part of the Ph.D. program in Reproductive Health Sciences. NAM received the funding from PAU. The University had no role in the study design and decision to publish, or preparation of the manuscript.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
NAM, OAA, MAO, YB, and JOA contributed equally to the design of the study. NAM and YB involved in the data collection. NAM and YB, JOA, OAA, and MAO involved in the data analysis. NAM and OAA drafted the manuscript and all the authors revised and approved the manuscript.
