Abstract
In patients on peritoneal dialysis (PD) peritonitis continues to be the main cause of PD-related death, and the leading reason of transfer to hemodialysis (HD). International guidelines recommend that peritoneal catheter should be removed if PD effluent does not clear after 5 days of adequate antibiotics defining the case as refractory peritonitis. The simultaneous removal and replacement of the peritoneal catheter (SCR) has been used as treatment for recurrent or catheter-related peritonitis after the utter healing of the acute infection to spare patient the interruption of PD and the transfer to HD. On the other hand, in case of refractory episodes the employment of SCR is discouraged. However, the clinical trend of refractory peritonitis is not homogenous: some episodes are totally unresponsive to medical therapy, while others show to be partially responsive. Thus, the treatment should be diversified according to the different clinical evolution. We report two cases of refractory peritonitis sustained by P. aeruginosa that were successfully treated by SCR after a partial response to antibiotic therapy. Along with these preliminary data, we propose a novel therapeutical algorithm differentiating between complete refractory peritonitis and partial refractory peritonitis.
Keywords
Introduction
In patients on peritoneal dialysis (PD) infectious complications still represent the leading reason of transfer to hemodialysis (HD) as well as the main cause of PD-related death.1,2
In case of peritonitis episode, the start of adequate antibiotic treatment usually leads to significant clinical improvement within 72 hours. Therefore, ISPD guidelines recommend removing the catheter if PD effluent does not clear after 5 days of appropriate antibiotic therapy, defining the episode as refractory peritonitis. 3 The catheter removal determines the interruption of PD and the transfer to HD with the creation of a temporary vascular access via a central venous catheter. Notably, more than half of those patients will never resume PD. 4 To avoid the transfer to HD, the simultaneous removal and replacement of the peritoneal catheter (SCR) has been employed with satisfactory results as treatment for recurrent or catheter-related peritonitis after the utter healing of the acute infection.5,6 On the other hand, in case of refractory episodes the employment of SCR is discouraged. 7 However, the clinical trend of refractory peritonitis is not homogenous: some episodes are totally unresponsive to medical therapy, while others show to be partially responsive. Thus, logically the treatment should be diversified according to the different clinical evolution.
We report two cases of refractory peritonitis sustained by P. aeruginosa that were successfully treated by SCR after a partial response to antibiotic therapy. Along with these preliminary data, we propose a novel therapeutical algorithm differentiating between complete refractory peritonitis and partial refractory peritonitis.
Case patient 1
The first case has been previously described. 8 In brief, an 80-year-old white man affected by end-stage renal disease (ESRD) due to unknown cause initiated three exchanges (1.36% glucose) continuous ambulatory PD (CAPD) in June 2020 with no complications. In December 2022 due to the occurrence of peritonitis, the patient was started on empirical antibiotic therapy with ceftriaxone and vancomycin ip. Ultrasonography did not detect any anechoic collection along the tunnel of the catheter. P. aeruginosa was identified in peritoneal liquid culture and according to the antibiogram, the antibiotic therapy was changed to tobramycin ip and meropenem iv. However, after 10 days of appropriate antibiotic therapy, there were still 1800 WBCs/µL (vs 8500 WBCs/µL on the first day) and moderate abdominal pain, while the peritoneal liquid culture resulted negative (Figure 1). It was decided to perform SCR. The maneuver took place without complications and PD exchanges with low volume (1000 mL) were resumed immediately after the procedure. 9 The day after the replacement of the catheter the WBC count in the peritoneal liquid decreased to 50 WBCs/µL along with the resolution of the symptoms (Figure 1). The patient no more experienced PD-related complications and died 16 months later due to cachexy.
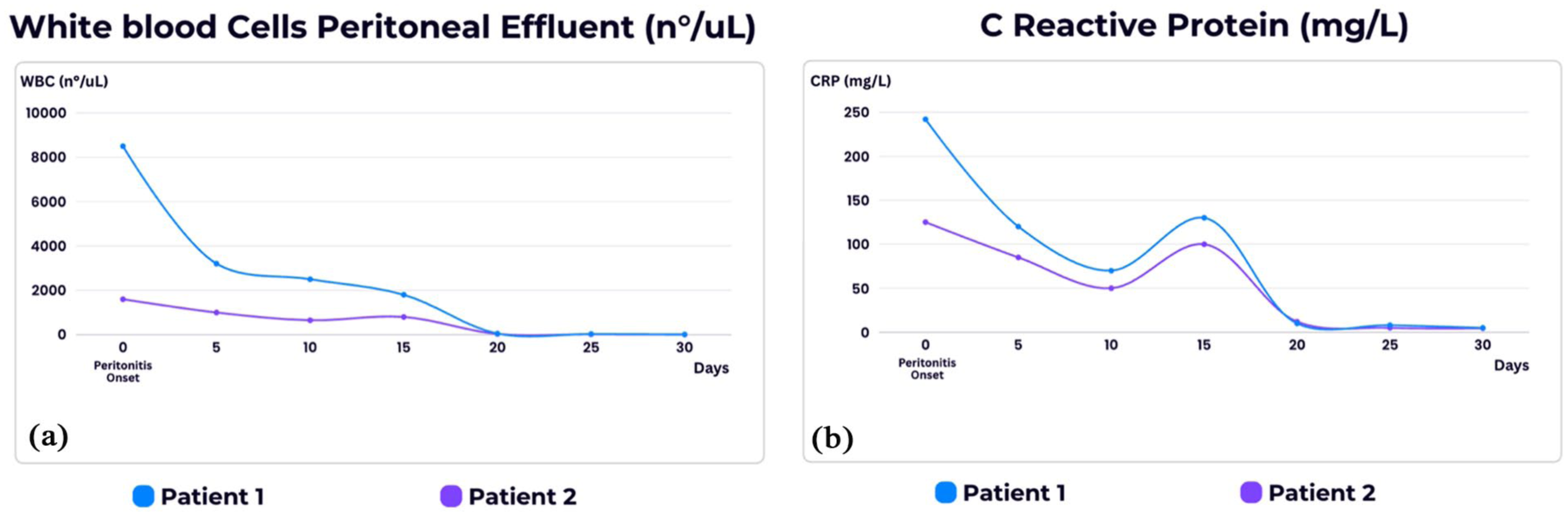
Graphical visualization of (a) white blood cells number in the peritoneal effluent and (b) serum C reactive protein value in relation to the time from peritonitis onset (day 0).
Case patient 2
An 87-year-old white man suffering from ESRD due to undetermined cause started three exchanges (1.36% glucose, 1.1% aminoacids, and 7.5% icodextrin) CAPD in June 2023 with no complications.
His medical history is notable for type 2 diabetes, non-alcoholic fatty liver disease, chronic coronary syndromes, chronic heart failure, and previous acute biliary pancreatis requiring cholecystectomy.
In February 2025 the patient presented at the emergency room reporting the appearance of cloudy peritoneal fluid and complaining abdominal pain. At physical examination the abdomen was moderately hard, not distended, but with rebound tenderness, while at the exit-site no presence of erythema or purulent discharge was observed. The ultrasonography did not detect any anechoic collection along the tunnel of the catheter. The microscopic exam of the peritoneal liquid detected 1600 WBCs/µL, while the blood test results showed (Figure 1): WBCs 9.43 × 109/L, CRP 125 mg/L (normal range <7.5). Empirical therapy with cefazolin and tobramicin ip was started. P. aeruginosa was identified in peritoneal liquid culture and according to the antibiogram, the cefazolin ip was changed to ceftazidime ip while maintaining tobramicin ip. However, despite the improvement of the clinical signs (residual mild diffuse abdominal pain), the reduction of inflammation indexes (WBCs 8.96 × 109/L, CRP 100 mg/L) and the negative liquid peritoneal culture, after 10 days of appropriate antibiotic therapy there were still 800 WBCs/µL in the effluent. It was decided to perform SCR. The maneuver took place without complications and PD exchanges were resumed immediately after the procedure by low volume exchanges (1000 mL). The day after the replacement of the catheter the WBC count in the peritoneal liquid decreased to 168 WBCs/µL along with the resolution of the abdominal symptoms. The inflammatory index started to normalize (blood exams after 5 days: CRP 12.6 mg/L). The microbiological exam carried out on the superficial and deep cuff was negative, while the tip of the catheter resulted positive for P. aeruginosa. The antibiotic therapy was prolonged for further 2 weeks. At the end of therapy, the patient presented a WBC count in the peritoneal liquid equal to 5 WBCs/µL and CRP to 4.5 mg/L (Figure 1). The patient did not experience PD-related complications during the following 3 months and is currently continuing PD.
Discussion
Although the use of SCR as a treatment for refractory peritonitis has been discouraged, the clinical experience shows that the response to antibiotic therapy is heterogenous. In fact, some episodes defined as refractory peritonitis presents an initial clinical and laboratory improvement leading eventually to a steady state without obtaining the complete clearance of leucocytes (<100 WBCs/µL) in the peritoneal effluent. In most of those cases, when a peritoneal liquid culture is repeated, it appears to be negative suggesting an eradication of the microorganism at least in the peritoneal cavity.
Currently, there is growing evidence that refractory peritonitis might be associated with either bacterial adherence to the catheter silastic and biofilm formation along the intraperitoneal portion of the catheter. 10 Assuming this theory, the removal of the catheter should lead to the clearance of the WBC into the dialysate thanks to the removal of the source that hinders the complete healing of the infectious process. At the same time the simultaneous replacement of the catheter would not seem an irrational option in the light of the microbiological negativity of the peritoneal liquid.
On those assumptions, we would propose a novel sub-classification of the refractory peritonitis into “partial” and “complete.” Precisely, we would define complete refractory peritonitis an episode that after 5 days of appropriate antibiotic therapy do not show a significative improvement of clinical signs/symptoms, neither a decrease of WBCs in dialysis effluent ⩾30% with persistent dialysis effluent leukocyte count >100 WBCs/µL. On the other hand, we would describe partial refractory peritonitis as an episode that after 5 days of appropriate antibiotic therapy shows an improvement of clinical signs/symptoms along with a reduction of WBCs in dialysis effluent ⩾30%, but still with an absolute count >100 WBCs/µL.
This distinction could be very relevant to guide the therapeutical approach. In case of partial refractory peritonitis, it could be reasonable to wait for catheter removal while repeating a new effluent culture. In this situation, if after 10 days of appropriate antibiotic therapy dialysis effluent leukocyte count remains >100 WBCs/µL while the peritoneal culture results negative, SCR should take into consideration (Figure 2).
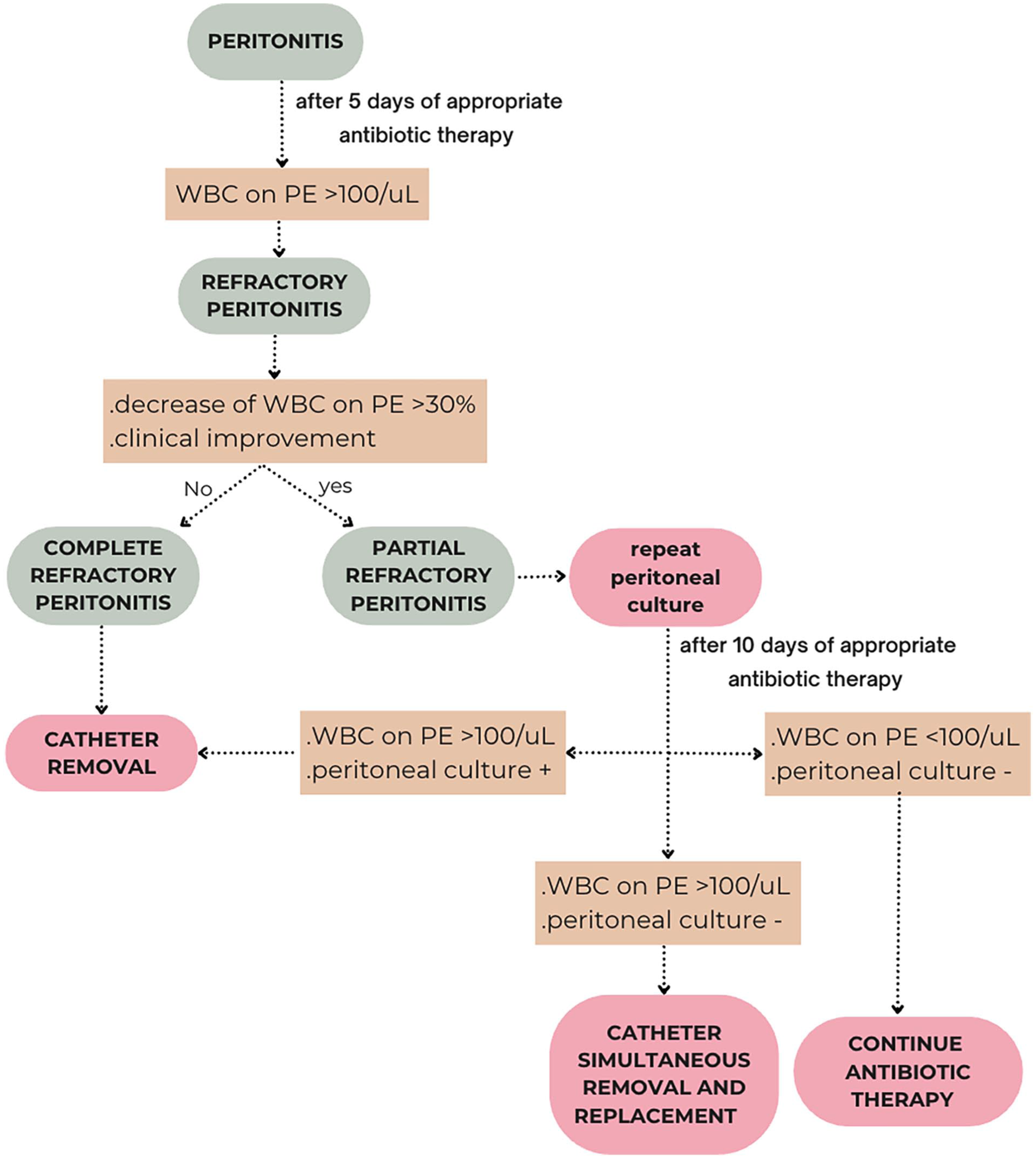
Proposed novel therapeutical algorithm for refractory peritonitis differentiating between complete and partial refractory peritonitis.
In conclusion, we would propose a novel therapeutical algorithm that, extending the concept of refractory peritonitis, distinguishes “complete refractory” from “partial refractory” peritonitis, so that in the latter case SCR could be employed to treat the infectious episode, while at the same time spare the patient the transfer to HD.
Footnotes
Author contributions
Research idea and study design: LN, AS, FT, CA, GC. Each author contributed important intellectual content during manuscript drafting or revision and accepts accountability for the overall work by ensuring that questions pertaining to the accuracy or integrity of any portion of the work are appropriately investigated and resolved.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
No required (retrospective case report undertaken through a case note review).
Informed consent
Informed consent obtained by the patients.
